Quiz
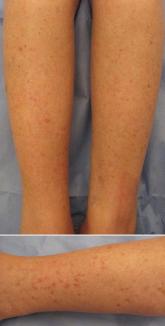
Erythematous Scaly Papules on the Shins and Calves
- Author:
- Julia G. Gosis, MD
- Stephanie Y. Daniel, MD
- Barbara B. Wilson, MD
A 73-year-old white woman presented to the dermatology clinic with a mildly pruritic, slowly progressive rash on the shins and calves of 10 years...
