User login
Dark Blue Facial Lesion Worries Mother of Young Boy
ANSWER
The correct answer is pilomatricoma (choice “a”), also know as calcifying epithelioma of Malherbe. See discussion.
Dermatofibromas (choice “b”) can be dark, especially in darker-skinned individuals, but are rare in children and even more so on the face.
Sebaceous cysts (choice “c”) are quite common on the face and can develop in children but are more likely to have a fluctuant feel rather than a firm one. They are also unlikely to be hyperpigmented and will usually involve an overlying punctum (comedone) on the surface.
Spitz tumors (choice “d”) can range from red to black and papular to macular. They tend to be intradermal in terms of vertical placement and are quite unlikely to be subcutaneous and indurated. They belong in the differential diagnosis because of their color and the fact that they are usually seen on children.
DISCUSSION
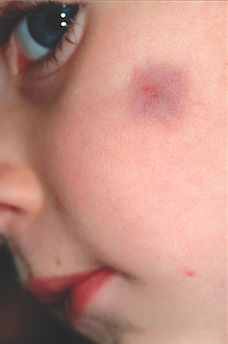
Pilomatricomas are uncommon but not at all rare. They usually manifest on the head, neck, or upper extremities of children as bluish subcutaneous masses devoid of overlying skin changes (eg, atrophy, comedones, or breaks in the skin). Though not seen in this case, the deep lesion often “tents” the overlying skin in one or more foci, a phenomenon termed the tent sign.
Although the exact reason they appear is not known, it is clear that they derive histologically from hair matrix cells. Quite rarely, they can undergo malignant transformation. They can also be quite a bit larger than this one and can present in multiples, with color ranging from deep blue (as in this case) to pinkish brown.
TREATMENT
For the purposes of positive identification and cosmesis, pilomatricomas are usually excised. At that time, identifying features such as the lack of an organized cyst wall and the granular, calcified contents are typically seen.
ANSWER
The correct answer is pilomatricoma (choice “a”), also know as calcifying epithelioma of Malherbe. See discussion.
Dermatofibromas (choice “b”) can be dark, especially in darker-skinned individuals, but are rare in children and even more so on the face.
Sebaceous cysts (choice “c”) are quite common on the face and can develop in children but are more likely to have a fluctuant feel rather than a firm one. They are also unlikely to be hyperpigmented and will usually involve an overlying punctum (comedone) on the surface.
Spitz tumors (choice “d”) can range from red to black and papular to macular. They tend to be intradermal in terms of vertical placement and are quite unlikely to be subcutaneous and indurated. They belong in the differential diagnosis because of their color and the fact that they are usually seen on children.
DISCUSSION
Pilomatricomas are uncommon but not at all rare. They usually manifest on the head, neck, or upper extremities of children as bluish subcutaneous masses devoid of overlying skin changes (eg, atrophy, comedones, or breaks in the skin). Though not seen in this case, the deep lesion often “tents” the overlying skin in one or more foci, a phenomenon termed the tent sign.
Although the exact reason they appear is not known, it is clear that they derive histologically from hair matrix cells. Quite rarely, they can undergo malignant transformation. They can also be quite a bit larger than this one and can present in multiples, with color ranging from deep blue (as in this case) to pinkish brown.
TREATMENT
For the purposes of positive identification and cosmesis, pilomatricomas are usually excised. At that time, identifying features such as the lack of an organized cyst wall and the granular, calcified contents are typically seen.
ANSWER
The correct answer is pilomatricoma (choice “a”), also know as calcifying epithelioma of Malherbe. See discussion.
Dermatofibromas (choice “b”) can be dark, especially in darker-skinned individuals, but are rare in children and even more so on the face.
Sebaceous cysts (choice “c”) are quite common on the face and can develop in children but are more likely to have a fluctuant feel rather than a firm one. They are also unlikely to be hyperpigmented and will usually involve an overlying punctum (comedone) on the surface.
Spitz tumors (choice “d”) can range from red to black and papular to macular. They tend to be intradermal in terms of vertical placement and are quite unlikely to be subcutaneous and indurated. They belong in the differential diagnosis because of their color and the fact that they are usually seen on children.
DISCUSSION
Pilomatricomas are uncommon but not at all rare. They usually manifest on the head, neck, or upper extremities of children as bluish subcutaneous masses devoid of overlying skin changes (eg, atrophy, comedones, or breaks in the skin). Though not seen in this case, the deep lesion often “tents” the overlying skin in one or more foci, a phenomenon termed the tent sign.
Although the exact reason they appear is not known, it is clear that they derive histologically from hair matrix cells. Quite rarely, they can undergo malignant transformation. They can also be quite a bit larger than this one and can present in multiples, with color ranging from deep blue (as in this case) to pinkish brown.
TREATMENT
For the purposes of positive identification and cosmesis, pilomatricomas are usually excised. At that time, identifying features such as the lack of an organized cyst wall and the granular, calcified contents are typically seen.
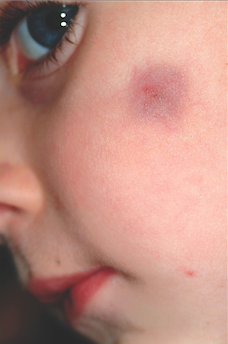
A 6-year-old boy is brought in by his mother for evaluation of a lesion that has been present on his face, with little change, for about two years. Though asymptomatic, the lesion is nonetheless worrisome, since the boy’s pediatrician isn’t sure what it is. The boy is in good health otherwise. His mother’s expectation is that the lesion will be removed at this initial visit to dermatology, since this is the reason she consulted the pediatrician in the first place. The 2-cm left facial lesion can be seen from across the room; it is quite large, round, and dark blue. While no changes are seen on the surface of the skin, palpation reveals definite, deep induration. No punctum can be seen on the overlying surface, and there is no palpable adenopathy in the area.
What Is This Long-Standing Loss of Pigment?
ANSWER
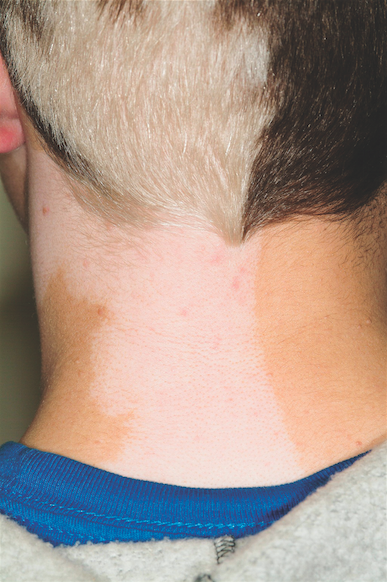
The correct answer is poliosis (choice “d”), which has been described as a reliable indicator of tuberous sclerosis when seen early in life.1 Poliosis is the specific term for focal loss of color in scalp hair. Technically, this process is a form of hypomelanosis (choice “b”), although the latter is a more generic term used to refer to loss of pigment in any area. Graying (choice “a”) usually refers to uniform loss of hair color all over the scalp—albeit with focal accentuation over the temples, as opposed to the sharply demarcated areas of complete color loss seen in poliosis. Poliosis can be seen as a feature of vitiligo (choice “c”), but the latter usually also involves pigment loss elsewhere.
DISCUSSION/TREATMENT
Poliosis, which is often idiopathic, can be seen in a number of conditions besides tuberous sclerosis and vitiligo, including halo nevi of the scalp, alopecia areata (as hair regrows), and Waardenburg’s syndrome. As mentioned above, it can appear early in life as an indicator of tuberous sclerosis, particularly when coupled with involvement of adjacent dermatomal skin. This was likely the case with this patient. No permanent treatment exists for this problem.
REFERENCE
1. Apibal Y, Reakatanan W, Chunharas A. Poliosis as the first clue of tuberous sclerosis. Pediatr Dermatol. 2008;25(4):486-487.
ANSWER
The correct answer is poliosis (choice “d”), which has been described as a reliable indicator of tuberous sclerosis when seen early in life.1 Poliosis is the specific term for focal loss of color in scalp hair. Technically, this process is a form of hypomelanosis (choice “b”), although the latter is a more generic term used to refer to loss of pigment in any area. Graying (choice “a”) usually refers to uniform loss of hair color all over the scalp—albeit with focal accentuation over the temples, as opposed to the sharply demarcated areas of complete color loss seen in poliosis. Poliosis can be seen as a feature of vitiligo (choice “c”), but the latter usually also involves pigment loss elsewhere.
DISCUSSION/TREATMENT
Poliosis, which is often idiopathic, can be seen in a number of conditions besides tuberous sclerosis and vitiligo, including halo nevi of the scalp, alopecia areata (as hair regrows), and Waardenburg’s syndrome. As mentioned above, it can appear early in life as an indicator of tuberous sclerosis, particularly when coupled with involvement of adjacent dermatomal skin. This was likely the case with this patient. No permanent treatment exists for this problem.
REFERENCE
1. Apibal Y, Reakatanan W, Chunharas A. Poliosis as the first clue of tuberous sclerosis. Pediatr Dermatol. 2008;25(4):486-487.
ANSWER
The correct answer is poliosis (choice “d”), which has been described as a reliable indicator of tuberous sclerosis when seen early in life.1 Poliosis is the specific term for focal loss of color in scalp hair. Technically, this process is a form of hypomelanosis (choice “b”), although the latter is a more generic term used to refer to loss of pigment in any area. Graying (choice “a”) usually refers to uniform loss of hair color all over the scalp—albeit with focal accentuation over the temples, as opposed to the sharply demarcated areas of complete color loss seen in poliosis. Poliosis can be seen as a feature of vitiligo (choice “c”), but the latter usually also involves pigment loss elsewhere.
DISCUSSION/TREATMENT
Poliosis, which is often idiopathic, can be seen in a number of conditions besides tuberous sclerosis and vitiligo, including halo nevi of the scalp, alopecia areata (as hair regrows), and Waardenburg’s syndrome. As mentioned above, it can appear early in life as an indicator of tuberous sclerosis, particularly when coupled with involvement of adjacent dermatomal skin. This was likely the case with this patient. No permanent treatment exists for this problem.
REFERENCE
1. Apibal Y, Reakatanan W, Chunharas A. Poliosis as the first clue of tuberous sclerosis. Pediatr Dermatol. 2008;25(4):486-487.

A 14-year-old boy presents for evaluation of a long-standing condition involving loss of pigment of the hair and the adjacent neck skin. This discoloration has been present since shortly after his birth. The patient is specifically interested in treatment options. His history includes a diagnosis of tuberous sclerosis, which he received at an early age. On examination, you note a complete loss of pigment in the posterior scalp on the patient’s left side, along with total loss of color in the skin on the adjacent part of the neck. The medial margins of both stop abruptly at midline. Additional inspection reveals several other abnormalities, including dart-shaped hypopigmented macules on the patient’s trunk, fleshy 1- to 3-mm papules clustered about the midface, and periungual fibromatous papules around several toenails.
Skin Changes on Hands Lead to Daily Living Problems
ANSWER
Although this woman may end up having to see all of these specialists, she first needs confirmation of the suspected diagnosis: CREST syndrome, considered a variant of systemic sclerosis (aka scleroderma) and a condition marked by sclerotic transformation of virtually all the organs in and on the body. For more on this condition, see below.
The definitive diagnosis and expert management of this condition are generally considered the province of the rheumatologist, so choice “d” is the correct answer. Any of the other specialists, who often become involved in such cases early on, could likely identify this condition but would defer to rheumatology for definitive diagnosis and management.
DISCUSSION/TREATMENT
Systemic sclerosis (SSc) patients, like those with other rare conditions with protean manifestations, often go through long periods in which they see various specialists for each subset of symptoms—with a delay in arriving at a definitive, unifying diagnosis. This is a good example of the role played in such cases by dermatology, which is often able to “connect the dots” in patients with disparate complaints. Biopsy in such patients, for example, will show increased collagen deposition (among other changes), leading to heightened suspicion and confirmation by specific blood tests and expert clinical corroboration.
SSc affects approximately two million to 10 million people, almost four times as many women as men, and very few Asian patients. There are several variants of the condition, including cases of CREST in which skin changes are limited to the hands and face for decades before internal organs begin to be affected (if ever).
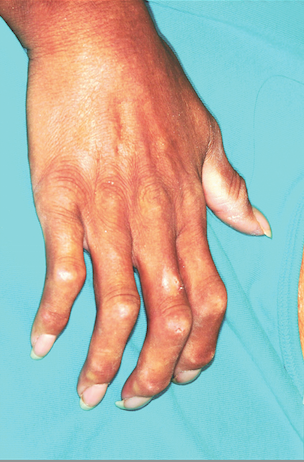
The CREST acronym stands for calcinosis (the scaly foci on our patient’s fingers), Raynaud’s phenomenon, esophageal dysmotility (due to collagen infiltration), sclerodactyly (sclerosis of finger skin), and telangiectasias (often on face and chest). CREST often starts, as in this case, with chronic edema of the hands, which gives way eventually to sclerodactyly and often to reabsorption of the bony tufts on distal digits. Dyschromia, particularly of the hands (as in this patient), is another common finding. SSc can also present with generalized pruritus.
SSc has a poor prognosis, progressing steadily as it begins to affect the lungs, liver, kidneys, and joints. Despite treatment, death may occur (most commonly from renal or respiratory failure).
ANSWER
Although this woman may end up having to see all of these specialists, she first needs confirmation of the suspected diagnosis: CREST syndrome, considered a variant of systemic sclerosis (aka scleroderma) and a condition marked by sclerotic transformation of virtually all the organs in and on the body. For more on this condition, see below.
The definitive diagnosis and expert management of this condition are generally considered the province of the rheumatologist, so choice “d” is the correct answer. Any of the other specialists, who often become involved in such cases early on, could likely identify this condition but would defer to rheumatology for definitive diagnosis and management.
DISCUSSION/TREATMENT
Systemic sclerosis (SSc) patients, like those with other rare conditions with protean manifestations, often go through long periods in which they see various specialists for each subset of symptoms—with a delay in arriving at a definitive, unifying diagnosis. This is a good example of the role played in such cases by dermatology, which is often able to “connect the dots” in patients with disparate complaints. Biopsy in such patients, for example, will show increased collagen deposition (among other changes), leading to heightened suspicion and confirmation by specific blood tests and expert clinical corroboration.
SSc affects approximately two million to 10 million people, almost four times as many women as men, and very few Asian patients. There are several variants of the condition, including cases of CREST in which skin changes are limited to the hands and face for decades before internal organs begin to be affected (if ever).
The CREST acronym stands for calcinosis (the scaly foci on our patient’s fingers), Raynaud’s phenomenon, esophageal dysmotility (due to collagen infiltration), sclerodactyly (sclerosis of finger skin), and telangiectasias (often on face and chest). CREST often starts, as in this case, with chronic edema of the hands, which gives way eventually to sclerodactyly and often to reabsorption of the bony tufts on distal digits. Dyschromia, particularly of the hands (as in this patient), is another common finding. SSc can also present with generalized pruritus.
SSc has a poor prognosis, progressing steadily as it begins to affect the lungs, liver, kidneys, and joints. Despite treatment, death may occur (most commonly from renal or respiratory failure).
ANSWER
Although this woman may end up having to see all of these specialists, she first needs confirmation of the suspected diagnosis: CREST syndrome, considered a variant of systemic sclerosis (aka scleroderma) and a condition marked by sclerotic transformation of virtually all the organs in and on the body. For more on this condition, see below.
The definitive diagnosis and expert management of this condition are generally considered the province of the rheumatologist, so choice “d” is the correct answer. Any of the other specialists, who often become involved in such cases early on, could likely identify this condition but would defer to rheumatology for definitive diagnosis and management.
DISCUSSION/TREATMENT
Systemic sclerosis (SSc) patients, like those with other rare conditions with protean manifestations, often go through long periods in which they see various specialists for each subset of symptoms—with a delay in arriving at a definitive, unifying diagnosis. This is a good example of the role played in such cases by dermatology, which is often able to “connect the dots” in patients with disparate complaints. Biopsy in such patients, for example, will show increased collagen deposition (among other changes), leading to heightened suspicion and confirmation by specific blood tests and expert clinical corroboration.
SSc affects approximately two million to 10 million people, almost four times as many women as men, and very few Asian patients. There are several variants of the condition, including cases of CREST in which skin changes are limited to the hands and face for decades before internal organs begin to be affected (if ever).
The CREST acronym stands for calcinosis (the scaly foci on our patient’s fingers), Raynaud’s phenomenon, esophageal dysmotility (due to collagen infiltration), sclerodactyly (sclerosis of finger skin), and telangiectasias (often on face and chest). CREST often starts, as in this case, with chronic edema of the hands, which gives way eventually to sclerodactyly and often to reabsorption of the bony tufts on distal digits. Dyschromia, particularly of the hands (as in this patient), is another common finding. SSc can also present with generalized pruritus.
SSc has a poor prognosis, progressing steadily as it begins to affect the lungs, liver, kidneys, and joints. Despite treatment, death may occur (most commonly from renal or respiratory failure).

A 54-year-old woman presents with changes to the skin on her hands. These began several years ago and have progressed to the point that it is becoming harder and harder for her to use her hands in normal activities of daily living. Several years ago, when the problems began, the first thing the patient noted was bilateral edema. This symptom was always at its worst when the patient woke up and got better as the day went on. It has gradually subsided, giving way to the slow advance of skin hardening on all her fingers. She has also developed a claw-like incurving of the fingers and occasional “ulcers” on the fingertips. Exposure to modest cold turns her fingers quite cold and white. More history taking reveals that during this time, she also began to experience fatigue, shortness of breath, and difficulty swallowing. On examination, the skin on all her fingers is uniformly tight and hard, the tips are all tapered and slender, and all the fingers are firmly fixed in a moderately flexed position. Dermatoscopic exam shows tortuous, dilated capillaries in the cuticular areas of all fingers. Several papulosquamous shallow erosions are seen on the phalanges, ranging in diameter from a pinpoint to 1.0 cm. Groups of telangiectasias are noted on the upper chest and lateral face.
Two Different Diagnoses, But One Location
ANSWER
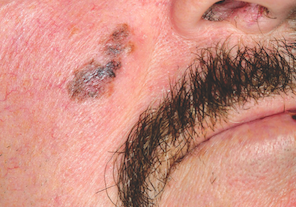
The white, round spots seen in this lesion were entirely consistent with SK and were not misinterpreted (choice “a”). Since melanoma is not known to display this type of spot, choice “b” is also incorrect. Biopsy reports are occasionally wrong, of course, but the diagnosis of melanoma is fraught with such serious implications that the call is not made if specific criteria are not met. These include specific stains for that diagnosis, histologic findings, and the concurrence of multiple observers, so it is unlikely that the histologic diagnosis is incorrect (choice “d”).
This leaves the correct answer, choice “c,” discussed below.
DISCUSSION
There is truly no law saying that two lesions can’t appear in the same location—and as this case illustrates, it definitely happens. Had we performed additional biopsies, no doubt features of SK would have been seen in corroboration of the dermatoscopic findings.
This case also emphasizes another useful principle: Pay just as much attention to the owner as to the lesion itself. This patient was quite fair and sun-damaged, so any odd lesion he developed would be suspect, let alone one that looked like this.
One final thing to be learned from this case is that as useful as dermatoscopes can be, they still must take a backseat to common sense.
ANSWER
The white, round spots seen in this lesion were entirely consistent with SK and were not misinterpreted (choice “a”). Since melanoma is not known to display this type of spot, choice “b” is also incorrect. Biopsy reports are occasionally wrong, of course, but the diagnosis of melanoma is fraught with such serious implications that the call is not made if specific criteria are not met. These include specific stains for that diagnosis, histologic findings, and the concurrence of multiple observers, so it is unlikely that the histologic diagnosis is incorrect (choice “d”).
This leaves the correct answer, choice “c,” discussed below.
DISCUSSION
There is truly no law saying that two lesions can’t appear in the same location—and as this case illustrates, it definitely happens. Had we performed additional biopsies, no doubt features of SK would have been seen in corroboration of the dermatoscopic findings.
This case also emphasizes another useful principle: Pay just as much attention to the owner as to the lesion itself. This patient was quite fair and sun-damaged, so any odd lesion he developed would be suspect, let alone one that looked like this.
One final thing to be learned from this case is that as useful as dermatoscopes can be, they still must take a backseat to common sense.
ANSWER
The white, round spots seen in this lesion were entirely consistent with SK and were not misinterpreted (choice “a”). Since melanoma is not known to display this type of spot, choice “b” is also incorrect. Biopsy reports are occasionally wrong, of course, but the diagnosis of melanoma is fraught with such serious implications that the call is not made if specific criteria are not met. These include specific stains for that diagnosis, histologic findings, and the concurrence of multiple observers, so it is unlikely that the histologic diagnosis is incorrect (choice “d”).
This leaves the correct answer, choice “c,” discussed below.
DISCUSSION
There is truly no law saying that two lesions can’t appear in the same location—and as this case illustrates, it definitely happens. Had we performed additional biopsies, no doubt features of SK would have been seen in corroboration of the dermatoscopic findings.
This case also emphasizes another useful principle: Pay just as much attention to the owner as to the lesion itself. This patient was quite fair and sun-damaged, so any odd lesion he developed would be suspect, let alone one that looked like this.
One final thing to be learned from this case is that as useful as dermatoscopes can be, they still must take a backseat to common sense.
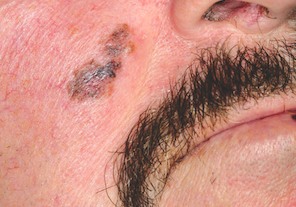
A 57-year-old man self-refers for evaluation of a facial lesion that has been present for several years. As the lesion slowly grew larger, family members became worried and urged him to seek treatment. The man has spent many years in the sun during his adult life, both at work and when engaging in various hobbies, and he burns easily and often. In addition, 20 years ago, he was diagnosed with psoriasis, which was eventually treated with a year’s worth of phototherapy. History also includes a coronary artery bypass graft (undergone 10 years ago) and current smoker status. On examination, the facial lesion proves to be macular, with ominously irregular colors of black and brown, along with ragged borders. The overall size is almost 4 × 2 cm. The lesion is seen in the context of very fair, sun-damaged skin, characterized by widespread actinic keratoses and telangiectasias. Through use of a dermatoscope (a power-viewing instrument that provides 10× magnification, used to examine suspicious lesions for specific changes suggestive of cancer), definite signs of seborrheic keratosis (SK; pseudocysts) are seen. Nonetheless, the overall appearance of the lesion—as well as the patient’s high-risk status—dictates that a punch biopsy be performed. The subsequent report reveals the lesion to be a Clark’s level II superficial melanoma, Breslow 0.6 mm.
If it’s not acne, warts, or molluscum contagiosum, what is this condition?
ANSWER
All of the above choices are correct and, in fact, were seen on this patient. These findings served to confirm the diagnosis of tuberous sclerosis.
DISCUSSION
Also called Bourneville’s disease or epiloia (an acronym for epilepsy, low intelligence, and adenoma sebaceum—all major findings in this disease), tuberous sclerosis (TS) occurs in one of 10,000 births and affects both genders equally. It is considered a genodermatosis, with 75% of cases related to spontaneous mutations and 25% to autosomal dominant transmission. Two separate genes have been identified.
The earliest skin finding in these patients is that of hypopigmented macules, especially the so-called mountain ash leaf spots typically seen on the trunk and extremities—better observed sometimes with the aid of a Wood’s lamp.
Another common early finding is that of seizures, occurring in 75% of TS patients with central nervous system lesions. Facial angiofibromas, called adenoma sebaceum, also appear in early childhood, increase during adolescence, and are permanent. About 80% of affected patients will eventually develop the connective tissue nevus called shagreen patch, which usually occurs on the low back.
Conical smooth papular projections originating from the nail folds of fingers and toes appear at puberty in a high percentage of TS patients and are permanent. Redundant and sometimes papular lesions are seen in the gingival mucosa. Numerous other signs of the disease—in lungs, heart, and bony tissue—have been described.
The acronym mentioned above, epiloia, has been largely abandoned, in part because it suggests that low intelligence with TS patients is inevitable. The truth is, many patients, such as this one, function quite normally, typifying the variable penetrance of the genetic changes so common to TS.
TREATMENT
The main focus for this patient is to get his seizures under control and arrange for proper follow-up, as well as genetic counseling. Unfortunately, there is no effective treatment for the facial lesions.
ANSWER
All of the above choices are correct and, in fact, were seen on this patient. These findings served to confirm the diagnosis of tuberous sclerosis.
DISCUSSION
Also called Bourneville’s disease or epiloia (an acronym for epilepsy, low intelligence, and adenoma sebaceum—all major findings in this disease), tuberous sclerosis (TS) occurs in one of 10,000 births and affects both genders equally. It is considered a genodermatosis, with 75% of cases related to spontaneous mutations and 25% to autosomal dominant transmission. Two separate genes have been identified.
The earliest skin finding in these patients is that of hypopigmented macules, especially the so-called mountain ash leaf spots typically seen on the trunk and extremities—better observed sometimes with the aid of a Wood’s lamp.
Another common early finding is that of seizures, occurring in 75% of TS patients with central nervous system lesions. Facial angiofibromas, called adenoma sebaceum, also appear in early childhood, increase during adolescence, and are permanent. About 80% of affected patients will eventually develop the connective tissue nevus called shagreen patch, which usually occurs on the low back.
Conical smooth papular projections originating from the nail folds of fingers and toes appear at puberty in a high percentage of TS patients and are permanent. Redundant and sometimes papular lesions are seen in the gingival mucosa. Numerous other signs of the disease—in lungs, heart, and bony tissue—have been described.
The acronym mentioned above, epiloia, has been largely abandoned, in part because it suggests that low intelligence with TS patients is inevitable. The truth is, many patients, such as this one, function quite normally, typifying the variable penetrance of the genetic changes so common to TS.
TREATMENT
The main focus for this patient is to get his seizures under control and arrange for proper follow-up, as well as genetic counseling. Unfortunately, there is no effective treatment for the facial lesions.
ANSWER
All of the above choices are correct and, in fact, were seen on this patient. These findings served to confirm the diagnosis of tuberous sclerosis.
DISCUSSION
Also called Bourneville’s disease or epiloia (an acronym for epilepsy, low intelligence, and adenoma sebaceum—all major findings in this disease), tuberous sclerosis (TS) occurs in one of 10,000 births and affects both genders equally. It is considered a genodermatosis, with 75% of cases related to spontaneous mutations and 25% to autosomal dominant transmission. Two separate genes have been identified.
The earliest skin finding in these patients is that of hypopigmented macules, especially the so-called mountain ash leaf spots typically seen on the trunk and extremities—better observed sometimes with the aid of a Wood’s lamp.
Another common early finding is that of seizures, occurring in 75% of TS patients with central nervous system lesions. Facial angiofibromas, called adenoma sebaceum, also appear in early childhood, increase during adolescence, and are permanent. About 80% of affected patients will eventually develop the connective tissue nevus called shagreen patch, which usually occurs on the low back.
Conical smooth papular projections originating from the nail folds of fingers and toes appear at puberty in a high percentage of TS patients and are permanent. Redundant and sometimes papular lesions are seen in the gingival mucosa. Numerous other signs of the disease—in lungs, heart, and bony tissue—have been described.
The acronym mentioned above, epiloia, has been largely abandoned, in part because it suggests that low intelligence with TS patients is inevitable. The truth is, many patients, such as this one, function quite normally, typifying the variable penetrance of the genetic changes so common to TS.
TREATMENT
The main focus for this patient is to get his seizures under control and arrange for proper follow-up, as well as genetic counseling. Unfortunately, there is no effective treatment for the facial lesions.
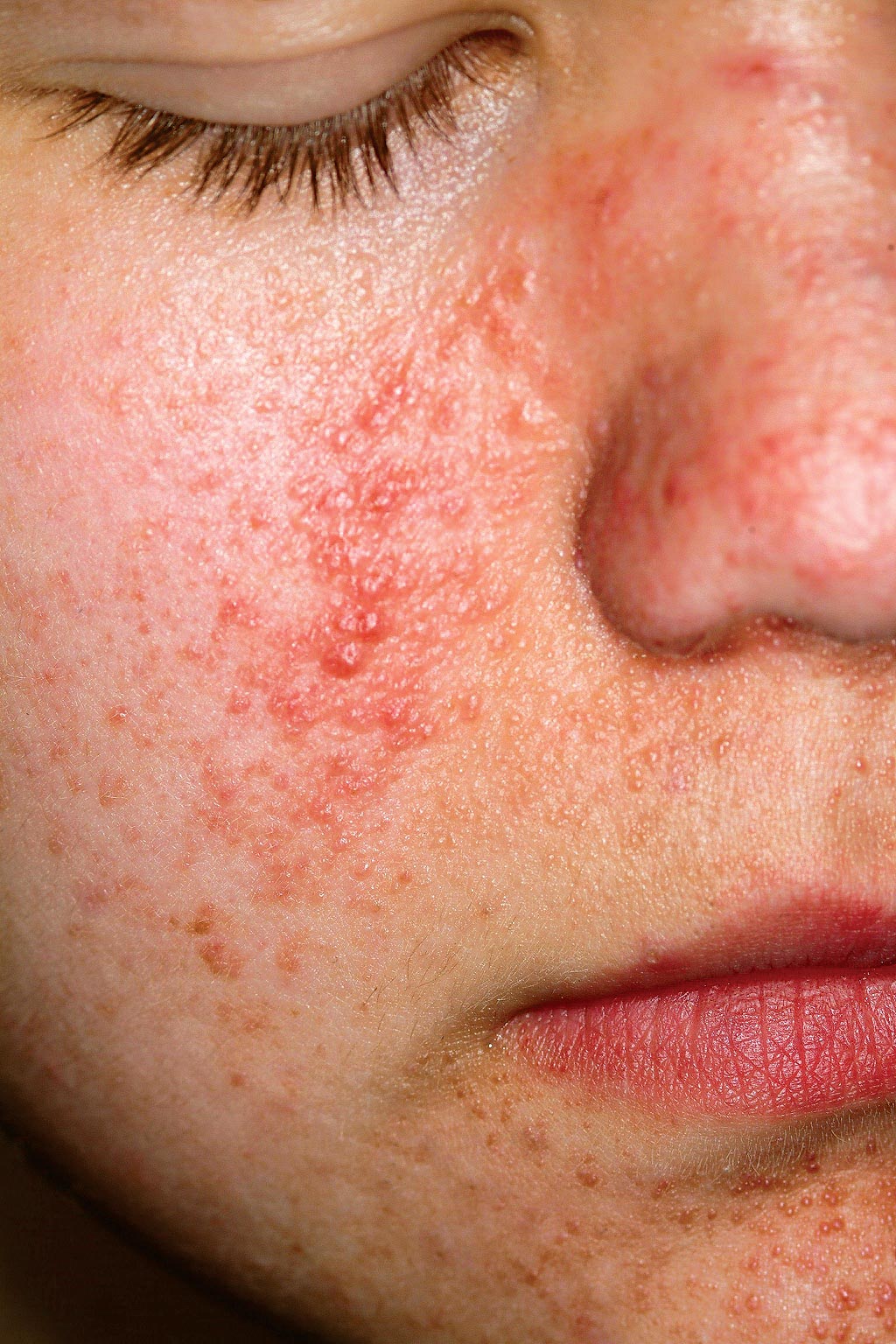
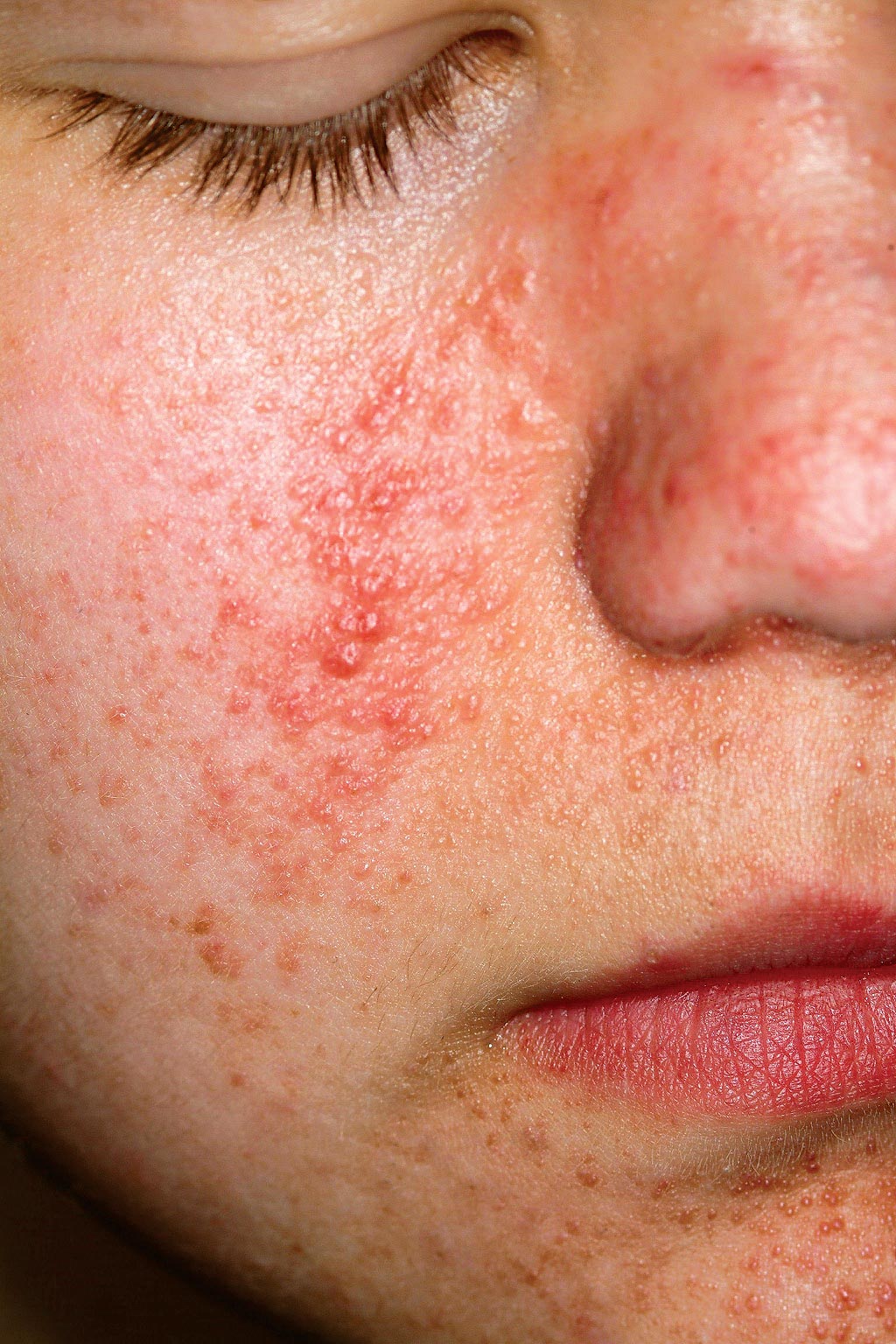
A 14-year-old boy is seen for “acne” that has been unresponsive to oral and topical antibiotics. There is no family history of acne, but the boy has a history of unexplained grand mal seizures. The dermatologic condition, which has been present since an early age, has been variously diagnosed as warts and molluscum contagiosum, as well as acne. However, since none of the treatments offered has been successful, the patient is referred to dermatology. On examination, you note a dense collection of fleshy papules in bilateral nasolabial areas, thinning out around the mouth.