Article
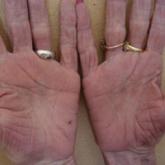
Paraneoplastic Palmoplantar Keratoderma Secondary to Metastatic Uterine Adenocarcinoma
- Author:
- Joseph R. Kallini, MD
- Khosro Sadeghani, MD
- Amor Khachemoune, MD
Palmoplantar keratoderma (PPK) is a dermatosis that presents as hyperkeratosis of the palms and soles. It may be acquired or heritable. Acquired...
