User login
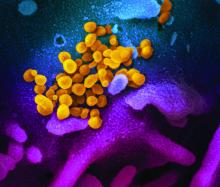
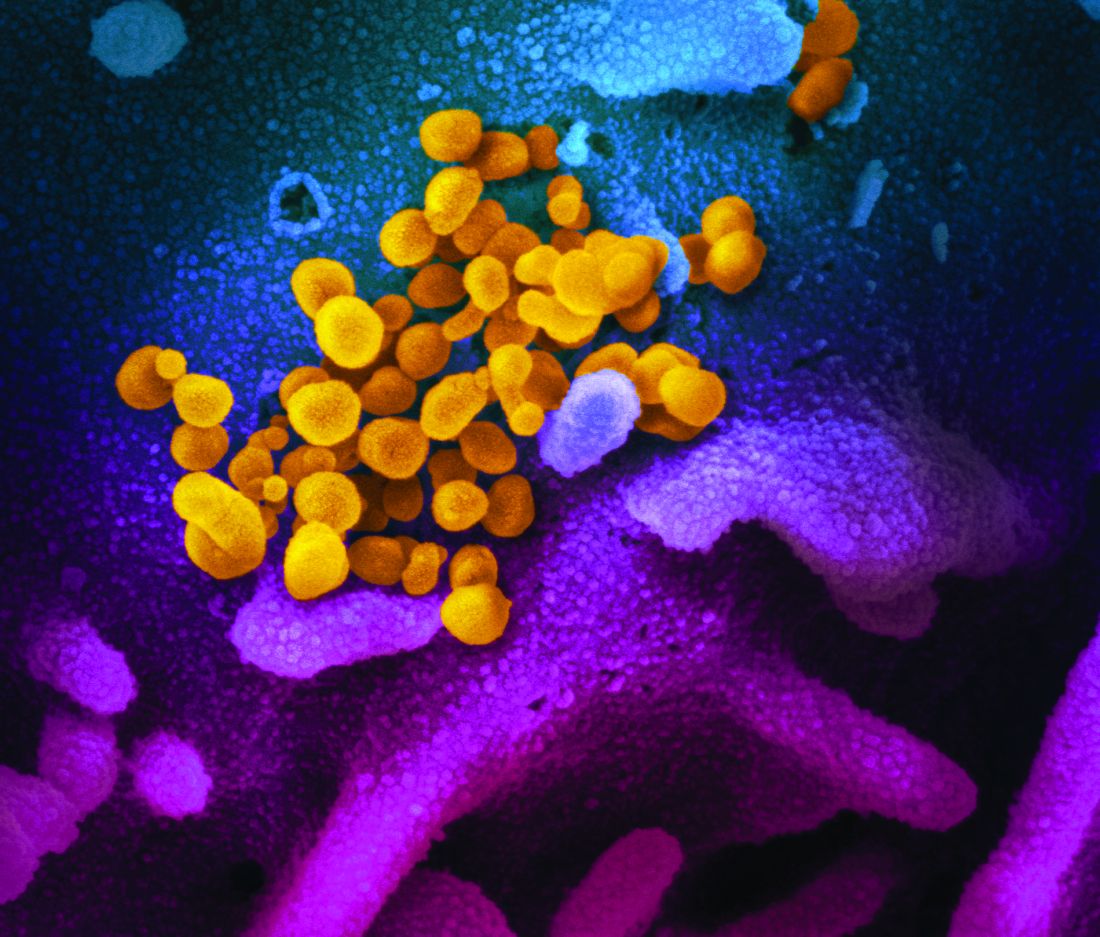
COVID-19: Time to ‘take the risk of scaring people’
It’s past time to call the novel coronavirus, COVID-19, a pandemic and “time to push people to prepare, and guide their prep,” according to risk communication experts.
Medical messaging about containing or stopping the spread of the virus is doing more harm than good, write Peter Sandman, PhD, and Jody Lanard, MD, both based in New York City, in a recent blog post.
“We are near-certain that the desperate-sounding last-ditch containment messaging of recent days is contributing to a massive global misperception,” they warn.
“The most crucial (and overdue) risk communication task … is to help people visualize their communities when ‘keeping it out’ – containment – is no longer relevant.”
That message is embraced by several experts who spoke to Medscape Medical News.
“I’m jealous of what [they] have written: It is so clear, so correct, and so practical,” said David Fisman, MD, MPH, professor of epidemiology at the University of Toronto, Canada. “I think WHO [World Health Organization] is shying away from the P word,” he continued, referring to the organization’s continuing decision not to call the outbreak a pandemic.
“I fully support exactly what [Sandman and Lanard] are saying,” said Michael Osterholm, PhD, MPH, professor of environmental health sciences and director of the Center for Infectious Disease Research and Policy (CIDRAP) at the University of Minnesota in Minneapolis.
Sandman and Lanard write. “Hardly any officials are telling civil society and the general public how to get ready for this pandemic.”
Effective communication should inform people of what to expect now, they continue: “[T]he end of most quarantines, travel restrictions, contact tracing, and other measures designed to keep ‘them’ from infecting ‘us,’ and the switch to measures like canceling mass events designed to keep us from infecting each other.”
Among the new messages that should be delivered are things like:
- Stockpiling nonperishable food and prescription meds.
- Considering care of sick family members.
- Cross-training work personnel so one person’s absence won’t derail an organization’s ability to function.
“We hope that governments and healthcare institutions are using this time wisely,” Sandman and Lanard continue. “We know that ordinary citizens are not being asked to do so. In most countries … ordinary citizens have not been asked to prepare. Instead, they have been led to expect that their governments will keep the virus from their doors.”
This article first appeared on Medscape.com.
It’s past time to call the novel coronavirus, COVID-19, a pandemic and “time to push people to prepare, and guide their prep,” according to risk communication experts.
Medical messaging about containing or stopping the spread of the virus is doing more harm than good, write Peter Sandman, PhD, and Jody Lanard, MD, both based in New York City, in a recent blog post.
“We are near-certain that the desperate-sounding last-ditch containment messaging of recent days is contributing to a massive global misperception,” they warn.
“The most crucial (and overdue) risk communication task … is to help people visualize their communities when ‘keeping it out’ – containment – is no longer relevant.”
That message is embraced by several experts who spoke to Medscape Medical News.
“I’m jealous of what [they] have written: It is so clear, so correct, and so practical,” said David Fisman, MD, MPH, professor of epidemiology at the University of Toronto, Canada. “I think WHO [World Health Organization] is shying away from the P word,” he continued, referring to the organization’s continuing decision not to call the outbreak a pandemic.
“I fully support exactly what [Sandman and Lanard] are saying,” said Michael Osterholm, PhD, MPH, professor of environmental health sciences and director of the Center for Infectious Disease Research and Policy (CIDRAP) at the University of Minnesota in Minneapolis.
Sandman and Lanard write. “Hardly any officials are telling civil society and the general public how to get ready for this pandemic.”
Effective communication should inform people of what to expect now, they continue: “[T]he end of most quarantines, travel restrictions, contact tracing, and other measures designed to keep ‘them’ from infecting ‘us,’ and the switch to measures like canceling mass events designed to keep us from infecting each other.”
Among the new messages that should be delivered are things like:
- Stockpiling nonperishable food and prescription meds.
- Considering care of sick family members.
- Cross-training work personnel so one person’s absence won’t derail an organization’s ability to function.
“We hope that governments and healthcare institutions are using this time wisely,” Sandman and Lanard continue. “We know that ordinary citizens are not being asked to do so. In most countries … ordinary citizens have not been asked to prepare. Instead, they have been led to expect that their governments will keep the virus from their doors.”
This article first appeared on Medscape.com.
It’s past time to call the novel coronavirus, COVID-19, a pandemic and “time to push people to prepare, and guide their prep,” according to risk communication experts.
Medical messaging about containing or stopping the spread of the virus is doing more harm than good, write Peter Sandman, PhD, and Jody Lanard, MD, both based in New York City, in a recent blog post.
“We are near-certain that the desperate-sounding last-ditch containment messaging of recent days is contributing to a massive global misperception,” they warn.
“The most crucial (and overdue) risk communication task … is to help people visualize their communities when ‘keeping it out’ – containment – is no longer relevant.”
That message is embraced by several experts who spoke to Medscape Medical News.
“I’m jealous of what [they] have written: It is so clear, so correct, and so practical,” said David Fisman, MD, MPH, professor of epidemiology at the University of Toronto, Canada. “I think WHO [World Health Organization] is shying away from the P word,” he continued, referring to the organization’s continuing decision not to call the outbreak a pandemic.
“I fully support exactly what [Sandman and Lanard] are saying,” said Michael Osterholm, PhD, MPH, professor of environmental health sciences and director of the Center for Infectious Disease Research and Policy (CIDRAP) at the University of Minnesota in Minneapolis.
Sandman and Lanard write. “Hardly any officials are telling civil society and the general public how to get ready for this pandemic.”
Effective communication should inform people of what to expect now, they continue: “[T]he end of most quarantines, travel restrictions, contact tracing, and other measures designed to keep ‘them’ from infecting ‘us,’ and the switch to measures like canceling mass events designed to keep us from infecting each other.”
Among the new messages that should be delivered are things like:
- Stockpiling nonperishable food and prescription meds.
- Considering care of sick family members.
- Cross-training work personnel so one person’s absence won’t derail an organization’s ability to function.
“We hope that governments and healthcare institutions are using this time wisely,” Sandman and Lanard continue. “We know that ordinary citizens are not being asked to do so. In most countries … ordinary citizens have not been asked to prepare. Instead, they have been led to expect that their governments will keep the virus from their doors.”
This article first appeared on Medscape.com.
Prenatal Stress May Have Long-Term Effects
MONTREAL – Cognitive, behavioral, and physical problems still persist today in a group of children exposed to prenatal stress during the Quebec ice storm of January 1998, according to research presented at the annual meeting of the International Society for Traumatic Stress Studies.
"The fetus is not immune to a certain amount of stress, which can be transmitted – probably biologically – from the mother, with resulting cognitive, emotional, physical, and motor development problems," reported Suzanne King, Ph.D., associate professor of psychiatry at McGill University and director of the psychosocial research division of the Douglas Hospital, both in Montreal.
The study measured subjective stress and objective hardship in 150 women during the ice storm, which was described as "the worst natural disaster in Canadian history" by the Insurance Bureau of Canada.
During the midwinter storm, 3 million people were left with no electricity, some for as long as 45 days, and 454 shelters were set up to house more than 17,000 people.
The study is the first prospective analysis of the effects of stress from a natural disaster on pregnant women and their children, said Dr. King. It used questionnaires to measure subjective and objective maternal stress during the storm, and then followed the offspring at 6 months, 2 years, 5.5 years, and 11.5 years.
From a sample of 1,440 women, only 224 responded (15%), and 150 completed the study. "Our resulting sample ended up being a highly educated group with a higher socioeconomic standard than average, which adds significance to the findings," she said.
On average, women in the study were without electricity for 15 days (range, 0-45) and without telephone contact for 4 days (range, 0-34). Two-thirds of them were forced to leave their homes during the storm, and possible posttraumatic stress disorder was present in 4%-17%, said Dr. King.
Although the rates of postpartum depression and premature birth (before 37 weeks) were within normal ranges at 17% and 8%, respectively, there was evidence of compromised cognitive development in the offspring at 2 years, with an odds ratio of 4.4 for delayed development in offspring exposed to high versus low levels of maternal objective stress. "This was controlling for subjective stress, which did not have a significant impact on this outcome. This was objective stress – just the facts – what happened to them," she said.
Additionally, at 2 years, there was a 10-point difference in IQ levels between these two sets of offspring, and these differences persisted at 8.5 years, the most recent data available.
In terms of subjective stress, high levels of maternal subjective stress were associated with increasing levels of offspring internalizing problems such as anxiety and depression, and externalizing problems such as aggression, she added.
"The kids are doing very well because they are from such highly resourced families – their IQs are still quite high, they’re above average – but even in these families we see this significant effect."
Additionally, an analysis of autisticlike symptoms at 6.5 years showed an interaction between both maternal stress and trimester of pregnancy. "For kids who were exposed to stress during the first trimester only, there were increasingly severe autisticlike symptoms with increasing objective stress. None of these kids are autistic, or even close, but in terms of these types of traits we are seeing an effect."
The researchers also examined dermatoglyphic asymmetry of fingertip ridges, a characteristic found more commonly in schizophrenia than in healthy individuals, which may reflect fetal disruptions in development between weeks 14 and 26. This finding was more common among offspring of mothers exposed during this period of their pregnancy, compared with children of mothers exposed during a different period (Dev. Psychopathol. 2009;21:343-53).
Dr. King and her group believe that much of the effect of maternal prenatal stress on an offspring’s cognition and emotional development is a result of direct effects on the fetal brain. In fact, when computational analysis of high-resolution structural magnetic resonance images was used to assess individual and group differences in brain structure, there was a decrease in hippocampal volume observed in boys, but not in girls. "The hippocampus is the part of the brain that is involved in stress reaction, memory, and emotions," she explained.
Similarly, an analysis of breastfed versus nonbreastfed infants during and after the ice storm showed a link between breastfeeding and decreased hippocampal volume, decreased salivary cortisol stress response, and increased internalizing problems in offspring aged 11.5 years, the group reported in a poster at the meeting.
Session chair Yael Danieli, Ph.D., said Dr. King’s study underscores the necessity of taking a full family history when assessing cognitive and psychological problems. "For a complete assessment of a human being’s state of health, one has to know a full history of trauma of prior generations," Dr. Danieli, a New York clinical psychologist, past president of the ISTSS, and editor of the International Handbook of Multigenerational Legacies of Trauma (1988), said in an interview.
But another presenter in the session urged caution. "I do believe fetuses are sensitive to maternal stress but in a complex way," said Cécile Rousseau, M.D., associate professor of psychiatry at McGill. "In some studies, the more a family has been exposed to stress, the better the kids are doing. We should build complex models because these are huge stresses. Let’s look for links for autism and schizophrenia, but let’s be very, very careful. My gut feeling is there are relationships but this is utterly complex."
The investigators have no commercial relationships.
MONTREAL – Cognitive, behavioral, and physical problems still persist today in a group of children exposed to prenatal stress during the Quebec ice storm of January 1998, according to research presented at the annual meeting of the International Society for Traumatic Stress Studies.
"The fetus is not immune to a certain amount of stress, which can be transmitted – probably biologically – from the mother, with resulting cognitive, emotional, physical, and motor development problems," reported Suzanne King, Ph.D., associate professor of psychiatry at McGill University and director of the psychosocial research division of the Douglas Hospital, both in Montreal.
The study measured subjective stress and objective hardship in 150 women during the ice storm, which was described as "the worst natural disaster in Canadian history" by the Insurance Bureau of Canada.
During the midwinter storm, 3 million people were left with no electricity, some for as long as 45 days, and 454 shelters were set up to house more than 17,000 people.
The study is the first prospective analysis of the effects of stress from a natural disaster on pregnant women and their children, said Dr. King. It used questionnaires to measure subjective and objective maternal stress during the storm, and then followed the offspring at 6 months, 2 years, 5.5 years, and 11.5 years.
From a sample of 1,440 women, only 224 responded (15%), and 150 completed the study. "Our resulting sample ended up being a highly educated group with a higher socioeconomic standard than average, which adds significance to the findings," she said.
On average, women in the study were without electricity for 15 days (range, 0-45) and without telephone contact for 4 days (range, 0-34). Two-thirds of them were forced to leave their homes during the storm, and possible posttraumatic stress disorder was present in 4%-17%, said Dr. King.
Although the rates of postpartum depression and premature birth (before 37 weeks) were within normal ranges at 17% and 8%, respectively, there was evidence of compromised cognitive development in the offspring at 2 years, with an odds ratio of 4.4 for delayed development in offspring exposed to high versus low levels of maternal objective stress. "This was controlling for subjective stress, which did not have a significant impact on this outcome. This was objective stress – just the facts – what happened to them," she said.
Additionally, at 2 years, there was a 10-point difference in IQ levels between these two sets of offspring, and these differences persisted at 8.5 years, the most recent data available.
In terms of subjective stress, high levels of maternal subjective stress were associated with increasing levels of offspring internalizing problems such as anxiety and depression, and externalizing problems such as aggression, she added.
"The kids are doing very well because they are from such highly resourced families – their IQs are still quite high, they’re above average – but even in these families we see this significant effect."
Additionally, an analysis of autisticlike symptoms at 6.5 years showed an interaction between both maternal stress and trimester of pregnancy. "For kids who were exposed to stress during the first trimester only, there were increasingly severe autisticlike symptoms with increasing objective stress. None of these kids are autistic, or even close, but in terms of these types of traits we are seeing an effect."
The researchers also examined dermatoglyphic asymmetry of fingertip ridges, a characteristic found more commonly in schizophrenia than in healthy individuals, which may reflect fetal disruptions in development between weeks 14 and 26. This finding was more common among offspring of mothers exposed during this period of their pregnancy, compared with children of mothers exposed during a different period (Dev. Psychopathol. 2009;21:343-53).
Dr. King and her group believe that much of the effect of maternal prenatal stress on an offspring’s cognition and emotional development is a result of direct effects on the fetal brain. In fact, when computational analysis of high-resolution structural magnetic resonance images was used to assess individual and group differences in brain structure, there was a decrease in hippocampal volume observed in boys, but not in girls. "The hippocampus is the part of the brain that is involved in stress reaction, memory, and emotions," she explained.
Similarly, an analysis of breastfed versus nonbreastfed infants during and after the ice storm showed a link between breastfeeding and decreased hippocampal volume, decreased salivary cortisol stress response, and increased internalizing problems in offspring aged 11.5 years, the group reported in a poster at the meeting.
Session chair Yael Danieli, Ph.D., said Dr. King’s study underscores the necessity of taking a full family history when assessing cognitive and psychological problems. "For a complete assessment of a human being’s state of health, one has to know a full history of trauma of prior generations," Dr. Danieli, a New York clinical psychologist, past president of the ISTSS, and editor of the International Handbook of Multigenerational Legacies of Trauma (1988), said in an interview.
But another presenter in the session urged caution. "I do believe fetuses are sensitive to maternal stress but in a complex way," said Cécile Rousseau, M.D., associate professor of psychiatry at McGill. "In some studies, the more a family has been exposed to stress, the better the kids are doing. We should build complex models because these are huge stresses. Let’s look for links for autism and schizophrenia, but let’s be very, very careful. My gut feeling is there are relationships but this is utterly complex."
The investigators have no commercial relationships.
MONTREAL – Cognitive, behavioral, and physical problems still persist today in a group of children exposed to prenatal stress during the Quebec ice storm of January 1998, according to research presented at the annual meeting of the International Society for Traumatic Stress Studies.
"The fetus is not immune to a certain amount of stress, which can be transmitted – probably biologically – from the mother, with resulting cognitive, emotional, physical, and motor development problems," reported Suzanne King, Ph.D., associate professor of psychiatry at McGill University and director of the psychosocial research division of the Douglas Hospital, both in Montreal.
The study measured subjective stress and objective hardship in 150 women during the ice storm, which was described as "the worst natural disaster in Canadian history" by the Insurance Bureau of Canada.
During the midwinter storm, 3 million people were left with no electricity, some for as long as 45 days, and 454 shelters were set up to house more than 17,000 people.
The study is the first prospective analysis of the effects of stress from a natural disaster on pregnant women and their children, said Dr. King. It used questionnaires to measure subjective and objective maternal stress during the storm, and then followed the offspring at 6 months, 2 years, 5.5 years, and 11.5 years.
From a sample of 1,440 women, only 224 responded (15%), and 150 completed the study. "Our resulting sample ended up being a highly educated group with a higher socioeconomic standard than average, which adds significance to the findings," she said.
On average, women in the study were without electricity for 15 days (range, 0-45) and without telephone contact for 4 days (range, 0-34). Two-thirds of them were forced to leave their homes during the storm, and possible posttraumatic stress disorder was present in 4%-17%, said Dr. King.
Although the rates of postpartum depression and premature birth (before 37 weeks) were within normal ranges at 17% and 8%, respectively, there was evidence of compromised cognitive development in the offspring at 2 years, with an odds ratio of 4.4 for delayed development in offspring exposed to high versus low levels of maternal objective stress. "This was controlling for subjective stress, which did not have a significant impact on this outcome. This was objective stress – just the facts – what happened to them," she said.
Additionally, at 2 years, there was a 10-point difference in IQ levels between these two sets of offspring, and these differences persisted at 8.5 years, the most recent data available.
In terms of subjective stress, high levels of maternal subjective stress were associated with increasing levels of offspring internalizing problems such as anxiety and depression, and externalizing problems such as aggression, she added.
"The kids are doing very well because they are from such highly resourced families – their IQs are still quite high, they’re above average – but even in these families we see this significant effect."
Additionally, an analysis of autisticlike symptoms at 6.5 years showed an interaction between both maternal stress and trimester of pregnancy. "For kids who were exposed to stress during the first trimester only, there were increasingly severe autisticlike symptoms with increasing objective stress. None of these kids are autistic, or even close, but in terms of these types of traits we are seeing an effect."
The researchers also examined dermatoglyphic asymmetry of fingertip ridges, a characteristic found more commonly in schizophrenia than in healthy individuals, which may reflect fetal disruptions in development between weeks 14 and 26. This finding was more common among offspring of mothers exposed during this period of their pregnancy, compared with children of mothers exposed during a different period (Dev. Psychopathol. 2009;21:343-53).
Dr. King and her group believe that much of the effect of maternal prenatal stress on an offspring’s cognition and emotional development is a result of direct effects on the fetal brain. In fact, when computational analysis of high-resolution structural magnetic resonance images was used to assess individual and group differences in brain structure, there was a decrease in hippocampal volume observed in boys, but not in girls. "The hippocampus is the part of the brain that is involved in stress reaction, memory, and emotions," she explained.
Similarly, an analysis of breastfed versus nonbreastfed infants during and after the ice storm showed a link between breastfeeding and decreased hippocampal volume, decreased salivary cortisol stress response, and increased internalizing problems in offspring aged 11.5 years, the group reported in a poster at the meeting.
Session chair Yael Danieli, Ph.D., said Dr. King’s study underscores the necessity of taking a full family history when assessing cognitive and psychological problems. "For a complete assessment of a human being’s state of health, one has to know a full history of trauma of prior generations," Dr. Danieli, a New York clinical psychologist, past president of the ISTSS, and editor of the International Handbook of Multigenerational Legacies of Trauma (1988), said in an interview.
But another presenter in the session urged caution. "I do believe fetuses are sensitive to maternal stress but in a complex way," said Cécile Rousseau, M.D., associate professor of psychiatry at McGill. "In some studies, the more a family has been exposed to stress, the better the kids are doing. We should build complex models because these are huge stresses. Let’s look for links for autism and schizophrenia, but let’s be very, very careful. My gut feeling is there are relationships but this is utterly complex."
The investigators have no commercial relationships.
FROM THE ANNUAL MEETING OF THE INTERNATIONAL SOCIETY FOR TRAUMATIC STRESS STUDIES
Major Finding: An increase in cognitive, behavioral, and physical problems was seen among offspring of women who were pregnant during or immediately after a natural disaster.
Data Source: A total of 150 children whose mothers were pregnant during or immediately after the Quebec ice storm of January 1998.
Disclosures: The investigators have no commercial relationships.
Quality of Life Declined After Brain Radiotherapy
Major Finding: Global HRQOL scores at 9 months were significantly worse in patients who received WBRT than in those who underwent observation alone (52.2 vs. 63.2, respectively).
Data Source: Randomized trial of 359 patients who underwent either observation or adjuvant whole-brain radiotherapy after surgical or radiosurgical resection of between 1 and 3 brain metastases.
Disclosures: The European Organization for Research and Treatment of Cancer sponsored the trial. Dr. Soffietti did not offer disclosure information.
MONTREAL – Adjuvant whole-brain radiotherapy following surgical or radiosurgical resection of brain metastases provided no survival benefit and modestly reduced health-related quality of life when compared with close MRI observation alone in a randomized study of 359 patients.
The worsening of health-related quality of life with whole-brain radiotherapy (WBRT) was slight and transient, first author Dr. Riccardo Soffietti said at the annual meeting of the Society for Neuro-Oncology. He noted that few scores “reached clinical or statistical significance, and most scores that differed significantly at the first time-point had a tendency to recover over time.”
The study was a secondary analysis of a phase III study in which patients were randomized to receive WBRT (180 patients) or undergo observation with MRI every 3 months (179) after undergoing surgery or radiosurgery for one to three brain metastases. The primary results of the study were published online in the Journal of Clinical Oncology (doi:10.1200/JCO.2010.30.1655).
For the primary outcome of overall survival at 1 year, there was no difference in between the WBRT (median of 10.9 months) and observation groups (10.7 months). Both groups also had a similar degree of functional independence.
There was a modest increase in progression-free survival in the WBRT group “probably due to their significant reduction in intracranial progression,” said Dr. Soffietti, professor of neuro-oncology at the University of Torino (Italy).
Intracranial progression causing death occurred in 28% of the WBRT group, compared with 44% of the observation group.
For the secondary end point of health-related quality of life (HRQOL), there was low patient compliance in completing the brain-specific questionnaires QLQ-C30 and BN-20. Only 315 (88%) of the participants completed baseline assessments, while many fewer completed 6-month (51%) or 1-year assessments (45%).
Among the patients for whom all assessments were available, Dr. Soffietti and his colleagues noted “a statistically significant and clinically relevant difference between the two arms at 9 months favoring patients who did not receive whole-brain radiation therapy.” However, the difference in global HRQOL scores at that time (52.2 in the WBRT group and 63.2 in the observation group) was only transitory and was not maintained by the 1-year mark.
Major Finding: Global HRQOL scores at 9 months were significantly worse in patients who received WBRT than in those who underwent observation alone (52.2 vs. 63.2, respectively).
Data Source: Randomized trial of 359 patients who underwent either observation or adjuvant whole-brain radiotherapy after surgical or radiosurgical resection of between 1 and 3 brain metastases.
Disclosures: The European Organization for Research and Treatment of Cancer sponsored the trial. Dr. Soffietti did not offer disclosure information.
MONTREAL – Adjuvant whole-brain radiotherapy following surgical or radiosurgical resection of brain metastases provided no survival benefit and modestly reduced health-related quality of life when compared with close MRI observation alone in a randomized study of 359 patients.
The worsening of health-related quality of life with whole-brain radiotherapy (WBRT) was slight and transient, first author Dr. Riccardo Soffietti said at the annual meeting of the Society for Neuro-Oncology. He noted that few scores “reached clinical or statistical significance, and most scores that differed significantly at the first time-point had a tendency to recover over time.”
The study was a secondary analysis of a phase III study in which patients were randomized to receive WBRT (180 patients) or undergo observation with MRI every 3 months (179) after undergoing surgery or radiosurgery for one to three brain metastases. The primary results of the study were published online in the Journal of Clinical Oncology (doi:10.1200/JCO.2010.30.1655).
For the primary outcome of overall survival at 1 year, there was no difference in between the WBRT (median of 10.9 months) and observation groups (10.7 months). Both groups also had a similar degree of functional independence.
There was a modest increase in progression-free survival in the WBRT group “probably due to their significant reduction in intracranial progression,” said Dr. Soffietti, professor of neuro-oncology at the University of Torino (Italy).
Intracranial progression causing death occurred in 28% of the WBRT group, compared with 44% of the observation group.
For the secondary end point of health-related quality of life (HRQOL), there was low patient compliance in completing the brain-specific questionnaires QLQ-C30 and BN-20. Only 315 (88%) of the participants completed baseline assessments, while many fewer completed 6-month (51%) or 1-year assessments (45%).
Among the patients for whom all assessments were available, Dr. Soffietti and his colleagues noted “a statistically significant and clinically relevant difference between the two arms at 9 months favoring patients who did not receive whole-brain radiation therapy.” However, the difference in global HRQOL scores at that time (52.2 in the WBRT group and 63.2 in the observation group) was only transitory and was not maintained by the 1-year mark.
Major Finding: Global HRQOL scores at 9 months were significantly worse in patients who received WBRT than in those who underwent observation alone (52.2 vs. 63.2, respectively).
Data Source: Randomized trial of 359 patients who underwent either observation or adjuvant whole-brain radiotherapy after surgical or radiosurgical resection of between 1 and 3 brain metastases.
Disclosures: The European Organization for Research and Treatment of Cancer sponsored the trial. Dr. Soffietti did not offer disclosure information.
MONTREAL – Adjuvant whole-brain radiotherapy following surgical or radiosurgical resection of brain metastases provided no survival benefit and modestly reduced health-related quality of life when compared with close MRI observation alone in a randomized study of 359 patients.
The worsening of health-related quality of life with whole-brain radiotherapy (WBRT) was slight and transient, first author Dr. Riccardo Soffietti said at the annual meeting of the Society for Neuro-Oncology. He noted that few scores “reached clinical or statistical significance, and most scores that differed significantly at the first time-point had a tendency to recover over time.”
The study was a secondary analysis of a phase III study in which patients were randomized to receive WBRT (180 patients) or undergo observation with MRI every 3 months (179) after undergoing surgery or radiosurgery for one to three brain metastases. The primary results of the study were published online in the Journal of Clinical Oncology (doi:10.1200/JCO.2010.30.1655).
For the primary outcome of overall survival at 1 year, there was no difference in between the WBRT (median of 10.9 months) and observation groups (10.7 months). Both groups also had a similar degree of functional independence.
There was a modest increase in progression-free survival in the WBRT group “probably due to their significant reduction in intracranial progression,” said Dr. Soffietti, professor of neuro-oncology at the University of Torino (Italy).
Intracranial progression causing death occurred in 28% of the WBRT group, compared with 44% of the observation group.
For the secondary end point of health-related quality of life (HRQOL), there was low patient compliance in completing the brain-specific questionnaires QLQ-C30 and BN-20. Only 315 (88%) of the participants completed baseline assessments, while many fewer completed 6-month (51%) or 1-year assessments (45%).
Among the patients for whom all assessments were available, Dr. Soffietti and his colleagues noted “a statistically significant and clinically relevant difference between the two arms at 9 months favoring patients who did not receive whole-brain radiation therapy.” However, the difference in global HRQOL scores at that time (52.2 in the WBRT group and 63.2 in the observation group) was only transitory and was not maintained by the 1-year mark.
New Drugs Deter Progression in Recurrent Meningioma
Major Finding: Two phase II studies of vatalanib and sunitinib showed 6-month progression-free survival rates of 57% and 36%, respectively.
Data Source: Two cohorts of 25 and 36 patients with recurrent grade II and III meningiomas.
Disclosures: Pfizer funded the study on its drug, sunitinib, and Novartis funded the study on its investigational drug, vatalanib. The investigators did not provide financial disclosure information at the meeting and did not respond to inquiries about disclosures.
MONTREAL – The tyrosine kinase inhibitors vatalanib and sunitinib may offer alternative approaches to treating patients with recurrent, high-grade meningioma who have failed surgery and radiation therapy, according to two separate phase II studies.
Both drugs significantly improved survival compared with what is generally expected in this patient population, most of whom had grade II or III tumors. Progression-free survival at 6 months occurred in 57% of 25 patients with meningioma who received the investigational drug vatalanib in one study, and in 36% of 36 patients who received sunitinib in another study. Both drugs are inhibitors of receptors for vascular endothelial growth factor and platelet-derived growth factor.
Sunitinib is marketed under the brand name Sutent and has been approved by the Food and Drug Administration for the treatment of advanced renal cell carcinoma and gastrointestinal stromal tumor after disease progression on – or intolerance to – imatinib mesylate (Gleevec).
Progression-free survival (PFS) for patients with recurrent grade II and III tumors is usually considered to occur in fewer than 5%, said Dr. Jeffrey Raizer, who presented the vatalanib study at the meeting.
“For recurrence of meningioma, treatment options are limited once patients have failed surgery and radiation, and chemotherapies have been very limited to date,” said Dr. Raizer, director of medical neuro-oncology at the cancer center of Northwestern University and Northwestern Memorial Hospital, both in Chicago.
Despite the encouraging findings of the two studies, a lack of information on the natural history of these tumors makes it difficult to interpret the studies, said Dr. Michael Vogelbaum, who chaired the session in which the studies were presented.
“While the studies suggest there may be some promise, we don't really know what to expect from that mix of grade II and III tumors on their own,” Dr. Vogelbaum said in an interview. He is chair of neuro-oncology at the Cleveland Clinic Neurological Institute.
Dr. Fred Barker of the department of neurosurgery at Massachusetts General Hospital, Boston, echoed Dr. Vogelbaum's comments. “The results are interesting, but we don't know exactly what the natural history would be without treatment, so whether there's a benefit to giving these drugs will require further study.”
In Dr. Raizer's Pfizer-sponsored study of vatalanib in meningioma patients, the median PFS was 5.9 months, and the median overall survival was 22.3 months. Of the 25 patients in the study, 22 had grade II and III tumors and 14 were men. The PFS at 6 months was comparable between patients with grade II (39%) or grade III disease only (43%).
Dosing of vatalanib began at 250 mg twice daily and rose by 250 mg/day every 7 days until it reached 500 mg twice daily.
For 21 patients with available imaging data, tumors partially responded to treatment in 1, remained stable in 15, and progressed in 5 patients.
The most common adverse events were fatigue, rash, and elevated transaminases.
The sunitinib study, sponsored by Novartis, included 36 patients (median age, 62 years) with recurrent grade II and III meningiomas who had exhausted all surgical and radiation options. The patients had a median of five recurrences.
The primary end point of PFS at 6 months was 36% and the median PFS was 5.1 months. The overall survival rate is not known, as only eight patients have died, reported Dr. Thomas Kaley, codirector of the neuro-oncology fellowship program at Memorial Sloan-Kettering Cancer Center in New York.
Imaging was available for 34 patients and showed stable disease in 26, a partial response in 1, and progressive disease in 7 patients, he said. The dose of sunitinib was 50 mg/day orally on a 4-week-on, 2-week-off cycle.
Major Finding: Two phase II studies of vatalanib and sunitinib showed 6-month progression-free survival rates of 57% and 36%, respectively.
Data Source: Two cohorts of 25 and 36 patients with recurrent grade II and III meningiomas.
Disclosures: Pfizer funded the study on its drug, sunitinib, and Novartis funded the study on its investigational drug, vatalanib. The investigators did not provide financial disclosure information at the meeting and did not respond to inquiries about disclosures.
MONTREAL – The tyrosine kinase inhibitors vatalanib and sunitinib may offer alternative approaches to treating patients with recurrent, high-grade meningioma who have failed surgery and radiation therapy, according to two separate phase II studies.
Both drugs significantly improved survival compared with what is generally expected in this patient population, most of whom had grade II or III tumors. Progression-free survival at 6 months occurred in 57% of 25 patients with meningioma who received the investigational drug vatalanib in one study, and in 36% of 36 patients who received sunitinib in another study. Both drugs are inhibitors of receptors for vascular endothelial growth factor and platelet-derived growth factor.
Sunitinib is marketed under the brand name Sutent and has been approved by the Food and Drug Administration for the treatment of advanced renal cell carcinoma and gastrointestinal stromal tumor after disease progression on – or intolerance to – imatinib mesylate (Gleevec).
Progression-free survival (PFS) for patients with recurrent grade II and III tumors is usually considered to occur in fewer than 5%, said Dr. Jeffrey Raizer, who presented the vatalanib study at the meeting.
“For recurrence of meningioma, treatment options are limited once patients have failed surgery and radiation, and chemotherapies have been very limited to date,” said Dr. Raizer, director of medical neuro-oncology at the cancer center of Northwestern University and Northwestern Memorial Hospital, both in Chicago.
Despite the encouraging findings of the two studies, a lack of information on the natural history of these tumors makes it difficult to interpret the studies, said Dr. Michael Vogelbaum, who chaired the session in which the studies were presented.
“While the studies suggest there may be some promise, we don't really know what to expect from that mix of grade II and III tumors on their own,” Dr. Vogelbaum said in an interview. He is chair of neuro-oncology at the Cleveland Clinic Neurological Institute.
Dr. Fred Barker of the department of neurosurgery at Massachusetts General Hospital, Boston, echoed Dr. Vogelbaum's comments. “The results are interesting, but we don't know exactly what the natural history would be without treatment, so whether there's a benefit to giving these drugs will require further study.”
In Dr. Raizer's Pfizer-sponsored study of vatalanib in meningioma patients, the median PFS was 5.9 months, and the median overall survival was 22.3 months. Of the 25 patients in the study, 22 had grade II and III tumors and 14 were men. The PFS at 6 months was comparable between patients with grade II (39%) or grade III disease only (43%).
Dosing of vatalanib began at 250 mg twice daily and rose by 250 mg/day every 7 days until it reached 500 mg twice daily.
For 21 patients with available imaging data, tumors partially responded to treatment in 1, remained stable in 15, and progressed in 5 patients.
The most common adverse events were fatigue, rash, and elevated transaminases.
The sunitinib study, sponsored by Novartis, included 36 patients (median age, 62 years) with recurrent grade II and III meningiomas who had exhausted all surgical and radiation options. The patients had a median of five recurrences.
The primary end point of PFS at 6 months was 36% and the median PFS was 5.1 months. The overall survival rate is not known, as only eight patients have died, reported Dr. Thomas Kaley, codirector of the neuro-oncology fellowship program at Memorial Sloan-Kettering Cancer Center in New York.
Imaging was available for 34 patients and showed stable disease in 26, a partial response in 1, and progressive disease in 7 patients, he said. The dose of sunitinib was 50 mg/day orally on a 4-week-on, 2-week-off cycle.
Major Finding: Two phase II studies of vatalanib and sunitinib showed 6-month progression-free survival rates of 57% and 36%, respectively.
Data Source: Two cohorts of 25 and 36 patients with recurrent grade II and III meningiomas.
Disclosures: Pfizer funded the study on its drug, sunitinib, and Novartis funded the study on its investigational drug, vatalanib. The investigators did not provide financial disclosure information at the meeting and did not respond to inquiries about disclosures.
MONTREAL – The tyrosine kinase inhibitors vatalanib and sunitinib may offer alternative approaches to treating patients with recurrent, high-grade meningioma who have failed surgery and radiation therapy, according to two separate phase II studies.
Both drugs significantly improved survival compared with what is generally expected in this patient population, most of whom had grade II or III tumors. Progression-free survival at 6 months occurred in 57% of 25 patients with meningioma who received the investigational drug vatalanib in one study, and in 36% of 36 patients who received sunitinib in another study. Both drugs are inhibitors of receptors for vascular endothelial growth factor and platelet-derived growth factor.
Sunitinib is marketed under the brand name Sutent and has been approved by the Food and Drug Administration for the treatment of advanced renal cell carcinoma and gastrointestinal stromal tumor after disease progression on – or intolerance to – imatinib mesylate (Gleevec).
Progression-free survival (PFS) for patients with recurrent grade II and III tumors is usually considered to occur in fewer than 5%, said Dr. Jeffrey Raizer, who presented the vatalanib study at the meeting.
“For recurrence of meningioma, treatment options are limited once patients have failed surgery and radiation, and chemotherapies have been very limited to date,” said Dr. Raizer, director of medical neuro-oncology at the cancer center of Northwestern University and Northwestern Memorial Hospital, both in Chicago.
Despite the encouraging findings of the two studies, a lack of information on the natural history of these tumors makes it difficult to interpret the studies, said Dr. Michael Vogelbaum, who chaired the session in which the studies were presented.
“While the studies suggest there may be some promise, we don't really know what to expect from that mix of grade II and III tumors on their own,” Dr. Vogelbaum said in an interview. He is chair of neuro-oncology at the Cleveland Clinic Neurological Institute.
Dr. Fred Barker of the department of neurosurgery at Massachusetts General Hospital, Boston, echoed Dr. Vogelbaum's comments. “The results are interesting, but we don't know exactly what the natural history would be without treatment, so whether there's a benefit to giving these drugs will require further study.”
In Dr. Raizer's Pfizer-sponsored study of vatalanib in meningioma patients, the median PFS was 5.9 months, and the median overall survival was 22.3 months. Of the 25 patients in the study, 22 had grade II and III tumors and 14 were men. The PFS at 6 months was comparable between patients with grade II (39%) or grade III disease only (43%).
Dosing of vatalanib began at 250 mg twice daily and rose by 250 mg/day every 7 days until it reached 500 mg twice daily.
For 21 patients with available imaging data, tumors partially responded to treatment in 1, remained stable in 15, and progressed in 5 patients.
The most common adverse events were fatigue, rash, and elevated transaminases.
The sunitinib study, sponsored by Novartis, included 36 patients (median age, 62 years) with recurrent grade II and III meningiomas who had exhausted all surgical and radiation options. The patients had a median of five recurrences.
The primary end point of PFS at 6 months was 36% and the median PFS was 5.1 months. The overall survival rate is not known, as only eight patients have died, reported Dr. Thomas Kaley, codirector of the neuro-oncology fellowship program at Memorial Sloan-Kettering Cancer Center in New York.
Imaging was available for 34 patients and showed stable disease in 26, a partial response in 1, and progressive disease in 7 patients, he said. The dose of sunitinib was 50 mg/day orally on a 4-week-on, 2-week-off cycle.
Temozolomide for Glioblastoma Benefits Elderly
Major Finding: More than half of patients with a median Karnofsky performance score of 60 improved their score by at least 10 points.
Data Source: A group of 70 elderly, poor-performance patients, treated with postsurgical temozolomide for newly diagnosed glioblastoma.
Disclosures: Dr. Pérez-Larraya reported having no relevant financial disclosures.
MONTREAL – Elderly patients with newly diagnosed glioblastoma and poor Karnofsky performance scores can benefit from postsurgical chemotherapy with temozolomide, based on the results of a single-arm study in 70 patients.
Most patients were able to withstand treatment-related toxicity, and survival rates and performance status appeared to improve with treatment, Dr. Jamie Gállego Pérez-Larraya said at the meetingo
Median overall survival, the primary end point, reached 25 weeks, with a 6-month overall survival rate of 44.3% and a 12-month rate of 11.4%, said Dr. Pérez-Larraya of Hôpital Pitié-Salpêtrière in Paris. Median progression-free survival, a secondary end point, was 16 weeks, with a 6-month rate of 30%. “These data compare favorably to the 17-week median survival reported in elderly patients with glioblastoma and good performance treated only with palliative care,” he said.
The trial from ANOCEF (Association des Neuro-Oncologues d'Expression Française) enrolled 70 patients aged 70 and up (median age, 77 years), with newly diagnosed and histologically confirmed glioblastoma, a median Karnofsky performance score of 60, and no previous radiotherapy or chemotherapy for the brain tumor. Most (92%) had undergone biopsy of their tumor; five patients had received a partial resection, and one had a complete resection.
Temozolomide chemotherapy started at 150 mg/m
Quality of life (QOL) and cognitive function outcomes were measured by EORTC (European Organisation for Research and Treatment of Cancer) questionnaires (QLQ-C30 and QLQ-BN20), and the Mini-Mental State Examination. The stuidy showed significant improvements on the global QOL scale and most functioning domains, with no decline in any domain, he said.
A third of the cohort improved in Karnofsky performance scores by at least 10 points, and 26% achieved a score of 70 or greater. “This is clinically significant because it means they became capable of self-care,” he noted.
Treatment with temozolomide was “generally well tolerated,” Dr. Pérez-Larraya reported. Twelve patients, (17%) had grade 3 or 4 thrombocytopenia or neutropenia, but these toxicities did not lead to dose delays or dose reductions. All of the cohort had died by the time of presentation – 87% as a result of disease progression, and 13% from other causes, with no deaths due to toxicity.
“Until a few years ago the treatment of these patients received little attention mainly because of their poor expected survival, but also because of the fear of treatment-related toxicity,” said Dr. Pérez-Larraya. Now patients with good performance scores can be treated with postsurgical radiotherapy, which has been shown to prolong survival from 17 weeks to 29 weeks without causing deterioration in QOL or cognitive function (N. Engl. J. Med. 2007;356(1527-35). But management of patients with poor scores has never been studied, he said. “Radiotherapy requires many trips to the hospital, and increasing fatigue makes this difficult for these severely impaired patients with such a short expected survival,” he said.
The results suggest that temozolomide in elderly patients with glioblastoma and poor performance scores “has an acceptable safety profile; is associated with an improvement in functional status in one-third of cases, and quality of life before progression; and seems to increase survival as compared to supportive care alone,” Dr. Pérez-Larraya concluded.
View on the News
Therapeutic Nihilism Unnecessary
This study clearly shows the acceptable toxicity and benefit of temozolomide in the treatment of elderly patients with low performance scores who received this drug after surgery for newly diagnosed glioblastoma. Temozolomide appeared to improve both survival rates and performance.
The findings highlight the need to get rid of the nihilistic approach toward this population, all too frequently relegated to hospice without any attempt at therapy. The toxicity was small and the benefits were real, a lesson all physicians caring for the elderly with glioblastoma should remember.
DR. HENRY S. FRIEDMAN is a professor of neuro-oncology and deputy director of the Preston Robert Tisch Brain Tumor Center at Duke University, Durham, N.C. He also serves as an advisor to Genentech.
Vitals
Major Finding: More than half of patients with a median Karnofsky performance score of 60 improved their score by at least 10 points.
Data Source: A group of 70 elderly, poor-performance patients, treated with postsurgical temozolomide for newly diagnosed glioblastoma.
Disclosures: Dr. Pérez-Larraya reported having no relevant financial disclosures.
MONTREAL – Elderly patients with newly diagnosed glioblastoma and poor Karnofsky performance scores can benefit from postsurgical chemotherapy with temozolomide, based on the results of a single-arm study in 70 patients.
Most patients were able to withstand treatment-related toxicity, and survival rates and performance status appeared to improve with treatment, Dr. Jamie Gállego Pérez-Larraya said at the meetingo
Median overall survival, the primary end point, reached 25 weeks, with a 6-month overall survival rate of 44.3% and a 12-month rate of 11.4%, said Dr. Pérez-Larraya of Hôpital Pitié-Salpêtrière in Paris. Median progression-free survival, a secondary end point, was 16 weeks, with a 6-month rate of 30%. “These data compare favorably to the 17-week median survival reported in elderly patients with glioblastoma and good performance treated only with palliative care,” he said.
The trial from ANOCEF (Association des Neuro-Oncologues d'Expression Française) enrolled 70 patients aged 70 and up (median age, 77 years), with newly diagnosed and histologically confirmed glioblastoma, a median Karnofsky performance score of 60, and no previous radiotherapy or chemotherapy for the brain tumor. Most (92%) had undergone biopsy of their tumor; five patients had received a partial resection, and one had a complete resection.
Temozolomide chemotherapy started at 150 mg/m
Quality of life (QOL) and cognitive function outcomes were measured by EORTC (European Organisation for Research and Treatment of Cancer) questionnaires (QLQ-C30 and QLQ-BN20), and the Mini-Mental State Examination. The stuidy showed significant improvements on the global QOL scale and most functioning domains, with no decline in any domain, he said.
A third of the cohort improved in Karnofsky performance scores by at least 10 points, and 26% achieved a score of 70 or greater. “This is clinically significant because it means they became capable of self-care,” he noted.
Treatment with temozolomide was “generally well tolerated,” Dr. Pérez-Larraya reported. Twelve patients, (17%) had grade 3 or 4 thrombocytopenia or neutropenia, but these toxicities did not lead to dose delays or dose reductions. All of the cohort had died by the time of presentation – 87% as a result of disease progression, and 13% from other causes, with no deaths due to toxicity.
“Until a few years ago the treatment of these patients received little attention mainly because of their poor expected survival, but also because of the fear of treatment-related toxicity,” said Dr. Pérez-Larraya. Now patients with good performance scores can be treated with postsurgical radiotherapy, which has been shown to prolong survival from 17 weeks to 29 weeks without causing deterioration in QOL or cognitive function (N. Engl. J. Med. 2007;356(1527-35). But management of patients with poor scores has never been studied, he said. “Radiotherapy requires many trips to the hospital, and increasing fatigue makes this difficult for these severely impaired patients with such a short expected survival,” he said.
The results suggest that temozolomide in elderly patients with glioblastoma and poor performance scores “has an acceptable safety profile; is associated with an improvement in functional status in one-third of cases, and quality of life before progression; and seems to increase survival as compared to supportive care alone,” Dr. Pérez-Larraya concluded.
View on the News
Therapeutic Nihilism Unnecessary
This study clearly shows the acceptable toxicity and benefit of temozolomide in the treatment of elderly patients with low performance scores who received this drug after surgery for newly diagnosed glioblastoma. Temozolomide appeared to improve both survival rates and performance.
The findings highlight the need to get rid of the nihilistic approach toward this population, all too frequently relegated to hospice without any attempt at therapy. The toxicity was small and the benefits were real, a lesson all physicians caring for the elderly with glioblastoma should remember.
DR. HENRY S. FRIEDMAN is a professor of neuro-oncology and deputy director of the Preston Robert Tisch Brain Tumor Center at Duke University, Durham, N.C. He also serves as an advisor to Genentech.
Vitals
Major Finding: More than half of patients with a median Karnofsky performance score of 60 improved their score by at least 10 points.
Data Source: A group of 70 elderly, poor-performance patients, treated with postsurgical temozolomide for newly diagnosed glioblastoma.
Disclosures: Dr. Pérez-Larraya reported having no relevant financial disclosures.
MONTREAL – Elderly patients with newly diagnosed glioblastoma and poor Karnofsky performance scores can benefit from postsurgical chemotherapy with temozolomide, based on the results of a single-arm study in 70 patients.
Most patients were able to withstand treatment-related toxicity, and survival rates and performance status appeared to improve with treatment, Dr. Jamie Gállego Pérez-Larraya said at the meetingo
Median overall survival, the primary end point, reached 25 weeks, with a 6-month overall survival rate of 44.3% and a 12-month rate of 11.4%, said Dr. Pérez-Larraya of Hôpital Pitié-Salpêtrière in Paris. Median progression-free survival, a secondary end point, was 16 weeks, with a 6-month rate of 30%. “These data compare favorably to the 17-week median survival reported in elderly patients with glioblastoma and good performance treated only with palliative care,” he said.
The trial from ANOCEF (Association des Neuro-Oncologues d'Expression Française) enrolled 70 patients aged 70 and up (median age, 77 years), with newly diagnosed and histologically confirmed glioblastoma, a median Karnofsky performance score of 60, and no previous radiotherapy or chemotherapy for the brain tumor. Most (92%) had undergone biopsy of their tumor; five patients had received a partial resection, and one had a complete resection.
Temozolomide chemotherapy started at 150 mg/m
Quality of life (QOL) and cognitive function outcomes were measured by EORTC (European Organisation for Research and Treatment of Cancer) questionnaires (QLQ-C30 and QLQ-BN20), and the Mini-Mental State Examination. The stuidy showed significant improvements on the global QOL scale and most functioning domains, with no decline in any domain, he said.
A third of the cohort improved in Karnofsky performance scores by at least 10 points, and 26% achieved a score of 70 or greater. “This is clinically significant because it means they became capable of self-care,” he noted.
Treatment with temozolomide was “generally well tolerated,” Dr. Pérez-Larraya reported. Twelve patients, (17%) had grade 3 or 4 thrombocytopenia or neutropenia, but these toxicities did not lead to dose delays or dose reductions. All of the cohort had died by the time of presentation – 87% as a result of disease progression, and 13% from other causes, with no deaths due to toxicity.
“Until a few years ago the treatment of these patients received little attention mainly because of their poor expected survival, but also because of the fear of treatment-related toxicity,” said Dr. Pérez-Larraya. Now patients with good performance scores can be treated with postsurgical radiotherapy, which has been shown to prolong survival from 17 weeks to 29 weeks without causing deterioration in QOL or cognitive function (N. Engl. J. Med. 2007;356(1527-35). But management of patients with poor scores has never been studied, he said. “Radiotherapy requires many trips to the hospital, and increasing fatigue makes this difficult for these severely impaired patients with such a short expected survival,” he said.
The results suggest that temozolomide in elderly patients with glioblastoma and poor performance scores “has an acceptable safety profile; is associated with an improvement in functional status in one-third of cases, and quality of life before progression; and seems to increase survival as compared to supportive care alone,” Dr. Pérez-Larraya concluded.
View on the News
Therapeutic Nihilism Unnecessary
This study clearly shows the acceptable toxicity and benefit of temozolomide in the treatment of elderly patients with low performance scores who received this drug after surgery for newly diagnosed glioblastoma. Temozolomide appeared to improve both survival rates and performance.
The findings highlight the need to get rid of the nihilistic approach toward this population, all too frequently relegated to hospice without any attempt at therapy. The toxicity was small and the benefits were real, a lesson all physicians caring for the elderly with glioblastoma should remember.
DR. HENRY S. FRIEDMAN is a professor of neuro-oncology and deputy director of the Preston Robert Tisch Brain Tumor Center at Duke University, Durham, N.C. He also serves as an advisor to Genentech.
Vitals
Device for Glioblastoma May Offer Advantage Over Chemo
Major Finding: 1-year overall survival in a subgroup of patients was significantly higher among those treated with NovoTTF-100A than it was in those who received chemotherapy (35.2% vs. 20.8%).
Data Source: Post hoc subgroup analysis of 237 patients with recurrent glioblastoma.
Disclosures: Dr. Zvi Ram disclosed that he is a consultant for NovoCure, which sponsored the trial and manufactures the device. Dr. Brandes said that she had no relevant financial disclosures.
MONTREAL – An investigational treatment for recurrent glioblastoma that delivers alternating electric fields through scalp electrodes has shown signs of improved survival in a post hoc analysis of results in particular subgroups of patients in a phase III trial.
Quality of life outcomes also favored patients who used the device, known as NovoTTF-100A, compared with those who received chemotherapy.
To date, reports about the device have elicited both antagonistic and enthusiastic reaction from oncologists, with “neither the enthusiasts nor the antagonists having significant basis for either kind of acute reaction,” Dr. Zvi Ram said in an interview after presenting the subgroup analyses at the meetingo “I think it is exciting that we're getting something completely new – a different, noninvasive modality with no side effects. I think we should be exhilarated.”
The device delivers low-amplitude “tumor treatment fields” of 100–300 kHz that have been shown in vitro to slow and reverse tumor cell proliferation by inhibiting mitosis, according to NovoCure Ltd., the manufacturer of the device and sponsor of the trial.
The portable device weighs about 6 pounds and connects to a battery pack. It is designed to be worn almost constantly, with a target of at least 20 hours of use each day.
In a phase III clinical trial presented earlier this year at the American Society of Clinical Oncology, an intent-to-treat analysis comparing NovoTTF vs. best-available chemotherapy found no statistical difference in 1-year overall survival (OS) among 237 recurrent glioblastoma patients randomized to either treatment.
However, a per-protocol analysis (which included only those patients who wore the device for at least 70% of the recommended time during the first month) showed a statistically significant benefit to NovoTTF in 1-year survival, compared with chemotherapy (29.5% vs. 19.1%, respectively; hazard ratio, 0.64; P = .01).
In the new post hoc analysis, a subgroup of 110 patients with a “good prognosis” (aged younger than 60 years, and with a Karnofsky performance status score greater than 80%) showed a “more robust” survival benefit than that seen in the overall intent-to-treat analysis, he said.
In this subgroup, patients treated with NovoTTF had a median survival of 9.2 months, vs. 6.6 months in those treated with chemotherapy (P less than .01). However, in the overall intent-to-treat group, median survival was 6.6 months and 6.0 months, respectively, he explained. Moreover, the 1-year OS in this subgroup was significantly higher in the NovoTTF group than in the chemotherapy group (35.2% vs. 20.8%, respectively; P less than .01), whereas the difference was nonsignificant in the larger analysis (23.6% vs. 20.7%).
Another subgroup analysis looked at patients who had previously failed treatment with bevacizumab (about 20% of the entire cohort). Both an intent-to-treat analysis and a per-protocol analysis showed significant OS advantages to NovoTTF, said Dr. Ram, chair of neurosurgery at Tel Aviv (Israel) Medical Center.
The median OS in 44 patients in the intent-to-treat group was 4 months with NovoTTF vs. 3.1 months with chemotherapy (HR, 0.43; P less than .02). NovoTTF also gave a significantly better median OS among 29 patients in the per-protocol analysis for this subgroup (6.3 months vs. 3.3 months; HR, 0.21; P = .02).
“You don't see this anywhere,” he said. “There's no drug in the world that could produce such response in patients who had already failed” bevacizumab.
The investigators also analyzed a surgery-naive group. “You know these are going to be poor responders, almost identical to [those with] bevacizumab failure,” Dr. Ram commented.
In this group of 38 patients, an intent-to-treat analysis showed that overall survival was 9.8 months with NovoTTF vs. 5.5 months with chemotherapy.
Patients also reported significantly better quality of life with NovoTTF than with chemotherapy. On the Quality of Life Symptom Scale, NovoTTF patients scored −34 and −35 on constipation and diarrhea, compared with scores of +77 and +50 for the chemotherapy group. Nausea and vomiting scores were 15 for the NovoTTF group and 61 for the chemotherapy group, and pain scores were −1 for the NovoTTF group and +63 for the chemotherapy group.
A quality of life analysis using the EORTC (European Organisation for Research and Treatment of Cancer) QLQ-C30 instrument showed scores of 14 vs. −7 in favor of NovoTTF for cognitive functioning, and scores of 7 vs. 1 in favor of NovoTTF for emotional functioning.
“We do this to all our patients. We intoxicate them,” Dr. Ram said. “So even if NovoTTF did not extend survival, if it was equivalent to chemotherapy [for survival], it may still improve quality of life.”
Dr. Ram did not know the median length of time that the NovoTTF cohort wore the device, but an earlier phase II study followed some patients up to 59 months. He noted that “70% are still alive; that's unheard of.”
“There were concerns that patients might have more headaches or seizures, but there were none,” he added.
In the current study, the rate of adverse events related to the central nervous system was similar (66% for NovoTTF and 67% for chemotherapy). Seizures occurred in 15% of the NovoTTF group and 12% of the chemotherapy group, and headaches occurred in 18% and 13%, respectively.
“It's very interesting and exciting, even if we do not yet have enough definitive data,” commented Dr. Alba B. Brandes, moderator of the session and the chair of medical oncology at Azienda USL, a group of nine hospitals in and around Bologna, Italy.
The investigators have been criticized for repackaging their nonsignificant intent-to-treat results into per-protocol results that show significance, she said. “An intention-to-treat population and per-protocol population are two different things, and from a statistical point of view, it is sometimes difficult for the oncologic community to accept.” Despite those reservations, she said that the per-protocol observations should not be dismissed, because when they are analyzed in this way the results are highly significant.
Dr. Ram acknowledged that per-protocol analysis is unconventional, but “there is no precedent for this kind of therapy and I think we may need to redesign the way we assess results in the future. We cannot use the same guidelines and definitions we were traditionally using.”
Major Finding: 1-year overall survival in a subgroup of patients was significantly higher among those treated with NovoTTF-100A than it was in those who received chemotherapy (35.2% vs. 20.8%).
Data Source: Post hoc subgroup analysis of 237 patients with recurrent glioblastoma.
Disclosures: Dr. Zvi Ram disclosed that he is a consultant for NovoCure, which sponsored the trial and manufactures the device. Dr. Brandes said that she had no relevant financial disclosures.
MONTREAL – An investigational treatment for recurrent glioblastoma that delivers alternating electric fields through scalp electrodes has shown signs of improved survival in a post hoc analysis of results in particular subgroups of patients in a phase III trial.
Quality of life outcomes also favored patients who used the device, known as NovoTTF-100A, compared with those who received chemotherapy.
To date, reports about the device have elicited both antagonistic and enthusiastic reaction from oncologists, with “neither the enthusiasts nor the antagonists having significant basis for either kind of acute reaction,” Dr. Zvi Ram said in an interview after presenting the subgroup analyses at the meetingo “I think it is exciting that we're getting something completely new – a different, noninvasive modality with no side effects. I think we should be exhilarated.”
The device delivers low-amplitude “tumor treatment fields” of 100–300 kHz that have been shown in vitro to slow and reverse tumor cell proliferation by inhibiting mitosis, according to NovoCure Ltd., the manufacturer of the device and sponsor of the trial.
The portable device weighs about 6 pounds and connects to a battery pack. It is designed to be worn almost constantly, with a target of at least 20 hours of use each day.
In a phase III clinical trial presented earlier this year at the American Society of Clinical Oncology, an intent-to-treat analysis comparing NovoTTF vs. best-available chemotherapy found no statistical difference in 1-year overall survival (OS) among 237 recurrent glioblastoma patients randomized to either treatment.
However, a per-protocol analysis (which included only those patients who wore the device for at least 70% of the recommended time during the first month) showed a statistically significant benefit to NovoTTF in 1-year survival, compared with chemotherapy (29.5% vs. 19.1%, respectively; hazard ratio, 0.64; P = .01).
In the new post hoc analysis, a subgroup of 110 patients with a “good prognosis” (aged younger than 60 years, and with a Karnofsky performance status score greater than 80%) showed a “more robust” survival benefit than that seen in the overall intent-to-treat analysis, he said.
In this subgroup, patients treated with NovoTTF had a median survival of 9.2 months, vs. 6.6 months in those treated with chemotherapy (P less than .01). However, in the overall intent-to-treat group, median survival was 6.6 months and 6.0 months, respectively, he explained. Moreover, the 1-year OS in this subgroup was significantly higher in the NovoTTF group than in the chemotherapy group (35.2% vs. 20.8%, respectively; P less than .01), whereas the difference was nonsignificant in the larger analysis (23.6% vs. 20.7%).
Another subgroup analysis looked at patients who had previously failed treatment with bevacizumab (about 20% of the entire cohort). Both an intent-to-treat analysis and a per-protocol analysis showed significant OS advantages to NovoTTF, said Dr. Ram, chair of neurosurgery at Tel Aviv (Israel) Medical Center.
The median OS in 44 patients in the intent-to-treat group was 4 months with NovoTTF vs. 3.1 months with chemotherapy (HR, 0.43; P less than .02). NovoTTF also gave a significantly better median OS among 29 patients in the per-protocol analysis for this subgroup (6.3 months vs. 3.3 months; HR, 0.21; P = .02).
“You don't see this anywhere,” he said. “There's no drug in the world that could produce such response in patients who had already failed” bevacizumab.
The investigators also analyzed a surgery-naive group. “You know these are going to be poor responders, almost identical to [those with] bevacizumab failure,” Dr. Ram commented.
In this group of 38 patients, an intent-to-treat analysis showed that overall survival was 9.8 months with NovoTTF vs. 5.5 months with chemotherapy.
Patients also reported significantly better quality of life with NovoTTF than with chemotherapy. On the Quality of Life Symptom Scale, NovoTTF patients scored −34 and −35 on constipation and diarrhea, compared with scores of +77 and +50 for the chemotherapy group. Nausea and vomiting scores were 15 for the NovoTTF group and 61 for the chemotherapy group, and pain scores were −1 for the NovoTTF group and +63 for the chemotherapy group.
A quality of life analysis using the EORTC (European Organisation for Research and Treatment of Cancer) QLQ-C30 instrument showed scores of 14 vs. −7 in favor of NovoTTF for cognitive functioning, and scores of 7 vs. 1 in favor of NovoTTF for emotional functioning.
“We do this to all our patients. We intoxicate them,” Dr. Ram said. “So even if NovoTTF did not extend survival, if it was equivalent to chemotherapy [for survival], it may still improve quality of life.”
Dr. Ram did not know the median length of time that the NovoTTF cohort wore the device, but an earlier phase II study followed some patients up to 59 months. He noted that “70% are still alive; that's unheard of.”
“There were concerns that patients might have more headaches or seizures, but there were none,” he added.
In the current study, the rate of adverse events related to the central nervous system was similar (66% for NovoTTF and 67% for chemotherapy). Seizures occurred in 15% of the NovoTTF group and 12% of the chemotherapy group, and headaches occurred in 18% and 13%, respectively.
“It's very interesting and exciting, even if we do not yet have enough definitive data,” commented Dr. Alba B. Brandes, moderator of the session and the chair of medical oncology at Azienda USL, a group of nine hospitals in and around Bologna, Italy.
The investigators have been criticized for repackaging their nonsignificant intent-to-treat results into per-protocol results that show significance, she said. “An intention-to-treat population and per-protocol population are two different things, and from a statistical point of view, it is sometimes difficult for the oncologic community to accept.” Despite those reservations, she said that the per-protocol observations should not be dismissed, because when they are analyzed in this way the results are highly significant.
Dr. Ram acknowledged that per-protocol analysis is unconventional, but “there is no precedent for this kind of therapy and I think we may need to redesign the way we assess results in the future. We cannot use the same guidelines and definitions we were traditionally using.”
Major Finding: 1-year overall survival in a subgroup of patients was significantly higher among those treated with NovoTTF-100A than it was in those who received chemotherapy (35.2% vs. 20.8%).
Data Source: Post hoc subgroup analysis of 237 patients with recurrent glioblastoma.
Disclosures: Dr. Zvi Ram disclosed that he is a consultant for NovoCure, which sponsored the trial and manufactures the device. Dr. Brandes said that she had no relevant financial disclosures.
MONTREAL – An investigational treatment for recurrent glioblastoma that delivers alternating electric fields through scalp electrodes has shown signs of improved survival in a post hoc analysis of results in particular subgroups of patients in a phase III trial.
Quality of life outcomes also favored patients who used the device, known as NovoTTF-100A, compared with those who received chemotherapy.
To date, reports about the device have elicited both antagonistic and enthusiastic reaction from oncologists, with “neither the enthusiasts nor the antagonists having significant basis for either kind of acute reaction,” Dr. Zvi Ram said in an interview after presenting the subgroup analyses at the meetingo “I think it is exciting that we're getting something completely new – a different, noninvasive modality with no side effects. I think we should be exhilarated.”
The device delivers low-amplitude “tumor treatment fields” of 100–300 kHz that have been shown in vitro to slow and reverse tumor cell proliferation by inhibiting mitosis, according to NovoCure Ltd., the manufacturer of the device and sponsor of the trial.
The portable device weighs about 6 pounds and connects to a battery pack. It is designed to be worn almost constantly, with a target of at least 20 hours of use each day.
In a phase III clinical trial presented earlier this year at the American Society of Clinical Oncology, an intent-to-treat analysis comparing NovoTTF vs. best-available chemotherapy found no statistical difference in 1-year overall survival (OS) among 237 recurrent glioblastoma patients randomized to either treatment.
However, a per-protocol analysis (which included only those patients who wore the device for at least 70% of the recommended time during the first month) showed a statistically significant benefit to NovoTTF in 1-year survival, compared with chemotherapy (29.5% vs. 19.1%, respectively; hazard ratio, 0.64; P = .01).
In the new post hoc analysis, a subgroup of 110 patients with a “good prognosis” (aged younger than 60 years, and with a Karnofsky performance status score greater than 80%) showed a “more robust” survival benefit than that seen in the overall intent-to-treat analysis, he said.
In this subgroup, patients treated with NovoTTF had a median survival of 9.2 months, vs. 6.6 months in those treated with chemotherapy (P less than .01). However, in the overall intent-to-treat group, median survival was 6.6 months and 6.0 months, respectively, he explained. Moreover, the 1-year OS in this subgroup was significantly higher in the NovoTTF group than in the chemotherapy group (35.2% vs. 20.8%, respectively; P less than .01), whereas the difference was nonsignificant in the larger analysis (23.6% vs. 20.7%).
Another subgroup analysis looked at patients who had previously failed treatment with bevacizumab (about 20% of the entire cohort). Both an intent-to-treat analysis and a per-protocol analysis showed significant OS advantages to NovoTTF, said Dr. Ram, chair of neurosurgery at Tel Aviv (Israel) Medical Center.
The median OS in 44 patients in the intent-to-treat group was 4 months with NovoTTF vs. 3.1 months with chemotherapy (HR, 0.43; P less than .02). NovoTTF also gave a significantly better median OS among 29 patients in the per-protocol analysis for this subgroup (6.3 months vs. 3.3 months; HR, 0.21; P = .02).
“You don't see this anywhere,” he said. “There's no drug in the world that could produce such response in patients who had already failed” bevacizumab.
The investigators also analyzed a surgery-naive group. “You know these are going to be poor responders, almost identical to [those with] bevacizumab failure,” Dr. Ram commented.
In this group of 38 patients, an intent-to-treat analysis showed that overall survival was 9.8 months with NovoTTF vs. 5.5 months with chemotherapy.
Patients also reported significantly better quality of life with NovoTTF than with chemotherapy. On the Quality of Life Symptom Scale, NovoTTF patients scored −34 and −35 on constipation and diarrhea, compared with scores of +77 and +50 for the chemotherapy group. Nausea and vomiting scores were 15 for the NovoTTF group and 61 for the chemotherapy group, and pain scores were −1 for the NovoTTF group and +63 for the chemotherapy group.
A quality of life analysis using the EORTC (European Organisation for Research and Treatment of Cancer) QLQ-C30 instrument showed scores of 14 vs. −7 in favor of NovoTTF for cognitive functioning, and scores of 7 vs. 1 in favor of NovoTTF for emotional functioning.
“We do this to all our patients. We intoxicate them,” Dr. Ram said. “So even if NovoTTF did not extend survival, if it was equivalent to chemotherapy [for survival], it may still improve quality of life.”
Dr. Ram did not know the median length of time that the NovoTTF cohort wore the device, but an earlier phase II study followed some patients up to 59 months. He noted that “70% are still alive; that's unheard of.”
“There were concerns that patients might have more headaches or seizures, but there were none,” he added.
In the current study, the rate of adverse events related to the central nervous system was similar (66% for NovoTTF and 67% for chemotherapy). Seizures occurred in 15% of the NovoTTF group and 12% of the chemotherapy group, and headaches occurred in 18% and 13%, respectively.
“It's very interesting and exciting, even if we do not yet have enough definitive data,” commented Dr. Alba B. Brandes, moderator of the session and the chair of medical oncology at Azienda USL, a group of nine hospitals in and around Bologna, Italy.
The investigators have been criticized for repackaging their nonsignificant intent-to-treat results into per-protocol results that show significance, she said. “An intention-to-treat population and per-protocol population are two different things, and from a statistical point of view, it is sometimes difficult for the oncologic community to accept.” Despite those reservations, she said that the per-protocol observations should not be dismissed, because when they are analyzed in this way the results are highly significant.
Dr. Ram acknowledged that per-protocol analysis is unconventional, but “there is no precedent for this kind of therapy and I think we may need to redesign the way we assess results in the future. We cannot use the same guidelines and definitions we were traditionally using.”
Bevacizumab Effective in Glioblastoma Trials
MONTREAL – Bevacizumab-containing regimens continued to show efficacy against glioblastoma in recent reports of phase II trial results, but the trials' designs have come under fire by some neuro-oncologists.
Investigators from Duke University, Durham, N.C., reported at the meeting that adding bevacizumab (Avastin) and irinotecan (Camptosar) to a standard temozolomide (Temodar)–based chemoradiation regimen for newly diagnosed glioblastoma increased progression-free and overall survival by about 6 months, compared with historical controls.
In a separate RTOG (Radiation Therapy Oncology Group) study, investigators defined efficacy as a progression-free survival rate of 35% at 6 months in patients with recurrent glioblastoma. Both regimens in the noncomparative trial – bevacizumab with dose-dense temozolomide and bevacizumab with irinotecan – cleared the mark at 40% and 39%, respectively. Median overall survival was longer with the temozolomide partnership (9.4 months vs. 7.7 months with irinotecan), but the difference was not significant.
In 2009, the Food and Drug Administration approved bevacizumab as a single agent for the second-line treatment of glioblastoma, based on objective response rates in two single-arm trials.
Newly Diagnosed in Duke Study
The Genentech-sponsored study from Duke began with 125 patients (mean age, 56 years; 59% male) with newly diagnosed grade IV malignant glioblastoma multiforme (GBM), reported Dr. Annick Desjardins of the university's brain tumor center. Most (70%) had Karnofsky performance scores greater than 90%.
Between 2 and 4 weeks after resection, patients started 6 weeks of radiotherapy and daily temozolomide at 75 mg/m
In the second phase of the trial, 113 patients went on to receive 6–12 more weeks of bevacizumab at the same dosage, combined with temozolomide at 200 mg/m
The first phase of treatment was associated with minimal toxicity, the investigators recently reported (Int. J. Radiat. Oncol. Biol. Phys. 2010 Oct 30 [doi: 10.1016/j.ijrobp.2010.08.058]). Grade 4 thrombocytopenia occurred in 2.4%, neutropenia in 0.8%, central nervous system hemorrhage in 0.8%, and deep vein thrombosis and pulmonary embolism in 1.6%, said Dr. Desjardins.
Five patients did not complete the first phase (one patient with grade 2 CNS hemorrhage, two with pulmonary emboli, one with grade 4 pancytopenia, and one with wound dehiscence). Seven other patients did not go on to the second phase (three with tumor progression, two withdrawing because of fatigue, and one each with a bowel perforation and a rectal abscess). Patients in the second phase have been followed for a median of 28 months, said Dr. Desjardins.
A final analysis for the original cohort of 125 shows that median progression-free survival reached 14.2 months and median overall survival was 21.3 months. This compares with medians of 6.9 months and 15.9 months, respectively, that had been reported in the literature, she said.
Additionally, progression-free survival rates were 88% at 6 months, 64% at 1 year, and 16% at 2 years in the Duke cohort; overall survival rates were 94%, 82%, and 44%, respectively.
For all 125 patients enrolled, the overall serious toxicities included 1 CNS hemorrhage, 9 VTEs, 2 wound dehiscences, 1 bowel perforation, 17 grade 4 hematologic toxicities, 1 secondary malignancy, and 2 cases of pneumocystis pneumonia. There were four toxicity-related deaths.
RTOG Trial in Recurrent GBM
The noncomparative RTOG study enrolled patients with recurrent glioblastoma who had failed previous chemoradiation with temozolomide. In all, 57 patients were assigned to bevacizumab 10 mg/kg IV plus irinotecan 200 mg/kg every 2 weeks, and 58 were assigned to the same bevacizumab dose plus dose-dense temozolomide 75–100 mg/m
The two arms had different end points: safety with temozolomide and efficacy in the irinotecan arm, noted the presenter, Dr. Mark Gilbert, a professor of neuro-oncology at the University of Texas M.D. Anderson Cancer Center in Houston.
Hematologic toxicities were seen more in the temozolomide arm, whereas gastrointestinal toxicities predominated in the irinotecan arm, said Dr. Gilbert. One case of gastrointestinal perforation resulted in death.
“The primary objectives were met,” he reported. “We found that administering bevacizumab regimens in a cooperative group setting was feasible. We had acceptable toxicity with the combination of bevacizumab and dose-dense temozolomide, and it supported our use of this type of regimen in the up-front setting. And, in fact, the efficacy of both arms reached our target.”
Trials' Protocols Criticized
Both study designs were challenged at the meeting.
Session moderator Dr. Martin van den Bent contended that exposing all patients to the bevacizumab/irinotecan regimen in the Duke study – rather than randomizing patients to one agent or the other – makes it impossible to know which drug is preferable.
“It's flatly outrageous. It should not have been done,” Dr. van den Bent elaborated in an interview after the session. “What I find very disturbing is they did a very big study of 120 patients … but by doing it in an uncontrolled fashion, they ended up with an impossible interpretation of whether the irinotecan added to the bevacizumab made any difference.”
Dr. van den Bent, professor of neuro-oncology at the cancer center of Erasmus University in Rotterdam, the Netherlands, charged that Duke has a history of doing uncontrolled trials, but he also criticized the field's eagerness to embrace bevacizumab based on such trials.
“The use of bevacizumab at present is based on uncontrolled studies; it's been FDA approved on a scientifically not valid end point,” said Dr. van den Bent, a past chair of the EORTC (European Organisation for Research and Treatment of Cancer) Brain Tumor Group.
Study design also triggered a complaint with the RTOG trial. Dr. Gilbert cautioned that randomization was not consistent because of safety concerns with the temozolomide regimen. Until these were resolved, the initial 90 patients were randomized 2:1 favoring irinotecan. Consequently, the final 30 temozolomide patients were assigned to that arm without randomization.
For these reasons, “we cannot on the basis of this study tell which of the two treatments” is better, “or in fact whether a combination of chemotherapy with bevacizumab is better than bevacizumab alone,” he said, stressing that the study was not powered for comparison.
A member of the audience asked whether this wasn't “kind of a charade,” since comparisons were being made anyway.
“It's not a charade,” Dr. Gilbert replied, reiterating that the investigators had two separate goals: safety with temozolomide and efficacy with irinotecan. “It is what it is,” he said. “We certainly weren't going to power it, because we weren't interested particularly in the question of which was the better regimen.”
Genentech sponsored the study from Duke University. Dr. Desjardins reported no conflicts of interest. Dr. Gilbert disclosed research support from Merck and Genentech, and honoraria/advisory board participation with Merck and Genentech. Dr. van den Bent said he is a consultant for eight companies, including F. Hoffmann-La Roche, parent company of Genentech.
MONTREAL – Bevacizumab-containing regimens continued to show efficacy against glioblastoma in recent reports of phase II trial results, but the trials' designs have come under fire by some neuro-oncologists.
Investigators from Duke University, Durham, N.C., reported at the meeting that adding bevacizumab (Avastin) and irinotecan (Camptosar) to a standard temozolomide (Temodar)–based chemoradiation regimen for newly diagnosed glioblastoma increased progression-free and overall survival by about 6 months, compared with historical controls.
In a separate RTOG (Radiation Therapy Oncology Group) study, investigators defined efficacy as a progression-free survival rate of 35% at 6 months in patients with recurrent glioblastoma. Both regimens in the noncomparative trial – bevacizumab with dose-dense temozolomide and bevacizumab with irinotecan – cleared the mark at 40% and 39%, respectively. Median overall survival was longer with the temozolomide partnership (9.4 months vs. 7.7 months with irinotecan), but the difference was not significant.
In 2009, the Food and Drug Administration approved bevacizumab as a single agent for the second-line treatment of glioblastoma, based on objective response rates in two single-arm trials.
Newly Diagnosed in Duke Study
The Genentech-sponsored study from Duke began with 125 patients (mean age, 56 years; 59% male) with newly diagnosed grade IV malignant glioblastoma multiforme (GBM), reported Dr. Annick Desjardins of the university's brain tumor center. Most (70%) had Karnofsky performance scores greater than 90%.
Between 2 and 4 weeks after resection, patients started 6 weeks of radiotherapy and daily temozolomide at 75 mg/m
In the second phase of the trial, 113 patients went on to receive 6–12 more weeks of bevacizumab at the same dosage, combined with temozolomide at 200 mg/m
The first phase of treatment was associated with minimal toxicity, the investigators recently reported (Int. J. Radiat. Oncol. Biol. Phys. 2010 Oct 30 [doi: 10.1016/j.ijrobp.2010.08.058]). Grade 4 thrombocytopenia occurred in 2.4%, neutropenia in 0.8%, central nervous system hemorrhage in 0.8%, and deep vein thrombosis and pulmonary embolism in 1.6%, said Dr. Desjardins.
Five patients did not complete the first phase (one patient with grade 2 CNS hemorrhage, two with pulmonary emboli, one with grade 4 pancytopenia, and one with wound dehiscence). Seven other patients did not go on to the second phase (three with tumor progression, two withdrawing because of fatigue, and one each with a bowel perforation and a rectal abscess). Patients in the second phase have been followed for a median of 28 months, said Dr. Desjardins.
A final analysis for the original cohort of 125 shows that median progression-free survival reached 14.2 months and median overall survival was 21.3 months. This compares with medians of 6.9 months and 15.9 months, respectively, that had been reported in the literature, she said.
Additionally, progression-free survival rates were 88% at 6 months, 64% at 1 year, and 16% at 2 years in the Duke cohort; overall survival rates were 94%, 82%, and 44%, respectively.
For all 125 patients enrolled, the overall serious toxicities included 1 CNS hemorrhage, 9 VTEs, 2 wound dehiscences, 1 bowel perforation, 17 grade 4 hematologic toxicities, 1 secondary malignancy, and 2 cases of pneumocystis pneumonia. There were four toxicity-related deaths.
RTOG Trial in Recurrent GBM
The noncomparative RTOG study enrolled patients with recurrent glioblastoma who had failed previous chemoradiation with temozolomide. In all, 57 patients were assigned to bevacizumab 10 mg/kg IV plus irinotecan 200 mg/kg every 2 weeks, and 58 were assigned to the same bevacizumab dose plus dose-dense temozolomide 75–100 mg/m
The two arms had different end points: safety with temozolomide and efficacy in the irinotecan arm, noted the presenter, Dr. Mark Gilbert, a professor of neuro-oncology at the University of Texas M.D. Anderson Cancer Center in Houston.
Hematologic toxicities were seen more in the temozolomide arm, whereas gastrointestinal toxicities predominated in the irinotecan arm, said Dr. Gilbert. One case of gastrointestinal perforation resulted in death.
“The primary objectives were met,” he reported. “We found that administering bevacizumab regimens in a cooperative group setting was feasible. We had acceptable toxicity with the combination of bevacizumab and dose-dense temozolomide, and it supported our use of this type of regimen in the up-front setting. And, in fact, the efficacy of both arms reached our target.”
Trials' Protocols Criticized
Both study designs were challenged at the meeting.
Session moderator Dr. Martin van den Bent contended that exposing all patients to the bevacizumab/irinotecan regimen in the Duke study – rather than randomizing patients to one agent or the other – makes it impossible to know which drug is preferable.
“It's flatly outrageous. It should not have been done,” Dr. van den Bent elaborated in an interview after the session. “What I find very disturbing is they did a very big study of 120 patients … but by doing it in an uncontrolled fashion, they ended up with an impossible interpretation of whether the irinotecan added to the bevacizumab made any difference.”
Dr. van den Bent, professor of neuro-oncology at the cancer center of Erasmus University in Rotterdam, the Netherlands, charged that Duke has a history of doing uncontrolled trials, but he also criticized the field's eagerness to embrace bevacizumab based on such trials.
“The use of bevacizumab at present is based on uncontrolled studies; it's been FDA approved on a scientifically not valid end point,” said Dr. van den Bent, a past chair of the EORTC (European Organisation for Research and Treatment of Cancer) Brain Tumor Group.
Study design also triggered a complaint with the RTOG trial. Dr. Gilbert cautioned that randomization was not consistent because of safety concerns with the temozolomide regimen. Until these were resolved, the initial 90 patients were randomized 2:1 favoring irinotecan. Consequently, the final 30 temozolomide patients were assigned to that arm without randomization.
For these reasons, “we cannot on the basis of this study tell which of the two treatments” is better, “or in fact whether a combination of chemotherapy with bevacizumab is better than bevacizumab alone,” he said, stressing that the study was not powered for comparison.
A member of the audience asked whether this wasn't “kind of a charade,” since comparisons were being made anyway.
“It's not a charade,” Dr. Gilbert replied, reiterating that the investigators had two separate goals: safety with temozolomide and efficacy with irinotecan. “It is what it is,” he said. “We certainly weren't going to power it, because we weren't interested particularly in the question of which was the better regimen.”
Genentech sponsored the study from Duke University. Dr. Desjardins reported no conflicts of interest. Dr. Gilbert disclosed research support from Merck and Genentech, and honoraria/advisory board participation with Merck and Genentech. Dr. van den Bent said he is a consultant for eight companies, including F. Hoffmann-La Roche, parent company of Genentech.
MONTREAL – Bevacizumab-containing regimens continued to show efficacy against glioblastoma in recent reports of phase II trial results, but the trials' designs have come under fire by some neuro-oncologists.
Investigators from Duke University, Durham, N.C., reported at the meeting that adding bevacizumab (Avastin) and irinotecan (Camptosar) to a standard temozolomide (Temodar)–based chemoradiation regimen for newly diagnosed glioblastoma increased progression-free and overall survival by about 6 months, compared with historical controls.
In a separate RTOG (Radiation Therapy Oncology Group) study, investigators defined efficacy as a progression-free survival rate of 35% at 6 months in patients with recurrent glioblastoma. Both regimens in the noncomparative trial – bevacizumab with dose-dense temozolomide and bevacizumab with irinotecan – cleared the mark at 40% and 39%, respectively. Median overall survival was longer with the temozolomide partnership (9.4 months vs. 7.7 months with irinotecan), but the difference was not significant.
In 2009, the Food and Drug Administration approved bevacizumab as a single agent for the second-line treatment of glioblastoma, based on objective response rates in two single-arm trials.
Newly Diagnosed in Duke Study
The Genentech-sponsored study from Duke began with 125 patients (mean age, 56 years; 59% male) with newly diagnosed grade IV malignant glioblastoma multiforme (GBM), reported Dr. Annick Desjardins of the university's brain tumor center. Most (70%) had Karnofsky performance scores greater than 90%.
Between 2 and 4 weeks after resection, patients started 6 weeks of radiotherapy and daily temozolomide at 75 mg/m
In the second phase of the trial, 113 patients went on to receive 6–12 more weeks of bevacizumab at the same dosage, combined with temozolomide at 200 mg/m
The first phase of treatment was associated with minimal toxicity, the investigators recently reported (Int. J. Radiat. Oncol. Biol. Phys. 2010 Oct 30 [doi: 10.1016/j.ijrobp.2010.08.058]). Grade 4 thrombocytopenia occurred in 2.4%, neutropenia in 0.8%, central nervous system hemorrhage in 0.8%, and deep vein thrombosis and pulmonary embolism in 1.6%, said Dr. Desjardins.
Five patients did not complete the first phase (one patient with grade 2 CNS hemorrhage, two with pulmonary emboli, one with grade 4 pancytopenia, and one with wound dehiscence). Seven other patients did not go on to the second phase (three with tumor progression, two withdrawing because of fatigue, and one each with a bowel perforation and a rectal abscess). Patients in the second phase have been followed for a median of 28 months, said Dr. Desjardins.
A final analysis for the original cohort of 125 shows that median progression-free survival reached 14.2 months and median overall survival was 21.3 months. This compares with medians of 6.9 months and 15.9 months, respectively, that had been reported in the literature, she said.
Additionally, progression-free survival rates were 88% at 6 months, 64% at 1 year, and 16% at 2 years in the Duke cohort; overall survival rates were 94%, 82%, and 44%, respectively.
For all 125 patients enrolled, the overall serious toxicities included 1 CNS hemorrhage, 9 VTEs, 2 wound dehiscences, 1 bowel perforation, 17 grade 4 hematologic toxicities, 1 secondary malignancy, and 2 cases of pneumocystis pneumonia. There were four toxicity-related deaths.
RTOG Trial in Recurrent GBM
The noncomparative RTOG study enrolled patients with recurrent glioblastoma who had failed previous chemoradiation with temozolomide. In all, 57 patients were assigned to bevacizumab 10 mg/kg IV plus irinotecan 200 mg/kg every 2 weeks, and 58 were assigned to the same bevacizumab dose plus dose-dense temozolomide 75–100 mg/m
The two arms had different end points: safety with temozolomide and efficacy in the irinotecan arm, noted the presenter, Dr. Mark Gilbert, a professor of neuro-oncology at the University of Texas M.D. Anderson Cancer Center in Houston.
Hematologic toxicities were seen more in the temozolomide arm, whereas gastrointestinal toxicities predominated in the irinotecan arm, said Dr. Gilbert. One case of gastrointestinal perforation resulted in death.
“The primary objectives were met,” he reported. “We found that administering bevacizumab regimens in a cooperative group setting was feasible. We had acceptable toxicity with the combination of bevacizumab and dose-dense temozolomide, and it supported our use of this type of regimen in the up-front setting. And, in fact, the efficacy of both arms reached our target.”
Trials' Protocols Criticized
Both study designs were challenged at the meeting.
Session moderator Dr. Martin van den Bent contended that exposing all patients to the bevacizumab/irinotecan regimen in the Duke study – rather than randomizing patients to one agent or the other – makes it impossible to know which drug is preferable.
“It's flatly outrageous. It should not have been done,” Dr. van den Bent elaborated in an interview after the session. “What I find very disturbing is they did a very big study of 120 patients … but by doing it in an uncontrolled fashion, they ended up with an impossible interpretation of whether the irinotecan added to the bevacizumab made any difference.”
Dr. van den Bent, professor of neuro-oncology at the cancer center of Erasmus University in Rotterdam, the Netherlands, charged that Duke has a history of doing uncontrolled trials, but he also criticized the field's eagerness to embrace bevacizumab based on such trials.
“The use of bevacizumab at present is based on uncontrolled studies; it's been FDA approved on a scientifically not valid end point,” said Dr. van den Bent, a past chair of the EORTC (European Organisation for Research and Treatment of Cancer) Brain Tumor Group.
Study design also triggered a complaint with the RTOG trial. Dr. Gilbert cautioned that randomization was not consistent because of safety concerns with the temozolomide regimen. Until these were resolved, the initial 90 patients were randomized 2:1 favoring irinotecan. Consequently, the final 30 temozolomide patients were assigned to that arm without randomization.
For these reasons, “we cannot on the basis of this study tell which of the two treatments” is better, “or in fact whether a combination of chemotherapy with bevacizumab is better than bevacizumab alone,” he said, stressing that the study was not powered for comparison.
A member of the audience asked whether this wasn't “kind of a charade,” since comparisons were being made anyway.
“It's not a charade,” Dr. Gilbert replied, reiterating that the investigators had two separate goals: safety with temozolomide and efficacy with irinotecan. “It is what it is,” he said. “We certainly weren't going to power it, because we weren't interested particularly in the question of which was the better regimen.”
Genentech sponsored the study from Duke University. Dr. Desjardins reported no conflicts of interest. Dr. Gilbert disclosed research support from Merck and Genentech, and honoraria/advisory board participation with Merck and Genentech. Dr. van den Bent said he is a consultant for eight companies, including F. Hoffmann-La Roche, parent company of Genentech.
Brief Decline in Quality of Life Seen After Brain Radiotherapy
MONTREAL – Adjuvant whole-brain radiotherapy following surgical or radiosurgical resection of brain metastases provided no survival benefit and modestly reduced health-related quality of life when compared with close MRI observation alone in a randomized study of 359 patients.
The worsening of health-related quality of life with whole-brain radiotherapy (WBRT) was slight and transient, first author Dr. Riccardo Soffietti said at the annual meeting of the Society for Neuro-Oncology. He noted that few scores "reached clinical or statistical significance, and most scores that differed significantly at the first time point had a tendency to recover over time."
The study was a secondary analysis of a phase III study in which patients were randomized to receive WBRT (180 patients) or undergo observation with MRI every 3 months (179) after undergoing surgery or radiosurgery for one to three brain metastases. The primary results of the study were published online Nov. 1 in the Journal of Clinical Oncology (doi:10.1200/JCO.2010.30.1655).
For the primary outcome of overall survival at 1 year, there was no difference in between the WBRT (median of 10.9 months) and observation groups (10.7 months). Both groups also had a similar degree of functional independence.
There was a modest increase in progression-free survival in the WBRT group "probably due to their significant reduction in intracranial progression," said Dr. Soffietti, professor of neuro-oncology at the University of Torino (Italy).
Intracranial progression causing death occurred in 28% of the WBRT group, compared with 44% of the observation group.
For the secondary end point of health-related quality of life (HRQOL), there was low patient compliance in completing the brain-specific questionnaires QLQ-C30 and BN-20. Only 315 (88%) of the participants completed baseline assessments, while many fewer completed 6-month (51%) or 1-year assessments (45%).
Among the patients for whom all assessments were available, Dr. Soffietti and his colleagues noted "a statistically significant and clinically relevant difference between the two arms at 9 months favoring patients who did not receive whole-brain radiation therapy." However, the difference in global HRQOL scores at that time (52.2 in the WBRT group and 63.2 in the observation group) was only transitory and was not maintained by the 1-year mark.
The European Organization for Research and Treatment of Cancer sponsored the trial. Dr. Soffietti did not offer disclosure information.
MONTREAL – Adjuvant whole-brain radiotherapy following surgical or radiosurgical resection of brain metastases provided no survival benefit and modestly reduced health-related quality of life when compared with close MRI observation alone in a randomized study of 359 patients.
The worsening of health-related quality of life with whole-brain radiotherapy (WBRT) was slight and transient, first author Dr. Riccardo Soffietti said at the annual meeting of the Society for Neuro-Oncology. He noted that few scores "reached clinical or statistical significance, and most scores that differed significantly at the first time point had a tendency to recover over time."
The study was a secondary analysis of a phase III study in which patients were randomized to receive WBRT (180 patients) or undergo observation with MRI every 3 months (179) after undergoing surgery or radiosurgery for one to three brain metastases. The primary results of the study were published online Nov. 1 in the Journal of Clinical Oncology (doi:10.1200/JCO.2010.30.1655).
For the primary outcome of overall survival at 1 year, there was no difference in between the WBRT (median of 10.9 months) and observation groups (10.7 months). Both groups also had a similar degree of functional independence.
There was a modest increase in progression-free survival in the WBRT group "probably due to their significant reduction in intracranial progression," said Dr. Soffietti, professor of neuro-oncology at the University of Torino (Italy).
Intracranial progression causing death occurred in 28% of the WBRT group, compared with 44% of the observation group.
For the secondary end point of health-related quality of life (HRQOL), there was low patient compliance in completing the brain-specific questionnaires QLQ-C30 and BN-20. Only 315 (88%) of the participants completed baseline assessments, while many fewer completed 6-month (51%) or 1-year assessments (45%).
Among the patients for whom all assessments were available, Dr. Soffietti and his colleagues noted "a statistically significant and clinically relevant difference between the two arms at 9 months favoring patients who did not receive whole-brain radiation therapy." However, the difference in global HRQOL scores at that time (52.2 in the WBRT group and 63.2 in the observation group) was only transitory and was not maintained by the 1-year mark.
The European Organization for Research and Treatment of Cancer sponsored the trial. Dr. Soffietti did not offer disclosure information.
MONTREAL – Adjuvant whole-brain radiotherapy following surgical or radiosurgical resection of brain metastases provided no survival benefit and modestly reduced health-related quality of life when compared with close MRI observation alone in a randomized study of 359 patients.
The worsening of health-related quality of life with whole-brain radiotherapy (WBRT) was slight and transient, first author Dr. Riccardo Soffietti said at the annual meeting of the Society for Neuro-Oncology. He noted that few scores "reached clinical or statistical significance, and most scores that differed significantly at the first time point had a tendency to recover over time."
The study was a secondary analysis of a phase III study in which patients were randomized to receive WBRT (180 patients) or undergo observation with MRI every 3 months (179) after undergoing surgery or radiosurgery for one to three brain metastases. The primary results of the study were published online Nov. 1 in the Journal of Clinical Oncology (doi:10.1200/JCO.2010.30.1655).
For the primary outcome of overall survival at 1 year, there was no difference in between the WBRT (median of 10.9 months) and observation groups (10.7 months). Both groups also had a similar degree of functional independence.
There was a modest increase in progression-free survival in the WBRT group "probably due to their significant reduction in intracranial progression," said Dr. Soffietti, professor of neuro-oncology at the University of Torino (Italy).
Intracranial progression causing death occurred in 28% of the WBRT group, compared with 44% of the observation group.
For the secondary end point of health-related quality of life (HRQOL), there was low patient compliance in completing the brain-specific questionnaires QLQ-C30 and BN-20. Only 315 (88%) of the participants completed baseline assessments, while many fewer completed 6-month (51%) or 1-year assessments (45%).
Among the patients for whom all assessments were available, Dr. Soffietti and his colleagues noted "a statistically significant and clinically relevant difference between the two arms at 9 months favoring patients who did not receive whole-brain radiation therapy." However, the difference in global HRQOL scores at that time (52.2 in the WBRT group and 63.2 in the observation group) was only transitory and was not maintained by the 1-year mark.
The European Organization for Research and Treatment of Cancer sponsored the trial. Dr. Soffietti did not offer disclosure information.
FROM THE ANNUAL MEETING OF THE SOCIETY FOR NEURO-ONCOLOGY
Major Finding: Global HRQOL scores at 9 months were significantly worse in patients who received WBRT than in those who underwent observation alone (52.2 vs. 63.2, respectively).
Data Source: Randomized trial of 359 patients who underwent either observation or adjuvant whole-brain radiotherapy after surgical or radiosurgical resection of between one and three brain metastases.
Disclosures: The European Organization for Research and Treatment of Cancer sponsored the trial. Dr. Soffietti did not offer disclosure information.
Frail Elderly Benefit From Post-Op Temozolomide for Glioblastoma
MONTREAL – Elderly patients with newly diagnosed glioblastoma and poor Karnofsky performance scores can benefit from postsurgical chemotherapy with temozolomide, based on the results of a single-arm study in 70 patients.
Not only were most patients able to withstand treatment-related toxicity, but survival rates and performance status appeared to improve with treatment, Dr. Jamie Gállego Pérez-Larraya reported at the annual meeting of the Society for Neuro-Oncology.
Median overall survival, the primary end point, reached 25 weeks, with a 6-month overall survival rate of 44.3% and a 12-month rate of 11.4%, said Dr. Pérez-Larraya of the Hôpital Pitié-Salpêtrière in Paris. Median progression-free survival, a secondary end point, was 16 weeks, with a 6-month rate of 30%.
"These data compare favorably to the 17-week median survival reported in elderly patients with glioblastoma and good performance treated only with palliative care," he said.
The trial from ANOCEF (Association des Neuro-Oncologues d'Expression Française) enrolled 70 patients aged 70 and up (median age, 77 years), with newly diagnosed and histologically confirmed glioblastoma, a median Karnofsky performance score of 60, and no previous radiotherapy or chemotherapy for the brain tumor. Most (92%) had undergone biopsy of their tumor; five patients had received a partial resection, and one had a complete resection.
Temozolomide chemotherapy started at 150 mg/m2 for 5 consecutive days every 28 days, with dose escalation up to 200 mg/m2 in the absence of grade 3 or 4 toxicities for a maximum of 12 cycles, or until disease progression. Patients who progressed received supportive care; no radiotherapy was given.
Quality of life (QOL) and cognitive function outcomes were measured by EORTC (European Organisation for Research and Treatment of Cancer) questionnaires (QLQ-C30 and QLQ-BN20), and the Mini-Mental State Examination (MMSE). The study showed significant improvements on the global QOL scale and most functioning domains, with no decline in any domain, he said.
A third of the cohort improved their Karnofsky performance scores by at least 10 points, and 26% achieved a score of 70 or greater. "This is clinically significant because it means they became capable of self-care," he noted.
Treatment with temozolomide was "generally well tolerated," Dr. Pérez-Larraya reported. Twelve patients, (17%) had grade 3 or 4 thrombocytopenia or neutropenia, but these toxicities did not lead to dose delays or dose reductions.
All of the cohort had died by the time of presentation – 87% as a result of disease progression, and 13% from other causes, with no deaths due to toxicity.
"Until a few years ago the treatment of these patients received little attention mainly because of their poor expected survival, but also because of the fear of treatment-related toxicity," said Dr. Pérez-Larraya.
Now patients with good performance scores can be treated with postsurgical radiotherapy, which has been shown to prolong survival from 17 weeks to 29 weeks without causing deterioration in quality of life or cognitive function (N. Engl. J. Med. 2007;356:1527-35), he said. But the management of patients with poor scores has never been studied and remains uncertain.
"Radiotherapy requires many trips to the hospital, and increasing fatigue makes this difficult for these severely impaired patients with such a short expected survival. As a result, these patients frequently receive only supportive care," he explained.
"These results suggest that treatment with temozolomide in elderly patients with glioblastoma and poor performance score has an acceptable safety profile; is associated with an improvement in functional status in one-third of cases, as well as quality of life before progression; and seems to increase survival as compared to supportive care alone," Dr. Pérez-Larraya concluded.
He reported having no relevant financial disclosures.
MONTREAL – Elderly patients with newly diagnosed glioblastoma and poor Karnofsky performance scores can benefit from postsurgical chemotherapy with temozolomide, based on the results of a single-arm study in 70 patients.
Not only were most patients able to withstand treatment-related toxicity, but survival rates and performance status appeared to improve with treatment, Dr. Jamie Gállego Pérez-Larraya reported at the annual meeting of the Society for Neuro-Oncology.
Median overall survival, the primary end point, reached 25 weeks, with a 6-month overall survival rate of 44.3% and a 12-month rate of 11.4%, said Dr. Pérez-Larraya of the Hôpital Pitié-Salpêtrière in Paris. Median progression-free survival, a secondary end point, was 16 weeks, with a 6-month rate of 30%.
"These data compare favorably to the 17-week median survival reported in elderly patients with glioblastoma and good performance treated only with palliative care," he said.
The trial from ANOCEF (Association des Neuro-Oncologues d'Expression Française) enrolled 70 patients aged 70 and up (median age, 77 years), with newly diagnosed and histologically confirmed glioblastoma, a median Karnofsky performance score of 60, and no previous radiotherapy or chemotherapy for the brain tumor. Most (92%) had undergone biopsy of their tumor; five patients had received a partial resection, and one had a complete resection.
Temozolomide chemotherapy started at 150 mg/m2 for 5 consecutive days every 28 days, with dose escalation up to 200 mg/m2 in the absence of grade 3 or 4 toxicities for a maximum of 12 cycles, or until disease progression. Patients who progressed received supportive care; no radiotherapy was given.
Quality of life (QOL) and cognitive function outcomes were measured by EORTC (European Organisation for Research and Treatment of Cancer) questionnaires (QLQ-C30 and QLQ-BN20), and the Mini-Mental State Examination (MMSE). The study showed significant improvements on the global QOL scale and most functioning domains, with no decline in any domain, he said.
A third of the cohort improved their Karnofsky performance scores by at least 10 points, and 26% achieved a score of 70 or greater. "This is clinically significant because it means they became capable of self-care," he noted.
Treatment with temozolomide was "generally well tolerated," Dr. Pérez-Larraya reported. Twelve patients, (17%) had grade 3 or 4 thrombocytopenia or neutropenia, but these toxicities did not lead to dose delays or dose reductions.
All of the cohort had died by the time of presentation – 87% as a result of disease progression, and 13% from other causes, with no deaths due to toxicity.
"Until a few years ago the treatment of these patients received little attention mainly because of their poor expected survival, but also because of the fear of treatment-related toxicity," said Dr. Pérez-Larraya.
Now patients with good performance scores can be treated with postsurgical radiotherapy, which has been shown to prolong survival from 17 weeks to 29 weeks without causing deterioration in quality of life or cognitive function (N. Engl. J. Med. 2007;356:1527-35), he said. But the management of patients with poor scores has never been studied and remains uncertain.
"Radiotherapy requires many trips to the hospital, and increasing fatigue makes this difficult for these severely impaired patients with such a short expected survival. As a result, these patients frequently receive only supportive care," he explained.
"These results suggest that treatment with temozolomide in elderly patients with glioblastoma and poor performance score has an acceptable safety profile; is associated with an improvement in functional status in one-third of cases, as well as quality of life before progression; and seems to increase survival as compared to supportive care alone," Dr. Pérez-Larraya concluded.
He reported having no relevant financial disclosures.
MONTREAL – Elderly patients with newly diagnosed glioblastoma and poor Karnofsky performance scores can benefit from postsurgical chemotherapy with temozolomide, based on the results of a single-arm study in 70 patients.
Not only were most patients able to withstand treatment-related toxicity, but survival rates and performance status appeared to improve with treatment, Dr. Jamie Gállego Pérez-Larraya reported at the annual meeting of the Society for Neuro-Oncology.
Median overall survival, the primary end point, reached 25 weeks, with a 6-month overall survival rate of 44.3% and a 12-month rate of 11.4%, said Dr. Pérez-Larraya of the Hôpital Pitié-Salpêtrière in Paris. Median progression-free survival, a secondary end point, was 16 weeks, with a 6-month rate of 30%.
"These data compare favorably to the 17-week median survival reported in elderly patients with glioblastoma and good performance treated only with palliative care," he said.
The trial from ANOCEF (Association des Neuro-Oncologues d'Expression Française) enrolled 70 patients aged 70 and up (median age, 77 years), with newly diagnosed and histologically confirmed glioblastoma, a median Karnofsky performance score of 60, and no previous radiotherapy or chemotherapy for the brain tumor. Most (92%) had undergone biopsy of their tumor; five patients had received a partial resection, and one had a complete resection.
Temozolomide chemotherapy started at 150 mg/m2 for 5 consecutive days every 28 days, with dose escalation up to 200 mg/m2 in the absence of grade 3 or 4 toxicities for a maximum of 12 cycles, or until disease progression. Patients who progressed received supportive care; no radiotherapy was given.
Quality of life (QOL) and cognitive function outcomes were measured by EORTC (European Organisation for Research and Treatment of Cancer) questionnaires (QLQ-C30 and QLQ-BN20), and the Mini-Mental State Examination (MMSE). The study showed significant improvements on the global QOL scale and most functioning domains, with no decline in any domain, he said.
A third of the cohort improved their Karnofsky performance scores by at least 10 points, and 26% achieved a score of 70 or greater. "This is clinically significant because it means they became capable of self-care," he noted.
Treatment with temozolomide was "generally well tolerated," Dr. Pérez-Larraya reported. Twelve patients, (17%) had grade 3 or 4 thrombocytopenia or neutropenia, but these toxicities did not lead to dose delays or dose reductions.
All of the cohort had died by the time of presentation – 87% as a result of disease progression, and 13% from other causes, with no deaths due to toxicity.
"Until a few years ago the treatment of these patients received little attention mainly because of their poor expected survival, but also because of the fear of treatment-related toxicity," said Dr. Pérez-Larraya.
Now patients with good performance scores can be treated with postsurgical radiotherapy, which has been shown to prolong survival from 17 weeks to 29 weeks without causing deterioration in quality of life or cognitive function (N. Engl. J. Med. 2007;356:1527-35), he said. But the management of patients with poor scores has never been studied and remains uncertain.
"Radiotherapy requires many trips to the hospital, and increasing fatigue makes this difficult for these severely impaired patients with such a short expected survival. As a result, these patients frequently receive only supportive care," he explained.
"These results suggest that treatment with temozolomide in elderly patients with glioblastoma and poor performance score has an acceptable safety profile; is associated with an improvement in functional status in one-third of cases, as well as quality of life before progression; and seems to increase survival as compared to supportive care alone," Dr. Pérez-Larraya concluded.
He reported having no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE SOCIETY FOR NEURO-ONCOLOGY
Major Finding: More than half of patients with a median Karnofsky performance score of 60 improved their score by at least 10 points.
Data Source: A group of 70 elderly, poor-performance patients, treated with postsurgical temozolomide for newly diagnosed glioblastoma.
Disclosures: Dr. Pérez-Larraya reported having no relevant financial disclosures.
New Drugs Target Recurrent Meningioma
MONTREAL – The tyrosine kinase inhibitors vatalanib and sunitinib may offer alternative approaches to treating patients with recurrent, high-grade meningioma who have failed surgery and radiation therapy, according to two separate phase II studies.
Both drugs significantly improved survival compared with what is generally expected in this patient population, most of whom had grade II or III tumors. Progression-free survival at 6 months occurred in 57% of 25 patients with meningioma who received the investigational drug vatalanib in one study, and in 36% of 36 patients who received sunitinib in another study. Both drugs are inhibitors of receptors for vascular endothelial growth factor and platelet-derived growth factor.
Sunitinib is marketed by the brand name Sutent and has been approved by the Food and Drug Administration for the treatment of advanced renal cell carcinoma and gastrointestinal stromal tumor after disease progression on – or intolerance to – imatinib mesylate (Gleevec).
Progression-free survival (PFS) for patients with recurrent grade II and III tumors is usually considered to occur in fewer than 5%, said Dr. Jeffrey Raizer, who presented the vatalanib study at the annual meeting of the Society for Neuro-Oncology.
"For recurrence of meningioma, treatment options are limited once patients have failed surgery and radiation, and chemotherapies have been very limited to date," said Dr. Raizer, director of medical neuro-oncology at the cancer center of Northwestern University and Northwestern Memorial Hospital, both in Chicago.
Despite the encouraging findings of the two studies, a lack of information on the natural history of these tumors makes it difficult to interpret the studies, said Dr. Michael Vogelbaum, who chaired the session in which the studies were presented.
"While the studies suggest there may be some promise, we don’t really know what to expect from that mix of grade II and III tumors on their own," Dr. Vogelbaum said in an interview. He is chair of neuro-oncology and associate director of the brain tumor and neuro-oncology center at the Cleveland Clinic Neurological Institute.
Dr. Fred Barker of the department of neurosurgery at Massachusetts General Hospital, Boston, echoed Dr. Vogelbaum’s comments. "There’s been very little organized effort to do chemotherapy trials for meningiomas, so these studies are important because they are the first. The results are interesting, but we don’t know exactly what the natural history would be without treatment, so whether there’s a benefit to giving these drugs will require further study."
In Dr. Raizer’s Pfizer-sponsored study of vatalanib in meningioma patients, the median PFS was 5.9 months, and the median overall survival (OS) was 22.3 months. Of the 25 patients in the study, 22 had grade II and III tumors and 14 were men. The PFS at 6 months was comparable between patients with grade II (39%) or grade III disease only (43%).
Dosing of vatalanib began at 250 mg twice daily and increased by 250 mg/day every 7 days until the dosage reached 500 mg twice daily, he said.
For 21 patients with available imaging data, tumors partially responded to treatment in 1, remained stable in 15, and progressed in 5 patients.
The most common adverse events observed were fatigue, rash, and elevated transaminases.
The sunitinib study, sponsored by Novartis, included 36 patients (median age, 62 years) with recurrent grade II and III meningiomas who had exhausted all surgical and radiation options. The patients had a median of five recurrences.
The primary end point of PFS at 6 months was 36% and the median PFS was 5.1 months. The overall survival rate is not known, as only eight patients have died, reported Dr. Thomas Kaley, codirector of the neuro-oncology fellowship program at Memorial Sloan-Kettering Cancer Center in New York.
Imaging was available for 34 patients and showed stable disease in 26, a partial response in 1, and progressive disease in 7 patients, he said.
The dose of sunitinib was 50 mg orally per day on a 4-week-on, 2-week-off cycle.
"The toxicity was high with this drug," Dr. Kaley commented.
A total of 18 patients required dose reductions, and 6 patients withdrew from the study because of toxicity. There was one fatal grade 5 intratumoral hemorrhage and two nonfatal intratumoral hemorrhages (grades 3 and 4). The most common toxicities included myelosuppression, fatigue, headache, and GI side effects.
The investigators reported having no relevant conflicts of interest.*
* CORRECTION, 1/17/2011: An earlier version of this story included incorrect information about the investigators' disclosures. The error has been corrected.
MONTREAL – The tyrosine kinase inhibitors vatalanib and sunitinib may offer alternative approaches to treating patients with recurrent, high-grade meningioma who have failed surgery and radiation therapy, according to two separate phase II studies.
Both drugs significantly improved survival compared with what is generally expected in this patient population, most of whom had grade II or III tumors. Progression-free survival at 6 months occurred in 57% of 25 patients with meningioma who received the investigational drug vatalanib in one study, and in 36% of 36 patients who received sunitinib in another study. Both drugs are inhibitors of receptors for vascular endothelial growth factor and platelet-derived growth factor.
Sunitinib is marketed by the brand name Sutent and has been approved by the Food and Drug Administration for the treatment of advanced renal cell carcinoma and gastrointestinal stromal tumor after disease progression on – or intolerance to – imatinib mesylate (Gleevec).
Progression-free survival (PFS) for patients with recurrent grade II and III tumors is usually considered to occur in fewer than 5%, said Dr. Jeffrey Raizer, who presented the vatalanib study at the annual meeting of the Society for Neuro-Oncology.
"For recurrence of meningioma, treatment options are limited once patients have failed surgery and radiation, and chemotherapies have been very limited to date," said Dr. Raizer, director of medical neuro-oncology at the cancer center of Northwestern University and Northwestern Memorial Hospital, both in Chicago.
Despite the encouraging findings of the two studies, a lack of information on the natural history of these tumors makes it difficult to interpret the studies, said Dr. Michael Vogelbaum, who chaired the session in which the studies were presented.
"While the studies suggest there may be some promise, we don’t really know what to expect from that mix of grade II and III tumors on their own," Dr. Vogelbaum said in an interview. He is chair of neuro-oncology and associate director of the brain tumor and neuro-oncology center at the Cleveland Clinic Neurological Institute.
Dr. Fred Barker of the department of neurosurgery at Massachusetts General Hospital, Boston, echoed Dr. Vogelbaum’s comments. "There’s been very little organized effort to do chemotherapy trials for meningiomas, so these studies are important because they are the first. The results are interesting, but we don’t know exactly what the natural history would be without treatment, so whether there’s a benefit to giving these drugs will require further study."
In Dr. Raizer’s Pfizer-sponsored study of vatalanib in meningioma patients, the median PFS was 5.9 months, and the median overall survival (OS) was 22.3 months. Of the 25 patients in the study, 22 had grade II and III tumors and 14 were men. The PFS at 6 months was comparable between patients with grade II (39%) or grade III disease only (43%).
Dosing of vatalanib began at 250 mg twice daily and increased by 250 mg/day every 7 days until the dosage reached 500 mg twice daily, he said.
For 21 patients with available imaging data, tumors partially responded to treatment in 1, remained stable in 15, and progressed in 5 patients.
The most common adverse events observed were fatigue, rash, and elevated transaminases.
The sunitinib study, sponsored by Novartis, included 36 patients (median age, 62 years) with recurrent grade II and III meningiomas who had exhausted all surgical and radiation options. The patients had a median of five recurrences.
The primary end point of PFS at 6 months was 36% and the median PFS was 5.1 months. The overall survival rate is not known, as only eight patients have died, reported Dr. Thomas Kaley, codirector of the neuro-oncology fellowship program at Memorial Sloan-Kettering Cancer Center in New York.
Imaging was available for 34 patients and showed stable disease in 26, a partial response in 1, and progressive disease in 7 patients, he said.
The dose of sunitinib was 50 mg orally per day on a 4-week-on, 2-week-off cycle.
"The toxicity was high with this drug," Dr. Kaley commented.
A total of 18 patients required dose reductions, and 6 patients withdrew from the study because of toxicity. There was one fatal grade 5 intratumoral hemorrhage and two nonfatal intratumoral hemorrhages (grades 3 and 4). The most common toxicities included myelosuppression, fatigue, headache, and GI side effects.
The investigators reported having no relevant conflicts of interest.*
* CORRECTION, 1/17/2011: An earlier version of this story included incorrect information about the investigators' disclosures. The error has been corrected.
MONTREAL – The tyrosine kinase inhibitors vatalanib and sunitinib may offer alternative approaches to treating patients with recurrent, high-grade meningioma who have failed surgery and radiation therapy, according to two separate phase II studies.
Both drugs significantly improved survival compared with what is generally expected in this patient population, most of whom had grade II or III tumors. Progression-free survival at 6 months occurred in 57% of 25 patients with meningioma who received the investigational drug vatalanib in one study, and in 36% of 36 patients who received sunitinib in another study. Both drugs are inhibitors of receptors for vascular endothelial growth factor and platelet-derived growth factor.
Sunitinib is marketed by the brand name Sutent and has been approved by the Food and Drug Administration for the treatment of advanced renal cell carcinoma and gastrointestinal stromal tumor after disease progression on – or intolerance to – imatinib mesylate (Gleevec).
Progression-free survival (PFS) for patients with recurrent grade II and III tumors is usually considered to occur in fewer than 5%, said Dr. Jeffrey Raizer, who presented the vatalanib study at the annual meeting of the Society for Neuro-Oncology.
"For recurrence of meningioma, treatment options are limited once patients have failed surgery and radiation, and chemotherapies have been very limited to date," said Dr. Raizer, director of medical neuro-oncology at the cancer center of Northwestern University and Northwestern Memorial Hospital, both in Chicago.
Despite the encouraging findings of the two studies, a lack of information on the natural history of these tumors makes it difficult to interpret the studies, said Dr. Michael Vogelbaum, who chaired the session in which the studies were presented.
"While the studies suggest there may be some promise, we don’t really know what to expect from that mix of grade II and III tumors on their own," Dr. Vogelbaum said in an interview. He is chair of neuro-oncology and associate director of the brain tumor and neuro-oncology center at the Cleveland Clinic Neurological Institute.
Dr. Fred Barker of the department of neurosurgery at Massachusetts General Hospital, Boston, echoed Dr. Vogelbaum’s comments. "There’s been very little organized effort to do chemotherapy trials for meningiomas, so these studies are important because they are the first. The results are interesting, but we don’t know exactly what the natural history would be without treatment, so whether there’s a benefit to giving these drugs will require further study."
In Dr. Raizer’s Pfizer-sponsored study of vatalanib in meningioma patients, the median PFS was 5.9 months, and the median overall survival (OS) was 22.3 months. Of the 25 patients in the study, 22 had grade II and III tumors and 14 were men. The PFS at 6 months was comparable between patients with grade II (39%) or grade III disease only (43%).
Dosing of vatalanib began at 250 mg twice daily and increased by 250 mg/day every 7 days until the dosage reached 500 mg twice daily, he said.
For 21 patients with available imaging data, tumors partially responded to treatment in 1, remained stable in 15, and progressed in 5 patients.
The most common adverse events observed were fatigue, rash, and elevated transaminases.
The sunitinib study, sponsored by Novartis, included 36 patients (median age, 62 years) with recurrent grade II and III meningiomas who had exhausted all surgical and radiation options. The patients had a median of five recurrences.
The primary end point of PFS at 6 months was 36% and the median PFS was 5.1 months. The overall survival rate is not known, as only eight patients have died, reported Dr. Thomas Kaley, codirector of the neuro-oncology fellowship program at Memorial Sloan-Kettering Cancer Center in New York.
Imaging was available for 34 patients and showed stable disease in 26, a partial response in 1, and progressive disease in 7 patients, he said.
The dose of sunitinib was 50 mg orally per day on a 4-week-on, 2-week-off cycle.
"The toxicity was high with this drug," Dr. Kaley commented.
A total of 18 patients required dose reductions, and 6 patients withdrew from the study because of toxicity. There was one fatal grade 5 intratumoral hemorrhage and two nonfatal intratumoral hemorrhages (grades 3 and 4). The most common toxicities included myelosuppression, fatigue, headache, and GI side effects.
The investigators reported having no relevant conflicts of interest.*
* CORRECTION, 1/17/2011: An earlier version of this story included incorrect information about the investigators' disclosures. The error has been corrected.