Article
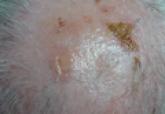
Pemphigus Vulgaris Successfully Treated With Doxycycline Monotherapy
- Author:
- Natalie L. Hone, MD
- Diya F. Mutasim, MD
Quiz

Hypopigmented Facial Papules on the Cheeks
- Author:
- Janelle M. King, MD
- Matthew J. Meier, MD
- Diya F. Mutasim, MD
A 73-year-old woman presented with multiple mildly pruritic, hypopigmented, thin papules involving both cheeks of 5 months’ duration. The patient...
