User login
This Rash Really Stinks!
ANSWER
The correct diagnosis is Darier disease (choice “d”).
DISCUSSION
Darier disease, also known as Darier-White disease or keratosis follicularis, is an inherited defect transmitted by autosomal dominant mode. The pathophysiologic process is a breakdown of cell adhesion that normally binds keratin filaments to tiny connecting fibers called desmosomes.
Darier disease manifests with a “branny” papulosquamous rash, typically arising in the third decade of life and affecting the chest, scalp, back, and intertriginous areas. The nail and intraoral findings noted in this patient are typical. In the author’s experience, the former is more commonly seen and is essentially pathognomic for the disease.
Darier disease is relatively rare, occurring in 1:30,000 to 1:100,000 population, depending on the geographic area studied. Men and women are equally affected, although it is more common in those with darker skin.
The differential outlined in the answer choices is reasonable, considering the condition’s rarity and how unlikely it is to manifest solely in the inframammary area. One could conclude that, just as with psoriasis (choice “b”) and seborrhea, intertrigo (choice “c”) is not always a primary process. And although yeast infection (choice “a”) can complicate any florid rash in this area, topical and oral anti-yeast treatment had utterly failed to help.
TREATMENT
Isotretinoin is used in cases such as this one, but it only offers temporary relief. For less severe cases, oral antibiotics (eg minocycline) or topical steroids (used with caution given the risk for atrophy in the inframammary area) often suffice. This patient’s prognosis is guarded at best, although control of the worst is certainly possible.
ANSWER
The correct diagnosis is Darier disease (choice “d”).
DISCUSSION
Darier disease, also known as Darier-White disease or keratosis follicularis, is an inherited defect transmitted by autosomal dominant mode. The pathophysiologic process is a breakdown of cell adhesion that normally binds keratin filaments to tiny connecting fibers called desmosomes.
Darier disease manifests with a “branny” papulosquamous rash, typically arising in the third decade of life and affecting the chest, scalp, back, and intertriginous areas. The nail and intraoral findings noted in this patient are typical. In the author’s experience, the former is more commonly seen and is essentially pathognomic for the disease.
Darier disease is relatively rare, occurring in 1:30,000 to 1:100,000 population, depending on the geographic area studied. Men and women are equally affected, although it is more common in those with darker skin.
The differential outlined in the answer choices is reasonable, considering the condition’s rarity and how unlikely it is to manifest solely in the inframammary area. One could conclude that, just as with psoriasis (choice “b”) and seborrhea, intertrigo (choice “c”) is not always a primary process. And although yeast infection (choice “a”) can complicate any florid rash in this area, topical and oral anti-yeast treatment had utterly failed to help.
TREATMENT
Isotretinoin is used in cases such as this one, but it only offers temporary relief. For less severe cases, oral antibiotics (eg minocycline) or topical steroids (used with caution given the risk for atrophy in the inframammary area) often suffice. This patient’s prognosis is guarded at best, although control of the worst is certainly possible.
ANSWER
The correct diagnosis is Darier disease (choice “d”).
DISCUSSION
Darier disease, also known as Darier-White disease or keratosis follicularis, is an inherited defect transmitted by autosomal dominant mode. The pathophysiologic process is a breakdown of cell adhesion that normally binds keratin filaments to tiny connecting fibers called desmosomes.
Darier disease manifests with a “branny” papulosquamous rash, typically arising in the third decade of life and affecting the chest, scalp, back, and intertriginous areas. The nail and intraoral findings noted in this patient are typical. In the author’s experience, the former is more commonly seen and is essentially pathognomic for the disease.
Darier disease is relatively rare, occurring in 1:30,000 to 1:100,000 population, depending on the geographic area studied. Men and women are equally affected, although it is more common in those with darker skin.
The differential outlined in the answer choices is reasonable, considering the condition’s rarity and how unlikely it is to manifest solely in the inframammary area. One could conclude that, just as with psoriasis (choice “b”) and seborrhea, intertrigo (choice “c”) is not always a primary process. And although yeast infection (choice “a”) can complicate any florid rash in this area, topical and oral anti-yeast treatment had utterly failed to help.
TREATMENT
Isotretinoin is used in cases such as this one, but it only offers temporary relief. For less severe cases, oral antibiotics (eg minocycline) or topical steroids (used with caution given the risk for atrophy in the inframammary area) often suffice. This patient’s prognosis is guarded at best, although control of the worst is certainly possible.

A 50-year-old woman is referred to dermatology with a “yeast” infection of several years’ duration. The condition causes considerable discomfort, especially during hot weather when the rash emits a very objectionable odor.
The florid, white, scaly rash under her breasts is a stark contrast to the patient’s type V skin. On both sides, the affected skin perfectly matches the inframammary fold. There are sharp margins and uniform moist scaling.
Looking elsewhere, 7 of 10 fingernails exhibit longitudinal white and red streaks, along with triangular nicks in the edges of several nails. The roof of the patient’s mouth is studded with fleshy nodules measuring 0.6 to 1.0 cm. Several pits are seen on her palms.
The patient is in no distress but is quite agitated by the lack of effective treatment. She reports trying a number of prescription and OTC anti-yeast creams, lotions, and oral medications, none of which resolved the problem.
History-taking reveals a family history of skin problems, although neither the patient nor anyone else in the family has ever been seen by a dermatologist. No one has ever suggested that a biopsy be done.
A punch biopsy is performed on the affected inframammary skin. The pathology report shows acantholysis with focal dyskeratotic keratinocytes. Intraepidermal separation is seen throughout the specimen.
I Spy, Near the Corner of My Eye
ANSWER
The correct answer—the false statement—is that SA has no pathologic implications (choice “a”).
DISCUSSION
SAs are usually benign and occur in 10% to 15% of the population (particularly in children). But they can sometimes be a sign of serious disease such as liver failure, with related esophageal varices, especially if > 3 lesions are present.
SAs are caused by a failure in the sphincter muscle surrounding a dilated cutaneous arteriole, which in turn is caused by increased estrogen levels in the blood. This increase can be related to the estrogen in birth control medications or to pregnancy.
A diseased liver, unable to metabolize estrogen properly, can contribute to increased blood levels of estrogen. For example, about one-third of patients with cirrhosis will develop multiple SAs.
SAs are seen only in the distribution of the superior vena cava. This means that—in addition to manifesting on the face—they can also appear on the arms, hands, trunk, and fingers.
Momentarily fading completely when central pressure is applied is a peculiar trait of SAs and is therefore diagnostic.
TREATMENT
While these lesions do, in fact, usually resolve on their own, treatment attempts are usually highly satisfactory. In my experience, destruction by laser ablation is superior to electrodessication, though recurrences are common. At the time of this presentation, the patient and her mother were still pondering the treatment options.
ANSWER
The correct answer—the false statement—is that SA has no pathologic implications (choice “a”).
DISCUSSION
SAs are usually benign and occur in 10% to 15% of the population (particularly in children). But they can sometimes be a sign of serious disease such as liver failure, with related esophageal varices, especially if > 3 lesions are present.
SAs are caused by a failure in the sphincter muscle surrounding a dilated cutaneous arteriole, which in turn is caused by increased estrogen levels in the blood. This increase can be related to the estrogen in birth control medications or to pregnancy.
A diseased liver, unable to metabolize estrogen properly, can contribute to increased blood levels of estrogen. For example, about one-third of patients with cirrhosis will develop multiple SAs.
SAs are seen only in the distribution of the superior vena cava. This means that—in addition to manifesting on the face—they can also appear on the arms, hands, trunk, and fingers.
Momentarily fading completely when central pressure is applied is a peculiar trait of SAs and is therefore diagnostic.
TREATMENT
While these lesions do, in fact, usually resolve on their own, treatment attempts are usually highly satisfactory. In my experience, destruction by laser ablation is superior to electrodessication, though recurrences are common. At the time of this presentation, the patient and her mother were still pondering the treatment options.
ANSWER
The correct answer—the false statement—is that SA has no pathologic implications (choice “a”).
DISCUSSION
SAs are usually benign and occur in 10% to 15% of the population (particularly in children). But they can sometimes be a sign of serious disease such as liver failure, with related esophageal varices, especially if > 3 lesions are present.
SAs are caused by a failure in the sphincter muscle surrounding a dilated cutaneous arteriole, which in turn is caused by increased estrogen levels in the blood. This increase can be related to the estrogen in birth control medications or to pregnancy.
A diseased liver, unable to metabolize estrogen properly, can contribute to increased blood levels of estrogen. For example, about one-third of patients with cirrhosis will develop multiple SAs.
SAs are seen only in the distribution of the superior vena cava. This means that—in addition to manifesting on the face—they can also appear on the arms, hands, trunk, and fingers.
Momentarily fading completely when central pressure is applied is a peculiar trait of SAs and is therefore diagnostic.
TREATMENT
While these lesions do, in fact, usually resolve on their own, treatment attempts are usually highly satisfactory. In my experience, destruction by laser ablation is superior to electrodessication, though recurrences are common. At the time of this presentation, the patient and her mother were still pondering the treatment options.
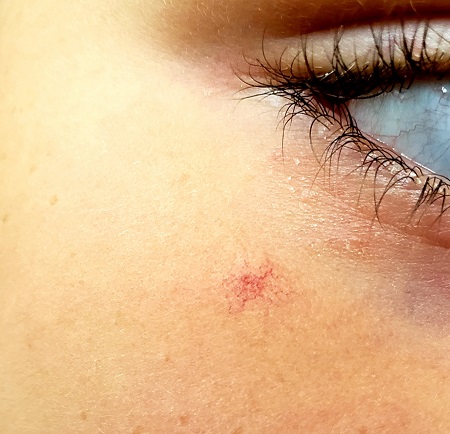
About 3 years ago, an asymptomatic lesion appeared on an 8-year-old girl’s right cheek. Because the spot made her feel self-conscious, the child’s mother had tried covering it up with makeup—but the makeup was even more obvious than the spot.
Their primary care provider (PCP) advised them to do nothing, noting that such lesions usually resolve on their own. The PCP did not believe the lesion was indicative of any related health problems. Dissatisfied with this instruction, the mother brings her daughter to dermatology for evaluation.
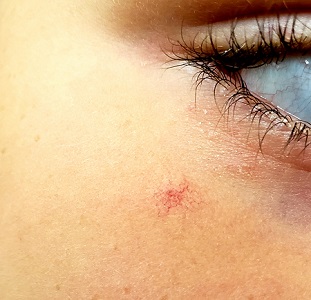
The girl is in otherwise good health. The lesion in question is a curious, bright red macule consisting of a tiny pinpoint red dot with very narrow “legs” (tiny, slender, red, vascular lines) emanating from the periphery. It is about 7 mm, and the center red dot is about 1 mm in diameter.
Using a dull pencil to create gentle pinpoint pressure causes the whole lesion to instantly and completely fade, only to return fully after pressure is released. The lesion is diagnosed as a typical spider angioma (SA; also known as spider nevi).
Sticking His Neck Out Leads to Diagnosis
ANSWER
The correct answer is all of the above (choice “d”).
DISCUSSION
For this patient, there could have been even more items in the differential, including melanoma, Merkel cell carcinoma, or even metastatic (from lung, colon, etc) origin. Dermatofibroma sarcoma protuberans is another possibility because it is rarely aggressive, though it is seldom as exophytic as this lesion. However, the prolonged, indolent course of the patient’s lesion was more consistent with the 3 choices listed. The overarching point is this: Why guess when the diagnosis is easily obtained by biopsy?
Biopsy of the lesion was ordered at the patient's first visit to dermatology. It revealed an invasive basal cell carcinoma (BCC), which almost never metastasizes. BCC requires extensive surgical removal and closure.
TREATMENT
The patient’s lesion needed a total excision with margins. Its size, location, and longevity called for the Mohs technique to assure clear margins and optimal closure.
Because of the findings and the patient’s history, he would also need to see dermatology every 6 months because he is a prime candidate for developing other skin cancers.
ANSWER
The correct answer is all of the above (choice “d”).
DISCUSSION
For this patient, there could have been even more items in the differential, including melanoma, Merkel cell carcinoma, or even metastatic (from lung, colon, etc) origin. Dermatofibroma sarcoma protuberans is another possibility because it is rarely aggressive, though it is seldom as exophytic as this lesion. However, the prolonged, indolent course of the patient’s lesion was more consistent with the 3 choices listed. The overarching point is this: Why guess when the diagnosis is easily obtained by biopsy?
Biopsy of the lesion was ordered at the patient's first visit to dermatology. It revealed an invasive basal cell carcinoma (BCC), which almost never metastasizes. BCC requires extensive surgical removal and closure.
TREATMENT
The patient’s lesion needed a total excision with margins. Its size, location, and longevity called for the Mohs technique to assure clear margins and optimal closure.
Because of the findings and the patient’s history, he would also need to see dermatology every 6 months because he is a prime candidate for developing other skin cancers.
ANSWER
The correct answer is all of the above (choice “d”).
DISCUSSION
For this patient, there could have been even more items in the differential, including melanoma, Merkel cell carcinoma, or even metastatic (from lung, colon, etc) origin. Dermatofibroma sarcoma protuberans is another possibility because it is rarely aggressive, though it is seldom as exophytic as this lesion. However, the prolonged, indolent course of the patient’s lesion was more consistent with the 3 choices listed. The overarching point is this: Why guess when the diagnosis is easily obtained by biopsy?
Biopsy of the lesion was ordered at the patient's first visit to dermatology. It revealed an invasive basal cell carcinoma (BCC), which almost never metastasizes. BCC requires extensive surgical removal and closure.
TREATMENT
The patient’s lesion needed a total excision with margins. Its size, location, and longevity called for the Mohs technique to assure clear margins and optimal closure.
Because of the findings and the patient’s history, he would also need to see dermatology every 6 months because he is a prime candidate for developing other skin cancers.
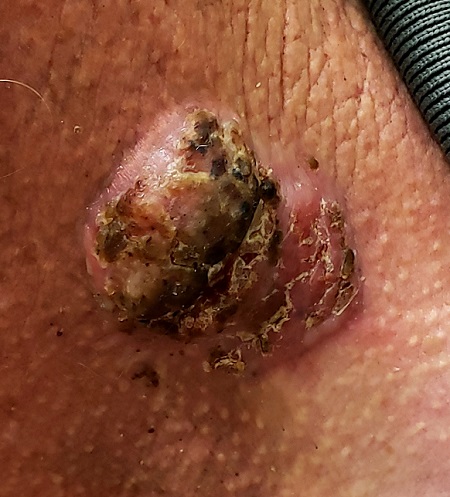
For 5 years, a lesion has been slowly growing on this 50-year-old man’s neck. He has seen several primary care providers who had provided different diagnoses, including wart, seborrheic keratosis, and keratoacanthoma. Throughout these visits, the only treatment he was offered was cryotherapy, but this was not effective at clearing the lesion. One family member convinced him it was time to try a dermatology provider.
In his lifetime, the patient has been exposed to a great deal of UV light. He has had several basal cell and squamous cell carcinomas removed from his face and arms.
He claims to be in otherwise good health, but further questioning reveals a > 40 pack-year history of smoking. He also has a recent diagnosis of early chronic obstructive pulmonary disease.
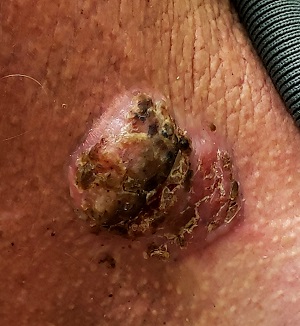
Physical examination of the lesion reveals a 4-x-3.5-cm sessile mass located on the left lateral neck. Its surface is rough and irregular, but there is no break in the skin.
On palpation, the lesion is quite firm and only partially mobile. No tenderness is detected. There are no palpable nodes in the region. There is evidence of advanced chronic sun damage on all sun-exposed areas, but especially on the head and neck. The rest of skin has no lesions.
Read This Rorschach Chest
ANSWER
The correct answer is Grover disease (choice “c”).
DISCUSSION
Grover disease—also known as transient acantholytic dermatosis—was first described in 1975 by Ralph Grover, MD, and is now recognized as a relatively common condition, especially in White men older than 40. Its appearance on darker skin is unusual. The morphologic presentation seen in this case is fairly typical, though most patients complain more about itching than this patient did.
The actual cause of Grover disease is unknown. Heat, sweat, and sunlight are suspected triggers. Its appearance can be associated with certain medications, recent treatment with ionizing radiation, or end-stage renal failure.
Biopsy is the key to diagnosis of Grover disease, especially in the context of the clinical presentation. This method also serves to rule out the other items in the differential.
Tinea corporis (choice “a”) was ruled out by the KOH as well as the rash’s appearance. Darier disease (choice “b”)—otherwise known as keratosis follicularis—is an inherited dermatosis that presents with multiple findings on skin, nails, and mucous membranes; however, the papulosquamous rash would be far more coarse than what manifests in Grover disease, and it would have manifested at a much earlier age. While folliculitis (choice “d”) was a possibility in this patient, the biopsy ruled it out.
TREATMENT
Grover disease is notoriously difficult to treat. Although it is described as a “transient” dermatosis, it can last months to years despite all therapeutic efforts.
This patient was treated with a stronger topical steroid (0.05% betamethasone cream) twice a day and minocycline (100 mg/d) for 2 months. These cleared his rash.
ANSWER
The correct answer is Grover disease (choice “c”).
DISCUSSION
Grover disease—also known as transient acantholytic dermatosis—was first described in 1975 by Ralph Grover, MD, and is now recognized as a relatively common condition, especially in White men older than 40. Its appearance on darker skin is unusual. The morphologic presentation seen in this case is fairly typical, though most patients complain more about itching than this patient did.
The actual cause of Grover disease is unknown. Heat, sweat, and sunlight are suspected triggers. Its appearance can be associated with certain medications, recent treatment with ionizing radiation, or end-stage renal failure.
Biopsy is the key to diagnosis of Grover disease, especially in the context of the clinical presentation. This method also serves to rule out the other items in the differential.
Tinea corporis (choice “a”) was ruled out by the KOH as well as the rash’s appearance. Darier disease (choice “b”)—otherwise known as keratosis follicularis—is an inherited dermatosis that presents with multiple findings on skin, nails, and mucous membranes; however, the papulosquamous rash would be far more coarse than what manifests in Grover disease, and it would have manifested at a much earlier age. While folliculitis (choice “d”) was a possibility in this patient, the biopsy ruled it out.
TREATMENT
Grover disease is notoriously difficult to treat. Although it is described as a “transient” dermatosis, it can last months to years despite all therapeutic efforts.
This patient was treated with a stronger topical steroid (0.05% betamethasone cream) twice a day and minocycline (100 mg/d) for 2 months. These cleared his rash.
ANSWER
The correct answer is Grover disease (choice “c”).
DISCUSSION
Grover disease—also known as transient acantholytic dermatosis—was first described in 1975 by Ralph Grover, MD, and is now recognized as a relatively common condition, especially in White men older than 40. Its appearance on darker skin is unusual. The morphologic presentation seen in this case is fairly typical, though most patients complain more about itching than this patient did.
The actual cause of Grover disease is unknown. Heat, sweat, and sunlight are suspected triggers. Its appearance can be associated with certain medications, recent treatment with ionizing radiation, or end-stage renal failure.
Biopsy is the key to diagnosis of Grover disease, especially in the context of the clinical presentation. This method also serves to rule out the other items in the differential.
Tinea corporis (choice “a”) was ruled out by the KOH as well as the rash’s appearance. Darier disease (choice “b”)—otherwise known as keratosis follicularis—is an inherited dermatosis that presents with multiple findings on skin, nails, and mucous membranes; however, the papulosquamous rash would be far more coarse than what manifests in Grover disease, and it would have manifested at a much earlier age. While folliculitis (choice “d”) was a possibility in this patient, the biopsy ruled it out.
TREATMENT
Grover disease is notoriously difficult to treat. Although it is described as a “transient” dermatosis, it can last months to years despite all therapeutic efforts.
This patient was treated with a stronger topical steroid (0.05% betamethasone cream) twice a day and minocycline (100 mg/d) for 2 months. These cleared his rash.
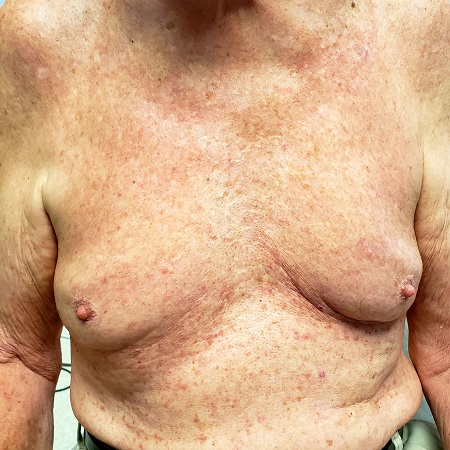
Several months ago, an asymptomatic rash manifested on the 63-year-old man’s chest. His primary care provider diagnosed this as eczema, though the patient has no history of atopic conditions. Initial treatment included 0.025% triamcinolone cream, which was later switched to 0.1%. This improved the appearance but failed to clear the condition, prompting a referral to dermatology.
The patient is in otherwise good health. He has no history of seasonal allergies, asthma, urticaria, or eczema. He takes no medications that could have caused the rash. There is no family history of atopy or any other skin disease.
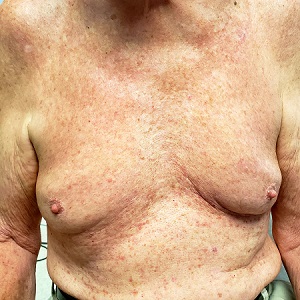
The florid, papulovesicular rash covers his chest, from the upper sternum to the mid-abdomen. Palpation reveals a rough texture to the condition that is faintly erythematous. The rash also affects small areas of his triceps, but the rest of his skin—including back, legs, and buttocks—are clear. His hair and nails appear normal.
A KOH prep shows fungal elements, but the lab results are negative. Longitudinal shave biopsy shows subcorneal separation along with acantholysis (destruction of connections between keratinocytes).
Keeping the Differential at Hand
ANSWER
The correct answer is granuloma annulare (GA; choice “a”).
DISCUSSION
One of the most difficult concepts to grasp in dermatologic diagnosis is that almost all lesions and conditions—even the most common—have a broad range of morphologic presentations. These will often differ from the textbook photos. In this digital age, a simple Internet search will provide many results showing a diverse morphologic spectrum for many diseases, conditions, and lesions.
GA is a good example of how the presentation can vary. It has raised rolled margins and delled (gently concave) centers. The brownish red color is typical, but this patient showed a deeper red than most cases of GA. Occasionally, the red color is even deeper, with large patches of darkened skin and no palpable component.
Unfortunately, the misdiagnosis of fungal infection in this patient is typical. But dermatophytosis (otherwise known as “ringworm”)—the most common fungal skin infection—involves the epidermis. This means the patient would have scaly skin, probably with a well-defined margin—factors missing in this case. In addition, this patient reported no contact with sources of infection: animals, children, or immunosuppressive agents.
Ultimately, the most basic information that this patient's past providers neglected was a differential diagnosis. By establishing a differential, there was a clear decision to biopsy, which not only revealed the correct diagnosis but effectively ruled out the other options.
In defense of the patient’s other providers, I must admit that as a young primary care provider, I made this same mistake for exactly the same reasons.
TREATMENT
Most cases of GA are mild and self-limited, requiring no treatment. This is fortunate because no effective treatment exists. Topical steroids and cryotherapy will lighten the lesion, but GA nearly always resolves on its own.
ANSWER
The correct answer is granuloma annulare (GA; choice “a”).
DISCUSSION
One of the most difficult concepts to grasp in dermatologic diagnosis is that almost all lesions and conditions—even the most common—have a broad range of morphologic presentations. These will often differ from the textbook photos. In this digital age, a simple Internet search will provide many results showing a diverse morphologic spectrum for many diseases, conditions, and lesions.
GA is a good example of how the presentation can vary. It has raised rolled margins and delled (gently concave) centers. The brownish red color is typical, but this patient showed a deeper red than most cases of GA. Occasionally, the red color is even deeper, with large patches of darkened skin and no palpable component.
Unfortunately, the misdiagnosis of fungal infection in this patient is typical. But dermatophytosis (otherwise known as “ringworm”)—the most common fungal skin infection—involves the epidermis. This means the patient would have scaly skin, probably with a well-defined margin—factors missing in this case. In addition, this patient reported no contact with sources of infection: animals, children, or immunosuppressive agents.
Ultimately, the most basic information that this patient's past providers neglected was a differential diagnosis. By establishing a differential, there was a clear decision to biopsy, which not only revealed the correct diagnosis but effectively ruled out the other options.
In defense of the patient’s other providers, I must admit that as a young primary care provider, I made this same mistake for exactly the same reasons.
TREATMENT
Most cases of GA are mild and self-limited, requiring no treatment. This is fortunate because no effective treatment exists. Topical steroids and cryotherapy will lighten the lesion, but GA nearly always resolves on its own.
ANSWER
The correct answer is granuloma annulare (GA; choice “a”).
DISCUSSION
One of the most difficult concepts to grasp in dermatologic diagnosis is that almost all lesions and conditions—even the most common—have a broad range of morphologic presentations. These will often differ from the textbook photos. In this digital age, a simple Internet search will provide many results showing a diverse morphologic spectrum for many diseases, conditions, and lesions.
GA is a good example of how the presentation can vary. It has raised rolled margins and delled (gently concave) centers. The brownish red color is typical, but this patient showed a deeper red than most cases of GA. Occasionally, the red color is even deeper, with large patches of darkened skin and no palpable component.
Unfortunately, the misdiagnosis of fungal infection in this patient is typical. But dermatophytosis (otherwise known as “ringworm”)—the most common fungal skin infection—involves the epidermis. This means the patient would have scaly skin, probably with a well-defined margin—factors missing in this case. In addition, this patient reported no contact with sources of infection: animals, children, or immunosuppressive agents.
Ultimately, the most basic information that this patient's past providers neglected was a differential diagnosis. By establishing a differential, there was a clear decision to biopsy, which not only revealed the correct diagnosis but effectively ruled out the other options.
In defense of the patient’s other providers, I must admit that as a young primary care provider, I made this same mistake for exactly the same reasons.
TREATMENT
Most cases of GA are mild and self-limited, requiring no treatment. This is fortunate because no effective treatment exists. Topical steroids and cryotherapy will lighten the lesion, but GA nearly always resolves on its own.
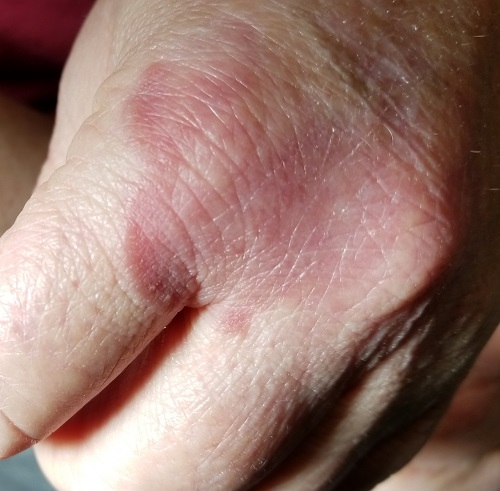
Several months ago, an asymptomatic rash slowly manifested on a 60-year-old woman’s hand. The rash—diagnosed previously as a fungal infection—continues to grow despite application of multiple antifungal creams, including tolnaftate, clotrimazole, and terbinafine. In addition, she was treated with a 1-month course of oral terbinafine 250 mg/d. Unfortunately, no treatment has provided her relief.
The patient is in otherwise good health. She denies any injury to the area. She also reports no exposure to children or animals.
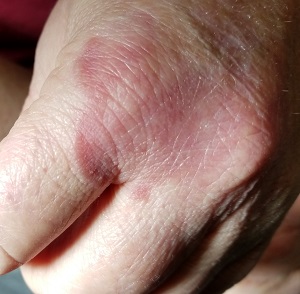
The rash is a reddish brown, annular patch of skin that covers most of the dorsum of her left hand. The borders are slightly raised and thickened. It is nontender and readily blanchable. It is intradermal, with no surface disturbance such as scaling.
Punch biopsy shows palisaded granulomatous features, with no epidermal changes. Stains for fungi and bacteria fail to demonstrate any organisms.
Was This Tattoo a Rash Choice?
ANSWER
The correct answer is koebnerization of pre-existing psoriasis (choice “c”).
DISCUSSION
Tattoos have been known to cause bacterial infection (choice “a”), but this was unlikely given the diffuse nature of the rash and the lack of pain or adenopathy. Allergic reactions to tattoo dyes (choice “b”) are certainly common, but usually red or yellow dyes—which were not used for this tattoo—provoke the worst reactions. Furthermore, itching would have been a more prominent feature of the patient's complaint. Had it been fungal infection (choice “d”), the steroid cream would have made it worse.
One possibility remained: the so-called isomorphic phenomenon (otherwise known as koebnerization). First described by Heinrich Koebner in the mid-19th century, koebnerization is characterized by the appearance of psoriasis in traumatized skin such as surgical wounds, abrasions, burns, or even tattoos. Several other conditions also exhibit this same linear response to trauma, including warts, molluscum, and lichen planus.
To test for this diagnosis, corroborative findings of psoriasis were sought and found in the patient’s nails. His history of rashes on the knees and elbows also contributed to establishing the diagnosis. Moreover, his complaint of arthritis was quite suggestive of psoriatic arthropathy, which afflicts about 25% of patients with psoriasis and has little to do with the severity of the skin disease itself. Once the diagnosis became more apparent, the patient recalled a family history of psoriasis. Had any question remained, a biopsy could remove doubt.
TREATMENT
For the patient, twice-daily application of a stronger steroid cream (augmented betamethasone) was prescribed. Though this quickly cleared the koebnerizing psoriasis, it is likely we haven’t seen the last of this disease.
ANSWER
The correct answer is koebnerization of pre-existing psoriasis (choice “c”).
DISCUSSION
Tattoos have been known to cause bacterial infection (choice “a”), but this was unlikely given the diffuse nature of the rash and the lack of pain or adenopathy. Allergic reactions to tattoo dyes (choice “b”) are certainly common, but usually red or yellow dyes—which were not used for this tattoo—provoke the worst reactions. Furthermore, itching would have been a more prominent feature of the patient's complaint. Had it been fungal infection (choice “d”), the steroid cream would have made it worse.
One possibility remained: the so-called isomorphic phenomenon (otherwise known as koebnerization). First described by Heinrich Koebner in the mid-19th century, koebnerization is characterized by the appearance of psoriasis in traumatized skin such as surgical wounds, abrasions, burns, or even tattoos. Several other conditions also exhibit this same linear response to trauma, including warts, molluscum, and lichen planus.
To test for this diagnosis, corroborative findings of psoriasis were sought and found in the patient’s nails. His history of rashes on the knees and elbows also contributed to establishing the diagnosis. Moreover, his complaint of arthritis was quite suggestive of psoriatic arthropathy, which afflicts about 25% of patients with psoriasis and has little to do with the severity of the skin disease itself. Once the diagnosis became more apparent, the patient recalled a family history of psoriasis. Had any question remained, a biopsy could remove doubt.
TREATMENT
For the patient, twice-daily application of a stronger steroid cream (augmented betamethasone) was prescribed. Though this quickly cleared the koebnerizing psoriasis, it is likely we haven’t seen the last of this disease.
ANSWER
The correct answer is koebnerization of pre-existing psoriasis (choice “c”).
DISCUSSION
Tattoos have been known to cause bacterial infection (choice “a”), but this was unlikely given the diffuse nature of the rash and the lack of pain or adenopathy. Allergic reactions to tattoo dyes (choice “b”) are certainly common, but usually red or yellow dyes—which were not used for this tattoo—provoke the worst reactions. Furthermore, itching would have been a more prominent feature of the patient's complaint. Had it been fungal infection (choice “d”), the steroid cream would have made it worse.
One possibility remained: the so-called isomorphic phenomenon (otherwise known as koebnerization). First described by Heinrich Koebner in the mid-19th century, koebnerization is characterized by the appearance of psoriasis in traumatized skin such as surgical wounds, abrasions, burns, or even tattoos. Several other conditions also exhibit this same linear response to trauma, including warts, molluscum, and lichen planus.
To test for this diagnosis, corroborative findings of psoriasis were sought and found in the patient’s nails. His history of rashes on the knees and elbows also contributed to establishing the diagnosis. Moreover, his complaint of arthritis was quite suggestive of psoriatic arthropathy, which afflicts about 25% of patients with psoriasis and has little to do with the severity of the skin disease itself. Once the diagnosis became more apparent, the patient recalled a family history of psoriasis. Had any question remained, a biopsy could remove doubt.
TREATMENT
For the patient, twice-daily application of a stronger steroid cream (augmented betamethasone) was prescribed. Though this quickly cleared the koebnerizing psoriasis, it is likely we haven’t seen the last of this disease.

Weeks ago, a 43-year-old man received a birthday tattoo of his choice: a geometric pattern etched in blue ink on his wrist. Unfortunately, a rash began to develop within the lines of the tattoo. The rash itches, but its appearance is of greater concern to the patient. He’s gotten some relief from topical creams, although the rash quickly returns with cessation of treatment.
Past medical history is notable for arthritis affecting his left elbow and right heel. He also has intermittent rashes that manifest on his elbows and knees, but these are partially relieved by a steroid cream (triamcinolone 0.1%).
His tattoo is located on the extensor right wrist. The affected areas show a brisk, red, inflammatory response, which—in several locations—is also scaly. There is no tenderness or induration on palpation of the rash and no palpable adenopathy in local nodal locations (epitrochlear and axillary). Elsewhere, 5 of his 10 fingernails demonstrate pitting; 2 show onycholysis and oil spotting. His scalp, knees, and elbows are free of any notable changes.
What a Slow Boil Got Him
ANSWER
The correct answer is hidradenitis suppurativa (HS; choice “c”).
DISCUSSION
HS (also known as acne inversa) is a relatively common condition first described in 1839 by French physician Frederick Velpeau, who thought it was probably a form of acne. Because HS only affects intertriginous areas (groin, axillae, inframammary, intergluteal, and abdominal folds rich in apocrine glands), during the next 130 years, it was presumed that this disease was solely caused by malfunctioning apocrine glands.
Though experts disagree about the true etiology of HS, most agree that it is caused by several environmental and genetic factors leading to plugged or malfunctioning hair follicles and apocrine glands that become inflamed, swollen, painful, and purulent. In severe cases, tracts develop between lesions, resulting in the formation of ropy, linear hypertrophic scarring. Early on and in milder cases, comedones can manifest—often in multiples—along with widely scattered cysts. It appears that a case can be made for a genetic predisposition to develop HS because at least one-third of affected patients report a positive family history.
Females (usually postpubescent) are affected at 3 times the rate of males. Hormones, especially androgens, appear to play a role. This assertion is bolstered not only by the age of onset, but also because HS has been observed to improve after pregnancy and after menopause.
Though not causative, smoking and obesity have a strong statistical correlation with HS as exacerbating factors. Many patients with HS find movement from exercise too painful, which may contribute to obesity.
Because HS has a wide range of clinical presentations, the Hurley Staging scale can help clinicians distinguish the condition’s severity by stages I, II, or III. Stage I manifests with scant signs of disease, including comedones and sparsely separated small cysts. Stage II includes numerous painful cysts with tract formation between lesions. Stage III involves symptoms described in the other stages as well as multiple large, painful, draining cysts; widespread erythema; and extensive hypertrophic scarring.
Regarding the differential, the culture would have identified community-acquired methicillin-resistant Staphylococcus aureus (choice “a”) or flesh-eating bacterial infection (choice “d”), but neither would be as chronic as the patient’s disease. Acne conglobata (choice “b”) manifests with chronic dense acne largely confined to the trunk. Interestingly, acne conglobata, HS, dissecting cellulitis of the scalp, and pilonidal cyst are collectively known as the follicular occlusion tetrad.
TREATMENT
Treatment for HS is limited. Adalimumab is the most recent and promising biologic, though its use comes at a high cost ($60,000/y) and with an adverse effect profile that should give any prescriber pause. Also, the best one could hope for in using adalimumab is about a 30% improvement in the patient.
Before using a biologic, other options should at least be considered. Though not entirely satisfactory, there are oral antibiotics (minocycline, trimethoprim/sulfa, or a combination of rifampin and clindamycin) or intralesional steroids. Incision and drainage of individual lesions and isotretinoin therapy can temporarily relieve pain, but they are not effective as long-term therapies. Large-scale surgical extirpation of the affected tissue can be considered in extreme cases, but there can be recurrences and associated morbidity (eg, chronic lymphedema in the affected arm, extreme scarring, and postoperative pain).
ANSWER
The correct answer is hidradenitis suppurativa (HS; choice “c”).
DISCUSSION
HS (also known as acne inversa) is a relatively common condition first described in 1839 by French physician Frederick Velpeau, who thought it was probably a form of acne. Because HS only affects intertriginous areas (groin, axillae, inframammary, intergluteal, and abdominal folds rich in apocrine glands), during the next 130 years, it was presumed that this disease was solely caused by malfunctioning apocrine glands.
Though experts disagree about the true etiology of HS, most agree that it is caused by several environmental and genetic factors leading to plugged or malfunctioning hair follicles and apocrine glands that become inflamed, swollen, painful, and purulent. In severe cases, tracts develop between lesions, resulting in the formation of ropy, linear hypertrophic scarring. Early on and in milder cases, comedones can manifest—often in multiples—along with widely scattered cysts. It appears that a case can be made for a genetic predisposition to develop HS because at least one-third of affected patients report a positive family history.
Females (usually postpubescent) are affected at 3 times the rate of males. Hormones, especially androgens, appear to play a role. This assertion is bolstered not only by the age of onset, but also because HS has been observed to improve after pregnancy and after menopause.
Though not causative, smoking and obesity have a strong statistical correlation with HS as exacerbating factors. Many patients with HS find movement from exercise too painful, which may contribute to obesity.
Because HS has a wide range of clinical presentations, the Hurley Staging scale can help clinicians distinguish the condition’s severity by stages I, II, or III. Stage I manifests with scant signs of disease, including comedones and sparsely separated small cysts. Stage II includes numerous painful cysts with tract formation between lesions. Stage III involves symptoms described in the other stages as well as multiple large, painful, draining cysts; widespread erythema; and extensive hypertrophic scarring.
Regarding the differential, the culture would have identified community-acquired methicillin-resistant Staphylococcus aureus (choice “a”) or flesh-eating bacterial infection (choice “d”), but neither would be as chronic as the patient’s disease. Acne conglobata (choice “b”) manifests with chronic dense acne largely confined to the trunk. Interestingly, acne conglobata, HS, dissecting cellulitis of the scalp, and pilonidal cyst are collectively known as the follicular occlusion tetrad.
TREATMENT
Treatment for HS is limited. Adalimumab is the most recent and promising biologic, though its use comes at a high cost ($60,000/y) and with an adverse effect profile that should give any prescriber pause. Also, the best one could hope for in using adalimumab is about a 30% improvement in the patient.
Before using a biologic, other options should at least be considered. Though not entirely satisfactory, there are oral antibiotics (minocycline, trimethoprim/sulfa, or a combination of rifampin and clindamycin) or intralesional steroids. Incision and drainage of individual lesions and isotretinoin therapy can temporarily relieve pain, but they are not effective as long-term therapies. Large-scale surgical extirpation of the affected tissue can be considered in extreme cases, but there can be recurrences and associated morbidity (eg, chronic lymphedema in the affected arm, extreme scarring, and postoperative pain).
ANSWER
The correct answer is hidradenitis suppurativa (HS; choice “c”).
DISCUSSION
HS (also known as acne inversa) is a relatively common condition first described in 1839 by French physician Frederick Velpeau, who thought it was probably a form of acne. Because HS only affects intertriginous areas (groin, axillae, inframammary, intergluteal, and abdominal folds rich in apocrine glands), during the next 130 years, it was presumed that this disease was solely caused by malfunctioning apocrine glands.
Though experts disagree about the true etiology of HS, most agree that it is caused by several environmental and genetic factors leading to plugged or malfunctioning hair follicles and apocrine glands that become inflamed, swollen, painful, and purulent. In severe cases, tracts develop between lesions, resulting in the formation of ropy, linear hypertrophic scarring. Early on and in milder cases, comedones can manifest—often in multiples—along with widely scattered cysts. It appears that a case can be made for a genetic predisposition to develop HS because at least one-third of affected patients report a positive family history.
Females (usually postpubescent) are affected at 3 times the rate of males. Hormones, especially androgens, appear to play a role. This assertion is bolstered not only by the age of onset, but also because HS has been observed to improve after pregnancy and after menopause.
Though not causative, smoking and obesity have a strong statistical correlation with HS as exacerbating factors. Many patients with HS find movement from exercise too painful, which may contribute to obesity.
Because HS has a wide range of clinical presentations, the Hurley Staging scale can help clinicians distinguish the condition’s severity by stages I, II, or III. Stage I manifests with scant signs of disease, including comedones and sparsely separated small cysts. Stage II includes numerous painful cysts with tract formation between lesions. Stage III involves symptoms described in the other stages as well as multiple large, painful, draining cysts; widespread erythema; and extensive hypertrophic scarring.
Regarding the differential, the culture would have identified community-acquired methicillin-resistant Staphylococcus aureus (choice “a”) or flesh-eating bacterial infection (choice “d”), but neither would be as chronic as the patient’s disease. Acne conglobata (choice “b”) manifests with chronic dense acne largely confined to the trunk. Interestingly, acne conglobata, HS, dissecting cellulitis of the scalp, and pilonidal cyst are collectively known as the follicular occlusion tetrad.
TREATMENT
Treatment for HS is limited. Adalimumab is the most recent and promising biologic, though its use comes at a high cost ($60,000/y) and with an adverse effect profile that should give any prescriber pause. Also, the best one could hope for in using adalimumab is about a 30% improvement in the patient.
Before using a biologic, other options should at least be considered. Though not entirely satisfactory, there are oral antibiotics (minocycline, trimethoprim/sulfa, or a combination of rifampin and clindamycin) or intralesional steroids. Incision and drainage of individual lesions and isotretinoin therapy can temporarily relieve pain, but they are not effective as long-term therapies. Large-scale surgical extirpation of the affected tissue can be considered in extreme cases, but there can be recurrences and associated morbidity (eg, chronic lymphedema in the affected arm, extreme scarring, and postoperative pain).
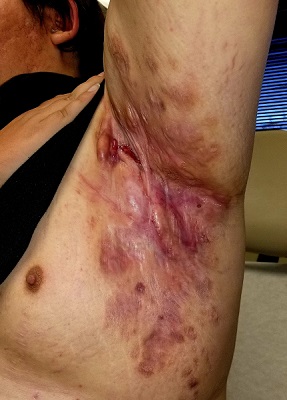
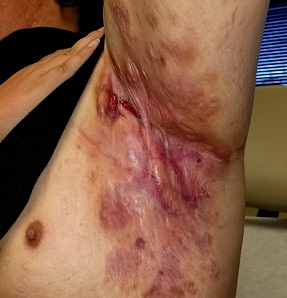
Boils first manifested on this 25-year-old man’s axillae when he was 13 (at the onset of puberty). As he grew older, they appeared in other intertriginous areas, including the groin and between the buttocks. As he became increasingly overweight, the folds under his breasts and abdomen became affected.
Over the years, several primary care providers consistently diagnosed him with either boils or staph infection. They also would reliably admonish him regarding his weight and lack of cleanliness. Treatment included various oral antibiotics that would only calm the condition for a short time. At no point was he referred to dermatology. Family history revealed similar skin problems in his mother and 1 sister.
Recently, his lesions have grown more numerous and painful. They drain pustular fluid, which makes it difficult for him to function in classrooms or at work. Even walking is excruciatingly painful. As a result, he is more sedentary. He also has started smoking.
On examination, the patient is 5 ft 8 in and grossly obese (weight, 300 lb). His affect is decidedly morose. His gait is ponderous and halting. His type 4 skin is swarthy, sweaty, and oily.
All intertriginous areas are similarly affected with large, ropy keloidal and hypertrophic scars, as well as diffuse bright red erythema and edema. There are dozens of single and multiple comedones, along with multiple draining sinuses.
A bacterial culture is collected from the fluid draining from the lesions. The results show a mixed, normal, cutaneous flora—including staph epidermidis—with no predominant organism.
A Roundabout Journey to Diagnosis
ANSWER
The correct answer is all the above (choice “e”).
DISCUSSION
The differential for round or annular, scaly lesions is lengthy. In addition to all 4 conditions listed above, it includes eczema, basal cell carcinoma, and irritant or contact dermatitis.
With this patient’s history, the diagnosis of fungal infection was not unreasonable. However, the total lack of response to antifungal treatment—along with a negative KOH prep—made that diagnosis questionable at best. Then there was the lack of lymphadenopathy, which would almost certainly have been present with such longstanding infection. Given her country of origin, cutaneous New World leishmaniasis (caused by a protozoan delivered to the patient by an insect vector) was a possibility.
For this patient, skin biopsy with a 4-mm punch was the only way to establish the correct diagnosis. The defect from the biopsy was closed with 5-0 nylon sutures to minimize scarring.
The pathological findings included interface dermatitis, apoptotic keratinocytes, and a brisk periadnexal lymphocytic infiltrate, which—given the morphological and historical context—were entirely consistent with discoid lupus erythematosus (DLE; otherwise known as subacute cutaneous lupus erythematosus). Subsequent bloodwork failed to show any connection with systemic lupus erythematosus (SLE), which is not surprising because only about 18% of DLE cases evolve into SLE.
DLE is more common in women, especially in those with skin of color. The associated lesions are seldom as impressive as this patient’s, manifesting as papulosquamous patches typically found on the ears, neck, face, arms, and other sun-exposed areas. Indeed, it appears that sun exposure is a major trigger for the disease—a clue that can assist with the diagnosis.
TREATMENT
In addition to proscribing excessive sun exposure, providers should encourage the use of sunscreen. DLE is often treated with topical steroids. More advanced cases, such as this patient’s, may require oral hydroxychloroquine (200 mg bid). Though these treatments are effective in most cases, DLE can leave serious scarring and/or discoloration, especially in those with darker skin.
ANSWER
The correct answer is all the above (choice “e”).
DISCUSSION
The differential for round or annular, scaly lesions is lengthy. In addition to all 4 conditions listed above, it includes eczema, basal cell carcinoma, and irritant or contact dermatitis.
With this patient’s history, the diagnosis of fungal infection was not unreasonable. However, the total lack of response to antifungal treatment—along with a negative KOH prep—made that diagnosis questionable at best. Then there was the lack of lymphadenopathy, which would almost certainly have been present with such longstanding infection. Given her country of origin, cutaneous New World leishmaniasis (caused by a protozoan delivered to the patient by an insect vector) was a possibility.
For this patient, skin biopsy with a 4-mm punch was the only way to establish the correct diagnosis. The defect from the biopsy was closed with 5-0 nylon sutures to minimize scarring.
The pathological findings included interface dermatitis, apoptotic keratinocytes, and a brisk periadnexal lymphocytic infiltrate, which—given the morphological and historical context—were entirely consistent with discoid lupus erythematosus (DLE; otherwise known as subacute cutaneous lupus erythematosus). Subsequent bloodwork failed to show any connection with systemic lupus erythematosus (SLE), which is not surprising because only about 18% of DLE cases evolve into SLE.
DLE is more common in women, especially in those with skin of color. The associated lesions are seldom as impressive as this patient’s, manifesting as papulosquamous patches typically found on the ears, neck, face, arms, and other sun-exposed areas. Indeed, it appears that sun exposure is a major trigger for the disease—a clue that can assist with the diagnosis.
TREATMENT
In addition to proscribing excessive sun exposure, providers should encourage the use of sunscreen. DLE is often treated with topical steroids. More advanced cases, such as this patient’s, may require oral hydroxychloroquine (200 mg bid). Though these treatments are effective in most cases, DLE can leave serious scarring and/or discoloration, especially in those with darker skin.
ANSWER
The correct answer is all the above (choice “e”).
DISCUSSION
The differential for round or annular, scaly lesions is lengthy. In addition to all 4 conditions listed above, it includes eczema, basal cell carcinoma, and irritant or contact dermatitis.
With this patient’s history, the diagnosis of fungal infection was not unreasonable. However, the total lack of response to antifungal treatment—along with a negative KOH prep—made that diagnosis questionable at best. Then there was the lack of lymphadenopathy, which would almost certainly have been present with such longstanding infection. Given her country of origin, cutaneous New World leishmaniasis (caused by a protozoan delivered to the patient by an insect vector) was a possibility.
For this patient, skin biopsy with a 4-mm punch was the only way to establish the correct diagnosis. The defect from the biopsy was closed with 5-0 nylon sutures to minimize scarring.
The pathological findings included interface dermatitis, apoptotic keratinocytes, and a brisk periadnexal lymphocytic infiltrate, which—given the morphological and historical context—were entirely consistent with discoid lupus erythematosus (DLE; otherwise known as subacute cutaneous lupus erythematosus). Subsequent bloodwork failed to show any connection with systemic lupus erythematosus (SLE), which is not surprising because only about 18% of DLE cases evolve into SLE.
DLE is more common in women, especially in those with skin of color. The associated lesions are seldom as impressive as this patient’s, manifesting as papulosquamous patches typically found on the ears, neck, face, arms, and other sun-exposed areas. Indeed, it appears that sun exposure is a major trigger for the disease—a clue that can assist with the diagnosis.
TREATMENT
In addition to proscribing excessive sun exposure, providers should encourage the use of sunscreen. DLE is often treated with topical steroids. More advanced cases, such as this patient’s, may require oral hydroxychloroquine (200 mg bid). Though these treatments are effective in most cases, DLE can leave serious scarring and/or discoloration, especially in those with darker skin.
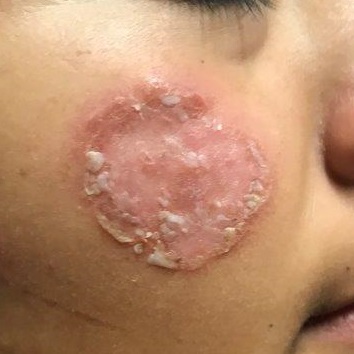
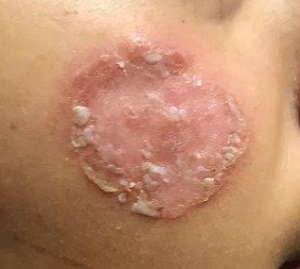
After journeying for several months from Honduras, this 30-year-old woman visits the clinic for evaluation of a lesion that has been growing on her cheek since before she started traveling. She saw several providers—mostly in NGO clinics—along her journey. The diagnosis they gave was consistently “ringworm.” She was offered various topical creams, none of which produced any results.
Though the lesion is not painful, it causes some itching. The patient is much more concerned about its appearance. Through interpreters, she claims to be in otherwise good health. She has no other lesions, joint pain, fever, or malaise. She reports neither her family nor fellow travelers have such lesions.
Examination reveals an impressive 3-cm, round, papulosquamous plaque on the right side of her face (below the malar area). The lesion is neither tender nor notably warm. There are no palpable lymph nodes in the area. The scaling is mostly on the periphery. A KOH prep of the scaling shows no fungal elements.
He Doesn’t Love It Warts and All
ANSWER
The correct answer is lichen planus (choice “c”).
DISCUSSION
Condyloma accuminata can demonstrate amazing lability, sometimes appearing decades after exposure. And spouses may not always be truthful when questioned about such exposure. To further confuse the issue, it's entirely possible that a patient may be unaware he or she has condyloma. So, this might well have been condyloma. But the differential for penile lesions would include this condition—and more.
Psoriasis (choice “a”) commonly affects the penis, manifesting as pinkish plaques and papules. But there is a good chance that examination would have revealed corroborative signs of this disease. Furthermore, the histologic results would have been entirely different.
While syphilis (choice “b”), especially in its primary stage, can present with nonhealing sores, in no way do they resemble the patient’s lesions. There is also no source for such an infection. And biopsy would have shown a predominately plasma cell infiltrate in an entirely different pattern.
Lichen sclerosus et atrophicus (choice “d”) is quite uncommon, especially on the penis, where it is usually known as balanitis xerotica obliterans (BXO). As its name suggests, BXO is usually atrophic—therefore macular—and whitish. Exclusive to uncircumcised men, it bears no resemblance to condyloma.
Though idiopathic, lichen planus is not contagious. Unless neglected, this condition seldom causes any suffering aside from mental anguish over its appearance. To make a more accurate diagnosis, it is always helpful for providers to consider a mnemonic device for “7 Ps” associated with lichen planus:
- Penile
- Pruritic
- Plaque-like
- Purple
- Papular
- Planar
- Puzzling.
TREATMENT
Fortunately, lichen planus affecting the penis responds readily to treatment with mid-strength topical steroid cream and the "tincture of time," which improves its appearance until it eventually disappears. For this patient, the PCP treated the affected area with triamcinolone 0.1% cream bid for 2 weeks. This was then applied once a day every other day for a month, which cleared the patient’s lesions.
ANSWER
The correct answer is lichen planus (choice “c”).
DISCUSSION
Condyloma accuminata can demonstrate amazing lability, sometimes appearing decades after exposure. And spouses may not always be truthful when questioned about such exposure. To further confuse the issue, it's entirely possible that a patient may be unaware he or she has condyloma. So, this might well have been condyloma. But the differential for penile lesions would include this condition—and more.
Psoriasis (choice “a”) commonly affects the penis, manifesting as pinkish plaques and papules. But there is a good chance that examination would have revealed corroborative signs of this disease. Furthermore, the histologic results would have been entirely different.
While syphilis (choice “b”), especially in its primary stage, can present with nonhealing sores, in no way do they resemble the patient’s lesions. There is also no source for such an infection. And biopsy would have shown a predominately plasma cell infiltrate in an entirely different pattern.
Lichen sclerosus et atrophicus (choice “d”) is quite uncommon, especially on the penis, where it is usually known as balanitis xerotica obliterans (BXO). As its name suggests, BXO is usually atrophic—therefore macular—and whitish. Exclusive to uncircumcised men, it bears no resemblance to condyloma.
Though idiopathic, lichen planus is not contagious. Unless neglected, this condition seldom causes any suffering aside from mental anguish over its appearance. To make a more accurate diagnosis, it is always helpful for providers to consider a mnemonic device for “7 Ps” associated with lichen planus:
- Penile
- Pruritic
- Plaque-like
- Purple
- Papular
- Planar
- Puzzling.
TREATMENT
Fortunately, lichen planus affecting the penis responds readily to treatment with mid-strength topical steroid cream and the "tincture of time," which improves its appearance until it eventually disappears. For this patient, the PCP treated the affected area with triamcinolone 0.1% cream bid for 2 weeks. This was then applied once a day every other day for a month, which cleared the patient’s lesions.
ANSWER
The correct answer is lichen planus (choice “c”).
DISCUSSION
Condyloma accuminata can demonstrate amazing lability, sometimes appearing decades after exposure. And spouses may not always be truthful when questioned about such exposure. To further confuse the issue, it's entirely possible that a patient may be unaware he or she has condyloma. So, this might well have been condyloma. But the differential for penile lesions would include this condition—and more.
Psoriasis (choice “a”) commonly affects the penis, manifesting as pinkish plaques and papules. But there is a good chance that examination would have revealed corroborative signs of this disease. Furthermore, the histologic results would have been entirely different.
While syphilis (choice “b”), especially in its primary stage, can present with nonhealing sores, in no way do they resemble the patient’s lesions. There is also no source for such an infection. And biopsy would have shown a predominately plasma cell infiltrate in an entirely different pattern.
Lichen sclerosus et atrophicus (choice “d”) is quite uncommon, especially on the penis, where it is usually known as balanitis xerotica obliterans (BXO). As its name suggests, BXO is usually atrophic—therefore macular—and whitish. Exclusive to uncircumcised men, it bears no resemblance to condyloma.
Though idiopathic, lichen planus is not contagious. Unless neglected, this condition seldom causes any suffering aside from mental anguish over its appearance. To make a more accurate diagnosis, it is always helpful for providers to consider a mnemonic device for “7 Ps” associated with lichen planus:
- Penile
- Pruritic
- Plaque-like
- Purple
- Papular
- Planar
- Puzzling.
TREATMENT
Fortunately, lichen planus affecting the penis responds readily to treatment with mid-strength topical steroid cream and the "tincture of time," which improves its appearance until it eventually disappears. For this patient, the PCP treated the affected area with triamcinolone 0.1% cream bid for 2 weeks. This was then applied once a day every other day for a month, which cleared the patient’s lesions.
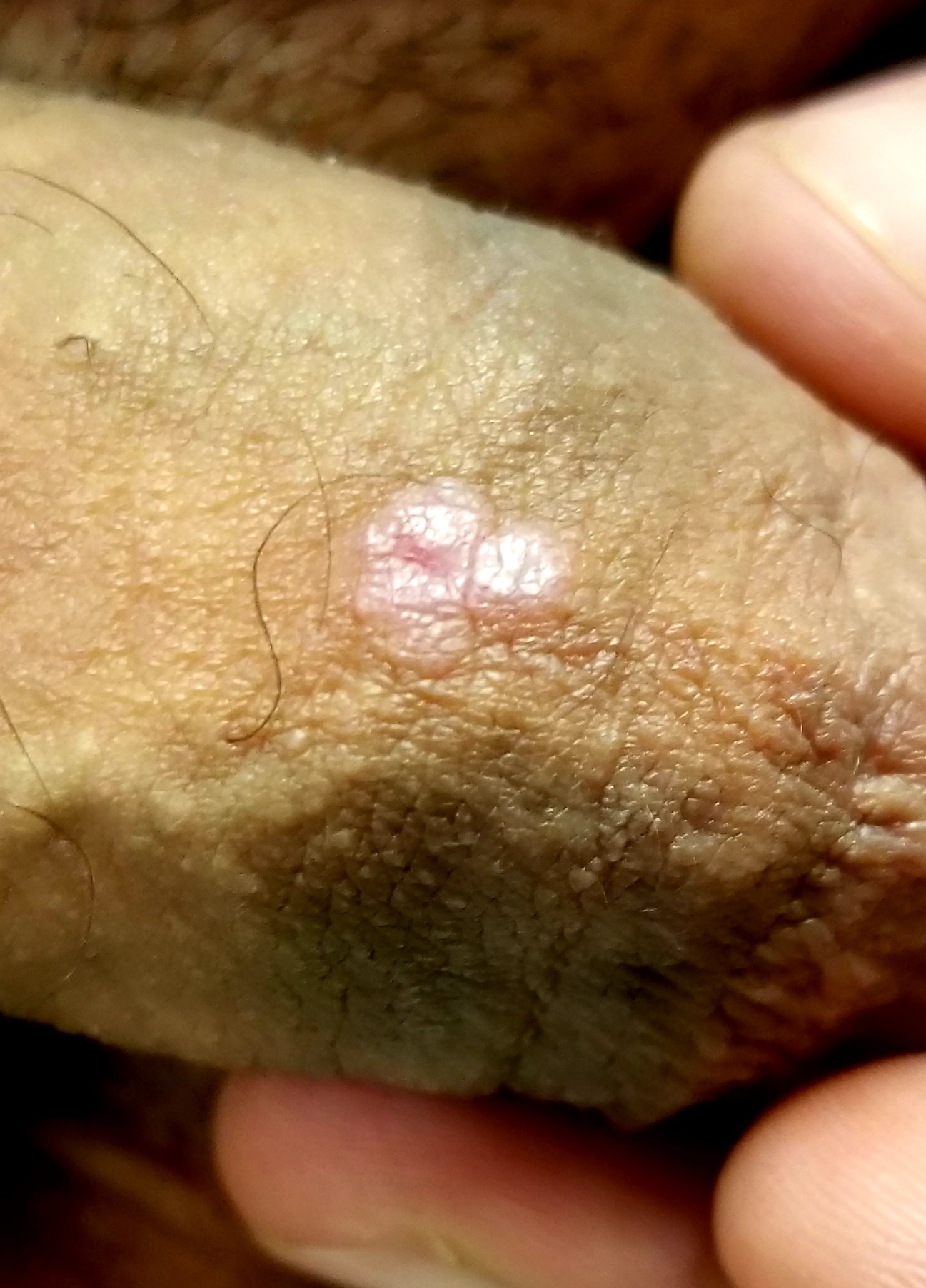
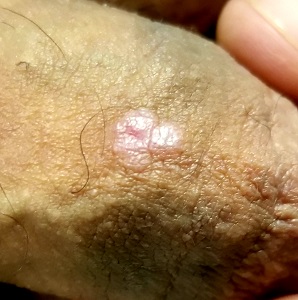
A 41-year-old man is understandably upset when his primary care provider (PCP) diagnoses him with penile warts. Still, he is more than willing to allow his PCP to treat the area with liquid nitrogen, which clears the affected area. However, after about a month, the warts reappear in the same area, with the same appearance, and the patient decides to consult his PCP about additional treatment.
To his distress, his PCP suggests that the warts may continue to return despite treatment. This prompts the patient to ask a more upsetting question: How had he even acquired the warts? Neither he nor his wife of 20 years has had any other sexual contact. Prior to marriage, he had no sexual encounters by which he might have acquired human papillomavirus (HPV).
The patient is otherwise quite healthy, though anxious to have his warts treated again despite the possibility of recurrence. At no point have the warts been symptomatic. His wife's Pap smears have been completely normal.
Examination reveals 4 tiny, pink, planar (flat-topped), 2-to-4-mm papules in 2 locations on the penile shaft. Each has a soft shiny surface. There is also a soft, smooth, pink, annular, 2-cm plaque on the distal shaft that spills over onto the corona focally.
Shave biopsy of 1 lesion shows a brisk lymphocytic infiltrate, which obliterated the dermo-epidermal junction, imparting a jagged sawtooth pattern to its usually smooth wave-like pattern. There are no signs of HPV. The patient has no other remarkable lesions or changes on his elbows, knees, trunk, legs, nails, or scalp.
She Can’t Turn the Other Cheek on the Lesion
ANSWER
The correct answer is seborrheic keratosis (choice “a”).
DISCUSSION
Seborrheic keratosis could not be in the differential because it is, by definition, an epidermal lesion—that is, “stuck on” the surface of the skin. It creates a rough surface that can be easily scraped off. The lesion could have been an actual scar, but other factors (its continuous growth) and the history of excessive ultraviolet exposure pushed us away from including this condition in the differential.
The differential for this patient included sun-caused skin cancers: basal cell carcinoma (BCC; choice “b”), squamous cell carcinoma (SCC; choice “d”), and amelanotic melanoma (choice “c”). These conditions can have a colorless and scar-like appearance, and they also destroy surface adnexae. Therefore, the lack of hairs, pores, or skin lines in a circumscribed area should raise concern for possible skin cancer, especially in at-risk patients such as this one.
BCC (otherwise known as cicatricial basal cell carcinoma) is by far the most common of all sun-caused skin cancers, but it usually presents as an obvious papule or nodule, often with telltale features such as pearly, rolled borders and focal erosion or ulceration. But there are exceptions, and the scar-like BCC is one.
SCC can also occasionally present in this manner, as can amelanotic melanoma, which is a colorless melanoma and very easy to miss. This case perfectly illustrates the point I often make to the students and residents I teach: When skin cancer is suspected, pay at least as much attention to the owner as to the lesion. Also, when in doubt, biopsy will settle the matter.
TREATMENT
For the patient, shave biopsy confirmed the presence of BCC. She was then referred for Mohs micrographic surgery because of the lesion’s size, location, and uncertain visible margins.
ANSWER
The correct answer is seborrheic keratosis (choice “a”).
DISCUSSION
Seborrheic keratosis could not be in the differential because it is, by definition, an epidermal lesion—that is, “stuck on” the surface of the skin. It creates a rough surface that can be easily scraped off. The lesion could have been an actual scar, but other factors (its continuous growth) and the history of excessive ultraviolet exposure pushed us away from including this condition in the differential.
The differential for this patient included sun-caused skin cancers: basal cell carcinoma (BCC; choice “b”), squamous cell carcinoma (SCC; choice “d”), and amelanotic melanoma (choice “c”). These conditions can have a colorless and scar-like appearance, and they also destroy surface adnexae. Therefore, the lack of hairs, pores, or skin lines in a circumscribed area should raise concern for possible skin cancer, especially in at-risk patients such as this one.
BCC (otherwise known as cicatricial basal cell carcinoma) is by far the most common of all sun-caused skin cancers, but it usually presents as an obvious papule or nodule, often with telltale features such as pearly, rolled borders and focal erosion or ulceration. But there are exceptions, and the scar-like BCC is one.
SCC can also occasionally present in this manner, as can amelanotic melanoma, which is a colorless melanoma and very easy to miss. This case perfectly illustrates the point I often make to the students and residents I teach: When skin cancer is suspected, pay at least as much attention to the owner as to the lesion. Also, when in doubt, biopsy will settle the matter.
TREATMENT
For the patient, shave biopsy confirmed the presence of BCC. She was then referred for Mohs micrographic surgery because of the lesion’s size, location, and uncertain visible margins.
ANSWER
The correct answer is seborrheic keratosis (choice “a”).
DISCUSSION
Seborrheic keratosis could not be in the differential because it is, by definition, an epidermal lesion—that is, “stuck on” the surface of the skin. It creates a rough surface that can be easily scraped off. The lesion could have been an actual scar, but other factors (its continuous growth) and the history of excessive ultraviolet exposure pushed us away from including this condition in the differential.
The differential for this patient included sun-caused skin cancers: basal cell carcinoma (BCC; choice “b”), squamous cell carcinoma (SCC; choice “d”), and amelanotic melanoma (choice “c”). These conditions can have a colorless and scar-like appearance, and they also destroy surface adnexae. Therefore, the lack of hairs, pores, or skin lines in a circumscribed area should raise concern for possible skin cancer, especially in at-risk patients such as this one.
BCC (otherwise known as cicatricial basal cell carcinoma) is by far the most common of all sun-caused skin cancers, but it usually presents as an obvious papule or nodule, often with telltale features such as pearly, rolled borders and focal erosion or ulceration. But there are exceptions, and the scar-like BCC is one.
SCC can also occasionally present in this manner, as can amelanotic melanoma, which is a colorless melanoma and very easy to miss. This case perfectly illustrates the point I often make to the students and residents I teach: When skin cancer is suspected, pay at least as much attention to the owner as to the lesion. Also, when in doubt, biopsy will settle the matter.
TREATMENT
For the patient, shave biopsy confirmed the presence of BCC. She was then referred for Mohs micrographic surgery because of the lesion’s size, location, and uncertain visible margins.
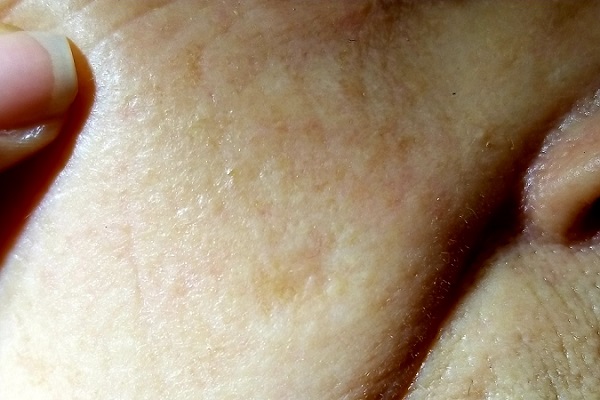
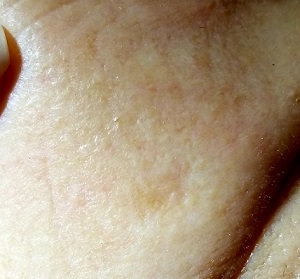
For several years, a 70-year-old woman has had an asymptomatic lesion on her cheek that has been growing slowly and steadily. Her primary care provider has reassured her at multiple visits that it should not cause her worry. Still, because of the lesion’s continued growth and her history of excessive sun exposure when she was young, she self-refers to dermatology for evaluation.
The patient has no history of skin cancer but her 2 sisters do, including a recent diagnosis of melanoma for one of them. During the 1950s, the 3 sisters were often outdoors—all burning easily and often and tanning only with difficulty. Since then, the sisters’ sun-drenched days have ended. All are in otherwise excellent health.
Examination reveals a patient with quite fair (type 2) skin and blue eyes. There is abundant evidence of past overexposure to ultraviolet light, including a weathered effect, scattered telangiectasias, and patches of white mottled skin (otherwise known as solar elastosis).
The lesion in question is quite faint and difficult to see. Magnification shows a 2-cm round patch that is slightly lighter than the surrounding skin and completely macular. No induration is felt on palpation, and no nodes are detected in the region.
An even closer and meticulous examination reveals that the surface adnexal structures—such as pores, skin lines, and even tiny hairs—that should be inside the lesion are completely missing. Slightly yellowish discoloration can be seen in the center of the patch. The rest of her skin shows no other worrisome features or lesions.