The hospital is altogether the most complex human organization ever devised. Peter Drucker 1
The ever-changing landscape of today’s increasingly complex health care system depends on implementing multifaceted, team-based methods of care delivery to provide safe, effective patient care.2 Critical to establishing and sustaining exceptionally safe, effective patient care is open, transparent communication among members of interprofessional teams with senior leaders.3 However, current evidence shows that poor communication among interprofessional health care teams and leadership is commonplace and a significant contributing factor to inefficiencies, medical errors, and poor outcomes.4 One strategy for improving communication is through the implementation of leader rounding for high reliability. The concept of high reliability pertains to organizations that operate in high-risk environments for prolonged periods without serious adverse events or catastrophic failures.5 The overarching goal of implementation is to ensure that efficient communication exists among members of the health care team, which is essential for providing safe, quality patient care.
We describe the importance of leader rounding for high reliability as an approach to improving patient safety. Based on a review of the literature, our experiences, and lessons learned, we offer recommendations for how health care organizations on the journey to high reliability can improve patient safety.
Rounding in health care is not new. In fact, rounding has been a strong principal practice globally for more than 2 decades.6 During this time, varied rounding approaches have emerged, oftentimes focused on areas of interest, such as patient care, environmental services, facilities management, and discharge planning.4,7 Variations also might involve the location of the rounds, such as a patient’s bedside, unit hallways, and conference rooms as well as the naming of rounds, such as interdisciplinary/multidisciplinary, teaching, and walkrounds.7-10
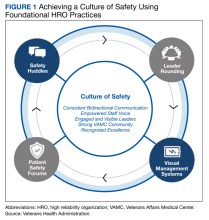
A different type of rounding that is characteristic of high reliability organizations (HROs) is leader rounding for high reliability. The Veterans Health Administration (VHA) formally launched its journey to becoming an enterprise HRO in February 2019, using 3 cohorts. At the Veterans Affairs Bedford Healthcare System (VABHS) in Massachusetts, the journey commenced in 2021 as part of the third cohort. Leader rounding for high reliability is one of VHAs 4 HRO foundational practices for achieving a culture of safety (Figure 1).11