User login
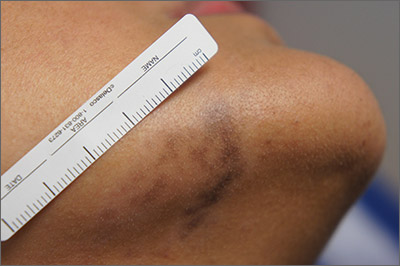
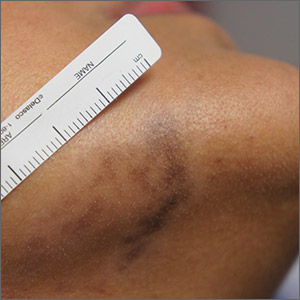
Exam and biopsy led to a diagnosis of erythema dyschromicum perstans. Notably, the punch biopsy was performed as superficially as possible to avoid injuring the marginal mandibular branch of the facial nerve. Histology showed focal vacuolar interface changes, pigmentary incontinence, and prominent dermal melanophages—consistent with erythema dyschromicum perstans.
Erythema dyschromicum perstans is an uncommon dermal macular hyperpigmentation that can affect patients of all ages. It is more often seen in patients with Fitzpatrick skin types III and IV. Some patients have a preceding inflammatory phase with associated erythema.
It is believed that erythema dyschromicum perstans may be a form of pigmented lichen planus with similar histologic changes. Genetic predisposition and medications, such as penicillamine and omeprazole, have been suggested as predisposing risk factors, although these risk factors are not always present. Similarly, cases of erythema dyschromicum perstans associated with human immunodeficiency virus and hepatitis C virus have been reported, but a causal link has not been established. Commonly affected sites include the face and neck, although patches on the trunk and extremities occur, as well.
The differential diagnosis includes lichen planus, discoid lupus, drug-induced hyperpigmentation, Hansen disease, and fixed drug eruption.
Erythema dyschromicum perstans is resistant to most therapies, yet it may clear spontaneously over the years. Therapies that have been successful in case reports include Q-switched ruby laser, topical steroids, UV therapy, isotretinoin, and clofazimine. This patient used desonide cream 0.05% bid for 3 weeks without improvement. She then used camouflage concealer for a year, at which point the area had faded almost completely.
Photos and text for Photo Rounds Friday courtesy of Jonathan Karnes, MD (copyright retained). Dr. Karnes is the medical director of MDFMR Dermatology Services, Augusta, ME.
Gutierrez D, Krueger LD, Tan A, et al. Proton pump inhibitor-induced erythema dyschromicum perstans-like pigmentation. JAAD Case Rep. 2019;5:701-703.
Exam and biopsy led to a diagnosis of erythema dyschromicum perstans. Notably, the punch biopsy was performed as superficially as possible to avoid injuring the marginal mandibular branch of the facial nerve. Histology showed focal vacuolar interface changes, pigmentary incontinence, and prominent dermal melanophages—consistent with erythema dyschromicum perstans.
Erythema dyschromicum perstans is an uncommon dermal macular hyperpigmentation that can affect patients of all ages. It is more often seen in patients with Fitzpatrick skin types III and IV. Some patients have a preceding inflammatory phase with associated erythema.
It is believed that erythema dyschromicum perstans may be a form of pigmented lichen planus with similar histologic changes. Genetic predisposition and medications, such as penicillamine and omeprazole, have been suggested as predisposing risk factors, although these risk factors are not always present. Similarly, cases of erythema dyschromicum perstans associated with human immunodeficiency virus and hepatitis C virus have been reported, but a causal link has not been established. Commonly affected sites include the face and neck, although patches on the trunk and extremities occur, as well.
The differential diagnosis includes lichen planus, discoid lupus, drug-induced hyperpigmentation, Hansen disease, and fixed drug eruption.
Erythema dyschromicum perstans is resistant to most therapies, yet it may clear spontaneously over the years. Therapies that have been successful in case reports include Q-switched ruby laser, topical steroids, UV therapy, isotretinoin, and clofazimine. This patient used desonide cream 0.05% bid for 3 weeks without improvement. She then used camouflage concealer for a year, at which point the area had faded almost completely.
Photos and text for Photo Rounds Friday courtesy of Jonathan Karnes, MD (copyright retained). Dr. Karnes is the medical director of MDFMR Dermatology Services, Augusta, ME.
Exam and biopsy led to a diagnosis of erythema dyschromicum perstans. Notably, the punch biopsy was performed as superficially as possible to avoid injuring the marginal mandibular branch of the facial nerve. Histology showed focal vacuolar interface changes, pigmentary incontinence, and prominent dermal melanophages—consistent with erythema dyschromicum perstans.
Erythema dyschromicum perstans is an uncommon dermal macular hyperpigmentation that can affect patients of all ages. It is more often seen in patients with Fitzpatrick skin types III and IV. Some patients have a preceding inflammatory phase with associated erythema.
It is believed that erythema dyschromicum perstans may be a form of pigmented lichen planus with similar histologic changes. Genetic predisposition and medications, such as penicillamine and omeprazole, have been suggested as predisposing risk factors, although these risk factors are not always present. Similarly, cases of erythema dyschromicum perstans associated with human immunodeficiency virus and hepatitis C virus have been reported, but a causal link has not been established. Commonly affected sites include the face and neck, although patches on the trunk and extremities occur, as well.
The differential diagnosis includes lichen planus, discoid lupus, drug-induced hyperpigmentation, Hansen disease, and fixed drug eruption.
Erythema dyschromicum perstans is resistant to most therapies, yet it may clear spontaneously over the years. Therapies that have been successful in case reports include Q-switched ruby laser, topical steroids, UV therapy, isotretinoin, and clofazimine. This patient used desonide cream 0.05% bid for 3 weeks without improvement. She then used camouflage concealer for a year, at which point the area had faded almost completely.
Photos and text for Photo Rounds Friday courtesy of Jonathan Karnes, MD (copyright retained). Dr. Karnes is the medical director of MDFMR Dermatology Services, Augusta, ME.
Gutierrez D, Krueger LD, Tan A, et al. Proton pump inhibitor-induced erythema dyschromicum perstans-like pigmentation. JAAD Case Rep. 2019;5:701-703.
Gutierrez D, Krueger LD, Tan A, et al. Proton pump inhibitor-induced erythema dyschromicum perstans-like pigmentation. JAAD Case Rep. 2019;5:701-703.