User login
Cutting back ICU antibiotics could significantly reduce MDRO transmissions
Cutting back on antibiotic courses in intensive care unit settings can significantly reduce the number of multidrug-resistant organism (MDRO) transmissions, according to the findings of a modeling study.
“Significant opportunities exist to optimize and reduce antibiotic usage, [but] the impact of reducing overall antibiotic usage on antibiotic resistance is not known and would be difficult to assess using traditional study designs,” wrote Sean L. Barnes, PhD, of the University of Maryland, College Park, and his colleagues. “Therefore, we applied mathematical modeling to estimate the effect of reducing antibiotic usage on antibiotic resistance.”
Using an agent-based model – which allows for a realistic prediction of interactions between patients and health care workers, while also allowing for heterogeneity in the characteristics of each distinct “person” – Dr. Barnes and his coinvestigators simulated the transmission of MDROs from health care workers to patients.
Methicillin-resistant Staphylococcus aureus and vancomycin-resistant enterococci were deemed “high-prevalence pathogens;” carbapenem-resistant Enterobacteriaceae, multidrug-resistant Acinetobacter baumannii, and multidrug-resistant Pseudomonas aeruginosa were deemed low-prevalence pathogens. These designations were based on transmission rates found in existing literature.
Patients on antibiotic courses were set at 75% (0.75) at baseline, which was then adjusted to determine its effect on overall MDRO transmission. The number of patients at baseline was 18, with nine nurses, two physicians, and six other health care workers. Mean length-of-stay was 3.5 days, hand hygiene rates were set at 80% for nurses and 50% for physicians, with a 0.83 (83%) efficacy rate when followed. The probability of worker-to-patient transmission was set at 0.025 (2.5%), and set at 0.075 (7.5%) for transmission going the other way.
“We simulated the transmission of the high- and low-prevalence MDROs for 1 year [and] performed 200 replications each for 33 parameter-based scenarios,” the authors said.
When the number of patients on an antibiotic course was dropped from 75% to 65% (a drop of 10%), the rate of high-prevalence MDRO transmission dropped by 11.2% (P < .001). When reduced from 75% to 50% (a drop of 25%), the high-prevalence MDRO transmission rate fell by 28.3% (P < .001), according to the model.
Low-prevalence MDROs also reduced by significant amounts when antibiotic regimens were cut back by the same percentages, with transmission rates falling by 14.3% (P < .001) and 29.8% (P < .001), respectively.
In terms of microbiome effects, the 10% reduction in antibiotics lowered high-prevalence rates by an effect of 1.5, and low-prevalence rates by 1.7; those numbers were 1.2 and 1.4, respectively, when antibiotics were dropped by 25%.
“These reductions are statistically significant and proportionally similar for both high- and low-prevalence MDROs,” the authors concluded, “and they can potentially decrease MDRO acquisition among patients who are receiving antibiotics, as well as among patients who are not receiving antibiotics.”
The National Institutes of Health and the Department of Veterans Affairs’ Health Services Research and Development Department funded the study. Dr. Barnes and his coauthors reported no relevant financial disclosures.
Cutting back on antibiotic courses in intensive care unit settings can significantly reduce the number of multidrug-resistant organism (MDRO) transmissions, according to the findings of a modeling study.
“Significant opportunities exist to optimize and reduce antibiotic usage, [but] the impact of reducing overall antibiotic usage on antibiotic resistance is not known and would be difficult to assess using traditional study designs,” wrote Sean L. Barnes, PhD, of the University of Maryland, College Park, and his colleagues. “Therefore, we applied mathematical modeling to estimate the effect of reducing antibiotic usage on antibiotic resistance.”
Using an agent-based model – which allows for a realistic prediction of interactions between patients and health care workers, while also allowing for heterogeneity in the characteristics of each distinct “person” – Dr. Barnes and his coinvestigators simulated the transmission of MDROs from health care workers to patients.
Methicillin-resistant Staphylococcus aureus and vancomycin-resistant enterococci were deemed “high-prevalence pathogens;” carbapenem-resistant Enterobacteriaceae, multidrug-resistant Acinetobacter baumannii, and multidrug-resistant Pseudomonas aeruginosa were deemed low-prevalence pathogens. These designations were based on transmission rates found in existing literature.
Patients on antibiotic courses were set at 75% (0.75) at baseline, which was then adjusted to determine its effect on overall MDRO transmission. The number of patients at baseline was 18, with nine nurses, two physicians, and six other health care workers. Mean length-of-stay was 3.5 days, hand hygiene rates were set at 80% for nurses and 50% for physicians, with a 0.83 (83%) efficacy rate when followed. The probability of worker-to-patient transmission was set at 0.025 (2.5%), and set at 0.075 (7.5%) for transmission going the other way.
“We simulated the transmission of the high- and low-prevalence MDROs for 1 year [and] performed 200 replications each for 33 parameter-based scenarios,” the authors said.
When the number of patients on an antibiotic course was dropped from 75% to 65% (a drop of 10%), the rate of high-prevalence MDRO transmission dropped by 11.2% (P < .001). When reduced from 75% to 50% (a drop of 25%), the high-prevalence MDRO transmission rate fell by 28.3% (P < .001), according to the model.
Low-prevalence MDROs also reduced by significant amounts when antibiotic regimens were cut back by the same percentages, with transmission rates falling by 14.3% (P < .001) and 29.8% (P < .001), respectively.
In terms of microbiome effects, the 10% reduction in antibiotics lowered high-prevalence rates by an effect of 1.5, and low-prevalence rates by 1.7; those numbers were 1.2 and 1.4, respectively, when antibiotics were dropped by 25%.
“These reductions are statistically significant and proportionally similar for both high- and low-prevalence MDROs,” the authors concluded, “and they can potentially decrease MDRO acquisition among patients who are receiving antibiotics, as well as among patients who are not receiving antibiotics.”
The National Institutes of Health and the Department of Veterans Affairs’ Health Services Research and Development Department funded the study. Dr. Barnes and his coauthors reported no relevant financial disclosures.
Cutting back on antibiotic courses in intensive care unit settings can significantly reduce the number of multidrug-resistant organism (MDRO) transmissions, according to the findings of a modeling study.
“Significant opportunities exist to optimize and reduce antibiotic usage, [but] the impact of reducing overall antibiotic usage on antibiotic resistance is not known and would be difficult to assess using traditional study designs,” wrote Sean L. Barnes, PhD, of the University of Maryland, College Park, and his colleagues. “Therefore, we applied mathematical modeling to estimate the effect of reducing antibiotic usage on antibiotic resistance.”
Using an agent-based model – which allows for a realistic prediction of interactions between patients and health care workers, while also allowing for heterogeneity in the characteristics of each distinct “person” – Dr. Barnes and his coinvestigators simulated the transmission of MDROs from health care workers to patients.
Methicillin-resistant Staphylococcus aureus and vancomycin-resistant enterococci were deemed “high-prevalence pathogens;” carbapenem-resistant Enterobacteriaceae, multidrug-resistant Acinetobacter baumannii, and multidrug-resistant Pseudomonas aeruginosa were deemed low-prevalence pathogens. These designations were based on transmission rates found in existing literature.
Patients on antibiotic courses were set at 75% (0.75) at baseline, which was then adjusted to determine its effect on overall MDRO transmission. The number of patients at baseline was 18, with nine nurses, two physicians, and six other health care workers. Mean length-of-stay was 3.5 days, hand hygiene rates were set at 80% for nurses and 50% for physicians, with a 0.83 (83%) efficacy rate when followed. The probability of worker-to-patient transmission was set at 0.025 (2.5%), and set at 0.075 (7.5%) for transmission going the other way.
“We simulated the transmission of the high- and low-prevalence MDROs for 1 year [and] performed 200 replications each for 33 parameter-based scenarios,” the authors said.
When the number of patients on an antibiotic course was dropped from 75% to 65% (a drop of 10%), the rate of high-prevalence MDRO transmission dropped by 11.2% (P < .001). When reduced from 75% to 50% (a drop of 25%), the high-prevalence MDRO transmission rate fell by 28.3% (P < .001), according to the model.
Low-prevalence MDROs also reduced by significant amounts when antibiotic regimens were cut back by the same percentages, with transmission rates falling by 14.3% (P < .001) and 29.8% (P < .001), respectively.
In terms of microbiome effects, the 10% reduction in antibiotics lowered high-prevalence rates by an effect of 1.5, and low-prevalence rates by 1.7; those numbers were 1.2 and 1.4, respectively, when antibiotics were dropped by 25%.
“These reductions are statistically significant and proportionally similar for both high- and low-prevalence MDROs,” the authors concluded, “and they can potentially decrease MDRO acquisition among patients who are receiving antibiotics, as well as among patients who are not receiving antibiotics.”
The National Institutes of Health and the Department of Veterans Affairs’ Health Services Research and Development Department funded the study. Dr. Barnes and his coauthors reported no relevant financial disclosures.
FROM INFECTION CONTROL & HOSPITAL EPIDEMIOLOGY
Key clinical point:
Major finding: A 10% reduction in prescribed antibiotic courses saw high-prevalence MDRO transmission drop by 11.2%, and a 25% reduction caused a drop of 28.3%; low-prevalence MDROs dropped by 14.3% and 29.8%, respectively (P < .001 for all).
Data source: An agent-based model of a single ICU with 18 patients and 17 health care workers at baseline.
Disclosures: The National Institutes of Health and the Department of Veterans Affairs’ Health Services Research and Development Department funded the study. Dr. Barnes and his coauthors reported no relevant financial disclosures.
New antibody shows potential as prognostic marker in early rheumatoid arthritis
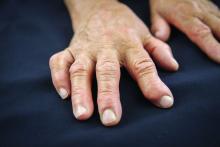
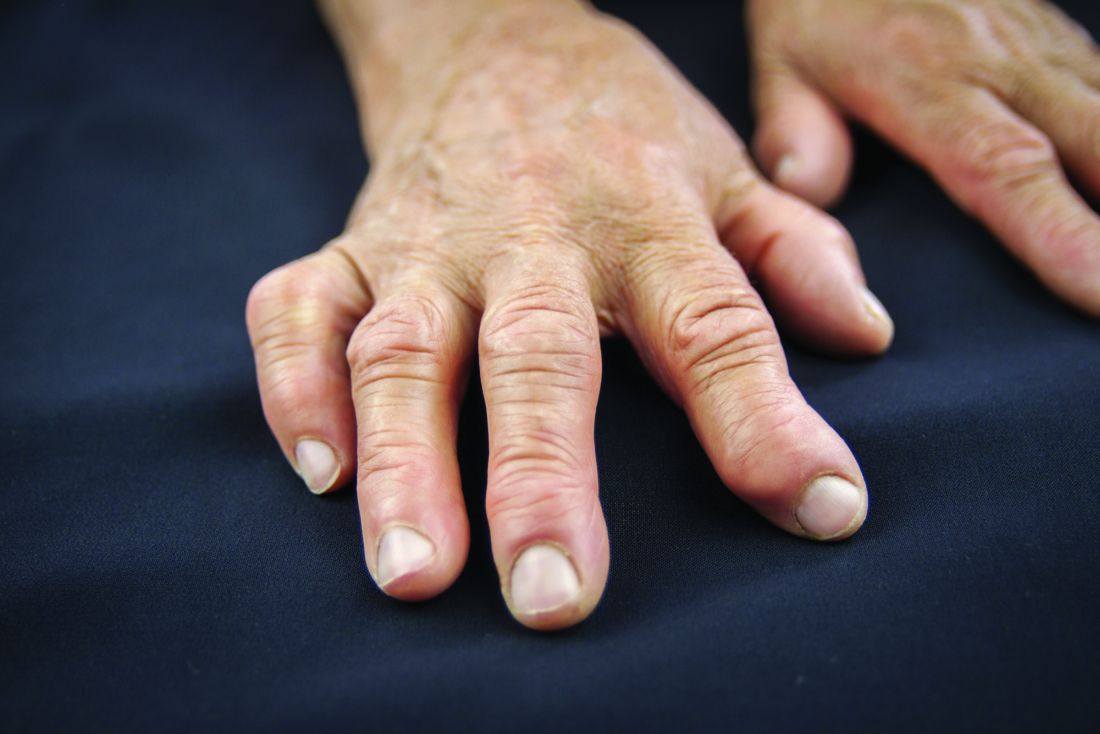
Individuals with rheumatoid arthritis who have antifibrillar collagen type II antibodies appear to have a unique disease phenotype characterized by acute but transient inflammation around the time of diagnosis, as well as a favorable prognosis, according to findings from a retrospective cohort study.
The antifibrillar collagen type II (anti-CII) phenotype also differed from the phenotype of individuals with anti–cyclic citrullinated peptide 2 (anti-CCP2) antibodies who typically exhibit inflammatory markers and higher disease activity later in the disease course, reported Vivek Anand Manivel of Uppsala (Sweden) University and his colleagues (Ann Rheum Dis. 2017 Mar 23. doi: 10.1136/annrheumdis-2016-210873).
Overall, the investigators detected anti-CII positivity in 6.6% and anti-CCP2 in 57.9%, including only anti-CII antibodies in 2.6%, only anti-CCP2 in 54%, double positivity in 3.9%, and double negativity in 39.4%. A control group of 960 patients from the Swedish general population who were matched for age, locality, and sex were positive for anti-CII in 1.6% and anti-CCP2 in 1.7%.
Significant differences were discovered between anti-CII positive and negative groups for C-reactive protein (CRP), erythrocyte sedimentation rate (ESR), swollen joint count (SJC), and Disease Activity Score encompassing 28 joints (DAS28). Anti-CII seropositive patients had higher CRP at 0-6 months, higher ESR at 0-3 months, a higher SJC at 0-6 months, and a higher DAS28 at 0-3 months.
“Anti-CCP2 [seropositivity] on the other hand was associated with higher disease activity later during the 5-year follow-up, and with CRP and ESR during the full period,” the investigators wrote.
The same respective phenotypic patterns occurred when the comparisons were limited to patients with anti-CII positivity alone or anti-CCP2 positivity alone, the investigators noted. However, “patients in the anti-CII and anti-CCP2 double-positive group mainly followed the anti-CII pattern, with early but not late increased values for CRP, ESR, DAS28, and DAS28CRP, but with a mixed pattern for SJC.”
In comparisons where baseline clinical and laboratory measures were associated with anti-CII or anti-CCP2 positivity, anti-CII was more often associated with favorable late changes in CRP, ESR, SJC, TJC, DAS28, DAS28CRP, Health Assessment Questionnaire, and pain and global measurements on a visual analog scale when compared with antibody double-negative patients. There were fewer changes in clinical and laboratory measures associated with anti-CCP2 positivity. These significant changes associated with anti-CII positivity were always larger improvements than were seen for antibody double-negative patients, whereas the significant changes observed with anti-CCP2 patients were always smaller improvements than those for antibody double-negative patients.
Moderate or good European League Against Rheumatism responses were significantly associated with anti-CII positivity at 12, 24, 36, and 60 months, whereas they were negatively associated with anti-CCP2 positivity at 36 and 60 months.
Overall, the findings of the study show that since “anti-CII-positive patients with RA have an acute onset, but favorable prognosis” and anti-CCP2 is associated with poor prognosis, “the combined analysis of anti-CII and ACPA/anti-CCP2 may be a new two-dimensional tool for predicting the prognosis and choosing therapy in newly diagnosed patients with RA,” the authors suggested.
The study was funded by grants from the Swedish Research Council, Swedish Rheumatism Association, King Gustav Vth 80-Year Foundation, and Uppsala County Council. Dr. Manivel and his coauthors reported no relevant financial disclosures.
Individuals with rheumatoid arthritis who have antifibrillar collagen type II antibodies appear to have a unique disease phenotype characterized by acute but transient inflammation around the time of diagnosis, as well as a favorable prognosis, according to findings from a retrospective cohort study.
The antifibrillar collagen type II (anti-CII) phenotype also differed from the phenotype of individuals with anti–cyclic citrullinated peptide 2 (anti-CCP2) antibodies who typically exhibit inflammatory markers and higher disease activity later in the disease course, reported Vivek Anand Manivel of Uppsala (Sweden) University and his colleagues (Ann Rheum Dis. 2017 Mar 23. doi: 10.1136/annrheumdis-2016-210873).
Overall, the investigators detected anti-CII positivity in 6.6% and anti-CCP2 in 57.9%, including only anti-CII antibodies in 2.6%, only anti-CCP2 in 54%, double positivity in 3.9%, and double negativity in 39.4%. A control group of 960 patients from the Swedish general population who were matched for age, locality, and sex were positive for anti-CII in 1.6% and anti-CCP2 in 1.7%.
Significant differences were discovered between anti-CII positive and negative groups for C-reactive protein (CRP), erythrocyte sedimentation rate (ESR), swollen joint count (SJC), and Disease Activity Score encompassing 28 joints (DAS28). Anti-CII seropositive patients had higher CRP at 0-6 months, higher ESR at 0-3 months, a higher SJC at 0-6 months, and a higher DAS28 at 0-3 months.
“Anti-CCP2 [seropositivity] on the other hand was associated with higher disease activity later during the 5-year follow-up, and with CRP and ESR during the full period,” the investigators wrote.
The same respective phenotypic patterns occurred when the comparisons were limited to patients with anti-CII positivity alone or anti-CCP2 positivity alone, the investigators noted. However, “patients in the anti-CII and anti-CCP2 double-positive group mainly followed the anti-CII pattern, with early but not late increased values for CRP, ESR, DAS28, and DAS28CRP, but with a mixed pattern for SJC.”
In comparisons where baseline clinical and laboratory measures were associated with anti-CII or anti-CCP2 positivity, anti-CII was more often associated with favorable late changes in CRP, ESR, SJC, TJC, DAS28, DAS28CRP, Health Assessment Questionnaire, and pain and global measurements on a visual analog scale when compared with antibody double-negative patients. There were fewer changes in clinical and laboratory measures associated with anti-CCP2 positivity. These significant changes associated with anti-CII positivity were always larger improvements than were seen for antibody double-negative patients, whereas the significant changes observed with anti-CCP2 patients were always smaller improvements than those for antibody double-negative patients.
Moderate or good European League Against Rheumatism responses were significantly associated with anti-CII positivity at 12, 24, 36, and 60 months, whereas they were negatively associated with anti-CCP2 positivity at 36 and 60 months.
Overall, the findings of the study show that since “anti-CII-positive patients with RA have an acute onset, but favorable prognosis” and anti-CCP2 is associated with poor prognosis, “the combined analysis of anti-CII and ACPA/anti-CCP2 may be a new two-dimensional tool for predicting the prognosis and choosing therapy in newly diagnosed patients with RA,” the authors suggested.
The study was funded by grants from the Swedish Research Council, Swedish Rheumatism Association, King Gustav Vth 80-Year Foundation, and Uppsala County Council. Dr. Manivel and his coauthors reported no relevant financial disclosures.
Individuals with rheumatoid arthritis who have antifibrillar collagen type II antibodies appear to have a unique disease phenotype characterized by acute but transient inflammation around the time of diagnosis, as well as a favorable prognosis, according to findings from a retrospective cohort study.
The antifibrillar collagen type II (anti-CII) phenotype also differed from the phenotype of individuals with anti–cyclic citrullinated peptide 2 (anti-CCP2) antibodies who typically exhibit inflammatory markers and higher disease activity later in the disease course, reported Vivek Anand Manivel of Uppsala (Sweden) University and his colleagues (Ann Rheum Dis. 2017 Mar 23. doi: 10.1136/annrheumdis-2016-210873).
Overall, the investigators detected anti-CII positivity in 6.6% and anti-CCP2 in 57.9%, including only anti-CII antibodies in 2.6%, only anti-CCP2 in 54%, double positivity in 3.9%, and double negativity in 39.4%. A control group of 960 patients from the Swedish general population who were matched for age, locality, and sex were positive for anti-CII in 1.6% and anti-CCP2 in 1.7%.
Significant differences were discovered between anti-CII positive and negative groups for C-reactive protein (CRP), erythrocyte sedimentation rate (ESR), swollen joint count (SJC), and Disease Activity Score encompassing 28 joints (DAS28). Anti-CII seropositive patients had higher CRP at 0-6 months, higher ESR at 0-3 months, a higher SJC at 0-6 months, and a higher DAS28 at 0-3 months.
“Anti-CCP2 [seropositivity] on the other hand was associated with higher disease activity later during the 5-year follow-up, and with CRP and ESR during the full period,” the investigators wrote.
The same respective phenotypic patterns occurred when the comparisons were limited to patients with anti-CII positivity alone or anti-CCP2 positivity alone, the investigators noted. However, “patients in the anti-CII and anti-CCP2 double-positive group mainly followed the anti-CII pattern, with early but not late increased values for CRP, ESR, DAS28, and DAS28CRP, but with a mixed pattern for SJC.”
In comparisons where baseline clinical and laboratory measures were associated with anti-CII or anti-CCP2 positivity, anti-CII was more often associated with favorable late changes in CRP, ESR, SJC, TJC, DAS28, DAS28CRP, Health Assessment Questionnaire, and pain and global measurements on a visual analog scale when compared with antibody double-negative patients. There were fewer changes in clinical and laboratory measures associated with anti-CCP2 positivity. These significant changes associated with anti-CII positivity were always larger improvements than were seen for antibody double-negative patients, whereas the significant changes observed with anti-CCP2 patients were always smaller improvements than those for antibody double-negative patients.
Moderate or good European League Against Rheumatism responses were significantly associated with anti-CII positivity at 12, 24, 36, and 60 months, whereas they were negatively associated with anti-CCP2 positivity at 36 and 60 months.
Overall, the findings of the study show that since “anti-CII-positive patients with RA have an acute onset, but favorable prognosis” and anti-CCP2 is associated with poor prognosis, “the combined analysis of anti-CII and ACPA/anti-CCP2 may be a new two-dimensional tool for predicting the prognosis and choosing therapy in newly diagnosed patients with RA,” the authors suggested.
The study was funded by grants from the Swedish Research Council, Swedish Rheumatism Association, King Gustav Vth 80-Year Foundation, and Uppsala County Council. Dr. Manivel and his coauthors reported no relevant financial disclosures.
FROM ANNALS OF THE RHEUMATIC DISEASES
Key clinical point:
Major finding: RA patients with anti-CII seropositivity had significantly higher C-reactive protein levels at 0-6 months, higher ESR at 0-3 months, a higher SJC at 0-6 months, and a higher DAS28 at 0-3 months than did anti-CII seronegative patients.
Data source: Retrospective cohort study of EIRA study patients and 960 controls.
Disclosures: Study funded by Swedish Research Council, Swedish Rheumatism Association, King Gustav Vth 80-Year Foundation, and Uppsala County Council. The authors reported no relevant financial disclosures.
VIDEO: Compassionate care, decriminalization crucial to mitigating addiction epidemic
SAN DIEGO – Health care providers need to practice compassionate care to achieve the best results when managing patients who are dealing with opioid addiction, according to a panel of experts who spoke at the annual meeting of the American College of Physicians.
Caring “compassionately is not enabling, [it’s] doing the right thing by the patient,” explained Chwen-Yuen Angie Chen, MD, of Stanford (Calif.) University. “You can practice compassionate care if you have a knowledge base. Knowledge is extremely powerful and enables you to follow evidence-based medicine, which is truly compassionate care.”
Dr. Chen spoke at length about addiction medicine during a press conference outlining the ACP’s new position paper on preventing and treating substance abuse, where she was joined by ACP President Nitin S. Damle, MD, and ACP Board of Regents Chair Thomas G. Tape, MD. All three emphasized the need for decriminalization and destigmatization of opioid abuse, and they called on physicians to guide patients through resources and compassionate care to help them overcome the affliction.
“We know that we need to either taper, detoxify, or reduce opioid dosing. We know that we ought not to coprescribe with sedatives. We know that, if you need addiction treatment, you get referred, and you don’t just get cut off,” explained Dr. Chen.
In a video interview, Dr. Chen talked about the key take-home messages of the position paper, and she explained other aspects of substance abuse that requires provider’s awareness.
Dr. Chen did not report any relevant financial disclosures.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
SAN DIEGO – Health care providers need to practice compassionate care to achieve the best results when managing patients who are dealing with opioid addiction, according to a panel of experts who spoke at the annual meeting of the American College of Physicians.
Caring “compassionately is not enabling, [it’s] doing the right thing by the patient,” explained Chwen-Yuen Angie Chen, MD, of Stanford (Calif.) University. “You can practice compassionate care if you have a knowledge base. Knowledge is extremely powerful and enables you to follow evidence-based medicine, which is truly compassionate care.”
Dr. Chen spoke at length about addiction medicine during a press conference outlining the ACP’s new position paper on preventing and treating substance abuse, where she was joined by ACP President Nitin S. Damle, MD, and ACP Board of Regents Chair Thomas G. Tape, MD. All three emphasized the need for decriminalization and destigmatization of opioid abuse, and they called on physicians to guide patients through resources and compassionate care to help them overcome the affliction.
“We know that we need to either taper, detoxify, or reduce opioid dosing. We know that we ought not to coprescribe with sedatives. We know that, if you need addiction treatment, you get referred, and you don’t just get cut off,” explained Dr. Chen.
In a video interview, Dr. Chen talked about the key take-home messages of the position paper, and she explained other aspects of substance abuse that requires provider’s awareness.
Dr. Chen did not report any relevant financial disclosures.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
SAN DIEGO – Health care providers need to practice compassionate care to achieve the best results when managing patients who are dealing with opioid addiction, according to a panel of experts who spoke at the annual meeting of the American College of Physicians.
Caring “compassionately is not enabling, [it’s] doing the right thing by the patient,” explained Chwen-Yuen Angie Chen, MD, of Stanford (Calif.) University. “You can practice compassionate care if you have a knowledge base. Knowledge is extremely powerful and enables you to follow evidence-based medicine, which is truly compassionate care.”
Dr. Chen spoke at length about addiction medicine during a press conference outlining the ACP’s new position paper on preventing and treating substance abuse, where she was joined by ACP President Nitin S. Damle, MD, and ACP Board of Regents Chair Thomas G. Tape, MD. All three emphasized the need for decriminalization and destigmatization of opioid abuse, and they called on physicians to guide patients through resources and compassionate care to help them overcome the affliction.
“We know that we need to either taper, detoxify, or reduce opioid dosing. We know that we ought not to coprescribe with sedatives. We know that, if you need addiction treatment, you get referred, and you don’t just get cut off,” explained Dr. Chen.
In a video interview, Dr. Chen talked about the key take-home messages of the position paper, and she explained other aspects of substance abuse that requires provider’s awareness.
Dr. Chen did not report any relevant financial disclosures.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT ACP INTERNAL MEDICINE
New guidance: Bone health is front and center in functional hypothalamic amenorrhea care
Evaluate bone health no longer than 6 months after onset of functional hypothalamic amenorrhea (FHA), according to new guidance on its diagnosis and management.
The preferred measure of bone mineral density (BMD) is dual-energy x-ray absorptiometry (DXA), guidance lead author Catherine M. Gordon, MD, of Cincinnati Children’s Hospital Medical Center noted in an interview.
“Our group has tried to raise awareness with our guideline about bone health,” said Dr. Gordon. “Bone is unfortunately detrimentally affected in adolescents and adult women with FHA, [so] our guideline now formally recommends bone density screening after 6 months of amenorrhea.”
Among the available therapies to preserve or restore bone density is short-term use of transdermal E2 therapy, with cyclic oral progestin, only after conventional intervention with nurtritional and exercise modification has been attempted for a “reasonable” amount of time but menstrual cycles have not yet been reestablished. Bisphosphonates, denosumab, testosterone, and leptin also can be used to improve bone mineral density (BMD), with recombinant parathyroid hormone 1-34 (rPTH) recommended in rare cases of extremely low BMD.
“Patients should not use oral contraceptives as a way to induce menstruation or improve BMD,” she said.
“We anticipate that some clinicians will be surprised to see that combined oral contraceptive pills do not provide bone protection for patients with FHA,” Dr. Gordon explained. “Our guideline reviews data on this point, which led to our recommendation that short-term transdermal estrogen may be helpful in restoring menses for select patients with longstanding amenorrhea despite efforts to correct their ‘energy deficit.’ ”
Clinicians also should be aware that FHA can mask the signs and symptoms of polycystic ovary syndrome in some young women. It’s therefore important for providers to understand that a patient could carry both diagnoses: Such patients should have a baseline BMD measurement taken, along with “clinical monitoring for hyper-response in those treated with exogenous gonadotropins for infertility,” according to the guidelines.
In general, “FHA is a ‘diagnosis of exclusion,’ meaning that underlying anatomic or organic pathologies must first be ruled out. It is important to consider other etiologies first before the amenorrhea is attributed to inadequate intake, overexercise, or stress,” Dr. Gordon said.
According to the guidelines, patients should only undergo evaluation for FHA if menstrual cycle interval exceeds 45 days on a consistent basis, or if they present with amenorrhea for at least 3 months. Patients with suspected FHA should be screened for psychological stressors that could be inducing anovulation.
When trying to make a diagnosis of FHA, providers should be “obtaining a detailed personal history with a focus on diet; eating disorders; exercise and athletic training; attitudes, such as perfectionism and high need for social approval; ambitions and expectations for self and others; weight fluctuations; sleep patterns; stressors; mood; menstrual pattern; fractures; and substance abuse,” the guidelines state.
Family histories also should be evaluated, and patients should undergo a full physical. Once a diagnosis of FHA is made, however, clinicians should help educate patients about different menstrual cycles while letting women know that an irregular cycle does not necessarily prevent them from conceiving.
The most important aspect of managing FHA is to take a multidiscipinary approach, according to Dr. Gordon and her colleagues (J Clin Endocrinol Metab. May 2017;102[5]:1-27).
“We emphasize that the mainstay of therapy for these adolescents and women is close attention to nutrition, exercise, and alleviating stressors through psychological support, best achieved through a multidisciplinary team,” Dr. Gordon stated.
Any patient diagnosed with FHA who also develops severe bradycardia, hypotension, orthostasis, or electrolyte imbalance should be treated as an inpatient. Energy imbalances can affect the hypothalamic-pituitary-ovarian (HPO) axis function, so correcting that should be considered a priority.
Adolescents and women for whom pregnancy has been excluded are recommended to undergo a progestin challenge, which should indicate chronic estrogen exposure via induced withdrawal bleeding. A brain MRI also can be conducted if the patient complains about chronic headaches, vomiting, or problems with vision or thirst.
FHA patients who wish to conceive have a number of options outlined by the guidelines. Pulsatile gonadotropin-releasing hormone (GnRH) should be the first treatment, followed by gonadotropin therapy, which must be administered as carefully as possible. Clomiphene citrate also can be used in certain situations, and cognitive behavior therapy is also a viable option, although the guidelines note that only one relatively small study offered any evidence of its efficacy. Kisspeptin and leptin should not be used as a treatment for infertility under any circumstances.
These guidelines were created in conjunction with the American Society for Reproductive Medicine, the European Society of Endocrinology, and the Pediatric Endocrine Society. An evidence-based approach was undertaken by a panel of eight experts, a methodologist, and a medical writer.
“There is currently a lack of consistency in clinical practice regarding the evaluation for patients with FHA,” said Dr. Gordon. “Our guideline attempts to clarify for clinicians what the appropriate general, endocrine, and imaging work-up would entail.”
The creation of these guidelines was funded by the Endocrine Society.
Evaluate bone health no longer than 6 months after onset of functional hypothalamic amenorrhea (FHA), according to new guidance on its diagnosis and management.
The preferred measure of bone mineral density (BMD) is dual-energy x-ray absorptiometry (DXA), guidance lead author Catherine M. Gordon, MD, of Cincinnati Children’s Hospital Medical Center noted in an interview.
“Our group has tried to raise awareness with our guideline about bone health,” said Dr. Gordon. “Bone is unfortunately detrimentally affected in adolescents and adult women with FHA, [so] our guideline now formally recommends bone density screening after 6 months of amenorrhea.”
Among the available therapies to preserve or restore bone density is short-term use of transdermal E2 therapy, with cyclic oral progestin, only after conventional intervention with nurtritional and exercise modification has been attempted for a “reasonable” amount of time but menstrual cycles have not yet been reestablished. Bisphosphonates, denosumab, testosterone, and leptin also can be used to improve bone mineral density (BMD), with recombinant parathyroid hormone 1-34 (rPTH) recommended in rare cases of extremely low BMD.
“Patients should not use oral contraceptives as a way to induce menstruation or improve BMD,” she said.
“We anticipate that some clinicians will be surprised to see that combined oral contraceptive pills do not provide bone protection for patients with FHA,” Dr. Gordon explained. “Our guideline reviews data on this point, which led to our recommendation that short-term transdermal estrogen may be helpful in restoring menses for select patients with longstanding amenorrhea despite efforts to correct their ‘energy deficit.’ ”
Clinicians also should be aware that FHA can mask the signs and symptoms of polycystic ovary syndrome in some young women. It’s therefore important for providers to understand that a patient could carry both diagnoses: Such patients should have a baseline BMD measurement taken, along with “clinical monitoring for hyper-response in those treated with exogenous gonadotropins for infertility,” according to the guidelines.
In general, “FHA is a ‘diagnosis of exclusion,’ meaning that underlying anatomic or organic pathologies must first be ruled out. It is important to consider other etiologies first before the amenorrhea is attributed to inadequate intake, overexercise, or stress,” Dr. Gordon said.
According to the guidelines, patients should only undergo evaluation for FHA if menstrual cycle interval exceeds 45 days on a consistent basis, or if they present with amenorrhea for at least 3 months. Patients with suspected FHA should be screened for psychological stressors that could be inducing anovulation.
When trying to make a diagnosis of FHA, providers should be “obtaining a detailed personal history with a focus on diet; eating disorders; exercise and athletic training; attitudes, such as perfectionism and high need for social approval; ambitions and expectations for self and others; weight fluctuations; sleep patterns; stressors; mood; menstrual pattern; fractures; and substance abuse,” the guidelines state.
Family histories also should be evaluated, and patients should undergo a full physical. Once a diagnosis of FHA is made, however, clinicians should help educate patients about different menstrual cycles while letting women know that an irregular cycle does not necessarily prevent them from conceiving.
The most important aspect of managing FHA is to take a multidiscipinary approach, according to Dr. Gordon and her colleagues (J Clin Endocrinol Metab. May 2017;102[5]:1-27).
“We emphasize that the mainstay of therapy for these adolescents and women is close attention to nutrition, exercise, and alleviating stressors through psychological support, best achieved through a multidisciplinary team,” Dr. Gordon stated.
Any patient diagnosed with FHA who also develops severe bradycardia, hypotension, orthostasis, or electrolyte imbalance should be treated as an inpatient. Energy imbalances can affect the hypothalamic-pituitary-ovarian (HPO) axis function, so correcting that should be considered a priority.
Adolescents and women for whom pregnancy has been excluded are recommended to undergo a progestin challenge, which should indicate chronic estrogen exposure via induced withdrawal bleeding. A brain MRI also can be conducted if the patient complains about chronic headaches, vomiting, or problems with vision or thirst.
FHA patients who wish to conceive have a number of options outlined by the guidelines. Pulsatile gonadotropin-releasing hormone (GnRH) should be the first treatment, followed by gonadotropin therapy, which must be administered as carefully as possible. Clomiphene citrate also can be used in certain situations, and cognitive behavior therapy is also a viable option, although the guidelines note that only one relatively small study offered any evidence of its efficacy. Kisspeptin and leptin should not be used as a treatment for infertility under any circumstances.
These guidelines were created in conjunction with the American Society for Reproductive Medicine, the European Society of Endocrinology, and the Pediatric Endocrine Society. An evidence-based approach was undertaken by a panel of eight experts, a methodologist, and a medical writer.
“There is currently a lack of consistency in clinical practice regarding the evaluation for patients with FHA,” said Dr. Gordon. “Our guideline attempts to clarify for clinicians what the appropriate general, endocrine, and imaging work-up would entail.”
The creation of these guidelines was funded by the Endocrine Society.
Evaluate bone health no longer than 6 months after onset of functional hypothalamic amenorrhea (FHA), according to new guidance on its diagnosis and management.
The preferred measure of bone mineral density (BMD) is dual-energy x-ray absorptiometry (DXA), guidance lead author Catherine M. Gordon, MD, of Cincinnati Children’s Hospital Medical Center noted in an interview.
“Our group has tried to raise awareness with our guideline about bone health,” said Dr. Gordon. “Bone is unfortunately detrimentally affected in adolescents and adult women with FHA, [so] our guideline now formally recommends bone density screening after 6 months of amenorrhea.”
Among the available therapies to preserve or restore bone density is short-term use of transdermal E2 therapy, with cyclic oral progestin, only after conventional intervention with nurtritional and exercise modification has been attempted for a “reasonable” amount of time but menstrual cycles have not yet been reestablished. Bisphosphonates, denosumab, testosterone, and leptin also can be used to improve bone mineral density (BMD), with recombinant parathyroid hormone 1-34 (rPTH) recommended in rare cases of extremely low BMD.
“Patients should not use oral contraceptives as a way to induce menstruation or improve BMD,” she said.
“We anticipate that some clinicians will be surprised to see that combined oral contraceptive pills do not provide bone protection for patients with FHA,” Dr. Gordon explained. “Our guideline reviews data on this point, which led to our recommendation that short-term transdermal estrogen may be helpful in restoring menses for select patients with longstanding amenorrhea despite efforts to correct their ‘energy deficit.’ ”
Clinicians also should be aware that FHA can mask the signs and symptoms of polycystic ovary syndrome in some young women. It’s therefore important for providers to understand that a patient could carry both diagnoses: Such patients should have a baseline BMD measurement taken, along with “clinical monitoring for hyper-response in those treated with exogenous gonadotropins for infertility,” according to the guidelines.
In general, “FHA is a ‘diagnosis of exclusion,’ meaning that underlying anatomic or organic pathologies must first be ruled out. It is important to consider other etiologies first before the amenorrhea is attributed to inadequate intake, overexercise, or stress,” Dr. Gordon said.
According to the guidelines, patients should only undergo evaluation for FHA if menstrual cycle interval exceeds 45 days on a consistent basis, or if they present with amenorrhea for at least 3 months. Patients with suspected FHA should be screened for psychological stressors that could be inducing anovulation.
When trying to make a diagnosis of FHA, providers should be “obtaining a detailed personal history with a focus on diet; eating disorders; exercise and athletic training; attitudes, such as perfectionism and high need for social approval; ambitions and expectations for self and others; weight fluctuations; sleep patterns; stressors; mood; menstrual pattern; fractures; and substance abuse,” the guidelines state.
Family histories also should be evaluated, and patients should undergo a full physical. Once a diagnosis of FHA is made, however, clinicians should help educate patients about different menstrual cycles while letting women know that an irregular cycle does not necessarily prevent them from conceiving.
The most important aspect of managing FHA is to take a multidiscipinary approach, according to Dr. Gordon and her colleagues (J Clin Endocrinol Metab. May 2017;102[5]:1-27).
“We emphasize that the mainstay of therapy for these adolescents and women is close attention to nutrition, exercise, and alleviating stressors through psychological support, best achieved through a multidisciplinary team,” Dr. Gordon stated.
Any patient diagnosed with FHA who also develops severe bradycardia, hypotension, orthostasis, or electrolyte imbalance should be treated as an inpatient. Energy imbalances can affect the hypothalamic-pituitary-ovarian (HPO) axis function, so correcting that should be considered a priority.
Adolescents and women for whom pregnancy has been excluded are recommended to undergo a progestin challenge, which should indicate chronic estrogen exposure via induced withdrawal bleeding. A brain MRI also can be conducted if the patient complains about chronic headaches, vomiting, or problems with vision or thirst.
FHA patients who wish to conceive have a number of options outlined by the guidelines. Pulsatile gonadotropin-releasing hormone (GnRH) should be the first treatment, followed by gonadotropin therapy, which must be administered as carefully as possible. Clomiphene citrate also can be used in certain situations, and cognitive behavior therapy is also a viable option, although the guidelines note that only one relatively small study offered any evidence of its efficacy. Kisspeptin and leptin should not be used as a treatment for infertility under any circumstances.
These guidelines were created in conjunction with the American Society for Reproductive Medicine, the European Society of Endocrinology, and the Pediatric Endocrine Society. An evidence-based approach was undertaken by a panel of eight experts, a methodologist, and a medical writer.
“There is currently a lack of consistency in clinical practice regarding the evaluation for patients with FHA,” said Dr. Gordon. “Our guideline attempts to clarify for clinicians what the appropriate general, endocrine, and imaging work-up would entail.”
The creation of these guidelines was funded by the Endocrine Society.
FROM THE JOURNAL OF CLINICAL ENDOCRINOLOGY AND METABOLISM
Preoperative opioid use linked to worse outcomes following abdominal surgery
Surgeons need to do more to identify patients who are taking opioids preoperatively, because this is a population that appears to be at a higher risk of worse surgical outcomes, according to a large retrospective investigation.
“Opioid users represent a potentially high-risk surgical population and may require tailored perioperative care [and] the prevalence and clinical impact of this problem in the general surgery population remain unclear,” wrote the authors of a study, led by David C. Cron, a medical student of the University of Michigan, Ann Arbor. “Given the impact of pain control and gastrointestinal function on hospital stay, it is intuitive that opioid users may have increased hospital length of stay (LOS) and may incur more costs [and] also be at higher risk for surgical complications.”
The study was published in the Annals of Surgery (2017;465[4]696-701).
Mr. Cron and his coauthors made a study cohort retrospectively from abdominopelvic surgery patients from the Michigan Surgical Quality Collaborative (MSQC) database who had surgery between 2008 and 2014. All patients were treated at the University of Michigan, and were admitted within 2 days of undergoing their operation. Any patient with data indicating use of buprenorphine prior to surgery, or those were who opioid naive before admission but received opioids after being admitted, were excluded.
Investigators found a total of 3,107 patients in the MSQC database that underwent abdominopelvic surgery at the University of Michigan during the designated time frame; from that group, 2,413 were ultimately found to match the inclusion criteria for the study. The primary outcomes were 90-day total hospital costs, along with patient LOS, and 30-day rates of complications and readmissions. Data underwent covariate risk adjustment to account for age, race, gender, body mass index, insurance class, and other factors.
“Major complications are recorded by the MSQC and include: surgical site infection, deep venous thrombosis, acute renal failure, postoperative bleeding requiring transfusion, stroke, unplanned intubation, fascial dehiscence, prolonged mechanical ventilation longer than 48 hours, myocardial infarction, pneumonia, pulmonary embolism, sepsis, vascular graft loss, and renal insufficiency,” the authors noted.
Of the 2,413 subjects overall, 502 (20.8%) were found to use opioids before surgery. Differences between opioid users and nonusers were not significant in terms of age (P = .10), gender (P = .76), and race (P = .78). After adjustment, data indicated that preoperative opioid users had 9.2% higher hospital costs than nonusers (95% confidence interval, 2.8%-15.6%, P = .005) and 12.4% longer hospital stay (95% CI, 2.3%-23.5%; P = .015). Complications and readmission rates were quantified by odds ratios, which were also found to be significantly higher in subjects who were preoperative opioid users: OR = 1.36 (95% CI, 1.04-1.78; P = .023) and OR = 1.57 (95% CI, 1.08-2.29; P = .018), respectively.
The study had some limitations, including being conducted at a single center and potentially not generalizable to other types of health care facilities and population types. Additionally, information on opioid dosage and duration of use was lacking, making it that “possible that some opioid users in our study were using opioids over a shorter time period for pain related to their surgical disease,” according to the investigators.
“These results argue the potential cost-effectiveness of intervention in this unique patient population,” Mr. Cron and his colleagues concluded. “Opioid use is a potentially modifiable risk factor, and major surgery can provide powerful leverage to improve health behavior [and] our institution has implemented a preoperative program to optimize high-risk patients for surgery.”
Mr. Cron received funding from the 2015 AOA Carolyn L. Kuckein Student Research Fellowship and the Blue Cross Blue Shield of Michigan Foundation Student Research Award for this study. He and his coauthors reported no relevant financial disclosures.
The opioid epidemic is probably the biggest health care problem in the United States, and it’s getting worse. Opioids are absolutely affecting surgical outcomes on a large scale. Unfortunately, there’s no great solution in terms of how to better manage these patients – in a perfect world, we’d take the time to wean them off opioids before operating, but that isn’t very pragmatic. With such a large and expanding proportion of our patients presenting to the operating room on long-term opioids, we have developed a new cohort of high-risk surgical patients over the past several years.
Michael J. Englesbe, MD , is a professor of surgery at the University of Michigan, Ann Arbor, and a coauthor on this study.
The opioid epidemic is probably the biggest health care problem in the United States, and it’s getting worse. Opioids are absolutely affecting surgical outcomes on a large scale. Unfortunately, there’s no great solution in terms of how to better manage these patients – in a perfect world, we’d take the time to wean them off opioids before operating, but that isn’t very pragmatic. With such a large and expanding proportion of our patients presenting to the operating room on long-term opioids, we have developed a new cohort of high-risk surgical patients over the past several years.
Michael J. Englesbe, MD , is a professor of surgery at the University of Michigan, Ann Arbor, and a coauthor on this study.
The opioid epidemic is probably the biggest health care problem in the United States, and it’s getting worse. Opioids are absolutely affecting surgical outcomes on a large scale. Unfortunately, there’s no great solution in terms of how to better manage these patients – in a perfect world, we’d take the time to wean them off opioids before operating, but that isn’t very pragmatic. With such a large and expanding proportion of our patients presenting to the operating room on long-term opioids, we have developed a new cohort of high-risk surgical patients over the past several years.
Michael J. Englesbe, MD , is a professor of surgery at the University of Michigan, Ann Arbor, and a coauthor on this study.
Surgeons need to do more to identify patients who are taking opioids preoperatively, because this is a population that appears to be at a higher risk of worse surgical outcomes, according to a large retrospective investigation.
“Opioid users represent a potentially high-risk surgical population and may require tailored perioperative care [and] the prevalence and clinical impact of this problem in the general surgery population remain unclear,” wrote the authors of a study, led by David C. Cron, a medical student of the University of Michigan, Ann Arbor. “Given the impact of pain control and gastrointestinal function on hospital stay, it is intuitive that opioid users may have increased hospital length of stay (LOS) and may incur more costs [and] also be at higher risk for surgical complications.”
The study was published in the Annals of Surgery (2017;465[4]696-701).
Mr. Cron and his coauthors made a study cohort retrospectively from abdominopelvic surgery patients from the Michigan Surgical Quality Collaborative (MSQC) database who had surgery between 2008 and 2014. All patients were treated at the University of Michigan, and were admitted within 2 days of undergoing their operation. Any patient with data indicating use of buprenorphine prior to surgery, or those were who opioid naive before admission but received opioids after being admitted, were excluded.
Investigators found a total of 3,107 patients in the MSQC database that underwent abdominopelvic surgery at the University of Michigan during the designated time frame; from that group, 2,413 were ultimately found to match the inclusion criteria for the study. The primary outcomes were 90-day total hospital costs, along with patient LOS, and 30-day rates of complications and readmissions. Data underwent covariate risk adjustment to account for age, race, gender, body mass index, insurance class, and other factors.
“Major complications are recorded by the MSQC and include: surgical site infection, deep venous thrombosis, acute renal failure, postoperative bleeding requiring transfusion, stroke, unplanned intubation, fascial dehiscence, prolonged mechanical ventilation longer than 48 hours, myocardial infarction, pneumonia, pulmonary embolism, sepsis, vascular graft loss, and renal insufficiency,” the authors noted.
Of the 2,413 subjects overall, 502 (20.8%) were found to use opioids before surgery. Differences between opioid users and nonusers were not significant in terms of age (P = .10), gender (P = .76), and race (P = .78). After adjustment, data indicated that preoperative opioid users had 9.2% higher hospital costs than nonusers (95% confidence interval, 2.8%-15.6%, P = .005) and 12.4% longer hospital stay (95% CI, 2.3%-23.5%; P = .015). Complications and readmission rates were quantified by odds ratios, which were also found to be significantly higher in subjects who were preoperative opioid users: OR = 1.36 (95% CI, 1.04-1.78; P = .023) and OR = 1.57 (95% CI, 1.08-2.29; P = .018), respectively.
The study had some limitations, including being conducted at a single center and potentially not generalizable to other types of health care facilities and population types. Additionally, information on opioid dosage and duration of use was lacking, making it that “possible that some opioid users in our study were using opioids over a shorter time period for pain related to their surgical disease,” according to the investigators.
“These results argue the potential cost-effectiveness of intervention in this unique patient population,” Mr. Cron and his colleagues concluded. “Opioid use is a potentially modifiable risk factor, and major surgery can provide powerful leverage to improve health behavior [and] our institution has implemented a preoperative program to optimize high-risk patients for surgery.”
Mr. Cron received funding from the 2015 AOA Carolyn L. Kuckein Student Research Fellowship and the Blue Cross Blue Shield of Michigan Foundation Student Research Award for this study. He and his coauthors reported no relevant financial disclosures.
Surgeons need to do more to identify patients who are taking opioids preoperatively, because this is a population that appears to be at a higher risk of worse surgical outcomes, according to a large retrospective investigation.
“Opioid users represent a potentially high-risk surgical population and may require tailored perioperative care [and] the prevalence and clinical impact of this problem in the general surgery population remain unclear,” wrote the authors of a study, led by David C. Cron, a medical student of the University of Michigan, Ann Arbor. “Given the impact of pain control and gastrointestinal function on hospital stay, it is intuitive that opioid users may have increased hospital length of stay (LOS) and may incur more costs [and] also be at higher risk for surgical complications.”
The study was published in the Annals of Surgery (2017;465[4]696-701).
Mr. Cron and his coauthors made a study cohort retrospectively from abdominopelvic surgery patients from the Michigan Surgical Quality Collaborative (MSQC) database who had surgery between 2008 and 2014. All patients were treated at the University of Michigan, and were admitted within 2 days of undergoing their operation. Any patient with data indicating use of buprenorphine prior to surgery, or those were who opioid naive before admission but received opioids after being admitted, were excluded.
Investigators found a total of 3,107 patients in the MSQC database that underwent abdominopelvic surgery at the University of Michigan during the designated time frame; from that group, 2,413 were ultimately found to match the inclusion criteria for the study. The primary outcomes were 90-day total hospital costs, along with patient LOS, and 30-day rates of complications and readmissions. Data underwent covariate risk adjustment to account for age, race, gender, body mass index, insurance class, and other factors.
“Major complications are recorded by the MSQC and include: surgical site infection, deep venous thrombosis, acute renal failure, postoperative bleeding requiring transfusion, stroke, unplanned intubation, fascial dehiscence, prolonged mechanical ventilation longer than 48 hours, myocardial infarction, pneumonia, pulmonary embolism, sepsis, vascular graft loss, and renal insufficiency,” the authors noted.
Of the 2,413 subjects overall, 502 (20.8%) were found to use opioids before surgery. Differences between opioid users and nonusers were not significant in terms of age (P = .10), gender (P = .76), and race (P = .78). After adjustment, data indicated that preoperative opioid users had 9.2% higher hospital costs than nonusers (95% confidence interval, 2.8%-15.6%, P = .005) and 12.4% longer hospital stay (95% CI, 2.3%-23.5%; P = .015). Complications and readmission rates were quantified by odds ratios, which were also found to be significantly higher in subjects who were preoperative opioid users: OR = 1.36 (95% CI, 1.04-1.78; P = .023) and OR = 1.57 (95% CI, 1.08-2.29; P = .018), respectively.
The study had some limitations, including being conducted at a single center and potentially not generalizable to other types of health care facilities and population types. Additionally, information on opioid dosage and duration of use was lacking, making it that “possible that some opioid users in our study were using opioids over a shorter time period for pain related to their surgical disease,” according to the investigators.
“These results argue the potential cost-effectiveness of intervention in this unique patient population,” Mr. Cron and his colleagues concluded. “Opioid use is a potentially modifiable risk factor, and major surgery can provide powerful leverage to improve health behavior [and] our institution has implemented a preoperative program to optimize high-risk patients for surgery.”
Mr. Cron received funding from the 2015 AOA Carolyn L. Kuckein Student Research Fellowship and the Blue Cross Blue Shield of Michigan Foundation Student Research Award for this study. He and his coauthors reported no relevant financial disclosures.
FROM THE ANNALS OF SURGERY
Key clinical point:
Major finding: Preoperative opioid users had 9.2% higher costs and 12.4% longer LOS, with higher ORs for complications and readmissions, than patients who did not take opioids.
Data source: Retrospective analysis of data on 2,413 abdominopelvic surgery patients during 2008-2014.
Disclosures: Study funded by grants awarded to Mr. Cron from the 2015 AOA Carolyn L. Kuckein Student Research Fellowship and the Blue Cross Blue Shield of Michigan Foundation Student Research Award. Authors reported no relevant financial disclosures.
American Samoa could be a model for responding to Zika outbreaks
Syndromic and enhanced surveillance employed during a Zika outbreak in American Samoa last year is credited for bringing a quick end to ongoing transmission and could be used to predict when ongoing transmission in similarly small populations will end.
“Establishing a timeline for discontinuing screening of asymptomatic pregnant women allows ASDoH [the American Samoa Department of Health] to allocate resources appropriately toward early interventions for children and families affected by Zika virus,” W. Thane Hancock, MD, of the CDC’s Office of Public Health Preparedness and Response, and his colleagues wrote in the Morbidity and Mortality Weekly Report (2017 Mar 24;66[11]:299-301).
Laboratory-confirmed Zika cases first cropped up in American Samoa in January 2016, prompting the implementation of protocols to reduce the mosquito population, along with syndromic surveillance based on electronic health records to determine which patients may be at higher risk. Routine testing of all asymptomatic pregnant woman, along with individuals with one or more symptoms of Zika virus, also became standard procedure. Real-time, reverse transcription–polymerase chain reaction (rRT-PCR) testing was used to confirm suspected Zika virus cases.
“Early in the response, collection and testing of specimens from pregnant women was prioritized over the collection from symptomatic nonpregnant patients because of limited testing and shipping capacity,” the researchers wrote.
By May 2016, suspected cases had dropped from six per week during January and February, to just one per week, with the last laboratory-confirmed case occurring on June 19, 2016. In August, the ASDoH proposed ending routine screening of asymptomatic pregnant women by Oct. 15, 2016. Transmission data from American Samoa and the CDC were used to determine the Oct. 15 date as an estimate for when active mosquito-borne transmission would end.
To confirm that local transmission was no longer ongoing, enhanced surveillance was implemented from Aug. 31 to Oct. 15, involving free testing at local clinics. Over the course of 45 days, there were a total of 32 patients suspected of having a Zika virus infection.
Two of these subjects’ specimens were not sufficient in sample size to be tested, but the other 30 underwent rRT-PCR testing within 30 days of symptom onset, and all the results were negative. Additionally, 277 asymptomatic pregnant women were tested and 86 (31%) tested anti-Zika IgM–positive or equivocal. All 86 specimens later tested negative by rRT-PCR.
Given the possibility that Zika virus can persist in semen for 6 months, officials recommended permissive testing of asymptomatic pregnant women who conceive through April 15, 2017 “as a conservative approach.”
“The surveillance processes outlined and the timeline established for American Samoa might have implications for jurisdictions where small populations and similar population immunity following widespread Zika virus exposure can facilitate interruption of transmission,” the researchers wrote.
Syndromic and enhanced surveillance employed during a Zika outbreak in American Samoa last year is credited for bringing a quick end to ongoing transmission and could be used to predict when ongoing transmission in similarly small populations will end.
“Establishing a timeline for discontinuing screening of asymptomatic pregnant women allows ASDoH [the American Samoa Department of Health] to allocate resources appropriately toward early interventions for children and families affected by Zika virus,” W. Thane Hancock, MD, of the CDC’s Office of Public Health Preparedness and Response, and his colleagues wrote in the Morbidity and Mortality Weekly Report (2017 Mar 24;66[11]:299-301).
Laboratory-confirmed Zika cases first cropped up in American Samoa in January 2016, prompting the implementation of protocols to reduce the mosquito population, along with syndromic surveillance based on electronic health records to determine which patients may be at higher risk. Routine testing of all asymptomatic pregnant woman, along with individuals with one or more symptoms of Zika virus, also became standard procedure. Real-time, reverse transcription–polymerase chain reaction (rRT-PCR) testing was used to confirm suspected Zika virus cases.
“Early in the response, collection and testing of specimens from pregnant women was prioritized over the collection from symptomatic nonpregnant patients because of limited testing and shipping capacity,” the researchers wrote.
By May 2016, suspected cases had dropped from six per week during January and February, to just one per week, with the last laboratory-confirmed case occurring on June 19, 2016. In August, the ASDoH proposed ending routine screening of asymptomatic pregnant women by Oct. 15, 2016. Transmission data from American Samoa and the CDC were used to determine the Oct. 15 date as an estimate for when active mosquito-borne transmission would end.
To confirm that local transmission was no longer ongoing, enhanced surveillance was implemented from Aug. 31 to Oct. 15, involving free testing at local clinics. Over the course of 45 days, there were a total of 32 patients suspected of having a Zika virus infection.
Two of these subjects’ specimens were not sufficient in sample size to be tested, but the other 30 underwent rRT-PCR testing within 30 days of symptom onset, and all the results were negative. Additionally, 277 asymptomatic pregnant women were tested and 86 (31%) tested anti-Zika IgM–positive or equivocal. All 86 specimens later tested negative by rRT-PCR.
Given the possibility that Zika virus can persist in semen for 6 months, officials recommended permissive testing of asymptomatic pregnant women who conceive through April 15, 2017 “as a conservative approach.”
“The surveillance processes outlined and the timeline established for American Samoa might have implications for jurisdictions where small populations and similar population immunity following widespread Zika virus exposure can facilitate interruption of transmission,” the researchers wrote.
Syndromic and enhanced surveillance employed during a Zika outbreak in American Samoa last year is credited for bringing a quick end to ongoing transmission and could be used to predict when ongoing transmission in similarly small populations will end.
“Establishing a timeline for discontinuing screening of asymptomatic pregnant women allows ASDoH [the American Samoa Department of Health] to allocate resources appropriately toward early interventions for children and families affected by Zika virus,” W. Thane Hancock, MD, of the CDC’s Office of Public Health Preparedness and Response, and his colleagues wrote in the Morbidity and Mortality Weekly Report (2017 Mar 24;66[11]:299-301).
Laboratory-confirmed Zika cases first cropped up in American Samoa in January 2016, prompting the implementation of protocols to reduce the mosquito population, along with syndromic surveillance based on electronic health records to determine which patients may be at higher risk. Routine testing of all asymptomatic pregnant woman, along with individuals with one or more symptoms of Zika virus, also became standard procedure. Real-time, reverse transcription–polymerase chain reaction (rRT-PCR) testing was used to confirm suspected Zika virus cases.
“Early in the response, collection and testing of specimens from pregnant women was prioritized over the collection from symptomatic nonpregnant patients because of limited testing and shipping capacity,” the researchers wrote.
By May 2016, suspected cases had dropped from six per week during January and February, to just one per week, with the last laboratory-confirmed case occurring on June 19, 2016. In August, the ASDoH proposed ending routine screening of asymptomatic pregnant women by Oct. 15, 2016. Transmission data from American Samoa and the CDC were used to determine the Oct. 15 date as an estimate for when active mosquito-borne transmission would end.
To confirm that local transmission was no longer ongoing, enhanced surveillance was implemented from Aug. 31 to Oct. 15, involving free testing at local clinics. Over the course of 45 days, there were a total of 32 patients suspected of having a Zika virus infection.
Two of these subjects’ specimens were not sufficient in sample size to be tested, but the other 30 underwent rRT-PCR testing within 30 days of symptom onset, and all the results were negative. Additionally, 277 asymptomatic pregnant women were tested and 86 (31%) tested anti-Zika IgM–positive or equivocal. All 86 specimens later tested negative by rRT-PCR.
Given the possibility that Zika virus can persist in semen for 6 months, officials recommended permissive testing of asymptomatic pregnant women who conceive through April 15, 2017 “as a conservative approach.”
“The surveillance processes outlined and the timeline established for American Samoa might have implications for jurisdictions where small populations and similar population immunity following widespread Zika virus exposure can facilitate interruption of transmission,” the researchers wrote.
FROM MMWR
Levosimendan does not improve 30-day mortality following cardiac surgery
Adding a low dose of levosimendan to the standard care for patients on perioperative hemodynamic support does not improve outcomes to any significant extent, according to the findings of a new study presented at the annual congress of the European Society of Intensive Care Medicine and published simultaneously online in the New England Journal of Medicine.
“Levosimendan (Simdax, Orion) is an inotropic agent that has been shown to be associated with a higher rate of survival than other inotropic agents in meta-analyses, especially those involving patients undergoing cardiac surgery,” wrote the authors of the study, led by Giovanni Landoni, MD, of Vita-Salute San Raffaele University in Milan, adding, “Considering the pharmacologic properties of levosimendan and the results of previous studies, we hypothesized that the administration of levosimendan, in addition to standard treatment, might result in lower mortality in this context.”
Dr. Landoni and his colleagues conducted the Levosimendan to Reduce Mortality in High Risk Cardiac Surgery Patients: A Multicenter Randomized Controlled Trial, known more commonly as CHEETAH. Written consent was given by 4,725 patients from 14 centers located in Italy, Russia, and Brazil between November 2009 and April 2016. The investigators recruited a total of 506 patients. All subjects included in the study underwent cardiac surgery and experienced a perioperative cardiovascular dysfunction (N Engl J Med. 2017 Mar 21. doi: 10.1056/NEJMoa1616325).
Subjects were then randomized into a cohort receiving either a placebo or a low dose of levosimendan, which varied between 0.025 to 0.2 mcg/kg of body weight per minute continuously for up to 48 hours. A total of 248 subjects received levosimendan and 258 received placebo. All patients were administered the treatment while in the ICU; patients were taken off their regimen prior to 48 hours if they were discharged from the ICU. Anyone screened for inclusion who already had experienced a negative reaction to levosimendan was excluded from the study.
“We collected preoperative data on baseline characteristics and coexisting conditions, intraoperative and postoperative treatment data, postoperative laboratory values, duration of mechanical ventilation, durations of ICU and hospital stays, and major outcomes,” the authors explained, adding that “telephone follow-up was performed at 30 days and 180 days after randomization by an investigator who was unaware of the trial group assignments.”
The primary outcome of the study was 30-day mortality. The levosimendan cohort experienced 32 deaths (12.9%), while the placebo cohort saw 33 (12.8%), a nonsignificant difference (P = .97) between the two groups. Similarly, the median time spent on mechanical ventilation was 19 hours for those on levosimendan, versus 21 hours for those on placebo (P = .48), and median length of hospital stay was 14 days in both groups (P = .39).
“Previous meta-analyses of randomized, controlled trials showed a higher rate of survival with levosimendan than with other treatment regimens among patients undergoing cardiac surgery,” Dr. Landoni and his coauthors noted. Previous studies also had a number of key differences, such as the number of subjects who underwent coronary artery bypass grafting, the dosing of levosimendan, and inclusion of patients who had reduced preoperative ejection fraction instead of ones with myocardial dysfunction who needed inotropic support, which the current study used.
The study was funded by the Italian Ministry of Health. Dr. Landoni reported receiving nonfinancial support from the Orion Corporation while the study was ongoing; several other coauthors reported similar disclosures.
Adding a low dose of levosimendan to the standard care for patients on perioperative hemodynamic support does not improve outcomes to any significant extent, according to the findings of a new study presented at the annual congress of the European Society of Intensive Care Medicine and published simultaneously online in the New England Journal of Medicine.
“Levosimendan (Simdax, Orion) is an inotropic agent that has been shown to be associated with a higher rate of survival than other inotropic agents in meta-analyses, especially those involving patients undergoing cardiac surgery,” wrote the authors of the study, led by Giovanni Landoni, MD, of Vita-Salute San Raffaele University in Milan, adding, “Considering the pharmacologic properties of levosimendan and the results of previous studies, we hypothesized that the administration of levosimendan, in addition to standard treatment, might result in lower mortality in this context.”
Dr. Landoni and his colleagues conducted the Levosimendan to Reduce Mortality in High Risk Cardiac Surgery Patients: A Multicenter Randomized Controlled Trial, known more commonly as CHEETAH. Written consent was given by 4,725 patients from 14 centers located in Italy, Russia, and Brazil between November 2009 and April 2016. The investigators recruited a total of 506 patients. All subjects included in the study underwent cardiac surgery and experienced a perioperative cardiovascular dysfunction (N Engl J Med. 2017 Mar 21. doi: 10.1056/NEJMoa1616325).
Subjects were then randomized into a cohort receiving either a placebo or a low dose of levosimendan, which varied between 0.025 to 0.2 mcg/kg of body weight per minute continuously for up to 48 hours. A total of 248 subjects received levosimendan and 258 received placebo. All patients were administered the treatment while in the ICU; patients were taken off their regimen prior to 48 hours if they were discharged from the ICU. Anyone screened for inclusion who already had experienced a negative reaction to levosimendan was excluded from the study.
“We collected preoperative data on baseline characteristics and coexisting conditions, intraoperative and postoperative treatment data, postoperative laboratory values, duration of mechanical ventilation, durations of ICU and hospital stays, and major outcomes,” the authors explained, adding that “telephone follow-up was performed at 30 days and 180 days after randomization by an investigator who was unaware of the trial group assignments.”
The primary outcome of the study was 30-day mortality. The levosimendan cohort experienced 32 deaths (12.9%), while the placebo cohort saw 33 (12.8%), a nonsignificant difference (P = .97) between the two groups. Similarly, the median time spent on mechanical ventilation was 19 hours for those on levosimendan, versus 21 hours for those on placebo (P = .48), and median length of hospital stay was 14 days in both groups (P = .39).
“Previous meta-analyses of randomized, controlled trials showed a higher rate of survival with levosimendan than with other treatment regimens among patients undergoing cardiac surgery,” Dr. Landoni and his coauthors noted. Previous studies also had a number of key differences, such as the number of subjects who underwent coronary artery bypass grafting, the dosing of levosimendan, and inclusion of patients who had reduced preoperative ejection fraction instead of ones with myocardial dysfunction who needed inotropic support, which the current study used.
The study was funded by the Italian Ministry of Health. Dr. Landoni reported receiving nonfinancial support from the Orion Corporation while the study was ongoing; several other coauthors reported similar disclosures.
Adding a low dose of levosimendan to the standard care for patients on perioperative hemodynamic support does not improve outcomes to any significant extent, according to the findings of a new study presented at the annual congress of the European Society of Intensive Care Medicine and published simultaneously online in the New England Journal of Medicine.
“Levosimendan (Simdax, Orion) is an inotropic agent that has been shown to be associated with a higher rate of survival than other inotropic agents in meta-analyses, especially those involving patients undergoing cardiac surgery,” wrote the authors of the study, led by Giovanni Landoni, MD, of Vita-Salute San Raffaele University in Milan, adding, “Considering the pharmacologic properties of levosimendan and the results of previous studies, we hypothesized that the administration of levosimendan, in addition to standard treatment, might result in lower mortality in this context.”
Dr. Landoni and his colleagues conducted the Levosimendan to Reduce Mortality in High Risk Cardiac Surgery Patients: A Multicenter Randomized Controlled Trial, known more commonly as CHEETAH. Written consent was given by 4,725 patients from 14 centers located in Italy, Russia, and Brazil between November 2009 and April 2016. The investigators recruited a total of 506 patients. All subjects included in the study underwent cardiac surgery and experienced a perioperative cardiovascular dysfunction (N Engl J Med. 2017 Mar 21. doi: 10.1056/NEJMoa1616325).
Subjects were then randomized into a cohort receiving either a placebo or a low dose of levosimendan, which varied between 0.025 to 0.2 mcg/kg of body weight per minute continuously for up to 48 hours. A total of 248 subjects received levosimendan and 258 received placebo. All patients were administered the treatment while in the ICU; patients were taken off their regimen prior to 48 hours if they were discharged from the ICU. Anyone screened for inclusion who already had experienced a negative reaction to levosimendan was excluded from the study.
“We collected preoperative data on baseline characteristics and coexisting conditions, intraoperative and postoperative treatment data, postoperative laboratory values, duration of mechanical ventilation, durations of ICU and hospital stays, and major outcomes,” the authors explained, adding that “telephone follow-up was performed at 30 days and 180 days after randomization by an investigator who was unaware of the trial group assignments.”
The primary outcome of the study was 30-day mortality. The levosimendan cohort experienced 32 deaths (12.9%), while the placebo cohort saw 33 (12.8%), a nonsignificant difference (P = .97) between the two groups. Similarly, the median time spent on mechanical ventilation was 19 hours for those on levosimendan, versus 21 hours for those on placebo (P = .48), and median length of hospital stay was 14 days in both groups (P = .39).
“Previous meta-analyses of randomized, controlled trials showed a higher rate of survival with levosimendan than with other treatment regimens among patients undergoing cardiac surgery,” Dr. Landoni and his coauthors noted. Previous studies also had a number of key differences, such as the number of subjects who underwent coronary artery bypass grafting, the dosing of levosimendan, and inclusion of patients who had reduced preoperative ejection fraction instead of ones with myocardial dysfunction who needed inotropic support, which the current study used.
The study was funded by the Italian Ministry of Health. Dr. Landoni reported receiving nonfinancial support from the Orion Corporation while the study was ongoing; several other coauthors reported similar disclosures.
Key clinical point:
Major finding: Among other things, 30-day mortality rates between levosimendan (12.9%) and placebo (12.8%) cohorts were not significantly different (P = .97).
Data source: The CHEETAH study is a multicenter, randomized, double-blind, placebo-controlled trial of 506 cardiac surgery patients recommended for perioperative hemodynamic support.
Disclosures: Funded by the Italian Ministry of Health. Several coauthors reported potentially relevant conflicts of interest.
Older TAVR implant devices significantly less effective than newer ones in bicuspid AS patients
Using transcatheter aortic valve replacement (TAVR) to treat bicuspid aortic valve stenosis (AS) can be significantly less effective than using TAVR to treat tricuspid AS, according to the findings of a new study presented at the annual meeting of the American College of Cardiology and published simultaneously in the Journal of the American College of Cardiology.
“There is a paucity of data comparing the clinical outcomes of TAVR in bicuspid and tricuspid AS,” wrote the authors of the study, led by Sung-Han Yoon, MD, of the Cedars-Sinai Heart Institute in Los Angeles. “Given the increasing frequency of bicuspid AS in younger patients, coupled with the worldwide shift of treating younger and lower–surgical-risk patients with TAVR, the clinical outcomes of TAVR in bicuspid AS warrants special attention.”
Dr. Yoon and his coinvestigators began by collecting data from the Bicuspid AS TAVR registry, which began in December 2013 and contains information on patients from 33 health care centers around the world. Patients who entered the database prior to the initiation of the study were screened retroactively, while those who joined afterward were followed prospectively.
Eventually, 561 bicuspid AS patients were included in the study, out of a total of 576 that were treated between April 2005 and May 2016. Twelve centers also performed tricuspid AS, with investigators able to collect data on 5,900 patients who underwent the procedure during the same period of time. Ultimately, 4,546 were included in the study.
“Given the differences in baseline clinical, echocardiographic, and procedural characteristics between patients with bicuspid and tricuspid AS, propensity-score matching was applied to identify a cohort of patients with similar baseline characteristics, and thus clinical outcomes of propensity-score matched cohorts were compared,” the authors explained.
Variables used when establishing propensity-score matches included age, sex, New York Heart Association functional class III or IV, the presence of certain conditions such as chronic lung disease and diabetes, and procedural data. Dr. Yoon and his colleagues were able to create 546 pairs of matched patients between the bicuspid AS and tricuspid AS cohorts.
The devices implanted in subjects also underwent classification by the investigators, either as early-generation or new-generation devices. The former consisted of Sapien XT and CoreValve devices, while Sapien 3, Lotus, and Evolut R devices comprised the latter classification. A total of 320 bicuspid AS and 321 tricuspid AS patients received early-generation implant devices, with 226 and 225 patients, respectively, receiving new-generation devices.
Devices were less successful in bicuspid AS patients versus tricuspid AS patients: 85.3% and 91.4%, respectively (P = .002). Furthermore, a significantly higher rate of bicuspid AS patients had to be converted to surgery, compared with tricuspid AS patients: 2.0% and 0.2%, respectively (P = .006). Early-generation implant devices had considerably higher rates of issues in bicuspid AS patients, with 4.5% of those receiving Sapien XT experiencing aortic root injury and 0% of tricuspid AS patients with the same device having the same problem (P = .015). Bicuspid AS patients who received the CoreValve implant experienced paravalvular leak 19.4% of the time, compared with 10.5% in tricuspid AS patients (P = .02); these leaks were classified as “moderate to severe.”
“In addition, patients with bicuspid AS had more frequent second valve implantation (11.6% vs. 2.9%; P = .002) [and] subsequent lower device success rates (72.1% vs. 86.0%; P = .002) than those with tricuspid AS when receiving the CoreValve,” the authors noted. “However, there were no significant differences in these adverse procedural events between groups when receiving the Sapien 3 and Lotus.”
There were also no significant differences between the bicuspid and tricuspid AS in terms of mortality rates. At 2 years postoperation, all-cause mortality rates were 17.2% for bicuspid AS patients and 19.4% for tricuspid AS patients, regardless of the type of device implant (P = .28). When comparing early and new-generation devices, results were similarly nonsignificant: early-generation bicuspid vs. tricuspid AS all-cause mortality rates were 14.5% and 13.7%, respectively (P = .80) and 4.5% vs. 7.4% (P = .64) for new-generation devices.
“The present study is the first large-scale study that compared the safety, efficacy, and clinical outcomes of TAVR in patients with bicuspid and tricuspid AS,” Dr. Yoon and his colleagues noted, adding that, in regards to the disparity in device effectiveness, “The present study showed that the initial attempt of device advancement succeeded in overcoming the procedural limitations in tricuspid AS and now go beyond the challenges in treating bicuspid AS.”
No funding source for this study was disclosed. Dr. Yoon did not report any relevant financial disclosures, but several coauthors disclosed potentially relevant financial conflicts.
Using transcatheter aortic valve replacement (TAVR) to treat bicuspid aortic valve stenosis (AS) can be significantly less effective than using TAVR to treat tricuspid AS, according to the findings of a new study presented at the annual meeting of the American College of Cardiology and published simultaneously in the Journal of the American College of Cardiology.
“There is a paucity of data comparing the clinical outcomes of TAVR in bicuspid and tricuspid AS,” wrote the authors of the study, led by Sung-Han Yoon, MD, of the Cedars-Sinai Heart Institute in Los Angeles. “Given the increasing frequency of bicuspid AS in younger patients, coupled with the worldwide shift of treating younger and lower–surgical-risk patients with TAVR, the clinical outcomes of TAVR in bicuspid AS warrants special attention.”
Dr. Yoon and his coinvestigators began by collecting data from the Bicuspid AS TAVR registry, which began in December 2013 and contains information on patients from 33 health care centers around the world. Patients who entered the database prior to the initiation of the study were screened retroactively, while those who joined afterward were followed prospectively.
Eventually, 561 bicuspid AS patients were included in the study, out of a total of 576 that were treated between April 2005 and May 2016. Twelve centers also performed tricuspid AS, with investigators able to collect data on 5,900 patients who underwent the procedure during the same period of time. Ultimately, 4,546 were included in the study.
“Given the differences in baseline clinical, echocardiographic, and procedural characteristics between patients with bicuspid and tricuspid AS, propensity-score matching was applied to identify a cohort of patients with similar baseline characteristics, and thus clinical outcomes of propensity-score matched cohorts were compared,” the authors explained.
Variables used when establishing propensity-score matches included age, sex, New York Heart Association functional class III or IV, the presence of certain conditions such as chronic lung disease and diabetes, and procedural data. Dr. Yoon and his colleagues were able to create 546 pairs of matched patients between the bicuspid AS and tricuspid AS cohorts.
The devices implanted in subjects also underwent classification by the investigators, either as early-generation or new-generation devices. The former consisted of Sapien XT and CoreValve devices, while Sapien 3, Lotus, and Evolut R devices comprised the latter classification. A total of 320 bicuspid AS and 321 tricuspid AS patients received early-generation implant devices, with 226 and 225 patients, respectively, receiving new-generation devices.
Devices were less successful in bicuspid AS patients versus tricuspid AS patients: 85.3% and 91.4%, respectively (P = .002). Furthermore, a significantly higher rate of bicuspid AS patients had to be converted to surgery, compared with tricuspid AS patients: 2.0% and 0.2%, respectively (P = .006). Early-generation implant devices had considerably higher rates of issues in bicuspid AS patients, with 4.5% of those receiving Sapien XT experiencing aortic root injury and 0% of tricuspid AS patients with the same device having the same problem (P = .015). Bicuspid AS patients who received the CoreValve implant experienced paravalvular leak 19.4% of the time, compared with 10.5% in tricuspid AS patients (P = .02); these leaks were classified as “moderate to severe.”
“In addition, patients with bicuspid AS had more frequent second valve implantation (11.6% vs. 2.9%; P = .002) [and] subsequent lower device success rates (72.1% vs. 86.0%; P = .002) than those with tricuspid AS when receiving the CoreValve,” the authors noted. “However, there were no significant differences in these adverse procedural events between groups when receiving the Sapien 3 and Lotus.”
There were also no significant differences between the bicuspid and tricuspid AS in terms of mortality rates. At 2 years postoperation, all-cause mortality rates were 17.2% for bicuspid AS patients and 19.4% for tricuspid AS patients, regardless of the type of device implant (P = .28). When comparing early and new-generation devices, results were similarly nonsignificant: early-generation bicuspid vs. tricuspid AS all-cause mortality rates were 14.5% and 13.7%, respectively (P = .80) and 4.5% vs. 7.4% (P = .64) for new-generation devices.
“The present study is the first large-scale study that compared the safety, efficacy, and clinical outcomes of TAVR in patients with bicuspid and tricuspid AS,” Dr. Yoon and his colleagues noted, adding that, in regards to the disparity in device effectiveness, “The present study showed that the initial attempt of device advancement succeeded in overcoming the procedural limitations in tricuspid AS and now go beyond the challenges in treating bicuspid AS.”
No funding source for this study was disclosed. Dr. Yoon did not report any relevant financial disclosures, but several coauthors disclosed potentially relevant financial conflicts.
Using transcatheter aortic valve replacement (TAVR) to treat bicuspid aortic valve stenosis (AS) can be significantly less effective than using TAVR to treat tricuspid AS, according to the findings of a new study presented at the annual meeting of the American College of Cardiology and published simultaneously in the Journal of the American College of Cardiology.
“There is a paucity of data comparing the clinical outcomes of TAVR in bicuspid and tricuspid AS,” wrote the authors of the study, led by Sung-Han Yoon, MD, of the Cedars-Sinai Heart Institute in Los Angeles. “Given the increasing frequency of bicuspid AS in younger patients, coupled with the worldwide shift of treating younger and lower–surgical-risk patients with TAVR, the clinical outcomes of TAVR in bicuspid AS warrants special attention.”
Dr. Yoon and his coinvestigators began by collecting data from the Bicuspid AS TAVR registry, which began in December 2013 and contains information on patients from 33 health care centers around the world. Patients who entered the database prior to the initiation of the study were screened retroactively, while those who joined afterward were followed prospectively.
Eventually, 561 bicuspid AS patients were included in the study, out of a total of 576 that were treated between April 2005 and May 2016. Twelve centers also performed tricuspid AS, with investigators able to collect data on 5,900 patients who underwent the procedure during the same period of time. Ultimately, 4,546 were included in the study.
“Given the differences in baseline clinical, echocardiographic, and procedural characteristics between patients with bicuspid and tricuspid AS, propensity-score matching was applied to identify a cohort of patients with similar baseline characteristics, and thus clinical outcomes of propensity-score matched cohorts were compared,” the authors explained.
Variables used when establishing propensity-score matches included age, sex, New York Heart Association functional class III or IV, the presence of certain conditions such as chronic lung disease and diabetes, and procedural data. Dr. Yoon and his colleagues were able to create 546 pairs of matched patients between the bicuspid AS and tricuspid AS cohorts.
The devices implanted in subjects also underwent classification by the investigators, either as early-generation or new-generation devices. The former consisted of Sapien XT and CoreValve devices, while Sapien 3, Lotus, and Evolut R devices comprised the latter classification. A total of 320 bicuspid AS and 321 tricuspid AS patients received early-generation implant devices, with 226 and 225 patients, respectively, receiving new-generation devices.
Devices were less successful in bicuspid AS patients versus tricuspid AS patients: 85.3% and 91.4%, respectively (P = .002). Furthermore, a significantly higher rate of bicuspid AS patients had to be converted to surgery, compared with tricuspid AS patients: 2.0% and 0.2%, respectively (P = .006). Early-generation implant devices had considerably higher rates of issues in bicuspid AS patients, with 4.5% of those receiving Sapien XT experiencing aortic root injury and 0% of tricuspid AS patients with the same device having the same problem (P = .015). Bicuspid AS patients who received the CoreValve implant experienced paravalvular leak 19.4% of the time, compared with 10.5% in tricuspid AS patients (P = .02); these leaks were classified as “moderate to severe.”
“In addition, patients with bicuspid AS had more frequent second valve implantation (11.6% vs. 2.9%; P = .002) [and] subsequent lower device success rates (72.1% vs. 86.0%; P = .002) than those with tricuspid AS when receiving the CoreValve,” the authors noted. “However, there were no significant differences in these adverse procedural events between groups when receiving the Sapien 3 and Lotus.”
There were also no significant differences between the bicuspid and tricuspid AS in terms of mortality rates. At 2 years postoperation, all-cause mortality rates were 17.2% for bicuspid AS patients and 19.4% for tricuspid AS patients, regardless of the type of device implant (P = .28). When comparing early and new-generation devices, results were similarly nonsignificant: early-generation bicuspid vs. tricuspid AS all-cause mortality rates were 14.5% and 13.7%, respectively (P = .80) and 4.5% vs. 7.4% (P = .64) for new-generation devices.
“The present study is the first large-scale study that compared the safety, efficacy, and clinical outcomes of TAVR in patients with bicuspid and tricuspid AS,” Dr. Yoon and his colleagues noted, adding that, in regards to the disparity in device effectiveness, “The present study showed that the initial attempt of device advancement succeeded in overcoming the procedural limitations in tricuspid AS and now go beyond the challenges in treating bicuspid AS.”
No funding source for this study was disclosed. Dr. Yoon did not report any relevant financial disclosures, but several coauthors disclosed potentially relevant financial conflicts.
From ACC 17
Key clinical point:
Major finding: Bicuspid AS patients had significantly lower device success rates than those getting tricuspid AS: 85.3% vs. 91.4% (P = .002); also were more likely to convert to surgery: 2.0% vs. 0.2% (P = .006).
Data source: Matched cohort study of 561 bicuspid AS and 4,546 tricuspid AS patients; data collected both retrospectively and prospectively.
Disclosures: No funding source disclosed. Dr. Yoon reported no relevant disclosures.
EBUS scope, EUS-FNA similarly effective
When assessing a patient for lung cancer, a procedure involving the insertion of an EBUS scope in the esophagus – EUS-B-FNA – can achieve similarly accurate results as endoscopic ultrasound guided–fine-needle aspiration (EUS-FNA), according to a new study.
This finding could lead patients to choose EUS-B-FNA over EUS-FNA – the standard of care for analyzing potential metastasis of the left adrenal glands (LAGs) – resulting in both time and cost savings for patients.
“A recent report showed that LAG visualization using the EBUS scope was possible in 85% of patients,” according to the authors of this study, including Prof. Jouke T. Annema, MD of the University of Amsterdam. Prior to this new research, it was unknown to what extent a single EBUS scope adequately assess and sample the LAGs and how its performance related to the use of a conventional endoscopic ultrasound–guided scope (Lung Cancer. 2017. doi: org/10.1016/j.lungcan.2017.02.011).
Dr. Annema and his coauthors recruited patients from four centers – three in the Netherlands, one in Poland – and followed them prospectively. Patients with “(suspected) lung cancer [who] had an indication for both mediastinal lymph node and LAG sampling” were recruited for the study. The researchers followed 44 patients through final diagnosis to determine if they ultimately had lung cancer.
Subjects first received complete mediastinal and hilar staging of lung cancer and any present tumors via an EBUS and EUS-B procedure. Following an EBUS examination of the mediastinum, the EBUS scope was retracted from the trachea and positioned into the esophagus for an examination of the mediastinal nodes. Then, the EBUS scope was advanced into the stomach for identification of the LAG. Afterward, the routine EUS-FNA was performed. LAG analysis across both methods involved visualizing the LAG and collecting an adequate tissue sample for testing.
“In short, in order to locate the LAG, a structured three step approach was used according to the EUS assessment tool (EUS-AT): identification of the liver, abdominal aorta, coeliac trunk, left kidney, and LAG,” the authors noted. “By turning the EBUS scope clockwise from the liver, the abdominal aorta and coeliac trun[k] are identified. By subsequently turning the EBUS scope gently in caudal direction, the left kidney and LAG are identified.”
Endoscopists then evaluated both procedures in each subject according to feasibility and practicability to determine if the findings of the experimental procedure were usable. Finally, a cytologic exam was conducted, using Giemsa or Papanicolaou staining to determine if any present cancer had metastasized, and a final diagnosis was made.
LAG analysis had a success rate of 89% (39/44; 95% confidence interval, 76-95%) for EUS-B-FNA, compared with 93% (41/44; 95% CI, 82-98%) for EUS-FNA. Similarly, when looking at the rate of sensitivity for LAG metastases, EUS-B had a rate of sensitivity for LAG metastases of at least 87% (95% CI, 65-97%), while EUS-FNA was found to be at least 83% (95% CI, 62-95%. Endoscopists were equally satisfied with both procedures in the “majority” of cases in this study.
“In [five] cases (11%), the EUS-B-FNA procedure was unsuccessful, due to the inability to make good contact of the ultrasound transducer and the stomach wall,” the authors explained. “The conventional EUS scope is more stable as a result of the increased tube diameter. Another advantage of the conventional echo-endoscope is its wider scanning angle. ... The conventional EUS scope is also longer than the EBUS scope, [but that] does not seem to be the limiting factor.”
No funding source was disclosed for this study. The authors reported no relevant financial disclosures.
When assessing a patient for lung cancer, a procedure involving the insertion of an EBUS scope in the esophagus – EUS-B-FNA – can achieve similarly accurate results as endoscopic ultrasound guided–fine-needle aspiration (EUS-FNA), according to a new study.
This finding could lead patients to choose EUS-B-FNA over EUS-FNA – the standard of care for analyzing potential metastasis of the left adrenal glands (LAGs) – resulting in both time and cost savings for patients.
“A recent report showed that LAG visualization using the EBUS scope was possible in 85% of patients,” according to the authors of this study, including Prof. Jouke T. Annema, MD of the University of Amsterdam. Prior to this new research, it was unknown to what extent a single EBUS scope adequately assess and sample the LAGs and how its performance related to the use of a conventional endoscopic ultrasound–guided scope (Lung Cancer. 2017. doi: org/10.1016/j.lungcan.2017.02.011).
Dr. Annema and his coauthors recruited patients from four centers – three in the Netherlands, one in Poland – and followed them prospectively. Patients with “(suspected) lung cancer [who] had an indication for both mediastinal lymph node and LAG sampling” were recruited for the study. The researchers followed 44 patients through final diagnosis to determine if they ultimately had lung cancer.
Subjects first received complete mediastinal and hilar staging of lung cancer and any present tumors via an EBUS and EUS-B procedure. Following an EBUS examination of the mediastinum, the EBUS scope was retracted from the trachea and positioned into the esophagus for an examination of the mediastinal nodes. Then, the EBUS scope was advanced into the stomach for identification of the LAG. Afterward, the routine EUS-FNA was performed. LAG analysis across both methods involved visualizing the LAG and collecting an adequate tissue sample for testing.
“In short, in order to locate the LAG, a structured three step approach was used according to the EUS assessment tool (EUS-AT): identification of the liver, abdominal aorta, coeliac trunk, left kidney, and LAG,” the authors noted. “By turning the EBUS scope clockwise from the liver, the abdominal aorta and coeliac trun[k] are identified. By subsequently turning the EBUS scope gently in caudal direction, the left kidney and LAG are identified.”
Endoscopists then evaluated both procedures in each subject according to feasibility and practicability to determine if the findings of the experimental procedure were usable. Finally, a cytologic exam was conducted, using Giemsa or Papanicolaou staining to determine if any present cancer had metastasized, and a final diagnosis was made.
LAG analysis had a success rate of 89% (39/44; 95% confidence interval, 76-95%) for EUS-B-FNA, compared with 93% (41/44; 95% CI, 82-98%) for EUS-FNA. Similarly, when looking at the rate of sensitivity for LAG metastases, EUS-B had a rate of sensitivity for LAG metastases of at least 87% (95% CI, 65-97%), while EUS-FNA was found to be at least 83% (95% CI, 62-95%. Endoscopists were equally satisfied with both procedures in the “majority” of cases in this study.
“In [five] cases (11%), the EUS-B-FNA procedure was unsuccessful, due to the inability to make good contact of the ultrasound transducer and the stomach wall,” the authors explained. “The conventional EUS scope is more stable as a result of the increased tube diameter. Another advantage of the conventional echo-endoscope is its wider scanning angle. ... The conventional EUS scope is also longer than the EBUS scope, [but that] does not seem to be the limiting factor.”
No funding source was disclosed for this study. The authors reported no relevant financial disclosures.
When assessing a patient for lung cancer, a procedure involving the insertion of an EBUS scope in the esophagus – EUS-B-FNA – can achieve similarly accurate results as endoscopic ultrasound guided–fine-needle aspiration (EUS-FNA), according to a new study.
This finding could lead patients to choose EUS-B-FNA over EUS-FNA – the standard of care for analyzing potential metastasis of the left adrenal glands (LAGs) – resulting in both time and cost savings for patients.
“A recent report showed that LAG visualization using the EBUS scope was possible in 85% of patients,” according to the authors of this study, including Prof. Jouke T. Annema, MD of the University of Amsterdam. Prior to this new research, it was unknown to what extent a single EBUS scope adequately assess and sample the LAGs and how its performance related to the use of a conventional endoscopic ultrasound–guided scope (Lung Cancer. 2017. doi: org/10.1016/j.lungcan.2017.02.011).
Dr. Annema and his coauthors recruited patients from four centers – three in the Netherlands, one in Poland – and followed them prospectively. Patients with “(suspected) lung cancer [who] had an indication for both mediastinal lymph node and LAG sampling” were recruited for the study. The researchers followed 44 patients through final diagnosis to determine if they ultimately had lung cancer.
Subjects first received complete mediastinal and hilar staging of lung cancer and any present tumors via an EBUS and EUS-B procedure. Following an EBUS examination of the mediastinum, the EBUS scope was retracted from the trachea and positioned into the esophagus for an examination of the mediastinal nodes. Then, the EBUS scope was advanced into the stomach for identification of the LAG. Afterward, the routine EUS-FNA was performed. LAG analysis across both methods involved visualizing the LAG and collecting an adequate tissue sample for testing.
“In short, in order to locate the LAG, a structured three step approach was used according to the EUS assessment tool (EUS-AT): identification of the liver, abdominal aorta, coeliac trunk, left kidney, and LAG,” the authors noted. “By turning the EBUS scope clockwise from the liver, the abdominal aorta and coeliac trun[k] are identified. By subsequently turning the EBUS scope gently in caudal direction, the left kidney and LAG are identified.”
Endoscopists then evaluated both procedures in each subject according to feasibility and practicability to determine if the findings of the experimental procedure were usable. Finally, a cytologic exam was conducted, using Giemsa or Papanicolaou staining to determine if any present cancer had metastasized, and a final diagnosis was made.
LAG analysis had a success rate of 89% (39/44; 95% confidence interval, 76-95%) for EUS-B-FNA, compared with 93% (41/44; 95% CI, 82-98%) for EUS-FNA. Similarly, when looking at the rate of sensitivity for LAG metastases, EUS-B had a rate of sensitivity for LAG metastases of at least 87% (95% CI, 65-97%), while EUS-FNA was found to be at least 83% (95% CI, 62-95%. Endoscopists were equally satisfied with both procedures in the “majority” of cases in this study.
“In [five] cases (11%), the EUS-B-FNA procedure was unsuccessful, due to the inability to make good contact of the ultrasound transducer and the stomach wall,” the authors explained. “The conventional EUS scope is more stable as a result of the increased tube diameter. Another advantage of the conventional echo-endoscope is its wider scanning angle. ... The conventional EUS scope is also longer than the EBUS scope, [but that] does not seem to be the limiting factor.”
No funding source was disclosed for this study. The authors reported no relevant financial disclosures.
FROM LUNG CANCER
Key clinical point:
Major finding: EUS-B-FNA had a success rate of 89%, versus 93% for EUS-FNA, while sensitivity for LAG metastases were 87% and 83%, respectively.
Data source: Multicenter, prospective study of 44 consecutive suspected lung cancer patients.
Disclosures: No funding source disclosed. Authors reported no relevant financial disclosures.
CDC: Greater activity limitations accompany rising arthritis prevalence
The number of adults with arthritis in the United States continues to rise, with the number projected to climb as high as 78 million by the year 2040. Some of the keys to stemming this rising tide are exercise, along with greater knowledge of how to manage symptoms, according to a new report from the Centers for Disease Control and Prevention.
“Arthritis is at an all-time high: more than 54 million people report a diagnosis of it, and alarmingly, more people with arthritis are suffering from it,” said Anne Schuchat, MD, acting director of the CDC, during a conference call regarding the agency’s latest Vital Signs report (MMWR Morb Mortal Wkly Rep. 2017 Mar 7. doi: org/10.15585/mmwr.mm6609e1). “Among adults with arthritis, the percentage whose lives are particularly limited has increased by about 20% since 2002, from about 36% in 2002 to 43% in 2015. We’re seeing this increase independent of aging of the population.”
“Physical activity can be the antidote for many people [and] can actually decrease pain and improve function by almost 40%,” Dr. Schuchat explained. “Right now, one in three adults with arthritis report being inactive [because of] pain or fear of pain or not knowing what exercise is safe for their joints.”
This inactivity can lead to arthritis patients developing other serious chronic conditions, such as heart disease, diabetes and obesity – conditions that all require physical activity in order to properly manage them. Arthritis alone puts an extraordinary financial burden on the domestic health care industry, as direct medical costs associated with the condition total roughly $81 billion per year, according to the CDC. Additionally, about half of all adults with heart disease or diabetes, and about one-third of obese adults, also have arthritis.
In addition to engaging in regular physical activity, the Vital Signs report also recommends that arthritis patients attend disease management education programs, which are available regionally but often go underutilized, largely due to lack of awareness about them or trepidation regarding how effective the programs really are. To combat this, the CDC is calling on health care providers to help them educate patients about these classes and spread the word about the steps that can be taken to manage arthritis. In 2017, the CDC is funding arthritis programs in 12 states (California, Kansas, Kentucky, Michigan, Missouri, Montana, New York, Oregon, Pennsylvania, Rhode Island, South Carolina, and Utah) to disseminate arthritis-appropriate evidence-based physical activity and self-management education interventions.
“Men or women with arthritis can reduce their symptoms by 10%-20% by participating in disease management education programs to acquire skills to better manage their symptoms. Right now, these programs are only reaching about 1 in 10 people with arthritis, but the classes are available in many community settings,” Dr. Schuchat said. “We know that adults with arthritis are significantly more likely to attend a disease management education program when a health care provider recommends it to them.”
When seeing patients with arthritis, Dr. Schuchat advised health care providers to recommend routine physical activity, such as walking, biking, swimming, and physical activity programs offered by local parks and recreation centers, as well as weight loss, in order to ease joint pain. The American College of Rheumatology and other professional organizations provide guidelines for discussing treatment options with patients. Providing treatment or additional services for depression or anxiety, which occur in about one-third of adult arthritis patients, may help individuals to better manage their arthritis symptoms.
The agency’s report derives from its analysis of 2013-2015 data from the National Health Interview Survey, which comprised a nationally representative sample of about 36,000 in-person interviews. The survey classifies individuals with physician-diagnosed arthritis as those who answered “yes” to the question “Have you ever been told by a doctor or other health professional that you have some form of arthritis, rheumatoid arthritis, gout, lupus, or fibromyalgia?”
The number of adults with arthritis in the United States continues to rise, with the number projected to climb as high as 78 million by the year 2040. Some of the keys to stemming this rising tide are exercise, along with greater knowledge of how to manage symptoms, according to a new report from the Centers for Disease Control and Prevention.
“Arthritis is at an all-time high: more than 54 million people report a diagnosis of it, and alarmingly, more people with arthritis are suffering from it,” said Anne Schuchat, MD, acting director of the CDC, during a conference call regarding the agency’s latest Vital Signs report (MMWR Morb Mortal Wkly Rep. 2017 Mar 7. doi: org/10.15585/mmwr.mm6609e1). “Among adults with arthritis, the percentage whose lives are particularly limited has increased by about 20% since 2002, from about 36% in 2002 to 43% in 2015. We’re seeing this increase independent of aging of the population.”
“Physical activity can be the antidote for many people [and] can actually decrease pain and improve function by almost 40%,” Dr. Schuchat explained. “Right now, one in three adults with arthritis report being inactive [because of] pain or fear of pain or not knowing what exercise is safe for their joints.”
This inactivity can lead to arthritis patients developing other serious chronic conditions, such as heart disease, diabetes and obesity – conditions that all require physical activity in order to properly manage them. Arthritis alone puts an extraordinary financial burden on the domestic health care industry, as direct medical costs associated with the condition total roughly $81 billion per year, according to the CDC. Additionally, about half of all adults with heart disease or diabetes, and about one-third of obese adults, also have arthritis.
In addition to engaging in regular physical activity, the Vital Signs report also recommends that arthritis patients attend disease management education programs, which are available regionally but often go underutilized, largely due to lack of awareness about them or trepidation regarding how effective the programs really are. To combat this, the CDC is calling on health care providers to help them educate patients about these classes and spread the word about the steps that can be taken to manage arthritis. In 2017, the CDC is funding arthritis programs in 12 states (California, Kansas, Kentucky, Michigan, Missouri, Montana, New York, Oregon, Pennsylvania, Rhode Island, South Carolina, and Utah) to disseminate arthritis-appropriate evidence-based physical activity and self-management education interventions.
“Men or women with arthritis can reduce their symptoms by 10%-20% by participating in disease management education programs to acquire skills to better manage their symptoms. Right now, these programs are only reaching about 1 in 10 people with arthritis, but the classes are available in many community settings,” Dr. Schuchat said. “We know that adults with arthritis are significantly more likely to attend a disease management education program when a health care provider recommends it to them.”
When seeing patients with arthritis, Dr. Schuchat advised health care providers to recommend routine physical activity, such as walking, biking, swimming, and physical activity programs offered by local parks and recreation centers, as well as weight loss, in order to ease joint pain. The American College of Rheumatology and other professional organizations provide guidelines for discussing treatment options with patients. Providing treatment or additional services for depression or anxiety, which occur in about one-third of adult arthritis patients, may help individuals to better manage their arthritis symptoms.
The agency’s report derives from its analysis of 2013-2015 data from the National Health Interview Survey, which comprised a nationally representative sample of about 36,000 in-person interviews. The survey classifies individuals with physician-diagnosed arthritis as those who answered “yes” to the question “Have you ever been told by a doctor or other health professional that you have some form of arthritis, rheumatoid arthritis, gout, lupus, or fibromyalgia?”
The number of adults with arthritis in the United States continues to rise, with the number projected to climb as high as 78 million by the year 2040. Some of the keys to stemming this rising tide are exercise, along with greater knowledge of how to manage symptoms, according to a new report from the Centers for Disease Control and Prevention.
“Arthritis is at an all-time high: more than 54 million people report a diagnosis of it, and alarmingly, more people with arthritis are suffering from it,” said Anne Schuchat, MD, acting director of the CDC, during a conference call regarding the agency’s latest Vital Signs report (MMWR Morb Mortal Wkly Rep. 2017 Mar 7. doi: org/10.15585/mmwr.mm6609e1). “Among adults with arthritis, the percentage whose lives are particularly limited has increased by about 20% since 2002, from about 36% in 2002 to 43% in 2015. We’re seeing this increase independent of aging of the population.”
“Physical activity can be the antidote for many people [and] can actually decrease pain and improve function by almost 40%,” Dr. Schuchat explained. “Right now, one in three adults with arthritis report being inactive [because of] pain or fear of pain or not knowing what exercise is safe for their joints.”
This inactivity can lead to arthritis patients developing other serious chronic conditions, such as heart disease, diabetes and obesity – conditions that all require physical activity in order to properly manage them. Arthritis alone puts an extraordinary financial burden on the domestic health care industry, as direct medical costs associated with the condition total roughly $81 billion per year, according to the CDC. Additionally, about half of all adults with heart disease or diabetes, and about one-third of obese adults, also have arthritis.
In addition to engaging in regular physical activity, the Vital Signs report also recommends that arthritis patients attend disease management education programs, which are available regionally but often go underutilized, largely due to lack of awareness about them or trepidation regarding how effective the programs really are. To combat this, the CDC is calling on health care providers to help them educate patients about these classes and spread the word about the steps that can be taken to manage arthritis. In 2017, the CDC is funding arthritis programs in 12 states (California, Kansas, Kentucky, Michigan, Missouri, Montana, New York, Oregon, Pennsylvania, Rhode Island, South Carolina, and Utah) to disseminate arthritis-appropriate evidence-based physical activity and self-management education interventions.
“Men or women with arthritis can reduce their symptoms by 10%-20% by participating in disease management education programs to acquire skills to better manage their symptoms. Right now, these programs are only reaching about 1 in 10 people with arthritis, but the classes are available in many community settings,” Dr. Schuchat said. “We know that adults with arthritis are significantly more likely to attend a disease management education program when a health care provider recommends it to them.”
When seeing patients with arthritis, Dr. Schuchat advised health care providers to recommend routine physical activity, such as walking, biking, swimming, and physical activity programs offered by local parks and recreation centers, as well as weight loss, in order to ease joint pain. The American College of Rheumatology and other professional organizations provide guidelines for discussing treatment options with patients. Providing treatment or additional services for depression or anxiety, which occur in about one-third of adult arthritis patients, may help individuals to better manage their arthritis symptoms.
The agency’s report derives from its analysis of 2013-2015 data from the National Health Interview Survey, which comprised a nationally representative sample of about 36,000 in-person interviews. The survey classifies individuals with physician-diagnosed arthritis as those who answered “yes” to the question “Have you ever been told by a doctor or other health professional that you have some form of arthritis, rheumatoid arthritis, gout, lupus, or fibromyalgia?”
FROM MMWR
Key clinical point:
Major finding: About 24 million American adults report being significantly limited due to their arthritis.
Data source: 2013-2015 data from the National Health Interview Survey.
Disclosures: No disclosures were reported.