Article
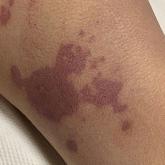
Purpura Fulminans Induced by Vibrio vulnificus
- Author:
- Christine C. Akoh, PhD
- Gaurav Singh, MD, MPH
- Margo Lederhandler, MD
- Randie H. Kim, MD, PhD
- Miriam Keltz Pomeranz, MD
Purpura fulminans is an acute, life-threatening condition characterized by intravascular thrombosis and hemorrhagic necrosis of the skin.
