User login
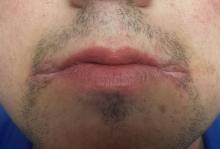
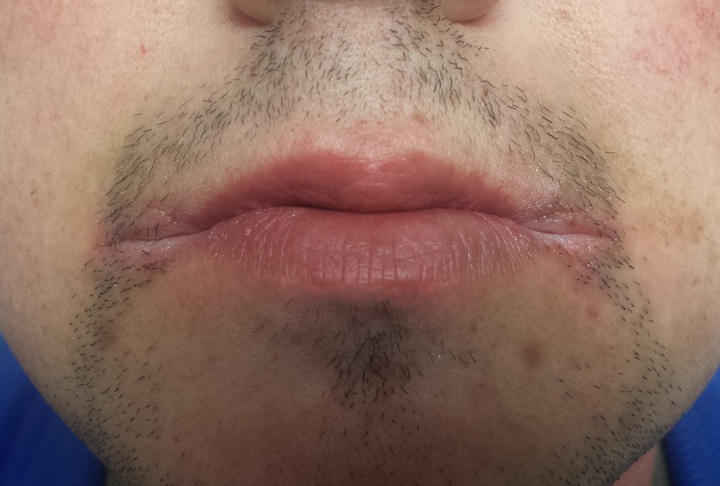
A 25-year-old man presents to dermatology with a “yeast infection” at the corners of his mouth that has failed to respond to anti-yeast creams (nystatin, clotrimazole) and oral medications (fluconazole). He has also tried a variety of “home remedies,” including hydrogen peroxide, rubbing alcohol, mouthwash, diaper cream, triple-antibiotic ointment, and tea tree oil. If anything, these seemed to worsen the problem.
He is fairly sure the problem developed because, several weeks ago, he shaved too close in the affected area. Soon after, he went to the dentist, who suggested the problem might be caused by a vitamin deficiency—but several weeks of taking a multivitamin produced no discernable result.
The affected area is irritated and sometimes painful, and he has a hard time leaving it alone. Several times a day, despite knowing how counterproductive it is, he finds himself picking at it. But worst of all, to the patient, is the fact that his girlfriend refuses to let him near her, citing fears of contagion.
The patient claims to be in good health otherwise, although his history includes seasonal allergies and eczema.
EXAMINATION
The corners of the patient’s mouth are quite macerated, eroded, and focally scaly, with modest erythema. There is no edema or tenderness on palpation. Examination of the inside of his mouth is within normal limits.
What is the diagnosis?
DISCUSSION
This is a typical clinical and historical snapshot of a very common problem: angular stomatitis (AS), also known as perleche or angular cheilitis (among others). A rather simple problem, it nonetheless causes confusion in primary care settings.
Virtually every AS patient I’ve seen was referred to dermatology after trying at least half a dozen different treatments. These attempts rarely work—and even if one of them did, the average AS patient wouldn’t realize it, because he’s almost always using several medications simultaneously.
AS, in its usual form, is not a complex problem. Thin tissue at the corner of the mouth is traumatized (shaving is one method, but another is holding the mouth open for two hours while at the dentist), and then the patient often picks at the resulting scale, making it worse. During sleep, saliva may flow onto the affected area, causing maceration and further damaging already irritated skin. The saliva introduces a multitude of bacteria, yeast, and other micro-organisms to this damaged tissue, further contributing to the inflammation.
At this point, some patients will panic, compounding the problem by throwing anything and everything they can think of at it: lip balm, peroxide, alcohol, triple-antibiotic ointment. If they seek professional help, they are often given a prescription for an oral anti-yeast medication (eg, fluconazole). Seldom does this help, and for a very good reason: Even though Candida is almost always present in and around the mouth—and may well contribute to the problem—only rarely is the issue a “yeast infection.” In the rare instances I’ve seen this, the patient was immunosuppressed.
In its simplest and most common form, AS is a form of intertrigo, in which inflammation is perpetuated by moist skin on skin—in this case, by the little channel created by the labial commissures. We see essentially the same thing under the breasts, in the axillae, in the folds of the abdomen, and in the groin. These manifestations are almost always diagnosed as “yeast infection,” even though treatment for such usually fails.
Patients who might find themselves particularly susceptible to AS include those with poorly fitting dentures, which allow overclosure of the mouth, accentuating the labial folds; those with atopy, whose skin is already thin and easily irritated; and those with seasonal allergies, who mouth-breathe while sleeping, drying out their lips while drooling from the corners of the mouth. Select patients may have true vitamin or mineral deficiencies (eg, zinc) due to poor dietary intake.
The majority of AS patients respond quite well to a combination of a topical imidazole cream or ointment (eg, miconazole or oxiconazole) and a mid-strength topical steroid ointment (eg, 2.5% hydrocortisone), mixed half and half by hand and applied twice a day. The patient must be persuaded to stop using all other contactants, since these often perpetuate the problem. Once the condition is under control (usually within a week), the application of petroleum jelly will help to prevent recurrences.
TAKE-HOME LEARNING POINTS
• Angular stomatitis (AS) typically represents inflammation of thin, sensitive lip skin; the irritation is perpetuated by saliva, which causes maceration and makes the tissue vulnerable to the normal flora present in every human mouth.
• Though AS is not an infection, it can be worsened by micro-organisms, especially yeast—but monotherapy with anti-yeast medication almost always fails.
• Effective treatment must address the inflammation, via the application of a topical steroid and cessation of all other topical treatments in case they’re contributory.
• Prevention of recurrences may require the patient to address a chronic dental problem, or the provider to rule out less typical causes (eg, dietary deficiencies).
A 25-year-old man presents to dermatology with a “yeast infection” at the corners of his mouth that has failed to respond to anti-yeast creams (nystatin, clotrimazole) and oral medications (fluconazole). He has also tried a variety of “home remedies,” including hydrogen peroxide, rubbing alcohol, mouthwash, diaper cream, triple-antibiotic ointment, and tea tree oil. If anything, these seemed to worsen the problem.
He is fairly sure the problem developed because, several weeks ago, he shaved too close in the affected area. Soon after, he went to the dentist, who suggested the problem might be caused by a vitamin deficiency—but several weeks of taking a multivitamin produced no discernable result.
The affected area is irritated and sometimes painful, and he has a hard time leaving it alone. Several times a day, despite knowing how counterproductive it is, he finds himself picking at it. But worst of all, to the patient, is the fact that his girlfriend refuses to let him near her, citing fears of contagion.
The patient claims to be in good health otherwise, although his history includes seasonal allergies and eczema.
EXAMINATION
The corners of the patient’s mouth are quite macerated, eroded, and focally scaly, with modest erythema. There is no edema or tenderness on palpation. Examination of the inside of his mouth is within normal limits.
What is the diagnosis?
DISCUSSION
This is a typical clinical and historical snapshot of a very common problem: angular stomatitis (AS), also known as perleche or angular cheilitis (among others). A rather simple problem, it nonetheless causes confusion in primary care settings.
Virtually every AS patient I’ve seen was referred to dermatology after trying at least half a dozen different treatments. These attempts rarely work—and even if one of them did, the average AS patient wouldn’t realize it, because he’s almost always using several medications simultaneously.
AS, in its usual form, is not a complex problem. Thin tissue at the corner of the mouth is traumatized (shaving is one method, but another is holding the mouth open for two hours while at the dentist), and then the patient often picks at the resulting scale, making it worse. During sleep, saliva may flow onto the affected area, causing maceration and further damaging already irritated skin. The saliva introduces a multitude of bacteria, yeast, and other micro-organisms to this damaged tissue, further contributing to the inflammation.
At this point, some patients will panic, compounding the problem by throwing anything and everything they can think of at it: lip balm, peroxide, alcohol, triple-antibiotic ointment. If they seek professional help, they are often given a prescription for an oral anti-yeast medication (eg, fluconazole). Seldom does this help, and for a very good reason: Even though Candida is almost always present in and around the mouth—and may well contribute to the problem—only rarely is the issue a “yeast infection.” In the rare instances I’ve seen this, the patient was immunosuppressed.
In its simplest and most common form, AS is a form of intertrigo, in which inflammation is perpetuated by moist skin on skin—in this case, by the little channel created by the labial commissures. We see essentially the same thing under the breasts, in the axillae, in the folds of the abdomen, and in the groin. These manifestations are almost always diagnosed as “yeast infection,” even though treatment for such usually fails.
Patients who might find themselves particularly susceptible to AS include those with poorly fitting dentures, which allow overclosure of the mouth, accentuating the labial folds; those with atopy, whose skin is already thin and easily irritated; and those with seasonal allergies, who mouth-breathe while sleeping, drying out their lips while drooling from the corners of the mouth. Select patients may have true vitamin or mineral deficiencies (eg, zinc) due to poor dietary intake.
The majority of AS patients respond quite well to a combination of a topical imidazole cream or ointment (eg, miconazole or oxiconazole) and a mid-strength topical steroid ointment (eg, 2.5% hydrocortisone), mixed half and half by hand and applied twice a day. The patient must be persuaded to stop using all other contactants, since these often perpetuate the problem. Once the condition is under control (usually within a week), the application of petroleum jelly will help to prevent recurrences.
TAKE-HOME LEARNING POINTS
• Angular stomatitis (AS) typically represents inflammation of thin, sensitive lip skin; the irritation is perpetuated by saliva, which causes maceration and makes the tissue vulnerable to the normal flora present in every human mouth.
• Though AS is not an infection, it can be worsened by micro-organisms, especially yeast—but monotherapy with anti-yeast medication almost always fails.
• Effective treatment must address the inflammation, via the application of a topical steroid and cessation of all other topical treatments in case they’re contributory.
• Prevention of recurrences may require the patient to address a chronic dental problem, or the provider to rule out less typical causes (eg, dietary deficiencies).
A 25-year-old man presents to dermatology with a “yeast infection” at the corners of his mouth that has failed to respond to anti-yeast creams (nystatin, clotrimazole) and oral medications (fluconazole). He has also tried a variety of “home remedies,” including hydrogen peroxide, rubbing alcohol, mouthwash, diaper cream, triple-antibiotic ointment, and tea tree oil. If anything, these seemed to worsen the problem.
He is fairly sure the problem developed because, several weeks ago, he shaved too close in the affected area. Soon after, he went to the dentist, who suggested the problem might be caused by a vitamin deficiency—but several weeks of taking a multivitamin produced no discernable result.
The affected area is irritated and sometimes painful, and he has a hard time leaving it alone. Several times a day, despite knowing how counterproductive it is, he finds himself picking at it. But worst of all, to the patient, is the fact that his girlfriend refuses to let him near her, citing fears of contagion.
The patient claims to be in good health otherwise, although his history includes seasonal allergies and eczema.
EXAMINATION
The corners of the patient’s mouth are quite macerated, eroded, and focally scaly, with modest erythema. There is no edema or tenderness on palpation. Examination of the inside of his mouth is within normal limits.
What is the diagnosis?
DISCUSSION
This is a typical clinical and historical snapshot of a very common problem: angular stomatitis (AS), also known as perleche or angular cheilitis (among others). A rather simple problem, it nonetheless causes confusion in primary care settings.
Virtually every AS patient I’ve seen was referred to dermatology after trying at least half a dozen different treatments. These attempts rarely work—and even if one of them did, the average AS patient wouldn’t realize it, because he’s almost always using several medications simultaneously.
AS, in its usual form, is not a complex problem. Thin tissue at the corner of the mouth is traumatized (shaving is one method, but another is holding the mouth open for two hours while at the dentist), and then the patient often picks at the resulting scale, making it worse. During sleep, saliva may flow onto the affected area, causing maceration and further damaging already irritated skin. The saliva introduces a multitude of bacteria, yeast, and other micro-organisms to this damaged tissue, further contributing to the inflammation.
At this point, some patients will panic, compounding the problem by throwing anything and everything they can think of at it: lip balm, peroxide, alcohol, triple-antibiotic ointment. If they seek professional help, they are often given a prescription for an oral anti-yeast medication (eg, fluconazole). Seldom does this help, and for a very good reason: Even though Candida is almost always present in and around the mouth—and may well contribute to the problem—only rarely is the issue a “yeast infection.” In the rare instances I’ve seen this, the patient was immunosuppressed.
In its simplest and most common form, AS is a form of intertrigo, in which inflammation is perpetuated by moist skin on skin—in this case, by the little channel created by the labial commissures. We see essentially the same thing under the breasts, in the axillae, in the folds of the abdomen, and in the groin. These manifestations are almost always diagnosed as “yeast infection,” even though treatment for such usually fails.
Patients who might find themselves particularly susceptible to AS include those with poorly fitting dentures, which allow overclosure of the mouth, accentuating the labial folds; those with atopy, whose skin is already thin and easily irritated; and those with seasonal allergies, who mouth-breathe while sleeping, drying out their lips while drooling from the corners of the mouth. Select patients may have true vitamin or mineral deficiencies (eg, zinc) due to poor dietary intake.
The majority of AS patients respond quite well to a combination of a topical imidazole cream or ointment (eg, miconazole or oxiconazole) and a mid-strength topical steroid ointment (eg, 2.5% hydrocortisone), mixed half and half by hand and applied twice a day. The patient must be persuaded to stop using all other contactants, since these often perpetuate the problem. Once the condition is under control (usually within a week), the application of petroleum jelly will help to prevent recurrences.
TAKE-HOME LEARNING POINTS
• Angular stomatitis (AS) typically represents inflammation of thin, sensitive lip skin; the irritation is perpetuated by saliva, which causes maceration and makes the tissue vulnerable to the normal flora present in every human mouth.
• Though AS is not an infection, it can be worsened by micro-organisms, especially yeast—but monotherapy with anti-yeast medication almost always fails.
• Effective treatment must address the inflammation, via the application of a topical steroid and cessation of all other topical treatments in case they’re contributory.
• Prevention of recurrences may require the patient to address a chronic dental problem, or the provider to rule out less typical causes (eg, dietary deficiencies).