User login
Diagnostic puzzler: Acute eyelid edema
A 68-year-old man sought care in our emergency department for unilateral ptosis following superior and inferior right eyelid edema. The patient said that the edema had developed 3 days earlier and was getting worse each day; the ptosis was impairing his vision. The patient indicated that the edema was accompanied by mild burning in the right periocular region. His medical history included arterial hypertension, which was under control, and bilateral cataract surgery 5 years ago.
On examination, we noted superior and inferior nontender painless eyelid edema on the right eye, with no signs of acute inflammation (FIGURE). The patient also had right supraciliary folliculitis that was improving; the folliculitis had been treated 3 days earlier at a primary care facility.
We performed a complete ocular examination, including visual acuity (20/20 in both eyes) and found no other significant problems. Nor did the patient have a fever or any other systemic symptoms.
FIGURE 1
Edema of the upper and lower eyelid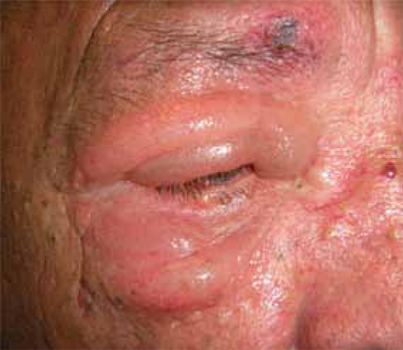
The swelling was not accompanied by inflammation or fever, but it did impair the patient’s vision.
WHAT IS YOUR DIAGNOSIS?
HOW WOULD YOU TREAT THIS PATIENT?
Diagnosis: Noninflammatory eyelid edema
The fact that the patient’s eyelid was edematous (but not tender or red) and that he’d been scratching the area following a case of folliculitis prompted us to diagnose noninflammatory eyelid edema.
Noninflammatory eyelid edema—also called noninflammatory palpebral edema—is a relatively common disorder that usually occurs after some local irritation or microtrauma. In its early phase, patients start out with nonerythematous, painless edema of the upper eyelid, which eventually affects the lower eyelid.
As was the case with our patient, this disorder is not associated with fever or any other systemic sign or symptom. Complete blood count and C-reactive protein will be negative, as no infection or systemic alteration is present.
Consider these infectious alternatives
In cases like this one, be sure to differentiate between noninflammatory palpebral edema and other common but less benign ocular conditions. Among the infectious causes of unilateral edema to rule out:
Preseptal cellulitis is an infection that is localized between the skin and the orbital septum. This disorder usually appears as a tender erythematous eyelid edema with no proptosis and no pain with eye movement.1 It is usually accompanied by an elevated white blood cell (WBC) count. Blood cultures are rarely positive, but when they are, Haemophilus influenzae is the most frequent pathogen.2 Preseptal cellulitis is treated with broad-spectrum oral antibiotics (amoxicillin/ clavulanate) for at least 7 days.
Orbital cellulitis is an infection that affects the orbital extraocular structures. It can lead to blindness, so prompt diagnosis is critical.
Orbital cellulitis usually develops when a sinus infection spreads into the orbit.3 Suspect it in a patient with proptosis, orbital pain, tenderness, conjunctival chemosis, decreased vision, elevated intraocular pressure, and pain on eye movement. Also look for an elevated WBC count. Perform blood cultures to confirm the presence of a pathogen.
If you suspect orbital cellulitis, order an orbital computed tomography scan with contrast infusion, including axial and coronal views; it may reveal an infection of the soft tissue behind the orbital septum. Treat this condition with broad-spectrum intravenous antibiotics (ceftriaxone) for 1 week, followed by 2 weeks of oral antibiotics, completing a total of 21 days of antibiotics.
Hordeolum is a localized infection that occurs when a meibomian gland becomes blocked. It usually appears as a palpable subcutaneous nodule within the eyelid and requires treatment with warm compresses and a combination of antibiotics and steroid topical ointment (tobramycin and dexamethasone ophthalmic ointment 4 times a day for a week).4
Acute dacryoadenitis is a lacrimal gland infection that usually causes unilateral, painful swelling of the outer third of the upper lid. You may also see tearing and discharge.5 Look for an elevated WBC count; however, blood cultures are rarely positive. These patients must be referred to an ophthalmologist as treatment varies from symptomatic measures in viral cases (warm compresses and a nonsteroidal anti-inflammatory drug, such as ibuprofen) to hospitalization and oral or intravenous antibiotics (eg, amoxicillin/ clavulanate for at least 7 days), depending on the severity and origin of the infection.6
Ruling out other noninfectious disorders
Noninfectious inflammatory diseases should also be part of the differential diagnosis, including:
Idiopathic orbital inflammation. Also known as orbital pseudotumor, this disorder is a nongranulomatous acute-to-subacute inflammatory disease with no systemic manifestations.7 It frequently involves the lacrimal gland and can cause abrupt pain, conjunctival edema, and lid edema. Other common signs are proptosis and ocular motility alterations, which the patient may report as diplopia and visual impairment.
This disorder can result from optic neuropathy, exudative retinal detachment, or uveitis. It is a diagnosis of exclusion and is often arrived at by seeing the patient respond to systemic corticosteroids. The specific drug and dose will vary based on disease severity.
Graves’ ophthalmopathy. This bilateral, asymmetric immunological disorder affects the conjunctiva, eyelids,8 extraocular muscles, lacrimal gland, and optic nerve. Although it is typically diagnosed clinically, thyroid hormone abnormalities (increased T4 and a drop in thyroid-stimulating hormone) help support the diagnosis. In the acute phase, it has to be treated with systemic steroids; if the condition becomes chronic, the complications may require surgery. Treatment of the underlying hyperthyroidism may, in some cases, worsen the ophthalmopathy.
One more consideration. Finally, consider a local allergic reaction in the eyelids,9 which can also cause painless palpebral edema. Expect to see erythematous edema and intense itching a few hours after exposure to the allergen. A cosmetic product is often the culprit. As you might expect, initial treatment calls for withdrawal of the offending product. Instruct the patient to apply a topical steroid ointment on the eyelid if the edema is intense.
Good news for our patient
Diagnosing noninflammatory eyelid edema requires keen observational skills and a knowledge of several alternative diagnoses. Fortunately for our patient, this benign condition did not require any local or systemic treatment. The edema resolved on its own in 6 days.
CORRESPONDENCE
Omar Rayward, MD, Calle Profesor Martín Lagos, Madrid, Spain 28040; orayward@yahoo.com
1. Bilyk JR. Periocular infection. Curr Opin Ophthalmol. 2007;18:414-423.
2. Jackson K, Baker SR. Periorbital cellulitis. Head Neck Surg. 1987;9:227-234.
3. Adam R, Gupta V, Harvey J. Question: can you identify this condition? This condition is orbital cellulitis. Can Fam Physician. 2009;55:1097.-
4. Lindsley K, Nichols JJ, Dickersin K. Interventions for acute internal hordeolum. Cochrane Database Syst Rev. 2010;(9):CD007742.-
5. Colegrove JA. Localized orbital inflammation: a case of dacryoadenitis. Optom Vis Sci. 2000;77:121-124.
6. Durand ML. Periocular infections. In: Mandell GL, Bennett JE, Dolin R, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 7th ed. Philadelphia, Pa: Elsevier Churchill Livingstone; 2009:1569–1575.
7. Cooney NL. Orbital pseudotumor. Int J Emerg Med. 2009;2:263.-
8. Imaizumi M. Recurrent upper eyelid edema as first sign of Graves’ disease. Thyroid. 2006;16:95-96.
9. Friedlaender MH. Objective measurement of allergic reactions in the eye. Curr Opin Allergy Clin Immunol. 2004;4:447-453.
A 68-year-old man sought care in our emergency department for unilateral ptosis following superior and inferior right eyelid edema. The patient said that the edema had developed 3 days earlier and was getting worse each day; the ptosis was impairing his vision. The patient indicated that the edema was accompanied by mild burning in the right periocular region. His medical history included arterial hypertension, which was under control, and bilateral cataract surgery 5 years ago.
On examination, we noted superior and inferior nontender painless eyelid edema on the right eye, with no signs of acute inflammation (FIGURE). The patient also had right supraciliary folliculitis that was improving; the folliculitis had been treated 3 days earlier at a primary care facility.
We performed a complete ocular examination, including visual acuity (20/20 in both eyes) and found no other significant problems. Nor did the patient have a fever or any other systemic symptoms.
FIGURE 1
Edema of the upper and lower eyelid
The swelling was not accompanied by inflammation or fever, but it did impair the patient’s vision.
WHAT IS YOUR DIAGNOSIS?
HOW WOULD YOU TREAT THIS PATIENT?
Diagnosis: Noninflammatory eyelid edema
The fact that the patient’s eyelid was edematous (but not tender or red) and that he’d been scratching the area following a case of folliculitis prompted us to diagnose noninflammatory eyelid edema.
Noninflammatory eyelid edema—also called noninflammatory palpebral edema—is a relatively common disorder that usually occurs after some local irritation or microtrauma. In its early phase, patients start out with nonerythematous, painless edema of the upper eyelid, which eventually affects the lower eyelid.
As was the case with our patient, this disorder is not associated with fever or any other systemic sign or symptom. Complete blood count and C-reactive protein will be negative, as no infection or systemic alteration is present.
Consider these infectious alternatives
In cases like this one, be sure to differentiate between noninflammatory palpebral edema and other common but less benign ocular conditions. Among the infectious causes of unilateral edema to rule out:
Preseptal cellulitis is an infection that is localized between the skin and the orbital septum. This disorder usually appears as a tender erythematous eyelid edema with no proptosis and no pain with eye movement.1 It is usually accompanied by an elevated white blood cell (WBC) count. Blood cultures are rarely positive, but when they are, Haemophilus influenzae is the most frequent pathogen.2 Preseptal cellulitis is treated with broad-spectrum oral antibiotics (amoxicillin/ clavulanate) for at least 7 days.
Orbital cellulitis is an infection that affects the orbital extraocular structures. It can lead to blindness, so prompt diagnosis is critical.
Orbital cellulitis usually develops when a sinus infection spreads into the orbit.3 Suspect it in a patient with proptosis, orbital pain, tenderness, conjunctival chemosis, decreased vision, elevated intraocular pressure, and pain on eye movement. Also look for an elevated WBC count. Perform blood cultures to confirm the presence of a pathogen.
If you suspect orbital cellulitis, order an orbital computed tomography scan with contrast infusion, including axial and coronal views; it may reveal an infection of the soft tissue behind the orbital septum. Treat this condition with broad-spectrum intravenous antibiotics (ceftriaxone) for 1 week, followed by 2 weeks of oral antibiotics, completing a total of 21 days of antibiotics.
Hordeolum is a localized infection that occurs when a meibomian gland becomes blocked. It usually appears as a palpable subcutaneous nodule within the eyelid and requires treatment with warm compresses and a combination of antibiotics and steroid topical ointment (tobramycin and dexamethasone ophthalmic ointment 4 times a day for a week).4
Acute dacryoadenitis is a lacrimal gland infection that usually causes unilateral, painful swelling of the outer third of the upper lid. You may also see tearing and discharge.5 Look for an elevated WBC count; however, blood cultures are rarely positive. These patients must be referred to an ophthalmologist as treatment varies from symptomatic measures in viral cases (warm compresses and a nonsteroidal anti-inflammatory drug, such as ibuprofen) to hospitalization and oral or intravenous antibiotics (eg, amoxicillin/ clavulanate for at least 7 days), depending on the severity and origin of the infection.6
Ruling out other noninfectious disorders
Noninfectious inflammatory diseases should also be part of the differential diagnosis, including:
Idiopathic orbital inflammation. Also known as orbital pseudotumor, this disorder is a nongranulomatous acute-to-subacute inflammatory disease with no systemic manifestations.7 It frequently involves the lacrimal gland and can cause abrupt pain, conjunctival edema, and lid edema. Other common signs are proptosis and ocular motility alterations, which the patient may report as diplopia and visual impairment.
This disorder can result from optic neuropathy, exudative retinal detachment, or uveitis. It is a diagnosis of exclusion and is often arrived at by seeing the patient respond to systemic corticosteroids. The specific drug and dose will vary based on disease severity.
Graves’ ophthalmopathy. This bilateral, asymmetric immunological disorder affects the conjunctiva, eyelids,8 extraocular muscles, lacrimal gland, and optic nerve. Although it is typically diagnosed clinically, thyroid hormone abnormalities (increased T4 and a drop in thyroid-stimulating hormone) help support the diagnosis. In the acute phase, it has to be treated with systemic steroids; if the condition becomes chronic, the complications may require surgery. Treatment of the underlying hyperthyroidism may, in some cases, worsen the ophthalmopathy.
One more consideration. Finally, consider a local allergic reaction in the eyelids,9 which can also cause painless palpebral edema. Expect to see erythematous edema and intense itching a few hours after exposure to the allergen. A cosmetic product is often the culprit. As you might expect, initial treatment calls for withdrawal of the offending product. Instruct the patient to apply a topical steroid ointment on the eyelid if the edema is intense.
Good news for our patient
Diagnosing noninflammatory eyelid edema requires keen observational skills and a knowledge of several alternative diagnoses. Fortunately for our patient, this benign condition did not require any local or systemic treatment. The edema resolved on its own in 6 days.
CORRESPONDENCE
Omar Rayward, MD, Calle Profesor Martín Lagos, Madrid, Spain 28040; orayward@yahoo.com
A 68-year-old man sought care in our emergency department for unilateral ptosis following superior and inferior right eyelid edema. The patient said that the edema had developed 3 days earlier and was getting worse each day; the ptosis was impairing his vision. The patient indicated that the edema was accompanied by mild burning in the right periocular region. His medical history included arterial hypertension, which was under control, and bilateral cataract surgery 5 years ago.
On examination, we noted superior and inferior nontender painless eyelid edema on the right eye, with no signs of acute inflammation (FIGURE). The patient also had right supraciliary folliculitis that was improving; the folliculitis had been treated 3 days earlier at a primary care facility.
We performed a complete ocular examination, including visual acuity (20/20 in both eyes) and found no other significant problems. Nor did the patient have a fever or any other systemic symptoms.
FIGURE 1
Edema of the upper and lower eyelid
The swelling was not accompanied by inflammation or fever, but it did impair the patient’s vision.
WHAT IS YOUR DIAGNOSIS?
HOW WOULD YOU TREAT THIS PATIENT?
Diagnosis: Noninflammatory eyelid edema
The fact that the patient’s eyelid was edematous (but not tender or red) and that he’d been scratching the area following a case of folliculitis prompted us to diagnose noninflammatory eyelid edema.
Noninflammatory eyelid edema—also called noninflammatory palpebral edema—is a relatively common disorder that usually occurs after some local irritation or microtrauma. In its early phase, patients start out with nonerythematous, painless edema of the upper eyelid, which eventually affects the lower eyelid.
As was the case with our patient, this disorder is not associated with fever or any other systemic sign or symptom. Complete blood count and C-reactive protein will be negative, as no infection or systemic alteration is present.
Consider these infectious alternatives
In cases like this one, be sure to differentiate between noninflammatory palpebral edema and other common but less benign ocular conditions. Among the infectious causes of unilateral edema to rule out:
Preseptal cellulitis is an infection that is localized between the skin and the orbital septum. This disorder usually appears as a tender erythematous eyelid edema with no proptosis and no pain with eye movement.1 It is usually accompanied by an elevated white blood cell (WBC) count. Blood cultures are rarely positive, but when they are, Haemophilus influenzae is the most frequent pathogen.2 Preseptal cellulitis is treated with broad-spectrum oral antibiotics (amoxicillin/ clavulanate) for at least 7 days.
Orbital cellulitis is an infection that affects the orbital extraocular structures. It can lead to blindness, so prompt diagnosis is critical.
Orbital cellulitis usually develops when a sinus infection spreads into the orbit.3 Suspect it in a patient with proptosis, orbital pain, tenderness, conjunctival chemosis, decreased vision, elevated intraocular pressure, and pain on eye movement. Also look for an elevated WBC count. Perform blood cultures to confirm the presence of a pathogen.
If you suspect orbital cellulitis, order an orbital computed tomography scan with contrast infusion, including axial and coronal views; it may reveal an infection of the soft tissue behind the orbital septum. Treat this condition with broad-spectrum intravenous antibiotics (ceftriaxone) for 1 week, followed by 2 weeks of oral antibiotics, completing a total of 21 days of antibiotics.
Hordeolum is a localized infection that occurs when a meibomian gland becomes blocked. It usually appears as a palpable subcutaneous nodule within the eyelid and requires treatment with warm compresses and a combination of antibiotics and steroid topical ointment (tobramycin and dexamethasone ophthalmic ointment 4 times a day for a week).4
Acute dacryoadenitis is a lacrimal gland infection that usually causes unilateral, painful swelling of the outer third of the upper lid. You may also see tearing and discharge.5 Look for an elevated WBC count; however, blood cultures are rarely positive. These patients must be referred to an ophthalmologist as treatment varies from symptomatic measures in viral cases (warm compresses and a nonsteroidal anti-inflammatory drug, such as ibuprofen) to hospitalization and oral or intravenous antibiotics (eg, amoxicillin/ clavulanate for at least 7 days), depending on the severity and origin of the infection.6
Ruling out other noninfectious disorders
Noninfectious inflammatory diseases should also be part of the differential diagnosis, including:
Idiopathic orbital inflammation. Also known as orbital pseudotumor, this disorder is a nongranulomatous acute-to-subacute inflammatory disease with no systemic manifestations.7 It frequently involves the lacrimal gland and can cause abrupt pain, conjunctival edema, and lid edema. Other common signs are proptosis and ocular motility alterations, which the patient may report as diplopia and visual impairment.
This disorder can result from optic neuropathy, exudative retinal detachment, or uveitis. It is a diagnosis of exclusion and is often arrived at by seeing the patient respond to systemic corticosteroids. The specific drug and dose will vary based on disease severity.
Graves’ ophthalmopathy. This bilateral, asymmetric immunological disorder affects the conjunctiva, eyelids,8 extraocular muscles, lacrimal gland, and optic nerve. Although it is typically diagnosed clinically, thyroid hormone abnormalities (increased T4 and a drop in thyroid-stimulating hormone) help support the diagnosis. In the acute phase, it has to be treated with systemic steroids; if the condition becomes chronic, the complications may require surgery. Treatment of the underlying hyperthyroidism may, in some cases, worsen the ophthalmopathy.
One more consideration. Finally, consider a local allergic reaction in the eyelids,9 which can also cause painless palpebral edema. Expect to see erythematous edema and intense itching a few hours after exposure to the allergen. A cosmetic product is often the culprit. As you might expect, initial treatment calls for withdrawal of the offending product. Instruct the patient to apply a topical steroid ointment on the eyelid if the edema is intense.
Good news for our patient
Diagnosing noninflammatory eyelid edema requires keen observational skills and a knowledge of several alternative diagnoses. Fortunately for our patient, this benign condition did not require any local or systemic treatment. The edema resolved on its own in 6 days.
CORRESPONDENCE
Omar Rayward, MD, Calle Profesor Martín Lagos, Madrid, Spain 28040; orayward@yahoo.com
1. Bilyk JR. Periocular infection. Curr Opin Ophthalmol. 2007;18:414-423.
2. Jackson K, Baker SR. Periorbital cellulitis. Head Neck Surg. 1987;9:227-234.
3. Adam R, Gupta V, Harvey J. Question: can you identify this condition? This condition is orbital cellulitis. Can Fam Physician. 2009;55:1097.-
4. Lindsley K, Nichols JJ, Dickersin K. Interventions for acute internal hordeolum. Cochrane Database Syst Rev. 2010;(9):CD007742.-
5. Colegrove JA. Localized orbital inflammation: a case of dacryoadenitis. Optom Vis Sci. 2000;77:121-124.
6. Durand ML. Periocular infections. In: Mandell GL, Bennett JE, Dolin R, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 7th ed. Philadelphia, Pa: Elsevier Churchill Livingstone; 2009:1569–1575.
7. Cooney NL. Orbital pseudotumor. Int J Emerg Med. 2009;2:263.-
8. Imaizumi M. Recurrent upper eyelid edema as first sign of Graves’ disease. Thyroid. 2006;16:95-96.
9. Friedlaender MH. Objective measurement of allergic reactions in the eye. Curr Opin Allergy Clin Immunol. 2004;4:447-453.
1. Bilyk JR. Periocular infection. Curr Opin Ophthalmol. 2007;18:414-423.
2. Jackson K, Baker SR. Periorbital cellulitis. Head Neck Surg. 1987;9:227-234.
3. Adam R, Gupta V, Harvey J. Question: can you identify this condition? This condition is orbital cellulitis. Can Fam Physician. 2009;55:1097.-
4. Lindsley K, Nichols JJ, Dickersin K. Interventions for acute internal hordeolum. Cochrane Database Syst Rev. 2010;(9):CD007742.-
5. Colegrove JA. Localized orbital inflammation: a case of dacryoadenitis. Optom Vis Sci. 2000;77:121-124.
6. Durand ML. Periocular infections. In: Mandell GL, Bennett JE, Dolin R, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 7th ed. Philadelphia, Pa: Elsevier Churchill Livingstone; 2009:1569–1575.
7. Cooney NL. Orbital pseudotumor. Int J Emerg Med. 2009;2:263.-
8. Imaizumi M. Recurrent upper eyelid edema as first sign of Graves’ disease. Thyroid. 2006;16:95-96.
9. Friedlaender MH. Objective measurement of allergic reactions in the eye. Curr Opin Allergy Clin Immunol. 2004;4:447-453.