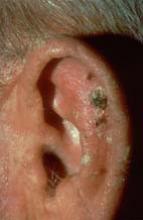
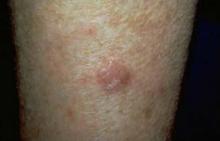
NAPA, CALIF. – A preventive approach is needed in the treatment of actinic keratoses to curtail the potential emergence of nonmelanoma skin cancer, according to Dr. Miriam S. Bettencourt.
"In addition to the visible AKs that we see, there’s a lot more in the field area of the AK below the skin surface," she said. "AKs are just the tip of the iceberg."
Because nonmelanoma skin cancer can be easily missed in AK patients, Dr. Bettencourt, of the University of Nevada in Las Vegas, recommended treating all AK lesions.
Many factors should be taken into consideration when determining the best AK treatment for patients, she said, including the number of lesions and location, patient compliance, cosmetic implications, age of patient, history of skin cancer, and insurance coverage.
The treatment of AK involves lesion-directed destructive procedures, topical field-directed therapies, or combination treatment.
Lesion Destruction Therapies
For treating nonspecific lesions, Dr. Bettencourt recommended considering cryosurgery, noting an efficacy rate of 67%-88% and a 1-year recurrence rate of 1.2%-12%. Side effects are mild, the most common being pain, redness, edema, and hypo- or hyperpigmentation.
Chemical peels are an option for extensive AKs, she said, noting an efficacy rate of 75% and a recurrence rate of 25%-35% at 1 year, depending on the agent. Side effects with peels are mild, the most common being pain, inflammation, and pigment alterations.
For single lesions on the face, scalp, or neck, or for full-face resurfacing, CO2 and YAG lasers can be used. While device dependent, 90% of patients achieve lesion remission; however, the recurrence rate is 10%-15% at 3-6 months.
Photodynamic therapy (PDT) offers selective destruction of atypical cells through light activation of a photosensitizer. She noted an efficacy rate of 70%-78% after one treatment session, and a rate of 90% after two sessions. However, there is a risk of photosensitivity and pain from treatment, and it tends to cost more than other therapies, she noted.
Topical Treatment
Topical 5-fluorouracil "inhibits thymidylate synthetase and causes cell death in actively proliferating cells," reported Dr. Bettencourt. A 5% cream or solution is the most popular form of 5-FU, but it is also available in 2%, 1%, and 0.5% formulas.
The 5% cream should be applied twice a day for a month. Common side effects include temporary ulcers, erythema, crusting, and scarring. She highly recommended reviewing the adverse effects with patients before treatment. She noted that she has patients sign the package insert before she begins treatment with 5-FU.
Imiquimod is another topical treatment available for AKs that upregulates a variety of cytokines, she said. "Experimental evidence suggests that patients may develop T-cell memory after treatment, and thus develop less AKs in the future." She recommended Aldara 5%, which is applied 2-3 times per week for up to 4 months, or Zyclara 3.75%, which is applied once a day for two cycles of 2 weeks (with a 2-week free interval in the middle).
The last topical agent she recommended was diclofenac sodium 3% gel (Solaraze), which is a nonsteroidal anti-inflammatory drug that is well tolerated. "The treatment inhibits cyclooxygenase, which is essential for biosynthesis of prostaglandins," she said. Hyaluronic acid delays uptake of the drug, which leads to higher concentrations in the skin. Patients should be treated with the gel twice a day for 3 months. Little to no inflammation may occur during treatment; however, the drug has been known to cause hepatotoxicity.
She noted that diclofenac is her treatment of choice for AKs on the lips.
Combination Therapy
Consider combination, sequential therapy with 0.5% micronized 5-FU before cryotherapy for better results than cryotherapy alone, said Dr. Bettencourt. In a study of 144 patients, 5-FU plus cryotherapy resulted in partial remission in 62% of patients, and complete remission in 17% of patients after 4 weeks of treatment (Arch. Dermatol. 2004;140:813-6).
Low-dose 5-FU plus salicylic acid has also been found to be an effective treatment for AKs, she said. A 2009 study found that 5-FU combined with Jessner’s solution or a 70% glycolic acid peel every other week had an 80% clearance rate and offered photodamage improvement (Int. J. Dermatol. 2009;48:902-7).
PDT followed by treatment with imiquimod 5% was found to reduce lesions by 89.9%, compared with 74.5% with placebo at 12 months (J. Drugs Dermatol. 2009;8:35-9). The randomized vehicle-controlled study enrolled 25 patients (24 completed the study), with a at least 10 AKs. The entire face of each patient was treated with PDT and aminolevulinic acid 20% at baseline and at 1 month; then, at month 2, imiquimod 5% was applied to one-half of each patient’s face and a vehicle to the other half two times a week for 16 weeks. Erythema and flaking were the most serious skin reactions reported during the study.