User login
HISTORY
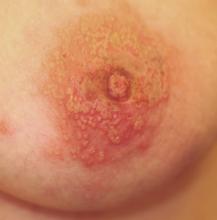
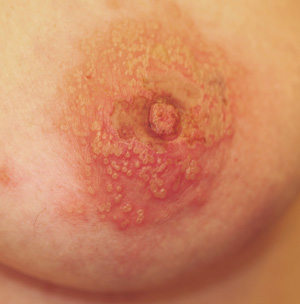
A 43-year-old woman presents with a six-day history of what began with tingling and itching in her left nipple area, but quickly progressed into a collection of tiny blisters that almost cover the central two-thirds of her breast. In the past few days, the itching has subsided, only to be replaced by lancinating pain.
She claims good health otherwise, but admits that lately she has felt a little achy and tired. On questioning, she recalls that about a week before the first signs of the eruption, she had an upper respiratory tract infection. Though she has had cold sores in her life, episodes have been widely spaced and minor, with extralabial involvement.
DIAGNOSIS
The collection of discrete and confluent vesicles is truly impressive and is underlain with an erythematous base. Swelling is minimal, and there is no tenderness. Several of the discrete vesicles are umbilicated, and most are full of what appear to be pus.
In all likelihood, this presentation represents herpes zoster rather than herpes simplex virus (HSV). In my opinion, it’s not worth trying to distinguish between the two, since they’re treated essentially the same in an immunocompetent patient.
LEARNING POINTS
The factor that most helped me arrive at the correct diagnosis was the pain, which was moderately severe and which is seldom seen with HSV. Also supportive of zoster were the widely scattered, sparse clusters of tiny vesicles on faintly erythematous bases, seen elsewhere on the trunk. I’m confident that these are lesions caused by zoster and not HSV.
The real “test” that will differentiate between zoster and HSV is this: If it’s HSV, chances are it will recur in the same area, probably repeatedly. Only a tiny percentage of zoster patients ever experience a recurrence.
As you might suspect, the pus seen in these lesions led the primary care providers the patient consulted first to prescribe oral antibiotics and topical mupirocin ointment. But far from pathognomic for bacterial infection, pus—a liquefied collection of dead white cells—is seen in many other conditions, such as fungal infections, psoriasis, yeast infection, and viral infection.
Other diagnostic features favoring zoster were:
• The premonitory symptoms of tingling and itch that preceded the appearance of the vesicles
• The umbilicated centers of many of the lesions
• The sensitivity in response to mild stroking, which was far more notable in the left breast than in the right; called dysesthesia, this sensation is typical of the many effects of the neurotropic herpes family
• The particular kind of pain (“lancinating”) the patient felt; this is thought to represent inflammation of the affected nerves
TREATMENT/PROGNOSIS
I treated this patient with valacyclovir (1 g tid for a week), plus prednisone (20 mg, two every morning after meals for seven days, then one every morning after meals for seven days). These are given more in an effort to reduce post-herpetic neuralgia (PHN) than to treat the actual viral infection. An emerging consensus suggests the use of gabapentin in this period to prevent the worst effects of PHN. Our patient declined that option, but given her relative youth and limited skin involvement, her prognosis is excellent.
HISTORY
A 43-year-old woman presents with a six-day history of what began with tingling and itching in her left nipple area, but quickly progressed into a collection of tiny blisters that almost cover the central two-thirds of her breast. In the past few days, the itching has subsided, only to be replaced by lancinating pain.
She claims good health otherwise, but admits that lately she has felt a little achy and tired. On questioning, she recalls that about a week before the first signs of the eruption, she had an upper respiratory tract infection. Though she has had cold sores in her life, episodes have been widely spaced and minor, with extralabial involvement.
DIAGNOSIS
The collection of discrete and confluent vesicles is truly impressive and is underlain with an erythematous base. Swelling is minimal, and there is no tenderness. Several of the discrete vesicles are umbilicated, and most are full of what appear to be pus.
In all likelihood, this presentation represents herpes zoster rather than herpes simplex virus (HSV). In my opinion, it’s not worth trying to distinguish between the two, since they’re treated essentially the same in an immunocompetent patient.
LEARNING POINTS
The factor that most helped me arrive at the correct diagnosis was the pain, which was moderately severe and which is seldom seen with HSV. Also supportive of zoster were the widely scattered, sparse clusters of tiny vesicles on faintly erythematous bases, seen elsewhere on the trunk. I’m confident that these are lesions caused by zoster and not HSV.
The real “test” that will differentiate between zoster and HSV is this: If it’s HSV, chances are it will recur in the same area, probably repeatedly. Only a tiny percentage of zoster patients ever experience a recurrence.
As you might suspect, the pus seen in these lesions led the primary care providers the patient consulted first to prescribe oral antibiotics and topical mupirocin ointment. But far from pathognomic for bacterial infection, pus—a liquefied collection of dead white cells—is seen in many other conditions, such as fungal infections, psoriasis, yeast infection, and viral infection.
Other diagnostic features favoring zoster were:
• The premonitory symptoms of tingling and itch that preceded the appearance of the vesicles
• The umbilicated centers of many of the lesions
• The sensitivity in response to mild stroking, which was far more notable in the left breast than in the right; called dysesthesia, this sensation is typical of the many effects of the neurotropic herpes family
• The particular kind of pain (“lancinating”) the patient felt; this is thought to represent inflammation of the affected nerves
TREATMENT/PROGNOSIS
I treated this patient with valacyclovir (1 g tid for a week), plus prednisone (20 mg, two every morning after meals for seven days, then one every morning after meals for seven days). These are given more in an effort to reduce post-herpetic neuralgia (PHN) than to treat the actual viral infection. An emerging consensus suggests the use of gabapentin in this period to prevent the worst effects of PHN. Our patient declined that option, but given her relative youth and limited skin involvement, her prognosis is excellent.
HISTORY
A 43-year-old woman presents with a six-day history of what began with tingling and itching in her left nipple area, but quickly progressed into a collection of tiny blisters that almost cover the central two-thirds of her breast. In the past few days, the itching has subsided, only to be replaced by lancinating pain.
She claims good health otherwise, but admits that lately she has felt a little achy and tired. On questioning, she recalls that about a week before the first signs of the eruption, she had an upper respiratory tract infection. Though she has had cold sores in her life, episodes have been widely spaced and minor, with extralabial involvement.
DIAGNOSIS
The collection of discrete and confluent vesicles is truly impressive and is underlain with an erythematous base. Swelling is minimal, and there is no tenderness. Several of the discrete vesicles are umbilicated, and most are full of what appear to be pus.
In all likelihood, this presentation represents herpes zoster rather than herpes simplex virus (HSV). In my opinion, it’s not worth trying to distinguish between the two, since they’re treated essentially the same in an immunocompetent patient.
LEARNING POINTS
The factor that most helped me arrive at the correct diagnosis was the pain, which was moderately severe and which is seldom seen with HSV. Also supportive of zoster were the widely scattered, sparse clusters of tiny vesicles on faintly erythematous bases, seen elsewhere on the trunk. I’m confident that these are lesions caused by zoster and not HSV.
The real “test” that will differentiate between zoster and HSV is this: If it’s HSV, chances are it will recur in the same area, probably repeatedly. Only a tiny percentage of zoster patients ever experience a recurrence.
As you might suspect, the pus seen in these lesions led the primary care providers the patient consulted first to prescribe oral antibiotics and topical mupirocin ointment. But far from pathognomic for bacterial infection, pus—a liquefied collection of dead white cells—is seen in many other conditions, such as fungal infections, psoriasis, yeast infection, and viral infection.
Other diagnostic features favoring zoster were:
• The premonitory symptoms of tingling and itch that preceded the appearance of the vesicles
• The umbilicated centers of many of the lesions
• The sensitivity in response to mild stroking, which was far more notable in the left breast than in the right; called dysesthesia, this sensation is typical of the many effects of the neurotropic herpes family
• The particular kind of pain (“lancinating”) the patient felt; this is thought to represent inflammation of the affected nerves
TREATMENT/PROGNOSIS
I treated this patient with valacyclovir (1 g tid for a week), plus prednisone (20 mg, two every morning after meals for seven days, then one every morning after meals for seven days). These are given more in an effort to reduce post-herpetic neuralgia (PHN) than to treat the actual viral infection. An emerging consensus suggests the use of gabapentin in this period to prevent the worst effects of PHN. Our patient declined that option, but given her relative youth and limited skin involvement, her prognosis is excellent.