Article
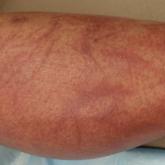
Flagellate Shiitake Mushroom Reaction With Histologic Features of Acute Generalized Exanthematous Pustulosis
- Author:
- Richard J. Browning, MD
- Ramin Fathi, MD
- Mahsa A. Smith, MD
- Theodore Alkousakis, MD
Ingestion of shiitake mushrooms and bleomycin is associated with flagellate dermatitis.
Article
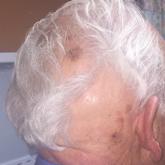
Remote-Onset Alopecia Areata Attributed to Ipilimumab
- Author:
- David R. Pearson, MD
- Karl Lewis, MD
- Theodore Alkousakis, MD
Cutaneous immune-related adverse effects (irAEs) are among the most common adverse effects of ipilimumab used to treat advanced-stage melanoma....
