User login
Watch for cutaneous manifestations of tropical infectious diseases
Treatments designed to combat tropical infectious diseases are lacking, so the best thing travelers to these regions of the world can do is defend themselves against mosquito bites, according to Stephen K. Tyring, MD.
“We have no specific therapies for these infections,” explained Dr. Tyring of the University of Texas in Houston.
“Therefore, the best management is to avoid mosquito bites [by using] DEET, protective clothing, etc.,” he said in an interview prior to the Caribbean Dermatology Symposium.
“Treatment [of Zika virus infections] is supportive,” he said, because currently, there are no vaccine and no antiviral therapy aimed specifically at treating Zika virus infections. It’s also important for clinicians to rule out dengue and chikungunya when testing for Zika virus, and to avoid prescribing NSAIDs and aspirin until a definitive diagnosis is made, to avoid causing hemorrhaging.
Dr. Tyring also advised refraining from sexual contact with any individuals who have been to tropical areas and may have been exposed to the Zika virus.
Dr. Tyring also discussed the cutaneous manifestations and other symptoms of the flavivirus infections dengue and chikungunya.
“[About] 40% of the world’s population live in areas where there is a risk of dengue transmission, [and] the World Health Organization estimates that 50 to 100 million infections occur yearly, including 500,000 DHF [dengue hemorrhagic fever] cases and 22,000 deaths,” mostly in children, he said in his presentation at the meeting provided by Global Academy for Medical Education.
The tourniquet test is a useful tool to determine if a patient has dengue fever. This involves taking the patient’s blood pressure, then inflating the cuff to a point midway between the systolic and diastolic blood pressure, and maintaining it for 5 minutes. Deflate the cuff and wait for 2 minutes; then count the petechiae below the antecubital fossa. A positive test result is 10 or more petechiae per square inch, according to the CDC definition.
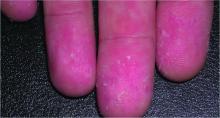
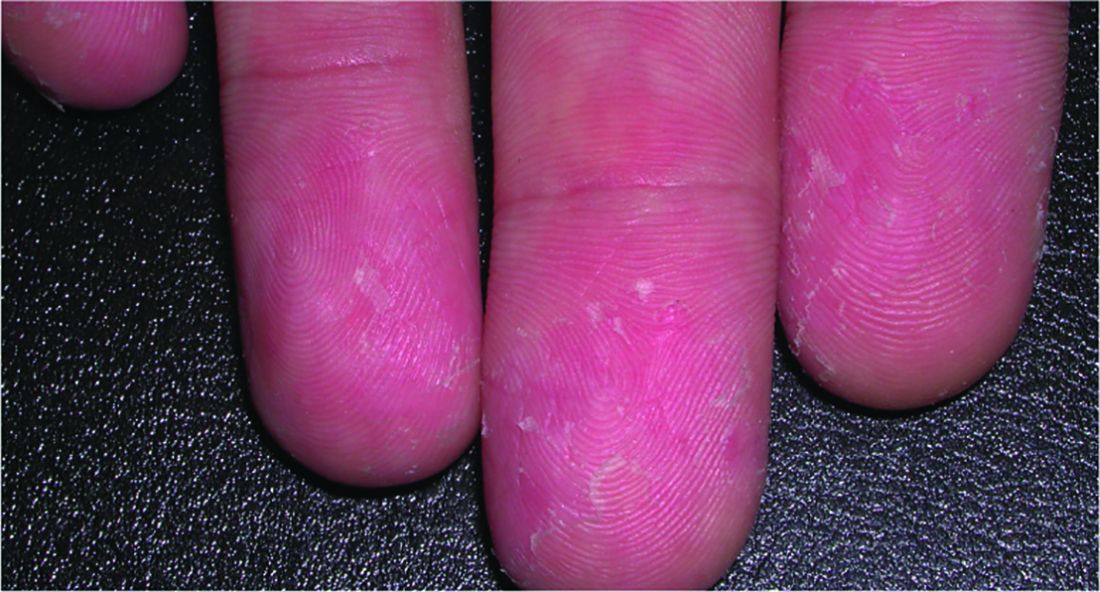
A relative of dengue, the chikungunya virus can present in the form of a morbilliform rash, nasal hyperpigmentation, purpuric macules, and erythema, the latter of which can sometimes be accompanied by ulcers. In addition to dermatologic symptoms (occurring in 40%-75% of patients), joint pain and fever also are associated with a chikungunya virus infection.
“Redness, swelling, and pain of the scrotum and groin region” also can occur, while “ulceration on the vulva in women has occasionally been reported in other outbreaks,” Dr. Tyring explained.
For further reading on this matter, Dr. Tyring recommended a report by Nawas et al. entitled, “Emerging infectious diseases with cutaneous manifestations” (J Am Acad Dermatol. 2016 Jul;75[1]:1-16) and a 2008 JAMA study on dengue and DHF coauthored by Anthony S. Fauci, MD (299[2]:214-6).
Dr. Tyring reported no relevant financial disclosures. Global Academy and this news organization are owned by the same parent company.
Treatments designed to combat tropical infectious diseases are lacking, so the best thing travelers to these regions of the world can do is defend themselves against mosquito bites, according to Stephen K. Tyring, MD.
“We have no specific therapies for these infections,” explained Dr. Tyring of the University of Texas in Houston.
“Therefore, the best management is to avoid mosquito bites [by using] DEET, protective clothing, etc.,” he said in an interview prior to the Caribbean Dermatology Symposium.
“Treatment [of Zika virus infections] is supportive,” he said, because currently, there are no vaccine and no antiviral therapy aimed specifically at treating Zika virus infections. It’s also important for clinicians to rule out dengue and chikungunya when testing for Zika virus, and to avoid prescribing NSAIDs and aspirin until a definitive diagnosis is made, to avoid causing hemorrhaging.
Dr. Tyring also advised refraining from sexual contact with any individuals who have been to tropical areas and may have been exposed to the Zika virus.
Dr. Tyring also discussed the cutaneous manifestations and other symptoms of the flavivirus infections dengue and chikungunya.
“[About] 40% of the world’s population live in areas where there is a risk of dengue transmission, [and] the World Health Organization estimates that 50 to 100 million infections occur yearly, including 500,000 DHF [dengue hemorrhagic fever] cases and 22,000 deaths,” mostly in children, he said in his presentation at the meeting provided by Global Academy for Medical Education.
The tourniquet test is a useful tool to determine if a patient has dengue fever. This involves taking the patient’s blood pressure, then inflating the cuff to a point midway between the systolic and diastolic blood pressure, and maintaining it for 5 minutes. Deflate the cuff and wait for 2 minutes; then count the petechiae below the antecubital fossa. A positive test result is 10 or more petechiae per square inch, according to the CDC definition.
A relative of dengue, the chikungunya virus can present in the form of a morbilliform rash, nasal hyperpigmentation, purpuric macules, and erythema, the latter of which can sometimes be accompanied by ulcers. In addition to dermatologic symptoms (occurring in 40%-75% of patients), joint pain and fever also are associated with a chikungunya virus infection.
“Redness, swelling, and pain of the scrotum and groin region” also can occur, while “ulceration on the vulva in women has occasionally been reported in other outbreaks,” Dr. Tyring explained.
For further reading on this matter, Dr. Tyring recommended a report by Nawas et al. entitled, “Emerging infectious diseases with cutaneous manifestations” (J Am Acad Dermatol. 2016 Jul;75[1]:1-16) and a 2008 JAMA study on dengue and DHF coauthored by Anthony S. Fauci, MD (299[2]:214-6).
Dr. Tyring reported no relevant financial disclosures. Global Academy and this news organization are owned by the same parent company.
Treatments designed to combat tropical infectious diseases are lacking, so the best thing travelers to these regions of the world can do is defend themselves against mosquito bites, according to Stephen K. Tyring, MD.
“We have no specific therapies for these infections,” explained Dr. Tyring of the University of Texas in Houston.
“Therefore, the best management is to avoid mosquito bites [by using] DEET, protective clothing, etc.,” he said in an interview prior to the Caribbean Dermatology Symposium.
“Treatment [of Zika virus infections] is supportive,” he said, because currently, there are no vaccine and no antiviral therapy aimed specifically at treating Zika virus infections. It’s also important for clinicians to rule out dengue and chikungunya when testing for Zika virus, and to avoid prescribing NSAIDs and aspirin until a definitive diagnosis is made, to avoid causing hemorrhaging.
Dr. Tyring also advised refraining from sexual contact with any individuals who have been to tropical areas and may have been exposed to the Zika virus.
Dr. Tyring also discussed the cutaneous manifestations and other symptoms of the flavivirus infections dengue and chikungunya.
“[About] 40% of the world’s population live in areas where there is a risk of dengue transmission, [and] the World Health Organization estimates that 50 to 100 million infections occur yearly, including 500,000 DHF [dengue hemorrhagic fever] cases and 22,000 deaths,” mostly in children, he said in his presentation at the meeting provided by Global Academy for Medical Education.
The tourniquet test is a useful tool to determine if a patient has dengue fever. This involves taking the patient’s blood pressure, then inflating the cuff to a point midway between the systolic and diastolic blood pressure, and maintaining it for 5 minutes. Deflate the cuff and wait for 2 minutes; then count the petechiae below the antecubital fossa. A positive test result is 10 or more petechiae per square inch, according to the CDC definition.
A relative of dengue, the chikungunya virus can present in the form of a morbilliform rash, nasal hyperpigmentation, purpuric macules, and erythema, the latter of which can sometimes be accompanied by ulcers. In addition to dermatologic symptoms (occurring in 40%-75% of patients), joint pain and fever also are associated with a chikungunya virus infection.
“Redness, swelling, and pain of the scrotum and groin region” also can occur, while “ulceration on the vulva in women has occasionally been reported in other outbreaks,” Dr. Tyring explained.
For further reading on this matter, Dr. Tyring recommended a report by Nawas et al. entitled, “Emerging infectious diseases with cutaneous manifestations” (J Am Acad Dermatol. 2016 Jul;75[1]:1-16) and a 2008 JAMA study on dengue and DHF coauthored by Anthony S. Fauci, MD (299[2]:214-6).
Dr. Tyring reported no relevant financial disclosures. Global Academy and this news organization are owned by the same parent company.
EXPERT ANALYSIS FROM THE CARIBBEAN DERMATOLOGY SYMPOSIUM
Expert reviews options for refractory pediatric warts
For refractory warts, there are some “last resort” treatments every dermatologist should have on hand, according to pediatric dermatologist Fred E. Ghali, MD.
“It’s good to know about these, although it’s also good to know that sometimes you just have to wait out the warts and let them clear up on their own,” said Dr. Ghali, of the departments of dermatology at University of Texas, Dallas, and Baylor College of Medicine, Houston. Because very few treatment options are approved for warts, Dr. Ghali shared some of his preferred off-label approaches at the meeting provided by Global Academy for Medical Education.
By the time patients make it to his clinic, Dr. Ghali noted that many patients have failed home remedies such as salicylic acid or duct tape. In some cases, however, warts may not respond well to the standard in-office options such as cryotherapy. For refractory cases, he said that one of the following approaches can be considered:
Sectional cryotherapy
For larger, solitary warts, especially ring warts, freezing them in sections can be a good option, according to Dr. Ghali. This can be done best using a cotton-tip applicator rather than the traditional spray gun. In his experience, this minimizes the risk of ring wart formation, which may occur from aggressive cryotherapy focused primarily on the central portion of the wart, sometimes creating a resultant blister much larger than the original wart, with the formation of a ring wart.
Topical immunotherapy
When it comes to refractory cases in younger children, or in cases with multiple warts on the hands and feet, topical immunotherapy is often a preferred treatment. In these cases, Dr. Ghali recommended squaric acid. “The general principle with topical immunotherapy is that you would induce contact allergy with the treatment by applying it to one place on the skin, usually the arm, in the office setting,” he said. If using squaric acid, he recommended starting with 2% to sensitize in the office; then for home use, prescribing a lower concentration of the treatment – usually 0.6% – painted directly onto the lesions to provoke an immune response. This should be done three times a week at first, and then adding one application each week until the warts are being treated daily.
“If there is no response in 2 months, then increase the strength used at home,” Dr. Ghali said.
With this treatment, there is the potential for contact dermatitis, which is usually localized, but can be widespread beyond the areas of application, he cautioned. When this occurs, he recommended decreasing or discontinuing the applications and considering a topical steroid or oral steroid depending upon the severity of the reaction. “I mainly use squaric acid for the hands and feet, and almost always avoid it on the face, neck, and groin,” Dr. Ghali said.
In his practice, he finds this treatment is effective about three-quarters of the time, and seems to work particularly well with plantar warts, clearing them up in 2-4 months. The advantages of this approach are that it is not painful, is relatively easy for patients to comply with, and can be combined with other treatments if desired.
Intralesional immunotherapy
When squaric acid or cryotherapy fails, Candida antigen injection is a commonly used technique used to train the immune system to attack the warts, inducing a delayed hypersensitivity reaction. “Injectable immunotherapy is ideal in cases of a solitary [wart] or a limited number of warts,” Dr. Ghali said in an interview. “For most patients, I typically inject 0.1-0.2 cc of Candida antigen per wart. In the case of larger, ring-type warts, especially on the knees and elbows, we may need to use larger volumes, up to 0.2 cc-0.6cc,” he added.
“It’s important to remind patients that temporary, localized swelling may occur after injections; thus, care should be taken when injecting near periungual locations,” Dr. Ghali continued, noting that “it’s probably best practice to avoid subungual injections.”
Immunotherapy has relatively few side effects, and may be effective in about three-quarters of cases, according to Dr. Ghali, although he cautioned that younger children may be anxious about receiving injections and may resist treatment.
Electrodessication and curettage
For challenging warts, such as stubborn palmar or plantar warts, Dr. Ghali suggested using local anesthesia plus electrodessication and curettage.
“Sometimes with these refractory warts, we resort to off-label therapies compounded for home use,” he added. Such therapies may include salicylic acid with 5-fluorouracil, or topical cidofovir 2%-3%. These compounds can be costly depending upon the patient’s insurance coverage.
Dr. Ghali concluded by presenting his top three rules to consider when treating warts, regardless of treatment: There is no cure for warts, no therapy is uniformly effective, and the chosen therapy should take into account the family’s costs, according to their insurance coverage.
Since the landscape of insurance coverage has changed over recent years, the code most often used to treat warts in the office, often applies to the patient’s or family’s deductible. “It’s important to discuss this with the family beforehand, especially since treatment for warts may require several visits,” he said.
Dr. Ghali disclosed several financial relationships with the pharmaceutical industry including Astellas, Galderma, and Valeant, among others.
Global Academy and this news organization are owned by the same parent company.
For refractory warts, there are some “last resort” treatments every dermatologist should have on hand, according to pediatric dermatologist Fred E. Ghali, MD.
“It’s good to know about these, although it’s also good to know that sometimes you just have to wait out the warts and let them clear up on their own,” said Dr. Ghali, of the departments of dermatology at University of Texas, Dallas, and Baylor College of Medicine, Houston. Because very few treatment options are approved for warts, Dr. Ghali shared some of his preferred off-label approaches at the meeting provided by Global Academy for Medical Education.
By the time patients make it to his clinic, Dr. Ghali noted that many patients have failed home remedies such as salicylic acid or duct tape. In some cases, however, warts may not respond well to the standard in-office options such as cryotherapy. For refractory cases, he said that one of the following approaches can be considered:
Sectional cryotherapy
For larger, solitary warts, especially ring warts, freezing them in sections can be a good option, according to Dr. Ghali. This can be done best using a cotton-tip applicator rather than the traditional spray gun. In his experience, this minimizes the risk of ring wart formation, which may occur from aggressive cryotherapy focused primarily on the central portion of the wart, sometimes creating a resultant blister much larger than the original wart, with the formation of a ring wart.
Topical immunotherapy
When it comes to refractory cases in younger children, or in cases with multiple warts on the hands and feet, topical immunotherapy is often a preferred treatment. In these cases, Dr. Ghali recommended squaric acid. “The general principle with topical immunotherapy is that you would induce contact allergy with the treatment by applying it to one place on the skin, usually the arm, in the office setting,” he said. If using squaric acid, he recommended starting with 2% to sensitize in the office; then for home use, prescribing a lower concentration of the treatment – usually 0.6% – painted directly onto the lesions to provoke an immune response. This should be done three times a week at first, and then adding one application each week until the warts are being treated daily.
“If there is no response in 2 months, then increase the strength used at home,” Dr. Ghali said.
With this treatment, there is the potential for contact dermatitis, which is usually localized, but can be widespread beyond the areas of application, he cautioned. When this occurs, he recommended decreasing or discontinuing the applications and considering a topical steroid or oral steroid depending upon the severity of the reaction. “I mainly use squaric acid for the hands and feet, and almost always avoid it on the face, neck, and groin,” Dr. Ghali said.
In his practice, he finds this treatment is effective about three-quarters of the time, and seems to work particularly well with plantar warts, clearing them up in 2-4 months. The advantages of this approach are that it is not painful, is relatively easy for patients to comply with, and can be combined with other treatments if desired.
Intralesional immunotherapy
When squaric acid or cryotherapy fails, Candida antigen injection is a commonly used technique used to train the immune system to attack the warts, inducing a delayed hypersensitivity reaction. “Injectable immunotherapy is ideal in cases of a solitary [wart] or a limited number of warts,” Dr. Ghali said in an interview. “For most patients, I typically inject 0.1-0.2 cc of Candida antigen per wart. In the case of larger, ring-type warts, especially on the knees and elbows, we may need to use larger volumes, up to 0.2 cc-0.6cc,” he added.
“It’s important to remind patients that temporary, localized swelling may occur after injections; thus, care should be taken when injecting near periungual locations,” Dr. Ghali continued, noting that “it’s probably best practice to avoid subungual injections.”
Immunotherapy has relatively few side effects, and may be effective in about three-quarters of cases, according to Dr. Ghali, although he cautioned that younger children may be anxious about receiving injections and may resist treatment.
Electrodessication and curettage
For challenging warts, such as stubborn palmar or plantar warts, Dr. Ghali suggested using local anesthesia plus electrodessication and curettage.
“Sometimes with these refractory warts, we resort to off-label therapies compounded for home use,” he added. Such therapies may include salicylic acid with 5-fluorouracil, or topical cidofovir 2%-3%. These compounds can be costly depending upon the patient’s insurance coverage.
Dr. Ghali concluded by presenting his top three rules to consider when treating warts, regardless of treatment: There is no cure for warts, no therapy is uniformly effective, and the chosen therapy should take into account the family’s costs, according to their insurance coverage.
Since the landscape of insurance coverage has changed over recent years, the code most often used to treat warts in the office, often applies to the patient’s or family’s deductible. “It’s important to discuss this with the family beforehand, especially since treatment for warts may require several visits,” he said.
Dr. Ghali disclosed several financial relationships with the pharmaceutical industry including Astellas, Galderma, and Valeant, among others.
Global Academy and this news organization are owned by the same parent company.
For refractory warts, there are some “last resort” treatments every dermatologist should have on hand, according to pediatric dermatologist Fred E. Ghali, MD.
“It’s good to know about these, although it’s also good to know that sometimes you just have to wait out the warts and let them clear up on their own,” said Dr. Ghali, of the departments of dermatology at University of Texas, Dallas, and Baylor College of Medicine, Houston. Because very few treatment options are approved for warts, Dr. Ghali shared some of his preferred off-label approaches at the meeting provided by Global Academy for Medical Education.
By the time patients make it to his clinic, Dr. Ghali noted that many patients have failed home remedies such as salicylic acid or duct tape. In some cases, however, warts may not respond well to the standard in-office options such as cryotherapy. For refractory cases, he said that one of the following approaches can be considered:
Sectional cryotherapy
For larger, solitary warts, especially ring warts, freezing them in sections can be a good option, according to Dr. Ghali. This can be done best using a cotton-tip applicator rather than the traditional spray gun. In his experience, this minimizes the risk of ring wart formation, which may occur from aggressive cryotherapy focused primarily on the central portion of the wart, sometimes creating a resultant blister much larger than the original wart, with the formation of a ring wart.
Topical immunotherapy
When it comes to refractory cases in younger children, or in cases with multiple warts on the hands and feet, topical immunotherapy is often a preferred treatment. In these cases, Dr. Ghali recommended squaric acid. “The general principle with topical immunotherapy is that you would induce contact allergy with the treatment by applying it to one place on the skin, usually the arm, in the office setting,” he said. If using squaric acid, he recommended starting with 2% to sensitize in the office; then for home use, prescribing a lower concentration of the treatment – usually 0.6% – painted directly onto the lesions to provoke an immune response. This should be done three times a week at first, and then adding one application each week until the warts are being treated daily.
“If there is no response in 2 months, then increase the strength used at home,” Dr. Ghali said.
With this treatment, there is the potential for contact dermatitis, which is usually localized, but can be widespread beyond the areas of application, he cautioned. When this occurs, he recommended decreasing or discontinuing the applications and considering a topical steroid or oral steroid depending upon the severity of the reaction. “I mainly use squaric acid for the hands and feet, and almost always avoid it on the face, neck, and groin,” Dr. Ghali said.
In his practice, he finds this treatment is effective about three-quarters of the time, and seems to work particularly well with plantar warts, clearing them up in 2-4 months. The advantages of this approach are that it is not painful, is relatively easy for patients to comply with, and can be combined with other treatments if desired.
Intralesional immunotherapy
When squaric acid or cryotherapy fails, Candida antigen injection is a commonly used technique used to train the immune system to attack the warts, inducing a delayed hypersensitivity reaction. “Injectable immunotherapy is ideal in cases of a solitary [wart] or a limited number of warts,” Dr. Ghali said in an interview. “For most patients, I typically inject 0.1-0.2 cc of Candida antigen per wart. In the case of larger, ring-type warts, especially on the knees and elbows, we may need to use larger volumes, up to 0.2 cc-0.6cc,” he added.
“It’s important to remind patients that temporary, localized swelling may occur after injections; thus, care should be taken when injecting near periungual locations,” Dr. Ghali continued, noting that “it’s probably best practice to avoid subungual injections.”
Immunotherapy has relatively few side effects, and may be effective in about three-quarters of cases, according to Dr. Ghali, although he cautioned that younger children may be anxious about receiving injections and may resist treatment.
Electrodessication and curettage
For challenging warts, such as stubborn palmar or plantar warts, Dr. Ghali suggested using local anesthesia plus electrodessication and curettage.
“Sometimes with these refractory warts, we resort to off-label therapies compounded for home use,” he added. Such therapies may include salicylic acid with 5-fluorouracil, or topical cidofovir 2%-3%. These compounds can be costly depending upon the patient’s insurance coverage.
Dr. Ghali concluded by presenting his top three rules to consider when treating warts, regardless of treatment: There is no cure for warts, no therapy is uniformly effective, and the chosen therapy should take into account the family’s costs, according to their insurance coverage.
Since the landscape of insurance coverage has changed over recent years, the code most often used to treat warts in the office, often applies to the patient’s or family’s deductible. “It’s important to discuss this with the family beforehand, especially since treatment for warts may require several visits,” he said.
Dr. Ghali disclosed several financial relationships with the pharmaceutical industry including Astellas, Galderma, and Valeant, among others.
Global Academy and this news organization are owned by the same parent company.
EXPERT ANALYSIS FROM THE CARIBBEAN DERMATOLOGY SYMPOSIUM
Topical crisaborole new option for AD
There’s a new addition to the armamentarium for atopic dermatitis: a topical phosphodiesterase 4 (PDE-4) inhibitor.
“It’s a real boon to patients, now that we have crisaborole as a first-line treatment for mild to moderate atopic dermatitis,” Joseph F. Fowler Jr., MD, of the University of Louisville (Ky.), said in an interview. “In the trials leading up to its approval, crisaborole was impressive in that it was well tolerated, and the results held up across all age groups over time.” Dr. Fowler spoke at the meeting provided by Global Academy for Medical Education.
Topical ointment crisaborole 2% (Eucrisa) was approved by the Food and Drug Administration in December 2016 for mild to moderate atopic dermatitis in patients aged 2 years and older. Approval was based on two placebo-controlled trials with more than 1,500 participants between the ages of 2 and 79 years with mild to moderate atopic dermatitis.
“That it’s not a steroid is important since there are so few options for this pesky condition. We have topical steroids, but a lot of patients get nervous about the overuse of those, just as they do about the box warning for cancer risk on topical calcineurin inhibitors,” Dr. Fowler said. The most common treatment-related adverse event recorded during the trials were burning and stinging at the site of application.
“While topical corticosteroids are certainly effective, I am concerned about the risk of atrophy, especially in children and on sensitive areas such as the face and intertriginous areas. This new treatment does not have that potential adverse effect,” he said.
Global Academy and this news organization are owned by the same parent company.
Dr. Fowler disclosed that he has financial relationships with Anacor Pharmaceuticals – the manufacturer of crisaborole – and Pfizer, among other companies.
There’s a new addition to the armamentarium for atopic dermatitis: a topical phosphodiesterase 4 (PDE-4) inhibitor.
“It’s a real boon to patients, now that we have crisaborole as a first-line treatment for mild to moderate atopic dermatitis,” Joseph F. Fowler Jr., MD, of the University of Louisville (Ky.), said in an interview. “In the trials leading up to its approval, crisaborole was impressive in that it was well tolerated, and the results held up across all age groups over time.” Dr. Fowler spoke at the meeting provided by Global Academy for Medical Education.
Topical ointment crisaborole 2% (Eucrisa) was approved by the Food and Drug Administration in December 2016 for mild to moderate atopic dermatitis in patients aged 2 years and older. Approval was based on two placebo-controlled trials with more than 1,500 participants between the ages of 2 and 79 years with mild to moderate atopic dermatitis.
“That it’s not a steroid is important since there are so few options for this pesky condition. We have topical steroids, but a lot of patients get nervous about the overuse of those, just as they do about the box warning for cancer risk on topical calcineurin inhibitors,” Dr. Fowler said. The most common treatment-related adverse event recorded during the trials were burning and stinging at the site of application.
“While topical corticosteroids are certainly effective, I am concerned about the risk of atrophy, especially in children and on sensitive areas such as the face and intertriginous areas. This new treatment does not have that potential adverse effect,” he said.
Global Academy and this news organization are owned by the same parent company.
Dr. Fowler disclosed that he has financial relationships with Anacor Pharmaceuticals – the manufacturer of crisaborole – and Pfizer, among other companies.
There’s a new addition to the armamentarium for atopic dermatitis: a topical phosphodiesterase 4 (PDE-4) inhibitor.
“It’s a real boon to patients, now that we have crisaborole as a first-line treatment for mild to moderate atopic dermatitis,” Joseph F. Fowler Jr., MD, of the University of Louisville (Ky.), said in an interview. “In the trials leading up to its approval, crisaborole was impressive in that it was well tolerated, and the results held up across all age groups over time.” Dr. Fowler spoke at the meeting provided by Global Academy for Medical Education.
Topical ointment crisaborole 2% (Eucrisa) was approved by the Food and Drug Administration in December 2016 for mild to moderate atopic dermatitis in patients aged 2 years and older. Approval was based on two placebo-controlled trials with more than 1,500 participants between the ages of 2 and 79 years with mild to moderate atopic dermatitis.
“That it’s not a steroid is important since there are so few options for this pesky condition. We have topical steroids, but a lot of patients get nervous about the overuse of those, just as they do about the box warning for cancer risk on topical calcineurin inhibitors,” Dr. Fowler said. The most common treatment-related adverse event recorded during the trials were burning and stinging at the site of application.
“While topical corticosteroids are certainly effective, I am concerned about the risk of atrophy, especially in children and on sensitive areas such as the face and intertriginous areas. This new treatment does not have that potential adverse effect,” he said.
Global Academy and this news organization are owned by the same parent company.
Dr. Fowler disclosed that he has financial relationships with Anacor Pharmaceuticals – the manufacturer of crisaborole – and Pfizer, among other companies.
FROM THE CARIBBEAN DERMATOLOGY SYMPOSIUM