Article

Quality and Quantity of the Elbow Arthroscopy Literature: A Systematic Review and Meta-Analysis
- Author:
- Erickson BJ
- Chalmers PN
- Cvetanovich GL
- Frank RM
- Romeo AA
- Harris JD
The purpose of this article is to perform a systematic review and meta-analysis of elbow arthroscopy literature to answer the following questions...
Article

Predicting and Preventing Injury in Major League Baseball
- Author:
- Erickson BJ
- Chalmers PN
- Bush-Joseph CA
- Romeo AA
Major League Baseball (MLB) players are at significant risk for both chronic, repetitive overuse injuries as well as acute traumatic injuries....
Article
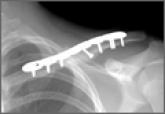
Is Skin Tenting Secondary to Displaced Clavicle Fracture More Than a Theoretical Risk? A Report of 2 Adolescent Cases
- Author:
- Chalmers PN
- Van Thiel Gs
- Ferry ST
While one traditional indication for open reduction and internal fixation (ORIF) of clavicle fractures was tenting of the skin because of concern...
