Article
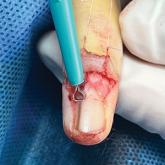
Customized Dermal Curette: An Alternative and Effective Shaving Tool in Nail Surgery
- Author:
- Wei Zhang, MD
- Hui Fan, MD
- Lingxi Gu, MS
- Hongguang Lu, MD, PhD
Surgical excision of the pigmented nail matrix followed by histopathologic examination is a common procedure aimed at managing longitudinal...
Article
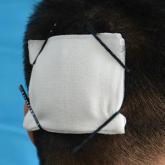
Affixing a Scalp Dressing With Hairpins
- Author:
- Jun Zhang, MD
- Yu Wang, PhD
- Wei Zhang, MD
- Hongguang Lu, PhD
We describe a method for using hairpins to affix a dressing after scalp surgery or trauma that is sturdy, does not compromise aesthetics, and does...
