Another confusing aspect of toddler’s fracture is that the causative injury is often considered insignificant by parents—eg, tripping, falling from a modest height, or a twisting motion.7,8 These events may occur countless times during the average day of a toddler. Often parents do not witness the injury and are unable to describe the mechanism of injury.7
When to suspect child abuse. When a child presents with fracture after an unwitnessed trauma and the story does not match the injury pattern, consider child abuse. With tibial fractures, the location of the fracture can help distinguish a result of abuse from a toddler’s fracture. Toddler’s fracture is classically described as a distal tibial fracture. In contrast, a midshaft tibial fracture often suggests child abuse.8,13 In a small retrospective study of 37 children diagnosed with toddler’s fracture, 4 midshaft tibial fractures were found.8 Child abuse was confirmed in 2 of these cases.8 However, other authors, including Dr. Dunbar in his sentinel article,6 assert that toddler’s fracture may occasionally extend into the midshaft of the tibia. Consequently, a midshaft tibial fracture is not pathognomonic for child abuse. But the diagnosis should be considered. Perform a careful examination for other signs of abuse or neglect, and do not hesitate to report suspected child abuse to the proper local and state authorities.14
Transient synovitis vs septic arthritis
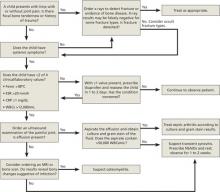
A child who limps or refuses to bear weight on a limb often has associated symptoms of acute illness. In these cases, or when radiographs have ruled out apparent abnormalities such as Legg-Calve-Perthes disease, SCFE, and fracture, consider septic arthritis or transient synovitis (FIGURE). Both may present with limp and fever as well as pain, decreased range of motion, bone tenderness, swelling, and warmth.15
Transient synovitis is the most common cause of hip pain in children up to 10 years of age, with a 3% risk of occurrence through childhood.16,17 Its cause is unclear, but many experts have proposed a viral agent.17 Transient synovitis universally resolves without sequelae in 1 to 2 weeks. Therefore, prescribe rest and nonsteroidal anti-inflammatory drugs (NSAIDs) for symptomatic relief, and reassure parents.16
Septic arthritis, although often similar in presentation to transient synovitis, requires hospitalization, operative drainage, and parenteral antibiotics.18 A delay in diagnosis is associated with poor outcome, including osteonecrosis, growth arrest, permanent loss of joint function, and sepsis.3,18
Several studies have shown children with septic arthritis usually appear more acutely ill than those with transient synovitis.4,18-21 They are described as toxic-appearing, and have leukocytosis, a high erythrocyte sedimentation rate (ESR), and a high fever.19 However, no single marker or specific laboratory value consistently identifies septic arthritis. Many studies have been performed in an effort to identify a collection of factors, or an algorithm, that can predict the probability of septic arthritis.
Fever, an elevated ESR, and leukocytosis are independent multivariate clinical predictors for septic arthritis. The prediction algorithm published by Jung et al is the only study to have included C-reactive protein (CRP) as a predictive factor,4 which happens to be an excellent independent predictor of septic arthritis. Specifically, with a normal CRP <1 mg/dL, the probability of a patientnot having septic arthritis is 87%.22
While no predictive algorithm has been conclusively validated, the fact that the same clinical and laboratory predictors are consistently identified can be useful. Simply, if a patient presents with joint pain and 2 or more of the 4 predictors, septic arthritis must be fully evaluated. The presence of 2 of 4 predictors suggests a risk of septic arthritis between 10% and 40%.4,18,20 A single predictor is associated with a risk of 1% to 10%.4,18,20 Yet, you must interpret these clinical predictors in light of the full clinical picture, as septic arthritis is still possible in patients with only 1 predictor. Such possibilities require cautious management and close follow-up.
With 2 of 4 predictors present, suspect septic arthritis and order an ultrasound of the affected joint. If effusion is present, aspirate the joint. Some authors suggest that all patients with hip pain should undergo ultrasound, and that those with a joint effusion should undergo aspiration.15 However, joint aspiration, particularly of the hip, can be associated with multiple complications and should be avoided if possible.22 Effusion is also possible with transient synovitis and noninfectious causes of joint pain, but the aspirate will have a negative culture and normal gram stain findings. Ultrasound has been shown to be 100% accurate in predicting the presence of effusion.23
FIGURE
Diagnostic algorithm for pediatric limp3,4,6,8-12,15
CRP, C-reactive protein; ESR, erythrocyte sedimentation rate; MRI, magnetic resonance imaging; NSAIDs, nonsteroidal anti-inflammatory drugs; WBCs, white blood cells.