News
One practice’s experience with obesity treatment
- Author:
- Ian Lacy
WASHINGTON – “We have heard about a lot of really interesting new things in therapy, but the reality is that they are just not economically viable...
News
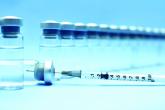
Cost is high for Japanese encephalitis vaccinations
- Author:
- Ian Lacy
A model of Japanese encephalitis showed a low chance of transmission coupled with large individual and societal...
News
Disparities found in access to medication treatment for OUDs
- Author:
- Ian Lacy
Medicaid recipients living in counties with fewer black and Hispanic residents – and lower poverty rates – are more likely to receive OUD...
News

FDA approves topical anticholinergic for primary axillary hyperhidrosis
- Author:
- Ian Lacy
Glycopyrronium, approved for children and adults ages 9 years and older, comes in a single-use cloth wipe applied once a day to both axillae.
News
Screen sooner and more often for those with family history of CRC
- Author:
- Ian Lacy
A family history of colorectal cancer is associated with risk of colorectal cancer, and screening guidelines should be adjusted accordingly.
News
Anthrax vaccine recommendations updated in the event of a wide-area release
- Author:
- Ian Lacy
The committee recommended three updates to its current policy of anthrax vaccination.
News
Bullae associated with pediatric human parvovirus B19 infection
- Author:
- Ian Lacy
Parvovirus is generally associated with a “slapped-cheek” appearance, with the appearance of bullae rare.
News
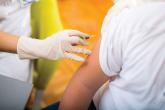
ACIP votes to recommend new strains for the 2018-2019 flu vaccine
- Author:
- Ian Lacy
FluMist is back in the midst of available flu vaccine options.
News

Preterm infant GER is a normal phenomenon
- Author:
- Ian Lacy
Traditional and pharmacologic interventions do not appear to work. Patience may be the best medicine.
News
Pancreatic cancer has a pancreatopathy distinct from type 2 diabetes
- Author:
- Ian Lacy
WASHINGTON – The relationship between pancreatic cancer and diabetes is complex, but certain pathological markers differentiate them.
News
FDA approves pembrolizumab for relapsed/refractory PMBCL
- Author:
- Ian Lacy
The FDA granted accelerated approval based on results from the KEYNOTE-170 trial.
Video

Web portal does not reduce phone encounters or office visits for IBD patients
- Author:
- Ian Lacy
WASHINGTON - The web portal MyChart allows patients to send messages to their providers, but does not improve patient outcomes.
News

Multiple therapies for NAFLD and NASH are now in phase 3 clinical trials
- Author:
- Ian Lacy
WASHINGTON – The trials are tricky, but these much-needed therapies may get conditional approval through reduction of liver inflammation and...
News
Barrett’s segment length, low-grade dysplasia tied to increased risk of neoplastic progression
- Author:
- Ian Lacy
A Dutch study found that age at baseline endoscopy, length of Barrett’s segment, and low-grade dysplasia were significant predictors of neoplastic...
News

FDA approves Olumiant for treatment of rheumatoid arthritis
- Author:
- Ian Lacy
Lilly said it expects the JAK inhibitor to be available in the second quarter of 2018.
