Article
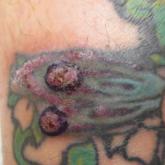
Pseudoepitheliomatous Hyperplasia Arising From Purple Tattoo Pigment
- Author:
- Shiva Kheradmand, DO
- Benjamin M. Perry, DO
- Angela Bohlke, MD
Pseudoepitheliomatous hyperplasia is a rare benign condition that can arise in response to multiple underlying triggers such as tattoo pigment.
Article
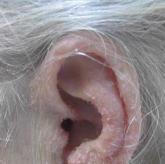
Trichodysplasia Spinulosa in the Setting of Colon Cancer
- Author:
- R. Scott Thomas, DO
- William Lear, MD
- Angela Bohlke, MD
Trichodysplasia spinulosa (TS) is a rare skin condition seen in immunosuppressed patients that is characterized by folliculocentric papules with...
