Article
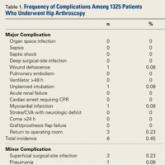
Complications and Risk Factors for Morbidity in Elective Hip Arthroscopy: A Review of 1325 Cases
- Author:
- Chris A. Anthony, MD
- Andrew J. Pugely, MD
- Yubo Gao, PhD
- Robert R. Westermann, MD
- Christopher T. Martin, MD
- Brian R. Wolf, MD, MS
- Annunziato Amendola, MD
We conducted a study of elective hip arthroscopy patients to determine type and incidence of complications and rates of and risk factors for minor...
