User login
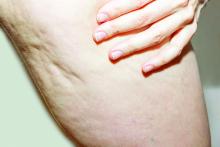
A glimpse at devices designed to tackle cellulite
SAN DIEGO –
A noninvasive treatment, rapid acoustic pulse (RAP) technology (RESONIC), was cleared by the Food and Drug Administration in 2021 for short-term improvement in the appearance of cellulite. The device emits rapid acoustic pulses (shock waves) that are transmitted through the skin to rupture or shear the fibrotic septa; release of the septa results in the smoothing of skin dimples, Arisa E. Ortiz, MD, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual Masters of Aesthetics Symposium. RAP, however, was “taken off the market temporarily to refine the design.”
According to Dr. Ortiz, RAP’s repetition rate and short rise time provides microscopic mechanical disruption to the targeted cellular level structures and vacuoles, while high peak pressure and the fast repetition rate exploit the viscoelastic nature of tissue. Compressed pulses from electronic filtering and the reflector shape eliminate cavitation, heat, and pain. Researchers have postulated that the procedure stimulates collagenesis and angiogenesis.
“There’s no heat to this; it just uses sound,” Dr. Ortiz explained. “It’s also time dependent. The longer you do the treatment, the more disruption of the septa you see. The procedure takes 20-30 minutes. Unlike other treatments, it’s not just for discreet dimples. You can treat entire areas like the buttock or posterior leg,” said Dr. Ortiz, who did not use the RAP device in her practice.
Another device, targeted verifiable subcision (TVS, marketed as Avéli), is FDA cleared for temporary reduction in the appearance of cellulite in the buttock and thigh areas of adult women. “But studies show lasting results, at least through a year,” Dr. Ortiz said. The device features a light-guided probe and a hook. The light enables clinicians to navigate under the skin, while the hook releases a tiny blade that severs the septa. “Once you find the septa, then you activate the blade and release the septa. You go right to left because the direction of the blade is on the left of the probe. Then you go back to verify that you got everything that was creating that dimple.”
Previous devices, she said, would “blindly shear the area, so you would find the dimple and blindly cut, so there was no way to verify that you got the target dimple. The results were sometimes mediocre because you didn’t really know if you effectively treated the area.”
She emphasized that TVS is only useful for discreet dimples. “Many patients who come in asking for cellulite treatment have a lot of laxity and rippled texture,” said Dr. Ortiz, who is also president-elect of the American Society for Laser Medicine and Surgery. “This is not going to be appropriate for those cases. Setting expectations is important. If patients have laxity and discreet dimples and it’s just the dimples that bother them, that’s fine. They just need to understand the difference,” she said, noting that this is “safe for all skin types.”
Tumescent anesthesia is used to control pain during the procedure. The most common adverse events are bruising and soreness. Results from a pivotal trial showed that clinically significant improvements in the primary endpoint, Cellulite Severity Scale scores, were sustained 1 year after treatment. “Hemosiderin staining can occur, but it eventually dissipates on its own,” Dr. Ortiz added. “You can use laser to speed up healing but sometimes that can make it worse, so you want to be careful with that. Most of the time I have patients wait it out; it does go away on its own.”
She noted that the development of RAP and TVS have helped clinicians better understand the makeup of septa. “We used to think of septa as singular bands that are vertically oriented in cellulite, but what we’ve realized is that it’s more like a network of septa,” she said.
Another noninvasive technology, synchronous parallel ultrasound beam technology from Sofwave (marketed as SUPERB), was FDA cleared in December 2022 for the short-term improvement in the appearance of cellulite. The device has seven parallel beam transducers that increase tissue temperatures of the treatment area to 60-70° C, inducing collagen remodeling and collagen denaturation, she said.
In the pivotal study of 68 women, two blinded reviewers reported an 89% improvement rate for both cellulite and skin laxity, after two treatments 2-4 weeks apart, according to data she presented at the meeting. The mean pain score during treatment was 4.55 on a scale of 1-10. No safety issues were observed and immediate responses were limited to erythema and edema.
Dr. Ortiz disclosed having financial relationships with several pharmaceutical and device companies, including receipt of speaker fees and honoraria from Sofwave. She is also cochair of MOAS.
SAN DIEGO –
A noninvasive treatment, rapid acoustic pulse (RAP) technology (RESONIC), was cleared by the Food and Drug Administration in 2021 for short-term improvement in the appearance of cellulite. The device emits rapid acoustic pulses (shock waves) that are transmitted through the skin to rupture or shear the fibrotic septa; release of the septa results in the smoothing of skin dimples, Arisa E. Ortiz, MD, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual Masters of Aesthetics Symposium. RAP, however, was “taken off the market temporarily to refine the design.”
According to Dr. Ortiz, RAP’s repetition rate and short rise time provides microscopic mechanical disruption to the targeted cellular level structures and vacuoles, while high peak pressure and the fast repetition rate exploit the viscoelastic nature of tissue. Compressed pulses from electronic filtering and the reflector shape eliminate cavitation, heat, and pain. Researchers have postulated that the procedure stimulates collagenesis and angiogenesis.
“There’s no heat to this; it just uses sound,” Dr. Ortiz explained. “It’s also time dependent. The longer you do the treatment, the more disruption of the septa you see. The procedure takes 20-30 minutes. Unlike other treatments, it’s not just for discreet dimples. You can treat entire areas like the buttock or posterior leg,” said Dr. Ortiz, who did not use the RAP device in her practice.
Another device, targeted verifiable subcision (TVS, marketed as Avéli), is FDA cleared for temporary reduction in the appearance of cellulite in the buttock and thigh areas of adult women. “But studies show lasting results, at least through a year,” Dr. Ortiz said. The device features a light-guided probe and a hook. The light enables clinicians to navigate under the skin, while the hook releases a tiny blade that severs the septa. “Once you find the septa, then you activate the blade and release the septa. You go right to left because the direction of the blade is on the left of the probe. Then you go back to verify that you got everything that was creating that dimple.”
Previous devices, she said, would “blindly shear the area, so you would find the dimple and blindly cut, so there was no way to verify that you got the target dimple. The results were sometimes mediocre because you didn’t really know if you effectively treated the area.”
She emphasized that TVS is only useful for discreet dimples. “Many patients who come in asking for cellulite treatment have a lot of laxity and rippled texture,” said Dr. Ortiz, who is also president-elect of the American Society for Laser Medicine and Surgery. “This is not going to be appropriate for those cases. Setting expectations is important. If patients have laxity and discreet dimples and it’s just the dimples that bother them, that’s fine. They just need to understand the difference,” she said, noting that this is “safe for all skin types.”
Tumescent anesthesia is used to control pain during the procedure. The most common adverse events are bruising and soreness. Results from a pivotal trial showed that clinically significant improvements in the primary endpoint, Cellulite Severity Scale scores, were sustained 1 year after treatment. “Hemosiderin staining can occur, but it eventually dissipates on its own,” Dr. Ortiz added. “You can use laser to speed up healing but sometimes that can make it worse, so you want to be careful with that. Most of the time I have patients wait it out; it does go away on its own.”
She noted that the development of RAP and TVS have helped clinicians better understand the makeup of septa. “We used to think of septa as singular bands that are vertically oriented in cellulite, but what we’ve realized is that it’s more like a network of septa,” she said.
Another noninvasive technology, synchronous parallel ultrasound beam technology from Sofwave (marketed as SUPERB), was FDA cleared in December 2022 for the short-term improvement in the appearance of cellulite. The device has seven parallel beam transducers that increase tissue temperatures of the treatment area to 60-70° C, inducing collagen remodeling and collagen denaturation, she said.
In the pivotal study of 68 women, two blinded reviewers reported an 89% improvement rate for both cellulite and skin laxity, after two treatments 2-4 weeks apart, according to data she presented at the meeting. The mean pain score during treatment was 4.55 on a scale of 1-10. No safety issues were observed and immediate responses were limited to erythema and edema.
Dr. Ortiz disclosed having financial relationships with several pharmaceutical and device companies, including receipt of speaker fees and honoraria from Sofwave. She is also cochair of MOAS.
SAN DIEGO –
A noninvasive treatment, rapid acoustic pulse (RAP) technology (RESONIC), was cleared by the Food and Drug Administration in 2021 for short-term improvement in the appearance of cellulite. The device emits rapid acoustic pulses (shock waves) that are transmitted through the skin to rupture or shear the fibrotic septa; release of the septa results in the smoothing of skin dimples, Arisa E. Ortiz, MD, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual Masters of Aesthetics Symposium. RAP, however, was “taken off the market temporarily to refine the design.”
According to Dr. Ortiz, RAP’s repetition rate and short rise time provides microscopic mechanical disruption to the targeted cellular level structures and vacuoles, while high peak pressure and the fast repetition rate exploit the viscoelastic nature of tissue. Compressed pulses from electronic filtering and the reflector shape eliminate cavitation, heat, and pain. Researchers have postulated that the procedure stimulates collagenesis and angiogenesis.
“There’s no heat to this; it just uses sound,” Dr. Ortiz explained. “It’s also time dependent. The longer you do the treatment, the more disruption of the septa you see. The procedure takes 20-30 minutes. Unlike other treatments, it’s not just for discreet dimples. You can treat entire areas like the buttock or posterior leg,” said Dr. Ortiz, who did not use the RAP device in her practice.
Another device, targeted verifiable subcision (TVS, marketed as Avéli), is FDA cleared for temporary reduction in the appearance of cellulite in the buttock and thigh areas of adult women. “But studies show lasting results, at least through a year,” Dr. Ortiz said. The device features a light-guided probe and a hook. The light enables clinicians to navigate under the skin, while the hook releases a tiny blade that severs the septa. “Once you find the septa, then you activate the blade and release the septa. You go right to left because the direction of the blade is on the left of the probe. Then you go back to verify that you got everything that was creating that dimple.”
Previous devices, she said, would “blindly shear the area, so you would find the dimple and blindly cut, so there was no way to verify that you got the target dimple. The results were sometimes mediocre because you didn’t really know if you effectively treated the area.”
She emphasized that TVS is only useful for discreet dimples. “Many patients who come in asking for cellulite treatment have a lot of laxity and rippled texture,” said Dr. Ortiz, who is also president-elect of the American Society for Laser Medicine and Surgery. “This is not going to be appropriate for those cases. Setting expectations is important. If patients have laxity and discreet dimples and it’s just the dimples that bother them, that’s fine. They just need to understand the difference,” she said, noting that this is “safe for all skin types.”
Tumescent anesthesia is used to control pain during the procedure. The most common adverse events are bruising and soreness. Results from a pivotal trial showed that clinically significant improvements in the primary endpoint, Cellulite Severity Scale scores, were sustained 1 year after treatment. “Hemosiderin staining can occur, but it eventually dissipates on its own,” Dr. Ortiz added. “You can use laser to speed up healing but sometimes that can make it worse, so you want to be careful with that. Most of the time I have patients wait it out; it does go away on its own.”
She noted that the development of RAP and TVS have helped clinicians better understand the makeup of septa. “We used to think of septa as singular bands that are vertically oriented in cellulite, but what we’ve realized is that it’s more like a network of septa,” she said.
Another noninvasive technology, synchronous parallel ultrasound beam technology from Sofwave (marketed as SUPERB), was FDA cleared in December 2022 for the short-term improvement in the appearance of cellulite. The device has seven parallel beam transducers that increase tissue temperatures of the treatment area to 60-70° C, inducing collagen remodeling and collagen denaturation, she said.
In the pivotal study of 68 women, two blinded reviewers reported an 89% improvement rate for both cellulite and skin laxity, after two treatments 2-4 weeks apart, according to data she presented at the meeting. The mean pain score during treatment was 4.55 on a scale of 1-10. No safety issues were observed and immediate responses were limited to erythema and edema.
Dr. Ortiz disclosed having financial relationships with several pharmaceutical and device companies, including receipt of speaker fees and honoraria from Sofwave. She is also cochair of MOAS.
AT MOAS 2023
‘Old school’ laser resurfacing remains an effective option for rejuvenation
SAN DIEGO – , according to Arisa E. Ortiz, MD.
“Fractional resurfacing is great because there is less downtime, but the results are not as dramatic as with fully ablative resurfacing,” Dr. Ortiz, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual Masters of Aesthetics Symposium. In her practice, she said, “we do a combination,” which can include “fully ablative around the mouth and eyes and fractional everywhere else.”
Key drawbacks to fully ablative laser resurfacing include significant downtime and extensive wound care, “so it’s not for everybody,” she said. Prolonged erythema following treatment is expected, “so patients need to plan for this. It can last 3-4 months, and it will continue to fade and can be covered up with makeup, but it does last a while,” she noted. “One of the things that made ablative resurfacing fall out of favor was the delayed and permanent hypopigmentation where there’s a stark line of demarcation because you can’t treat the neck [with this modality], so patients have this pearly white looking face that appears 6 months after the treatment,” she added.
Preoperatively, Dr. Ortiz asks patients what other cosmetic procedures they have had in the past. For example, if they have had a facelift, they might have neck skin on their jawline, which will react differently to fully ablative resurfacing than facial skin. “I don’t perform fully ablative resurfacing on the neck or body, or in patients with darker skin types,” she said.
To optimize results, she recommends pretreatment of the area with a neuromodulator a week or 2 before the procedure, “so that they’re not actively contracting and recreating creases,” she said. Studies, she noted, have shown that this approach results in better outcomes. She also asks patients to apply a tripeptide serum daily a week or 2 prior to their procedure to stimulate wound healing and collagen remodeling.
For antibiotic and antiviral prophylaxis, Dr. Ortiz typically prescribes doxycycline 100 mg b.i.d. for 7 days and valacyclovir 500 mg b.i.d. for 7 days and asks patients to start the course the night before the procedure. “If they break through the antiviral, I increase to zoster dosing,” she said. “I make sure they have my cell phone number and call me right away if that happens. I don’t routinely prescribe an antifungal, but you can if you want to.”
For anesthesia, Dr. Ortiz applies lidocaine 23%/tetracaine 7% an hour before the procedure and performs nerve blocks at the mentalis, infraorbital, supraorbital, and nasalis muscles. “I also do local infiltration with a three-pronged Mesoram adapter,” she said. “That has changed the comfort level for these patients. I don’t offer any sedation in my practice but that is an option if you have it available. If you’re going to be resurfacing within the orbital rim you need to know how to place corneal shields. Only use injectable lidocaine in this area because if topical lidocaine gets into the eye, it can cause a chemical corneal abrasion. Nothing happens to their vision permanently, but it’s extremely painful for 24-48 hours.”
Dr. Ortiz described postoperative wound care as “the hardest part” of fully ablative laser resurfacing treatments. The treated area will look “bloody and crusty” for 1-2 weeks. She instructs patients to do vinegar soaks four times per day for 2-3 weeks, “depending on how quickly they heal,” she said. She also counsels patients to apply petrolatum ointment to the area and provides them with a bottle of hypochlorous acid spray, an antiseptic – which also helps with the itching they may experience. “They need to avoid the sun, so I recommend full face visors,” she added.
In her clinical experience, postoperative pain medications are not required. “If the patient calls you on day 3 with increased pain, that’s usually a sign of infection; don’t ignore that,” said Dr. Ortiz, who is also president-elect of the American Society for Laser Medicine and Surgery. In a case of suspected infection, she asks the patient to come in right away, and obtains a bacterial culture. “If they break through the doxycycline, it’s usually a gram-negative infection, so I’ll treat them prophylactically for that,” she said.
“Significant itching may be a sign of Candida infection,” she noted. “Because the epidermis has been disrupted, if they have systemic symptoms then you want to consider IV antibiotics because the infection can spread rapidly.”
Dr. Ortiz disclosed having financial relationships with several pharmaceutical and device companies. She is also cochair of the MOAS.
SAN DIEGO – , according to Arisa E. Ortiz, MD.
“Fractional resurfacing is great because there is less downtime, but the results are not as dramatic as with fully ablative resurfacing,” Dr. Ortiz, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual Masters of Aesthetics Symposium. In her practice, she said, “we do a combination,” which can include “fully ablative around the mouth and eyes and fractional everywhere else.”
Key drawbacks to fully ablative laser resurfacing include significant downtime and extensive wound care, “so it’s not for everybody,” she said. Prolonged erythema following treatment is expected, “so patients need to plan for this. It can last 3-4 months, and it will continue to fade and can be covered up with makeup, but it does last a while,” she noted. “One of the things that made ablative resurfacing fall out of favor was the delayed and permanent hypopigmentation where there’s a stark line of demarcation because you can’t treat the neck [with this modality], so patients have this pearly white looking face that appears 6 months after the treatment,” she added.
Preoperatively, Dr. Ortiz asks patients what other cosmetic procedures they have had in the past. For example, if they have had a facelift, they might have neck skin on their jawline, which will react differently to fully ablative resurfacing than facial skin. “I don’t perform fully ablative resurfacing on the neck or body, or in patients with darker skin types,” she said.
To optimize results, she recommends pretreatment of the area with a neuromodulator a week or 2 before the procedure, “so that they’re not actively contracting and recreating creases,” she said. Studies, she noted, have shown that this approach results in better outcomes. She also asks patients to apply a tripeptide serum daily a week or 2 prior to their procedure to stimulate wound healing and collagen remodeling.
For antibiotic and antiviral prophylaxis, Dr. Ortiz typically prescribes doxycycline 100 mg b.i.d. for 7 days and valacyclovir 500 mg b.i.d. for 7 days and asks patients to start the course the night before the procedure. “If they break through the antiviral, I increase to zoster dosing,” she said. “I make sure they have my cell phone number and call me right away if that happens. I don’t routinely prescribe an antifungal, but you can if you want to.”
For anesthesia, Dr. Ortiz applies lidocaine 23%/tetracaine 7% an hour before the procedure and performs nerve blocks at the mentalis, infraorbital, supraorbital, and nasalis muscles. “I also do local infiltration with a three-pronged Mesoram adapter,” she said. “That has changed the comfort level for these patients. I don’t offer any sedation in my practice but that is an option if you have it available. If you’re going to be resurfacing within the orbital rim you need to know how to place corneal shields. Only use injectable lidocaine in this area because if topical lidocaine gets into the eye, it can cause a chemical corneal abrasion. Nothing happens to their vision permanently, but it’s extremely painful for 24-48 hours.”
Dr. Ortiz described postoperative wound care as “the hardest part” of fully ablative laser resurfacing treatments. The treated area will look “bloody and crusty” for 1-2 weeks. She instructs patients to do vinegar soaks four times per day for 2-3 weeks, “depending on how quickly they heal,” she said. She also counsels patients to apply petrolatum ointment to the area and provides them with a bottle of hypochlorous acid spray, an antiseptic – which also helps with the itching they may experience. “They need to avoid the sun, so I recommend full face visors,” she added.
In her clinical experience, postoperative pain medications are not required. “If the patient calls you on day 3 with increased pain, that’s usually a sign of infection; don’t ignore that,” said Dr. Ortiz, who is also president-elect of the American Society for Laser Medicine and Surgery. In a case of suspected infection, she asks the patient to come in right away, and obtains a bacterial culture. “If they break through the doxycycline, it’s usually a gram-negative infection, so I’ll treat them prophylactically for that,” she said.
“Significant itching may be a sign of Candida infection,” she noted. “Because the epidermis has been disrupted, if they have systemic symptoms then you want to consider IV antibiotics because the infection can spread rapidly.”
Dr. Ortiz disclosed having financial relationships with several pharmaceutical and device companies. She is also cochair of the MOAS.
SAN DIEGO – , according to Arisa E. Ortiz, MD.
“Fractional resurfacing is great because there is less downtime, but the results are not as dramatic as with fully ablative resurfacing,” Dr. Ortiz, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual Masters of Aesthetics Symposium. In her practice, she said, “we do a combination,” which can include “fully ablative around the mouth and eyes and fractional everywhere else.”
Key drawbacks to fully ablative laser resurfacing include significant downtime and extensive wound care, “so it’s not for everybody,” she said. Prolonged erythema following treatment is expected, “so patients need to plan for this. It can last 3-4 months, and it will continue to fade and can be covered up with makeup, but it does last a while,” she noted. “One of the things that made ablative resurfacing fall out of favor was the delayed and permanent hypopigmentation where there’s a stark line of demarcation because you can’t treat the neck [with this modality], so patients have this pearly white looking face that appears 6 months after the treatment,” she added.
Preoperatively, Dr. Ortiz asks patients what other cosmetic procedures they have had in the past. For example, if they have had a facelift, they might have neck skin on their jawline, which will react differently to fully ablative resurfacing than facial skin. “I don’t perform fully ablative resurfacing on the neck or body, or in patients with darker skin types,” she said.
To optimize results, she recommends pretreatment of the area with a neuromodulator a week or 2 before the procedure, “so that they’re not actively contracting and recreating creases,” she said. Studies, she noted, have shown that this approach results in better outcomes. She also asks patients to apply a tripeptide serum daily a week or 2 prior to their procedure to stimulate wound healing and collagen remodeling.
For antibiotic and antiviral prophylaxis, Dr. Ortiz typically prescribes doxycycline 100 mg b.i.d. for 7 days and valacyclovir 500 mg b.i.d. for 7 days and asks patients to start the course the night before the procedure. “If they break through the antiviral, I increase to zoster dosing,” she said. “I make sure they have my cell phone number and call me right away if that happens. I don’t routinely prescribe an antifungal, but you can if you want to.”
For anesthesia, Dr. Ortiz applies lidocaine 23%/tetracaine 7% an hour before the procedure and performs nerve blocks at the mentalis, infraorbital, supraorbital, and nasalis muscles. “I also do local infiltration with a three-pronged Mesoram adapter,” she said. “That has changed the comfort level for these patients. I don’t offer any sedation in my practice but that is an option if you have it available. If you’re going to be resurfacing within the orbital rim you need to know how to place corneal shields. Only use injectable lidocaine in this area because if topical lidocaine gets into the eye, it can cause a chemical corneal abrasion. Nothing happens to their vision permanently, but it’s extremely painful for 24-48 hours.”
Dr. Ortiz described postoperative wound care as “the hardest part” of fully ablative laser resurfacing treatments. The treated area will look “bloody and crusty” for 1-2 weeks. She instructs patients to do vinegar soaks four times per day for 2-3 weeks, “depending on how quickly they heal,” she said. She also counsels patients to apply petrolatum ointment to the area and provides them with a bottle of hypochlorous acid spray, an antiseptic – which also helps with the itching they may experience. “They need to avoid the sun, so I recommend full face visors,” she added.
In her clinical experience, postoperative pain medications are not required. “If the patient calls you on day 3 with increased pain, that’s usually a sign of infection; don’t ignore that,” said Dr. Ortiz, who is also president-elect of the American Society for Laser Medicine and Surgery. In a case of suspected infection, she asks the patient to come in right away, and obtains a bacterial culture. “If they break through the doxycycline, it’s usually a gram-negative infection, so I’ll treat them prophylactically for that,” she said.
“Significant itching may be a sign of Candida infection,” she noted. “Because the epidermis has been disrupted, if they have systemic symptoms then you want to consider IV antibiotics because the infection can spread rapidly.”
Dr. Ortiz disclosed having financial relationships with several pharmaceutical and device companies. She is also cochair of the MOAS.
AT MOAS 2023
Thread lifts an option for noninvasive facial tightening
SAN DIEGO – .
In the 1990s, clinicians used nonabsorbable sutures for thread lifts, including polypropylene-barbed threads, which caused adverse events ranging from extrusion and migration to thread expulsion, dimpling, granuloma formation, and prolonged pain, Dr. DiGiorgio, a laser and cosmetic dermatologist who practices in Boston, said at the annual Masters of Aesthetics Symposium. As a result, the Food and Drug Administration withdrew its approval of contour thread aesthetic procedures in 2009. Since then, the development of absorbable threads made from a hybrid of poly-l-lactic acid (PLLA) and polyglycolide/l-lactide (PLGA), and from polydioxanone (PDO) has led to renewed interest in thread lift procedures.
While a surgical facelift remains the gold standard, “we have some options to offer patients for noninvasive tightening,” Dr. DiGiorgio said. “We have devices that provide minimal downtime and are less costly, but results are inconsistent. Thread lifts, or suspension sutures, also have minimal downtime and are less costly, but the [results are] subtle and not long lasting.”
PLGA/PLLA threads consist of an 18% PLGA and 82% PLLA monofilament with bidirectional cones that shift the tissue. They are available in 8, 12, or 16 cones spaced 5-8 mm apart on either side of a 2-cm central cone-free area. “There is a 12-cm, 23-gauge needle on either side of the thread, to allow for insertion,” she explained. “These cones stimulate types I and II collagen, which results in collagenesis. The skin encapsulates the cones, resulting in lasting volume and contour.”
PDO threads, meanwhile, are biodegradable by hydrolysis over 4-8 months. They are inserted with a cannula or a needle and vary based on length, diameter, twined vs. braided, coned vs. barbed, and twisted vs. smooth. “The barbed PDO threads are what I use the most,” Dr. DiGiorgio said. “They provide slight tissue repositioning by anchoring and gripping.”
In 2019, researchers in Korea published results of a study that evaluated the collagen-producing effects of powdered PDO injection, compared with PLLA injection, in a murine model. They found that while both PDO and PLLA induced granulomatous reactions and collagen formation, PDO resulted in slightly more collagen formation than PLLA.
Dr. DiGiorgio, who transitioned to using PDO threads after first using the PLLA/PLGA threads, said that both are effective. “I find PDO threads to be easier. They’re less costly for me, they’re less costly for the patient, and the results are about equivalent.”
Absorbable threads are indicated for the cheek, jawline, neck, lips, forehead, and brow. She finds them most useful “for the lower face, below the nasolabial fold down to the jawline, for improvement of the jowls,” she said. “I don’t think they really work on the neck.”
As with any cosmetic procedure, patient selection is key. According to Dr. DiGiorgio, the patient should have specific and segmental areas of facial laxity amenable to lifting and recontouring along a straight-line vector, adequate dermal thickness, and appropriate expectations for the level of correction. “I like to re-volumize with filler before performing thread lifts to make sure that volume is restored, because you can’t really provide lift to someone with significant volume loss,” she said.
Procedural tips
Prior to the procedure, Dr. DiGiorgio marks the area to be treated while the patient is seated upright and holding a mirror. Then, she pulls back the amount of skin laxity the thread is going to correct. The plane of insertion for barbed threads is at the superficial musculoaponeurotic system (SMAS), and she typically uses 3-4 threads on each side of the face.
“How do you know you’re in the right plane?” If the patient is experiencing significant pain, “you’re too deep, and it’s not going to work,” she said. “You can see if the thread is too superficial as you do more of these.”
After the procedure she asks the patient to sit up prior to trimming the threads. “I take a look in the mirror with them and have them smile and make funny faces to see if there is any dimpling or crimpling, which is probably the most common side effect,” she said. “If I see that, I will pull the thread immediately, so we don’t have a problem. It’s a little uncomfortable to pull the thread but not more uncomfortable than the procedure itself, but I think it’s worth doing to avoid having a dimple or a crimple that can last up to a year.”
In her clinical experience, thread lifts last about 8-10 months. “I find that my patients will come in about once a year for this procedure, and the treated area feels tight afterward,” Dr. DiGiorgio said. “I think that sensation of feeling tight also provides satisfaction to the patient. Results are very subtle. It’s tissue repositioning; it is not a facelift. There’s not really any downtime, but further studies are required to see if threads are safe and effective in the long-term.”
In an interview after the meeting, she noted that the learning curve for thread lifts is variable, as with any new procedure a physician chooses to add to his or her practice. “It’s important to see these patients in follow-up 2 weeks after the procedure consistently, especially when someone first starts performing the procedure,” she recommended. “These patients are usually coming in to see me for other treatments, so I see them at regular 3-month intervals regardless. You begin to get a feel for what angles work and why and how to optimize the results. As with any procedure, the more experience you have performing the procedure will result in improved outcomes and improved management.”
Dr. DiGiorgio disclosed that she has been an advisory board member for Quthero and she holds stock options in the company. She is a consultant for Revelle and has received equipment from Acclaro.
SAN DIEGO – .
In the 1990s, clinicians used nonabsorbable sutures for thread lifts, including polypropylene-barbed threads, which caused adverse events ranging from extrusion and migration to thread expulsion, dimpling, granuloma formation, and prolonged pain, Dr. DiGiorgio, a laser and cosmetic dermatologist who practices in Boston, said at the annual Masters of Aesthetics Symposium. As a result, the Food and Drug Administration withdrew its approval of contour thread aesthetic procedures in 2009. Since then, the development of absorbable threads made from a hybrid of poly-l-lactic acid (PLLA) and polyglycolide/l-lactide (PLGA), and from polydioxanone (PDO) has led to renewed interest in thread lift procedures.
While a surgical facelift remains the gold standard, “we have some options to offer patients for noninvasive tightening,” Dr. DiGiorgio said. “We have devices that provide minimal downtime and are less costly, but results are inconsistent. Thread lifts, or suspension sutures, also have minimal downtime and are less costly, but the [results are] subtle and not long lasting.”
PLGA/PLLA threads consist of an 18% PLGA and 82% PLLA monofilament with bidirectional cones that shift the tissue. They are available in 8, 12, or 16 cones spaced 5-8 mm apart on either side of a 2-cm central cone-free area. “There is a 12-cm, 23-gauge needle on either side of the thread, to allow for insertion,” she explained. “These cones stimulate types I and II collagen, which results in collagenesis. The skin encapsulates the cones, resulting in lasting volume and contour.”
PDO threads, meanwhile, are biodegradable by hydrolysis over 4-8 months. They are inserted with a cannula or a needle and vary based on length, diameter, twined vs. braided, coned vs. barbed, and twisted vs. smooth. “The barbed PDO threads are what I use the most,” Dr. DiGiorgio said. “They provide slight tissue repositioning by anchoring and gripping.”
In 2019, researchers in Korea published results of a study that evaluated the collagen-producing effects of powdered PDO injection, compared with PLLA injection, in a murine model. They found that while both PDO and PLLA induced granulomatous reactions and collagen formation, PDO resulted in slightly more collagen formation than PLLA.
Dr. DiGiorgio, who transitioned to using PDO threads after first using the PLLA/PLGA threads, said that both are effective. “I find PDO threads to be easier. They’re less costly for me, they’re less costly for the patient, and the results are about equivalent.”
Absorbable threads are indicated for the cheek, jawline, neck, lips, forehead, and brow. She finds them most useful “for the lower face, below the nasolabial fold down to the jawline, for improvement of the jowls,” she said. “I don’t think they really work on the neck.”
As with any cosmetic procedure, patient selection is key. According to Dr. DiGiorgio, the patient should have specific and segmental areas of facial laxity amenable to lifting and recontouring along a straight-line vector, adequate dermal thickness, and appropriate expectations for the level of correction. “I like to re-volumize with filler before performing thread lifts to make sure that volume is restored, because you can’t really provide lift to someone with significant volume loss,” she said.
Procedural tips
Prior to the procedure, Dr. DiGiorgio marks the area to be treated while the patient is seated upright and holding a mirror. Then, she pulls back the amount of skin laxity the thread is going to correct. The plane of insertion for barbed threads is at the superficial musculoaponeurotic system (SMAS), and she typically uses 3-4 threads on each side of the face.
“How do you know you’re in the right plane?” If the patient is experiencing significant pain, “you’re too deep, and it’s not going to work,” she said. “You can see if the thread is too superficial as you do more of these.”
After the procedure she asks the patient to sit up prior to trimming the threads. “I take a look in the mirror with them and have them smile and make funny faces to see if there is any dimpling or crimpling, which is probably the most common side effect,” she said. “If I see that, I will pull the thread immediately, so we don’t have a problem. It’s a little uncomfortable to pull the thread but not more uncomfortable than the procedure itself, but I think it’s worth doing to avoid having a dimple or a crimple that can last up to a year.”
In her clinical experience, thread lifts last about 8-10 months. “I find that my patients will come in about once a year for this procedure, and the treated area feels tight afterward,” Dr. DiGiorgio said. “I think that sensation of feeling tight also provides satisfaction to the patient. Results are very subtle. It’s tissue repositioning; it is not a facelift. There’s not really any downtime, but further studies are required to see if threads are safe and effective in the long-term.”
In an interview after the meeting, she noted that the learning curve for thread lifts is variable, as with any new procedure a physician chooses to add to his or her practice. “It’s important to see these patients in follow-up 2 weeks after the procedure consistently, especially when someone first starts performing the procedure,” she recommended. “These patients are usually coming in to see me for other treatments, so I see them at regular 3-month intervals regardless. You begin to get a feel for what angles work and why and how to optimize the results. As with any procedure, the more experience you have performing the procedure will result in improved outcomes and improved management.”
Dr. DiGiorgio disclosed that she has been an advisory board member for Quthero and she holds stock options in the company. She is a consultant for Revelle and has received equipment from Acclaro.
SAN DIEGO – .
In the 1990s, clinicians used nonabsorbable sutures for thread lifts, including polypropylene-barbed threads, which caused adverse events ranging from extrusion and migration to thread expulsion, dimpling, granuloma formation, and prolonged pain, Dr. DiGiorgio, a laser and cosmetic dermatologist who practices in Boston, said at the annual Masters of Aesthetics Symposium. As a result, the Food and Drug Administration withdrew its approval of contour thread aesthetic procedures in 2009. Since then, the development of absorbable threads made from a hybrid of poly-l-lactic acid (PLLA) and polyglycolide/l-lactide (PLGA), and from polydioxanone (PDO) has led to renewed interest in thread lift procedures.
While a surgical facelift remains the gold standard, “we have some options to offer patients for noninvasive tightening,” Dr. DiGiorgio said. “We have devices that provide minimal downtime and are less costly, but results are inconsistent. Thread lifts, or suspension sutures, also have minimal downtime and are less costly, but the [results are] subtle and not long lasting.”
PLGA/PLLA threads consist of an 18% PLGA and 82% PLLA monofilament with bidirectional cones that shift the tissue. They are available in 8, 12, or 16 cones spaced 5-8 mm apart on either side of a 2-cm central cone-free area. “There is a 12-cm, 23-gauge needle on either side of the thread, to allow for insertion,” she explained. “These cones stimulate types I and II collagen, which results in collagenesis. The skin encapsulates the cones, resulting in lasting volume and contour.”
PDO threads, meanwhile, are biodegradable by hydrolysis over 4-8 months. They are inserted with a cannula or a needle and vary based on length, diameter, twined vs. braided, coned vs. barbed, and twisted vs. smooth. “The barbed PDO threads are what I use the most,” Dr. DiGiorgio said. “They provide slight tissue repositioning by anchoring and gripping.”
In 2019, researchers in Korea published results of a study that evaluated the collagen-producing effects of powdered PDO injection, compared with PLLA injection, in a murine model. They found that while both PDO and PLLA induced granulomatous reactions and collagen formation, PDO resulted in slightly more collagen formation than PLLA.
Dr. DiGiorgio, who transitioned to using PDO threads after first using the PLLA/PLGA threads, said that both are effective. “I find PDO threads to be easier. They’re less costly for me, they’re less costly for the patient, and the results are about equivalent.”
Absorbable threads are indicated for the cheek, jawline, neck, lips, forehead, and brow. She finds them most useful “for the lower face, below the nasolabial fold down to the jawline, for improvement of the jowls,” she said. “I don’t think they really work on the neck.”
As with any cosmetic procedure, patient selection is key. According to Dr. DiGiorgio, the patient should have specific and segmental areas of facial laxity amenable to lifting and recontouring along a straight-line vector, adequate dermal thickness, and appropriate expectations for the level of correction. “I like to re-volumize with filler before performing thread lifts to make sure that volume is restored, because you can’t really provide lift to someone with significant volume loss,” she said.
Procedural tips
Prior to the procedure, Dr. DiGiorgio marks the area to be treated while the patient is seated upright and holding a mirror. Then, she pulls back the amount of skin laxity the thread is going to correct. The plane of insertion for barbed threads is at the superficial musculoaponeurotic system (SMAS), and she typically uses 3-4 threads on each side of the face.
“How do you know you’re in the right plane?” If the patient is experiencing significant pain, “you’re too deep, and it’s not going to work,” she said. “You can see if the thread is too superficial as you do more of these.”
After the procedure she asks the patient to sit up prior to trimming the threads. “I take a look in the mirror with them and have them smile and make funny faces to see if there is any dimpling or crimpling, which is probably the most common side effect,” she said. “If I see that, I will pull the thread immediately, so we don’t have a problem. It’s a little uncomfortable to pull the thread but not more uncomfortable than the procedure itself, but I think it’s worth doing to avoid having a dimple or a crimple that can last up to a year.”
In her clinical experience, thread lifts last about 8-10 months. “I find that my patients will come in about once a year for this procedure, and the treated area feels tight afterward,” Dr. DiGiorgio said. “I think that sensation of feeling tight also provides satisfaction to the patient. Results are very subtle. It’s tissue repositioning; it is not a facelift. There’s not really any downtime, but further studies are required to see if threads are safe and effective in the long-term.”
In an interview after the meeting, she noted that the learning curve for thread lifts is variable, as with any new procedure a physician chooses to add to his or her practice. “It’s important to see these patients in follow-up 2 weeks after the procedure consistently, especially when someone first starts performing the procedure,” she recommended. “These patients are usually coming in to see me for other treatments, so I see them at regular 3-month intervals regardless. You begin to get a feel for what angles work and why and how to optimize the results. As with any procedure, the more experience you have performing the procedure will result in improved outcomes and improved management.”
Dr. DiGiorgio disclosed that she has been an advisory board member for Quthero and she holds stock options in the company. She is a consultant for Revelle and has received equipment from Acclaro.
FROM MOAS 2023
Combining lasers: A recipe for maximizing results and patient satisfaction
SAN DIEGO –
“Using a fractional laser as a solo treatment is missing an opportunity to achieve more dramatic improvement for your patients,” Dr. Avram, director of laser, cosmetics, and dermatologic surgery at Massachusetts General Hospital, Boston, said at the annual Masters of Aesthetics Symposium. Among the laser treatments he performs, “combination fractional treatments, typically using the 1927-nm laser” are associated with the highest patient satisfaction, he said.
The order of device use matters, he noted. First, he recommended, use a pulsed dye laser, KTP, or intense pulsed light (IPL) for erythema and telangiectasias, and/or a Q-switched or picosecond laser for pigment. Second, use an ablative or nonablative fractional laser for resurfacing. “A lot of seborrheic keratoses don’t respond to selective photothermolysis well, so I’ll use liquid nitrogen at the time of treatment and before or after treat with a picosecond laser,” added Dr. Avram. “This combined treatment approach is less painful than ablative fractional treatment. You’re going to have downtime anyway, so why not maximize the results at that one treatment session?”
The fractional 1927 laser delivers hundreds of thousands of microscopic pulses and fosters high water absorption, so it targets superficial skin conditions such as actinic keratoses, lentigines, and ephelides at depths of 200-250 microns. It thermally coagulates 30%-40% of skin, which heals without affecting surrounding skin and leaves no perceptible scar, he said.
Clinicians can also combine devices to treat scars. “For red scars, it’s often best to treat both erythema and scar texture with two lasers at the same session,” Dr. Avram said. Again, the order matters. First, he recommended using the pulse dye laser, IPL, or KTP at low fluence and short pulse duration. Second, treat with an ablative or nonablative fractional laser at a low density. “In my experience the ablative fractional lasers are far more efficacious,” he said. “Then we typically add a little Kenalog and 5-FU via laser-assisted drug delivery.”
Dr. Avram disclosed that he has received consulting fees from Allergan. He also reported holding shareholder interest and intellectual property rights with Cytrellis Biosystems.
SAN DIEGO –
“Using a fractional laser as a solo treatment is missing an opportunity to achieve more dramatic improvement for your patients,” Dr. Avram, director of laser, cosmetics, and dermatologic surgery at Massachusetts General Hospital, Boston, said at the annual Masters of Aesthetics Symposium. Among the laser treatments he performs, “combination fractional treatments, typically using the 1927-nm laser” are associated with the highest patient satisfaction, he said.
The order of device use matters, he noted. First, he recommended, use a pulsed dye laser, KTP, or intense pulsed light (IPL) for erythema and telangiectasias, and/or a Q-switched or picosecond laser for pigment. Second, use an ablative or nonablative fractional laser for resurfacing. “A lot of seborrheic keratoses don’t respond to selective photothermolysis well, so I’ll use liquid nitrogen at the time of treatment and before or after treat with a picosecond laser,” added Dr. Avram. “This combined treatment approach is less painful than ablative fractional treatment. You’re going to have downtime anyway, so why not maximize the results at that one treatment session?”
The fractional 1927 laser delivers hundreds of thousands of microscopic pulses and fosters high water absorption, so it targets superficial skin conditions such as actinic keratoses, lentigines, and ephelides at depths of 200-250 microns. It thermally coagulates 30%-40% of skin, which heals without affecting surrounding skin and leaves no perceptible scar, he said.
Clinicians can also combine devices to treat scars. “For red scars, it’s often best to treat both erythema and scar texture with two lasers at the same session,” Dr. Avram said. Again, the order matters. First, he recommended using the pulse dye laser, IPL, or KTP at low fluence and short pulse duration. Second, treat with an ablative or nonablative fractional laser at a low density. “In my experience the ablative fractional lasers are far more efficacious,” he said. “Then we typically add a little Kenalog and 5-FU via laser-assisted drug delivery.”
Dr. Avram disclosed that he has received consulting fees from Allergan. He also reported holding shareholder interest and intellectual property rights with Cytrellis Biosystems.
SAN DIEGO –
“Using a fractional laser as a solo treatment is missing an opportunity to achieve more dramatic improvement for your patients,” Dr. Avram, director of laser, cosmetics, and dermatologic surgery at Massachusetts General Hospital, Boston, said at the annual Masters of Aesthetics Symposium. Among the laser treatments he performs, “combination fractional treatments, typically using the 1927-nm laser” are associated with the highest patient satisfaction, he said.
The order of device use matters, he noted. First, he recommended, use a pulsed dye laser, KTP, or intense pulsed light (IPL) for erythema and telangiectasias, and/or a Q-switched or picosecond laser for pigment. Second, use an ablative or nonablative fractional laser for resurfacing. “A lot of seborrheic keratoses don’t respond to selective photothermolysis well, so I’ll use liquid nitrogen at the time of treatment and before or after treat with a picosecond laser,” added Dr. Avram. “This combined treatment approach is less painful than ablative fractional treatment. You’re going to have downtime anyway, so why not maximize the results at that one treatment session?”
The fractional 1927 laser delivers hundreds of thousands of microscopic pulses and fosters high water absorption, so it targets superficial skin conditions such as actinic keratoses, lentigines, and ephelides at depths of 200-250 microns. It thermally coagulates 30%-40% of skin, which heals without affecting surrounding skin and leaves no perceptible scar, he said.
Clinicians can also combine devices to treat scars. “For red scars, it’s often best to treat both erythema and scar texture with two lasers at the same session,” Dr. Avram said. Again, the order matters. First, he recommended using the pulse dye laser, IPL, or KTP at low fluence and short pulse duration. Second, treat with an ablative or nonablative fractional laser at a low density. “In my experience the ablative fractional lasers are far more efficacious,” he said. “Then we typically add a little Kenalog and 5-FU via laser-assisted drug delivery.”
Dr. Avram disclosed that he has received consulting fees from Allergan. He also reported holding shareholder interest and intellectual property rights with Cytrellis Biosystems.
AT MOAS 2023
When treating scars, ‘rehabilitation’ is the goal, not perfection
SAN DIEGO – , according to Victor Ross, MD.
“A lot of lip service is paid to how to inject the steroid,” Dr. Ross, director of laser and cosmetic dermatology at the Scripps Clinic in San Diego, said at the annual Masters of Aesthetics Symposium. “The most important part is the amount and the fastidiousness that you have injecting. You should see the tip of the needle and be very slow. Use a 1 cc syringe.” He used to inject scars with triamcinolone acetate 40 mg/mL, but now he almost always injects 10-20 mg/mL to avoid inducing white streak-like atrophy or hypopigmentation around the treated area.
“When you treat a scar, you treat the features of the scar that make it stand out,” Dr. Ross continued. “If it’s red, you address the hyperemia. If it’s brown, you address the pigment. You want to have a reasonable pathophysiological basis for what you’re doing. Understand how the scar got there and have a reasonable algorithm.” When he counsels patients about clinical outcomes to expect, he emphasizes rehabilitation instead of blemish-free perfection. “It’s not making the scar go away,” he said. “It’s not restoring completely normal skin form and function; it’s a restorative effort to get toward normality. That’s what it’s all about.”
Besides injecting scars with triamcinolone acetate, other scar treatment options include intralesional 5-fluorouracil, oral antihistamines, COX-2 inhibitors, hydrogel sheeting, compression, acoustic wave therapy, photodynamic therapy, radiofrequency, and lasers. “I’m not a big fan of low-level light; it probably does something [to scars], but I’m skeptical,” Dr. Ross said.
In his clinical opinion, most scars respond best to treatments with ablative and nonablative fractional lasers tuned to gentle settings such as an energy level of 20 millijoules at a density of 5%-10%. “Every scar deserves a chance for laser remediation and rehabilitation,” he said. “With radiation scars you want to be particularly gentle. If you have a Mohs scar that has been subsequently treated with radiation, I would lower my settings by half, because I’ve had some scars worsen with settings for red scars after radiation therapy.”
He often uses fractional lasers for stubborn acne scarring. “The hyperemic component you can treat with a vascular laser, then come back [and treat the scarring] with a nonablative fractional laser, or you could use radiofrequency microneedling as well,” Dr. Ross said.
New or innovative scar treatments coming down the pike, he said, include the following: mitomycin C (applied topically, he said that this has worked well for postoperative keloids), tamoxifen, oral methotrexate, imiquimod (which has mixed results to date), platelet-rich plasma, and retinoids.
Dr. Ross disclosed having research and financial ties to numerous pharmaceutical and device companies.
SAN DIEGO – , according to Victor Ross, MD.
“A lot of lip service is paid to how to inject the steroid,” Dr. Ross, director of laser and cosmetic dermatology at the Scripps Clinic in San Diego, said at the annual Masters of Aesthetics Symposium. “The most important part is the amount and the fastidiousness that you have injecting. You should see the tip of the needle and be very slow. Use a 1 cc syringe.” He used to inject scars with triamcinolone acetate 40 mg/mL, but now he almost always injects 10-20 mg/mL to avoid inducing white streak-like atrophy or hypopigmentation around the treated area.
“When you treat a scar, you treat the features of the scar that make it stand out,” Dr. Ross continued. “If it’s red, you address the hyperemia. If it’s brown, you address the pigment. You want to have a reasonable pathophysiological basis for what you’re doing. Understand how the scar got there and have a reasonable algorithm.” When he counsels patients about clinical outcomes to expect, he emphasizes rehabilitation instead of blemish-free perfection. “It’s not making the scar go away,” he said. “It’s not restoring completely normal skin form and function; it’s a restorative effort to get toward normality. That’s what it’s all about.”
Besides injecting scars with triamcinolone acetate, other scar treatment options include intralesional 5-fluorouracil, oral antihistamines, COX-2 inhibitors, hydrogel sheeting, compression, acoustic wave therapy, photodynamic therapy, radiofrequency, and lasers. “I’m not a big fan of low-level light; it probably does something [to scars], but I’m skeptical,” Dr. Ross said.
In his clinical opinion, most scars respond best to treatments with ablative and nonablative fractional lasers tuned to gentle settings such as an energy level of 20 millijoules at a density of 5%-10%. “Every scar deserves a chance for laser remediation and rehabilitation,” he said. “With radiation scars you want to be particularly gentle. If you have a Mohs scar that has been subsequently treated with radiation, I would lower my settings by half, because I’ve had some scars worsen with settings for red scars after radiation therapy.”
He often uses fractional lasers for stubborn acne scarring. “The hyperemic component you can treat with a vascular laser, then come back [and treat the scarring] with a nonablative fractional laser, or you could use radiofrequency microneedling as well,” Dr. Ross said.
New or innovative scar treatments coming down the pike, he said, include the following: mitomycin C (applied topically, he said that this has worked well for postoperative keloids), tamoxifen, oral methotrexate, imiquimod (which has mixed results to date), platelet-rich plasma, and retinoids.
Dr. Ross disclosed having research and financial ties to numerous pharmaceutical and device companies.
SAN DIEGO – , according to Victor Ross, MD.
“A lot of lip service is paid to how to inject the steroid,” Dr. Ross, director of laser and cosmetic dermatology at the Scripps Clinic in San Diego, said at the annual Masters of Aesthetics Symposium. “The most important part is the amount and the fastidiousness that you have injecting. You should see the tip of the needle and be very slow. Use a 1 cc syringe.” He used to inject scars with triamcinolone acetate 40 mg/mL, but now he almost always injects 10-20 mg/mL to avoid inducing white streak-like atrophy or hypopigmentation around the treated area.
“When you treat a scar, you treat the features of the scar that make it stand out,” Dr. Ross continued. “If it’s red, you address the hyperemia. If it’s brown, you address the pigment. You want to have a reasonable pathophysiological basis for what you’re doing. Understand how the scar got there and have a reasonable algorithm.” When he counsels patients about clinical outcomes to expect, he emphasizes rehabilitation instead of blemish-free perfection. “It’s not making the scar go away,” he said. “It’s not restoring completely normal skin form and function; it’s a restorative effort to get toward normality. That’s what it’s all about.”
Besides injecting scars with triamcinolone acetate, other scar treatment options include intralesional 5-fluorouracil, oral antihistamines, COX-2 inhibitors, hydrogel sheeting, compression, acoustic wave therapy, photodynamic therapy, radiofrequency, and lasers. “I’m not a big fan of low-level light; it probably does something [to scars], but I’m skeptical,” Dr. Ross said.
In his clinical opinion, most scars respond best to treatments with ablative and nonablative fractional lasers tuned to gentle settings such as an energy level of 20 millijoules at a density of 5%-10%. “Every scar deserves a chance for laser remediation and rehabilitation,” he said. “With radiation scars you want to be particularly gentle. If you have a Mohs scar that has been subsequently treated with radiation, I would lower my settings by half, because I’ve had some scars worsen with settings for red scars after radiation therapy.”
He often uses fractional lasers for stubborn acne scarring. “The hyperemic component you can treat with a vascular laser, then come back [and treat the scarring] with a nonablative fractional laser, or you could use radiofrequency microneedling as well,” Dr. Ross said.
New or innovative scar treatments coming down the pike, he said, include the following: mitomycin C (applied topically, he said that this has worked well for postoperative keloids), tamoxifen, oral methotrexate, imiquimod (which has mixed results to date), platelet-rich plasma, and retinoids.
Dr. Ross disclosed having research and financial ties to numerous pharmaceutical and device companies.
FROM MOAS 2023
Skin has different daytime and nighttime needs, emerging circadian research suggests
SAN DIEGO –
“Paying attention to the circadian rhythm of the skin is every bit as important as moisturizing the skin,” Dr. Shamban, a dermatologist who practices in Santa Monica, Calif., said at the annual Masters of Aesthetics Symposium. “It is paramount to both your morning and evening skin regimen routine,” she added.
Circadian rhythms are physical, mental, and behavioral changes that follow a 24-hour cycle. “These natural processes respond primarily to light and dark and affect most living things, including animals, plants, and microbes,” she said. “The circadian system is composed of peripheral circadian oscillators in many other cells, including the skin.”
The science has been around awhile, but dermatologists didn’t understand its impact until recently, she said.
In 1729, the French astronomer Jean-Jacques d’Ortous de Mairan demonstrated that mimosa leaves, which open at dawn and close at dusk, continued this cycle even when kept in darkness. In the 1970s, Seymour Benzer and Ronald Konopka showed that mutations in an unknown gene disrupted the circadian clock of fruit flies.
And in 2017, the Nobel Prize in Physiology or Medicine was awarded to Jeffrey C. Hall, Michael Rosbash, and Michael W. Young for discovering molecular mechanisms that control circadian rhythm. Using fruit flies as a model, they isolated a gene that controls the normal daily biological rhythm.
“They showed that this gene encodes a protein that accumulates in the cell during the night and is then degraded during the day, and they identified additional protein components, exposing the mechanism governing the self-sustaining clockwork inside the cell,” said Dr. Shamban.
In humans and other mammals, the primary body clock is located in the suprachiasmatic nucleus, a cluster of approximately 10,000 neurons located on either side of the midline above the optic chiasma, about 3 cm behind the eyes. Several clock genes have been identified that regulate and control transcription and translation.
“Expression of these core clock genes inside the cell influences many signaling pathways, which allows the cells to identify the time of day and perform their appropriate function,” Dr. Shamban said. “Furthermore, phosphorylation of core clock proteins leads to degradation to keep the 24-hour cycle in sync.”
Photoreceptive molecules known as opsins also appear to play a role in regulating the skin’s clock. A systematic review of 22 articles published in 2020 found that opsins are present in keratinocytes, melanocytes, dermal fibroblasts, and hair follicle cells, and they have been shown to mediate wound healing, melanogenesis, hair growth, and skin photoaging in human and nonhuman species.
“You may wonder, why does the skin respond so nicely to light?” Dr. Shamban said. “Because it contains opsins, and light exposure through opsin-regulated pathways stimulates melanin production.”
Patients can support their skin’s clock genes by understanding that skin barrier functions such as photoprotection and sebum production are increased during the day, while skin permeability processes such as DNA repair, cell proliferation, and blood flow are enhanced at night.
“Your skin has different daytime and nighttime needs,” Dr. Shamban commented. “Simply put, daytime is defense, and nighttime is offense. I think we’ve known this intuitively, but to know that there is science supporting this idea is important.”
Dr. Shamban wrote the book “Heal Your Skin: The Breakthrough Plan for Renewal” (Wiley, 2011). She disclosed that she conducts clinical trials for many pharmaceutical and device companies.
SAN DIEGO –
“Paying attention to the circadian rhythm of the skin is every bit as important as moisturizing the skin,” Dr. Shamban, a dermatologist who practices in Santa Monica, Calif., said at the annual Masters of Aesthetics Symposium. “It is paramount to both your morning and evening skin regimen routine,” she added.
Circadian rhythms are physical, mental, and behavioral changes that follow a 24-hour cycle. “These natural processes respond primarily to light and dark and affect most living things, including animals, plants, and microbes,” she said. “The circadian system is composed of peripheral circadian oscillators in many other cells, including the skin.”
The science has been around awhile, but dermatologists didn’t understand its impact until recently, she said.
In 1729, the French astronomer Jean-Jacques d’Ortous de Mairan demonstrated that mimosa leaves, which open at dawn and close at dusk, continued this cycle even when kept in darkness. In the 1970s, Seymour Benzer and Ronald Konopka showed that mutations in an unknown gene disrupted the circadian clock of fruit flies.
And in 2017, the Nobel Prize in Physiology or Medicine was awarded to Jeffrey C. Hall, Michael Rosbash, and Michael W. Young for discovering molecular mechanisms that control circadian rhythm. Using fruit flies as a model, they isolated a gene that controls the normal daily biological rhythm.
“They showed that this gene encodes a protein that accumulates in the cell during the night and is then degraded during the day, and they identified additional protein components, exposing the mechanism governing the self-sustaining clockwork inside the cell,” said Dr. Shamban.
In humans and other mammals, the primary body clock is located in the suprachiasmatic nucleus, a cluster of approximately 10,000 neurons located on either side of the midline above the optic chiasma, about 3 cm behind the eyes. Several clock genes have been identified that regulate and control transcription and translation.
“Expression of these core clock genes inside the cell influences many signaling pathways, which allows the cells to identify the time of day and perform their appropriate function,” Dr. Shamban said. “Furthermore, phosphorylation of core clock proteins leads to degradation to keep the 24-hour cycle in sync.”
Photoreceptive molecules known as opsins also appear to play a role in regulating the skin’s clock. A systematic review of 22 articles published in 2020 found that opsins are present in keratinocytes, melanocytes, dermal fibroblasts, and hair follicle cells, and they have been shown to mediate wound healing, melanogenesis, hair growth, and skin photoaging in human and nonhuman species.
“You may wonder, why does the skin respond so nicely to light?” Dr. Shamban said. “Because it contains opsins, and light exposure through opsin-regulated pathways stimulates melanin production.”
Patients can support their skin’s clock genes by understanding that skin barrier functions such as photoprotection and sebum production are increased during the day, while skin permeability processes such as DNA repair, cell proliferation, and blood flow are enhanced at night.
“Your skin has different daytime and nighttime needs,” Dr. Shamban commented. “Simply put, daytime is defense, and nighttime is offense. I think we’ve known this intuitively, but to know that there is science supporting this idea is important.”
Dr. Shamban wrote the book “Heal Your Skin: The Breakthrough Plan for Renewal” (Wiley, 2011). She disclosed that she conducts clinical trials for many pharmaceutical and device companies.
SAN DIEGO –
“Paying attention to the circadian rhythm of the skin is every bit as important as moisturizing the skin,” Dr. Shamban, a dermatologist who practices in Santa Monica, Calif., said at the annual Masters of Aesthetics Symposium. “It is paramount to both your morning and evening skin regimen routine,” she added.
Circadian rhythms are physical, mental, and behavioral changes that follow a 24-hour cycle. “These natural processes respond primarily to light and dark and affect most living things, including animals, plants, and microbes,” she said. “The circadian system is composed of peripheral circadian oscillators in many other cells, including the skin.”
The science has been around awhile, but dermatologists didn’t understand its impact until recently, she said.
In 1729, the French astronomer Jean-Jacques d’Ortous de Mairan demonstrated that mimosa leaves, which open at dawn and close at dusk, continued this cycle even when kept in darkness. In the 1970s, Seymour Benzer and Ronald Konopka showed that mutations in an unknown gene disrupted the circadian clock of fruit flies.
And in 2017, the Nobel Prize in Physiology or Medicine was awarded to Jeffrey C. Hall, Michael Rosbash, and Michael W. Young for discovering molecular mechanisms that control circadian rhythm. Using fruit flies as a model, they isolated a gene that controls the normal daily biological rhythm.
“They showed that this gene encodes a protein that accumulates in the cell during the night and is then degraded during the day, and they identified additional protein components, exposing the mechanism governing the self-sustaining clockwork inside the cell,” said Dr. Shamban.
In humans and other mammals, the primary body clock is located in the suprachiasmatic nucleus, a cluster of approximately 10,000 neurons located on either side of the midline above the optic chiasma, about 3 cm behind the eyes. Several clock genes have been identified that regulate and control transcription and translation.
“Expression of these core clock genes inside the cell influences many signaling pathways, which allows the cells to identify the time of day and perform their appropriate function,” Dr. Shamban said. “Furthermore, phosphorylation of core clock proteins leads to degradation to keep the 24-hour cycle in sync.”
Photoreceptive molecules known as opsins also appear to play a role in regulating the skin’s clock. A systematic review of 22 articles published in 2020 found that opsins are present in keratinocytes, melanocytes, dermal fibroblasts, and hair follicle cells, and they have been shown to mediate wound healing, melanogenesis, hair growth, and skin photoaging in human and nonhuman species.
“You may wonder, why does the skin respond so nicely to light?” Dr. Shamban said. “Because it contains opsins, and light exposure through opsin-regulated pathways stimulates melanin production.”
Patients can support their skin’s clock genes by understanding that skin barrier functions such as photoprotection and sebum production are increased during the day, while skin permeability processes such as DNA repair, cell proliferation, and blood flow are enhanced at night.
“Your skin has different daytime and nighttime needs,” Dr. Shamban commented. “Simply put, daytime is defense, and nighttime is offense. I think we’ve known this intuitively, but to know that there is science supporting this idea is important.”
Dr. Shamban wrote the book “Heal Your Skin: The Breakthrough Plan for Renewal” (Wiley, 2011). She disclosed that she conducts clinical trials for many pharmaceutical and device companies.
AT MOAS 2023
CoolSculpting remains most popular procedure for noninvasive fat removal, expert says
SAN DIEGO –, some aesthetic experts wondered how consumers would embrace the fat reduction procedure going forward.
The negative publicity surrounding this case “is thought to have detracted from some of the volume of it [in terms of demand], but it looks like it’s coming back again,” Omar A. Ibrahimi, MD, PhD, medical director of the Connecticut Skin Institute, Stamford, said during a presentation on noninvasive fat removal treatment options at the annual Masters of Aesthetics Symposium.
In fact, he said, CoolSculpting accounts for an estimated 72% of noninvasive fat removal treatments performed in the United States. “By and large, there is high satisfaction with this procedure,” said Dr. Ibrahimi. “There have been about 17 million procedures done worldwide. Paradoxical adipose hyperplasia is a very rare side effect. As newer iterations of this technology have come out, I think there is an even lower incidence.”
CoolSculpting, or cryolipolysis, freezes excess fat to remove it from stubborn areas via panniculitis. The technology was developed by Dieter Manstein MD, PhD, and R. Rox Anderson, MD, at Massachusetts General Hospital and Harvard Medical School, both in Boston, and cleared by the U.S. Food and Drug Administration for noninvasive fat removal in 2010.
“If you kill a fat cell in an adult, it can’t come back,” Dr. Ibrahimi said. “When this technology first came out it was very simple. We treated an area once and were done. Now we know to treat the area multiple times, and you can treat a much larger volume in a patient during one session safely. You can bring about dramatic results, but it often takes a series of 35-minute treatment cycles and about 3 months to see clinical results. There are published studies showing that results are persisting even 10 years after treatment. This is nice, because I tell my patients, ‘if you keep up with your diet and exercise, we don’t expect the fat to come back.’ ”
Other noninvasive options for fat removal include the following:
- Ultrasound. Options include high-intensity focused ultrasound (Liposonix) and pulsed focused ultrasound (UltraShape). Dr. Ibrahimi described these devices as “very painful, and the results were very difficult to reproduce from the initial clinical studies.”
- Low-level light therapy. Early devices on the market include Zerona and UltraSlim. “Oftentimes these lacked any sort of histological analysis,” he said. “There was no obvious mechanism of action, and questionable efficacy.”
- Laser. Powered by a 1060-nm laser, SculpSure can reduce fat cells safely in 25-minute treatment sessions, Dr. Ibrahimi said. Each session is delivered with one of four available applicators and involves 4 minutes of heating and the next 21 minutes alternating between heating and cooling. “You’re trying to reach a target temperature that kills fat cells,” he explained. “The beauty of having these applicators is that you can kind of customize to the individual patient; it uses contact cooling, and it’s safe for all Fitzpatrick skin types. This device results in a 10%-12% reduction in fat, so it’s clinically significant but very modest.”
A robotic version of the technology, known as the Robotic Fat Killer, is also available. So is the EON, a touchless 1064-nm laser FDA cleared for abdominal, flank, thigh, and back fat reduction. “It adapts to the body shape of the area and individual to deliver a customized treatment,” Dr. Ibrahimi said.
- Radiofrequency. Most devices on the market, such as truSculpt and Vanquish, are powered by monopolar radiofrequency (RF) energy. “Similar to the 1060-nm laser, you can customize these treatments,” he said. “You’re treating to a target temperature. It involves 15-minute cycles, and there are clinical, histology, and ultrasound data supporting this technology.”
Dr. Ibrahimi uses truSculpt and CoolSculpting in his practice, “but sometimes you have patients who are ‘too fit’ for CoolSculpting; they don’t fit the handpiece perfectly,” he said. “That’s where having a monopolar RF or a 1060-nm laser is useful, to help you hone in on those stubborn pockets of fat.”
- Deoxycholic acid. While not a device, deoxycholic acid (Kybella), administered subcutaneously, is approved by the FDA for improving “the appearance of moderate to severe convexity or fullness associated with submental fat” in adults. “A lot of people use it off-label on the abdomen and other stubborn areas,” Dr. Ibrahimi said. “It often requires a series of treatments. That’s the biggest limiting issue with using this technology. It works well, but compared to CoolSculpting, there is a lot of swelling and bruising, which you would expect with an injectable. Managing that down time and hand holding is difficult. But if you can get patients to buy into the downtime, [it yields] pretty impressive results.”
Dr. Ibrahimi also discussed the promise of electrical muscle stimulation for strengthening, firming, and toning muscles. The technology applies an electrical current through electrodes placed on the skin, which stimulates muscles, or through an electromagnetic field.
In a published study of 45 men and women, Dr. Ibrahimi, Anne Chapas, MD, medical director of UnionDerm in New York, and colleagues evaluated the safety and efficacy of an electrical muscle stimulation system for improving muscle strength and toning of the upper extremities.
For the treatments, they used disposable contact pads to place pairs of electrodes on the biceps and on the triceps. All patients (median age 42) received 30-minute treatments twice weekly for 2 or 3 weeks, corresponding to four or six total sessions respectively, depending on the study site. Follow-ups were conducted 30 and 90 days after treatment. They used a validated dynamometer device to measure strength at baseline, at the final treatment session, and at the post-treatment 30- and 90-day visits.
“We saw about a 40% increase in strength in the biceps and about a 30% increase in strength in the triceps,” Dr. Ibrahimi said. “Interestingly, the effect got greater at 30 and 90 days, so this is something that lingers on for quite a while.” In addition to the increase in strength, the researchers and patients noted an improvement in the appearance of the arms. He predicted that this technology “is going to play a role in functional medicine and getting injured athletes back to their sports faster.”
Dr. Ibrahimi disclosed that he is a member of the Advisory Board for Accure Acne, AbbVie, Cutera (manufacturer of truSculpt), Lutronic, Blueberry Therapeutics, Cytrellis, and Quthero. He also holds stock in many device and pharmaceutical companies (none are relevant to the treatments mentioned in this story).
SAN DIEGO –, some aesthetic experts wondered how consumers would embrace the fat reduction procedure going forward.
The negative publicity surrounding this case “is thought to have detracted from some of the volume of it [in terms of demand], but it looks like it’s coming back again,” Omar A. Ibrahimi, MD, PhD, medical director of the Connecticut Skin Institute, Stamford, said during a presentation on noninvasive fat removal treatment options at the annual Masters of Aesthetics Symposium.
In fact, he said, CoolSculpting accounts for an estimated 72% of noninvasive fat removal treatments performed in the United States. “By and large, there is high satisfaction with this procedure,” said Dr. Ibrahimi. “There have been about 17 million procedures done worldwide. Paradoxical adipose hyperplasia is a very rare side effect. As newer iterations of this technology have come out, I think there is an even lower incidence.”
CoolSculpting, or cryolipolysis, freezes excess fat to remove it from stubborn areas via panniculitis. The technology was developed by Dieter Manstein MD, PhD, and R. Rox Anderson, MD, at Massachusetts General Hospital and Harvard Medical School, both in Boston, and cleared by the U.S. Food and Drug Administration for noninvasive fat removal in 2010.
“If you kill a fat cell in an adult, it can’t come back,” Dr. Ibrahimi said. “When this technology first came out it was very simple. We treated an area once and were done. Now we know to treat the area multiple times, and you can treat a much larger volume in a patient during one session safely. You can bring about dramatic results, but it often takes a series of 35-minute treatment cycles and about 3 months to see clinical results. There are published studies showing that results are persisting even 10 years after treatment. This is nice, because I tell my patients, ‘if you keep up with your diet and exercise, we don’t expect the fat to come back.’ ”
Other noninvasive options for fat removal include the following:
- Ultrasound. Options include high-intensity focused ultrasound (Liposonix) and pulsed focused ultrasound (UltraShape). Dr. Ibrahimi described these devices as “very painful, and the results were very difficult to reproduce from the initial clinical studies.”
- Low-level light therapy. Early devices on the market include Zerona and UltraSlim. “Oftentimes these lacked any sort of histological analysis,” he said. “There was no obvious mechanism of action, and questionable efficacy.”
- Laser. Powered by a 1060-nm laser, SculpSure can reduce fat cells safely in 25-minute treatment sessions, Dr. Ibrahimi said. Each session is delivered with one of four available applicators and involves 4 minutes of heating and the next 21 minutes alternating between heating and cooling. “You’re trying to reach a target temperature that kills fat cells,” he explained. “The beauty of having these applicators is that you can kind of customize to the individual patient; it uses contact cooling, and it’s safe for all Fitzpatrick skin types. This device results in a 10%-12% reduction in fat, so it’s clinically significant but very modest.”
A robotic version of the technology, known as the Robotic Fat Killer, is also available. So is the EON, a touchless 1064-nm laser FDA cleared for abdominal, flank, thigh, and back fat reduction. “It adapts to the body shape of the area and individual to deliver a customized treatment,” Dr. Ibrahimi said.
- Radiofrequency. Most devices on the market, such as truSculpt and Vanquish, are powered by monopolar radiofrequency (RF) energy. “Similar to the 1060-nm laser, you can customize these treatments,” he said. “You’re treating to a target temperature. It involves 15-minute cycles, and there are clinical, histology, and ultrasound data supporting this technology.”
Dr. Ibrahimi uses truSculpt and CoolSculpting in his practice, “but sometimes you have patients who are ‘too fit’ for CoolSculpting; they don’t fit the handpiece perfectly,” he said. “That’s where having a monopolar RF or a 1060-nm laser is useful, to help you hone in on those stubborn pockets of fat.”
- Deoxycholic acid. While not a device, deoxycholic acid (Kybella), administered subcutaneously, is approved by the FDA for improving “the appearance of moderate to severe convexity or fullness associated with submental fat” in adults. “A lot of people use it off-label on the abdomen and other stubborn areas,” Dr. Ibrahimi said. “It often requires a series of treatments. That’s the biggest limiting issue with using this technology. It works well, but compared to CoolSculpting, there is a lot of swelling and bruising, which you would expect with an injectable. Managing that down time and hand holding is difficult. But if you can get patients to buy into the downtime, [it yields] pretty impressive results.”
Dr. Ibrahimi also discussed the promise of electrical muscle stimulation for strengthening, firming, and toning muscles. The technology applies an electrical current through electrodes placed on the skin, which stimulates muscles, or through an electromagnetic field.
In a published study of 45 men and women, Dr. Ibrahimi, Anne Chapas, MD, medical director of UnionDerm in New York, and colleagues evaluated the safety and efficacy of an electrical muscle stimulation system for improving muscle strength and toning of the upper extremities.
For the treatments, they used disposable contact pads to place pairs of electrodes on the biceps and on the triceps. All patients (median age 42) received 30-minute treatments twice weekly for 2 or 3 weeks, corresponding to four or six total sessions respectively, depending on the study site. Follow-ups were conducted 30 and 90 days after treatment. They used a validated dynamometer device to measure strength at baseline, at the final treatment session, and at the post-treatment 30- and 90-day visits.
“We saw about a 40% increase in strength in the biceps and about a 30% increase in strength in the triceps,” Dr. Ibrahimi said. “Interestingly, the effect got greater at 30 and 90 days, so this is something that lingers on for quite a while.” In addition to the increase in strength, the researchers and patients noted an improvement in the appearance of the arms. He predicted that this technology “is going to play a role in functional medicine and getting injured athletes back to their sports faster.”
Dr. Ibrahimi disclosed that he is a member of the Advisory Board for Accure Acne, AbbVie, Cutera (manufacturer of truSculpt), Lutronic, Blueberry Therapeutics, Cytrellis, and Quthero. He also holds stock in many device and pharmaceutical companies (none are relevant to the treatments mentioned in this story).
SAN DIEGO –, some aesthetic experts wondered how consumers would embrace the fat reduction procedure going forward.
The negative publicity surrounding this case “is thought to have detracted from some of the volume of it [in terms of demand], but it looks like it’s coming back again,” Omar A. Ibrahimi, MD, PhD, medical director of the Connecticut Skin Institute, Stamford, said during a presentation on noninvasive fat removal treatment options at the annual Masters of Aesthetics Symposium.
In fact, he said, CoolSculpting accounts for an estimated 72% of noninvasive fat removal treatments performed in the United States. “By and large, there is high satisfaction with this procedure,” said Dr. Ibrahimi. “There have been about 17 million procedures done worldwide. Paradoxical adipose hyperplasia is a very rare side effect. As newer iterations of this technology have come out, I think there is an even lower incidence.”
CoolSculpting, or cryolipolysis, freezes excess fat to remove it from stubborn areas via panniculitis. The technology was developed by Dieter Manstein MD, PhD, and R. Rox Anderson, MD, at Massachusetts General Hospital and Harvard Medical School, both in Boston, and cleared by the U.S. Food and Drug Administration for noninvasive fat removal in 2010.
“If you kill a fat cell in an adult, it can’t come back,” Dr. Ibrahimi said. “When this technology first came out it was very simple. We treated an area once and were done. Now we know to treat the area multiple times, and you can treat a much larger volume in a patient during one session safely. You can bring about dramatic results, but it often takes a series of 35-minute treatment cycles and about 3 months to see clinical results. There are published studies showing that results are persisting even 10 years after treatment. This is nice, because I tell my patients, ‘if you keep up with your diet and exercise, we don’t expect the fat to come back.’ ”
Other noninvasive options for fat removal include the following:
- Ultrasound. Options include high-intensity focused ultrasound (Liposonix) and pulsed focused ultrasound (UltraShape). Dr. Ibrahimi described these devices as “very painful, and the results were very difficult to reproduce from the initial clinical studies.”
- Low-level light therapy. Early devices on the market include Zerona and UltraSlim. “Oftentimes these lacked any sort of histological analysis,” he said. “There was no obvious mechanism of action, and questionable efficacy.”
- Laser. Powered by a 1060-nm laser, SculpSure can reduce fat cells safely in 25-minute treatment sessions, Dr. Ibrahimi said. Each session is delivered with one of four available applicators and involves 4 minutes of heating and the next 21 minutes alternating between heating and cooling. “You’re trying to reach a target temperature that kills fat cells,” he explained. “The beauty of having these applicators is that you can kind of customize to the individual patient; it uses contact cooling, and it’s safe for all Fitzpatrick skin types. This device results in a 10%-12% reduction in fat, so it’s clinically significant but very modest.”
A robotic version of the technology, known as the Robotic Fat Killer, is also available. So is the EON, a touchless 1064-nm laser FDA cleared for abdominal, flank, thigh, and back fat reduction. “It adapts to the body shape of the area and individual to deliver a customized treatment,” Dr. Ibrahimi said.
- Radiofrequency. Most devices on the market, such as truSculpt and Vanquish, are powered by monopolar radiofrequency (RF) energy. “Similar to the 1060-nm laser, you can customize these treatments,” he said. “You’re treating to a target temperature. It involves 15-minute cycles, and there are clinical, histology, and ultrasound data supporting this technology.”
Dr. Ibrahimi uses truSculpt and CoolSculpting in his practice, “but sometimes you have patients who are ‘too fit’ for CoolSculpting; they don’t fit the handpiece perfectly,” he said. “That’s where having a monopolar RF or a 1060-nm laser is useful, to help you hone in on those stubborn pockets of fat.”
- Deoxycholic acid. While not a device, deoxycholic acid (Kybella), administered subcutaneously, is approved by the FDA for improving “the appearance of moderate to severe convexity or fullness associated with submental fat” in adults. “A lot of people use it off-label on the abdomen and other stubborn areas,” Dr. Ibrahimi said. “It often requires a series of treatments. That’s the biggest limiting issue with using this technology. It works well, but compared to CoolSculpting, there is a lot of swelling and bruising, which you would expect with an injectable. Managing that down time and hand holding is difficult. But if you can get patients to buy into the downtime, [it yields] pretty impressive results.”
Dr. Ibrahimi also discussed the promise of electrical muscle stimulation for strengthening, firming, and toning muscles. The technology applies an electrical current through electrodes placed on the skin, which stimulates muscles, or through an electromagnetic field.
In a published study of 45 men and women, Dr. Ibrahimi, Anne Chapas, MD, medical director of UnionDerm in New York, and colleagues evaluated the safety and efficacy of an electrical muscle stimulation system for improving muscle strength and toning of the upper extremities.
For the treatments, they used disposable contact pads to place pairs of electrodes on the biceps and on the triceps. All patients (median age 42) received 30-minute treatments twice weekly for 2 or 3 weeks, corresponding to four or six total sessions respectively, depending on the study site. Follow-ups were conducted 30 and 90 days after treatment. They used a validated dynamometer device to measure strength at baseline, at the final treatment session, and at the post-treatment 30- and 90-day visits.
“We saw about a 40% increase in strength in the biceps and about a 30% increase in strength in the triceps,” Dr. Ibrahimi said. “Interestingly, the effect got greater at 30 and 90 days, so this is something that lingers on for quite a while.” In addition to the increase in strength, the researchers and patients noted an improvement in the appearance of the arms. He predicted that this technology “is going to play a role in functional medicine and getting injured athletes back to their sports faster.”
Dr. Ibrahimi disclosed that he is a member of the Advisory Board for Accure Acne, AbbVie, Cutera (manufacturer of truSculpt), Lutronic, Blueberry Therapeutics, Cytrellis, and Quthero. He also holds stock in many device and pharmaceutical companies (none are relevant to the treatments mentioned in this story).
Going into solo practice? An expert shares tips
SAN DIEGO – When the Boston-based cosmetic dermatology practice that employed Catherine M. DiGiorgio, MD, MS, was sold to a private equity firm a few years ago, she found herself at a crossroads: Stay and work for a large corporation, or open a solo practice?
She opted to start her own practice in Boston, “because I didn’t want to work for a large corporation, and I want to provide the best care for my patients in a more intimate manner,” Dr. DiGiorgio, a board-certified laser and cosmetic dermatologist, said at the annual Masters of Aesthetics Symposium.
The decision also tested her mettle. “I spoke to several colleagues and friends, and I was terrified,” she said. “I was like: ‘I don’t even know where to start.’ ”
On the heels of opening a new office in a matter of weeks, she offered the following tips and questions to consider when launching a solo dermatology practice:
Select a location. “That’s your first decision,” she said. “Where in the city are you going to open? Are you going to a new city, or are you moving back home? Don’t be afraid to start from scratch, and don’t be afraid to start a [solo] practice if you already have a patient base.”
Will you lease or purchase your space? After she secured a bank loan, Dr. DiGiorgio chose to lease the space for her new practice, “because you can kind of see where things go, get all the kinks out and figure out how to build things in a space that you don’t own. Then, when you’re ready and you have grown, you can invest more into your practice.”
Will you accept insurance? She built her practice around the direct specialty care model, which emphasizes the patient-physician relationship and removes third-party payors. “It’s not a concierge practice, but it’s a transparent, reasonable fee schedule for medical dermatology,” she explained. “I’ve done 100% cosmetics for about 5 years now, [but] I do medical dermatology for a fee. On my website I have a full price list on how much a full skin check is, [and] how much biopsies are. It’s completely transparent. Patients can submit to their insurance for reimbursement, but we don’t guarantee that they’re going to be reimbursed.”
Where will your patients come from? Will you advertise? Do you have physicians in the area who will refer to you if you’re a board-certified dermatologist? She emphasized the importance of “learning how to present yourself” on a website dedicated to your own practice. “Instagram, Facebook, and social media are great, but you don’t own those pages,” noted Dr. DiGiorgio, who served as the program cochair of the 2023 annual meeting of the American Society for Laser Medicine and Surgery and was recently elected to serve on the board of directors for the American Society for Dermatology Surgery. “You don’t own one of those pictures that are posted on your social media page. They can disappear in a second. If that happens, how are people going to find you?”
Are you going to hire more physicians in the future? That will influence the size of the new office and the floor plan.
Lawyer up. Hiring a health care attorney can “help you navigate transitioning from whatever position you’re in to opening up your own practice, as well as setting up the regulatory paperwork necessary for your new practice. You’ll also need a real estate attorney to help once you have selected a place, to help you navigate through that process,” she said, such as figuring out if the elevator in the building meets the Americans With Disabilities Act (ADA) requirements.
Create a mission statement. That way, “you know why you’re doing this, and it stays with you as you’re getting through the hard roadblocks.”
Find an architect, contractor, or designer. “If you’re building out a space from scratch, you’re going to need an architect,” she said. “Along with that architect will come a full-on contracting firm. I ended up hiring everyone individually, because I’m trying to spend as little money as possible.” She also hired a designer to help select furnishings and create the office atmosphere.
Secure a building permit ASAP. “It’s almost better to have the city permit before you sign the lease, because the permits can take a year, and you don’t want to pay rent on an empty space for a year if you don’t have a permit or if there are other hoops to go through,” Dr. DiGiorgio said.
Find an agent to help you set up medical malpractice insurance, liability insurance, and worker’s compensation insurance. “Make sure you read all the paperwork, because it can be very intricate,” she said.
Find an accountant. That person can help set up a bookkeeping process.
What equipment and devices will you need? That depends largely on the patient population a physician serves. Dr. DiGiorgio noted that eligible small businesses may take a tax credit of up to $5,000 per year for accommodations made to comply with the ADA. “That’s a nice feature, so that you can purchase ADA compliant items like a larger exam chair and custom reception areas.”
Dr. DiGiorgio reported having no relevant disclosures.
SAN DIEGO – When the Boston-based cosmetic dermatology practice that employed Catherine M. DiGiorgio, MD, MS, was sold to a private equity firm a few years ago, she found herself at a crossroads: Stay and work for a large corporation, or open a solo practice?
She opted to start her own practice in Boston, “because I didn’t want to work for a large corporation, and I want to provide the best care for my patients in a more intimate manner,” Dr. DiGiorgio, a board-certified laser and cosmetic dermatologist, said at the annual Masters of Aesthetics Symposium.
The decision also tested her mettle. “I spoke to several colleagues and friends, and I was terrified,” she said. “I was like: ‘I don’t even know where to start.’ ”
On the heels of opening a new office in a matter of weeks, she offered the following tips and questions to consider when launching a solo dermatology practice:
Select a location. “That’s your first decision,” she said. “Where in the city are you going to open? Are you going to a new city, or are you moving back home? Don’t be afraid to start from scratch, and don’t be afraid to start a [solo] practice if you already have a patient base.”
Will you lease or purchase your space? After she secured a bank loan, Dr. DiGiorgio chose to lease the space for her new practice, “because you can kind of see where things go, get all the kinks out and figure out how to build things in a space that you don’t own. Then, when you’re ready and you have grown, you can invest more into your practice.”
Will you accept insurance? She built her practice around the direct specialty care model, which emphasizes the patient-physician relationship and removes third-party payors. “It’s not a concierge practice, but it’s a transparent, reasonable fee schedule for medical dermatology,” she explained. “I’ve done 100% cosmetics for about 5 years now, [but] I do medical dermatology for a fee. On my website I have a full price list on how much a full skin check is, [and] how much biopsies are. It’s completely transparent. Patients can submit to their insurance for reimbursement, but we don’t guarantee that they’re going to be reimbursed.”
Where will your patients come from? Will you advertise? Do you have physicians in the area who will refer to you if you’re a board-certified dermatologist? She emphasized the importance of “learning how to present yourself” on a website dedicated to your own practice. “Instagram, Facebook, and social media are great, but you don’t own those pages,” noted Dr. DiGiorgio, who served as the program cochair of the 2023 annual meeting of the American Society for Laser Medicine and Surgery and was recently elected to serve on the board of directors for the American Society for Dermatology Surgery. “You don’t own one of those pictures that are posted on your social media page. They can disappear in a second. If that happens, how are people going to find you?”
Are you going to hire more physicians in the future? That will influence the size of the new office and the floor plan.
Lawyer up. Hiring a health care attorney can “help you navigate transitioning from whatever position you’re in to opening up your own practice, as well as setting up the regulatory paperwork necessary for your new practice. You’ll also need a real estate attorney to help once you have selected a place, to help you navigate through that process,” she said, such as figuring out if the elevator in the building meets the Americans With Disabilities Act (ADA) requirements.
Create a mission statement. That way, “you know why you’re doing this, and it stays with you as you’re getting through the hard roadblocks.”
Find an architect, contractor, or designer. “If you’re building out a space from scratch, you’re going to need an architect,” she said. “Along with that architect will come a full-on contracting firm. I ended up hiring everyone individually, because I’m trying to spend as little money as possible.” She also hired a designer to help select furnishings and create the office atmosphere.
Secure a building permit ASAP. “It’s almost better to have the city permit before you sign the lease, because the permits can take a year, and you don’t want to pay rent on an empty space for a year if you don’t have a permit or if there are other hoops to go through,” Dr. DiGiorgio said.
Find an agent to help you set up medical malpractice insurance, liability insurance, and worker’s compensation insurance. “Make sure you read all the paperwork, because it can be very intricate,” she said.
Find an accountant. That person can help set up a bookkeeping process.
What equipment and devices will you need? That depends largely on the patient population a physician serves. Dr. DiGiorgio noted that eligible small businesses may take a tax credit of up to $5,000 per year for accommodations made to comply with the ADA. “That’s a nice feature, so that you can purchase ADA compliant items like a larger exam chair and custom reception areas.”
Dr. DiGiorgio reported having no relevant disclosures.
SAN DIEGO – When the Boston-based cosmetic dermatology practice that employed Catherine M. DiGiorgio, MD, MS, was sold to a private equity firm a few years ago, she found herself at a crossroads: Stay and work for a large corporation, or open a solo practice?
She opted to start her own practice in Boston, “because I didn’t want to work for a large corporation, and I want to provide the best care for my patients in a more intimate manner,” Dr. DiGiorgio, a board-certified laser and cosmetic dermatologist, said at the annual Masters of Aesthetics Symposium.
The decision also tested her mettle. “I spoke to several colleagues and friends, and I was terrified,” she said. “I was like: ‘I don’t even know where to start.’ ”
On the heels of opening a new office in a matter of weeks, she offered the following tips and questions to consider when launching a solo dermatology practice:
Select a location. “That’s your first decision,” she said. “Where in the city are you going to open? Are you going to a new city, or are you moving back home? Don’t be afraid to start from scratch, and don’t be afraid to start a [solo] practice if you already have a patient base.”
Will you lease or purchase your space? After she secured a bank loan, Dr. DiGiorgio chose to lease the space for her new practice, “because you can kind of see where things go, get all the kinks out and figure out how to build things in a space that you don’t own. Then, when you’re ready and you have grown, you can invest more into your practice.”
Will you accept insurance? She built her practice around the direct specialty care model, which emphasizes the patient-physician relationship and removes third-party payors. “It’s not a concierge practice, but it’s a transparent, reasonable fee schedule for medical dermatology,” she explained. “I’ve done 100% cosmetics for about 5 years now, [but] I do medical dermatology for a fee. On my website I have a full price list on how much a full skin check is, [and] how much biopsies are. It’s completely transparent. Patients can submit to their insurance for reimbursement, but we don’t guarantee that they’re going to be reimbursed.”
Where will your patients come from? Will you advertise? Do you have physicians in the area who will refer to you if you’re a board-certified dermatologist? She emphasized the importance of “learning how to present yourself” on a website dedicated to your own practice. “Instagram, Facebook, and social media are great, but you don’t own those pages,” noted Dr. DiGiorgio, who served as the program cochair of the 2023 annual meeting of the American Society for Laser Medicine and Surgery and was recently elected to serve on the board of directors for the American Society for Dermatology Surgery. “You don’t own one of those pictures that are posted on your social media page. They can disappear in a second. If that happens, how are people going to find you?”
Are you going to hire more physicians in the future? That will influence the size of the new office and the floor plan.
Lawyer up. Hiring a health care attorney can “help you navigate transitioning from whatever position you’re in to opening up your own practice, as well as setting up the regulatory paperwork necessary for your new practice. You’ll also need a real estate attorney to help once you have selected a place, to help you navigate through that process,” she said, such as figuring out if the elevator in the building meets the Americans With Disabilities Act (ADA) requirements.
Create a mission statement. That way, “you know why you’re doing this, and it stays with you as you’re getting through the hard roadblocks.”
Find an architect, contractor, or designer. “If you’re building out a space from scratch, you’re going to need an architect,” she said. “Along with that architect will come a full-on contracting firm. I ended up hiring everyone individually, because I’m trying to spend as little money as possible.” She also hired a designer to help select furnishings and create the office atmosphere.
Secure a building permit ASAP. “It’s almost better to have the city permit before you sign the lease, because the permits can take a year, and you don’t want to pay rent on an empty space for a year if you don’t have a permit or if there are other hoops to go through,” Dr. DiGiorgio said.
Find an agent to help you set up medical malpractice insurance, liability insurance, and worker’s compensation insurance. “Make sure you read all the paperwork, because it can be very intricate,” she said.
Find an accountant. That person can help set up a bookkeeping process.
What equipment and devices will you need? That depends largely on the patient population a physician serves. Dr. DiGiorgio noted that eligible small businesses may take a tax credit of up to $5,000 per year for accommodations made to comply with the ADA. “That’s a nice feature, so that you can purchase ADA compliant items like a larger exam chair and custom reception areas.”
Dr. DiGiorgio reported having no relevant disclosures.
AT MOAS 2023