Article

Reflectance Confocal Microscopy as a Diagnostic Aid in Allergic Contact Dermatitis to Mango Sap
- Author:
- Grace Wei, MD, MPH
- Katharine Hanlon, BFA
- Alexei Gonzalez-Estrada, MD
- Lilia Correa-Selm, MD
The mango tree (Mangifera indica) produces nutrient-dense fruit that is consumed across the world. Interestingly, despite widespread...
Article
Does allergic conjunctivitis always require prescription eyedrops?
- Author:
- Alexei Gonzalez-Estrada, MD
- Lisanne P. Newton, MD
We reserve prescription drops for patients with persistent bothersome symptoms despite using over-the-counter drops.
Article
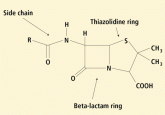
Penicillin allergy: A practical guide for clinicians
- Author:
- Alexei Gonzalez-Estrada, MD
- Cristine Radojicic, MD
Clinical presentation is key in classifying reactions as either medicated by immunoglobulin E or not.
