User login
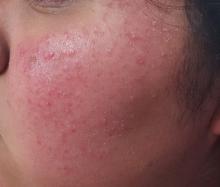
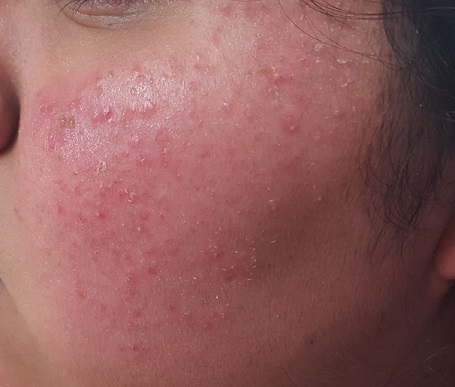
A recent treatment regimen worsened this 13-year-old Native American girl’s “acne.” Within hours of beginning the treatment (application of benzoyl peroxide–containing gel and twice-daily use of a benzoyl peroxide–based cleanser), she reported intense burning and redness in the treated areas. She stopped this regimen after a week, and her primary care provider referred her for evaluation.
The lesions have been on her face since age 2 and are not usually problematic.
The patient has a notable history of atopy, with seasonal allergies and occasional bouts of asthma. She claims to have no other health problems but does admit to being overweight for most of her life; this is an issue for most of her family members, as well. Several of her relatives developed diabetes as adults.
EXAMINATION
The patient is 5 ft tall and weighs 250 lb. She has type IV skin, consistent with her Native American heritage. The posterior aspects of both cheeks are quite red and covered with hyperkeratotic, rough, pinpoint papules. There are no comedones or pustules there or elsewhere on her body.
No other blemishes or lesions are seen on her face, but there are hundreds of hyperkeratotic papules on her bilateral triceps. The skin in all her intertriginous (skin-on-skin) areas is quite dark and has a faintly papular, velvety appearance.
What is the diagnosis?
DISCUSSION
This girl’s facial and arm condition is keratosis pilaris (KP), an extremely common and harmless problem that affects up to 70% of newborns, though it may not fully express until age 1 or 2. Caused by an overproduction of perifollicular keratin, KP is inherited in an autosomal dominant pattern and is often seen in conjunction with atopic dermatitis and related conditions (eg, eczema, xerosis, asthma, icthyosis). KP can affect skin anywhere on the body except glabrous skin (palms and soles).
Variants of KP are also common; the one affecting this patient is keratosis pilaris rubra facei. This condition is often confused with acne, but treating it as such worsens irritation—especially in the wintertime, when humidity levels are low.
The presence of the patient’s condition from such an early age, the lack of comedones or pustules, and the discovery of more typical KP lesions on her arms all served to rule out acne and rosacea (the other item in the differential). The intertriginous hyperpigmentation represents acanthosis nigricans, reflecting her obese and (probable) prediabetic state, and is unrelated to her KP.
She will be treated with a one-week course of 2.5% hydrocortisone cream (bid application) and cessation of benzoyl peroxide–containing products. The condition should improve rapidly and become less prominent over time. Given the nature of KP, I have also found it helpful to encourage parents of affected children to research the condition online, to reinforce the information I’ve provided in the clinic.
TAKE-HOME LEARNING POINTS
• Keratosis pilaris (KP) is extremely common, affecting up to 70% of all newborns.
• Keratosis pilaris rubra facei, a common variant, affects the posterior two-thirds of the cheeks. Virtually all patients with this form will also exhibit KP on more typical areas (eg, the triceps).
• While there is no cure, moisturization helps to ease symptoms, as do other products (eg, salicylic acid–containing creams).
• KP is often mistaken for acne; unfortunately, treatment as such is counterproductive.
A recent treatment regimen worsened this 13-year-old Native American girl’s “acne.” Within hours of beginning the treatment (application of benzoyl peroxide–containing gel and twice-daily use of a benzoyl peroxide–based cleanser), she reported intense burning and redness in the treated areas. She stopped this regimen after a week, and her primary care provider referred her for evaluation.
The lesions have been on her face since age 2 and are not usually problematic.
The patient has a notable history of atopy, with seasonal allergies and occasional bouts of asthma. She claims to have no other health problems but does admit to being overweight for most of her life; this is an issue for most of her family members, as well. Several of her relatives developed diabetes as adults.
EXAMINATION
The patient is 5 ft tall and weighs 250 lb. She has type IV skin, consistent with her Native American heritage. The posterior aspects of both cheeks are quite red and covered with hyperkeratotic, rough, pinpoint papules. There are no comedones or pustules there or elsewhere on her body.
No other blemishes or lesions are seen on her face, but there are hundreds of hyperkeratotic papules on her bilateral triceps. The skin in all her intertriginous (skin-on-skin) areas is quite dark and has a faintly papular, velvety appearance.
What is the diagnosis?
DISCUSSION
This girl’s facial and arm condition is keratosis pilaris (KP), an extremely common and harmless problem that affects up to 70% of newborns, though it may not fully express until age 1 or 2. Caused by an overproduction of perifollicular keratin, KP is inherited in an autosomal dominant pattern and is often seen in conjunction with atopic dermatitis and related conditions (eg, eczema, xerosis, asthma, icthyosis). KP can affect skin anywhere on the body except glabrous skin (palms and soles).
Variants of KP are also common; the one affecting this patient is keratosis pilaris rubra facei. This condition is often confused with acne, but treating it as such worsens irritation—especially in the wintertime, when humidity levels are low.
The presence of the patient’s condition from such an early age, the lack of comedones or pustules, and the discovery of more typical KP lesions on her arms all served to rule out acne and rosacea (the other item in the differential). The intertriginous hyperpigmentation represents acanthosis nigricans, reflecting her obese and (probable) prediabetic state, and is unrelated to her KP.
She will be treated with a one-week course of 2.5% hydrocortisone cream (bid application) and cessation of benzoyl peroxide–containing products. The condition should improve rapidly and become less prominent over time. Given the nature of KP, I have also found it helpful to encourage parents of affected children to research the condition online, to reinforce the information I’ve provided in the clinic.
TAKE-HOME LEARNING POINTS
• Keratosis pilaris (KP) is extremely common, affecting up to 70% of all newborns.
• Keratosis pilaris rubra facei, a common variant, affects the posterior two-thirds of the cheeks. Virtually all patients with this form will also exhibit KP on more typical areas (eg, the triceps).
• While there is no cure, moisturization helps to ease symptoms, as do other products (eg, salicylic acid–containing creams).
• KP is often mistaken for acne; unfortunately, treatment as such is counterproductive.
A recent treatment regimen worsened this 13-year-old Native American girl’s “acne.” Within hours of beginning the treatment (application of benzoyl peroxide–containing gel and twice-daily use of a benzoyl peroxide–based cleanser), she reported intense burning and redness in the treated areas. She stopped this regimen after a week, and her primary care provider referred her for evaluation.
The lesions have been on her face since age 2 and are not usually problematic.
The patient has a notable history of atopy, with seasonal allergies and occasional bouts of asthma. She claims to have no other health problems but does admit to being overweight for most of her life; this is an issue for most of her family members, as well. Several of her relatives developed diabetes as adults.
EXAMINATION
The patient is 5 ft tall and weighs 250 lb. She has type IV skin, consistent with her Native American heritage. The posterior aspects of both cheeks are quite red and covered with hyperkeratotic, rough, pinpoint papules. There are no comedones or pustules there or elsewhere on her body.
No other blemishes or lesions are seen on her face, but there are hundreds of hyperkeratotic papules on her bilateral triceps. The skin in all her intertriginous (skin-on-skin) areas is quite dark and has a faintly papular, velvety appearance.
What is the diagnosis?
DISCUSSION
This girl’s facial and arm condition is keratosis pilaris (KP), an extremely common and harmless problem that affects up to 70% of newborns, though it may not fully express until age 1 or 2. Caused by an overproduction of perifollicular keratin, KP is inherited in an autosomal dominant pattern and is often seen in conjunction with atopic dermatitis and related conditions (eg, eczema, xerosis, asthma, icthyosis). KP can affect skin anywhere on the body except glabrous skin (palms and soles).
Variants of KP are also common; the one affecting this patient is keratosis pilaris rubra facei. This condition is often confused with acne, but treating it as such worsens irritation—especially in the wintertime, when humidity levels are low.
The presence of the patient’s condition from such an early age, the lack of comedones or pustules, and the discovery of more typical KP lesions on her arms all served to rule out acne and rosacea (the other item in the differential). The intertriginous hyperpigmentation represents acanthosis nigricans, reflecting her obese and (probable) prediabetic state, and is unrelated to her KP.
She will be treated with a one-week course of 2.5% hydrocortisone cream (bid application) and cessation of benzoyl peroxide–containing products. The condition should improve rapidly and become less prominent over time. Given the nature of KP, I have also found it helpful to encourage parents of affected children to research the condition online, to reinforce the information I’ve provided in the clinic.
TAKE-HOME LEARNING POINTS
• Keratosis pilaris (KP) is extremely common, affecting up to 70% of all newborns.
• Keratosis pilaris rubra facei, a common variant, affects the posterior two-thirds of the cheeks. Virtually all patients with this form will also exhibit KP on more typical areas (eg, the triceps).
• While there is no cure, moisturization helps to ease symptoms, as do other products (eg, salicylic acid–containing creams).
• KP is often mistaken for acne; unfortunately, treatment as such is counterproductive.