ANSWER
The correct choice is iatrogenic (choice “a”)—that is, provider-caused—in this case, the result of prolonged application of a relatively powerful steroid cream. Such use eventuates in what is sometimes termed “steroid addiction.” These patients are often wrongly suspected of being alcoholics (choice “b”) because of their red faces, but there was no reason to suspect that in this case. It is thought that bacteria flourish on steroid-treated skin, which is theorized to worsen rosacea; however, this is not an outright infection (choice “c”). Nor is it the result of using the wrong soap on the face (choice “d”), as irritation from soap would not have been limited to such sharply demarcated areas.
DISCUSSION
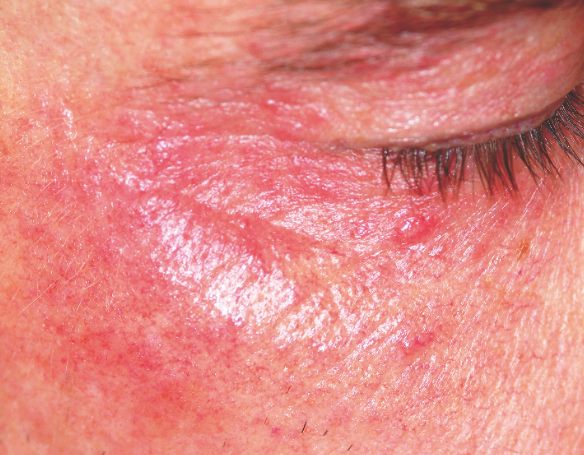
The injudicious application of topical steroids can have a number of negative effects, all demonstrated in this case. It thins the skin, literally uncovering normally hidden vasculature, which manifests as telangiectasia. The epidermis turns atrophic and shiny, and a rosacea-like eruption (so-called “iatrosacea”) often appears.
But the worst adverse effect is the one that forces the patient to keep using the medication long after the treated condition has disappeared: Burning and itching ensue immediately if the application stops or is reduced. This is especially true for atopic patients who are born with thin skin, and even more so for relatively thin facial skin. Eyelids and perioral areas are especially prone to this reaction, and it is often the fault of the prescribing provider who refills the medication over and over, while failing to educate patients about its potentially deleterious effects.
The differential diagnosis for this common condition includes contact versus irritant dermatitis (patients often make rosacea worse by applying numerous OTC products, such as triple-antibiotic ointment), rosacea, granulomatous faciale, and discoid lupus.
TREATMENT
Treatment in such cases begins with cessation of the steroid and a switch either to a steroid preparation of lower potency (such as hydrocortisone 2.5%) or better yet, to a calcineurin inhibitor (such as pimecrolimus or tacrolimus). In addition, oral tetracycline (500 mg bid) may be taken until the condition begins to improve markedly—a process that can take months. The latter treatment should be slowly tapered to one dose per day, then stopped only when the problem has totally cleared. These patients often need frequent return visits initially for reassurance and re-education