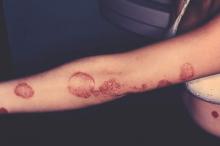
Self-reported psoriasis more than doubled the odds of major depression, even after accounting for demographic factors and comorbidities, reported the authors of a study that used data from the National Health and Nutrition Examination Survey.
In addition, depressive symptoms adversely affected the work and social lives of psoriasis patients in this first-in-kind study, said Dr. Brandon Cohen and his associates of the department of dermatology, New York University. “The risk of major depression was not associated with the self-reported degree of psoriasis. Therefore, our study supports that all patients with psoriasis, regardless of severity, are at risk for depressive symptoms and may benefit from depression screening,” they wrote. The study was published online on Sept. 30 in JAMA Dermatology (2015 Sep 30. doi: 10.1001/jamadermatol.2015.3605).
Psoriasis is known to increase the risk of major depression, as well as anxiety disorders, substance abuse, and suicidal ideation. To better understand whether disease severity or comorbidities affect the psoriasis-depression link, the researchers analyzed self-reported health data from 12,382 individuals who had responded to the National Health and Nutrition Examination Survey between 2009 and 2012. The investigators defined major depression as a score of at least 10 on the 27-point Patient Health Questionnaire-9 (PHQ-9). Psoriasis was self-reported, and some psoriasis patients were also asked to rate the severity of their skin disease.
After adjusting for factors such as age, sex, race, and history of myocardial infarction, stroke, and diabetes, the 351 individuals with psoriasis had more than twice the odds of major depression, compared with respondents without psoriasis (odds ratio, 2.09; 95% confidence interval, 1.41-3.11; P less than .001). Furthermore, the average PHQ-9 score among psoriasis patients was significantly higher than that among other respondents (4.54 vs. 3.22; P less than .001).
Neither severity of skin disease nor history of MI or stroke affected the relationship between psoriasis and depression. “The psychiatric burden of psoriasis may be more closely tied to patients’ perception of the social response to their appearance than objective disease severity,” the investigators said. They noted that as far as they know, this is the first study to use a nationally representative sample of patients to evaluate the association between psoriasis and major depression.
The investigators reported no funding sources and declared no competing interests.