Article
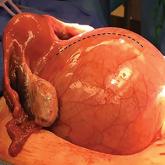
Myomectomy of a large cervical fibroid in a patient desiring future fertility
- Author:
- Morgan Booher, DO
- Mitchell Edelson, MD
- David Jaspan, DO
- Jay Goldberg, MD, MSCP
A technique for myomectomy with uterine preservation in a 33-year-old woman with a 20-cm cervical fibroid, as well as a strategy for preoperative...
