News
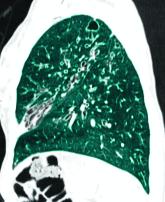
Cystic fibrosis: Advances, ongoing challenges
- Author:
- Walter Alexander
As testing and treatment for cystic fibrosis have advanced, care must include management of comorbidities.
News

Pulmonary telerehabilitation for COPD: Promising, but more data needed
- Author:
- Walter Alexander
Telehealth options for pulmonary rehabilitation may increase access, but reimbursement and assessment remain hurdles.
News
Asthma, COPD inhaler price caps set for summer
- Author:
- Walter Alexander
In addition to warmer weather, June will usher in changes in asthma and COPD inhaler costs for many patients, potentially reducing barriers to...
News
Digital Inhaler Discontinuations: Not Enough Uptake of Device
- Author:
- Walter Alexander
Another asthma inhaler is discontinued in 2024, further reducing available treatments for adults and children.
News

Both Promise and Concern for OSA and CPAP with GLP-1s
- Author:
- Walter Alexander
Weight loss drugs, GLP-1s, could aid in obesity-related conditions such as OSA, but do not eliminate the need for lifestyle changes.
News
Noninvasive AI-Driven Tool Speeds Idiopathic Pulmonary Fibrosis Diagnosis
- Author:
- Walter Alexander
AI tool given FDA approval for speeding up diagnosis of IPF.
News
Flovent Brand Discontinuation Likely Smooth for Many, Difficult for Some
- Author:
- Walter Alexander
Rising inhaler costs focus of US Senate committee letter to Pharma CEOs.
News
Recurrent Bleeding in Small-Intestinal Angiodysplasia Reduced by Thalidomide
- Author:
- Walter Alexander
Bleeding reductions persisting after treatment suggest that thalidomide may be disease modifying.
News
Pulmonary arterial hypertension: Promising results for investigational agents and catheter-based denervation
- Author:
- Walter Alexander
Evidence for three pulmonary artery hypertension treatments was presented at the American Heart Association 2023 scientific sessions.
News
Smartphone app detects voice quality changes indicating worsening heart failure
- Author:
- Walter Alexander
Early warnings were generated 24-26 days before heart failure events.
News
In-hospital mortality increased in COPD patients with acute exacerbations and high serum phosphate levels
- Author:
- Walter Alexander
Acute exacerbations of chronic obstructive pulmonary disease linked to higher in-hospital mortality among AECOPD patients with high serum...
News

Pediatric sleep-disordered breathing linked to multilevel risk factors
- Author:
- Walter Alexander
Exposure to indoor pests, maternal education, and neighborhood factors play into sleep-disordered breathing–related symptoms.
News

Tapering lupus drugs in stable patients: Large study outlines risks, benefits
- Author:
- Walter Alexander
A recent multinational, observational cohort study found that drug tapering warrants careful consideration of risks and benefits and is best...
News
First guidelines developed for childhood eosinophilic GI disorders beyond eosinophilic esophagitis
- Author:
- Walter Alexander
“Our ability to say: ‘Here are the established treatments,’ is lacking, though. We need research studies to verify that our recommended approaches...
News
App cuts alcohol intake in risky drinkers
- Author:
- Walter Alexander
“Our brief electronic intervention had clear impact on the drinking behavior of hazardous drinkers.”
