Article
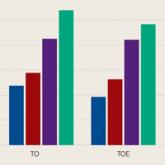
Arthroscopic Transosseous and Transosseous-Equivalent Rotator Cuff Repair: An Analysis of Cost, Operative Time, and Clinical Outcomes
- Author:
- Adam J. Seidl
- MD; Nicholas J. Lombardi
- BS; Mark D. Lazarus
- MD; Eric M. Black
- MD; Mitchell G. Maltenfort
- PhD; Matthew D. Pepe
- MD; Luke S. Austin
- MD
The rate of medical visits for rotator cuff pathology and the US incidence of arthroscopic rotator cuff repair (RCR) have increased...
