Article
Recalcitrant Folliculitis Decalvans Treatment Outcomes With Biologics and Small Molecule Inhibitors
- Author:
- Tamara Fakhoury, DO
- Katelyn Urban, DO
- Leila Ettefagh, MD
- Navid Nami, DO
Tumor necrosis factor inhibitors, Janus kinase inhibitors, phosphodiesterase 4 inhibitors, and monoclonal antibodies have shown success in the...
Article
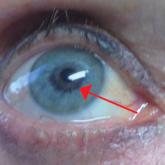
Bimatoprost-Induced Iris Hyperpigmentation: Beauty in the Darkened Eye of the Beholder
- Author:
- Michael B. Lipp, DO
- Leela Athalye, DO
- Navid Nami, DO
Iris hyperpigmentation can occur when bimatoprost eye drops are applied to the eyes for treatment of ocular hypertension and glaucoma, but reports...
Article
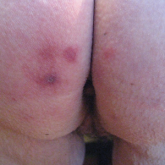
Ice Pack–Induced Perniosis: A Rare and Underrecognized Association
- Author:
- Donna Tran, DO
- Jessica Riley, DO
- Anny Xiao, DO
- Shirlene Jay, MD
- Paul Shitabata, MD
- Navid Nami, DO
Perniosis, or chilblain, is characterized by skin lesions that occur as an abnormal reaction to exposure to cold and damp conditions. Ice pack–...
Article
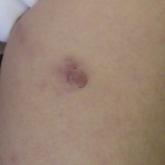
A Rare Case of Primary Cutaneous Diffuse Large B-Cell Lymphoma, Leg Type
- Author:
- Leela Athalye, DO
- Navid Nami, DO
- Paul Shitabata, MD
Primary cutaneous diffuse large B-cell lymphoma, leg type (DLBCLLT) is a rare, intermediately aggressive form of primary cutaneous B-cell lymphoma...
Article

Collagenous and Elastotic Marginal Plaques of the Hands
- Author:
- Mayha Patel, DO
- Leela Athalye, DO
- Paul Shitabata, MD
- Mark F. Maida, MD
- Navid Nami, DO
