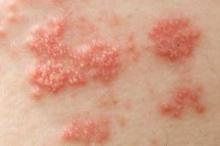
Combining tumor necrosis factor-alpha inhibitors with conventional disease-modifying antirheumatic drugs more than doubled the risk of shingles in patients with psoriatic arthritis, according to a retrospective cohort study.
Patients who took drugs from only one class or the other, however, were no more likely to develop herpes zoster than were untreated patients, said Dr. Devy Zisman of Carmel Medical Center in Haifa, Israel, and his associates.
Biological therapies for inflammatory arthritis have been linked to an increased risk of herpes zoster in some analyses. To investigate the issue, Dr. Zisman and associates studied 3,128 patients with psoriatic arthritis from a national Israeli health care database. The patients averaged 50 years of age, and 46% were male (Ann. Rheum. Dis. 2014 Sept. 26 [doi:10.1136/ annrheumdis-2013-205148]).
A total of 182 herpes zoster cases occurred during 20,096 person-years of observation, the researchers said. After controlling for sex, age, comorbidities, steroid treatment, and past treatment with conventional DMARDs, the hazard ratio for herpes zoster with coadministration of tumor necrosis factor-alpha (TNF-alpha) inhibitors and conventional DMARDs was 2.37 (95% confidence interval, 1.32-4.22; P = .004), compared with 1.28 for TNF-alpha inhibitors alone (95% CI, 0.69-2.4) and 1.11 for conventional DMARDs alone (95% CI, 0.76-1.62). The anti–TNF-alpha agents studied included infliximab, adalimumab, and etanercept, while DMARDs included salazopyrine, methotrexate, leflunomide, cyclosporine A, azathioprine, and hydroxychloroquine.
The incidence of herpes zoster in patients prescribed combination regimens was 17.86 cases per 1,000 person-years (95% CI, 10.91-27.58), far higher than for patients who took neither DMARDs nor anti–TNF-alpha agents (7.36), took only conventional DMARDs (9.21), or took only TNF-alpha inhibitors (8.64), the investigators reported.
Older age and treatment with steroids were linked to a slight rise in the risk of herpes zoster (HRs, 1.01 and 1.08, respectively), confirming prior findings, Dr. Zisman and his associates said.
The authors reported no funding sources or conflicts of interest.