User login
The ability to distinguish between the two key variants of actinic keratosis is key to effective management, according to Dr. Theodore Rosen.
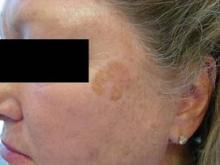
Pigmented actinic keratosis (AK) that spreads typically occurs in patients older than age 60 years and affects more women than men. The lesions are larger than 1.5 cm and have a history of lateral spread. "The lesions are flat, with a smooth, scaly surface, and they occur on sun-exposed skin, mostly the face, and near other manifestations of photodamage," noted Dr. Rosen at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Differential diagnosis includes solar lentigo, lentigo maligna, lentigo maligna melanoma, seborrheic keratosis, and pigmented squamous cell carcinoma in situ. "The presence of dots, globules, and asymmetry on dermatoscopy can help you distinguish spreading pigmented AKs from other lesions," said Dr. Rosen, professor of dermatology at Baylor College of Medicine, Houston.
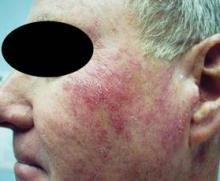
The other main variant, proliferating AK, also tends to affect patients older than age 60 but it occurs more commonly in men than in women. This variant is greater than 1.5 cm in size with a history of rapid lateral spread, and it is marked by a confluent scaly surface with some palpability. Affected areas include sun-exposed skin, mostly the face, and areas near other manifestations of photodamage. "This variant is resistant to usual topical therapy, and the differential diagnosis may include eczema, psoriasis, squamous cell carcinoma in situ, and superficial basal cell carcinoma," said Dr. Rosen, who is also chief of the dermatology clinic at the Houston-based Michael E. DeBakey VA Medical Center. Histology reveals fingerlike invasive projections into the dermis of atypical squamous cells.
The appearance of multiple AKs in a cosmetic unit indicates that the clinician should consider the entire photodamaged area to be diseased. This concept, known as field-directed therapy, "not only addresses apparent clinical lesions, but also reveals and may treat subclinical lesions," he said. "Field therapy may also offer the advantage of reversing basic cellular aberrations leading to transition into invasive cutaneous malignancy."
Another trend in the treatment of AKs is the development of new imiquimod formulations. Results from two placebo-controlled studies of daily application of 2.5% and 3.75% imiquimod creams to the face and balding scalp for two 3-week cycles revealed that both formulations were more effective than placebo and had an acceptable safety profile (J. Am. Acad. Dermatol. 2010;62:573-81). The final evaluation occurred 8 weeks after the final treatment, said Dr. Rosen, who was one of the study investigators. Results from this and other studies led to Food and Drug Administration approval of imiquimod 2.5% (Zyclara) for AKs on July 19, 2011, but the formulation is not yet commercially available.
In a more recent analysis, investigators assessed complete clearance rates in AK patients from four phase III trials of imiquimod who were followed for 1 year (J. Drugs Dermatol. 2011;10:165-70). For imiquimod 3.75% and 2.5% cream, respectively, complete clearance was sustained for 1 year in 40.5% and 33.3% of patients from the 2-week cycle studies, and in 47.9% and 43.2% of patients from the 3-week cycle studies.
Combination therapies for AKs have become increasingly popular. Treatments include cryosurgery followed by diclofenac, 5-fluorouracil followed by cryosurgery, cryosurgery followed by imiquimod 5% or 3.75%, photodynamic therapy (PTD) followed by imiquimod 5%, and tazarotene followed by PDT. "For all studies where field therapy is combined with lesion-directed therapy or with another field therapy, the combination proved superior to monotherapy," Dr. Rosen said.
He went on to note that there is considerable user variation – such as time, the distance the device is held from the skin, and the type of unit used – in the delivery of cryosurgery to treat AKs. The variation "may have more to do with skin temperature than any other variable," said Dr. Rosen. In one study, investigators used an infrared detector in a liquid nitrogen container to deliver cryotherapy to a temperature of –5° C in 36 patients with 180 thin AKs (Dermatol. Surg. 2010;36:1956-61). The clearance rates were 67% at 1 week and 100% at 6 weeks.
Treatment of AKs with radiation is another area of study. In one recent trial, 12 patients with refractory AK and 4 patients with AKs near a nonmelanoma skin cancer underwent external beam radiation therapy five times a week for 4-6 weeks. The total dose of radiation ranged from 4 to 60 Gy (J. Clin. Aesthet. Dermatol. 2011;4:47-50). Of the 16 patients, 13 had complete resolution of AKs, 1 noted a prompt recurrence, and 90% said they were "very satisfied" with the treatment results.
Treating AKs with methyl aminolevulinate photodynamic therapy (MAL-PDT) is also being investigated. In a multicenter study conducted in Scandinavia, 120 patients with 1,572 AKs underwent MAL-PDT followed by immediate exposure to the sun for 1.5-2.5 hours (Br. J. Dermatol. 2011;164:1083-90). At 3 months, 75%-77% of the lesions had cleared. This approach "has an advantage for the health care provider in that no equipment is needed," Dr. Rosen said. "The advantage for the patient is that the therapy is nearly pain free."
Dr. Rosen disclosed that he is a consultant and a member of the speakers bureau for Medicis, which makes imiquimod. He is also a consultant for LEO Pharma.
SDEF and this news organization are owned by Elsevier.
The ability to distinguish between the two key variants of actinic keratosis is key to effective management, according to Dr. Theodore Rosen.
Pigmented actinic keratosis (AK) that spreads typically occurs in patients older than age 60 years and affects more women than men. The lesions are larger than 1.5 cm and have a history of lateral spread. "The lesions are flat, with a smooth, scaly surface, and they occur on sun-exposed skin, mostly the face, and near other manifestations of photodamage," noted Dr. Rosen at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Differential diagnosis includes solar lentigo, lentigo maligna, lentigo maligna melanoma, seborrheic keratosis, and pigmented squamous cell carcinoma in situ. "The presence of dots, globules, and asymmetry on dermatoscopy can help you distinguish spreading pigmented AKs from other lesions," said Dr. Rosen, professor of dermatology at Baylor College of Medicine, Houston.
The other main variant, proliferating AK, also tends to affect patients older than age 60 but it occurs more commonly in men than in women. This variant is greater than 1.5 cm in size with a history of rapid lateral spread, and it is marked by a confluent scaly surface with some palpability. Affected areas include sun-exposed skin, mostly the face, and areas near other manifestations of photodamage. "This variant is resistant to usual topical therapy, and the differential diagnosis may include eczema, psoriasis, squamous cell carcinoma in situ, and superficial basal cell carcinoma," said Dr. Rosen, who is also chief of the dermatology clinic at the Houston-based Michael E. DeBakey VA Medical Center. Histology reveals fingerlike invasive projections into the dermis of atypical squamous cells.
The appearance of multiple AKs in a cosmetic unit indicates that the clinician should consider the entire photodamaged area to be diseased. This concept, known as field-directed therapy, "not only addresses apparent clinical lesions, but also reveals and may treat subclinical lesions," he said. "Field therapy may also offer the advantage of reversing basic cellular aberrations leading to transition into invasive cutaneous malignancy."
Another trend in the treatment of AKs is the development of new imiquimod formulations. Results from two placebo-controlled studies of daily application of 2.5% and 3.75% imiquimod creams to the face and balding scalp for two 3-week cycles revealed that both formulations were more effective than placebo and had an acceptable safety profile (J. Am. Acad. Dermatol. 2010;62:573-81). The final evaluation occurred 8 weeks after the final treatment, said Dr. Rosen, who was one of the study investigators. Results from this and other studies led to Food and Drug Administration approval of imiquimod 2.5% (Zyclara) for AKs on July 19, 2011, but the formulation is not yet commercially available.
In a more recent analysis, investigators assessed complete clearance rates in AK patients from four phase III trials of imiquimod who were followed for 1 year (J. Drugs Dermatol. 2011;10:165-70). For imiquimod 3.75% and 2.5% cream, respectively, complete clearance was sustained for 1 year in 40.5% and 33.3% of patients from the 2-week cycle studies, and in 47.9% and 43.2% of patients from the 3-week cycle studies.
Combination therapies for AKs have become increasingly popular. Treatments include cryosurgery followed by diclofenac, 5-fluorouracil followed by cryosurgery, cryosurgery followed by imiquimod 5% or 3.75%, photodynamic therapy (PTD) followed by imiquimod 5%, and tazarotene followed by PDT. "For all studies where field therapy is combined with lesion-directed therapy or with another field therapy, the combination proved superior to monotherapy," Dr. Rosen said.
He went on to note that there is considerable user variation – such as time, the distance the device is held from the skin, and the type of unit used – in the delivery of cryosurgery to treat AKs. The variation "may have more to do with skin temperature than any other variable," said Dr. Rosen. In one study, investigators used an infrared detector in a liquid nitrogen container to deliver cryotherapy to a temperature of –5° C in 36 patients with 180 thin AKs (Dermatol. Surg. 2010;36:1956-61). The clearance rates were 67% at 1 week and 100% at 6 weeks.
Treatment of AKs with radiation is another area of study. In one recent trial, 12 patients with refractory AK and 4 patients with AKs near a nonmelanoma skin cancer underwent external beam radiation therapy five times a week for 4-6 weeks. The total dose of radiation ranged from 4 to 60 Gy (J. Clin. Aesthet. Dermatol. 2011;4:47-50). Of the 16 patients, 13 had complete resolution of AKs, 1 noted a prompt recurrence, and 90% said they were "very satisfied" with the treatment results.
Treating AKs with methyl aminolevulinate photodynamic therapy (MAL-PDT) is also being investigated. In a multicenter study conducted in Scandinavia, 120 patients with 1,572 AKs underwent MAL-PDT followed by immediate exposure to the sun for 1.5-2.5 hours (Br. J. Dermatol. 2011;164:1083-90). At 3 months, 75%-77% of the lesions had cleared. This approach "has an advantage for the health care provider in that no equipment is needed," Dr. Rosen said. "The advantage for the patient is that the therapy is nearly pain free."
Dr. Rosen disclosed that he is a consultant and a member of the speakers bureau for Medicis, which makes imiquimod. He is also a consultant for LEO Pharma.
SDEF and this news organization are owned by Elsevier.
The ability to distinguish between the two key variants of actinic keratosis is key to effective management, according to Dr. Theodore Rosen.
Pigmented actinic keratosis (AK) that spreads typically occurs in patients older than age 60 years and affects more women than men. The lesions are larger than 1.5 cm and have a history of lateral spread. "The lesions are flat, with a smooth, scaly surface, and they occur on sun-exposed skin, mostly the face, and near other manifestations of photodamage," noted Dr. Rosen at the annual Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation (SDEF).
Differential diagnosis includes solar lentigo, lentigo maligna, lentigo maligna melanoma, seborrheic keratosis, and pigmented squamous cell carcinoma in situ. "The presence of dots, globules, and asymmetry on dermatoscopy can help you distinguish spreading pigmented AKs from other lesions," said Dr. Rosen, professor of dermatology at Baylor College of Medicine, Houston.
The other main variant, proliferating AK, also tends to affect patients older than age 60 but it occurs more commonly in men than in women. This variant is greater than 1.5 cm in size with a history of rapid lateral spread, and it is marked by a confluent scaly surface with some palpability. Affected areas include sun-exposed skin, mostly the face, and areas near other manifestations of photodamage. "This variant is resistant to usual topical therapy, and the differential diagnosis may include eczema, psoriasis, squamous cell carcinoma in situ, and superficial basal cell carcinoma," said Dr. Rosen, who is also chief of the dermatology clinic at the Houston-based Michael E. DeBakey VA Medical Center. Histology reveals fingerlike invasive projections into the dermis of atypical squamous cells.
The appearance of multiple AKs in a cosmetic unit indicates that the clinician should consider the entire photodamaged area to be diseased. This concept, known as field-directed therapy, "not only addresses apparent clinical lesions, but also reveals and may treat subclinical lesions," he said. "Field therapy may also offer the advantage of reversing basic cellular aberrations leading to transition into invasive cutaneous malignancy."
Another trend in the treatment of AKs is the development of new imiquimod formulations. Results from two placebo-controlled studies of daily application of 2.5% and 3.75% imiquimod creams to the face and balding scalp for two 3-week cycles revealed that both formulations were more effective than placebo and had an acceptable safety profile (J. Am. Acad. Dermatol. 2010;62:573-81). The final evaluation occurred 8 weeks after the final treatment, said Dr. Rosen, who was one of the study investigators. Results from this and other studies led to Food and Drug Administration approval of imiquimod 2.5% (Zyclara) for AKs on July 19, 2011, but the formulation is not yet commercially available.
In a more recent analysis, investigators assessed complete clearance rates in AK patients from four phase III trials of imiquimod who were followed for 1 year (J. Drugs Dermatol. 2011;10:165-70). For imiquimod 3.75% and 2.5% cream, respectively, complete clearance was sustained for 1 year in 40.5% and 33.3% of patients from the 2-week cycle studies, and in 47.9% and 43.2% of patients from the 3-week cycle studies.
Combination therapies for AKs have become increasingly popular. Treatments include cryosurgery followed by diclofenac, 5-fluorouracil followed by cryosurgery, cryosurgery followed by imiquimod 5% or 3.75%, photodynamic therapy (PTD) followed by imiquimod 5%, and tazarotene followed by PDT. "For all studies where field therapy is combined with lesion-directed therapy or with another field therapy, the combination proved superior to monotherapy," Dr. Rosen said.
He went on to note that there is considerable user variation – such as time, the distance the device is held from the skin, and the type of unit used – in the delivery of cryosurgery to treat AKs. The variation "may have more to do with skin temperature than any other variable," said Dr. Rosen. In one study, investigators used an infrared detector in a liquid nitrogen container to deliver cryotherapy to a temperature of –5° C in 36 patients with 180 thin AKs (Dermatol. Surg. 2010;36:1956-61). The clearance rates were 67% at 1 week and 100% at 6 weeks.
Treatment of AKs with radiation is another area of study. In one recent trial, 12 patients with refractory AK and 4 patients with AKs near a nonmelanoma skin cancer underwent external beam radiation therapy five times a week for 4-6 weeks. The total dose of radiation ranged from 4 to 60 Gy (J. Clin. Aesthet. Dermatol. 2011;4:47-50). Of the 16 patients, 13 had complete resolution of AKs, 1 noted a prompt recurrence, and 90% said they were "very satisfied" with the treatment results.
Treating AKs with methyl aminolevulinate photodynamic therapy (MAL-PDT) is also being investigated. In a multicenter study conducted in Scandinavia, 120 patients with 1,572 AKs underwent MAL-PDT followed by immediate exposure to the sun for 1.5-2.5 hours (Br. J. Dermatol. 2011;164:1083-90). At 3 months, 75%-77% of the lesions had cleared. This approach "has an advantage for the health care provider in that no equipment is needed," Dr. Rosen said. "The advantage for the patient is that the therapy is nearly pain free."
Dr. Rosen disclosed that he is a consultant and a member of the speakers bureau for Medicis, which makes imiquimod. He is also a consultant for LEO Pharma.
SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF HAWAII DERMATOLOGY SEMINAR