User login
Partially Blanchable Violaceous Lesions in an AIDS Patient
The Diagnosis: Eruptive Disseminated Kaposi Sarcoma
There are 5 types of Kaposi sarcoma (KS): classic KS, African cutaneous KS, African lymphadenopathic KS, AIDS-related KS, and immunosuppression-associated KS. Immunosuppression-associated KS can occur in the setting of lymphoma or in conjunction with immunosuppressive therapy related to organ transplants and long-term corticosteroid treatment.1,2 Kaposi sarcoma associated with highly active antiretroviral therapy–induced immune reconstitution inflammatory syndrome also may occur.3
The possible causes of the manifestation of KS in our patient were 2-fold: (1) AIDS associated given the patient’s CD4 lymphocyte count of 7 cells/mm3, and (2) iatrogenic secondary to drug-induced immunosuppression that was temporally induced by 2 sustained periods of intravenous dexamethasone for cerebral edema in the setting of primary central nervous system lymphoma. It is unlikely that our patient experienced immune reconstitution inflammatory syndrome–induced KS, as the dysphagia interfered with the ability to take antiretroviral therapy during hospitalization. In patients who have experienced KS in the setting of steroid use or organ transplantation, KS lesions spontaneously improved or completely regressed several months after immunosuppression reduction or removal.1,2,4
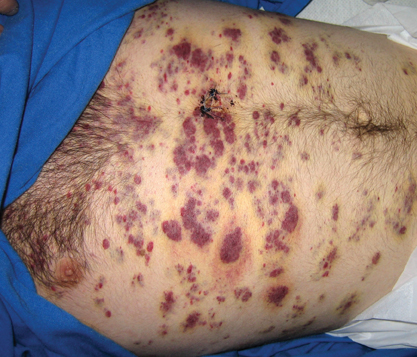
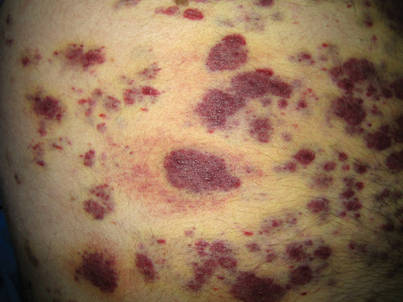
Clinically and morphologically, our patient also clearly demonstrated the occasionally seen striking manifestation of perilesional, ecchymotic-appearing or bruiselike halos surrounding the KS lesions (Figure).
The initial differential diagnosis included hemorrhagic diathesis but later included KS in the setting of AIDS and immunosuppressive therapy with dexamethasone, bacillary angiomatosis, and cutaneous lymphoma. A biopsy of one of the cutaneous lesions confirmed the diagnosis of KS.
Three standard treatments of primary central nervous system lymphoma currently exist: radiation therapy, intrathecal and/or intraventricular chemotherapy, and steroid therapy.5 Given the patient’s risk for opportunistic infections and immunodeficient state, the medical team was constrained in its treatment options, as all of the therapies would further weaken the patient’s immune system.
Treatment of KS can be local and/or systemic based on disease stage, progression, distribution, clinical type, and immune status.6,7 Our patient had generalized cutaneous KS covering more than 50% of the body, thus making local treatments such as radiation therapy, cryotherapy, intralesional chemotherapy with vincristine or vinblastine, excision, laser therapy, or alitretinoin gel impractical. Single- or multiple-agent systemic treatment options for disseminated cutaneous disease with or without internal organ involvement may include liposomal anthracyclines, paclitaxel, gemcitabine, vinblastine, vincristine, bleomycin, etoposide, and interferon-alfa.6,7 Potent combination antiretroviral therapy is the mainstay for treatment of AIDS-associated KS.8
- Nassar D, Schartz NEC, Bouche C, et al. Kaposi’s sarcoma after long-acting steroids: time until remission and drug washout. Dermatology. 2010;220:159-163.
- Trattner A, Hodak E, David M, et al. The appearance of Kaposi sarcoma during corticosteroid therapy. Cancer. 1993;72:1779-1783.
- Bower M, Nelson M, Young AM, et al. Immune reconstitution inflammatory syndrome associated with Kaposi’s Sarcoma. J Clin Oncol. 2005;23:5224-5228.
- Duman S, Töz H, Aşçi G, et al. Successful treatment of post-transplant Kaposi’s sarcoma by reduction of immunosuppression. Nephrol Dial Transplant. 2002;17:892-896.
- National Cancer Institute. Primary CNS lymphoma treatment. http://www.cancer.gov/cancertopics/pdq/treatment/primary-CNS-lymphoma/Patient/page4. Accessed June 10, 2014.
- Schwartz RA, Micali G, Nasca MR, et al. Kaposi sarcoma: a continuing conundrum. J Am Acad Dermatol. 2008;59:179-206.
- Lee F-C, Mitsuyasu RT. Chemotherapy of AIDS-related Kaposi’s sarcoma. Hematol Oncol Clin North Am. 1996;10:1051-1068.
- Dupont C, Vasseur E, Beauchet A, et al. Long-term efficacy on Kaposi’s sarcoma of highly active antiretroviral therapy in a cohort of HIV-positive patients. AIDS. 2000;14:987-993.
The Diagnosis: Eruptive Disseminated Kaposi Sarcoma
There are 5 types of Kaposi sarcoma (KS): classic KS, African cutaneous KS, African lymphadenopathic KS, AIDS-related KS, and immunosuppression-associated KS. Immunosuppression-associated KS can occur in the setting of lymphoma or in conjunction with immunosuppressive therapy related to organ transplants and long-term corticosteroid treatment.1,2 Kaposi sarcoma associated with highly active antiretroviral therapy–induced immune reconstitution inflammatory syndrome also may occur.3
The possible causes of the manifestation of KS in our patient were 2-fold: (1) AIDS associated given the patient’s CD4 lymphocyte count of 7 cells/mm3, and (2) iatrogenic secondary to drug-induced immunosuppression that was temporally induced by 2 sustained periods of intravenous dexamethasone for cerebral edema in the setting of primary central nervous system lymphoma. It is unlikely that our patient experienced immune reconstitution inflammatory syndrome–induced KS, as the dysphagia interfered with the ability to take antiretroviral therapy during hospitalization. In patients who have experienced KS in the setting of steroid use or organ transplantation, KS lesions spontaneously improved or completely regressed several months after immunosuppression reduction or removal.1,2,4
Clinically and morphologically, our patient also clearly demonstrated the occasionally seen striking manifestation of perilesional, ecchymotic-appearing or bruiselike halos surrounding the KS lesions (Figure).
The initial differential diagnosis included hemorrhagic diathesis but later included KS in the setting of AIDS and immunosuppressive therapy with dexamethasone, bacillary angiomatosis, and cutaneous lymphoma. A biopsy of one of the cutaneous lesions confirmed the diagnosis of KS.
Three standard treatments of primary central nervous system lymphoma currently exist: radiation therapy, intrathecal and/or intraventricular chemotherapy, and steroid therapy.5 Given the patient’s risk for opportunistic infections and immunodeficient state, the medical team was constrained in its treatment options, as all of the therapies would further weaken the patient’s immune system.

Treatment of KS can be local and/or systemic based on disease stage, progression, distribution, clinical type, and immune status.6,7 Our patient had generalized cutaneous KS covering more than 50% of the body, thus making local treatments such as radiation therapy, cryotherapy, intralesional chemotherapy with vincristine or vinblastine, excision, laser therapy, or alitretinoin gel impractical. Single- or multiple-agent systemic treatment options for disseminated cutaneous disease with or without internal organ involvement may include liposomal anthracyclines, paclitaxel, gemcitabine, vinblastine, vincristine, bleomycin, etoposide, and interferon-alfa.6,7 Potent combination antiretroviral therapy is the mainstay for treatment of AIDS-associated KS.8
The Diagnosis: Eruptive Disseminated Kaposi Sarcoma
There are 5 types of Kaposi sarcoma (KS): classic KS, African cutaneous KS, African lymphadenopathic KS, AIDS-related KS, and immunosuppression-associated KS. Immunosuppression-associated KS can occur in the setting of lymphoma or in conjunction with immunosuppressive therapy related to organ transplants and long-term corticosteroid treatment.1,2 Kaposi sarcoma associated with highly active antiretroviral therapy–induced immune reconstitution inflammatory syndrome also may occur.3
The possible causes of the manifestation of KS in our patient were 2-fold: (1) AIDS associated given the patient’s CD4 lymphocyte count of 7 cells/mm3, and (2) iatrogenic secondary to drug-induced immunosuppression that was temporally induced by 2 sustained periods of intravenous dexamethasone for cerebral edema in the setting of primary central nervous system lymphoma. It is unlikely that our patient experienced immune reconstitution inflammatory syndrome–induced KS, as the dysphagia interfered with the ability to take antiretroviral therapy during hospitalization. In patients who have experienced KS in the setting of steroid use or organ transplantation, KS lesions spontaneously improved or completely regressed several months after immunosuppression reduction or removal.1,2,4
Clinically and morphologically, our patient also clearly demonstrated the occasionally seen striking manifestation of perilesional, ecchymotic-appearing or bruiselike halos surrounding the KS lesions (Figure).
The initial differential diagnosis included hemorrhagic diathesis but later included KS in the setting of AIDS and immunosuppressive therapy with dexamethasone, bacillary angiomatosis, and cutaneous lymphoma. A biopsy of one of the cutaneous lesions confirmed the diagnosis of KS.
Three standard treatments of primary central nervous system lymphoma currently exist: radiation therapy, intrathecal and/or intraventricular chemotherapy, and steroid therapy.5 Given the patient’s risk for opportunistic infections and immunodeficient state, the medical team was constrained in its treatment options, as all of the therapies would further weaken the patient’s immune system.

Treatment of KS can be local and/or systemic based on disease stage, progression, distribution, clinical type, and immune status.6,7 Our patient had generalized cutaneous KS covering more than 50% of the body, thus making local treatments such as radiation therapy, cryotherapy, intralesional chemotherapy with vincristine or vinblastine, excision, laser therapy, or alitretinoin gel impractical. Single- or multiple-agent systemic treatment options for disseminated cutaneous disease with or without internal organ involvement may include liposomal anthracyclines, paclitaxel, gemcitabine, vinblastine, vincristine, bleomycin, etoposide, and interferon-alfa.6,7 Potent combination antiretroviral therapy is the mainstay for treatment of AIDS-associated KS.8
- Nassar D, Schartz NEC, Bouche C, et al. Kaposi’s sarcoma after long-acting steroids: time until remission and drug washout. Dermatology. 2010;220:159-163.
- Trattner A, Hodak E, David M, et al. The appearance of Kaposi sarcoma during corticosteroid therapy. Cancer. 1993;72:1779-1783.
- Bower M, Nelson M, Young AM, et al. Immune reconstitution inflammatory syndrome associated with Kaposi’s Sarcoma. J Clin Oncol. 2005;23:5224-5228.
- Duman S, Töz H, Aşçi G, et al. Successful treatment of post-transplant Kaposi’s sarcoma by reduction of immunosuppression. Nephrol Dial Transplant. 2002;17:892-896.
- National Cancer Institute. Primary CNS lymphoma treatment. http://www.cancer.gov/cancertopics/pdq/treatment/primary-CNS-lymphoma/Patient/page4. Accessed June 10, 2014.
- Schwartz RA, Micali G, Nasca MR, et al. Kaposi sarcoma: a continuing conundrum. J Am Acad Dermatol. 2008;59:179-206.
- Lee F-C, Mitsuyasu RT. Chemotherapy of AIDS-related Kaposi’s sarcoma. Hematol Oncol Clin North Am. 1996;10:1051-1068.
- Dupont C, Vasseur E, Beauchet A, et al. Long-term efficacy on Kaposi’s sarcoma of highly active antiretroviral therapy in a cohort of HIV-positive patients. AIDS. 2000;14:987-993.
- Nassar D, Schartz NEC, Bouche C, et al. Kaposi’s sarcoma after long-acting steroids: time until remission and drug washout. Dermatology. 2010;220:159-163.
- Trattner A, Hodak E, David M, et al. The appearance of Kaposi sarcoma during corticosteroid therapy. Cancer. 1993;72:1779-1783.
- Bower M, Nelson M, Young AM, et al. Immune reconstitution inflammatory syndrome associated with Kaposi’s Sarcoma. J Clin Oncol. 2005;23:5224-5228.
- Duman S, Töz H, Aşçi G, et al. Successful treatment of post-transplant Kaposi’s sarcoma by reduction of immunosuppression. Nephrol Dial Transplant. 2002;17:892-896.
- National Cancer Institute. Primary CNS lymphoma treatment. http://www.cancer.gov/cancertopics/pdq/treatment/primary-CNS-lymphoma/Patient/page4. Accessed June 10, 2014.
- Schwartz RA, Micali G, Nasca MR, et al. Kaposi sarcoma: a continuing conundrum. J Am Acad Dermatol. 2008;59:179-206.
- Lee F-C, Mitsuyasu RT. Chemotherapy of AIDS-related Kaposi’s sarcoma. Hematol Oncol Clin North Am. 1996;10:1051-1068.
- Dupont C, Vasseur E, Beauchet A, et al. Long-term efficacy on Kaposi’s sarcoma of highly active antiretroviral therapy in a cohort of HIV-positive patients. AIDS. 2000;14:987-993.
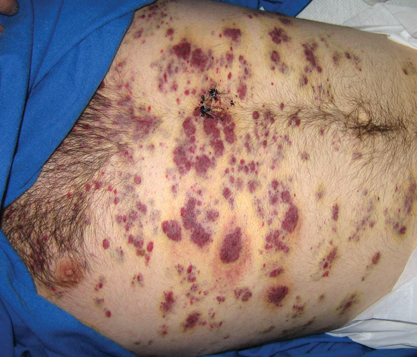
A 37-year-old AIDS patient (CD4 lymphocyte count, 7 cells/mm3 [reference range, 500–1000 cells/mm3]; viral load, >200,000 copies/mL) with a medical history of primary central nervous system lymphoma and recent Salmonella bacteremia was admitted with a 1-week history of dysphagia, generalized weakness, and a 15-lb weight loss over a 2-month period. Medications included prophylaxis with weekly azithromycin and daily atovoquone. The patient had a history of noncompliance with antiretroviral therapy, which included atazanavir sulfate, lamivudine, and zidovudine. One month prior to presentation the patient received a course of intravenous dexamethasone for cerebral edema secondary to mass effect from primary central nervous system lymphoma. On examination the patient was afebrile, cachectic, and in no acute distress. Initially, faint petechial lesions were noted on the torso and upper abdomen. Over the course of 10 days, after reintroduction of intravenous dexamethasone, the patient rapidly and diffusely developed partially blanchable, violaceous macules, patches, papules, and plaques that were most prominent on the trunk and lower extremities. Some of the lesions were surrounded by nonblanchable, yellowish brown, ecchymotic-appearing halos. Lesions spared the oral mucosa, face, and genitalia. There was no evidence of mucocutaneous involvement.