User login
A 25-year-old man presents with a 2-month history of generalized itching that began 5 weeks after returning from a trip to a beach in Brazil, during which he had sexual relations without protection. He has already been treated with topical steroids and antihistamines, with no improvement.
Q: What is the most likely diagnosis?
- Herpes simplex type 2
- Acute trypanosomiasis
- Syphilis
- Scabies
- Papular urticaria
A: The most likely diagnosis is scabies, an intensely pruritic skin infestation caused by the host-specific mite Sarcoptes scabiei var hominis.1 Herpes simplex type 2 infection presents with clustered vesicles, not nodules, on an erythematous base in the genital area, without generalized pruritus. Acute trypanosomiasis involves malaise, fever, vomiting, diarrhea, anorexia, rash, tachycardia, and even generalized lymphadenopathy and meningeal irritation, but generalized itching is not typical. The location and morphology of the patient’s lesions are not consistent with syphilis. Topical steroids and oral antihistamines should have improved the pruritus of papular urticaria.
A GLOBAL PUBLIC HEALTH PROBLEM
Scabies is a worldwide public health problem, affecting people of all ages, races, and socioeconomic groups.1 Overcrowding, delayed diagnosis and treatment, and poor public education contribute to the prevalence of scabies in both industrialized and nonindustrialized nations.2 Prevalence rates are higher in children and people who are sexually active.3
Sexual transmission is by close skin-to-skin contact. Poor sensory perception in conditions such as leprosy and compromised immunity due to organ transplantation, human immunodeficiency virus infection, or old age increase the risk for the crusted variant of scabies.2 Patients with the crusted variant tend to present with clinically atypical lesions, and because of this they are often misdiag-nosed, thus delaying treatment and elevating the risk of local epidemics.
CLINICAL ASPECTS
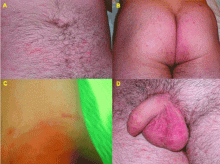
Scabies can mimic a broad range of skin diseases. Patients present with intense itching that is worse at night. The face and neck are rarely affected. The pathognomonic signs of scabies are burrows, erythematous papules, and generalized pruritus (also on non-infested skin) with nocturnal predominance.3 Reddish to brownish extremely pruritic nodules of 2 to 20 mm in diameter may be also present on the genitalia (more commonly in males than in females), buttocks, groin, and axillary regions. Patients usually have secondary papules, pustules, vesicles, and excoriations.
DIAGNOSIS
Every patient with intense pruritus should be suspected of having scabies, but especially if a family member reports similar symptoms.3 A diagnosis can be made clinically if a burrow is detected at a typical predilection site and if the lesion itches severely. In this case, even a single burrow is pathognomonic.2 The diagnosis is confirmed by light-microscopic identification of mites, larvae, ova, or scybala (fecal pellets) in skin scrapings.1
TREATMENT
Treatment includes a scabicidal agent, an antipruritic agent such as a sedating antihistamine, and an appropriate antimicrobial agent in cases of secondary infection. Permethrin (Acticin), a 5% synthetic pyrethroid cream, is an excellent scabicide and is the preferred treatment.1 All family members and close contacts must be evaluated and treated, even if they do not have symptoms.1
- Chosidow O. Clinical practices. Scabies. N Engl J Med 2006; 354:1718–1727.
- Heukelbach J, Feldmeier H. Scabies. Lancet 2006; 367:1767–1774.
- Hengge UR, Currie BJ, Jäger G, Lupi O, Schwartz RA. Scabies: a ubiquitous neglected skin disease. Lancet Infect Dis 2006; 6:769–779.
A 25-year-old man presents with a 2-month history of generalized itching that began 5 weeks after returning from a trip to a beach in Brazil, during which he had sexual relations without protection. He has already been treated with topical steroids and antihistamines, with no improvement.
Q: What is the most likely diagnosis?
- Herpes simplex type 2
- Acute trypanosomiasis
- Syphilis
- Scabies
- Papular urticaria
A: The most likely diagnosis is scabies, an intensely pruritic skin infestation caused by the host-specific mite Sarcoptes scabiei var hominis.1 Herpes simplex type 2 infection presents with clustered vesicles, not nodules, on an erythematous base in the genital area, without generalized pruritus. Acute trypanosomiasis involves malaise, fever, vomiting, diarrhea, anorexia, rash, tachycardia, and even generalized lymphadenopathy and meningeal irritation, but generalized itching is not typical. The location and morphology of the patient’s lesions are not consistent with syphilis. Topical steroids and oral antihistamines should have improved the pruritus of papular urticaria.
A GLOBAL PUBLIC HEALTH PROBLEM
Scabies is a worldwide public health problem, affecting people of all ages, races, and socioeconomic groups.1 Overcrowding, delayed diagnosis and treatment, and poor public education contribute to the prevalence of scabies in both industrialized and nonindustrialized nations.2 Prevalence rates are higher in children and people who are sexually active.3
Sexual transmission is by close skin-to-skin contact. Poor sensory perception in conditions such as leprosy and compromised immunity due to organ transplantation, human immunodeficiency virus infection, or old age increase the risk for the crusted variant of scabies.2 Patients with the crusted variant tend to present with clinically atypical lesions, and because of this they are often misdiag-nosed, thus delaying treatment and elevating the risk of local epidemics.
CLINICAL ASPECTS
Scabies can mimic a broad range of skin diseases. Patients present with intense itching that is worse at night. The face and neck are rarely affected. The pathognomonic signs of scabies are burrows, erythematous papules, and generalized pruritus (also on non-infested skin) with nocturnal predominance.3 Reddish to brownish extremely pruritic nodules of 2 to 20 mm in diameter may be also present on the genitalia (more commonly in males than in females), buttocks, groin, and axillary regions. Patients usually have secondary papules, pustules, vesicles, and excoriations.
DIAGNOSIS
Every patient with intense pruritus should be suspected of having scabies, but especially if a family member reports similar symptoms.3 A diagnosis can be made clinically if a burrow is detected at a typical predilection site and if the lesion itches severely. In this case, even a single burrow is pathognomonic.2 The diagnosis is confirmed by light-microscopic identification of mites, larvae, ova, or scybala (fecal pellets) in skin scrapings.1
TREATMENT
Treatment includes a scabicidal agent, an antipruritic agent such as a sedating antihistamine, and an appropriate antimicrobial agent in cases of secondary infection. Permethrin (Acticin), a 5% synthetic pyrethroid cream, is an excellent scabicide and is the preferred treatment.1 All family members and close contacts must be evaluated and treated, even if they do not have symptoms.1
A 25-year-old man presents with a 2-month history of generalized itching that began 5 weeks after returning from a trip to a beach in Brazil, during which he had sexual relations without protection. He has already been treated with topical steroids and antihistamines, with no improvement.
Q: What is the most likely diagnosis?
- Herpes simplex type 2
- Acute trypanosomiasis
- Syphilis
- Scabies
- Papular urticaria
A: The most likely diagnosis is scabies, an intensely pruritic skin infestation caused by the host-specific mite Sarcoptes scabiei var hominis.1 Herpes simplex type 2 infection presents with clustered vesicles, not nodules, on an erythematous base in the genital area, without generalized pruritus. Acute trypanosomiasis involves malaise, fever, vomiting, diarrhea, anorexia, rash, tachycardia, and even generalized lymphadenopathy and meningeal irritation, but generalized itching is not typical. The location and morphology of the patient’s lesions are not consistent with syphilis. Topical steroids and oral antihistamines should have improved the pruritus of papular urticaria.
A GLOBAL PUBLIC HEALTH PROBLEM
Scabies is a worldwide public health problem, affecting people of all ages, races, and socioeconomic groups.1 Overcrowding, delayed diagnosis and treatment, and poor public education contribute to the prevalence of scabies in both industrialized and nonindustrialized nations.2 Prevalence rates are higher in children and people who are sexually active.3
Sexual transmission is by close skin-to-skin contact. Poor sensory perception in conditions such as leprosy and compromised immunity due to organ transplantation, human immunodeficiency virus infection, or old age increase the risk for the crusted variant of scabies.2 Patients with the crusted variant tend to present with clinically atypical lesions, and because of this they are often misdiag-nosed, thus delaying treatment and elevating the risk of local epidemics.
CLINICAL ASPECTS
Scabies can mimic a broad range of skin diseases. Patients present with intense itching that is worse at night. The face and neck are rarely affected. The pathognomonic signs of scabies are burrows, erythematous papules, and generalized pruritus (also on non-infested skin) with nocturnal predominance.3 Reddish to brownish extremely pruritic nodules of 2 to 20 mm in diameter may be also present on the genitalia (more commonly in males than in females), buttocks, groin, and axillary regions. Patients usually have secondary papules, pustules, vesicles, and excoriations.
DIAGNOSIS
Every patient with intense pruritus should be suspected of having scabies, but especially if a family member reports similar symptoms.3 A diagnosis can be made clinically if a burrow is detected at a typical predilection site and if the lesion itches severely. In this case, even a single burrow is pathognomonic.2 The diagnosis is confirmed by light-microscopic identification of mites, larvae, ova, or scybala (fecal pellets) in skin scrapings.1
TREATMENT
Treatment includes a scabicidal agent, an antipruritic agent such as a sedating antihistamine, and an appropriate antimicrobial agent in cases of secondary infection. Permethrin (Acticin), a 5% synthetic pyrethroid cream, is an excellent scabicide and is the preferred treatment.1 All family members and close contacts must be evaluated and treated, even if they do not have symptoms.1
- Chosidow O. Clinical practices. Scabies. N Engl J Med 2006; 354:1718–1727.
- Heukelbach J, Feldmeier H. Scabies. Lancet 2006; 367:1767–1774.
- Hengge UR, Currie BJ, Jäger G, Lupi O, Schwartz RA. Scabies: a ubiquitous neglected skin disease. Lancet Infect Dis 2006; 6:769–779.
- Chosidow O. Clinical practices. Scabies. N Engl J Med 2006; 354:1718–1727.
- Heukelbach J, Feldmeier H. Scabies. Lancet 2006; 367:1767–1774.
- Hengge UR, Currie BJ, Jäger G, Lupi O, Schwartz RA. Scabies: a ubiquitous neglected skin disease. Lancet Infect Dis 2006; 6:769–779.