Article
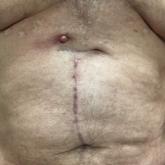
Erythematous Abdominal Nodule
- Author:
- Ryan Gall, MD
- Matthew Willett, MD
- John D. Peters, MD
A 71-year-old man presented with an inflamed erythematous papule on the right subcostal region of 12 months’ duration. It began as a small...
Quiz
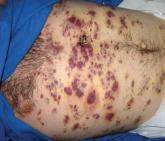
Partially Blanchable Violaceous Lesions in an AIDS Patient
- Author:
- Kermit L. Jones, MD, JD
- Matthew Willett, MD
- Catherine F. Decker, MD
- George W. Turiansky, MD
A 37-year-old AIDS patient (CD4 lymphocyte count, 7 cells/mm3 [reference range, 500–1000 cells/mm3]; viral load, >200,000...
