Article
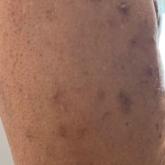
Miliarial Gout in an Immunocompromised Patient
- Author:
- Surya Patel MD
- Hysem Eldik, MD
- Maria Angelica Selim, MD
- Rami Nayef Al-Rohil, MBBS
- Matilda Nicholas, MD, PhD
Immunocompromised status may be a risk factor for miliarial gout, especially in patients with a history of gout or hyperuricemia.
Article
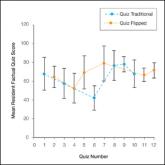
A Comparison of Knowledge Acquisition and Perceived Efficacy of a Traditional vs Flipped Classroom–Based Dermatology Residency Curriculum
- Author:
- Lauren N. Pontius, MD
- Joanna Hooten, MD
- Erin Lesesky, MD
- Caroline Rao, MD
- Matilda Nicholas, MD, PhD
- Rebecca Bialas, MD
- Beiyu Liu, PhD
- Cynthia L. Green, PhD
- Amber Reck Atwater, MD
Flipped and traditional classroom models were compared in the Duke University Medical Center (Durham, North Carolina) dermatology residency...
