User login
Privacy and maternal records
At the undergraduate level, classes on medical ethics tend to focus on the big ticket items like abortion, euthanasia, and social justice. Personally, I find the more interesting clinical cases involve relatively minor issues that accumulate to create problems. Privacy is one example.
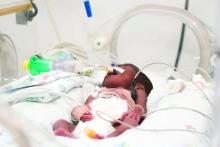
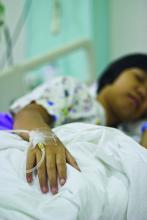
A large amount of information in the mother’s prenatal records potentially impacts a newborn’s care. Ideally, the EHR is transferring data to the newborn’s chart, but not everything automatically populates in the newborn record, so there will be times when a pediatrician needs to review the mother’s chart.
- The criteria for selecting which mothers’ charts to review involve racial profiling.
- Access to mental health records involving addiction treatment requires special authorization. State laws and hospital policies will vary.
- Mom is a Hollywood celebrity and, while reviewing her chart, prurient curiosity extends the search to records of her cosmetic surgeries.
In my opinion, most of what is and isn’t permissible is determined by medical custom and not by statutes. The judiciary reserves the power to intervene, so medical custom should be informed by laws and by legal principles. But, the primary basis for these decisions should be a commitment to patient advocacy and to common sense, which in this situation means, “Would the typical reasonable person be upset if she learned I had done something without telling her?” If the answer to that question is yes, or in any way equivocal, I think ethics would dictate obtaining consent or at least assent.
Opiate addiction has quadrupled in the past 15 years. Almost all states now have prescription registries to help detect doctor shopping, multiple prescribers, and misdirection. If you are prescribing an opiate, it is ethically reasonable (and now the law) for you to make writing the prescription contingent on your patient agreeing to your consulting the registry. No consent, no prescription.
I think the facts of that case (writing a prescription) can be distinguished (a legal term) from the case of a neonatologist accessing the narcotic registry of the mother while on a fishing expedition to find evidence that might help the baby. Perhaps it is okay with the mother’s uncoerced consent, but otherwise I think that practice reeks as an unreasonable search. Ethically and legally, it has parallels to Ferguson v. City of Charleston (SCOTUS 2001).
That was a 6-3 Supreme Court decision, so, while I agree with the majority, you may find hospital lawyers who disagree. Overall, I assert that consent and privacy are best considered ethically as advocacy for the patient and not as legalistic forms that the physician must complete.
The reverse situation also occurs. Sometimes maternal health information is placed into the newborn’s chart that doesn’t need to be there. For example, common practice has been to designate mom, after delivery, as G4P2022. This contains the information that mother has had two therapeutic abortions. Does that information belong in a newborn’s chart? Especially in the era of the EHR where this information will hang around forever and will be easily obtained by the baby 16 years later when she can access all her medical information online. Will the mother be upset for her teenage daughter to learn that mom has had two abortions? Is that private information, belonging to the mother, that was given in confidence to her obstetrician? I advocate respecting privacy.
I have similar concerns about STD information being transferred from maternal charts to the newborn’s EHR. A maternal history of gonorrhea treated 8 years previously is unlikely to be relevant and should not populate the newborn’s EHR. I can make an argument that chlamydia detected and treated during the pregnancy might be useful to the baby’s pediatrician because neither treatment nor tests of cure are perfect. Perhaps, it could exist as a Snapchat-type record and disappear from the newborn’s record in a year if no respiratory symptoms occur.
I’m aware of efforts to destigmatize abortion and STDs, but, until that occurs, sensitive information should be handled delicately to preserve privacy. That is a major component of the Hippocratic Oath.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis.
At the undergraduate level, classes on medical ethics tend to focus on the big ticket items like abortion, euthanasia, and social justice. Personally, I find the more interesting clinical cases involve relatively minor issues that accumulate to create problems. Privacy is one example.
A large amount of information in the mother’s prenatal records potentially impacts a newborn’s care. Ideally, the EHR is transferring data to the newborn’s chart, but not everything automatically populates in the newborn record, so there will be times when a pediatrician needs to review the mother’s chart.
- The criteria for selecting which mothers’ charts to review involve racial profiling.
- Access to mental health records involving addiction treatment requires special authorization. State laws and hospital policies will vary.
- Mom is a Hollywood celebrity and, while reviewing her chart, prurient curiosity extends the search to records of her cosmetic surgeries.
In my opinion, most of what is and isn’t permissible is determined by medical custom and not by statutes. The judiciary reserves the power to intervene, so medical custom should be informed by laws and by legal principles. But, the primary basis for these decisions should be a commitment to patient advocacy and to common sense, which in this situation means, “Would the typical reasonable person be upset if she learned I had done something without telling her?” If the answer to that question is yes, or in any way equivocal, I think ethics would dictate obtaining consent or at least assent.
Opiate addiction has quadrupled in the past 15 years. Almost all states now have prescription registries to help detect doctor shopping, multiple prescribers, and misdirection. If you are prescribing an opiate, it is ethically reasonable (and now the law) for you to make writing the prescription contingent on your patient agreeing to your consulting the registry. No consent, no prescription.
I think the facts of that case (writing a prescription) can be distinguished (a legal term) from the case of a neonatologist accessing the narcotic registry of the mother while on a fishing expedition to find evidence that might help the baby. Perhaps it is okay with the mother’s uncoerced consent, but otherwise I think that practice reeks as an unreasonable search. Ethically and legally, it has parallels to Ferguson v. City of Charleston (SCOTUS 2001).
That was a 6-3 Supreme Court decision, so, while I agree with the majority, you may find hospital lawyers who disagree. Overall, I assert that consent and privacy are best considered ethically as advocacy for the patient and not as legalistic forms that the physician must complete.
The reverse situation also occurs. Sometimes maternal health information is placed into the newborn’s chart that doesn’t need to be there. For example, common practice has been to designate mom, after delivery, as G4P2022. This contains the information that mother has had two therapeutic abortions. Does that information belong in a newborn’s chart? Especially in the era of the EHR where this information will hang around forever and will be easily obtained by the baby 16 years later when she can access all her medical information online. Will the mother be upset for her teenage daughter to learn that mom has had two abortions? Is that private information, belonging to the mother, that was given in confidence to her obstetrician? I advocate respecting privacy.
I have similar concerns about STD information being transferred from maternal charts to the newborn’s EHR. A maternal history of gonorrhea treated 8 years previously is unlikely to be relevant and should not populate the newborn’s EHR. I can make an argument that chlamydia detected and treated during the pregnancy might be useful to the baby’s pediatrician because neither treatment nor tests of cure are perfect. Perhaps, it could exist as a Snapchat-type record and disappear from the newborn’s record in a year if no respiratory symptoms occur.
I’m aware of efforts to destigmatize abortion and STDs, but, until that occurs, sensitive information should be handled delicately to preserve privacy. That is a major component of the Hippocratic Oath.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis.
At the undergraduate level, classes on medical ethics tend to focus on the big ticket items like abortion, euthanasia, and social justice. Personally, I find the more interesting clinical cases involve relatively minor issues that accumulate to create problems. Privacy is one example.
A large amount of information in the mother’s prenatal records potentially impacts a newborn’s care. Ideally, the EHR is transferring data to the newborn’s chart, but not everything automatically populates in the newborn record, so there will be times when a pediatrician needs to review the mother’s chart.
- The criteria for selecting which mothers’ charts to review involve racial profiling.
- Access to mental health records involving addiction treatment requires special authorization. State laws and hospital policies will vary.
- Mom is a Hollywood celebrity and, while reviewing her chart, prurient curiosity extends the search to records of her cosmetic surgeries.
In my opinion, most of what is and isn’t permissible is determined by medical custom and not by statutes. The judiciary reserves the power to intervene, so medical custom should be informed by laws and by legal principles. But, the primary basis for these decisions should be a commitment to patient advocacy and to common sense, which in this situation means, “Would the typical reasonable person be upset if she learned I had done something without telling her?” If the answer to that question is yes, or in any way equivocal, I think ethics would dictate obtaining consent or at least assent.
Opiate addiction has quadrupled in the past 15 years. Almost all states now have prescription registries to help detect doctor shopping, multiple prescribers, and misdirection. If you are prescribing an opiate, it is ethically reasonable (and now the law) for you to make writing the prescription contingent on your patient agreeing to your consulting the registry. No consent, no prescription.
I think the facts of that case (writing a prescription) can be distinguished (a legal term) from the case of a neonatologist accessing the narcotic registry of the mother while on a fishing expedition to find evidence that might help the baby. Perhaps it is okay with the mother’s uncoerced consent, but otherwise I think that practice reeks as an unreasonable search. Ethically and legally, it has parallels to Ferguson v. City of Charleston (SCOTUS 2001).
That was a 6-3 Supreme Court decision, so, while I agree with the majority, you may find hospital lawyers who disagree. Overall, I assert that consent and privacy are best considered ethically as advocacy for the patient and not as legalistic forms that the physician must complete.
The reverse situation also occurs. Sometimes maternal health information is placed into the newborn’s chart that doesn’t need to be there. For example, common practice has been to designate mom, after delivery, as G4P2022. This contains the information that mother has had two therapeutic abortions. Does that information belong in a newborn’s chart? Especially in the era of the EHR where this information will hang around forever and will be easily obtained by the baby 16 years later when she can access all her medical information online. Will the mother be upset for her teenage daughter to learn that mom has had two abortions? Is that private information, belonging to the mother, that was given in confidence to her obstetrician? I advocate respecting privacy.
I have similar concerns about STD information being transferred from maternal charts to the newborn’s EHR. A maternal history of gonorrhea treated 8 years previously is unlikely to be relevant and should not populate the newborn’s EHR. I can make an argument that chlamydia detected and treated during the pregnancy might be useful to the baby’s pediatrician because neither treatment nor tests of cure are perfect. Perhaps, it could exist as a Snapchat-type record and disappear from the newborn’s record in a year if no respiratory symptoms occur.
I’m aware of efforts to destigmatize abortion and STDs, but, until that occurs, sensitive information should be handled delicately to preserve privacy. That is a major component of the Hippocratic Oath.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis.
Changing ethics of pediatric health care: The last 50 years
The ethics of pediatric health care have changed radically in the past 50 years. “History,” they say, “is written by the victors.” So, if you are not careful, you will only get part of the story. Clinical ethicists learn to seek out, involve, and empower the voices of all stakeholders. To fully appreciate how much things have changed, you must learn more than one side of the story. Indeed, piecing together the history of medical ethics reminds me of the Indian story of five blind men describing an elephant, in which each can only describe a part of an ultimately much bigger animal.
If you ask philosophers about the history of medical ethics, they will point to events 50 years ago as the beginning of the modern era. In the 1960s, physicians tended to be paternalistic authoritarians. Some considered it best not to even tell a patient that he had cancer. There was minimal patient education provided. Medications were prescribed as orders for the patient to follow. Medical research had harmed volunteers, and new protections were needed.
In 1995, the American Academy of Pediatrics Section on Bioethics emphasized the importance of obtaining the child’s assent in addition to the parent’s consent.2 Most states have passed laws permitting minors to give consent for treatment for pregnancy, sexually transmitted diseases, drug addiction, and mental health care.
Technology alters ethics
At the same time, technology has been changing medicine. New life sustaining technologies in the 1960s – such as dialysis and ventilators – created new issues of extreme financial cost, allocation of scarce resources, and even the existential question of when life ends. In 1968, an ad hoc committee at Harvard created criteria for what is colloquially called “brain death.”3 Many landmark legal cases further developed the ethics of end-of-life care.
The boundaries were even less clear at the beginning of life. Technological advances in ventilators, improvements in nursing care by neonatal intensive care unit nurses, and the whole new subspecialty of neonatology progressively lowered the gestational age for survival. The distinction between clinical care and experimental care was again blurry as neonatologists sought to overcome previously unknown complications, like retinopathy of prematurity resulting from too much oxygen and bronchopulmonary dysplasia from the ventilator. Many babies survived with profound physical and neurological compromise. The ethical dilemmas were continuously present.
Change in the status of children
There is more to the story than philosophy, law, and technology. Pediatric ethics has been profoundly impacted by a change in the status of the children. One change from 50 years ago has been the social response to child abuse.4 Norms changed. Before, fathers pretty much could raise their children any way they saw fit, including corporal punishment. Neighbors didn’t intervene. The proverb was “spare the rod and spoil the child,” but abuse was not motivated by discipline. It was cruel, authoritarian, and demeaning. The landmark article describing the Battered Child Syndrome was published in 1962.5 By 1967, the local Society for the Prevention of Cruelty to Children had become nearly obsolete, but understaffed local government agencies were just beginning to respond. In 1974, federal action produced the Child Abuse Prevention and Treatment Act.6 Medical personnel became mandatory reporters, developed expertise, and, in 2009, child abuse became a boarded subspecialty in pediatrics.
Then, in 1971, a documentary “Who Should Survive?” explored the ethical decision making for babies with birth defects.7 The harms of institutionalization became recognized. The benefits of early intervention and special education have been established. Support for an Individual Education Plan has progressed through successive laws beginning in 1975 until the Individuals with Disabilities Education Improvement Act of 2004.
This is just another example of how ethics develops from a philosophical ideal to a change in social status, followed by consciousness raising, civil rights legislation, enabling legislation, funding, and program development and implementation.
It takes a village of philosophers, activists, lawyers, legislators, physicians, and other experts to implement ethics. There are also countervailing forces. The mainstreaming of children with disabilities is one factor in the movement of children into private schools and the pressure for a voucher system, as advocated by the new Secretary of Education, Betty DeVos.
There also has been a change in the status of children as future providers. Historically, children were relied upon to provide for the parents in their old age. With decreases in infant mortality, the availability of birth control, and legalized abortions, smaller families became the social norm. Worldwide, there has been a marked drop in fertility rates in developed nations. Governmental programs such as Social Security, particularly with the introduction of Medicare in 1965, meant that the elderly were less dependent on their descendants. China found that acceptance of the One Child policy was heavily dependent on convincing parents that the State would provide for them in their old age. The modern political state has assumed duties previously performed by the family.
More recent changes
Pediatric health care is strongly impacted by public health measures. Infant mortality has been reduced by improved nutrition and public health, not medication and surgery. Mass immunization programs were viewed as an appropriate function of civic government.
The introduction of polio vaccine in the 1950s made a large impact. Families lined up at any opportunity to get the vaccine. Polio went from hundreds of thousands of cases of paralysis each summer down to zero cases of wild polio transmitted within the western hemisphere. Measles cases went from 450,000 cases a year in the early 1960s down to zero, until a fraudulent link to autism led to a significant number of parents not immunizing their children. Vaccine refusal, previously a rare ethical issue related to religious liberty, became corrupted by efforts at boutique medicine and alternative facts. In modern America, the ethics of individualism and personal rights have eclipsed civic responsibility. With herd immunity compromised, a blip up to 100 cases of measles per year was histrionically described as a huge epidemic. That spin shows ignorance of the historical record, but the risk was enough for the liberal state of California in 2015 to ban philosophical exemptions to vaccination with one of the strictest state laws in the nation.
Ethics is about values. So, as I look at the changes over 50 years, the areas that have failed to make progress are illuminating. Mental health care for children has not made the same progress achieved with vaccines and cancer therapy. My most recent clinical ethics case involved a teenager who had made a suicidal gesture by taking a handful of pills. The nurses were caught between caring for their patient and meeting the demands of an upset, authoritarian parent in a world where customer satisfaction is critical. I spent much of the night exploring hospital policy and state law. I solicited and listened to widely disparate interpretations of law, medical ethics, and hospital policy from the floor nurse, the nursing supervisor, the nursing staff on the adult inpatient psychiatric unit, three ED docs, a social worker, a government agency, and a judge’s representative. The physician of 1967 was captain of the ship and would not recognize the chaotic teamwork of modern medicine. The exercise showed me how little progress we have made in mental health care for adolescents during my 25 years of practice.
It also reminded me that I have the luxury to debate ethical minutia like vaccine hesitancy and adolescent consent in a world with Syrian refugee camps and starvation in South Sudan. Mahatma Gandhi said, “There are people in the world so hungry that God cannot appear to them except in the form of bread.” That, unfortunately, has not changed in 50 years.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@frontlinemedcom.com.
References
1. www.hhs.gov/ohrp/regulations-and-policy/belmont-report/
2. Pediatrics 1995;95:314-7.
3. JAMA. 1968;205(6):337-40.
4. Family Law Quarterly. 2008 Fall;42(3):449-63.
5. JAMA. 1962;181(1):17-24.
6. National Child Abuse and Neglect Training and Publications Project (2014). The Child Abuse Prevention and Treatment Act: 40 years of safeguarding America’s children. Washington: U.S. Department of Health and Human Services, Children’s Bureau.
7. Kennedy Inst Ethics J. 2006 Sep;16(3):205-24.
The ethics of pediatric health care have changed radically in the past 50 years. “History,” they say, “is written by the victors.” So, if you are not careful, you will only get part of the story. Clinical ethicists learn to seek out, involve, and empower the voices of all stakeholders. To fully appreciate how much things have changed, you must learn more than one side of the story. Indeed, piecing together the history of medical ethics reminds me of the Indian story of five blind men describing an elephant, in which each can only describe a part of an ultimately much bigger animal.
If you ask philosophers about the history of medical ethics, they will point to events 50 years ago as the beginning of the modern era. In the 1960s, physicians tended to be paternalistic authoritarians. Some considered it best not to even tell a patient that he had cancer. There was minimal patient education provided. Medications were prescribed as orders for the patient to follow. Medical research had harmed volunteers, and new protections were needed.
In 1995, the American Academy of Pediatrics Section on Bioethics emphasized the importance of obtaining the child’s assent in addition to the parent’s consent.2 Most states have passed laws permitting minors to give consent for treatment for pregnancy, sexually transmitted diseases, drug addiction, and mental health care.
Technology alters ethics
At the same time, technology has been changing medicine. New life sustaining technologies in the 1960s – such as dialysis and ventilators – created new issues of extreme financial cost, allocation of scarce resources, and even the existential question of when life ends. In 1968, an ad hoc committee at Harvard created criteria for what is colloquially called “brain death.”3 Many landmark legal cases further developed the ethics of end-of-life care.
The boundaries were even less clear at the beginning of life. Technological advances in ventilators, improvements in nursing care by neonatal intensive care unit nurses, and the whole new subspecialty of neonatology progressively lowered the gestational age for survival. The distinction between clinical care and experimental care was again blurry as neonatologists sought to overcome previously unknown complications, like retinopathy of prematurity resulting from too much oxygen and bronchopulmonary dysplasia from the ventilator. Many babies survived with profound physical and neurological compromise. The ethical dilemmas were continuously present.
Change in the status of children
There is more to the story than philosophy, law, and technology. Pediatric ethics has been profoundly impacted by a change in the status of the children. One change from 50 years ago has been the social response to child abuse.4 Norms changed. Before, fathers pretty much could raise their children any way they saw fit, including corporal punishment. Neighbors didn’t intervene. The proverb was “spare the rod and spoil the child,” but abuse was not motivated by discipline. It was cruel, authoritarian, and demeaning. The landmark article describing the Battered Child Syndrome was published in 1962.5 By 1967, the local Society for the Prevention of Cruelty to Children had become nearly obsolete, but understaffed local government agencies were just beginning to respond. In 1974, federal action produced the Child Abuse Prevention and Treatment Act.6 Medical personnel became mandatory reporters, developed expertise, and, in 2009, child abuse became a boarded subspecialty in pediatrics.
Then, in 1971, a documentary “Who Should Survive?” explored the ethical decision making for babies with birth defects.7 The harms of institutionalization became recognized. The benefits of early intervention and special education have been established. Support for an Individual Education Plan has progressed through successive laws beginning in 1975 until the Individuals with Disabilities Education Improvement Act of 2004.
This is just another example of how ethics develops from a philosophical ideal to a change in social status, followed by consciousness raising, civil rights legislation, enabling legislation, funding, and program development and implementation.
It takes a village of philosophers, activists, lawyers, legislators, physicians, and other experts to implement ethics. There are also countervailing forces. The mainstreaming of children with disabilities is one factor in the movement of children into private schools and the pressure for a voucher system, as advocated by the new Secretary of Education, Betty DeVos.
There also has been a change in the status of children as future providers. Historically, children were relied upon to provide for the parents in their old age. With decreases in infant mortality, the availability of birth control, and legalized abortions, smaller families became the social norm. Worldwide, there has been a marked drop in fertility rates in developed nations. Governmental programs such as Social Security, particularly with the introduction of Medicare in 1965, meant that the elderly were less dependent on their descendants. China found that acceptance of the One Child policy was heavily dependent on convincing parents that the State would provide for them in their old age. The modern political state has assumed duties previously performed by the family.
More recent changes
Pediatric health care is strongly impacted by public health measures. Infant mortality has been reduced by improved nutrition and public health, not medication and surgery. Mass immunization programs were viewed as an appropriate function of civic government.
The introduction of polio vaccine in the 1950s made a large impact. Families lined up at any opportunity to get the vaccine. Polio went from hundreds of thousands of cases of paralysis each summer down to zero cases of wild polio transmitted within the western hemisphere. Measles cases went from 450,000 cases a year in the early 1960s down to zero, until a fraudulent link to autism led to a significant number of parents not immunizing their children. Vaccine refusal, previously a rare ethical issue related to religious liberty, became corrupted by efforts at boutique medicine and alternative facts. In modern America, the ethics of individualism and personal rights have eclipsed civic responsibility. With herd immunity compromised, a blip up to 100 cases of measles per year was histrionically described as a huge epidemic. That spin shows ignorance of the historical record, but the risk was enough for the liberal state of California in 2015 to ban philosophical exemptions to vaccination with one of the strictest state laws in the nation.
Ethics is about values. So, as I look at the changes over 50 years, the areas that have failed to make progress are illuminating. Mental health care for children has not made the same progress achieved with vaccines and cancer therapy. My most recent clinical ethics case involved a teenager who had made a suicidal gesture by taking a handful of pills. The nurses were caught between caring for their patient and meeting the demands of an upset, authoritarian parent in a world where customer satisfaction is critical. I spent much of the night exploring hospital policy and state law. I solicited and listened to widely disparate interpretations of law, medical ethics, and hospital policy from the floor nurse, the nursing supervisor, the nursing staff on the adult inpatient psychiatric unit, three ED docs, a social worker, a government agency, and a judge’s representative. The physician of 1967 was captain of the ship and would not recognize the chaotic teamwork of modern medicine. The exercise showed me how little progress we have made in mental health care for adolescents during my 25 years of practice.
It also reminded me that I have the luxury to debate ethical minutia like vaccine hesitancy and adolescent consent in a world with Syrian refugee camps and starvation in South Sudan. Mahatma Gandhi said, “There are people in the world so hungry that God cannot appear to them except in the form of bread.” That, unfortunately, has not changed in 50 years.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@frontlinemedcom.com.
References
1. www.hhs.gov/ohrp/regulations-and-policy/belmont-report/
2. Pediatrics 1995;95:314-7.
3. JAMA. 1968;205(6):337-40.
4. Family Law Quarterly. 2008 Fall;42(3):449-63.
5. JAMA. 1962;181(1):17-24.
6. National Child Abuse and Neglect Training and Publications Project (2014). The Child Abuse Prevention and Treatment Act: 40 years of safeguarding America’s children. Washington: U.S. Department of Health and Human Services, Children’s Bureau.
7. Kennedy Inst Ethics J. 2006 Sep;16(3):205-24.
The ethics of pediatric health care have changed radically in the past 50 years. “History,” they say, “is written by the victors.” So, if you are not careful, you will only get part of the story. Clinical ethicists learn to seek out, involve, and empower the voices of all stakeholders. To fully appreciate how much things have changed, you must learn more than one side of the story. Indeed, piecing together the history of medical ethics reminds me of the Indian story of five blind men describing an elephant, in which each can only describe a part of an ultimately much bigger animal.
If you ask philosophers about the history of medical ethics, they will point to events 50 years ago as the beginning of the modern era. In the 1960s, physicians tended to be paternalistic authoritarians. Some considered it best not to even tell a patient that he had cancer. There was minimal patient education provided. Medications were prescribed as orders for the patient to follow. Medical research had harmed volunteers, and new protections were needed.
In 1995, the American Academy of Pediatrics Section on Bioethics emphasized the importance of obtaining the child’s assent in addition to the parent’s consent.2 Most states have passed laws permitting minors to give consent for treatment for pregnancy, sexually transmitted diseases, drug addiction, and mental health care.
Technology alters ethics
At the same time, technology has been changing medicine. New life sustaining technologies in the 1960s – such as dialysis and ventilators – created new issues of extreme financial cost, allocation of scarce resources, and even the existential question of when life ends. In 1968, an ad hoc committee at Harvard created criteria for what is colloquially called “brain death.”3 Many landmark legal cases further developed the ethics of end-of-life care.
The boundaries were even less clear at the beginning of life. Technological advances in ventilators, improvements in nursing care by neonatal intensive care unit nurses, and the whole new subspecialty of neonatology progressively lowered the gestational age for survival. The distinction between clinical care and experimental care was again blurry as neonatologists sought to overcome previously unknown complications, like retinopathy of prematurity resulting from too much oxygen and bronchopulmonary dysplasia from the ventilator. Many babies survived with profound physical and neurological compromise. The ethical dilemmas were continuously present.
Change in the status of children
There is more to the story than philosophy, law, and technology. Pediatric ethics has been profoundly impacted by a change in the status of the children. One change from 50 years ago has been the social response to child abuse.4 Norms changed. Before, fathers pretty much could raise their children any way they saw fit, including corporal punishment. Neighbors didn’t intervene. The proverb was “spare the rod and spoil the child,” but abuse was not motivated by discipline. It was cruel, authoritarian, and demeaning. The landmark article describing the Battered Child Syndrome was published in 1962.5 By 1967, the local Society for the Prevention of Cruelty to Children had become nearly obsolete, but understaffed local government agencies were just beginning to respond. In 1974, federal action produced the Child Abuse Prevention and Treatment Act.6 Medical personnel became mandatory reporters, developed expertise, and, in 2009, child abuse became a boarded subspecialty in pediatrics.
Then, in 1971, a documentary “Who Should Survive?” explored the ethical decision making for babies with birth defects.7 The harms of institutionalization became recognized. The benefits of early intervention and special education have been established. Support for an Individual Education Plan has progressed through successive laws beginning in 1975 until the Individuals with Disabilities Education Improvement Act of 2004.
This is just another example of how ethics develops from a philosophical ideal to a change in social status, followed by consciousness raising, civil rights legislation, enabling legislation, funding, and program development and implementation.
It takes a village of philosophers, activists, lawyers, legislators, physicians, and other experts to implement ethics. There are also countervailing forces. The mainstreaming of children with disabilities is one factor in the movement of children into private schools and the pressure for a voucher system, as advocated by the new Secretary of Education, Betty DeVos.
There also has been a change in the status of children as future providers. Historically, children were relied upon to provide for the parents in their old age. With decreases in infant mortality, the availability of birth control, and legalized abortions, smaller families became the social norm. Worldwide, there has been a marked drop in fertility rates in developed nations. Governmental programs such as Social Security, particularly with the introduction of Medicare in 1965, meant that the elderly were less dependent on their descendants. China found that acceptance of the One Child policy was heavily dependent on convincing parents that the State would provide for them in their old age. The modern political state has assumed duties previously performed by the family.
More recent changes
Pediatric health care is strongly impacted by public health measures. Infant mortality has been reduced by improved nutrition and public health, not medication and surgery. Mass immunization programs were viewed as an appropriate function of civic government.
The introduction of polio vaccine in the 1950s made a large impact. Families lined up at any opportunity to get the vaccine. Polio went from hundreds of thousands of cases of paralysis each summer down to zero cases of wild polio transmitted within the western hemisphere. Measles cases went from 450,000 cases a year in the early 1960s down to zero, until a fraudulent link to autism led to a significant number of parents not immunizing their children. Vaccine refusal, previously a rare ethical issue related to religious liberty, became corrupted by efforts at boutique medicine and alternative facts. In modern America, the ethics of individualism and personal rights have eclipsed civic responsibility. With herd immunity compromised, a blip up to 100 cases of measles per year was histrionically described as a huge epidemic. That spin shows ignorance of the historical record, but the risk was enough for the liberal state of California in 2015 to ban philosophical exemptions to vaccination with one of the strictest state laws in the nation.
Ethics is about values. So, as I look at the changes over 50 years, the areas that have failed to make progress are illuminating. Mental health care for children has not made the same progress achieved with vaccines and cancer therapy. My most recent clinical ethics case involved a teenager who had made a suicidal gesture by taking a handful of pills. The nurses were caught between caring for their patient and meeting the demands of an upset, authoritarian parent in a world where customer satisfaction is critical. I spent much of the night exploring hospital policy and state law. I solicited and listened to widely disparate interpretations of law, medical ethics, and hospital policy from the floor nurse, the nursing supervisor, the nursing staff on the adult inpatient psychiatric unit, three ED docs, a social worker, a government agency, and a judge’s representative. The physician of 1967 was captain of the ship and would not recognize the chaotic teamwork of modern medicine. The exercise showed me how little progress we have made in mental health care for adolescents during my 25 years of practice.
It also reminded me that I have the luxury to debate ethical minutia like vaccine hesitancy and adolescent consent in a world with Syrian refugee camps and starvation in South Sudan. Mahatma Gandhi said, “There are people in the world so hungry that God cannot appear to them except in the form of bread.” That, unfortunately, has not changed in 50 years.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@frontlinemedcom.com.
References
1. www.hhs.gov/ohrp/regulations-and-policy/belmont-report/
2. Pediatrics 1995;95:314-7.
3. JAMA. 1968;205(6):337-40.
4. Family Law Quarterly. 2008 Fall;42(3):449-63.
5. JAMA. 1962;181(1):17-24.
6. National Child Abuse and Neglect Training and Publications Project (2014). The Child Abuse Prevention and Treatment Act: 40 years of safeguarding America’s children. Washington: U.S. Department of Health and Human Services, Children’s Bureau.
7. Kennedy Inst Ethics J. 2006 Sep;16(3):205-24.
Cooperation must overcome polarization
Each profession has its own core set of knowledge, skills, and values. For physicians, the core set of knowledge is anatomy, pathophysiology, and pharmacology. Skills include taking a history, the physical exam, and surgical procedures. The core values traditionally have been compassion and altruism. For modern medical practice, I urge adding cooperation as a core value. Medical school and the apprenticeship of residency are designed to teach, role model, foster, develop, and groom these core competencies.
Getting into medical school is highly competitive. Medical training uses methods that are very different than those used to train elite Olympic and professional athletes. Some competitiveness persists in medical school, but in general the faculty emphasizes cooperation rather than competition. The metric is not whether one student or resident is better than another. Gold and silver medals are not awarded. It is about whether each physician-to-be has passed the milestones needed to practice medicine.
But American health care is threatened by the continued polarization of our government and our society. For years both Cleveland Clinic and Dana Farber have held annual fundraising events at Mar-a-Lago. In February 2017, because of that location’s association with President Trump, some people associated with the organizations advocated boycotting those important fund-raisers. These past few months, it seems every action and every purchase has become a political statement. One restaurant mentioned immigrants on its receipt. The action went viral and caused other people to advocate boycotting the restaurant or not tipping the wait staff (“The new political battleground: Your restaurant receipt,” The Washington Post, by Maura Judkis, Feb. 14, 2017).
Secondary boycotts are an ethical quandary. In labor disputes, organized unions can go on strike. In the 1970s, Japanese cars were not welcome in the employee parking lot of a Ford assembly plant. People do vote with their pocketbook. But in labor disputes, there are legal restrictions on secondary boycotts against other companies. People do need to get along with their neighbors and so do businesses. Politics is the art of encouraging cooperation on one project amongst people who disagree about the goals of many other proposed projects. The Preamble to the United States Constitution enumerates the benefits of cooperation.
In any large-scale human endeavor, conflicts arise that may limit cooperation. Accommodating conscientious objection is the safety valve that permits cooperation when dealing with contested government endeavors such as war, abortion, and physician-assisted suicide. It is meant as a last ditch effort to maintain cohesion of both societal and individual moral integrity. But if every proposed action is met with votes divided along party lines, conscientious objection loses its moral high ground.
Judge Neil Gorsuch, the nominee for the U.S. Supreme Court, has a record of supporting religious freedom in Yellowbear v. Lambert (10th Cir. 2014). He would likely support conscientious objection in relation to assisted dying by physicians, contrary to the arguments made recently by bioethicists Julian Savulescu and Udo Schuklenk. In related news, the liberty of physicians to address gun safety was affirmed when a Florida appeals court upheld the overturning of the state’s Privacy of Firearm Owners Act.
Summing up a tumultuous month of medical ethics, I leave you with the words of Voltaire: “Cherish those who seek the truth but beware of those who find it.”
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@frontlinemedcom.com.
Each profession has its own core set of knowledge, skills, and values. For physicians, the core set of knowledge is anatomy, pathophysiology, and pharmacology. Skills include taking a history, the physical exam, and surgical procedures. The core values traditionally have been compassion and altruism. For modern medical practice, I urge adding cooperation as a core value. Medical school and the apprenticeship of residency are designed to teach, role model, foster, develop, and groom these core competencies.
Getting into medical school is highly competitive. Medical training uses methods that are very different than those used to train elite Olympic and professional athletes. Some competitiveness persists in medical school, but in general the faculty emphasizes cooperation rather than competition. The metric is not whether one student or resident is better than another. Gold and silver medals are not awarded. It is about whether each physician-to-be has passed the milestones needed to practice medicine.
But American health care is threatened by the continued polarization of our government and our society. For years both Cleveland Clinic and Dana Farber have held annual fundraising events at Mar-a-Lago. In February 2017, because of that location’s association with President Trump, some people associated with the organizations advocated boycotting those important fund-raisers. These past few months, it seems every action and every purchase has become a political statement. One restaurant mentioned immigrants on its receipt. The action went viral and caused other people to advocate boycotting the restaurant or not tipping the wait staff (“The new political battleground: Your restaurant receipt,” The Washington Post, by Maura Judkis, Feb. 14, 2017).
Secondary boycotts are an ethical quandary. In labor disputes, organized unions can go on strike. In the 1970s, Japanese cars were not welcome in the employee parking lot of a Ford assembly plant. People do vote with their pocketbook. But in labor disputes, there are legal restrictions on secondary boycotts against other companies. People do need to get along with their neighbors and so do businesses. Politics is the art of encouraging cooperation on one project amongst people who disagree about the goals of many other proposed projects. The Preamble to the United States Constitution enumerates the benefits of cooperation.
In any large-scale human endeavor, conflicts arise that may limit cooperation. Accommodating conscientious objection is the safety valve that permits cooperation when dealing with contested government endeavors such as war, abortion, and physician-assisted suicide. It is meant as a last ditch effort to maintain cohesion of both societal and individual moral integrity. But if every proposed action is met with votes divided along party lines, conscientious objection loses its moral high ground.
Judge Neil Gorsuch, the nominee for the U.S. Supreme Court, has a record of supporting religious freedom in Yellowbear v. Lambert (10th Cir. 2014). He would likely support conscientious objection in relation to assisted dying by physicians, contrary to the arguments made recently by bioethicists Julian Savulescu and Udo Schuklenk. In related news, the liberty of physicians to address gun safety was affirmed when a Florida appeals court upheld the overturning of the state’s Privacy of Firearm Owners Act.
Summing up a tumultuous month of medical ethics, I leave you with the words of Voltaire: “Cherish those who seek the truth but beware of those who find it.”
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@frontlinemedcom.com.
Each profession has its own core set of knowledge, skills, and values. For physicians, the core set of knowledge is anatomy, pathophysiology, and pharmacology. Skills include taking a history, the physical exam, and surgical procedures. The core values traditionally have been compassion and altruism. For modern medical practice, I urge adding cooperation as a core value. Medical school and the apprenticeship of residency are designed to teach, role model, foster, develop, and groom these core competencies.
Getting into medical school is highly competitive. Medical training uses methods that are very different than those used to train elite Olympic and professional athletes. Some competitiveness persists in medical school, but in general the faculty emphasizes cooperation rather than competition. The metric is not whether one student or resident is better than another. Gold and silver medals are not awarded. It is about whether each physician-to-be has passed the milestones needed to practice medicine.
But American health care is threatened by the continued polarization of our government and our society. For years both Cleveland Clinic and Dana Farber have held annual fundraising events at Mar-a-Lago. In February 2017, because of that location’s association with President Trump, some people associated with the organizations advocated boycotting those important fund-raisers. These past few months, it seems every action and every purchase has become a political statement. One restaurant mentioned immigrants on its receipt. The action went viral and caused other people to advocate boycotting the restaurant or not tipping the wait staff (“The new political battleground: Your restaurant receipt,” The Washington Post, by Maura Judkis, Feb. 14, 2017).
Secondary boycotts are an ethical quandary. In labor disputes, organized unions can go on strike. In the 1970s, Japanese cars were not welcome in the employee parking lot of a Ford assembly plant. People do vote with their pocketbook. But in labor disputes, there are legal restrictions on secondary boycotts against other companies. People do need to get along with their neighbors and so do businesses. Politics is the art of encouraging cooperation on one project amongst people who disagree about the goals of many other proposed projects. The Preamble to the United States Constitution enumerates the benefits of cooperation.
In any large-scale human endeavor, conflicts arise that may limit cooperation. Accommodating conscientious objection is the safety valve that permits cooperation when dealing with contested government endeavors such as war, abortion, and physician-assisted suicide. It is meant as a last ditch effort to maintain cohesion of both societal and individual moral integrity. But if every proposed action is met with votes divided along party lines, conscientious objection loses its moral high ground.
Judge Neil Gorsuch, the nominee for the U.S. Supreme Court, has a record of supporting religious freedom in Yellowbear v. Lambert (10th Cir. 2014). He would likely support conscientious objection in relation to assisted dying by physicians, contrary to the arguments made recently by bioethicists Julian Savulescu and Udo Schuklenk. In related news, the liberty of physicians to address gun safety was affirmed when a Florida appeals court upheld the overturning of the state’s Privacy of Firearm Owners Act.
Summing up a tumultuous month of medical ethics, I leave you with the words of Voltaire: “Cherish those who seek the truth but beware of those who find it.”
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@frontlinemedcom.com.
Scientific skepticism
Contrary to popular belief, great scientists do not spend their days proving that their new ideas are correct. That is just the romantic portrait of the field that is taught to schoolchildren. The reality is that great scientists do everything they can think of to disprove their theories. They exhaustively consider all other plausible explanations, challenge any potential bias in their methodology, rule out random flukes in the data collection, and refine any error in the data measurement. Only after doing all that, when no other conclusion is possible, do true scientists publish their new theories as truth. Then they await confirmation from their peers.
That is the philosophy behind the modern scientific method. In the hard sciences like chemistry and physics, this paradigm is reinforced because a scientist stakes his or her reputation on every publication. Funding from various government agencies often is controlled by peers in the field. If published work is inaccurate, the likelihood of receiving funding is markedly diminished.
Medicine has a long history of being biased by the belief that its therapies work. Even faith healers who consider themselves scientists will cite repeated examples of personal success as evidence that their approach works. However, they were looking for confirmation. To truly be a scientist, one cannot seek to affirm one’s beliefs. One must to the best of one’s ability seek to disprove them.
In 2016, postmodern voices have challenged the very existence of truth. The falsehoods rampant in politics have spilled over into a distrust of science. This distrust is manifest in vaccine deniers and the debate about climate change. There are a few charlatans and mercenaries in every field who sell their soul and skills to the highest bidder. Science is no exception. These disreputable scientists seek to obfuscate rather than clarify. They have been employed by the tobacco industry, the oil industry, and various groups with agendas other than seeking truth. They, with the help of weak journalism, have tainted the perception of science in the public arena. The uproar has prominent scientists defending the scientific method and arguing for science as the determiner of facts. Sen. Daniel Patrick Moynihan once said, “Everyone is entitled to his own opinion, but not to his own facts.”
In the 19th century, hawking snake oil was big business. In the early 20th century, the ethical drug industry was created in the United States. The Pure Food and Drug Act of 1906 and the Federal Food, Drug, and Cosmetic Act of 1938 empowered the Food and Drug Administration to regulate what has become 25% of U.S. industry. Those regulations demand honest labeling, good manufacturing processes, proof of efficacy, and an assessment of safety. The FDA deals with many stakeholders in the process for approving new drugs. The system is an imperfect balance between getting lifesaving new discoveries to market quickly while avoiding disasters. The most recent news has been the head of the FDA defending the need for proof of effectiveness in addition to proof of safety.
Even after a year in which truth seemed elusive and science hit a low point in prestige, it is still bizarre to me that the government would consider turning the drug industry into one in which proof of effectiveness is not a minimum requirement. That is postmodern thinking run amok. But the root of the problem lies deeper. When scientists stop being skeptics and instead focus on finding something publishable, the temptation is already leading them along the road illuminated by Dante Alighieri.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis.
Contrary to popular belief, great scientists do not spend their days proving that their new ideas are correct. That is just the romantic portrait of the field that is taught to schoolchildren. The reality is that great scientists do everything they can think of to disprove their theories. They exhaustively consider all other plausible explanations, challenge any potential bias in their methodology, rule out random flukes in the data collection, and refine any error in the data measurement. Only after doing all that, when no other conclusion is possible, do true scientists publish their new theories as truth. Then they await confirmation from their peers.
That is the philosophy behind the modern scientific method. In the hard sciences like chemistry and physics, this paradigm is reinforced because a scientist stakes his or her reputation on every publication. Funding from various government agencies often is controlled by peers in the field. If published work is inaccurate, the likelihood of receiving funding is markedly diminished.
Medicine has a long history of being biased by the belief that its therapies work. Even faith healers who consider themselves scientists will cite repeated examples of personal success as evidence that their approach works. However, they were looking for confirmation. To truly be a scientist, one cannot seek to affirm one’s beliefs. One must to the best of one’s ability seek to disprove them.
In 2016, postmodern voices have challenged the very existence of truth. The falsehoods rampant in politics have spilled over into a distrust of science. This distrust is manifest in vaccine deniers and the debate about climate change. There are a few charlatans and mercenaries in every field who sell their soul and skills to the highest bidder. Science is no exception. These disreputable scientists seek to obfuscate rather than clarify. They have been employed by the tobacco industry, the oil industry, and various groups with agendas other than seeking truth. They, with the help of weak journalism, have tainted the perception of science in the public arena. The uproar has prominent scientists defending the scientific method and arguing for science as the determiner of facts. Sen. Daniel Patrick Moynihan once said, “Everyone is entitled to his own opinion, but not to his own facts.”
In the 19th century, hawking snake oil was big business. In the early 20th century, the ethical drug industry was created in the United States. The Pure Food and Drug Act of 1906 and the Federal Food, Drug, and Cosmetic Act of 1938 empowered the Food and Drug Administration to regulate what has become 25% of U.S. industry. Those regulations demand honest labeling, good manufacturing processes, proof of efficacy, and an assessment of safety. The FDA deals with many stakeholders in the process for approving new drugs. The system is an imperfect balance between getting lifesaving new discoveries to market quickly while avoiding disasters. The most recent news has been the head of the FDA defending the need for proof of effectiveness in addition to proof of safety.
Even after a year in which truth seemed elusive and science hit a low point in prestige, it is still bizarre to me that the government would consider turning the drug industry into one in which proof of effectiveness is not a minimum requirement. That is postmodern thinking run amok. But the root of the problem lies deeper. When scientists stop being skeptics and instead focus on finding something publishable, the temptation is already leading them along the road illuminated by Dante Alighieri.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis.
Contrary to popular belief, great scientists do not spend their days proving that their new ideas are correct. That is just the romantic portrait of the field that is taught to schoolchildren. The reality is that great scientists do everything they can think of to disprove their theories. They exhaustively consider all other plausible explanations, challenge any potential bias in their methodology, rule out random flukes in the data collection, and refine any error in the data measurement. Only after doing all that, when no other conclusion is possible, do true scientists publish their new theories as truth. Then they await confirmation from their peers.
That is the philosophy behind the modern scientific method. In the hard sciences like chemistry and physics, this paradigm is reinforced because a scientist stakes his or her reputation on every publication. Funding from various government agencies often is controlled by peers in the field. If published work is inaccurate, the likelihood of receiving funding is markedly diminished.
Medicine has a long history of being biased by the belief that its therapies work. Even faith healers who consider themselves scientists will cite repeated examples of personal success as evidence that their approach works. However, they were looking for confirmation. To truly be a scientist, one cannot seek to affirm one’s beliefs. One must to the best of one’s ability seek to disprove them.
In 2016, postmodern voices have challenged the very existence of truth. The falsehoods rampant in politics have spilled over into a distrust of science. This distrust is manifest in vaccine deniers and the debate about climate change. There are a few charlatans and mercenaries in every field who sell their soul and skills to the highest bidder. Science is no exception. These disreputable scientists seek to obfuscate rather than clarify. They have been employed by the tobacco industry, the oil industry, and various groups with agendas other than seeking truth. They, with the help of weak journalism, have tainted the perception of science in the public arena. The uproar has prominent scientists defending the scientific method and arguing for science as the determiner of facts. Sen. Daniel Patrick Moynihan once said, “Everyone is entitled to his own opinion, but not to his own facts.”
In the 19th century, hawking snake oil was big business. In the early 20th century, the ethical drug industry was created in the United States. The Pure Food and Drug Act of 1906 and the Federal Food, Drug, and Cosmetic Act of 1938 empowered the Food and Drug Administration to regulate what has become 25% of U.S. industry. Those regulations demand honest labeling, good manufacturing processes, proof of efficacy, and an assessment of safety. The FDA deals with many stakeholders in the process for approving new drugs. The system is an imperfect balance between getting lifesaving new discoveries to market quickly while avoiding disasters. The most recent news has been the head of the FDA defending the need for proof of effectiveness in addition to proof of safety.
Even after a year in which truth seemed elusive and science hit a low point in prestige, it is still bizarre to me that the government would consider turning the drug industry into one in which proof of effectiveness is not a minimum requirement. That is postmodern thinking run amok. But the root of the problem lies deeper. When scientists stop being skeptics and instead focus on finding something publishable, the temptation is already leading them along the road illuminated by Dante Alighieri.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis.
The march of technology
Each year the American Academy of Pediatrics National Conference and Exhibition fills a huge convention hall with the latest products that can improve health and generate practice revenue.
Some products are solutions to the minor annoyances of everyday practice. For instance, there are ear curettes equipped with their own LED light and a magnifying lens. There are countless creams to treat rashes. There are new automated devices for testing hearing, vision, and attention. And at the far extreme, there are products with the potential to revolutionize clinical care or to bankrupt it. The latest technology in that category is whole exome sequencing.
A couple weeks earlier I had listened to a national meeting of pediatric ethicists discuss this technology. Some proponents discussed the possibility of doing whole exome sequencing (WES) for every newborn. Alas, many ethicists can’t do math. Even if the cost goes below $1,000 per test, at 4 million babies per year in the United States, that is $4 billion per year. That sounds like a small sum, compared with the current federal deficit, but the original budget for the entire, 10-year-long Human Genome Project (HGP) was $4.5 billion. There were complaints in that era that diverting such an enormous amount of money into the HGP would cut the funding of a lot of other very good research at the National Institutes of Health. Conversely, Medicare spends $4.5 billion on hepatitis C treatment.
Viewed differently, the yearly per capita payment to general pediatricians, excluding vaccine costs, is around $1,000. Perhaps I’m biased, but I think I provide much more value than a genetic sequence.
Precision medicine has a lot of potential. So far, it is mostly potential. One colleague related that, in the past year, he has done WES on three patients, at about $4,000 charge for each, and gotten positive results in two cases. He figures soon he will be ordering it on every child with symptoms of autism, developmental delay, or failure to thrive. Is that a wise idea? That, it seems, is the area in which there is the least illuminating research.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis.
Each year the American Academy of Pediatrics National Conference and Exhibition fills a huge convention hall with the latest products that can improve health and generate practice revenue.
Some products are solutions to the minor annoyances of everyday practice. For instance, there are ear curettes equipped with their own LED light and a magnifying lens. There are countless creams to treat rashes. There are new automated devices for testing hearing, vision, and attention. And at the far extreme, there are products with the potential to revolutionize clinical care or to bankrupt it. The latest technology in that category is whole exome sequencing.
A couple weeks earlier I had listened to a national meeting of pediatric ethicists discuss this technology. Some proponents discussed the possibility of doing whole exome sequencing (WES) for every newborn. Alas, many ethicists can’t do math. Even if the cost goes below $1,000 per test, at 4 million babies per year in the United States, that is $4 billion per year. That sounds like a small sum, compared with the current federal deficit, but the original budget for the entire, 10-year-long Human Genome Project (HGP) was $4.5 billion. There were complaints in that era that diverting such an enormous amount of money into the HGP would cut the funding of a lot of other very good research at the National Institutes of Health. Conversely, Medicare spends $4.5 billion on hepatitis C treatment.
Viewed differently, the yearly per capita payment to general pediatricians, excluding vaccine costs, is around $1,000. Perhaps I’m biased, but I think I provide much more value than a genetic sequence.
Precision medicine has a lot of potential. So far, it is mostly potential. One colleague related that, in the past year, he has done WES on three patients, at about $4,000 charge for each, and gotten positive results in two cases. He figures soon he will be ordering it on every child with symptoms of autism, developmental delay, or failure to thrive. Is that a wise idea? That, it seems, is the area in which there is the least illuminating research.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis.
Each year the American Academy of Pediatrics National Conference and Exhibition fills a huge convention hall with the latest products that can improve health and generate practice revenue.
Some products are solutions to the minor annoyances of everyday practice. For instance, there are ear curettes equipped with their own LED light and a magnifying lens. There are countless creams to treat rashes. There are new automated devices for testing hearing, vision, and attention. And at the far extreme, there are products with the potential to revolutionize clinical care or to bankrupt it. The latest technology in that category is whole exome sequencing.
A couple weeks earlier I had listened to a national meeting of pediatric ethicists discuss this technology. Some proponents discussed the possibility of doing whole exome sequencing (WES) for every newborn. Alas, many ethicists can’t do math. Even if the cost goes below $1,000 per test, at 4 million babies per year in the United States, that is $4 billion per year. That sounds like a small sum, compared with the current federal deficit, but the original budget for the entire, 10-year-long Human Genome Project (HGP) was $4.5 billion. There were complaints in that era that diverting such an enormous amount of money into the HGP would cut the funding of a lot of other very good research at the National Institutes of Health. Conversely, Medicare spends $4.5 billion on hepatitis C treatment.
Viewed differently, the yearly per capita payment to general pediatricians, excluding vaccine costs, is around $1,000. Perhaps I’m biased, but I think I provide much more value than a genetic sequence.
Precision medicine has a lot of potential. So far, it is mostly potential. One colleague related that, in the past year, he has done WES on three patients, at about $4,000 charge for each, and gotten positive results in two cases. He figures soon he will be ordering it on every child with symptoms of autism, developmental delay, or failure to thrive. Is that a wise idea? That, it seems, is the area in which there is the least illuminating research.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis.
Hospital medicine
It is important to step back occasionally to survey where one has been and to plot a new heading. In an online Aug. 10, 2016, release, the New England Journal of Medicine posted two opinion pieces that provide perspective on hospital medicine. As is often the case when journalism presents two opinions, the viewpoints represent opposite ends of a spectrum and the truth lies somewhere in between.
In one essay, Robert Wachter, MD, and Lee Goldman, MD, highlight the successful growth of hospital medicine (N Eng J Med. 2016, Aug 10. doi: 10.1056/NEJMp1607958). In just 2 decades, more than 50,000 physicians have changed their focus to the care of inpatients. The authors state that “many stars had to align” for hospital medicine to grow as rapidly as it has. I would argue instead that many talented leaders of the field have moved heaven and earth to create that alignment and birth this field.
In the other essay, Richard Gunderman, MD, focuses on what he sees as having been lost in this evolution (N Eng J Med. 2016, Aug 10. doi: 10.1056/NEJMp1608289). I believe Dr. Gunderman’s viewpoint nostalgically longs for the good old days and a model of an interpersonal doctor-patient relationship that never really existed for a large portion of the population. If you were wealthy, lived most of your life in one location, and had only intermittent or common diseases, then perhaps you had a trusted general internist to provide your medical care and provide the emotional reassurance that nourished both patient and doctor. But in modern medicine, that scenario is uncommon. With large group practices, there is only a small chance that your personal physician will be on call on the night of your admission to a hospital. The next day, as test results and specialty consults trickle in, that personal physician will be trapped in a busy outpatient clinic and not truly available at hospital bedside in “your moment of greatest need,” as Dr. Gunderman phrased it. When your personal physician finally does make rounds, s/he will find the hospital environment inefficient and repeating the same small mistakes that happened to his/her last patient.
I’ve been writing about and teaching professionalism for years. I agree with Dr. Gunderman about the importance of a doctor-patient relationship. I believe reducing physicians to being automatons in a hospital assembly line would be a bad idea. But this essay’s rose-colored and sienna-colored portrait of that relationship is not helpful guidance in the modern world. Surveyors and navigators need sharp, clear vision.
Trade-offs are being made. Many pediatricians in affluent communities do have the opportunity to establish long-term relationships with families, sometimes for multiple generations of children. Those relationships attract medical students into pediatrics and family medicine. I was fortunate enough to establish many of those relationships when I practiced outpatient pediatrics. During my last interstate move, the man packing the picture frames was amused to find amidst my many diplomas a framed crayon drawing. It was a gift to me from a young patient. I told the mover that I would be sadder to have that drawing damaged than if a diploma was damaged in the move. So he wrapped it with extra padding.
Those bonds established with families make up the emotional sustenance throughout a career that justifies the years of sacrifice spent becoming a physician. There is no doubt that it is easier to form those bonds in outpatient pediatrics. At a community hospital, with 7 days on/7 days off scheduling, I usually provide care for the entire hospitalization of a child. That provides emotional satisfaction for both the parents and for me as a physician in ways that 12-hour shifts usually don’t.
The diminishment of those relationships needs to be acknowledged, but not to the exclusion of what a hospitalist can provide. When I practiced general pediatrics and only admitted 1 or 2 children each week, I was often frustrated by inefficiency and errors in the hospital, but I had little recourse for changing it. As a hospitalist admitting 500 patients per year, I can perform problem solving and devote resources to continuously improve the quality and safety of inpatient care. I provide those improvements to all patients admitted to the hospital, whether they have a medical home or not. That fosters social justice. As a function-over-fashion person, that success is emotionally rewarding, too.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@frontlinemedcom.com.
It is important to step back occasionally to survey where one has been and to plot a new heading. In an online Aug. 10, 2016, release, the New England Journal of Medicine posted two opinion pieces that provide perspective on hospital medicine. As is often the case when journalism presents two opinions, the viewpoints represent opposite ends of a spectrum and the truth lies somewhere in between.
In one essay, Robert Wachter, MD, and Lee Goldman, MD, highlight the successful growth of hospital medicine (N Eng J Med. 2016, Aug 10. doi: 10.1056/NEJMp1607958). In just 2 decades, more than 50,000 physicians have changed their focus to the care of inpatients. The authors state that “many stars had to align” for hospital medicine to grow as rapidly as it has. I would argue instead that many talented leaders of the field have moved heaven and earth to create that alignment and birth this field.
In the other essay, Richard Gunderman, MD, focuses on what he sees as having been lost in this evolution (N Eng J Med. 2016, Aug 10. doi: 10.1056/NEJMp1608289). I believe Dr. Gunderman’s viewpoint nostalgically longs for the good old days and a model of an interpersonal doctor-patient relationship that never really existed for a large portion of the population. If you were wealthy, lived most of your life in one location, and had only intermittent or common diseases, then perhaps you had a trusted general internist to provide your medical care and provide the emotional reassurance that nourished both patient and doctor. But in modern medicine, that scenario is uncommon. With large group practices, there is only a small chance that your personal physician will be on call on the night of your admission to a hospital. The next day, as test results and specialty consults trickle in, that personal physician will be trapped in a busy outpatient clinic and not truly available at hospital bedside in “your moment of greatest need,” as Dr. Gunderman phrased it. When your personal physician finally does make rounds, s/he will find the hospital environment inefficient and repeating the same small mistakes that happened to his/her last patient.
I’ve been writing about and teaching professionalism for years. I agree with Dr. Gunderman about the importance of a doctor-patient relationship. I believe reducing physicians to being automatons in a hospital assembly line would be a bad idea. But this essay’s rose-colored and sienna-colored portrait of that relationship is not helpful guidance in the modern world. Surveyors and navigators need sharp, clear vision.
Trade-offs are being made. Many pediatricians in affluent communities do have the opportunity to establish long-term relationships with families, sometimes for multiple generations of children. Those relationships attract medical students into pediatrics and family medicine. I was fortunate enough to establish many of those relationships when I practiced outpatient pediatrics. During my last interstate move, the man packing the picture frames was amused to find amidst my many diplomas a framed crayon drawing. It was a gift to me from a young patient. I told the mover that I would be sadder to have that drawing damaged than if a diploma was damaged in the move. So he wrapped it with extra padding.
Those bonds established with families make up the emotional sustenance throughout a career that justifies the years of sacrifice spent becoming a physician. There is no doubt that it is easier to form those bonds in outpatient pediatrics. At a community hospital, with 7 days on/7 days off scheduling, I usually provide care for the entire hospitalization of a child. That provides emotional satisfaction for both the parents and for me as a physician in ways that 12-hour shifts usually don’t.
The diminishment of those relationships needs to be acknowledged, but not to the exclusion of what a hospitalist can provide. When I practiced general pediatrics and only admitted 1 or 2 children each week, I was often frustrated by inefficiency and errors in the hospital, but I had little recourse for changing it. As a hospitalist admitting 500 patients per year, I can perform problem solving and devote resources to continuously improve the quality and safety of inpatient care. I provide those improvements to all patients admitted to the hospital, whether they have a medical home or not. That fosters social justice. As a function-over-fashion person, that success is emotionally rewarding, too.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@frontlinemedcom.com.
It is important to step back occasionally to survey where one has been and to plot a new heading. In an online Aug. 10, 2016, release, the New England Journal of Medicine posted two opinion pieces that provide perspective on hospital medicine. As is often the case when journalism presents two opinions, the viewpoints represent opposite ends of a spectrum and the truth lies somewhere in between.
In one essay, Robert Wachter, MD, and Lee Goldman, MD, highlight the successful growth of hospital medicine (N Eng J Med. 2016, Aug 10. doi: 10.1056/NEJMp1607958). In just 2 decades, more than 50,000 physicians have changed their focus to the care of inpatients. The authors state that “many stars had to align” for hospital medicine to grow as rapidly as it has. I would argue instead that many talented leaders of the field have moved heaven and earth to create that alignment and birth this field.
In the other essay, Richard Gunderman, MD, focuses on what he sees as having been lost in this evolution (N Eng J Med. 2016, Aug 10. doi: 10.1056/NEJMp1608289). I believe Dr. Gunderman’s viewpoint nostalgically longs for the good old days and a model of an interpersonal doctor-patient relationship that never really existed for a large portion of the population. If you were wealthy, lived most of your life in one location, and had only intermittent or common diseases, then perhaps you had a trusted general internist to provide your medical care and provide the emotional reassurance that nourished both patient and doctor. But in modern medicine, that scenario is uncommon. With large group practices, there is only a small chance that your personal physician will be on call on the night of your admission to a hospital. The next day, as test results and specialty consults trickle in, that personal physician will be trapped in a busy outpatient clinic and not truly available at hospital bedside in “your moment of greatest need,” as Dr. Gunderman phrased it. When your personal physician finally does make rounds, s/he will find the hospital environment inefficient and repeating the same small mistakes that happened to his/her last patient.
I’ve been writing about and teaching professionalism for years. I agree with Dr. Gunderman about the importance of a doctor-patient relationship. I believe reducing physicians to being automatons in a hospital assembly line would be a bad idea. But this essay’s rose-colored and sienna-colored portrait of that relationship is not helpful guidance in the modern world. Surveyors and navigators need sharp, clear vision.
Trade-offs are being made. Many pediatricians in affluent communities do have the opportunity to establish long-term relationships with families, sometimes for multiple generations of children. Those relationships attract medical students into pediatrics and family medicine. I was fortunate enough to establish many of those relationships when I practiced outpatient pediatrics. During my last interstate move, the man packing the picture frames was amused to find amidst my many diplomas a framed crayon drawing. It was a gift to me from a young patient. I told the mover that I would be sadder to have that drawing damaged than if a diploma was damaged in the move. So he wrapped it with extra padding.
Those bonds established with families make up the emotional sustenance throughout a career that justifies the years of sacrifice spent becoming a physician. There is no doubt that it is easier to form those bonds in outpatient pediatrics. At a community hospital, with 7 days on/7 days off scheduling, I usually provide care for the entire hospitalization of a child. That provides emotional satisfaction for both the parents and for me as a physician in ways that 12-hour shifts usually don’t.
The diminishment of those relationships needs to be acknowledged, but not to the exclusion of what a hospitalist can provide. When I practiced general pediatrics and only admitted 1 or 2 children each week, I was often frustrated by inefficiency and errors in the hospital, but I had little recourse for changing it. As a hospitalist admitting 500 patients per year, I can perform problem solving and devote resources to continuously improve the quality and safety of inpatient care. I provide those improvements to all patients admitted to the hospital, whether they have a medical home or not. That fosters social justice. As a function-over-fashion person, that success is emotionally rewarding, too.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@frontlinemedcom.com.
The balm of reassurance
A toddler has had several brief episodes of mild perioral cyanosis noticed at day care. The parents see the primary care provider. The exam is normal. The child is admitted for a work-up. The CBC and comprehensive metabolic profile are unremarkable. The chest x-ray is normal. An ECG is normal. An echocardiogram is normal. The EEG is normal. Now what?
I was taught that an uncommon presentation of a common disease is still more common than a common presentation of an uncommon disease. Or simply, odd-looking horses are more common than zebras unless you practice in the savanna. There is a point in any safari at which you have to decide whether you are hunting a zebra or chasing a shadow. Clinical judgment is balancing the risk of missing something preventable that will actually harm the child against the harms of more tests.
The modern hospital has an array of equipment available. They are Greek Sirens calling to us. There is the video EEG room, the MR angiogram, the cardiac cath lab, and an endless list of blood tests. We are not even stopped by the walls of the hospital. We can order a follow-up ambulatory Holter ECG to search for intermittent arrhythmias. But are these Sirens really good medicine? At what point should we simply reassure the parents that the child is fine?
Physicians all worry about missing something. This fear was instilled when we were medical students and reinforced with the stress of residency. With years of experience, all physicians acquire a list of missed diagnoses. But I also have collected a list of times when the diagnostic tests themselves have caused harm, including death. I have a list of cases where nonspecific diagnostic testing has mislabeled a child with an obscure diagnosis that was later proven false, but not before harm was caused. There were patients with Stevens-Johnson syndrome who suffered serious harm from treatments for minor illnesses. Then there were the terrified families who, after extensive testing, became convinced that the child must have some horrible unknown disease because surely we wouldn’t have traumatized the child with all this work-up if there wasn’t really something seriously wrong. Each new test stoked their fear rather than soothed it.
A careful history is still the weapon of choice in the zebra hunt. On a first presentation of mild cyanosis, sepsis is the charging rhinoceros of preventable harm that will run you over if you are too slow to react. But this child has now had several episodes that have occurred: 1. in multiple settings, 2. with no distress, 3. while the child remained playful, and 4. that were self-limited. That history is incompatible with sepsis, so reflexively ordering a blood culture is an illogical choice. The history should be progressively explored using the differential diagnosis and an organ-based systematic approach to guide it. The thoroughness and thoughtfulness I put into the history taking can be key to finding the correct diagnosis. They also are a means of building trust and rapport with the parents. That will be important later if no definitive diagnosis is found.
Unclear and unusual presentations may merit a consult. The cardiologist knows the limits of an echo. Along with the technical expertise comes a new set of eyes and the additional perspective of a second opinion. It is great when a colleague can tell you that he or she too had a case like this years ago that was never solved, but did resolve on its own.
One advantage of being an office-based pediatrician, with an established relationship with a family over several years and a couple other children, is that parents do value and trust your clinical judgment. As a pediatrician, I know the most common product I sell is reassurance. It is not snake oil. There is a bedside manner in selling it. Put a positive spin on all the negative tests. Indicate that you and the parents can be vigilant in watching for new signs. Instruct the parents to bring the child back if the events are distressing for the child, which could justify more invasive testing. Arrange to recheck the child in the office in a week, then a month, then at the next well visit. Parents know that medicine isn’t perfect. Humans deal with fear and uncertainty better by knowing we aren’t facing the future alone. And that is why even with all this technology, I still lay a stethoscope on every child.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures.
A toddler has had several brief episodes of mild perioral cyanosis noticed at day care. The parents see the primary care provider. The exam is normal. The child is admitted for a work-up. The CBC and comprehensive metabolic profile are unremarkable. The chest x-ray is normal. An ECG is normal. An echocardiogram is normal. The EEG is normal. Now what?
I was taught that an uncommon presentation of a common disease is still more common than a common presentation of an uncommon disease. Or simply, odd-looking horses are more common than zebras unless you practice in the savanna. There is a point in any safari at which you have to decide whether you are hunting a zebra or chasing a shadow. Clinical judgment is balancing the risk of missing something preventable that will actually harm the child against the harms of more tests.
The modern hospital has an array of equipment available. They are Greek Sirens calling to us. There is the video EEG room, the MR angiogram, the cardiac cath lab, and an endless list of blood tests. We are not even stopped by the walls of the hospital. We can order a follow-up ambulatory Holter ECG to search for intermittent arrhythmias. But are these Sirens really good medicine? At what point should we simply reassure the parents that the child is fine?
Physicians all worry about missing something. This fear was instilled when we were medical students and reinforced with the stress of residency. With years of experience, all physicians acquire a list of missed diagnoses. But I also have collected a list of times when the diagnostic tests themselves have caused harm, including death. I have a list of cases where nonspecific diagnostic testing has mislabeled a child with an obscure diagnosis that was later proven false, but not before harm was caused. There were patients with Stevens-Johnson syndrome who suffered serious harm from treatments for minor illnesses. Then there were the terrified families who, after extensive testing, became convinced that the child must have some horrible unknown disease because surely we wouldn’t have traumatized the child with all this work-up if there wasn’t really something seriously wrong. Each new test stoked their fear rather than soothed it.
A careful history is still the weapon of choice in the zebra hunt. On a first presentation of mild cyanosis, sepsis is the charging rhinoceros of preventable harm that will run you over if you are too slow to react. But this child has now had several episodes that have occurred: 1. in multiple settings, 2. with no distress, 3. while the child remained playful, and 4. that were self-limited. That history is incompatible with sepsis, so reflexively ordering a blood culture is an illogical choice. The history should be progressively explored using the differential diagnosis and an organ-based systematic approach to guide it. The thoroughness and thoughtfulness I put into the history taking can be key to finding the correct diagnosis. They also are a means of building trust and rapport with the parents. That will be important later if no definitive diagnosis is found.
Unclear and unusual presentations may merit a consult. The cardiologist knows the limits of an echo. Along with the technical expertise comes a new set of eyes and the additional perspective of a second opinion. It is great when a colleague can tell you that he or she too had a case like this years ago that was never solved, but did resolve on its own.
One advantage of being an office-based pediatrician, with an established relationship with a family over several years and a couple other children, is that parents do value and trust your clinical judgment. As a pediatrician, I know the most common product I sell is reassurance. It is not snake oil. There is a bedside manner in selling it. Put a positive spin on all the negative tests. Indicate that you and the parents can be vigilant in watching for new signs. Instruct the parents to bring the child back if the events are distressing for the child, which could justify more invasive testing. Arrange to recheck the child in the office in a week, then a month, then at the next well visit. Parents know that medicine isn’t perfect. Humans deal with fear and uncertainty better by knowing we aren’t facing the future alone. And that is why even with all this technology, I still lay a stethoscope on every child.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures.
A toddler has had several brief episodes of mild perioral cyanosis noticed at day care. The parents see the primary care provider. The exam is normal. The child is admitted for a work-up. The CBC and comprehensive metabolic profile are unremarkable. The chest x-ray is normal. An ECG is normal. An echocardiogram is normal. The EEG is normal. Now what?
I was taught that an uncommon presentation of a common disease is still more common than a common presentation of an uncommon disease. Or simply, odd-looking horses are more common than zebras unless you practice in the savanna. There is a point in any safari at which you have to decide whether you are hunting a zebra or chasing a shadow. Clinical judgment is balancing the risk of missing something preventable that will actually harm the child against the harms of more tests.
The modern hospital has an array of equipment available. They are Greek Sirens calling to us. There is the video EEG room, the MR angiogram, the cardiac cath lab, and an endless list of blood tests. We are not even stopped by the walls of the hospital. We can order a follow-up ambulatory Holter ECG to search for intermittent arrhythmias. But are these Sirens really good medicine? At what point should we simply reassure the parents that the child is fine?
Physicians all worry about missing something. This fear was instilled when we were medical students and reinforced with the stress of residency. With years of experience, all physicians acquire a list of missed diagnoses. But I also have collected a list of times when the diagnostic tests themselves have caused harm, including death. I have a list of cases where nonspecific diagnostic testing has mislabeled a child with an obscure diagnosis that was later proven false, but not before harm was caused. There were patients with Stevens-Johnson syndrome who suffered serious harm from treatments for minor illnesses. Then there were the terrified families who, after extensive testing, became convinced that the child must have some horrible unknown disease because surely we wouldn’t have traumatized the child with all this work-up if there wasn’t really something seriously wrong. Each new test stoked their fear rather than soothed it.
A careful history is still the weapon of choice in the zebra hunt. On a first presentation of mild cyanosis, sepsis is the charging rhinoceros of preventable harm that will run you over if you are too slow to react. But this child has now had several episodes that have occurred: 1. in multiple settings, 2. with no distress, 3. while the child remained playful, and 4. that were self-limited. That history is incompatible with sepsis, so reflexively ordering a blood culture is an illogical choice. The history should be progressively explored using the differential diagnosis and an organ-based systematic approach to guide it. The thoroughness and thoughtfulness I put into the history taking can be key to finding the correct diagnosis. They also are a means of building trust and rapport with the parents. That will be important later if no definitive diagnosis is found.
Unclear and unusual presentations may merit a consult. The cardiologist knows the limits of an echo. Along with the technical expertise comes a new set of eyes and the additional perspective of a second opinion. It is great when a colleague can tell you that he or she too had a case like this years ago that was never solved, but did resolve on its own.
One advantage of being an office-based pediatrician, with an established relationship with a family over several years and a couple other children, is that parents do value and trust your clinical judgment. As a pediatrician, I know the most common product I sell is reassurance. It is not snake oil. There is a bedside manner in selling it. Put a positive spin on all the negative tests. Indicate that you and the parents can be vigilant in watching for new signs. Instruct the parents to bring the child back if the events are distressing for the child, which could justify more invasive testing. Arrange to recheck the child in the office in a week, then a month, then at the next well visit. Parents know that medicine isn’t perfect. Humans deal with fear and uncertainty better by knowing we aren’t facing the future alone. And that is why even with all this technology, I still lay a stethoscope on every child.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures.
Slaying the dragon of false research
John Ioannidis was introduced as a rock star. To the congregation at the 2016 Lown Institute Conference in Chicago, that is what he is. The Stanford University professor is most famous for the heavily cited (over 2,000 citations so far) paper in PLoS Medicine, titled, “Why Most Published Research Findings Are False.”1 The cheering audience of clinicians, researchers, community organizers, and patient advocates were obviously familiar with the work. His message about the poor state of medical research and the inaccurate application of evidence-based medicine resonated with this audience. The conference’s emphasis was on Right Care, a balance between the many benefits of modern medical care and the harms of overdiagnosis and overtreatment. There are many similar initiatives in medicine. For instance, in 2012 the American Board of Internal Medicine Foundation launched Choosing Wisely “with a goal of advancing a national dialogue on avoiding wasteful or unnecessary medical tests, treatments, and procedures.”2 The U.S. Preventive Services Task Force has been issuing many recommendations recently. Several of those have counseled reducing screening and treatment rather than touting medical advances.
Pediatric hospital medicine (PHM) is a leader in this value medicine movement. Pediatricians are aware of the emotional trauma of procedures and hospitalizations, of the harm caused by radiation exposure, and of the phobia and dread of needle pokes. Primum non nocere.
The medical care system has contributed to the improvement in life expectancy over the last 50 years. The life expectancy for U.S. adults has increased about 3-4 years during that interval, although it is unclear what fraction of that is attributable to medical care. The per capita cost of the U.S. health care system is far greater than in other democratic developed countries, so we probably spend most of those extra 3-4 years working to pay for it. Government health care contributes heavily to the national debt. That is important because, despite all the technological advances in medicine, the socioeconomic determinants of health are far more important.3 So if we are wasting money on ineffective care, we can improve health by safely doing less.
A recently released article documents a salient example of inaccurate research leading to ineffective treatment. For over five winters, the pediatric hospitalist community has been debating whether nebulized hypertonic saline is beneficial for infants hospitalized with bronchiolitis. At a pro/con SmackDown debate at the 2011 PHM conference, both of the speakers were cautious in presenting their side of the debate. Nebulized hypertonic saline is effective for improving pulmonary clearance of the thick mucus of older children with cystic fibrosis. A few initial studies had shown conflicting but promising responses for infants with bronchiolitis, but the studies were underpowered and used disparate methods.
Since then, the accumulated evidence has been disappointing. Many additional small, underpowered studies were published in 2013-2014. A total of 18 studies were included in the latest meta-analysis by Brooks, Harrison, and Ralston, published online as “Association Between Hypertonic Saline and Hospital Length of Stay in Acute Viral Bronchiolitis: A Reanalysis of 2 Meta-analyses” in JAMA Pediatrics.4
Meta-analyses often obscure important differences among the studies they are combining, resulting in comparing apples and oranges, or worse creating fruit salad. But in a tour de force analysis, this article did not hand wave away all the typical statistical assumptions made by the average published meta-analysis. The intrepid authors examined the differences among the publications and calculated that those studies were too heterogeneous to be combined simply. When studied in more depth, two publications from one study population in China were outliers. The average length of stay was much longer in that study. Among the remaining papers, there was a residual correlation in which the studies leaning toward showing benefit had admitted the treatment population later in the course of the illness.
After adjustment for these anomalies, the conclusion was that the nebulized hypertonic saline treatment did not produce a clinically significant benefit. After years of debate on the hospitalist Listserv, this new article had one commentator pronouncing the end of using nebulized hypertonic saline for hospitalized infants with bronchiolitis and asserting that the issue could now rest in peace.
References
1. PLoS Med. 2005. doi: 10.1371/journal.pmed.0020124.
4. JAMA Pediatr. 2016 Apr 18. doi: 10.1001/jamapediatrics.2016.0079.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures. E-mail him at pdnews@frontlinemedcom.com.
John Ioannidis was introduced as a rock star. To the congregation at the 2016 Lown Institute Conference in Chicago, that is what he is. The Stanford University professor is most famous for the heavily cited (over 2,000 citations so far) paper in PLoS Medicine, titled, “Why Most Published Research Findings Are False.”1 The cheering audience of clinicians, researchers, community organizers, and patient advocates were obviously familiar with the work. His message about the poor state of medical research and the inaccurate application of evidence-based medicine resonated with this audience. The conference’s emphasis was on Right Care, a balance between the many benefits of modern medical care and the harms of overdiagnosis and overtreatment. There are many similar initiatives in medicine. For instance, in 2012 the American Board of Internal Medicine Foundation launched Choosing Wisely “with a goal of advancing a national dialogue on avoiding wasteful or unnecessary medical tests, treatments, and procedures.”2 The U.S. Preventive Services Task Force has been issuing many recommendations recently. Several of those have counseled reducing screening and treatment rather than touting medical advances.
Pediatric hospital medicine (PHM) is a leader in this value medicine movement. Pediatricians are aware of the emotional trauma of procedures and hospitalizations, of the harm caused by radiation exposure, and of the phobia and dread of needle pokes. Primum non nocere.
The medical care system has contributed to the improvement in life expectancy over the last 50 years. The life expectancy for U.S. adults has increased about 3-4 years during that interval, although it is unclear what fraction of that is attributable to medical care. The per capita cost of the U.S. health care system is far greater than in other democratic developed countries, so we probably spend most of those extra 3-4 years working to pay for it. Government health care contributes heavily to the national debt. That is important because, despite all the technological advances in medicine, the socioeconomic determinants of health are far more important.3 So if we are wasting money on ineffective care, we can improve health by safely doing less.
A recently released article documents a salient example of inaccurate research leading to ineffective treatment. For over five winters, the pediatric hospitalist community has been debating whether nebulized hypertonic saline is beneficial for infants hospitalized with bronchiolitis. At a pro/con SmackDown debate at the 2011 PHM conference, both of the speakers were cautious in presenting their side of the debate. Nebulized hypertonic saline is effective for improving pulmonary clearance of the thick mucus of older children with cystic fibrosis. A few initial studies had shown conflicting but promising responses for infants with bronchiolitis, but the studies were underpowered and used disparate methods.
Since then, the accumulated evidence has been disappointing. Many additional small, underpowered studies were published in 2013-2014. A total of 18 studies were included in the latest meta-analysis by Brooks, Harrison, and Ralston, published online as “Association Between Hypertonic Saline and Hospital Length of Stay in Acute Viral Bronchiolitis: A Reanalysis of 2 Meta-analyses” in JAMA Pediatrics.4
Meta-analyses often obscure important differences among the studies they are combining, resulting in comparing apples and oranges, or worse creating fruit salad. But in a tour de force analysis, this article did not hand wave away all the typical statistical assumptions made by the average published meta-analysis. The intrepid authors examined the differences among the publications and calculated that those studies were too heterogeneous to be combined simply. When studied in more depth, two publications from one study population in China were outliers. The average length of stay was much longer in that study. Among the remaining papers, there was a residual correlation in which the studies leaning toward showing benefit had admitted the treatment population later in the course of the illness.
After adjustment for these anomalies, the conclusion was that the nebulized hypertonic saline treatment did not produce a clinically significant benefit. After years of debate on the hospitalist Listserv, this new article had one commentator pronouncing the end of using nebulized hypertonic saline for hospitalized infants with bronchiolitis and asserting that the issue could now rest in peace.
References
1. PLoS Med. 2005. doi: 10.1371/journal.pmed.0020124.
4. JAMA Pediatr. 2016 Apr 18. doi: 10.1001/jamapediatrics.2016.0079.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures. E-mail him at pdnews@frontlinemedcom.com.
John Ioannidis was introduced as a rock star. To the congregation at the 2016 Lown Institute Conference in Chicago, that is what he is. The Stanford University professor is most famous for the heavily cited (over 2,000 citations so far) paper in PLoS Medicine, titled, “Why Most Published Research Findings Are False.”1 The cheering audience of clinicians, researchers, community organizers, and patient advocates were obviously familiar with the work. His message about the poor state of medical research and the inaccurate application of evidence-based medicine resonated with this audience. The conference’s emphasis was on Right Care, a balance between the many benefits of modern medical care and the harms of overdiagnosis and overtreatment. There are many similar initiatives in medicine. For instance, in 2012 the American Board of Internal Medicine Foundation launched Choosing Wisely “with a goal of advancing a national dialogue on avoiding wasteful or unnecessary medical tests, treatments, and procedures.”2 The U.S. Preventive Services Task Force has been issuing many recommendations recently. Several of those have counseled reducing screening and treatment rather than touting medical advances.
Pediatric hospital medicine (PHM) is a leader in this value medicine movement. Pediatricians are aware of the emotional trauma of procedures and hospitalizations, of the harm caused by radiation exposure, and of the phobia and dread of needle pokes. Primum non nocere.
The medical care system has contributed to the improvement in life expectancy over the last 50 years. The life expectancy for U.S. adults has increased about 3-4 years during that interval, although it is unclear what fraction of that is attributable to medical care. The per capita cost of the U.S. health care system is far greater than in other democratic developed countries, so we probably spend most of those extra 3-4 years working to pay for it. Government health care contributes heavily to the national debt. That is important because, despite all the technological advances in medicine, the socioeconomic determinants of health are far more important.3 So if we are wasting money on ineffective care, we can improve health by safely doing less.
A recently released article documents a salient example of inaccurate research leading to ineffective treatment. For over five winters, the pediatric hospitalist community has been debating whether nebulized hypertonic saline is beneficial for infants hospitalized with bronchiolitis. At a pro/con SmackDown debate at the 2011 PHM conference, both of the speakers were cautious in presenting their side of the debate. Nebulized hypertonic saline is effective for improving pulmonary clearance of the thick mucus of older children with cystic fibrosis. A few initial studies had shown conflicting but promising responses for infants with bronchiolitis, but the studies were underpowered and used disparate methods.
Since then, the accumulated evidence has been disappointing. Many additional small, underpowered studies were published in 2013-2014. A total of 18 studies were included in the latest meta-analysis by Brooks, Harrison, and Ralston, published online as “Association Between Hypertonic Saline and Hospital Length of Stay in Acute Viral Bronchiolitis: A Reanalysis of 2 Meta-analyses” in JAMA Pediatrics.4
Meta-analyses often obscure important differences among the studies they are combining, resulting in comparing apples and oranges, or worse creating fruit salad. But in a tour de force analysis, this article did not hand wave away all the typical statistical assumptions made by the average published meta-analysis. The intrepid authors examined the differences among the publications and calculated that those studies were too heterogeneous to be combined simply. When studied in more depth, two publications from one study population in China were outliers. The average length of stay was much longer in that study. Among the remaining papers, there was a residual correlation in which the studies leaning toward showing benefit had admitted the treatment population later in the course of the illness.
After adjustment for these anomalies, the conclusion was that the nebulized hypertonic saline treatment did not produce a clinically significant benefit. After years of debate on the hospitalist Listserv, this new article had one commentator pronouncing the end of using nebulized hypertonic saline for hospitalized infants with bronchiolitis and asserting that the issue could now rest in peace.
References
1. PLoS Med. 2005. doi: 10.1371/journal.pmed.0020124.
4. JAMA Pediatr. 2016 Apr 18. doi: 10.1001/jamapediatrics.2016.0079.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures. E-mail him at pdnews@frontlinemedcom.com.
End of life care
As the busy days of a long, gray winter drag on and an early season of Lent has begun, this column flows from reflections on life, death, and the promise of a new season of spring and green trees, hopefully coming soon – no matter what that groundhog saw.
Clinical ethics consultation often involves end of life (EOL) care. When I recall patients from my career, many memories are of patients who died. I trained with an intensivist who said he felt he was under less stress than the general pediatricians. While his patients were sicker, if one of his patients died, it was not unexpected. The presumption was that in the ICU everything possible had been done. General pediatricians rarely have a patient who dies. When they do, everyone, including the pediatrician, will ponder over whether something might have been caught earlier or something could have been done differently. But the most difficult problems in pediatric EOL care involve deciding when to stop aggressive care and let nature take its course.
I think the natural tendency for scholars is to approach difficult decisions by seeking more information. The delusion (which scholars can usually elucidate in great postmodern detail as long as it doesn’t apply to our own behavior) is that extensive information and deep reflection will lead to the best, most accurate, immutable, and nonambivalent declaration of goals, desires, values, and intents. To even make this delusion plausible, a sci-fi writer had to create a nonhuman species of Vulcans. But medical ethicists routinely apply this paradigm to existentially frightening EOL matters in a medical world full of prognostic uncertainty. Ethicists have recommended that this method of decision making be adopted by a population with low health literacy and a predilection to using Tinder.
For the internists, EOL care is mostly about specifying which modalities to use and which to limit. Over time, it became evident that a single check box, labeled Do Not Resuscitate yes/no, was insufficient to capture patient preferences. I recall once seeing a draft document with 49 boxes. It was clearly unwieldy. Most states that have adopted a POLST (Physician Orders for Life-Sustaining Treatment) paradigm have settled for forms with five to seven options. I think that if it were possible to capture advance directives better than that, eharmony.com, with its plethora of questions, would have already created an app for it. In adult medicine, we always can lament that the conversation about EOL care was too brief, but in my experience raising expectations of a more comprehensive discussion usually lowers the likelihood of people ever undertaking even an abbreviated conversation. In ethics, if you raise the bar high enough, people seem to walk under it.
Pediatrics at the EOL tends to focus discussion more on the goals of care, the likely outcomes, and the quality of life. These perspectives are then sometimes mapped, with poor reliability, onto the POLST paradigm designed for adults. Parents are usually at the bedside often enough to recognize their child’s suffering during aggressive care. Surrogate decision makers for adult EOL care occasionally lack that insight.
While advance directive documents are helpful, I don’t think there is a substitute for a physician motivated by empathy and a caring, involved surrogate decision maker at bedside. Providing information is not the key focus. The process should emphasize building trusting relationships, clear understanding, and reasonable expectations. I am reminded in those situations of an ancient quote: Medical care is “to cure sometimes, to relieve often, and to comfort always.”
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures or conflicts of interest. E-mail him at pdnews@frontlinemedcom.com.
As the busy days of a long, gray winter drag on and an early season of Lent has begun, this column flows from reflections on life, death, and the promise of a new season of spring and green trees, hopefully coming soon – no matter what that groundhog saw.
Clinical ethics consultation often involves end of life (EOL) care. When I recall patients from my career, many memories are of patients who died. I trained with an intensivist who said he felt he was under less stress than the general pediatricians. While his patients were sicker, if one of his patients died, it was not unexpected. The presumption was that in the ICU everything possible had been done. General pediatricians rarely have a patient who dies. When they do, everyone, including the pediatrician, will ponder over whether something might have been caught earlier or something could have been done differently. But the most difficult problems in pediatric EOL care involve deciding when to stop aggressive care and let nature take its course.
I think the natural tendency for scholars is to approach difficult decisions by seeking more information. The delusion (which scholars can usually elucidate in great postmodern detail as long as it doesn’t apply to our own behavior) is that extensive information and deep reflection will lead to the best, most accurate, immutable, and nonambivalent declaration of goals, desires, values, and intents. To even make this delusion plausible, a sci-fi writer had to create a nonhuman species of Vulcans. But medical ethicists routinely apply this paradigm to existentially frightening EOL matters in a medical world full of prognostic uncertainty. Ethicists have recommended that this method of decision making be adopted by a population with low health literacy and a predilection to using Tinder.
For the internists, EOL care is mostly about specifying which modalities to use and which to limit. Over time, it became evident that a single check box, labeled Do Not Resuscitate yes/no, was insufficient to capture patient preferences. I recall once seeing a draft document with 49 boxes. It was clearly unwieldy. Most states that have adopted a POLST (Physician Orders for Life-Sustaining Treatment) paradigm have settled for forms with five to seven options. I think that if it were possible to capture advance directives better than that, eharmony.com, with its plethora of questions, would have already created an app for it. In adult medicine, we always can lament that the conversation about EOL care was too brief, but in my experience raising expectations of a more comprehensive discussion usually lowers the likelihood of people ever undertaking even an abbreviated conversation. In ethics, if you raise the bar high enough, people seem to walk under it.
Pediatrics at the EOL tends to focus discussion more on the goals of care, the likely outcomes, and the quality of life. These perspectives are then sometimes mapped, with poor reliability, onto the POLST paradigm designed for adults. Parents are usually at the bedside often enough to recognize their child’s suffering during aggressive care. Surrogate decision makers for adult EOL care occasionally lack that insight.
While advance directive documents are helpful, I don’t think there is a substitute for a physician motivated by empathy and a caring, involved surrogate decision maker at bedside. Providing information is not the key focus. The process should emphasize building trusting relationships, clear understanding, and reasonable expectations. I am reminded in those situations of an ancient quote: Medical care is “to cure sometimes, to relieve often, and to comfort always.”
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures or conflicts of interest. E-mail him at pdnews@frontlinemedcom.com.
As the busy days of a long, gray winter drag on and an early season of Lent has begun, this column flows from reflections on life, death, and the promise of a new season of spring and green trees, hopefully coming soon – no matter what that groundhog saw.
Clinical ethics consultation often involves end of life (EOL) care. When I recall patients from my career, many memories are of patients who died. I trained with an intensivist who said he felt he was under less stress than the general pediatricians. While his patients were sicker, if one of his patients died, it was not unexpected. The presumption was that in the ICU everything possible had been done. General pediatricians rarely have a patient who dies. When they do, everyone, including the pediatrician, will ponder over whether something might have been caught earlier or something could have been done differently. But the most difficult problems in pediatric EOL care involve deciding when to stop aggressive care and let nature take its course.
I think the natural tendency for scholars is to approach difficult decisions by seeking more information. The delusion (which scholars can usually elucidate in great postmodern detail as long as it doesn’t apply to our own behavior) is that extensive information and deep reflection will lead to the best, most accurate, immutable, and nonambivalent declaration of goals, desires, values, and intents. To even make this delusion plausible, a sci-fi writer had to create a nonhuman species of Vulcans. But medical ethicists routinely apply this paradigm to existentially frightening EOL matters in a medical world full of prognostic uncertainty. Ethicists have recommended that this method of decision making be adopted by a population with low health literacy and a predilection to using Tinder.
For the internists, EOL care is mostly about specifying which modalities to use and which to limit. Over time, it became evident that a single check box, labeled Do Not Resuscitate yes/no, was insufficient to capture patient preferences. I recall once seeing a draft document with 49 boxes. It was clearly unwieldy. Most states that have adopted a POLST (Physician Orders for Life-Sustaining Treatment) paradigm have settled for forms with five to seven options. I think that if it were possible to capture advance directives better than that, eharmony.com, with its plethora of questions, would have already created an app for it. In adult medicine, we always can lament that the conversation about EOL care was too brief, but in my experience raising expectations of a more comprehensive discussion usually lowers the likelihood of people ever undertaking even an abbreviated conversation. In ethics, if you raise the bar high enough, people seem to walk under it.
Pediatrics at the EOL tends to focus discussion more on the goals of care, the likely outcomes, and the quality of life. These perspectives are then sometimes mapped, with poor reliability, onto the POLST paradigm designed for adults. Parents are usually at the bedside often enough to recognize their child’s suffering during aggressive care. Surrogate decision makers for adult EOL care occasionally lack that insight.
While advance directive documents are helpful, I don’t think there is a substitute for a physician motivated by empathy and a caring, involved surrogate decision maker at bedside. Providing information is not the key focus. The process should emphasize building trusting relationships, clear understanding, and reasonable expectations. I am reminded in those situations of an ancient quote: Medical care is “to cure sometimes, to relieve often, and to comfort always.”
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures or conflicts of interest. E-mail him at pdnews@frontlinemedcom.com.
Stewardship at 3 a.m.
The 3-month-old infant presents to the emergency department with a fever of 101° F. The emergency physician decides the infant looks ill enough to warrant some investigation. A urinalysis indicates a urinary tract infection. I am consulted to complete the admission to the hospital. The question arises, “Is a lumbar puncture indicated to rule out meningitis?”
I’ve been down this pathway many times. For years I have relied on a meta-analysis which corrected the bias of an old article from 1972.1 Multiple studies in the 2000-2010 time frame have shown that the risk of concurrent meningitis in a young infant with a UTI is vanishingly small. It is much less than 2%, with many studies finding 0%. So on a typical day, my answer is no tap if there is no clinical suggestion of meningitis.
Hospital medicine has recently focused on reducing overdiagnosis and overtreatment. When you only occasionally admit patients to the hospital, untoward events appear random and uncommon. When you work there day in and day out, you appreciate that all medical interventions have risks and costs.
A recent editorial raised the question of stewardship in medicine.2 It asked why physicians would choose a very expensive drug when there is little evidence of its superiority over a much cheaper predecessor. Physicians, whose actions influence a $3 trillion industry, have not embraced stewardship as a major component of their professional responsibilities. The physician does have a fiduciary duty toward the patient. The physician recommends the best care possible to achieve the patient’s goals of care. Dentistry is distinctly different in this regard. Dentists often have several ways of repairing decayed teeth. Various types of fillings are available. Gold fillings are more expensive. Newer implants are several times more expensive than crowns. Dentists routinely adjust their treatment plan based on what the patient can afford.
While most other industries have market competition and profitability as incentives to avoid extravagance, U.S. health care seems unbridled by fiscal responsibility. The news that a small pharmaceutical company had raised the price of an old generic antibiotic by 5000%3 exposed the irrationality and capriciousness4 of the pricing of medications in the United States. Many politicians decried the behavior but to little effect. Most consumer products, especially computers, become more powerful and cheaper with each decade. Health care does not follow this pattern
There are many factors that influence physician behavior. Concerns about malpractice may bias physicians toward expensive overtreatment. Modern medical research is usually published expounding on the benefits of a new technology over a previous therapy without any acknowledgment that the newer and more expensive treatment may have a downside. This biases people to use the latest and greatest treatment even though it may have only demonstrated noninferiority in its trials.
I try to use evidence-based medicine when it is available. In the clinical case described earlier, I indicate to the emergency doctor that unless there is a clinical impression of coexisting meningitis, the lumbar puncture is not indicated. I cite the meta-analysis as I have many times before. But this night is different. I am simultaneously admitting a teenager whose gastrostomy tube had become dislodged and couldn’t be replaced. This neurologically devastated child had had meningitis as an infant. He is a stark reminder of the consequences of a missed diagnosis.
The parents of that child have provided him wonderful care. His skin is in excellent condition. His moderate contractures are testimony to dedicated stretching regimens at home. It is evident that the parents love the child as he is. But I am sure they would give anything to have avoided this scenario and to reverse the consequences of that meningitis. And so, the best evidence we have, that the risk of meningitis in an infant is low, is not as reassuring to me on this night. At 3 a.m., the juxtaposition of the two patients is unsettling. Is the risk low enough? Would that new test5, serum procalcitonin, help me to make a better decision? How certain must I be that an intervention is unnecessary?
Health care policy, economics, and practice guidelines can be debated with detached objectivity around a conference table in the middle of the day. The trepidation in an emergency room at 3 a.m. is different. This is my patient. I am his doctor. That is the heart of medical ethics.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures or conflicts of interest. E-mail him at pdnews@frontlinemedcom.com.
References
1. “How common is co-existing meningitis in infants with urinary tract infection?” on Bestbets.org.
2. “Why do doctors choose a $2,000 cure when a $50 one is just as good?” by Andrew Lam, Washington Post, Dec. 10, 2015.
3. “Drug Goes From $13.50 a Tablet to $750, Overnight” by Andrew Pollack, New York Times, Sept. 20, 2015.
4. “How an $84,000 drug got its price: ‘Let’s hold our position … whatever the headlines’ ” by Carolyn Y. Johnson and Brady Dennis, Washington Post, Dec. 1, 2015.
5. JAMA Pediatr. Published online, 2015 Nov 23. doi:10.1001/jamapediatrics.2015.3267.
The 3-month-old infant presents to the emergency department with a fever of 101° F. The emergency physician decides the infant looks ill enough to warrant some investigation. A urinalysis indicates a urinary tract infection. I am consulted to complete the admission to the hospital. The question arises, “Is a lumbar puncture indicated to rule out meningitis?”
I’ve been down this pathway many times. For years I have relied on a meta-analysis which corrected the bias of an old article from 1972.1 Multiple studies in the 2000-2010 time frame have shown that the risk of concurrent meningitis in a young infant with a UTI is vanishingly small. It is much less than 2%, with many studies finding 0%. So on a typical day, my answer is no tap if there is no clinical suggestion of meningitis.
Hospital medicine has recently focused on reducing overdiagnosis and overtreatment. When you only occasionally admit patients to the hospital, untoward events appear random and uncommon. When you work there day in and day out, you appreciate that all medical interventions have risks and costs.
A recent editorial raised the question of stewardship in medicine.2 It asked why physicians would choose a very expensive drug when there is little evidence of its superiority over a much cheaper predecessor. Physicians, whose actions influence a $3 trillion industry, have not embraced stewardship as a major component of their professional responsibilities. The physician does have a fiduciary duty toward the patient. The physician recommends the best care possible to achieve the patient’s goals of care. Dentistry is distinctly different in this regard. Dentists often have several ways of repairing decayed teeth. Various types of fillings are available. Gold fillings are more expensive. Newer implants are several times more expensive than crowns. Dentists routinely adjust their treatment plan based on what the patient can afford.
While most other industries have market competition and profitability as incentives to avoid extravagance, U.S. health care seems unbridled by fiscal responsibility. The news that a small pharmaceutical company had raised the price of an old generic antibiotic by 5000%3 exposed the irrationality and capriciousness4 of the pricing of medications in the United States. Many politicians decried the behavior but to little effect. Most consumer products, especially computers, become more powerful and cheaper with each decade. Health care does not follow this pattern
There are many factors that influence physician behavior. Concerns about malpractice may bias physicians toward expensive overtreatment. Modern medical research is usually published expounding on the benefits of a new technology over a previous therapy without any acknowledgment that the newer and more expensive treatment may have a downside. This biases people to use the latest and greatest treatment even though it may have only demonstrated noninferiority in its trials.
I try to use evidence-based medicine when it is available. In the clinical case described earlier, I indicate to the emergency doctor that unless there is a clinical impression of coexisting meningitis, the lumbar puncture is not indicated. I cite the meta-analysis as I have many times before. But this night is different. I am simultaneously admitting a teenager whose gastrostomy tube had become dislodged and couldn’t be replaced. This neurologically devastated child had had meningitis as an infant. He is a stark reminder of the consequences of a missed diagnosis.
The parents of that child have provided him wonderful care. His skin is in excellent condition. His moderate contractures are testimony to dedicated stretching regimens at home. It is evident that the parents love the child as he is. But I am sure they would give anything to have avoided this scenario and to reverse the consequences of that meningitis. And so, the best evidence we have, that the risk of meningitis in an infant is low, is not as reassuring to me on this night. At 3 a.m., the juxtaposition of the two patients is unsettling. Is the risk low enough? Would that new test5, serum procalcitonin, help me to make a better decision? How certain must I be that an intervention is unnecessary?
Health care policy, economics, and practice guidelines can be debated with detached objectivity around a conference table in the middle of the day. The trepidation in an emergency room at 3 a.m. is different. This is my patient. I am his doctor. That is the heart of medical ethics.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures or conflicts of interest. E-mail him at pdnews@frontlinemedcom.com.
References
1. “How common is co-existing meningitis in infants with urinary tract infection?” on Bestbets.org.
2. “Why do doctors choose a $2,000 cure when a $50 one is just as good?” by Andrew Lam, Washington Post, Dec. 10, 2015.
3. “Drug Goes From $13.50 a Tablet to $750, Overnight” by Andrew Pollack, New York Times, Sept. 20, 2015.
4. “How an $84,000 drug got its price: ‘Let’s hold our position … whatever the headlines’ ” by Carolyn Y. Johnson and Brady Dennis, Washington Post, Dec. 1, 2015.
5. JAMA Pediatr. Published online, 2015 Nov 23. doi:10.1001/jamapediatrics.2015.3267.
The 3-month-old infant presents to the emergency department with a fever of 101° F. The emergency physician decides the infant looks ill enough to warrant some investigation. A urinalysis indicates a urinary tract infection. I am consulted to complete the admission to the hospital. The question arises, “Is a lumbar puncture indicated to rule out meningitis?”
I’ve been down this pathway many times. For years I have relied on a meta-analysis which corrected the bias of an old article from 1972.1 Multiple studies in the 2000-2010 time frame have shown that the risk of concurrent meningitis in a young infant with a UTI is vanishingly small. It is much less than 2%, with many studies finding 0%. So on a typical day, my answer is no tap if there is no clinical suggestion of meningitis.
Hospital medicine has recently focused on reducing overdiagnosis and overtreatment. When you only occasionally admit patients to the hospital, untoward events appear random and uncommon. When you work there day in and day out, you appreciate that all medical interventions have risks and costs.
A recent editorial raised the question of stewardship in medicine.2 It asked why physicians would choose a very expensive drug when there is little evidence of its superiority over a much cheaper predecessor. Physicians, whose actions influence a $3 trillion industry, have not embraced stewardship as a major component of their professional responsibilities. The physician does have a fiduciary duty toward the patient. The physician recommends the best care possible to achieve the patient’s goals of care. Dentistry is distinctly different in this regard. Dentists often have several ways of repairing decayed teeth. Various types of fillings are available. Gold fillings are more expensive. Newer implants are several times more expensive than crowns. Dentists routinely adjust their treatment plan based on what the patient can afford.
While most other industries have market competition and profitability as incentives to avoid extravagance, U.S. health care seems unbridled by fiscal responsibility. The news that a small pharmaceutical company had raised the price of an old generic antibiotic by 5000%3 exposed the irrationality and capriciousness4 of the pricing of medications in the United States. Many politicians decried the behavior but to little effect. Most consumer products, especially computers, become more powerful and cheaper with each decade. Health care does not follow this pattern
There are many factors that influence physician behavior. Concerns about malpractice may bias physicians toward expensive overtreatment. Modern medical research is usually published expounding on the benefits of a new technology over a previous therapy without any acknowledgment that the newer and more expensive treatment may have a downside. This biases people to use the latest and greatest treatment even though it may have only demonstrated noninferiority in its trials.
I try to use evidence-based medicine when it is available. In the clinical case described earlier, I indicate to the emergency doctor that unless there is a clinical impression of coexisting meningitis, the lumbar puncture is not indicated. I cite the meta-analysis as I have many times before. But this night is different. I am simultaneously admitting a teenager whose gastrostomy tube had become dislodged and couldn’t be replaced. This neurologically devastated child had had meningitis as an infant. He is a stark reminder of the consequences of a missed diagnosis.
The parents of that child have provided him wonderful care. His skin is in excellent condition. His moderate contractures are testimony to dedicated stretching regimens at home. It is evident that the parents love the child as he is. But I am sure they would give anything to have avoided this scenario and to reverse the consequences of that meningitis. And so, the best evidence we have, that the risk of meningitis in an infant is low, is not as reassuring to me on this night. At 3 a.m., the juxtaposition of the two patients is unsettling. Is the risk low enough? Would that new test5, serum procalcitonin, help me to make a better decision? How certain must I be that an intervention is unnecessary?
Health care policy, economics, and practice guidelines can be debated with detached objectivity around a conference table in the middle of the day. The trepidation in an emergency room at 3 a.m. is different. This is my patient. I am his doctor. That is the heart of medical ethics.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Dr. Powell said he had no relevant financial disclosures or conflicts of interest. E-mail him at pdnews@frontlinemedcom.com.
References
1. “How common is co-existing meningitis in infants with urinary tract infection?” on Bestbets.org.
2. “Why do doctors choose a $2,000 cure when a $50 one is just as good?” by Andrew Lam, Washington Post, Dec. 10, 2015.
3. “Drug Goes From $13.50 a Tablet to $750, Overnight” by Andrew Pollack, New York Times, Sept. 20, 2015.
4. “How an $84,000 drug got its price: ‘Let’s hold our position … whatever the headlines’ ” by Carolyn Y. Johnson and Brady Dennis, Washington Post, Dec. 1, 2015.
5. JAMA Pediatr. Published online, 2015 Nov 23. doi:10.1001/jamapediatrics.2015.3267.