Clinical Review
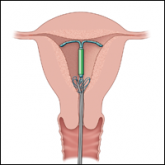
Overcoming LARC complications: 7 case challenges
The strings to your patient’s intrauterine device (IUD) are “missing.” Clinical experience and ACOG direction guide the management plans for this...
Dr. Burkman is Emeritus Professor of Obstetrics and Gynecology, Tufts University School of Medicine, Baystate Medical Center, Springfield, Massachusetts.
The author reports no financial relationships relevant to this article.

Yes—and their chances of continuing contraception at 2 years are greater and their chances of unintended pregnancy at 2 years are less than their SARC-using counterparts. This study included women randomly assigned to receive a LARC (long-acting reversible contraceptive) method (copper or levonorgestrel intrauterine device or subdermal implant) or a SARC (short-acting reversible contraceptive) method (oral contraceptives or depot medroxyprogesterone acetate); a separate cohort of women received a SARC method of preference. At 24 months, the randomized LARC users had a continuation probability of 64.3% compared with SARC users who were randomized or were in the preference group (25.5% and 40.0%, respectively). The unintended pregnancy probability was 3.6% in the randomized LARC group, while SARC users in either the randomized group or in the preferred methods group had pregnancy probability rates of 6.9% and 9.9%, respectively.
Hubacher D, Spector H, Monteith C, et al. Not seeking yet trying long-acting reversible contraception: a 24-month randomized trial on continuation, unintended pregnancy and satisfaction. Contraception. 2018;97:524-532.
EXPERT COMMENTARY
Because of women’s personal preference and aversion, for various reasons, to LARC methods, the current estimated use rate of 17% for LARC methods would increase only to 24% to 29% even if major barriers, such as cost and availability, were removed.1 To gain more insight into this issue, Hubacher and colleagues sought to determine if LARC methods would meet the contraceptive needs and be acceptable to a population of women who were not seeking these methods actively and who might have some reservation about using them.
The authors approached women actively seeking 1 of the 2 SARC methods but not a LARC method for contraception. They enrolled 524 women into a cohort study in which they received their desired SARC method. In addition, 392 women agreed to be enrolled in a randomized clinical trial comparing women beginning a LARC method for the first time with a group receiving 1 of the 2 SARC methods.
Importance of covered costs. Of note, the women in the randomized trial had the costs of the insertion or removal of the LARC method covered; those randomly assigned to the comparative SARC arm had the costs of their oral contraceptives (OCs) or depot medroxyprogesterone acetate (DMPA) covered for the first year of use. Underwriting the costs in the randomized study was likely important for study recruitment, since 47% of participants who were randomized to the LARC group cited cost as one of the reasons they did not try a LARC method previously.
Satisfaction with contraceptive method. In addition to the differences in continuation rates and pregnancy rates noted, it is interesting that, among women who tried a LARC method and who had some persistent negative feelings about the method, 65.9% would try the method again.
Satisfaction levels were estimated using 3 choices, with “happiness” being the highest level of satisfaction, followed by “neutral” and “unhappy.” At 24 months, the number of women indicating happiness was similar among the 3 study groups: 71.4% for the LARC randomized group, 75.0% for the randomized SARC group, and 77.6% for the preferred SARC cohort group.
Among women who discontinued their LARC method, occurrence of adverse effects was the reason given 74.2% of the time, while among SARC method users in both groups there was no dominant reason for discontinuation. Also, among women who discontinued their method, the percentage indicating happiness was 32.2% for the LARC randomized group compared with 69.9% and 68.2% for the randomized and preference cohort SARC groups, respectively.
This study had several strengths. The population from which the study groups were obtained was demographically diverse and was appropriate for determining if women with reservations about LARC methods could have satisfactory outcomes similar to women who self-select LARC methods. Further, the 24 months of observations indicate that, for the most part, satisfaction persisted.
One of the study’s shortcomings is the limited data on the subsets, that is, the specific method chosen, within each of the study groups.
Share your thoughts! Send your Letter to the Editor to rbarbieri@mdedge.com. Please include your name and the city and state in which you practice.

The strings to your patient’s intrauterine device (IUD) are “missing.” Clinical experience and ACOG direction guide the management plans for this...

How should you manage acne in an adolescent seeking progestin-based long-acting reversible contraception (LARC)?Examining the impact of...
