User login
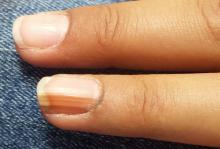
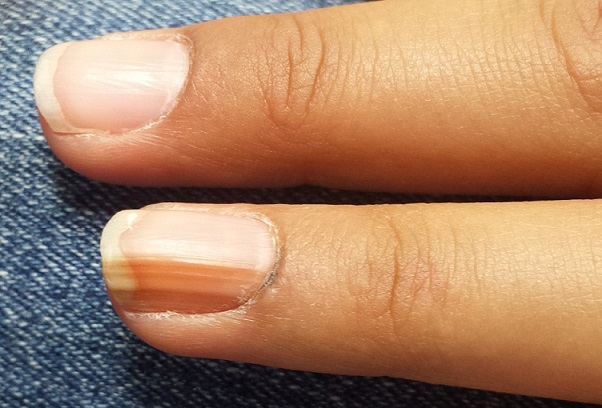
A 14-year-old girl is brought to dermatology by her mother, following referral from her pediatrician for evaluation of fingernail changes. Initially, a faint brown streak was observed in the nail of her left fourth finger. Over time, the spot darkened and widened, and the adjacent nail plate flattened.
A few weeks before presentation to dermatology, the adjacent cuticle darkened. The patient denies any sensitivity in the area. Her mother denies any significant or relevant medical history.
EXAMINATION
The dark brown streak measures 4.5 mm in width and runs longitudinally the entire length of the nail plate. The discolored area coincides exactly with flattening of the nail plate, which, when viewed on edge, also exhibits darkening. Significantly, the adjacent cuticle is similarly affected.
No changes are observed on other digits. The child is of Native American ancestry, with type IV skin.
What is the diagnosis?
DISCUSSION
Generically, this problem is termed melanonychia; this case represents the most common type, longitudinal melanonychia (LM). Typically, it originates in the nail matrix with increased melanin production; this causes darkening of the onchocytes, which migrate distally as the nail plate grows.
This benign version is an extremely common problem, especially in darker-skinned patients. Almost 100% of African-Americans older than 50 have it, often in several nails, as do 77% of African Americans older than 20 and 10% to 20% of Japanese persons. Comparatively, only 1% to 2% of white individuals are affected.
The main significance of LM, of course, is the fact that it can represent melanoma, which, for a variety of reasons, is often belatedly identified in subungual areas and is therefore associated with relatively poor survival. Five-year survival rates for subungual melanoma are around 30%, while 10-year survival is only 13%—much lower than for melanomas elsewhere on the body. For example, patients with melanomas removed from other areas of the hand demonstrate 100% five-year survival rates.
Subungual melanoma presenting in this manner is considered one of the so-called acrolentiginous melanomas, which present in peripheral “acral” locations (eg, scalp, soles, mucosal surfaces). While these are not inherently more dangerous in terms of biologic behavior, they tend to escape detection because of their location and (often) atypical appearance, thus having more time in which to become invasive.
Perhaps the most useful and puzzling conundrum associated with acrolentiginous melanomas is this: Darker-skinned patients are, in general, at low risk for melanoma compared to fair-skinned redheads and blondes. However, when dark-skinned patients do develop melanoma, it tends to manifest in an acral area (one reason why melanoma in these patients has a relatively poor prognosis).
Darkening under or in the nails can have other causes; it has been associated with Cushing disease, Addison disease, and alkaptonuria, to name just a few. It can also be associated with skin diseases, including psoriasis, Darier disease, lichen planus, and lichen striatus. A number of drugs, among them minocycline, can produce focal discoloration in or under the nails.
This subungual lesion was biopsied at its proximal origin, under digital block and using a tourniquet. The 3-mm punch specimen was sent for pathologic examination, which showed benign nevoid tissue—effectively ruling out melanoma. Even if the nail is permanently deformed, this was considered a small price to pay for the patient’s peace of mind.
TAKE-HOME LEARNING POINTS
• Dark streaks under fingernails are common in those with darker skin, in whom they often appear in multiple fingers. In the absence of change, these are usually safe.
• The related conundrum is that when those with darker skin develop melanoma, the subungual areas, or other light-skinned areas (sole, mouth, palms), are often where it manifests.
• New and/or changing areas of subungual pigmentation need to be referred to dermatology for evaluation and possible biopsy.
• When this discoloration also involves the adjacent cuticle or other perionychial skin, even more urgency is added to the referral.
A 14-year-old girl is brought to dermatology by her mother, following referral from her pediatrician for evaluation of fingernail changes. Initially, a faint brown streak was observed in the nail of her left fourth finger. Over time, the spot darkened and widened, and the adjacent nail plate flattened.
A few weeks before presentation to dermatology, the adjacent cuticle darkened. The patient denies any sensitivity in the area. Her mother denies any significant or relevant medical history.
EXAMINATION
The dark brown streak measures 4.5 mm in width and runs longitudinally the entire length of the nail plate. The discolored area coincides exactly with flattening of the nail plate, which, when viewed on edge, also exhibits darkening. Significantly, the adjacent cuticle is similarly affected.
No changes are observed on other digits. The child is of Native American ancestry, with type IV skin.
What is the diagnosis?
DISCUSSION
Generically, this problem is termed melanonychia; this case represents the most common type, longitudinal melanonychia (LM). Typically, it originates in the nail matrix with increased melanin production; this causes darkening of the onchocytes, which migrate distally as the nail plate grows.
This benign version is an extremely common problem, especially in darker-skinned patients. Almost 100% of African-Americans older than 50 have it, often in several nails, as do 77% of African Americans older than 20 and 10% to 20% of Japanese persons. Comparatively, only 1% to 2% of white individuals are affected.
The main significance of LM, of course, is the fact that it can represent melanoma, which, for a variety of reasons, is often belatedly identified in subungual areas and is therefore associated with relatively poor survival. Five-year survival rates for subungual melanoma are around 30%, while 10-year survival is only 13%—much lower than for melanomas elsewhere on the body. For example, patients with melanomas removed from other areas of the hand demonstrate 100% five-year survival rates.
Subungual melanoma presenting in this manner is considered one of the so-called acrolentiginous melanomas, which present in peripheral “acral” locations (eg, scalp, soles, mucosal surfaces). While these are not inherently more dangerous in terms of biologic behavior, they tend to escape detection because of their location and (often) atypical appearance, thus having more time in which to become invasive.
Perhaps the most useful and puzzling conundrum associated with acrolentiginous melanomas is this: Darker-skinned patients are, in general, at low risk for melanoma compared to fair-skinned redheads and blondes. However, when dark-skinned patients do develop melanoma, it tends to manifest in an acral area (one reason why melanoma in these patients has a relatively poor prognosis).
Darkening under or in the nails can have other causes; it has been associated with Cushing disease, Addison disease, and alkaptonuria, to name just a few. It can also be associated with skin diseases, including psoriasis, Darier disease, lichen planus, and lichen striatus. A number of drugs, among them minocycline, can produce focal discoloration in or under the nails.
This subungual lesion was biopsied at its proximal origin, under digital block and using a tourniquet. The 3-mm punch specimen was sent for pathologic examination, which showed benign nevoid tissue—effectively ruling out melanoma. Even if the nail is permanently deformed, this was considered a small price to pay for the patient’s peace of mind.
TAKE-HOME LEARNING POINTS
• Dark streaks under fingernails are common in those with darker skin, in whom they often appear in multiple fingers. In the absence of change, these are usually safe.
• The related conundrum is that when those with darker skin develop melanoma, the subungual areas, or other light-skinned areas (sole, mouth, palms), are often where it manifests.
• New and/or changing areas of subungual pigmentation need to be referred to dermatology for evaluation and possible biopsy.
• When this discoloration also involves the adjacent cuticle or other perionychial skin, even more urgency is added to the referral.
A 14-year-old girl is brought to dermatology by her mother, following referral from her pediatrician for evaluation of fingernail changes. Initially, a faint brown streak was observed in the nail of her left fourth finger. Over time, the spot darkened and widened, and the adjacent nail plate flattened.
A few weeks before presentation to dermatology, the adjacent cuticle darkened. The patient denies any sensitivity in the area. Her mother denies any significant or relevant medical history.
EXAMINATION
The dark brown streak measures 4.5 mm in width and runs longitudinally the entire length of the nail plate. The discolored area coincides exactly with flattening of the nail plate, which, when viewed on edge, also exhibits darkening. Significantly, the adjacent cuticle is similarly affected.
No changes are observed on other digits. The child is of Native American ancestry, with type IV skin.
What is the diagnosis?
DISCUSSION
Generically, this problem is termed melanonychia; this case represents the most common type, longitudinal melanonychia (LM). Typically, it originates in the nail matrix with increased melanin production; this causes darkening of the onchocytes, which migrate distally as the nail plate grows.
This benign version is an extremely common problem, especially in darker-skinned patients. Almost 100% of African-Americans older than 50 have it, often in several nails, as do 77% of African Americans older than 20 and 10% to 20% of Japanese persons. Comparatively, only 1% to 2% of white individuals are affected.
The main significance of LM, of course, is the fact that it can represent melanoma, which, for a variety of reasons, is often belatedly identified in subungual areas and is therefore associated with relatively poor survival. Five-year survival rates for subungual melanoma are around 30%, while 10-year survival is only 13%—much lower than for melanomas elsewhere on the body. For example, patients with melanomas removed from other areas of the hand demonstrate 100% five-year survival rates.
Subungual melanoma presenting in this manner is considered one of the so-called acrolentiginous melanomas, which present in peripheral “acral” locations (eg, scalp, soles, mucosal surfaces). While these are not inherently more dangerous in terms of biologic behavior, they tend to escape detection because of their location and (often) atypical appearance, thus having more time in which to become invasive.
Perhaps the most useful and puzzling conundrum associated with acrolentiginous melanomas is this: Darker-skinned patients are, in general, at low risk for melanoma compared to fair-skinned redheads and blondes. However, when dark-skinned patients do develop melanoma, it tends to manifest in an acral area (one reason why melanoma in these patients has a relatively poor prognosis).
Darkening under or in the nails can have other causes; it has been associated with Cushing disease, Addison disease, and alkaptonuria, to name just a few. It can also be associated with skin diseases, including psoriasis, Darier disease, lichen planus, and lichen striatus. A number of drugs, among them minocycline, can produce focal discoloration in or under the nails.
This subungual lesion was biopsied at its proximal origin, under digital block and using a tourniquet. The 3-mm punch specimen was sent for pathologic examination, which showed benign nevoid tissue—effectively ruling out melanoma. Even if the nail is permanently deformed, this was considered a small price to pay for the patient’s peace of mind.
TAKE-HOME LEARNING POINTS
• Dark streaks under fingernails are common in those with darker skin, in whom they often appear in multiple fingers. In the absence of change, these are usually safe.
• The related conundrum is that when those with darker skin develop melanoma, the subungual areas, or other light-skinned areas (sole, mouth, palms), are often where it manifests.
• New and/or changing areas of subungual pigmentation need to be referred to dermatology for evaluation and possible biopsy.
• When this discoloration also involves the adjacent cuticle or other perionychial skin, even more urgency is added to the referral.