User login
A consistent approach drives optimal scarring alopecia treatment
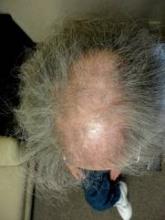
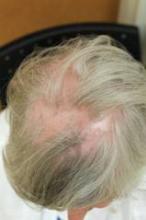
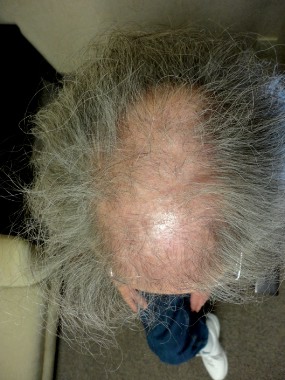
DENVER – To limit the progression of scarring alopecia, Dr. Jeff Donovan makes it a point to ask his patients about symptoms and shedding, and he always performs a thorough scalp examination to record the affected sites and signs of the condition.
"Everything on the history potentially may be important, but always ask about symptoms of itching, burning, pain, tenderness, and shedding," Dr. Donovan of the department of dermatology at the University of Toronto advised at the annual meeting of the American Academy of Dermatology.
Upon examination, he continued, document sites and signs by considering the following questions: Where is the hair loss – frontal, top, or occipital? Can you still see the follicular ostia? Is there erythema of the scalp? Is there perifollicular erythema or scale, crusting, pustules, or loss of eyebrow or body hair?
"When you perform dermoscopy of the normal scalp, one can see that the hairs are similar in ‘caliber’ (no miniaturization suggestive of androgenetic alopecia), and there are no changes around the hair follicles or between the hair follicles," Dr. Donovan said. "In scarring alopecia, a variety of findings may be present which help point to the correct diagnosis."
A 4-mm punch biopsy is helpful to confirm the diagnosis and is recommended in areas of early active disease, including areas that may have primary morphologic features, areas with a positive pull test (if possible), or areas that are symptomatic (if needed). "Diagnosing a hair disease with a biopsy requires a hair to be present in the biopsy," he noted. "Biopsies of completely scarred areas are not helpful." In scarring alopecias, inflammatory infiltrates are found in the upper parts of the hair follicle, which destroys hair follicle stem cells. "It’s this destruction of stem cells which ultimately leads to permanent hair loss," Dr. Donovan said.
Lichen planopilaris, a common form of scarring alopecia, typically occurs in middle age and is twice as common in women as in men. It most often affects the central scalp but may be present in other sites in up to half of cases. Key symptoms of lichen planopilaris (LPP) include hair loss, scalp pruritus, and pain/tenderness, often a burning sensation at the site of hair loss. On dermoscopy, most LPP cases appear as reduced hair density with scalp erythema and perifollicular scale, also called peripilar casts.
The goal of LPP treatment is to reduce symptoms and shedding and to stop the disease from occurring in new sites. "Regrowth is not possible in most scarring alopecias," said Dr. Donovan, who leads the University of Toronto’s program in hair transplantation and hair loss. "Treatments help to halt the underlying disease process. Disease activity may recur."
Treatment options for localized/limited LPP include intralesional triamcinolone acetonide and/or several treatments at home, including 0.05% clobetasol propionate lotion or foam, clobetasol propionate shampoo to help decrease itching and burning, fluocinolone acetonide oil one time per week to help with removal of scales, and topical 0.1% tacrolimus ointment (or compounded lotion) as needed.
Systemic treatment of LPP is also an option, and he said he relies on the dermatopathology report to guide his treatment decisions. If biopsy reveals minimal lymphocytic infiltrate, Dr. Donovan said he recommends doxycycline 100 mg b.i.d. as his first-line approach. If biopsy reveals moderate lymphocytic infiltrate, he turns to hydroxychloroquine 6 mg/kg.
His recommended second-line systemic treatment is mycophenolate mofetil 500 mg b.i.d. for 1 month, then 1,000 mg b.i.d. thereafter. Third-line systemic treatment options include cyclosporine 3-5 mg/kg per day and retinoids such as isotretinoin, but fewer than 20% of patients benefit from retinoids, he said. Once the disease becomes quiet, hair transplant surgery can sometimes be an option to restore hair density.
Dr. Donovan disclosed that he is the cofounder of Okavana Laboratories, a privately held company devoted to hair.
DENVER – To limit the progression of scarring alopecia, Dr. Jeff Donovan makes it a point to ask his patients about symptoms and shedding, and he always performs a thorough scalp examination to record the affected sites and signs of the condition.
"Everything on the history potentially may be important, but always ask about symptoms of itching, burning, pain, tenderness, and shedding," Dr. Donovan of the department of dermatology at the University of Toronto advised at the annual meeting of the American Academy of Dermatology.
Upon examination, he continued, document sites and signs by considering the following questions: Where is the hair loss – frontal, top, or occipital? Can you still see the follicular ostia? Is there erythema of the scalp? Is there perifollicular erythema or scale, crusting, pustules, or loss of eyebrow or body hair?
"When you perform dermoscopy of the normal scalp, one can see that the hairs are similar in ‘caliber’ (no miniaturization suggestive of androgenetic alopecia), and there are no changes around the hair follicles or between the hair follicles," Dr. Donovan said. "In scarring alopecia, a variety of findings may be present which help point to the correct diagnosis."
A 4-mm punch biopsy is helpful to confirm the diagnosis and is recommended in areas of early active disease, including areas that may have primary morphologic features, areas with a positive pull test (if possible), or areas that are symptomatic (if needed). "Diagnosing a hair disease with a biopsy requires a hair to be present in the biopsy," he noted. "Biopsies of completely scarred areas are not helpful." In scarring alopecias, inflammatory infiltrates are found in the upper parts of the hair follicle, which destroys hair follicle stem cells. "It’s this destruction of stem cells which ultimately leads to permanent hair loss," Dr. Donovan said.
Lichen planopilaris, a common form of scarring alopecia, typically occurs in middle age and is twice as common in women as in men. It most often affects the central scalp but may be present in other sites in up to half of cases. Key symptoms of lichen planopilaris (LPP) include hair loss, scalp pruritus, and pain/tenderness, often a burning sensation at the site of hair loss. On dermoscopy, most LPP cases appear as reduced hair density with scalp erythema and perifollicular scale, also called peripilar casts.
The goal of LPP treatment is to reduce symptoms and shedding and to stop the disease from occurring in new sites. "Regrowth is not possible in most scarring alopecias," said Dr. Donovan, who leads the University of Toronto’s program in hair transplantation and hair loss. "Treatments help to halt the underlying disease process. Disease activity may recur."
Treatment options for localized/limited LPP include intralesional triamcinolone acetonide and/or several treatments at home, including 0.05% clobetasol propionate lotion or foam, clobetasol propionate shampoo to help decrease itching and burning, fluocinolone acetonide oil one time per week to help with removal of scales, and topical 0.1% tacrolimus ointment (or compounded lotion) as needed.
Systemic treatment of LPP is also an option, and he said he relies on the dermatopathology report to guide his treatment decisions. If biopsy reveals minimal lymphocytic infiltrate, Dr. Donovan said he recommends doxycycline 100 mg b.i.d. as his first-line approach. If biopsy reveals moderate lymphocytic infiltrate, he turns to hydroxychloroquine 6 mg/kg.
His recommended second-line systemic treatment is mycophenolate mofetil 500 mg b.i.d. for 1 month, then 1,000 mg b.i.d. thereafter. Third-line systemic treatment options include cyclosporine 3-5 mg/kg per day and retinoids such as isotretinoin, but fewer than 20% of patients benefit from retinoids, he said. Once the disease becomes quiet, hair transplant surgery can sometimes be an option to restore hair density.
Dr. Donovan disclosed that he is the cofounder of Okavana Laboratories, a privately held company devoted to hair.
DENVER – To limit the progression of scarring alopecia, Dr. Jeff Donovan makes it a point to ask his patients about symptoms and shedding, and he always performs a thorough scalp examination to record the affected sites and signs of the condition.
"Everything on the history potentially may be important, but always ask about symptoms of itching, burning, pain, tenderness, and shedding," Dr. Donovan of the department of dermatology at the University of Toronto advised at the annual meeting of the American Academy of Dermatology.
Upon examination, he continued, document sites and signs by considering the following questions: Where is the hair loss – frontal, top, or occipital? Can you still see the follicular ostia? Is there erythema of the scalp? Is there perifollicular erythema or scale, crusting, pustules, or loss of eyebrow or body hair?
"When you perform dermoscopy of the normal scalp, one can see that the hairs are similar in ‘caliber’ (no miniaturization suggestive of androgenetic alopecia), and there are no changes around the hair follicles or between the hair follicles," Dr. Donovan said. "In scarring alopecia, a variety of findings may be present which help point to the correct diagnosis."
A 4-mm punch biopsy is helpful to confirm the diagnosis and is recommended in areas of early active disease, including areas that may have primary morphologic features, areas with a positive pull test (if possible), or areas that are symptomatic (if needed). "Diagnosing a hair disease with a biopsy requires a hair to be present in the biopsy," he noted. "Biopsies of completely scarred areas are not helpful." In scarring alopecias, inflammatory infiltrates are found in the upper parts of the hair follicle, which destroys hair follicle stem cells. "It’s this destruction of stem cells which ultimately leads to permanent hair loss," Dr. Donovan said.
Lichen planopilaris, a common form of scarring alopecia, typically occurs in middle age and is twice as common in women as in men. It most often affects the central scalp but may be present in other sites in up to half of cases. Key symptoms of lichen planopilaris (LPP) include hair loss, scalp pruritus, and pain/tenderness, often a burning sensation at the site of hair loss. On dermoscopy, most LPP cases appear as reduced hair density with scalp erythema and perifollicular scale, also called peripilar casts.
The goal of LPP treatment is to reduce symptoms and shedding and to stop the disease from occurring in new sites. "Regrowth is not possible in most scarring alopecias," said Dr. Donovan, who leads the University of Toronto’s program in hair transplantation and hair loss. "Treatments help to halt the underlying disease process. Disease activity may recur."
Treatment options for localized/limited LPP include intralesional triamcinolone acetonide and/or several treatments at home, including 0.05% clobetasol propionate lotion or foam, clobetasol propionate shampoo to help decrease itching and burning, fluocinolone acetonide oil one time per week to help with removal of scales, and topical 0.1% tacrolimus ointment (or compounded lotion) as needed.
Systemic treatment of LPP is also an option, and he said he relies on the dermatopathology report to guide his treatment decisions. If biopsy reveals minimal lymphocytic infiltrate, Dr. Donovan said he recommends doxycycline 100 mg b.i.d. as his first-line approach. If biopsy reveals moderate lymphocytic infiltrate, he turns to hydroxychloroquine 6 mg/kg.
His recommended second-line systemic treatment is mycophenolate mofetil 500 mg b.i.d. for 1 month, then 1,000 mg b.i.d. thereafter. Third-line systemic treatment options include cyclosporine 3-5 mg/kg per day and retinoids such as isotretinoin, but fewer than 20% of patients benefit from retinoids, he said. Once the disease becomes quiet, hair transplant surgery can sometimes be an option to restore hair density.
Dr. Donovan disclosed that he is the cofounder of Okavana Laboratories, a privately held company devoted to hair.
AT THE AAD ANNUAL MEETING
‘Culture of Safety’ Best Defense Against Sharps Injury
DENVER – Of all the procedures and behaviors that place dermatologists at risk for occupational exposure, needlestick injuries rank at the top.
According to 1999 data from the National Institute for Occupational Safety and Health, one in five health care workers sustains a needlestick injury each year, putting them at risk for acquiring pathogens such as HIV and hepatitis B and C viruses. "Conjunctival transmission of blood-borne pathogens can occur, and there are at least two cases of documented transmission of HIV via splashes," Dr. Joseph F. Sobanko said at the annual meeting of the American Academy of Dermatology. "Operating with exposed, nonintact skin also poses a risk of transmission of bloodborne pathogens."
Dr. Sobanko, a Mohs and reconstructive surgeon and director of dermatologic surgery education at the Hospital of the University of Pennsylvania, Philadelphia, emphasized that all health care employees are at risk of sharps injury. "Those physicians with the least experience are the most likely to receive an occupational exposure," he said. "When trainees and students receive injury, it is a risk factor for receiving future injuries, perhaps because of improper training early on."
A pilot study of sharps-related injuries in California health care facilities found that 49% occurred among nurses, followed by physicians (10%), phlebotomists (8%), and housekeeping and laundry personnel (7%), while the remainder occurred among a variety of other health care workers (Infect. Control Hosp. Epidemiol. 2003;24:113-21).
A separate survey study of needlestick injuries among 699 recent medical school graduates enrolled in a surgery residency at one of 17 medical centers in the United States found that 59% had a stick as a student, most commonly from suturing (42%), passing the needle (17%), and loading the needle (12%) (Academic Med. 2009;84:1815-21).
"Other studies have found that needlestick injuries commonly occur during device use and after device use during disposal," Dr. Sobanko noted.
Most occupational exposures are self-inflicted, and most sharps injuries tend to affect the left hand and digits, he continued. "When suturing, the injury that is self inflicted often happens on the nondominant hand," he said. "However, when not suturing but passing instruments (which shouldn’t be done), health care professionals are more likely to be injured on the dominant hand, because they accept the instrument with this hand. This is why ‘surgical neutral zones’ should be created to transfer instruments and eliminate this particular form of injury."
Occupational exposure is especially high in dermatology. One survey of 452 dermatologists queried in November of 2009 found a 90% injury rate (J. Am. Acad. Dermatol. 2011;65:648-50), while a separate, more recent survey of 336 dermatologists found an 85% injury rate 40% of the injuries had occurred within the year before the survey (Dermatol. Surg. 2013;39:1813-21). More than two-thirds of those same respondents (64%) reported having ever had a sharps injury that went unreported.
Procedures and behaviors that place dermatologists at highest risk for occupational exposure include drawing up solution, setting up a tray, injection, excision, biopsy, obtaining hemostasis, suturing, and disposal of sharps.
"Shortcuts, lack of focus, and improper training lead to avoidable accidents," Dr. Sobanko said. "Fostering a culture of safety can help reduce the risk of future injuries."
His recommended technique for uncapping a needle, for example, involves anchoring the top hand to the bottom hand, as in a golfer’s grip. Gentle extension releases the cap. His recommended technique for drawing solution involves resting the syringe on the hypothenar eminence of the left hand while holding the barrel with the thumb and index finger. This allows for safe placement of the bottle onto the needle. "This technique eliminates the risk of recoil injury if a cap is simply just pulled off a syringe at chest level, analogous to stretching a rubber band," he explained.
To avoid injuries while injecting, Dr. Sobanko advises ensuring that the hand or finger stabilizing the skin stays behind the path of the needle.
Dermatologists can keep themselves safe during office procedures by using protective sharps, eye protection, and gloves and by transferring instruments by implementing a neutral zone on the surgical tray. One review of seven studies of needle protective devices demonstrated an average 71% reduction in needlestick injuries (J. Hosp. Infect. 2003;53:237-42).
Dr. Sobanko described a safe needle device as one that is "easy to use and requires minimal effort to activate by the user. If activation is required, it must be a single-handed technique. The safety feature should click or be clear that it has activated, and the safety feature should remain protective throughout disposal."
Mental preparedness and motor repetition also play a role in protecting yourself. Dr. Sobanko’s five strategies for mental preparedness involve not rushing, knowing the pertinent anatomy for each case, having a proper tray set-up, having a proper preoperative plan, and not operating until an assistant is available.
Dr. Sobanko disclosed that he is a coeditor with Dr. Jacob Levitt of the forthcoming Springer book, "Atlas of Safe Practices in Office-Based Surgery."
DENVER – Of all the procedures and behaviors that place dermatologists at risk for occupational exposure, needlestick injuries rank at the top.
According to 1999 data from the National Institute for Occupational Safety and Health, one in five health care workers sustains a needlestick injury each year, putting them at risk for acquiring pathogens such as HIV and hepatitis B and C viruses. "Conjunctival transmission of blood-borne pathogens can occur, and there are at least two cases of documented transmission of HIV via splashes," Dr. Joseph F. Sobanko said at the annual meeting of the American Academy of Dermatology. "Operating with exposed, nonintact skin also poses a risk of transmission of bloodborne pathogens."
Dr. Sobanko, a Mohs and reconstructive surgeon and director of dermatologic surgery education at the Hospital of the University of Pennsylvania, Philadelphia, emphasized that all health care employees are at risk of sharps injury. "Those physicians with the least experience are the most likely to receive an occupational exposure," he said. "When trainees and students receive injury, it is a risk factor for receiving future injuries, perhaps because of improper training early on."
A pilot study of sharps-related injuries in California health care facilities found that 49% occurred among nurses, followed by physicians (10%), phlebotomists (8%), and housekeeping and laundry personnel (7%), while the remainder occurred among a variety of other health care workers (Infect. Control Hosp. Epidemiol. 2003;24:113-21).
A separate survey study of needlestick injuries among 699 recent medical school graduates enrolled in a surgery residency at one of 17 medical centers in the United States found that 59% had a stick as a student, most commonly from suturing (42%), passing the needle (17%), and loading the needle (12%) (Academic Med. 2009;84:1815-21).
"Other studies have found that needlestick injuries commonly occur during device use and after device use during disposal," Dr. Sobanko noted.
Most occupational exposures are self-inflicted, and most sharps injuries tend to affect the left hand and digits, he continued. "When suturing, the injury that is self inflicted often happens on the nondominant hand," he said. "However, when not suturing but passing instruments (which shouldn’t be done), health care professionals are more likely to be injured on the dominant hand, because they accept the instrument with this hand. This is why ‘surgical neutral zones’ should be created to transfer instruments and eliminate this particular form of injury."
Occupational exposure is especially high in dermatology. One survey of 452 dermatologists queried in November of 2009 found a 90% injury rate (J. Am. Acad. Dermatol. 2011;65:648-50), while a separate, more recent survey of 336 dermatologists found an 85% injury rate 40% of the injuries had occurred within the year before the survey (Dermatol. Surg. 2013;39:1813-21). More than two-thirds of those same respondents (64%) reported having ever had a sharps injury that went unreported.
Procedures and behaviors that place dermatologists at highest risk for occupational exposure include drawing up solution, setting up a tray, injection, excision, biopsy, obtaining hemostasis, suturing, and disposal of sharps.
"Shortcuts, lack of focus, and improper training lead to avoidable accidents," Dr. Sobanko said. "Fostering a culture of safety can help reduce the risk of future injuries."
His recommended technique for uncapping a needle, for example, involves anchoring the top hand to the bottom hand, as in a golfer’s grip. Gentle extension releases the cap. His recommended technique for drawing solution involves resting the syringe on the hypothenar eminence of the left hand while holding the barrel with the thumb and index finger. This allows for safe placement of the bottle onto the needle. "This technique eliminates the risk of recoil injury if a cap is simply just pulled off a syringe at chest level, analogous to stretching a rubber band," he explained.
To avoid injuries while injecting, Dr. Sobanko advises ensuring that the hand or finger stabilizing the skin stays behind the path of the needle.
Dermatologists can keep themselves safe during office procedures by using protective sharps, eye protection, and gloves and by transferring instruments by implementing a neutral zone on the surgical tray. One review of seven studies of needle protective devices demonstrated an average 71% reduction in needlestick injuries (J. Hosp. Infect. 2003;53:237-42).
Dr. Sobanko described a safe needle device as one that is "easy to use and requires minimal effort to activate by the user. If activation is required, it must be a single-handed technique. The safety feature should click or be clear that it has activated, and the safety feature should remain protective throughout disposal."
Mental preparedness and motor repetition also play a role in protecting yourself. Dr. Sobanko’s five strategies for mental preparedness involve not rushing, knowing the pertinent anatomy for each case, having a proper tray set-up, having a proper preoperative plan, and not operating until an assistant is available.
Dr. Sobanko disclosed that he is a coeditor with Dr. Jacob Levitt of the forthcoming Springer book, "Atlas of Safe Practices in Office-Based Surgery."
DENVER – Of all the procedures and behaviors that place dermatologists at risk for occupational exposure, needlestick injuries rank at the top.
According to 1999 data from the National Institute for Occupational Safety and Health, one in five health care workers sustains a needlestick injury each year, putting them at risk for acquiring pathogens such as HIV and hepatitis B and C viruses. "Conjunctival transmission of blood-borne pathogens can occur, and there are at least two cases of documented transmission of HIV via splashes," Dr. Joseph F. Sobanko said at the annual meeting of the American Academy of Dermatology. "Operating with exposed, nonintact skin also poses a risk of transmission of bloodborne pathogens."
Dr. Sobanko, a Mohs and reconstructive surgeon and director of dermatologic surgery education at the Hospital of the University of Pennsylvania, Philadelphia, emphasized that all health care employees are at risk of sharps injury. "Those physicians with the least experience are the most likely to receive an occupational exposure," he said. "When trainees and students receive injury, it is a risk factor for receiving future injuries, perhaps because of improper training early on."
A pilot study of sharps-related injuries in California health care facilities found that 49% occurred among nurses, followed by physicians (10%), phlebotomists (8%), and housekeeping and laundry personnel (7%), while the remainder occurred among a variety of other health care workers (Infect. Control Hosp. Epidemiol. 2003;24:113-21).
A separate survey study of needlestick injuries among 699 recent medical school graduates enrolled in a surgery residency at one of 17 medical centers in the United States found that 59% had a stick as a student, most commonly from suturing (42%), passing the needle (17%), and loading the needle (12%) (Academic Med. 2009;84:1815-21).
"Other studies have found that needlestick injuries commonly occur during device use and after device use during disposal," Dr. Sobanko noted.
Most occupational exposures are self-inflicted, and most sharps injuries tend to affect the left hand and digits, he continued. "When suturing, the injury that is self inflicted often happens on the nondominant hand," he said. "However, when not suturing but passing instruments (which shouldn’t be done), health care professionals are more likely to be injured on the dominant hand, because they accept the instrument with this hand. This is why ‘surgical neutral zones’ should be created to transfer instruments and eliminate this particular form of injury."
Occupational exposure is especially high in dermatology. One survey of 452 dermatologists queried in November of 2009 found a 90% injury rate (J. Am. Acad. Dermatol. 2011;65:648-50), while a separate, more recent survey of 336 dermatologists found an 85% injury rate 40% of the injuries had occurred within the year before the survey (Dermatol. Surg. 2013;39:1813-21). More than two-thirds of those same respondents (64%) reported having ever had a sharps injury that went unreported.
Procedures and behaviors that place dermatologists at highest risk for occupational exposure include drawing up solution, setting up a tray, injection, excision, biopsy, obtaining hemostasis, suturing, and disposal of sharps.
"Shortcuts, lack of focus, and improper training lead to avoidable accidents," Dr. Sobanko said. "Fostering a culture of safety can help reduce the risk of future injuries."
His recommended technique for uncapping a needle, for example, involves anchoring the top hand to the bottom hand, as in a golfer’s grip. Gentle extension releases the cap. His recommended technique for drawing solution involves resting the syringe on the hypothenar eminence of the left hand while holding the barrel with the thumb and index finger. This allows for safe placement of the bottle onto the needle. "This technique eliminates the risk of recoil injury if a cap is simply just pulled off a syringe at chest level, analogous to stretching a rubber band," he explained.
To avoid injuries while injecting, Dr. Sobanko advises ensuring that the hand or finger stabilizing the skin stays behind the path of the needle.
Dermatologists can keep themselves safe during office procedures by using protective sharps, eye protection, and gloves and by transferring instruments by implementing a neutral zone on the surgical tray. One review of seven studies of needle protective devices demonstrated an average 71% reduction in needlestick injuries (J. Hosp. Infect. 2003;53:237-42).
Dr. Sobanko described a safe needle device as one that is "easy to use and requires minimal effort to activate by the user. If activation is required, it must be a single-handed technique. The safety feature should click or be clear that it has activated, and the safety feature should remain protective throughout disposal."
Mental preparedness and motor repetition also play a role in protecting yourself. Dr. Sobanko’s five strategies for mental preparedness involve not rushing, knowing the pertinent anatomy for each case, having a proper tray set-up, having a proper preoperative plan, and not operating until an assistant is available.
Dr. Sobanko disclosed that he is a coeditor with Dr. Jacob Levitt of the forthcoming Springer book, "Atlas of Safe Practices in Office-Based Surgery."
AT THE AAD ANNUAL MEETING
‘Culture of Safety’ best defense against sharps injury
DENVER – Of all the procedures and behaviors that place dermatologists at risk for occupational exposure, needlestick injuries rank at the top.
According to 1999 data from the National Institute for Occupational Safety and Health, one in five health care workers sustains a needlestick injury each year, putting them at risk for acquiring pathogens such as HIV and hepatitis B and C viruses. "Conjunctival transmission of blood-borne pathogens can occur, and there are at least two cases of documented transmission of HIV via splashes," Dr. Joseph F. Sobanko said at the annual meeting of the American Academy of Dermatology. "Operating with exposed, nonintact skin also poses a risk of transmission of bloodborne pathogens."
Dr. Sobanko, a Mohs and reconstructive surgeon and director of dermatologic surgery education at the Hospital of the University of Pennsylvania, Philadelphia, emphasized that all health care employees are at risk of sharps injury. "Those physicians with the least experience are the most likely to receive an occupational exposure," he said. "When trainees and students receive injury, it is a risk factor for receiving future injuries, perhaps because of improper training early on."
A pilot study of sharps-related injuries in California health care facilities found that 49% occurred among nurses, followed by physicians (10%), phlebotomists (8%), and housekeeping and laundry personnel (7%), while the remainder occurred among a variety of other health care workers (Infect. Control Hosp. Epidemiol. 2003;24:113-21).
A separate survey study of needlestick injuries among 699 recent medical school graduates enrolled in a surgery residency at one of 17 medical centers in the United States found that 59% had a stick as a student, most commonly from suturing (42%), passing the needle (17%), and loading the needle (12%) (Academic Med. 2009;84:1815-21).
"Other studies have found that needlestick injuries commonly occur during device use and after device use during disposal," Dr. Sobanko noted.
Most occupational exposures are self-inflicted, and most sharps injuries tend to affect the left hand and digits, he continued. "When suturing, the injury that is self inflicted often happens on the nondominant hand," he said. "However, when not suturing but passing instruments (which shouldn’t be done), health care professionals are more likely to be injured on the dominant hand, because they accept the instrument with this hand. This is why ‘surgical neutral zones’ should be created to transfer instruments and eliminate this particular form of injury."
Occupational exposure is especially high in dermatology. One survey of 452 dermatologists queried in November of 2009 found a 90% injury rate (J. Am. Acad. Dermatol. 2011;65:648-50), while a separate, more recent survey of 336 dermatologists found an 85% injury rate 40% of the injuries had occurred within the year before the survey (Dermatol. Surg. 2013;39:1813-21). More than two-thirds of those same respondents (64%) reported having ever had a sharps injury that went unreported.
Procedures and behaviors that place dermatologists at highest risk for occupational exposure include drawing up solution, setting up a tray, injection, excision, biopsy, obtaining hemostasis, suturing, and disposal of sharps.
"Shortcuts, lack of focus, and improper training lead to avoidable accidents," Dr. Sobanko said. "Fostering a culture of safety can help reduce the risk of future injuries."
His recommended technique for uncapping a needle, for example, involves anchoring the top hand to the bottom hand, as in a golfer’s grip. Gentle extension releases the cap. His recommended technique for drawing solution involves resting the syringe on the hypothenar eminence of the left hand while holding the barrel with the thumb and index finger. This allows for safe placement of the bottle onto the needle. "This technique eliminates the risk of recoil injury if a cap is simply just pulled off a syringe at chest level, analogous to stretching a rubber band," he explained.
To avoid injuries while injecting, Dr. Sobanko advises ensuring that the hand or finger stabilizing the skin stays behind the path of the needle.
Dermatologists can keep themselves safe during office procedures by using protective sharps, eye protection, and gloves and by transferring instruments by implementing a neutral zone on the surgical tray. One review of seven studies of needle protective devices demonstrated an average 71% reduction in needlestick injuries (J. Hosp. Infect. 2003;53:237-42).
Dr. Sobanko described a safe needle device as one that is "easy to use and requires minimal effort to activate by the user. If activation is required, it must be a single-handed technique. The safety feature should click or be clear that it has activated, and the safety feature should remain protective throughout disposal."
Mental preparedness and motor repetition also play a role in protecting yourself. Dr. Sobanko’s five strategies for mental preparedness involve not rushing, knowing the pertinent anatomy for each case, having a proper tray set-up, having a proper preoperative plan, and not operating until an assistant is available.
Dr. Sobanko disclosed that he is a coeditor with Dr. Jacob Levitt of the forthcoming Springer book, "Atlas of Safe Practices in Office-Based Surgery."
DENVER – Of all the procedures and behaviors that place dermatologists at risk for occupational exposure, needlestick injuries rank at the top.
According to 1999 data from the National Institute for Occupational Safety and Health, one in five health care workers sustains a needlestick injury each year, putting them at risk for acquiring pathogens such as HIV and hepatitis B and C viruses. "Conjunctival transmission of blood-borne pathogens can occur, and there are at least two cases of documented transmission of HIV via splashes," Dr. Joseph F. Sobanko said at the annual meeting of the American Academy of Dermatology. "Operating with exposed, nonintact skin also poses a risk of transmission of bloodborne pathogens."
Dr. Sobanko, a Mohs and reconstructive surgeon and director of dermatologic surgery education at the Hospital of the University of Pennsylvania, Philadelphia, emphasized that all health care employees are at risk of sharps injury. "Those physicians with the least experience are the most likely to receive an occupational exposure," he said. "When trainees and students receive injury, it is a risk factor for receiving future injuries, perhaps because of improper training early on."
A pilot study of sharps-related injuries in California health care facilities found that 49% occurred among nurses, followed by physicians (10%), phlebotomists (8%), and housekeeping and laundry personnel (7%), while the remainder occurred among a variety of other health care workers (Infect. Control Hosp. Epidemiol. 2003;24:113-21).
A separate survey study of needlestick injuries among 699 recent medical school graduates enrolled in a surgery residency at one of 17 medical centers in the United States found that 59% had a stick as a student, most commonly from suturing (42%), passing the needle (17%), and loading the needle (12%) (Academic Med. 2009;84:1815-21).
"Other studies have found that needlestick injuries commonly occur during device use and after device use during disposal," Dr. Sobanko noted.
Most occupational exposures are self-inflicted, and most sharps injuries tend to affect the left hand and digits, he continued. "When suturing, the injury that is self inflicted often happens on the nondominant hand," he said. "However, when not suturing but passing instruments (which shouldn’t be done), health care professionals are more likely to be injured on the dominant hand, because they accept the instrument with this hand. This is why ‘surgical neutral zones’ should be created to transfer instruments and eliminate this particular form of injury."
Occupational exposure is especially high in dermatology. One survey of 452 dermatologists queried in November of 2009 found a 90% injury rate (J. Am. Acad. Dermatol. 2011;65:648-50), while a separate, more recent survey of 336 dermatologists found an 85% injury rate 40% of the injuries had occurred within the year before the survey (Dermatol. Surg. 2013;39:1813-21). More than two-thirds of those same respondents (64%) reported having ever had a sharps injury that went unreported.
Procedures and behaviors that place dermatologists at highest risk for occupational exposure include drawing up solution, setting up a tray, injection, excision, biopsy, obtaining hemostasis, suturing, and disposal of sharps.
"Shortcuts, lack of focus, and improper training lead to avoidable accidents," Dr. Sobanko said. "Fostering a culture of safety can help reduce the risk of future injuries."
His recommended technique for uncapping a needle, for example, involves anchoring the top hand to the bottom hand, as in a golfer’s grip. Gentle extension releases the cap. His recommended technique for drawing solution involves resting the syringe on the hypothenar eminence of the left hand while holding the barrel with the thumb and index finger. This allows for safe placement of the bottle onto the needle. "This technique eliminates the risk of recoil injury if a cap is simply just pulled off a syringe at chest level, analogous to stretching a rubber band," he explained.
To avoid injuries while injecting, Dr. Sobanko advises ensuring that the hand or finger stabilizing the skin stays behind the path of the needle.
Dermatologists can keep themselves safe during office procedures by using protective sharps, eye protection, and gloves and by transferring instruments by implementing a neutral zone on the surgical tray. One review of seven studies of needle protective devices demonstrated an average 71% reduction in needlestick injuries (J. Hosp. Infect. 2003;53:237-42).
Dr. Sobanko described a safe needle device as one that is "easy to use and requires minimal effort to activate by the user. If activation is required, it must be a single-handed technique. The safety feature should click or be clear that it has activated, and the safety feature should remain protective throughout disposal."
Mental preparedness and motor repetition also play a role in protecting yourself. Dr. Sobanko’s five strategies for mental preparedness involve not rushing, knowing the pertinent anatomy for each case, having a proper tray set-up, having a proper preoperative plan, and not operating until an assistant is available.
Dr. Sobanko disclosed that he is a coeditor with Dr. Jacob Levitt of the forthcoming Springer book, "Atlas of Safe Practices in Office-Based Surgery."
DENVER – Of all the procedures and behaviors that place dermatologists at risk for occupational exposure, needlestick injuries rank at the top.
According to 1999 data from the National Institute for Occupational Safety and Health, one in five health care workers sustains a needlestick injury each year, putting them at risk for acquiring pathogens such as HIV and hepatitis B and C viruses. "Conjunctival transmission of blood-borne pathogens can occur, and there are at least two cases of documented transmission of HIV via splashes," Dr. Joseph F. Sobanko said at the annual meeting of the American Academy of Dermatology. "Operating with exposed, nonintact skin also poses a risk of transmission of bloodborne pathogens."
Dr. Sobanko, a Mohs and reconstructive surgeon and director of dermatologic surgery education at the Hospital of the University of Pennsylvania, Philadelphia, emphasized that all health care employees are at risk of sharps injury. "Those physicians with the least experience are the most likely to receive an occupational exposure," he said. "When trainees and students receive injury, it is a risk factor for receiving future injuries, perhaps because of improper training early on."
A pilot study of sharps-related injuries in California health care facilities found that 49% occurred among nurses, followed by physicians (10%), phlebotomists (8%), and housekeeping and laundry personnel (7%), while the remainder occurred among a variety of other health care workers (Infect. Control Hosp. Epidemiol. 2003;24:113-21).
A separate survey study of needlestick injuries among 699 recent medical school graduates enrolled in a surgery residency at one of 17 medical centers in the United States found that 59% had a stick as a student, most commonly from suturing (42%), passing the needle (17%), and loading the needle (12%) (Academic Med. 2009;84:1815-21).
"Other studies have found that needlestick injuries commonly occur during device use and after device use during disposal," Dr. Sobanko noted.
Most occupational exposures are self-inflicted, and most sharps injuries tend to affect the left hand and digits, he continued. "When suturing, the injury that is self inflicted often happens on the nondominant hand," he said. "However, when not suturing but passing instruments (which shouldn’t be done), health care professionals are more likely to be injured on the dominant hand, because they accept the instrument with this hand. This is why ‘surgical neutral zones’ should be created to transfer instruments and eliminate this particular form of injury."
Occupational exposure is especially high in dermatology. One survey of 452 dermatologists queried in November of 2009 found a 90% injury rate (J. Am. Acad. Dermatol. 2011;65:648-50), while a separate, more recent survey of 336 dermatologists found an 85% injury rate 40% of the injuries had occurred within the year before the survey (Dermatol. Surg. 2013;39:1813-21). More than two-thirds of those same respondents (64%) reported having ever had a sharps injury that went unreported.
Procedures and behaviors that place dermatologists at highest risk for occupational exposure include drawing up solution, setting up a tray, injection, excision, biopsy, obtaining hemostasis, suturing, and disposal of sharps.
"Shortcuts, lack of focus, and improper training lead to avoidable accidents," Dr. Sobanko said. "Fostering a culture of safety can help reduce the risk of future injuries."
His recommended technique for uncapping a needle, for example, involves anchoring the top hand to the bottom hand, as in a golfer’s grip. Gentle extension releases the cap. His recommended technique for drawing solution involves resting the syringe on the hypothenar eminence of the left hand while holding the barrel with the thumb and index finger. This allows for safe placement of the bottle onto the needle. "This technique eliminates the risk of recoil injury if a cap is simply just pulled off a syringe at chest level, analogous to stretching a rubber band," he explained.
To avoid injuries while injecting, Dr. Sobanko advises ensuring that the hand or finger stabilizing the skin stays behind the path of the needle.
Dermatologists can keep themselves safe during office procedures by using protective sharps, eye protection, and gloves and by transferring instruments by implementing a neutral zone on the surgical tray. One review of seven studies of needle protective devices demonstrated an average 71% reduction in needlestick injuries (J. Hosp. Infect. 2003;53:237-42).
Dr. Sobanko described a safe needle device as one that is "easy to use and requires minimal effort to activate by the user. If activation is required, it must be a single-handed technique. The safety feature should click or be clear that it has activated, and the safety feature should remain protective throughout disposal."
Mental preparedness and motor repetition also play a role in protecting yourself. Dr. Sobanko’s five strategies for mental preparedness involve not rushing, knowing the pertinent anatomy for each case, having a proper tray set-up, having a proper preoperative plan, and not operating until an assistant is available.
Dr. Sobanko disclosed that he is a coeditor with Dr. Jacob Levitt of the forthcoming Springer book, "Atlas of Safe Practices in Office-Based Surgery."
AT THE AAD ANNUAL MEETING
Dr. Henry W. Lim previews AAD 2014
DENVER – As the annual meeting of the American Academy of Dermatology kicks off, we asked the meeting’s Scientific Assembly chair, Dr. Henry W. Lim, to give us an overview.
Dr. Lim, professor and chairman of dermatology at Henry Ford Hospital in Detroit, speaks about hot clinical topics, types of sessions, and important policy issues addressed during the meeting.
On Twitter @NaseemMiller
DENVER – As the annual meeting of the American Academy of Dermatology kicks off, we asked the meeting’s Scientific Assembly chair, Dr. Henry W. Lim, to give us an overview.
Dr. Lim, professor and chairman of dermatology at Henry Ford Hospital in Detroit, speaks about hot clinical topics, types of sessions, and important policy issues addressed during the meeting.
On Twitter @NaseemMiller
DENVER – As the annual meeting of the American Academy of Dermatology kicks off, we asked the meeting’s Scientific Assembly chair, Dr. Henry W. Lim, to give us an overview.
Dr. Lim, professor and chairman of dermatology at Henry Ford Hospital in Detroit, speaks about hot clinical topics, types of sessions, and important policy issues addressed during the meeting.
On Twitter @NaseemMiller
AT THE AAD ANNUAL MEETING
Show off your social media skills in AAD’s selfie photo contest
Social media take center stage at this year’s American Academy of Dermatology annual meeting, as the AAD offers its first Twitter "selfie" photo contest. The winner will receive a $50 Starbucks gift card; how’s that for an incentive?
To enter, you (or a friend) need to have a Twitter account. Send your best selfie (it can be one person, two people, or a group shot) of you and your friends enjoying the meeting. Note: Photos may be taken in or around the convention center, or out and about in Denver, but no photos may be taken from inside the meeting session rooms.
Once you’re on Twitter, tweet your best selfie to @AADMtgs, and be sure to use the hashtag #aad14.
The contest kicks off on Friday, March 21, at noon (Mountain Standard Time), and ends on Tuesday, March 25, at noon (MST). A panel will review the photos, and the winner will be notified by noon on Friday, March 28 (Central Standard Time). Gift cards will be mailed or e-mailed. More information is available at the AAD’s website, aad.org.
While you’re tweeting your selfies, keep up with the latest news and development from the meeting by following @sknews, as well as our intrepid reporter, Naseem Miller (@naseemmiller).
On Twitter @hsplete
Social media take center stage at this year’s American Academy of Dermatology annual meeting, as the AAD offers its first Twitter "selfie" photo contest. The winner will receive a $50 Starbucks gift card; how’s that for an incentive?
To enter, you (or a friend) need to have a Twitter account. Send your best selfie (it can be one person, two people, or a group shot) of you and your friends enjoying the meeting. Note: Photos may be taken in or around the convention center, or out and about in Denver, but no photos may be taken from inside the meeting session rooms.
Once you’re on Twitter, tweet your best selfie to @AADMtgs, and be sure to use the hashtag #aad14.
The contest kicks off on Friday, March 21, at noon (Mountain Standard Time), and ends on Tuesday, March 25, at noon (MST). A panel will review the photos, and the winner will be notified by noon on Friday, March 28 (Central Standard Time). Gift cards will be mailed or e-mailed. More information is available at the AAD’s website, aad.org.
While you’re tweeting your selfies, keep up with the latest news and development from the meeting by following @sknews, as well as our intrepid reporter, Naseem Miller (@naseemmiller).
On Twitter @hsplete
Social media take center stage at this year’s American Academy of Dermatology annual meeting, as the AAD offers its first Twitter "selfie" photo contest. The winner will receive a $50 Starbucks gift card; how’s that for an incentive?
To enter, you (or a friend) need to have a Twitter account. Send your best selfie (it can be one person, two people, or a group shot) of you and your friends enjoying the meeting. Note: Photos may be taken in or around the convention center, or out and about in Denver, but no photos may be taken from inside the meeting session rooms.
Once you’re on Twitter, tweet your best selfie to @AADMtgs, and be sure to use the hashtag #aad14.
The contest kicks off on Friday, March 21, at noon (Mountain Standard Time), and ends on Tuesday, March 25, at noon (MST). A panel will review the photos, and the winner will be notified by noon on Friday, March 28 (Central Standard Time). Gift cards will be mailed or e-mailed. More information is available at the AAD’s website, aad.org.
While you’re tweeting your selfies, keep up with the latest news and development from the meeting by following @sknews, as well as our intrepid reporter, Naseem Miller (@naseemmiller).
On Twitter @hsplete