User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
nav[contains(@class, 'nav-ce-stack nav-ce-stack__large-screen')]
header[@id='header']
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'main-prefix')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
div[contains(@class, 'view-medstat-quiz-listing-panes')]
div[contains(@class, 'pane-article-sidebar-latest-news')]
Low Vitamin D Levels May Signal CVD Risk in Young Adults
TOPLINE:
, small study finds.
METHODOLOGY:
- A secondary analysis of the Activating Brown Adipose Tissue Through Exercise (ACTIBATE) trial assessed the association between serum 25(OH)D levels and CVD risk factors.
- The cross-sectional study used baseline data of in 177 healthy sedentary adults ages 18-25 years (65% women; all White individuals), who were recruited between October 2015 and December 2016 from Granada, a region in the south of Spain.
- Study participants were nonsmokers, led a sedentary lifestyle, and did not have a prior history of CVD or chronic illnesses.
- The CVD risk factors included anthropometrical and body composition profiles, glucose and lipid metabolism, liver, and pro- and anti-inflammatory biomarkers.
- 25(OH)D serum concentrations were measured with a competitive chemiluminescence immunoassay and defined as deficient (< 20 ng/mL), insufficient (21-29 ng/mL), or normal (> 30 ng/mL).
TAKEAWAY:
- The levels correlated inversely with body mass index (BMI; standardized regression coefficient [beta], −0.177; P = .018), fat mass index (beta, −0.195; P = .011), and systolic blood pressure (beta, −0.137; P = .038), after adjusting for sex.
- Glucose metabolism markers (serum glucose and insulin concentrations, insulin/glucose ratio, and homeostatic model assessment of index) also correlated inversely with vitamin D levels.
- The trend was similar for liver markers serum γ-glutamyl transferase and alkaline phosphatase) and the anti-inflammatory marker interleukin-4.
- BMI, waist/hip ratio, fat mass index, blood pressure, and levels of glucose, insulin, , and liver markers were higher in the 44 participants with vitamin D deficiency vs 41 participants with normal vitamin D levels.
IN PRACTICE:
“Collectively, these findings support the idea that 25(OH)D concentrations may be used as a useful marker of CVD status, which can be easily monitored in young individuals,” the authors wrote.
SOURCE:
This study was led by first author Francisco J. AmaroGahete, MD, PhD, from the Department of Physiology, Faculty of Medicine, University of Granada, Spain, who also holds positions in other institutions. It was published online in the Journal of Endocrinological Investigation.
LIMITATIONS:
This study could not establish causal relationships due to its cross-sectional design. The results might not apply to younger or older people from different locations and ethnic backgrounds. The gold standard method for analyzing vitamin D levels, liquid chromatography–mass spectrometry, was not used in this study.
DISCLOSURES:
This study was supported by the Spanish Ministry of Economy and Competitiveness, Spanish Ministry of Education, AstraZeneca HealthCare Foundation, and other sources. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
, small study finds.
METHODOLOGY:
- A secondary analysis of the Activating Brown Adipose Tissue Through Exercise (ACTIBATE) trial assessed the association between serum 25(OH)D levels and CVD risk factors.
- The cross-sectional study used baseline data of in 177 healthy sedentary adults ages 18-25 years (65% women; all White individuals), who were recruited between October 2015 and December 2016 from Granada, a region in the south of Spain.
- Study participants were nonsmokers, led a sedentary lifestyle, and did not have a prior history of CVD or chronic illnesses.
- The CVD risk factors included anthropometrical and body composition profiles, glucose and lipid metabolism, liver, and pro- and anti-inflammatory biomarkers.
- 25(OH)D serum concentrations were measured with a competitive chemiluminescence immunoassay and defined as deficient (< 20 ng/mL), insufficient (21-29 ng/mL), or normal (> 30 ng/mL).
TAKEAWAY:
- The levels correlated inversely with body mass index (BMI; standardized regression coefficient [beta], −0.177; P = .018), fat mass index (beta, −0.195; P = .011), and systolic blood pressure (beta, −0.137; P = .038), after adjusting for sex.
- Glucose metabolism markers (serum glucose and insulin concentrations, insulin/glucose ratio, and homeostatic model assessment of index) also correlated inversely with vitamin D levels.
- The trend was similar for liver markers serum γ-glutamyl transferase and alkaline phosphatase) and the anti-inflammatory marker interleukin-4.
- BMI, waist/hip ratio, fat mass index, blood pressure, and levels of glucose, insulin, , and liver markers were higher in the 44 participants with vitamin D deficiency vs 41 participants with normal vitamin D levels.
IN PRACTICE:
“Collectively, these findings support the idea that 25(OH)D concentrations may be used as a useful marker of CVD status, which can be easily monitored in young individuals,” the authors wrote.
SOURCE:
This study was led by first author Francisco J. AmaroGahete, MD, PhD, from the Department of Physiology, Faculty of Medicine, University of Granada, Spain, who also holds positions in other institutions. It was published online in the Journal of Endocrinological Investigation.
LIMITATIONS:
This study could not establish causal relationships due to its cross-sectional design. The results might not apply to younger or older people from different locations and ethnic backgrounds. The gold standard method for analyzing vitamin D levels, liquid chromatography–mass spectrometry, was not used in this study.
DISCLOSURES:
This study was supported by the Spanish Ministry of Economy and Competitiveness, Spanish Ministry of Education, AstraZeneca HealthCare Foundation, and other sources. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
TOPLINE:
, small study finds.
METHODOLOGY:
- A secondary analysis of the Activating Brown Adipose Tissue Through Exercise (ACTIBATE) trial assessed the association between serum 25(OH)D levels and CVD risk factors.
- The cross-sectional study used baseline data of in 177 healthy sedentary adults ages 18-25 years (65% women; all White individuals), who were recruited between October 2015 and December 2016 from Granada, a region in the south of Spain.
- Study participants were nonsmokers, led a sedentary lifestyle, and did not have a prior history of CVD or chronic illnesses.
- The CVD risk factors included anthropometrical and body composition profiles, glucose and lipid metabolism, liver, and pro- and anti-inflammatory biomarkers.
- 25(OH)D serum concentrations were measured with a competitive chemiluminescence immunoassay and defined as deficient (< 20 ng/mL), insufficient (21-29 ng/mL), or normal (> 30 ng/mL).
TAKEAWAY:
- The levels correlated inversely with body mass index (BMI; standardized regression coefficient [beta], −0.177; P = .018), fat mass index (beta, −0.195; P = .011), and systolic blood pressure (beta, −0.137; P = .038), after adjusting for sex.
- Glucose metabolism markers (serum glucose and insulin concentrations, insulin/glucose ratio, and homeostatic model assessment of index) also correlated inversely with vitamin D levels.
- The trend was similar for liver markers serum γ-glutamyl transferase and alkaline phosphatase) and the anti-inflammatory marker interleukin-4.
- BMI, waist/hip ratio, fat mass index, blood pressure, and levels of glucose, insulin, , and liver markers were higher in the 44 participants with vitamin D deficiency vs 41 participants with normal vitamin D levels.
IN PRACTICE:
“Collectively, these findings support the idea that 25(OH)D concentrations may be used as a useful marker of CVD status, which can be easily monitored in young individuals,” the authors wrote.
SOURCE:
This study was led by first author Francisco J. AmaroGahete, MD, PhD, from the Department of Physiology, Faculty of Medicine, University of Granada, Spain, who also holds positions in other institutions. It was published online in the Journal of Endocrinological Investigation.
LIMITATIONS:
This study could not establish causal relationships due to its cross-sectional design. The results might not apply to younger or older people from different locations and ethnic backgrounds. The gold standard method for analyzing vitamin D levels, liquid chromatography–mass spectrometry, was not used in this study.
DISCLOSURES:
This study was supported by the Spanish Ministry of Economy and Competitiveness, Spanish Ministry of Education, AstraZeneca HealthCare Foundation, and other sources. The authors declared no conflicts of interest.
A version of this article appeared on Medscape.com.
Prolonged Sitting at Work Ups CVD and All-Cause Mortality, Daily Breaks May Help
However, daily breaks from sitting and leisure-time activity can help mitigate the “serious” risks associated with prolonged occupational sitting, the researchers say.
“As part of modern lifestyles, prolonged occupational sitting is considered normal and has not received due attention, even though its deleterious effect on health outcomes has been demonstrated,” wrote the authors, led by Wayne Gao, PhD, with Taipei Medical University College of Public Health, Taipei City, Taiwan.
“The importance of physical activity and moving around can never be overstated,” Michelle Bloom, MD, director of the cardio-oncology program at NYU Langone Health in New York, who wasn’t involved in the study, told this news organization.
“As a cardiologist, I bring this up at almost every visit with every patient regardless of why they’re seeing me, because I think that patients respond better when their doctor says it than when they just kind of know it in the back of their mind,” said Dr. Bloom, who is also a professor in the Division of Cardiology, NYU Grossman Long Island School of Medicine, New York.
The study was published online in JAMA Network Open.
Prolonged Sitting Hard on the Heart
2020 marked the first time that guidelines on physical activity from the World Health Organization recommended reducing sedentary behaviors owing to their health consequences. Less is known on the specific association of prolonged occupational sitting with health outcomes, especially in the context of low physical activity.
For their study, Dr. Gao and colleagues quantified health risks associated with prolonged sitting on the job and determined whether a certain threshold of physical activity may attenuate this risk.
Participants included 481,688 adults (mean age, 39 years; 53% women) in a health surveillance program in Taiwan. Data on occupational sitting, leisure-time physical activity, lifestyle, and metabolic parameters were collected.
During an average follow up of nearly 13 years, 26,257 participants died; more than half (57%) of the deaths occurred in individuals who mostly sat at work. There were 5371 CVD-related deaths, with 60% occurring in the mostly sitting group.
In multivariate analysis that adjusted for sex, age, education, smoking, drinking, and body mass index, adults who mostly sat at work had a 16% higher risk of dying of any cause (hazard ratio [HR], 1.16; 95% CI, 1.11-1.20) and a 34% increased risk of dying of CVD (HR, 1.34; 95% CI, 1.22-1.46) compared with those who mostly did not sit at work.
Adults who mostly alternated between sitting and not sitting at work were not at increased risk of all-cause mortality compared with individuals who mostly did not at work (HR, 1.01; 95% CI, 0.97-1.05).
Among adults who mostly sat at work and engaged in low (15-29 minutes) or no (< 15 minutes) daily leisure-time activity, increasing activity by 15 and 30 minutes per day, respectively, lowered the risk for mortality to a level similar to that of inactive individuals who mostly do not sit at work.
“Overall, our findings from a large prospective cohort help to strengthen the increasingly accumulating evidence linking a sedentary lifestyle and health risks,” the authors wrote.
“Systemic changes, such as more frequent breaks, standing desks, designated workplace areas for physical activity, and gym membership benefits, can help reduce risk,” they added.
Simple Yet Profound Message
Reached for comment, Anu Lala, MD, with Icahn School of Medicine at Mount Sinai and Mount Sinai Fuster Heart Hospital in New York, said this study provides a “simple yet profound message” about the dangers of prolonged sitting.
The finding of a 16% higher all-cause mortality in those who mostly sat at work after adjustment for major risk factors is “pretty remarkable. And for CVD mortality, it’s double that,” Dr. Lala told this news organization.
“I think we undervalue the importance of movement, however simple it is. Even simple actions, like squatting and standing up have benefits for the heart,” Dr. Lala added.
Dr. Bloom said she tells her patients, “You don’t have to go out tomorrow and run a marathon. Just get up a few times a day, walk a few laps in your office, walk back and forth from the mailbox, walk up and down your steps a couple of times — just do something more than you’re doing already.”
The study had no commercial funding. Dr. Gao and Dr. Bloom have no relevant disclosures. Dr. Lala has serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for Novartis, AstraZeneca, Merck, Bayer, Novo Nordisk, Cordio, Zoll, and Sequana Medical.
A version of this article appeared on Medscape.com.
However, daily breaks from sitting and leisure-time activity can help mitigate the “serious” risks associated with prolonged occupational sitting, the researchers say.
“As part of modern lifestyles, prolonged occupational sitting is considered normal and has not received due attention, even though its deleterious effect on health outcomes has been demonstrated,” wrote the authors, led by Wayne Gao, PhD, with Taipei Medical University College of Public Health, Taipei City, Taiwan.
“The importance of physical activity and moving around can never be overstated,” Michelle Bloom, MD, director of the cardio-oncology program at NYU Langone Health in New York, who wasn’t involved in the study, told this news organization.
“As a cardiologist, I bring this up at almost every visit with every patient regardless of why they’re seeing me, because I think that patients respond better when their doctor says it than when they just kind of know it in the back of their mind,” said Dr. Bloom, who is also a professor in the Division of Cardiology, NYU Grossman Long Island School of Medicine, New York.
The study was published online in JAMA Network Open.
Prolonged Sitting Hard on the Heart
2020 marked the first time that guidelines on physical activity from the World Health Organization recommended reducing sedentary behaviors owing to their health consequences. Less is known on the specific association of prolonged occupational sitting with health outcomes, especially in the context of low physical activity.
For their study, Dr. Gao and colleagues quantified health risks associated with prolonged sitting on the job and determined whether a certain threshold of physical activity may attenuate this risk.
Participants included 481,688 adults (mean age, 39 years; 53% women) in a health surveillance program in Taiwan. Data on occupational sitting, leisure-time physical activity, lifestyle, and metabolic parameters were collected.
During an average follow up of nearly 13 years, 26,257 participants died; more than half (57%) of the deaths occurred in individuals who mostly sat at work. There were 5371 CVD-related deaths, with 60% occurring in the mostly sitting group.
In multivariate analysis that adjusted for sex, age, education, smoking, drinking, and body mass index, adults who mostly sat at work had a 16% higher risk of dying of any cause (hazard ratio [HR], 1.16; 95% CI, 1.11-1.20) and a 34% increased risk of dying of CVD (HR, 1.34; 95% CI, 1.22-1.46) compared with those who mostly did not sit at work.
Adults who mostly alternated between sitting and not sitting at work were not at increased risk of all-cause mortality compared with individuals who mostly did not at work (HR, 1.01; 95% CI, 0.97-1.05).
Among adults who mostly sat at work and engaged in low (15-29 minutes) or no (< 15 minutes) daily leisure-time activity, increasing activity by 15 and 30 minutes per day, respectively, lowered the risk for mortality to a level similar to that of inactive individuals who mostly do not sit at work.
“Overall, our findings from a large prospective cohort help to strengthen the increasingly accumulating evidence linking a sedentary lifestyle and health risks,” the authors wrote.
“Systemic changes, such as more frequent breaks, standing desks, designated workplace areas for physical activity, and gym membership benefits, can help reduce risk,” they added.
Simple Yet Profound Message
Reached for comment, Anu Lala, MD, with Icahn School of Medicine at Mount Sinai and Mount Sinai Fuster Heart Hospital in New York, said this study provides a “simple yet profound message” about the dangers of prolonged sitting.
The finding of a 16% higher all-cause mortality in those who mostly sat at work after adjustment for major risk factors is “pretty remarkable. And for CVD mortality, it’s double that,” Dr. Lala told this news organization.
“I think we undervalue the importance of movement, however simple it is. Even simple actions, like squatting and standing up have benefits for the heart,” Dr. Lala added.
Dr. Bloom said she tells her patients, “You don’t have to go out tomorrow and run a marathon. Just get up a few times a day, walk a few laps in your office, walk back and forth from the mailbox, walk up and down your steps a couple of times — just do something more than you’re doing already.”
The study had no commercial funding. Dr. Gao and Dr. Bloom have no relevant disclosures. Dr. Lala has serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for Novartis, AstraZeneca, Merck, Bayer, Novo Nordisk, Cordio, Zoll, and Sequana Medical.
A version of this article appeared on Medscape.com.
However, daily breaks from sitting and leisure-time activity can help mitigate the “serious” risks associated with prolonged occupational sitting, the researchers say.
“As part of modern lifestyles, prolonged occupational sitting is considered normal and has not received due attention, even though its deleterious effect on health outcomes has been demonstrated,” wrote the authors, led by Wayne Gao, PhD, with Taipei Medical University College of Public Health, Taipei City, Taiwan.
“The importance of physical activity and moving around can never be overstated,” Michelle Bloom, MD, director of the cardio-oncology program at NYU Langone Health in New York, who wasn’t involved in the study, told this news organization.
“As a cardiologist, I bring this up at almost every visit with every patient regardless of why they’re seeing me, because I think that patients respond better when their doctor says it than when they just kind of know it in the back of their mind,” said Dr. Bloom, who is also a professor in the Division of Cardiology, NYU Grossman Long Island School of Medicine, New York.
The study was published online in JAMA Network Open.
Prolonged Sitting Hard on the Heart
2020 marked the first time that guidelines on physical activity from the World Health Organization recommended reducing sedentary behaviors owing to their health consequences. Less is known on the specific association of prolonged occupational sitting with health outcomes, especially in the context of low physical activity.
For their study, Dr. Gao and colleagues quantified health risks associated with prolonged sitting on the job and determined whether a certain threshold of physical activity may attenuate this risk.
Participants included 481,688 adults (mean age, 39 years; 53% women) in a health surveillance program in Taiwan. Data on occupational sitting, leisure-time physical activity, lifestyle, and metabolic parameters were collected.
During an average follow up of nearly 13 years, 26,257 participants died; more than half (57%) of the deaths occurred in individuals who mostly sat at work. There were 5371 CVD-related deaths, with 60% occurring in the mostly sitting group.
In multivariate analysis that adjusted for sex, age, education, smoking, drinking, and body mass index, adults who mostly sat at work had a 16% higher risk of dying of any cause (hazard ratio [HR], 1.16; 95% CI, 1.11-1.20) and a 34% increased risk of dying of CVD (HR, 1.34; 95% CI, 1.22-1.46) compared with those who mostly did not sit at work.
Adults who mostly alternated between sitting and not sitting at work were not at increased risk of all-cause mortality compared with individuals who mostly did not at work (HR, 1.01; 95% CI, 0.97-1.05).
Among adults who mostly sat at work and engaged in low (15-29 minutes) or no (< 15 minutes) daily leisure-time activity, increasing activity by 15 and 30 minutes per day, respectively, lowered the risk for mortality to a level similar to that of inactive individuals who mostly do not sit at work.
“Overall, our findings from a large prospective cohort help to strengthen the increasingly accumulating evidence linking a sedentary lifestyle and health risks,” the authors wrote.
“Systemic changes, such as more frequent breaks, standing desks, designated workplace areas for physical activity, and gym membership benefits, can help reduce risk,” they added.
Simple Yet Profound Message
Reached for comment, Anu Lala, MD, with Icahn School of Medicine at Mount Sinai and Mount Sinai Fuster Heart Hospital in New York, said this study provides a “simple yet profound message” about the dangers of prolonged sitting.
The finding of a 16% higher all-cause mortality in those who mostly sat at work after adjustment for major risk factors is “pretty remarkable. And for CVD mortality, it’s double that,” Dr. Lala told this news organization.
“I think we undervalue the importance of movement, however simple it is. Even simple actions, like squatting and standing up have benefits for the heart,” Dr. Lala added.
Dr. Bloom said she tells her patients, “You don’t have to go out tomorrow and run a marathon. Just get up a few times a day, walk a few laps in your office, walk back and forth from the mailbox, walk up and down your steps a couple of times — just do something more than you’re doing already.”
The study had no commercial funding. Dr. Gao and Dr. Bloom have no relevant disclosures. Dr. Lala has serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for Novartis, AstraZeneca, Merck, Bayer, Novo Nordisk, Cordio, Zoll, and Sequana Medical.
A version of this article appeared on Medscape.com.
FROM JAMA NETWORK OPEN
AI Boosts Diabetic Eye Screening and Follow-Up in Youth
TOPLINE:
Artificial intelligence (AI) boosts the screening rate for potentially blinding diabetes eye disorders in a diabetes clinic compared with referral to an eye care provider (ECP) in a racially and ethnically diverse youth population with diabetes.
METHODOLOGY:
- Although early screening and treatment can prevent diabetic eye diseases (DEDs), many people with diabetes in the United States lack access to and knowledge about diabetic eye exams.
- The trial included 164 patients aged 8-21 years (58% female, 35% Black, and 6% Hispanic) with type 1 or 2 diabetes with no known DED and no diabetic eye exam in the last 6 months.
- In a diabetes clinic, patients were randomly assigned to an AI diabetic eye exam (intervention arm) then and there or to standard of care, referred to an ECP with scripted educational material (control).
- Participants in the intervention arm underwent the 5- to 10-minute autonomous AI diabetic eye exam without pharmacologic dilation. The results were generated immediately as either “DED present” or “DED absent.”
- The primary outcome was the completion rate of documented diabetic eye exams within 6 months (“primary gap closure rate”), either by AI or going to the ECP. The secondary outcome was ECP follow-up by intervention participants with DED (intervention) and all control patients.
TAKEAWAY:
- Within 6 months, all the participants (100%) in the intervention arm completed their diabetic eye exam, a primary care gap closure rate of 100% (95% CI, 96%-100%).
- The rate of primary care gap closure was significantly higher in the intervention vs control arm (100% vs 22%; P < .001).
- In the intervention arm, 64% of patients with DED followed up with an eye care provider within 6 months compared with a mere 22% participants in the control arm (P < .001).
- Participants reported high levels of satisfaction with autonomous AI, with 92.5% expressing satisfaction with the exam’s duration and 96% expressing satisfaction with the whole experience.
IN PRACTICE:
“Autonomous AI increases diabetic eye exam completion rates and closes this care gap in a racially and ethnically diverse population of youth with diabetes, compared to standard of care,” the authors wrote.
SOURCE:
This study, which was led by Risa M. Wolf, MD, department of pediatrics, division of endocrinology, Johns Hopkins School of Medicine, Baltimore, was published online on January 11, 2024, in Nature Communications.
LIMITATIONS:
This study used autonomous AI in the youth although it’s not approved by the US Food and Drug Administration for use in individuals aged 21 years and younger. Some of the participants in this study were already familiar with autonomous AI diabetic eye exams, which might have contributed to their willingness to participate in the current study. The autonomous AI used in the study was shown to have a lack of racial and ethnic bias, but any AI bias caused by differences in retinal pigment has potential to increase rather than decrease health disparities.
DISCLOSURES:
The clinical trial was supported by the National Eye Institute of the National Institutes of Health and the Diabetes Research Connection. Wolf, the lead author, declared receiving research support from Boehringer Ingelheim and Novo Nordisk outside the submitted work. Coauthor Michael D. Abramoff, MD, declared serving in various roles such as investor, director, and consultant for Digital Diagnostics Inc., as well as other ties with many sources.
A version of this article appeared on Medscape.com.
TOPLINE:
Artificial intelligence (AI) boosts the screening rate for potentially blinding diabetes eye disorders in a diabetes clinic compared with referral to an eye care provider (ECP) in a racially and ethnically diverse youth population with diabetes.
METHODOLOGY:
- Although early screening and treatment can prevent diabetic eye diseases (DEDs), many people with diabetes in the United States lack access to and knowledge about diabetic eye exams.
- The trial included 164 patients aged 8-21 years (58% female, 35% Black, and 6% Hispanic) with type 1 or 2 diabetes with no known DED and no diabetic eye exam in the last 6 months.
- In a diabetes clinic, patients were randomly assigned to an AI diabetic eye exam (intervention arm) then and there or to standard of care, referred to an ECP with scripted educational material (control).
- Participants in the intervention arm underwent the 5- to 10-minute autonomous AI diabetic eye exam without pharmacologic dilation. The results were generated immediately as either “DED present” or “DED absent.”
- The primary outcome was the completion rate of documented diabetic eye exams within 6 months (“primary gap closure rate”), either by AI or going to the ECP. The secondary outcome was ECP follow-up by intervention participants with DED (intervention) and all control patients.
TAKEAWAY:
- Within 6 months, all the participants (100%) in the intervention arm completed their diabetic eye exam, a primary care gap closure rate of 100% (95% CI, 96%-100%).
- The rate of primary care gap closure was significantly higher in the intervention vs control arm (100% vs 22%; P < .001).
- In the intervention arm, 64% of patients with DED followed up with an eye care provider within 6 months compared with a mere 22% participants in the control arm (P < .001).
- Participants reported high levels of satisfaction with autonomous AI, with 92.5% expressing satisfaction with the exam’s duration and 96% expressing satisfaction with the whole experience.
IN PRACTICE:
“Autonomous AI increases diabetic eye exam completion rates and closes this care gap in a racially and ethnically diverse population of youth with diabetes, compared to standard of care,” the authors wrote.
SOURCE:
This study, which was led by Risa M. Wolf, MD, department of pediatrics, division of endocrinology, Johns Hopkins School of Medicine, Baltimore, was published online on January 11, 2024, in Nature Communications.
LIMITATIONS:
This study used autonomous AI in the youth although it’s not approved by the US Food and Drug Administration for use in individuals aged 21 years and younger. Some of the participants in this study were already familiar with autonomous AI diabetic eye exams, which might have contributed to their willingness to participate in the current study. The autonomous AI used in the study was shown to have a lack of racial and ethnic bias, but any AI bias caused by differences in retinal pigment has potential to increase rather than decrease health disparities.
DISCLOSURES:
The clinical trial was supported by the National Eye Institute of the National Institutes of Health and the Diabetes Research Connection. Wolf, the lead author, declared receiving research support from Boehringer Ingelheim and Novo Nordisk outside the submitted work. Coauthor Michael D. Abramoff, MD, declared serving in various roles such as investor, director, and consultant for Digital Diagnostics Inc., as well as other ties with many sources.
A version of this article appeared on Medscape.com.
TOPLINE:
Artificial intelligence (AI) boosts the screening rate for potentially blinding diabetes eye disorders in a diabetes clinic compared with referral to an eye care provider (ECP) in a racially and ethnically diverse youth population with diabetes.
METHODOLOGY:
- Although early screening and treatment can prevent diabetic eye diseases (DEDs), many people with diabetes in the United States lack access to and knowledge about diabetic eye exams.
- The trial included 164 patients aged 8-21 years (58% female, 35% Black, and 6% Hispanic) with type 1 or 2 diabetes with no known DED and no diabetic eye exam in the last 6 months.
- In a diabetes clinic, patients were randomly assigned to an AI diabetic eye exam (intervention arm) then and there or to standard of care, referred to an ECP with scripted educational material (control).
- Participants in the intervention arm underwent the 5- to 10-minute autonomous AI diabetic eye exam without pharmacologic dilation. The results were generated immediately as either “DED present” or “DED absent.”
- The primary outcome was the completion rate of documented diabetic eye exams within 6 months (“primary gap closure rate”), either by AI or going to the ECP. The secondary outcome was ECP follow-up by intervention participants with DED (intervention) and all control patients.
TAKEAWAY:
- Within 6 months, all the participants (100%) in the intervention arm completed their diabetic eye exam, a primary care gap closure rate of 100% (95% CI, 96%-100%).
- The rate of primary care gap closure was significantly higher in the intervention vs control arm (100% vs 22%; P < .001).
- In the intervention arm, 64% of patients with DED followed up with an eye care provider within 6 months compared with a mere 22% participants in the control arm (P < .001).
- Participants reported high levels of satisfaction with autonomous AI, with 92.5% expressing satisfaction with the exam’s duration and 96% expressing satisfaction with the whole experience.
IN PRACTICE:
“Autonomous AI increases diabetic eye exam completion rates and closes this care gap in a racially and ethnically diverse population of youth with diabetes, compared to standard of care,” the authors wrote.
SOURCE:
This study, which was led by Risa M. Wolf, MD, department of pediatrics, division of endocrinology, Johns Hopkins School of Medicine, Baltimore, was published online on January 11, 2024, in Nature Communications.
LIMITATIONS:
This study used autonomous AI in the youth although it’s not approved by the US Food and Drug Administration for use in individuals aged 21 years and younger. Some of the participants in this study were already familiar with autonomous AI diabetic eye exams, which might have contributed to their willingness to participate in the current study. The autonomous AI used in the study was shown to have a lack of racial and ethnic bias, but any AI bias caused by differences in retinal pigment has potential to increase rather than decrease health disparities.
DISCLOSURES:
The clinical trial was supported by the National Eye Institute of the National Institutes of Health and the Diabetes Research Connection. Wolf, the lead author, declared receiving research support from Boehringer Ingelheim and Novo Nordisk outside the submitted work. Coauthor Michael D. Abramoff, MD, declared serving in various roles such as investor, director, and consultant for Digital Diagnostics Inc., as well as other ties with many sources.
A version of this article appeared on Medscape.com.
Vibrating Belt Receives Approval to Help Women With Osteopenia Keep Bone Strength
The US Food and Drug Administration (FDA) has approved a wearable belt device for postmenopausal women with osteopenia, the precursor to osteoporosis, according to the company’s manufacturer, Bone Health Technologies.
According to the company, the device (Osteoboost) is the first nonpharmacologic device-based, prescription-only treatment for postmenopausal women with low bone density. It has not been tested for ability to reduce fracture risk.
The device is worn around the hips and delivers calibrated mild vibrations to the hips and lumbar spine to help preserve bone strength and density. A vibration pack is mounted to the back of the belt.
FDA approval, announced on January 18, was based on the findings of a National Institutes of Health–funded double-blinded, sham-controlled study of 126 women with low bone density conducted at the University of Nebraska Medical Center in Omaha. The data were shared at the 2023 Endocrine Society and American Society for Bone and Mineral Research annual meetings and published in the Journal of the Endocrine Society.
Lead investigator Laura D. Bilek, PT, PhD, associate dean for research and associate professor at the University of Nebraska, and colleagues wrote that the primary outcome measurement was the change in vertebral strength measured by CT scans for women who used the device a minimum of three times per week compared with a sham group who wore a belt that emitted sound but had no vibrations.
Compressive strength and volumetric density of the first lumbar vertebra were analyzed.
In the active-belt group, women lost, on average, 0.48% bone strength, while those in the sham group lost nearly 2.84% (P = .014), about five times as much. Results also showed that participants in the active treatment group who used the device three times per week lost 0.29% bone mineral density (BMD) compared with the 1.97% BMD lost in the control group. No adverse events were reported in the study.
Sonali Khandelwal, MD, a rheumatologist at Rush University in Chicago, told this news organization there’s considerable fear among some patients about long-term use of available medications for bone health, “so any modality that is nontherapeutic — not a pill — is always exciting.”
The endpoints of the study are one good measure, she said, but she emphasized that it will be important to show that the improved bone density from the belt that is described in this study “is a true marker of decreased fracture risk.”
Because there are no apparent side effects, she said it may be effective in combination with weight-bearing exercise, vitamin D and calcium, and/or medication, depending on severity of bone loss.
Current medications on the market for osteoporosis have been shown to improve bone strength and reduce fracture risk, she noted.
“It could help; I just don’t think we have enough evidence that it will completely treat the bone loss,” Dr. Khandelwal said.
She said she sees the potential population most interested in the belt as premenopausal women with a family history of bone loss who may not meet the level of bone loss for medical management but are interested in prevention.
“I also think of individuals who might already meet medication needs but are completely averse to being on medication,” she said. The bulk of her practice is treating bone loss, she said, estimating that 20% of her patients do not want to be on medication.
Bone Health Technologies CEO Laura Yecies, MBA, told this news organization the company has not yet set the price for the device and noted that because it will be available by prescription only, out-of-pocket costs and copays will differ. She said the company expects to begin shipping later this year. Requests for update notifications can be made at the company’s website.
Dr. Bilek told this news organization the device was tested for a year, so it’s unclear how long people with osteopenia would need to wear the belt for maximum benefit.
The theory behind the mechanism of action, she said, “is that the vibration actually inhibits the cells [osteoclasts] that take away bone mass.”
The researchers included only postmenopausal women with osteopenia in the study, but Dr. Bilek said she would like to test the device on other groups, such as men with prostate cancer getting testosterone-blocking therapy, which can result in loss of bone density. An estimated 34 million people in the United States have osteopenia.
Dr. Bilek said a next step for the study is to enroll a more diverse cohort at an additional center to test the device because most of the women in this one were White.
She noted that women’s bone mass peaks at age 30 and then starts to decline.
“When women hit menopause, there’s a really rapid decline [in bone strength] for the next 5-7 years and then the decline levels off. If we can slow that decline, hopefully that woman’s bone density is maintained at a higher level throughout their life,” Dr. Bilek said.
Dr. Bilek is a scientific adviser to Bone Health Technologies. She and many coauthors of the study received grants or fees from the company and own stock in or are employees of the company. Ms. Yecies is the founder and CEO of Bone Health Technologies. Dr. Khandelwal had no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The US Food and Drug Administration (FDA) has approved a wearable belt device for postmenopausal women with osteopenia, the precursor to osteoporosis, according to the company’s manufacturer, Bone Health Technologies.
According to the company, the device (Osteoboost) is the first nonpharmacologic device-based, prescription-only treatment for postmenopausal women with low bone density. It has not been tested for ability to reduce fracture risk.
The device is worn around the hips and delivers calibrated mild vibrations to the hips and lumbar spine to help preserve bone strength and density. A vibration pack is mounted to the back of the belt.
FDA approval, announced on January 18, was based on the findings of a National Institutes of Health–funded double-blinded, sham-controlled study of 126 women with low bone density conducted at the University of Nebraska Medical Center in Omaha. The data were shared at the 2023 Endocrine Society and American Society for Bone and Mineral Research annual meetings and published in the Journal of the Endocrine Society.
Lead investigator Laura D. Bilek, PT, PhD, associate dean for research and associate professor at the University of Nebraska, and colleagues wrote that the primary outcome measurement was the change in vertebral strength measured by CT scans for women who used the device a minimum of three times per week compared with a sham group who wore a belt that emitted sound but had no vibrations.
Compressive strength and volumetric density of the first lumbar vertebra were analyzed.
In the active-belt group, women lost, on average, 0.48% bone strength, while those in the sham group lost nearly 2.84% (P = .014), about five times as much. Results also showed that participants in the active treatment group who used the device three times per week lost 0.29% bone mineral density (BMD) compared with the 1.97% BMD lost in the control group. No adverse events were reported in the study.
Sonali Khandelwal, MD, a rheumatologist at Rush University in Chicago, told this news organization there’s considerable fear among some patients about long-term use of available medications for bone health, “so any modality that is nontherapeutic — not a pill — is always exciting.”
The endpoints of the study are one good measure, she said, but she emphasized that it will be important to show that the improved bone density from the belt that is described in this study “is a true marker of decreased fracture risk.”
Because there are no apparent side effects, she said it may be effective in combination with weight-bearing exercise, vitamin D and calcium, and/or medication, depending on severity of bone loss.
Current medications on the market for osteoporosis have been shown to improve bone strength and reduce fracture risk, she noted.
“It could help; I just don’t think we have enough evidence that it will completely treat the bone loss,” Dr. Khandelwal said.
She said she sees the potential population most interested in the belt as premenopausal women with a family history of bone loss who may not meet the level of bone loss for medical management but are interested in prevention.
“I also think of individuals who might already meet medication needs but are completely averse to being on medication,” she said. The bulk of her practice is treating bone loss, she said, estimating that 20% of her patients do not want to be on medication.
Bone Health Technologies CEO Laura Yecies, MBA, told this news organization the company has not yet set the price for the device and noted that because it will be available by prescription only, out-of-pocket costs and copays will differ. She said the company expects to begin shipping later this year. Requests for update notifications can be made at the company’s website.
Dr. Bilek told this news organization the device was tested for a year, so it’s unclear how long people with osteopenia would need to wear the belt for maximum benefit.
The theory behind the mechanism of action, she said, “is that the vibration actually inhibits the cells [osteoclasts] that take away bone mass.”
The researchers included only postmenopausal women with osteopenia in the study, but Dr. Bilek said she would like to test the device on other groups, such as men with prostate cancer getting testosterone-blocking therapy, which can result in loss of bone density. An estimated 34 million people in the United States have osteopenia.
Dr. Bilek said a next step for the study is to enroll a more diverse cohort at an additional center to test the device because most of the women in this one were White.
She noted that women’s bone mass peaks at age 30 and then starts to decline.
“When women hit menopause, there’s a really rapid decline [in bone strength] for the next 5-7 years and then the decline levels off. If we can slow that decline, hopefully that woman’s bone density is maintained at a higher level throughout their life,” Dr. Bilek said.
Dr. Bilek is a scientific adviser to Bone Health Technologies. She and many coauthors of the study received grants or fees from the company and own stock in or are employees of the company. Ms. Yecies is the founder and CEO of Bone Health Technologies. Dr. Khandelwal had no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The US Food and Drug Administration (FDA) has approved a wearable belt device for postmenopausal women with osteopenia, the precursor to osteoporosis, according to the company’s manufacturer, Bone Health Technologies.
According to the company, the device (Osteoboost) is the first nonpharmacologic device-based, prescription-only treatment for postmenopausal women with low bone density. It has not been tested for ability to reduce fracture risk.
The device is worn around the hips and delivers calibrated mild vibrations to the hips and lumbar spine to help preserve bone strength and density. A vibration pack is mounted to the back of the belt.
FDA approval, announced on January 18, was based on the findings of a National Institutes of Health–funded double-blinded, sham-controlled study of 126 women with low bone density conducted at the University of Nebraska Medical Center in Omaha. The data were shared at the 2023 Endocrine Society and American Society for Bone and Mineral Research annual meetings and published in the Journal of the Endocrine Society.
Lead investigator Laura D. Bilek, PT, PhD, associate dean for research and associate professor at the University of Nebraska, and colleagues wrote that the primary outcome measurement was the change in vertebral strength measured by CT scans for women who used the device a minimum of three times per week compared with a sham group who wore a belt that emitted sound but had no vibrations.
Compressive strength and volumetric density of the first lumbar vertebra were analyzed.
In the active-belt group, women lost, on average, 0.48% bone strength, while those in the sham group lost nearly 2.84% (P = .014), about five times as much. Results also showed that participants in the active treatment group who used the device three times per week lost 0.29% bone mineral density (BMD) compared with the 1.97% BMD lost in the control group. No adverse events were reported in the study.
Sonali Khandelwal, MD, a rheumatologist at Rush University in Chicago, told this news organization there’s considerable fear among some patients about long-term use of available medications for bone health, “so any modality that is nontherapeutic — not a pill — is always exciting.”
The endpoints of the study are one good measure, she said, but she emphasized that it will be important to show that the improved bone density from the belt that is described in this study “is a true marker of decreased fracture risk.”
Because there are no apparent side effects, she said it may be effective in combination with weight-bearing exercise, vitamin D and calcium, and/or medication, depending on severity of bone loss.
Current medications on the market for osteoporosis have been shown to improve bone strength and reduce fracture risk, she noted.
“It could help; I just don’t think we have enough evidence that it will completely treat the bone loss,” Dr. Khandelwal said.
She said she sees the potential population most interested in the belt as premenopausal women with a family history of bone loss who may not meet the level of bone loss for medical management but are interested in prevention.
“I also think of individuals who might already meet medication needs but are completely averse to being on medication,” she said. The bulk of her practice is treating bone loss, she said, estimating that 20% of her patients do not want to be on medication.
Bone Health Technologies CEO Laura Yecies, MBA, told this news organization the company has not yet set the price for the device and noted that because it will be available by prescription only, out-of-pocket costs and copays will differ. She said the company expects to begin shipping later this year. Requests for update notifications can be made at the company’s website.
Dr. Bilek told this news organization the device was tested for a year, so it’s unclear how long people with osteopenia would need to wear the belt for maximum benefit.
The theory behind the mechanism of action, she said, “is that the vibration actually inhibits the cells [osteoclasts] that take away bone mass.”
The researchers included only postmenopausal women with osteopenia in the study, but Dr. Bilek said she would like to test the device on other groups, such as men with prostate cancer getting testosterone-blocking therapy, which can result in loss of bone density. An estimated 34 million people in the United States have osteopenia.
Dr. Bilek said a next step for the study is to enroll a more diverse cohort at an additional center to test the device because most of the women in this one were White.
She noted that women’s bone mass peaks at age 30 and then starts to decline.
“When women hit menopause, there’s a really rapid decline [in bone strength] for the next 5-7 years and then the decline levels off. If we can slow that decline, hopefully that woman’s bone density is maintained at a higher level throughout their life,” Dr. Bilek said.
Dr. Bilek is a scientific adviser to Bone Health Technologies. She and many coauthors of the study received grants or fees from the company and own stock in or are employees of the company. Ms. Yecies is the founder and CEO of Bone Health Technologies. Dr. Khandelwal had no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Weight Loss Not Enough to Sustain Type 2 Diabetes Remission
Very few patients with type 2 diabetes (T2D) achieve and sustain diabetes remission via weight loss alone, new research suggests.
Among more than 37,000 people with T2D in Hong Kong, only 6% had achieved and sustained diabetes remission solely through weight loss up to 8 years after diagnosis. Among those who initially achieved remission, 67% had hyperglycemia at 3 years.
People who lost the most weight (10% of their body weight or more) in the first year after diagnosis were most likely to have sustained remission.
The study “helped to confirm the low rate of diabetes remission and high rate of returning to hyperglycemia in real-world practice,” Andrea Luk, MD, of the Chinese University of Hong Kong, told this news organization. “Over 80% of diabetes remission occurred within the first 5 years of a diabetes diagnosis. This is in line with our understanding that beta cell function will gradually decline over time, making diabetes remission increasingly difficult even with weight reduction.”
The study was published in PLOS Medicine.
Early Weight Management Works
Recent clinical trials have demonstrated that T2D remission can be achieved following sustained weight loss through bariatric surgery or lifestyle interventions, the authors noted. In this study, they investigated the association of weight change at 1 year after a diabetes diagnosis with the long-term incidence and sustainability of T2D remission in real-world settings, using data from the territory-wide Risk Assessment and Management Programme-Diabetes Mellitus (RAMP-DM).
A total of 37,326 people with newly diagnosed T2D who were enrolled in the RAMP-DM between 2000 and 2017 were included and followed until 2019.
At baseline, participants’ mean age was 56.6 years, mean body mass index (BMI) was 26.4 kg/m2, and mean A1c was 7.7%, and 65% were using glucose-lowering drugs (GLDs).
T2D remission was defined as two consecutive A1c < 6.5% measurements at least 6 months apart without GLDs currently or in the previous 3 months.
During a median follow-up of 7.9 years, 6.1% of people achieved remission, with an incidence rate of 7.8 per 1000 person-years. The proportion was higher among those with greater weight loss: 14.4% of people who lost 10% of their body weight or more achieved remission compared with 9.9% of those with 5%-9.9% weight loss, 6.5% of those with 0%-4.9% weight loss, and 4.5% of those who gained weight.
After adjustment for age at diagnosis, sex, assessment year, BMI, other metabolic indices, smoking, alcohol drinking, and medication use, the hazard ratio (HR) for diabetes remission was 3.28 for those with 10% or greater weight loss within 1 year of diagnosis, 2.29 for 5%-9.9% weight loss, and 1.34 for 0%-4.9% weight loss compared to weight gain.
The incidence of diabetes remission in the study was significantly lower than that in clinical trials, possibly because trial participants were in structured programs that included intensive lifestyle interventions, regular monitoring and feedback, and reinforcement of a holistic approach to managing diabetes, the authors noted. Real-world settings may or may not include such interventions.
Further analyses showed that within a median follow-up of 3.1 years, 67.2% of people who had achieved diabetes remission returned to hyperglycemia — an incidence rate of 184.8 per 1000 person-years.
The adjusted HR for returning to hyperglycemia was 0.52 for people with 10% or greater weight loss, 0.78 for those with 5%-9.9% weight loss, and 0.90 for those with 0%-4.9% weight loss compared to people with weight gain.
In addition, diabetes remission was associated with a 31% (HR, 0.69) decreased risk for all-cause mortality.
The study “provides evidence for policymakers to design and implement early weight management interventions” for people diagnosed with T2D, the authors concluded.
Clinicians also have a role to play, Dr. Luk said. “At the first encounter with an individual with newly diagnosed T2D, clinicians should emphasize the importance of weight reduction and guide the individual on how this can be achieved through making healthy lifestyle choices. Pharmacotherapy and metabolic surgery for weight management can be considered in appropriate individuals.”
Overall, she added, “clinicians should be informed that the likelihood of achieving and maintaining diabetes remission is low, and patients should be counseled accordingly.”
Similar to US Experience
Mona Mshayekhi, MD, PhD, an assistant professor of medicine in the division of Diabetes, Endocrinology and Metabolism at Vanderbilt University Medical Center, Nashville, Tennessee, commented on the study for this news organization.
“These findings mirror clinical experience in the US very well,” she said. “We know that sustained weight loss without the use of medications or surgery is extremely difficult in the real-world setting due to the hormonal drivers of obesity, in combination with socioeconomic challenges.”
The study was done before newer weight-management strategies such as glucagon-like peptide 1 receptor agonists were widely available, she noted. “This actually strengthens the finding that weight loss without the routine use of medications has a multitude of benefits, including diabetes remission and reduction of all-cause mortality.”
That said, she added, “I suspect that future studies with more modern cohorts will reveal much higher rates of diabetes remission with the use of newer medications.”
“Our ability to help our patients lose meaningful weight has been limited until recently,” she said. “With new tools in our armamentarium, clinicians need to take the lead in helping patients address and treat obesity and fight the stigma that prevents many from even discussing it with their providers.”
The study did not receive funding. Dr. Luk has received research grants or contracts from Amgen, AstraZeneca, Bayer, Biogen, Boehringer Ingelheim, Eli Lilly, Junshi, Lee Pharmaceutical, MSD, Novo Nordisk, Roche, Sanofi, Shanghai Junshi Biosciences, Sugardown, and Takeda and received travel grants and honoraria for speaking from AstraZeneca, Boehringer Ingelheim, Eli Lilly, and MSD. Dr. Mshayekhi reported no conflicts of interest.
A version of this article appeared on Medscape.com.
Very few patients with type 2 diabetes (T2D) achieve and sustain diabetes remission via weight loss alone, new research suggests.
Among more than 37,000 people with T2D in Hong Kong, only 6% had achieved and sustained diabetes remission solely through weight loss up to 8 years after diagnosis. Among those who initially achieved remission, 67% had hyperglycemia at 3 years.
People who lost the most weight (10% of their body weight or more) in the first year after diagnosis were most likely to have sustained remission.
The study “helped to confirm the low rate of diabetes remission and high rate of returning to hyperglycemia in real-world practice,” Andrea Luk, MD, of the Chinese University of Hong Kong, told this news organization. “Over 80% of diabetes remission occurred within the first 5 years of a diabetes diagnosis. This is in line with our understanding that beta cell function will gradually decline over time, making diabetes remission increasingly difficult even with weight reduction.”
The study was published in PLOS Medicine.
Early Weight Management Works
Recent clinical trials have demonstrated that T2D remission can be achieved following sustained weight loss through bariatric surgery or lifestyle interventions, the authors noted. In this study, they investigated the association of weight change at 1 year after a diabetes diagnosis with the long-term incidence and sustainability of T2D remission in real-world settings, using data from the territory-wide Risk Assessment and Management Programme-Diabetes Mellitus (RAMP-DM).
A total of 37,326 people with newly diagnosed T2D who were enrolled in the RAMP-DM between 2000 and 2017 were included and followed until 2019.
At baseline, participants’ mean age was 56.6 years, mean body mass index (BMI) was 26.4 kg/m2, and mean A1c was 7.7%, and 65% were using glucose-lowering drugs (GLDs).
T2D remission was defined as two consecutive A1c < 6.5% measurements at least 6 months apart without GLDs currently or in the previous 3 months.
During a median follow-up of 7.9 years, 6.1% of people achieved remission, with an incidence rate of 7.8 per 1000 person-years. The proportion was higher among those with greater weight loss: 14.4% of people who lost 10% of their body weight or more achieved remission compared with 9.9% of those with 5%-9.9% weight loss, 6.5% of those with 0%-4.9% weight loss, and 4.5% of those who gained weight.
After adjustment for age at diagnosis, sex, assessment year, BMI, other metabolic indices, smoking, alcohol drinking, and medication use, the hazard ratio (HR) for diabetes remission was 3.28 for those with 10% or greater weight loss within 1 year of diagnosis, 2.29 for 5%-9.9% weight loss, and 1.34 for 0%-4.9% weight loss compared to weight gain.
The incidence of diabetes remission in the study was significantly lower than that in clinical trials, possibly because trial participants were in structured programs that included intensive lifestyle interventions, regular monitoring and feedback, and reinforcement of a holistic approach to managing diabetes, the authors noted. Real-world settings may or may not include such interventions.
Further analyses showed that within a median follow-up of 3.1 years, 67.2% of people who had achieved diabetes remission returned to hyperglycemia — an incidence rate of 184.8 per 1000 person-years.
The adjusted HR for returning to hyperglycemia was 0.52 for people with 10% or greater weight loss, 0.78 for those with 5%-9.9% weight loss, and 0.90 for those with 0%-4.9% weight loss compared to people with weight gain.
In addition, diabetes remission was associated with a 31% (HR, 0.69) decreased risk for all-cause mortality.
The study “provides evidence for policymakers to design and implement early weight management interventions” for people diagnosed with T2D, the authors concluded.
Clinicians also have a role to play, Dr. Luk said. “At the first encounter with an individual with newly diagnosed T2D, clinicians should emphasize the importance of weight reduction and guide the individual on how this can be achieved through making healthy lifestyle choices. Pharmacotherapy and metabolic surgery for weight management can be considered in appropriate individuals.”
Overall, she added, “clinicians should be informed that the likelihood of achieving and maintaining diabetes remission is low, and patients should be counseled accordingly.”
Similar to US Experience
Mona Mshayekhi, MD, PhD, an assistant professor of medicine in the division of Diabetes, Endocrinology and Metabolism at Vanderbilt University Medical Center, Nashville, Tennessee, commented on the study for this news organization.
“These findings mirror clinical experience in the US very well,” she said. “We know that sustained weight loss without the use of medications or surgery is extremely difficult in the real-world setting due to the hormonal drivers of obesity, in combination with socioeconomic challenges.”
The study was done before newer weight-management strategies such as glucagon-like peptide 1 receptor agonists were widely available, she noted. “This actually strengthens the finding that weight loss without the routine use of medications has a multitude of benefits, including diabetes remission and reduction of all-cause mortality.”
That said, she added, “I suspect that future studies with more modern cohorts will reveal much higher rates of diabetes remission with the use of newer medications.”
“Our ability to help our patients lose meaningful weight has been limited until recently,” she said. “With new tools in our armamentarium, clinicians need to take the lead in helping patients address and treat obesity and fight the stigma that prevents many from even discussing it with their providers.”
The study did not receive funding. Dr. Luk has received research grants or contracts from Amgen, AstraZeneca, Bayer, Biogen, Boehringer Ingelheim, Eli Lilly, Junshi, Lee Pharmaceutical, MSD, Novo Nordisk, Roche, Sanofi, Shanghai Junshi Biosciences, Sugardown, and Takeda and received travel grants and honoraria for speaking from AstraZeneca, Boehringer Ingelheim, Eli Lilly, and MSD. Dr. Mshayekhi reported no conflicts of interest.
A version of this article appeared on Medscape.com.
Very few patients with type 2 diabetes (T2D) achieve and sustain diabetes remission via weight loss alone, new research suggests.
Among more than 37,000 people with T2D in Hong Kong, only 6% had achieved and sustained diabetes remission solely through weight loss up to 8 years after diagnosis. Among those who initially achieved remission, 67% had hyperglycemia at 3 years.
People who lost the most weight (10% of their body weight or more) in the first year after diagnosis were most likely to have sustained remission.
The study “helped to confirm the low rate of diabetes remission and high rate of returning to hyperglycemia in real-world practice,” Andrea Luk, MD, of the Chinese University of Hong Kong, told this news organization. “Over 80% of diabetes remission occurred within the first 5 years of a diabetes diagnosis. This is in line with our understanding that beta cell function will gradually decline over time, making diabetes remission increasingly difficult even with weight reduction.”
The study was published in PLOS Medicine.
Early Weight Management Works
Recent clinical trials have demonstrated that T2D remission can be achieved following sustained weight loss through bariatric surgery or lifestyle interventions, the authors noted. In this study, they investigated the association of weight change at 1 year after a diabetes diagnosis with the long-term incidence and sustainability of T2D remission in real-world settings, using data from the territory-wide Risk Assessment and Management Programme-Diabetes Mellitus (RAMP-DM).
A total of 37,326 people with newly diagnosed T2D who were enrolled in the RAMP-DM between 2000 and 2017 were included and followed until 2019.
At baseline, participants’ mean age was 56.6 years, mean body mass index (BMI) was 26.4 kg/m2, and mean A1c was 7.7%, and 65% were using glucose-lowering drugs (GLDs).
T2D remission was defined as two consecutive A1c < 6.5% measurements at least 6 months apart without GLDs currently or in the previous 3 months.
During a median follow-up of 7.9 years, 6.1% of people achieved remission, with an incidence rate of 7.8 per 1000 person-years. The proportion was higher among those with greater weight loss: 14.4% of people who lost 10% of their body weight or more achieved remission compared with 9.9% of those with 5%-9.9% weight loss, 6.5% of those with 0%-4.9% weight loss, and 4.5% of those who gained weight.
After adjustment for age at diagnosis, sex, assessment year, BMI, other metabolic indices, smoking, alcohol drinking, and medication use, the hazard ratio (HR) for diabetes remission was 3.28 for those with 10% or greater weight loss within 1 year of diagnosis, 2.29 for 5%-9.9% weight loss, and 1.34 for 0%-4.9% weight loss compared to weight gain.
The incidence of diabetes remission in the study was significantly lower than that in clinical trials, possibly because trial participants were in structured programs that included intensive lifestyle interventions, regular monitoring and feedback, and reinforcement of a holistic approach to managing diabetes, the authors noted. Real-world settings may or may not include such interventions.
Further analyses showed that within a median follow-up of 3.1 years, 67.2% of people who had achieved diabetes remission returned to hyperglycemia — an incidence rate of 184.8 per 1000 person-years.
The adjusted HR for returning to hyperglycemia was 0.52 for people with 10% or greater weight loss, 0.78 for those with 5%-9.9% weight loss, and 0.90 for those with 0%-4.9% weight loss compared to people with weight gain.
In addition, diabetes remission was associated with a 31% (HR, 0.69) decreased risk for all-cause mortality.
The study “provides evidence for policymakers to design and implement early weight management interventions” for people diagnosed with T2D, the authors concluded.
Clinicians also have a role to play, Dr. Luk said. “At the first encounter with an individual with newly diagnosed T2D, clinicians should emphasize the importance of weight reduction and guide the individual on how this can be achieved through making healthy lifestyle choices. Pharmacotherapy and metabolic surgery for weight management can be considered in appropriate individuals.”
Overall, she added, “clinicians should be informed that the likelihood of achieving and maintaining diabetes remission is low, and patients should be counseled accordingly.”
Similar to US Experience
Mona Mshayekhi, MD, PhD, an assistant professor of medicine in the division of Diabetes, Endocrinology and Metabolism at Vanderbilt University Medical Center, Nashville, Tennessee, commented on the study for this news organization.
“These findings mirror clinical experience in the US very well,” she said. “We know that sustained weight loss without the use of medications or surgery is extremely difficult in the real-world setting due to the hormonal drivers of obesity, in combination with socioeconomic challenges.”
The study was done before newer weight-management strategies such as glucagon-like peptide 1 receptor agonists were widely available, she noted. “This actually strengthens the finding that weight loss without the routine use of medications has a multitude of benefits, including diabetes remission and reduction of all-cause mortality.”
That said, she added, “I suspect that future studies with more modern cohorts will reveal much higher rates of diabetes remission with the use of newer medications.”
“Our ability to help our patients lose meaningful weight has been limited until recently,” she said. “With new tools in our armamentarium, clinicians need to take the lead in helping patients address and treat obesity and fight the stigma that prevents many from even discussing it with their providers.”
The study did not receive funding. Dr. Luk has received research grants or contracts from Amgen, AstraZeneca, Bayer, Biogen, Boehringer Ingelheim, Eli Lilly, Junshi, Lee Pharmaceutical, MSD, Novo Nordisk, Roche, Sanofi, Shanghai Junshi Biosciences, Sugardown, and Takeda and received travel grants and honoraria for speaking from AstraZeneca, Boehringer Ingelheim, Eli Lilly, and MSD. Dr. Mshayekhi reported no conflicts of interest.
A version of this article appeared on Medscape.com.
FROM PLOS MEDICINE
A Military Nurse Saves a Life After a Brutal Rollover Crash
Emergencies happen anywhere and anytime, and sometimes, medical professionals find themselves in situations where they are the only ones who can help. Is There a Doctor in the House? is a series telling these stories.
A week earlier I’d had a heart surgery and was heading out for a post-op appointment when I saw it: I had a flat tire. It didn’t make sense. The tire was brand new, and there was no puncture. But it was flat.
I swapped out the flat for the spare and went off base to a tire shop. While I was there, my surgeon’s office called and rescheduled my appointment for a couple of hours later. That was lucky because by the time the tire was fixed, I had just enough time to get there.
The hospital is right near I-35 in San Antonio, Texas. I got off the freeway and onto the access road and paused to turn into the parking lot. That’s when I heard an enormous crash.
I saw a big poof of white smoke, and a car barreled off the freeway and came rolling down the embankment.
When the car hit the access road, I saw a woman ejected through the windshield. She bounced and landed in the road about 25 feet in front of me.
I put my car in park, grabbed my face mask and gloves, and started running toward her. But another vehicle — a truck towing a trailer — came from behind to drive around me. The driver didn’t realize what had happened and couldn’t stop in time…
The trailer ran over her.
I didn’t know if anyone could’ve survived that, but I went to her. I saw several other bystanders, but they were frozen in shock. I was praying, dear God, if she’s alive, let me do whatever I need to do to save her life.
It was a horrible scene. This poor lady was in a bloody heap in the middle of the road. Her right arm was twisted up under her neck so tightly, she was choking herself. So, the first thing I did was straighten her arm out to protect her airway.
I started yelling at people, “Call 9-1-1! Run to the hospital! Let them know there’s an accident out here, and I need help!”
The woman had a pulse, but it was super rapid. On first glance, she clearly had multiple fractures and a bad head bleed. With the sheer number of times she’d been injured, I didn’t know what was going on internally, but it was bad. She was gargling on her own blood and spitting it up. She was drowning.
A couple of technicians from the hospital came and brought me a tiny emergency kit. It had a blood pressure cuff and an oral airway. All the vital signs indicated the lady was going into shock. She’d lost a lot of blood on the pavement.
I was able to get the oral airway in. A few minutes later, a fire chief showed up. By now, the traffic had backed up so badly, the emergency vehicles couldn’t get in. But he managed to get there another way and gave me a cervical collar (C collar) and an Ambu bag.
I was hyper-focused on what I could do at that moment and what I needed to do next. Her stats were going down, but she still had a pulse. If she lost the pulse or went into a lethal rhythm, I’d have to start cardiopulmonary resuscitation (CPR). I asked the other people, but nobody else knew CPR, so I wouldn’t have help.
I could tell the lady had a pelvic fracture, and we needed to stabilize her. I directed people how to hold her neck safely and log-roll her flat on the ground. I also needed to put pressure on the back of her head because of all the bleeding. I got people to give me their clothes and tried to do that as I was bagging her.
The windows of her vehicle had all been blown out. I asked somebody to go find her purse with her ID. Then I noticed something …
My heart jumped into my stomach.
A car seat. There was an empty child’s car seat in the back of the car.
I started yelling at everyone, “Look for a baby! Go up and down the embankment and across the road. There might have been a baby in the car!”
But there wasn’t. Thank God. She hadn’t been driving with her child.
At that point, a paramedic came running from behind all the traffic. We did life support together until the ambulance finally arrived.
Emergency medical services got an intravenous line in and used medical anti-shock trousers. Thankfully, I already had the C collar on, and we’d been bagging her, so they could load her very quickly.
I got rid of my bloody gloves. I told a police officer I would come back. And then I went to my doctor’s appointment.
The window at my doctor’s office faced the access road, so the people there had seen all the traffic. They asked me what happened, and I said, “It was me. I saw it happen. I tried to help.” I was a little frazzled.
When I got back to the scene, the police and the fire chief kept thanking me for stopping. Why wouldn’t I stop? It was astounding to realize that they imagined somebody wouldn’t stop in a situation like this.
They told me the lady was alive. She was in the intensive care unit in critical condition, but she had survived. At that moment, I had this overwhelming feeling: God had put me in this exact place at the exact time to save her life.
Looking back, I think about how God ordered my steps. Without the mysterious flat tire, I would’ve gone to the hospital earlier. If my appointment hadn’t been rescheduled, I wouldn’t have been on the access road. All those events brought me there.
Several months later, the woman’s family contacted me and asked if we could meet. I found out more about her injuries. She’d had multiple skull fractures, facial fractures, and a broken jaw. Her upper arm was broken in three places. Her clavicle was broken. She had internal bleeding, a pelvic fracture, and a broken leg. She was 28 years old.
She’d had multiple surgeries, spent 2 months in the ICU, and another 3 months in intensive rehab. But she survived. It was incredible.
We all met up at a McDonald’s. First, her little son — who was the baby I thought might have been in the car — ran up to me and said, “Thank you for saving my mommy’s life.”
Then I turned, and there she was — a beautiful lady looking at me with awe and crying, saying, “It’s me.”
She obviously had gone through a transformation from all the injuries and the medications. She had a little bit of a speech delay, but mentally, she was there. She could walk.
She said, “You’re my angel. God put you there to save my life.” Her family all came up and hugged me. It was so beautiful.
She told me about the accident. She’d been speeding that day, zigzagging through lanes to get around the traffic. And she didn’t have her seatbelt on. She’d driven onto the shoulder to try to pass everyone, but it started narrowing. She clipped somebody’s bumper, went into a tailspin, and collided with a second vehicle, which caused her to flip over and down the embankment.
“God’s given me a new lease on life,” she said, “a fresh start. I will forever wear my seatbelt. And I’m going to do whatever I can to give back to other people because I don’t even feel like I deserve this.”
I just cried.
I’ve been a nurse for 29 years, first on the civilian side and later in the military. I’ve led codes and responded to trauma in a hospital setting or a deployed environment. I was well prepared to do what I did. But doing it under such stress with adrenaline bombarding me ... I’m amazed. I just think God’s hand was on me.
At that time, I was personally going through some things. After my heart surgery, I was in an emotional place where I didn’t feel loved or valued. But when I had that realization — when I knew that I was meant to be there to save her life, I also got the very clear message that I was valued and loved so much.
I know I have a very strong purpose. That day changed my life.
US Air Force Lt. Col. Anne Staley is the officer in charge of the Military Training Network, a division of the Defense Health Agency Education and Training Directorate in San Antonio, Texas.
A version of this article appeared on Medscape.com.
Emergencies happen anywhere and anytime, and sometimes, medical professionals find themselves in situations where they are the only ones who can help. Is There a Doctor in the House? is a series telling these stories.
A week earlier I’d had a heart surgery and was heading out for a post-op appointment when I saw it: I had a flat tire. It didn’t make sense. The tire was brand new, and there was no puncture. But it was flat.
I swapped out the flat for the spare and went off base to a tire shop. While I was there, my surgeon’s office called and rescheduled my appointment for a couple of hours later. That was lucky because by the time the tire was fixed, I had just enough time to get there.
The hospital is right near I-35 in San Antonio, Texas. I got off the freeway and onto the access road and paused to turn into the parking lot. That’s when I heard an enormous crash.
I saw a big poof of white smoke, and a car barreled off the freeway and came rolling down the embankment.
When the car hit the access road, I saw a woman ejected through the windshield. She bounced and landed in the road about 25 feet in front of me.
I put my car in park, grabbed my face mask and gloves, and started running toward her. But another vehicle — a truck towing a trailer — came from behind to drive around me. The driver didn’t realize what had happened and couldn’t stop in time…
The trailer ran over her.
I didn’t know if anyone could’ve survived that, but I went to her. I saw several other bystanders, but they were frozen in shock. I was praying, dear God, if she’s alive, let me do whatever I need to do to save her life.
It was a horrible scene. This poor lady was in a bloody heap in the middle of the road. Her right arm was twisted up under her neck so tightly, she was choking herself. So, the first thing I did was straighten her arm out to protect her airway.
I started yelling at people, “Call 9-1-1! Run to the hospital! Let them know there’s an accident out here, and I need help!”
The woman had a pulse, but it was super rapid. On first glance, she clearly had multiple fractures and a bad head bleed. With the sheer number of times she’d been injured, I didn’t know what was going on internally, but it was bad. She was gargling on her own blood and spitting it up. She was drowning.
A couple of technicians from the hospital came and brought me a tiny emergency kit. It had a blood pressure cuff and an oral airway. All the vital signs indicated the lady was going into shock. She’d lost a lot of blood on the pavement.
I was able to get the oral airway in. A few minutes later, a fire chief showed up. By now, the traffic had backed up so badly, the emergency vehicles couldn’t get in. But he managed to get there another way and gave me a cervical collar (C collar) and an Ambu bag.
I was hyper-focused on what I could do at that moment and what I needed to do next. Her stats were going down, but she still had a pulse. If she lost the pulse or went into a lethal rhythm, I’d have to start cardiopulmonary resuscitation (CPR). I asked the other people, but nobody else knew CPR, so I wouldn’t have help.
I could tell the lady had a pelvic fracture, and we needed to stabilize her. I directed people how to hold her neck safely and log-roll her flat on the ground. I also needed to put pressure on the back of her head because of all the bleeding. I got people to give me their clothes and tried to do that as I was bagging her.
The windows of her vehicle had all been blown out. I asked somebody to go find her purse with her ID. Then I noticed something …
My heart jumped into my stomach.
A car seat. There was an empty child’s car seat in the back of the car.
I started yelling at everyone, “Look for a baby! Go up and down the embankment and across the road. There might have been a baby in the car!”
But there wasn’t. Thank God. She hadn’t been driving with her child.
At that point, a paramedic came running from behind all the traffic. We did life support together until the ambulance finally arrived.
Emergency medical services got an intravenous line in and used medical anti-shock trousers. Thankfully, I already had the C collar on, and we’d been bagging her, so they could load her very quickly.
I got rid of my bloody gloves. I told a police officer I would come back. And then I went to my doctor’s appointment.
The window at my doctor’s office faced the access road, so the people there had seen all the traffic. They asked me what happened, and I said, “It was me. I saw it happen. I tried to help.” I was a little frazzled.
When I got back to the scene, the police and the fire chief kept thanking me for stopping. Why wouldn’t I stop? It was astounding to realize that they imagined somebody wouldn’t stop in a situation like this.
They told me the lady was alive. She was in the intensive care unit in critical condition, but she had survived. At that moment, I had this overwhelming feeling: God had put me in this exact place at the exact time to save her life.
Looking back, I think about how God ordered my steps. Without the mysterious flat tire, I would’ve gone to the hospital earlier. If my appointment hadn’t been rescheduled, I wouldn’t have been on the access road. All those events brought me there.
Several months later, the woman’s family contacted me and asked if we could meet. I found out more about her injuries. She’d had multiple skull fractures, facial fractures, and a broken jaw. Her upper arm was broken in three places. Her clavicle was broken. She had internal bleeding, a pelvic fracture, and a broken leg. She was 28 years old.
She’d had multiple surgeries, spent 2 months in the ICU, and another 3 months in intensive rehab. But she survived. It was incredible.
We all met up at a McDonald’s. First, her little son — who was the baby I thought might have been in the car — ran up to me and said, “Thank you for saving my mommy’s life.”
Then I turned, and there she was — a beautiful lady looking at me with awe and crying, saying, “It’s me.”
She obviously had gone through a transformation from all the injuries and the medications. She had a little bit of a speech delay, but mentally, she was there. She could walk.
She said, “You’re my angel. God put you there to save my life.” Her family all came up and hugged me. It was so beautiful.
She told me about the accident. She’d been speeding that day, zigzagging through lanes to get around the traffic. And she didn’t have her seatbelt on. She’d driven onto the shoulder to try to pass everyone, but it started narrowing. She clipped somebody’s bumper, went into a tailspin, and collided with a second vehicle, which caused her to flip over and down the embankment.
“God’s given me a new lease on life,” she said, “a fresh start. I will forever wear my seatbelt. And I’m going to do whatever I can to give back to other people because I don’t even feel like I deserve this.”
I just cried.
I’ve been a nurse for 29 years, first on the civilian side and later in the military. I’ve led codes and responded to trauma in a hospital setting or a deployed environment. I was well prepared to do what I did. But doing it under such stress with adrenaline bombarding me ... I’m amazed. I just think God’s hand was on me.
At that time, I was personally going through some things. After my heart surgery, I was in an emotional place where I didn’t feel loved or valued. But when I had that realization — when I knew that I was meant to be there to save her life, I also got the very clear message that I was valued and loved so much.
I know I have a very strong purpose. That day changed my life.
US Air Force Lt. Col. Anne Staley is the officer in charge of the Military Training Network, a division of the Defense Health Agency Education and Training Directorate in San Antonio, Texas.
A version of this article appeared on Medscape.com.
Emergencies happen anywhere and anytime, and sometimes, medical professionals find themselves in situations where they are the only ones who can help. Is There a Doctor in the House? is a series telling these stories.
A week earlier I’d had a heart surgery and was heading out for a post-op appointment when I saw it: I had a flat tire. It didn’t make sense. The tire was brand new, and there was no puncture. But it was flat.
I swapped out the flat for the spare and went off base to a tire shop. While I was there, my surgeon’s office called and rescheduled my appointment for a couple of hours later. That was lucky because by the time the tire was fixed, I had just enough time to get there.
The hospital is right near I-35 in San Antonio, Texas. I got off the freeway and onto the access road and paused to turn into the parking lot. That’s when I heard an enormous crash.
I saw a big poof of white smoke, and a car barreled off the freeway and came rolling down the embankment.
When the car hit the access road, I saw a woman ejected through the windshield. She bounced and landed in the road about 25 feet in front of me.
I put my car in park, grabbed my face mask and gloves, and started running toward her. But another vehicle — a truck towing a trailer — came from behind to drive around me. The driver didn’t realize what had happened and couldn’t stop in time…
The trailer ran over her.
I didn’t know if anyone could’ve survived that, but I went to her. I saw several other bystanders, but they were frozen in shock. I was praying, dear God, if she’s alive, let me do whatever I need to do to save her life.
It was a horrible scene. This poor lady was in a bloody heap in the middle of the road. Her right arm was twisted up under her neck so tightly, she was choking herself. So, the first thing I did was straighten her arm out to protect her airway.
I started yelling at people, “Call 9-1-1! Run to the hospital! Let them know there’s an accident out here, and I need help!”
The woman had a pulse, but it was super rapid. On first glance, she clearly had multiple fractures and a bad head bleed. With the sheer number of times she’d been injured, I didn’t know what was going on internally, but it was bad. She was gargling on her own blood and spitting it up. She was drowning.
A couple of technicians from the hospital came and brought me a tiny emergency kit. It had a blood pressure cuff and an oral airway. All the vital signs indicated the lady was going into shock. She’d lost a lot of blood on the pavement.
I was able to get the oral airway in. A few minutes later, a fire chief showed up. By now, the traffic had backed up so badly, the emergency vehicles couldn’t get in. But he managed to get there another way and gave me a cervical collar (C collar) and an Ambu bag.
I was hyper-focused on what I could do at that moment and what I needed to do next. Her stats were going down, but she still had a pulse. If she lost the pulse or went into a lethal rhythm, I’d have to start cardiopulmonary resuscitation (CPR). I asked the other people, but nobody else knew CPR, so I wouldn’t have help.
I could tell the lady had a pelvic fracture, and we needed to stabilize her. I directed people how to hold her neck safely and log-roll her flat on the ground. I also needed to put pressure on the back of her head because of all the bleeding. I got people to give me their clothes and tried to do that as I was bagging her.
The windows of her vehicle had all been blown out. I asked somebody to go find her purse with her ID. Then I noticed something …
My heart jumped into my stomach.
A car seat. There was an empty child’s car seat in the back of the car.
I started yelling at everyone, “Look for a baby! Go up and down the embankment and across the road. There might have been a baby in the car!”
But there wasn’t. Thank God. She hadn’t been driving with her child.
At that point, a paramedic came running from behind all the traffic. We did life support together until the ambulance finally arrived.
Emergency medical services got an intravenous line in and used medical anti-shock trousers. Thankfully, I already had the C collar on, and we’d been bagging her, so they could load her very quickly.
I got rid of my bloody gloves. I told a police officer I would come back. And then I went to my doctor’s appointment.
The window at my doctor’s office faced the access road, so the people there had seen all the traffic. They asked me what happened, and I said, “It was me. I saw it happen. I tried to help.” I was a little frazzled.
When I got back to the scene, the police and the fire chief kept thanking me for stopping. Why wouldn’t I stop? It was astounding to realize that they imagined somebody wouldn’t stop in a situation like this.
They told me the lady was alive. She was in the intensive care unit in critical condition, but she had survived. At that moment, I had this overwhelming feeling: God had put me in this exact place at the exact time to save her life.
Looking back, I think about how God ordered my steps. Without the mysterious flat tire, I would’ve gone to the hospital earlier. If my appointment hadn’t been rescheduled, I wouldn’t have been on the access road. All those events brought me there.
Several months later, the woman’s family contacted me and asked if we could meet. I found out more about her injuries. She’d had multiple skull fractures, facial fractures, and a broken jaw. Her upper arm was broken in three places. Her clavicle was broken. She had internal bleeding, a pelvic fracture, and a broken leg. She was 28 years old.
She’d had multiple surgeries, spent 2 months in the ICU, and another 3 months in intensive rehab. But she survived. It was incredible.
We all met up at a McDonald’s. First, her little son — who was the baby I thought might have been in the car — ran up to me and said, “Thank you for saving my mommy’s life.”
Then I turned, and there she was — a beautiful lady looking at me with awe and crying, saying, “It’s me.”
She obviously had gone through a transformation from all the injuries and the medications. She had a little bit of a speech delay, but mentally, she was there. She could walk.
She said, “You’re my angel. God put you there to save my life.” Her family all came up and hugged me. It was so beautiful.
She told me about the accident. She’d been speeding that day, zigzagging through lanes to get around the traffic. And she didn’t have her seatbelt on. She’d driven onto the shoulder to try to pass everyone, but it started narrowing. She clipped somebody’s bumper, went into a tailspin, and collided with a second vehicle, which caused her to flip over and down the embankment.
“God’s given me a new lease on life,” she said, “a fresh start. I will forever wear my seatbelt. And I’m going to do whatever I can to give back to other people because I don’t even feel like I deserve this.”
I just cried.
I’ve been a nurse for 29 years, first on the civilian side and later in the military. I’ve led codes and responded to trauma in a hospital setting or a deployed environment. I was well prepared to do what I did. But doing it under such stress with adrenaline bombarding me ... I’m amazed. I just think God’s hand was on me.
At that time, I was personally going through some things. After my heart surgery, I was in an emotional place where I didn’t feel loved or valued. But when I had that realization — when I knew that I was meant to be there to save her life, I also got the very clear message that I was valued and loved so much.
I know I have a very strong purpose. That day changed my life.
US Air Force Lt. Col. Anne Staley is the officer in charge of the Military Training Network, a division of the Defense Health Agency Education and Training Directorate in San Antonio, Texas.
A version of this article appeared on Medscape.com.
Blue to Slate Gray Discoloration of the Proximal Fingernails
The Diagnosis: Argyria-Induced Azure Lunulae
Argyria is an acquired condition resulting from excessive exogenous exposure to silver with subsequent gastrointestinal absorption and pigmentary tissue deposition. Upon further questioning, our patient disclosed a lifetime history of colloidal silver use, both as a topical antiseptic agent and intraorally for aphthous ulcers. Silver has a predilection for granular deposition in stromal tissues and basement membranes with sparing of the epidermis, manifesting as progressive, permanent, blue to slate gray discoloration of sunexposed skin, mucous membranes, and nail beds.1 The patient was advised to discontinue use of colloidal silver to avoid development of further pigmentary changes. The appearance of his nails remained unchanged in the months following initial presentation, as expected, since argyria pigmentation is not anticipated to reverse upon colloidal silver cessation.
Nail involvement may be an early presentation of generalized argyria or may be found in isolation, as seen in our patient. Early recognition and patient education are essential to minimize cumulative silver deposition. Although dyspigmentation may impact psychosocial well-being secondary to aesthetic concerns, there is limited research supporting adverse systemic effects of argyria confined to the nail beds. Similarly, the majority of generalized cases are not associated with systemic complications; however, potential toxicities, as described in isolated case reports without conclusive causal relationships, include nyctalopia, renal or hepatic toxicity, pulmonary fibrosis, and neuropsychiatric events.1-6 Successful treatment of cutaneous argyria has been reported with the 1064-nm Q-switched Nd:YAG laser; however, there have been no reported treatments for nail bed involvement.7 Due to the absence of systemic symptoms, additional mucocutaneous dyspigmentation, or cosmetic concerns regarding nail bed lunulae discoloration in our patient, no further intervention was pursued, except for continued colloidal silver cessation.
The differential diagnosis of blue-gray nail bed dyspigmentation is broad and includes cyanosis secondary to cardiopulmonary disease, drug-induced dyspigmentation, Wilson disease, argyria, chrysiasis, hereditary acrolabial telangiectasia, and pseudomonal infection or chloronychia.1,8,9 Etiologic insight may be provided from a thorough review of prescription and over-the-counter medications as well as careful attention to the distribution of dyspigmentation. Medications commonly associated with bluish nail bed dyspigmentation include antimalarials, amiodarone, minocycline, clofazimine, chlorpromazine/phenothiazines, and various chemotherapeutic drugs; our patient was not taking any of these.1,9
Cyanotic nail bed dyspigmentation secondary to cardiopulmonary disease likely manifests with more diffuse nail bed dyspigmentation and is not confined solely to the lunulae. Only drug-induced dyspigmentation, classically due to phenolphthalein-containing laxatives; Wilson disease; and argyria have a tendency to spare the distal nail bed, which is a presentation termed azure lunulae.8 The toenails typically are spared in argyria, while toenail involvement is variable in Wilson disease, and additional systemic symptoms—including hepatic, ophthalmologic, and neuropsychiatric—as well as potential family history would be expected.8 Phenolphthalein is no longer available in over-the-counter laxatives, as it was formally banned by the US Food and Drug Administration in 1999 due to concerns of carcinogenicity.10
Hereditary acrolabial telangiectasia is a familial condition with autosomal-dominant inheritance that can manifest similarly to argyria with blue-gray discoloration of the proximal nail bed; however, this condition also would demonstrate involvement of the vermilion border and nipple areolae, often with associated telangiectasia and migraine headaches.11
Chloronychia (also known as green nail syndrome) is an infection of the nail bed with Pseudomonas aeruginosa that more commonly presents with greenblack discoloration with variable involvement of the fingernails and toenails. Chloronychia, often with associated onycholysis, typically is found in individuals with repeated exposure to water, soaps, and detergents.12 Our patient’s long-standing and unwavering nail bed appearance, involvement of all fingernail lunulae, lack of additional symptoms, and disclosed use of over-the-counter colloidal silver supported a clinical diagnosis of argyriainduced azure lunulae.
Argyria-induced azure lunulae secondary to colloidal silver exposure is an uncommon yet clinically significant cause of nail bed dyspigmentation. Prompt identification and cessation of the offending agent can prevent progression of mucocutaneous dyspigmentation and avoid potential long-term sequelae from systemic deposition.
- Mota L, Dinis-Oliveira RJ. Clinical and forensic aspects of the different subtypes of argyria. J Clin Med. 2021;10:2086. doi:10.3390/ jcm10102086
- Osin´ska J, Poborc-Godlewska J, Kiec´-Swierczyn´ska M, et al. 6 cases of argyria among workers engaged in silverplating radio subunits. Med Pr. 1982;33:361-364.
- Mayr M, Kim MJ, Wanner D, et al. Argyria and decreased kidney function: are silver compounds toxic to the kidney? Am J Kidney Dis. 2009;53:890-894. doi:10.1053/j.ajkd.2008.08.028
- Trop M, Novak M, Rodl S, et al. Silver-coated dressing acticoat caused raised liver enzymes and argyria-like symptoms in burn patient. J Trauma. 2006;60:648-652. doi:10.1097/01.ta.0000208126 .22089.b6
- Mirsattari SM, Hammond RR, Sharpe MD, et al. Myoclonic status epilepticus following repeated oral ingestion of colloidal silver. Neurology. 2004;62:1408-1410. doi:10.1212/01.wnl.0000120671.73335.ec
- Barrie HJ, Harding HE. Argyro-siderosis of the lungs in silver finishers. Br J Ind Med. 1947;4:225-229. doi:10.1136/oem.4.4.225
- Griffith RD, Simmons BJ, Bray FN, et al. 1064 nm Q-switched Nd:YAG laser for the treatment of argyria: a systematic review. J Eur Acad Dermatol Venereol. 2015;29:2100-2103. doi:10.111 1/jdv.13117
- Rubin AI, Jellinek NJ, Daniel CR III, et al, eds. Scher and Daniel’s Nails: Diagnosis, Surgery, Therapy. 4th ed. Springer; 2018.
- Slater K, Sommariva E, Kartono F. A case study of argyria of the nails secondary to colloidal silver ingestion [published online October 28, 2022]. Cureus. 2022;14:E30818. doi:10.7759/cureus.30818
- Hubbard WK. Laxative drug products for over-the-counter human use. Fed Register. 1999;64:4535-4540. Accessed January 5, 2024. https://www.govinfo.gov/content/pkg/FR-1999-01-29/html/99-1938.htm
- Millns JL, Dicken CH. Hereditary acrolabial telangiectasia. a report of familial blue lips, nails, and nipples. Arch Dermatol. 1979;115:474-478. doi:10.1001/archderm.115.4.474
- Chiriac A, Brzezinski P, Foia L, et al. Chloronychia: green nail syndrome caused by Pseudomonas aeruginosa in elderly persons [published online January 14, 2015]. Clin Interv Aging. 2015;10:265-267. doi:10.2147/CIA.S75525
The Diagnosis: Argyria-Induced Azure Lunulae
Argyria is an acquired condition resulting from excessive exogenous exposure to silver with subsequent gastrointestinal absorption and pigmentary tissue deposition. Upon further questioning, our patient disclosed a lifetime history of colloidal silver use, both as a topical antiseptic agent and intraorally for aphthous ulcers. Silver has a predilection for granular deposition in stromal tissues and basement membranes with sparing of the epidermis, manifesting as progressive, permanent, blue to slate gray discoloration of sunexposed skin, mucous membranes, and nail beds.1 The patient was advised to discontinue use of colloidal silver to avoid development of further pigmentary changes. The appearance of his nails remained unchanged in the months following initial presentation, as expected, since argyria pigmentation is not anticipated to reverse upon colloidal silver cessation.
Nail involvement may be an early presentation of generalized argyria or may be found in isolation, as seen in our patient. Early recognition and patient education are essential to minimize cumulative silver deposition. Although dyspigmentation may impact psychosocial well-being secondary to aesthetic concerns, there is limited research supporting adverse systemic effects of argyria confined to the nail beds. Similarly, the majority of generalized cases are not associated with systemic complications; however, potential toxicities, as described in isolated case reports without conclusive causal relationships, include nyctalopia, renal or hepatic toxicity, pulmonary fibrosis, and neuropsychiatric events.1-6 Successful treatment of cutaneous argyria has been reported with the 1064-nm Q-switched Nd:YAG laser; however, there have been no reported treatments for nail bed involvement.7 Due to the absence of systemic symptoms, additional mucocutaneous dyspigmentation, or cosmetic concerns regarding nail bed lunulae discoloration in our patient, no further intervention was pursued, except for continued colloidal silver cessation.
The differential diagnosis of blue-gray nail bed dyspigmentation is broad and includes cyanosis secondary to cardiopulmonary disease, drug-induced dyspigmentation, Wilson disease, argyria, chrysiasis, hereditary acrolabial telangiectasia, and pseudomonal infection or chloronychia.1,8,9 Etiologic insight may be provided from a thorough review of prescription and over-the-counter medications as well as careful attention to the distribution of dyspigmentation. Medications commonly associated with bluish nail bed dyspigmentation include antimalarials, amiodarone, minocycline, clofazimine, chlorpromazine/phenothiazines, and various chemotherapeutic drugs; our patient was not taking any of these.1,9
Cyanotic nail bed dyspigmentation secondary to cardiopulmonary disease likely manifests with more diffuse nail bed dyspigmentation and is not confined solely to the lunulae. Only drug-induced dyspigmentation, classically due to phenolphthalein-containing laxatives; Wilson disease; and argyria have a tendency to spare the distal nail bed, which is a presentation termed azure lunulae.8 The toenails typically are spared in argyria, while toenail involvement is variable in Wilson disease, and additional systemic symptoms—including hepatic, ophthalmologic, and neuropsychiatric—as well as potential family history would be expected.8 Phenolphthalein is no longer available in over-the-counter laxatives, as it was formally banned by the US Food and Drug Administration in 1999 due to concerns of carcinogenicity.10
Hereditary acrolabial telangiectasia is a familial condition with autosomal-dominant inheritance that can manifest similarly to argyria with blue-gray discoloration of the proximal nail bed; however, this condition also would demonstrate involvement of the vermilion border and nipple areolae, often with associated telangiectasia and migraine headaches.11
Chloronychia (also known as green nail syndrome) is an infection of the nail bed with Pseudomonas aeruginosa that more commonly presents with greenblack discoloration with variable involvement of the fingernails and toenails. Chloronychia, often with associated onycholysis, typically is found in individuals with repeated exposure to water, soaps, and detergents.12 Our patient’s long-standing and unwavering nail bed appearance, involvement of all fingernail lunulae, lack of additional symptoms, and disclosed use of over-the-counter colloidal silver supported a clinical diagnosis of argyriainduced azure lunulae.
Argyria-induced azure lunulae secondary to colloidal silver exposure is an uncommon yet clinically significant cause of nail bed dyspigmentation. Prompt identification and cessation of the offending agent can prevent progression of mucocutaneous dyspigmentation and avoid potential long-term sequelae from systemic deposition.
The Diagnosis: Argyria-Induced Azure Lunulae
Argyria is an acquired condition resulting from excessive exogenous exposure to silver with subsequent gastrointestinal absorption and pigmentary tissue deposition. Upon further questioning, our patient disclosed a lifetime history of colloidal silver use, both as a topical antiseptic agent and intraorally for aphthous ulcers. Silver has a predilection for granular deposition in stromal tissues and basement membranes with sparing of the epidermis, manifesting as progressive, permanent, blue to slate gray discoloration of sunexposed skin, mucous membranes, and nail beds.1 The patient was advised to discontinue use of colloidal silver to avoid development of further pigmentary changes. The appearance of his nails remained unchanged in the months following initial presentation, as expected, since argyria pigmentation is not anticipated to reverse upon colloidal silver cessation.
Nail involvement may be an early presentation of generalized argyria or may be found in isolation, as seen in our patient. Early recognition and patient education are essential to minimize cumulative silver deposition. Although dyspigmentation may impact psychosocial well-being secondary to aesthetic concerns, there is limited research supporting adverse systemic effects of argyria confined to the nail beds. Similarly, the majority of generalized cases are not associated with systemic complications; however, potential toxicities, as described in isolated case reports without conclusive causal relationships, include nyctalopia, renal or hepatic toxicity, pulmonary fibrosis, and neuropsychiatric events.1-6 Successful treatment of cutaneous argyria has been reported with the 1064-nm Q-switched Nd:YAG laser; however, there have been no reported treatments for nail bed involvement.7 Due to the absence of systemic symptoms, additional mucocutaneous dyspigmentation, or cosmetic concerns regarding nail bed lunulae discoloration in our patient, no further intervention was pursued, except for continued colloidal silver cessation.
The differential diagnosis of blue-gray nail bed dyspigmentation is broad and includes cyanosis secondary to cardiopulmonary disease, drug-induced dyspigmentation, Wilson disease, argyria, chrysiasis, hereditary acrolabial telangiectasia, and pseudomonal infection or chloronychia.1,8,9 Etiologic insight may be provided from a thorough review of prescription and over-the-counter medications as well as careful attention to the distribution of dyspigmentation. Medications commonly associated with bluish nail bed dyspigmentation include antimalarials, amiodarone, minocycline, clofazimine, chlorpromazine/phenothiazines, and various chemotherapeutic drugs; our patient was not taking any of these.1,9
Cyanotic nail bed dyspigmentation secondary to cardiopulmonary disease likely manifests with more diffuse nail bed dyspigmentation and is not confined solely to the lunulae. Only drug-induced dyspigmentation, classically due to phenolphthalein-containing laxatives; Wilson disease; and argyria have a tendency to spare the distal nail bed, which is a presentation termed azure lunulae.8 The toenails typically are spared in argyria, while toenail involvement is variable in Wilson disease, and additional systemic symptoms—including hepatic, ophthalmologic, and neuropsychiatric—as well as potential family history would be expected.8 Phenolphthalein is no longer available in over-the-counter laxatives, as it was formally banned by the US Food and Drug Administration in 1999 due to concerns of carcinogenicity.10
Hereditary acrolabial telangiectasia is a familial condition with autosomal-dominant inheritance that can manifest similarly to argyria with blue-gray discoloration of the proximal nail bed; however, this condition also would demonstrate involvement of the vermilion border and nipple areolae, often with associated telangiectasia and migraine headaches.11
Chloronychia (also known as green nail syndrome) is an infection of the nail bed with Pseudomonas aeruginosa that more commonly presents with greenblack discoloration with variable involvement of the fingernails and toenails. Chloronychia, often with associated onycholysis, typically is found in individuals with repeated exposure to water, soaps, and detergents.12 Our patient’s long-standing and unwavering nail bed appearance, involvement of all fingernail lunulae, lack of additional symptoms, and disclosed use of over-the-counter colloidal silver supported a clinical diagnosis of argyriainduced azure lunulae.
Argyria-induced azure lunulae secondary to colloidal silver exposure is an uncommon yet clinically significant cause of nail bed dyspigmentation. Prompt identification and cessation of the offending agent can prevent progression of mucocutaneous dyspigmentation and avoid potential long-term sequelae from systemic deposition.
- Mota L, Dinis-Oliveira RJ. Clinical and forensic aspects of the different subtypes of argyria. J Clin Med. 2021;10:2086. doi:10.3390/ jcm10102086
- Osin´ska J, Poborc-Godlewska J, Kiec´-Swierczyn´ska M, et al. 6 cases of argyria among workers engaged in silverplating radio subunits. Med Pr. 1982;33:361-364.
- Mayr M, Kim MJ, Wanner D, et al. Argyria and decreased kidney function: are silver compounds toxic to the kidney? Am J Kidney Dis. 2009;53:890-894. doi:10.1053/j.ajkd.2008.08.028
- Trop M, Novak M, Rodl S, et al. Silver-coated dressing acticoat caused raised liver enzymes and argyria-like symptoms in burn patient. J Trauma. 2006;60:648-652. doi:10.1097/01.ta.0000208126 .22089.b6
- Mirsattari SM, Hammond RR, Sharpe MD, et al. Myoclonic status epilepticus following repeated oral ingestion of colloidal silver. Neurology. 2004;62:1408-1410. doi:10.1212/01.wnl.0000120671.73335.ec
- Barrie HJ, Harding HE. Argyro-siderosis of the lungs in silver finishers. Br J Ind Med. 1947;4:225-229. doi:10.1136/oem.4.4.225
- Griffith RD, Simmons BJ, Bray FN, et al. 1064 nm Q-switched Nd:YAG laser for the treatment of argyria: a systematic review. J Eur Acad Dermatol Venereol. 2015;29:2100-2103. doi:10.111 1/jdv.13117
- Rubin AI, Jellinek NJ, Daniel CR III, et al, eds. Scher and Daniel’s Nails: Diagnosis, Surgery, Therapy. 4th ed. Springer; 2018.
- Slater K, Sommariva E, Kartono F. A case study of argyria of the nails secondary to colloidal silver ingestion [published online October 28, 2022]. Cureus. 2022;14:E30818. doi:10.7759/cureus.30818
- Hubbard WK. Laxative drug products for over-the-counter human use. Fed Register. 1999;64:4535-4540. Accessed January 5, 2024. https://www.govinfo.gov/content/pkg/FR-1999-01-29/html/99-1938.htm
- Millns JL, Dicken CH. Hereditary acrolabial telangiectasia. a report of familial blue lips, nails, and nipples. Arch Dermatol. 1979;115:474-478. doi:10.1001/archderm.115.4.474
- Chiriac A, Brzezinski P, Foia L, et al. Chloronychia: green nail syndrome caused by Pseudomonas aeruginosa in elderly persons [published online January 14, 2015]. Clin Interv Aging. 2015;10:265-267. doi:10.2147/CIA.S75525
- Mota L, Dinis-Oliveira RJ. Clinical and forensic aspects of the different subtypes of argyria. J Clin Med. 2021;10:2086. doi:10.3390/ jcm10102086
- Osin´ska J, Poborc-Godlewska J, Kiec´-Swierczyn´ska M, et al. 6 cases of argyria among workers engaged in silverplating radio subunits. Med Pr. 1982;33:361-364.
- Mayr M, Kim MJ, Wanner D, et al. Argyria and decreased kidney function: are silver compounds toxic to the kidney? Am J Kidney Dis. 2009;53:890-894. doi:10.1053/j.ajkd.2008.08.028
- Trop M, Novak M, Rodl S, et al. Silver-coated dressing acticoat caused raised liver enzymes and argyria-like symptoms in burn patient. J Trauma. 2006;60:648-652. doi:10.1097/01.ta.0000208126 .22089.b6
- Mirsattari SM, Hammond RR, Sharpe MD, et al. Myoclonic status epilepticus following repeated oral ingestion of colloidal silver. Neurology. 2004;62:1408-1410. doi:10.1212/01.wnl.0000120671.73335.ec
- Barrie HJ, Harding HE. Argyro-siderosis of the lungs in silver finishers. Br J Ind Med. 1947;4:225-229. doi:10.1136/oem.4.4.225
- Griffith RD, Simmons BJ, Bray FN, et al. 1064 nm Q-switched Nd:YAG laser for the treatment of argyria: a systematic review. J Eur Acad Dermatol Venereol. 2015;29:2100-2103. doi:10.111 1/jdv.13117
- Rubin AI, Jellinek NJ, Daniel CR III, et al, eds. Scher and Daniel’s Nails: Diagnosis, Surgery, Therapy. 4th ed. Springer; 2018.
- Slater K, Sommariva E, Kartono F. A case study of argyria of the nails secondary to colloidal silver ingestion [published online October 28, 2022]. Cureus. 2022;14:E30818. doi:10.7759/cureus.30818
- Hubbard WK. Laxative drug products for over-the-counter human use. Fed Register. 1999;64:4535-4540. Accessed January 5, 2024. https://www.govinfo.gov/content/pkg/FR-1999-01-29/html/99-1938.htm
- Millns JL, Dicken CH. Hereditary acrolabial telangiectasia. a report of familial blue lips, nails, and nipples. Arch Dermatol. 1979;115:474-478. doi:10.1001/archderm.115.4.474
- Chiriac A, Brzezinski P, Foia L, et al. Chloronychia: green nail syndrome caused by Pseudomonas aeruginosa in elderly persons [published online January 14, 2015]. Clin Interv Aging. 2015;10:265-267. doi:10.2147/CIA.S75525
An 88-year-old man presented with asymptomatic and unchanging discoloration of the proximal fingernails of both hands of 50 years’ duration. Physical examination revealed blue to slate gray, subungual pigmentary changes of the fingernails of both hands sparing the nail bed distal to the lunulae. There was no overlying plate dystrophy, toenail involvement, or additional mucocutaneous abnormalities. His medical history was notable for heart failure, obstructive sleep apnea, and type 2 diabetes mellitus. He had no history of hepatic, ophthalmologic, or neurologic dysfunction.
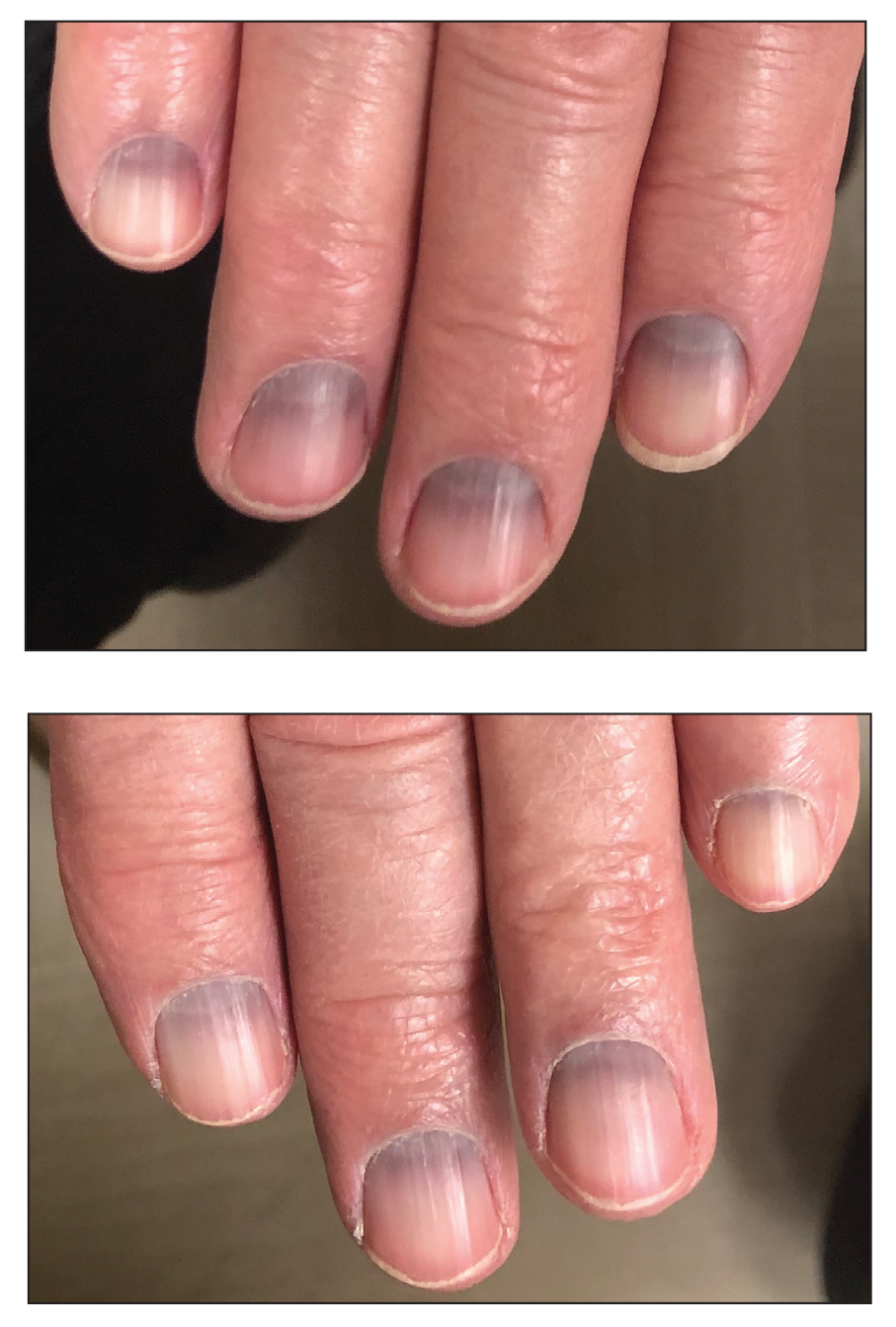
Deaths Linked to Substance Use, CVD on the Rise
TOPLINE:
, with the most pronounced rise among women, American Indians, younger people, rural residents, and users of cannabis and psychostimulants, results of new research suggest.
METHODOLOGY:
- From the Centers for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research (CDC WONDER) database and using International Classification of Diseases (ICD) codes, researchers collected data on deaths within the United States where both SU and CVD (SU+CVD) were a contributing or an underlying cause and gathered information on location of death (medical facility, home, hospice, nursing home/long-term care facility), demographics (sex, race/ethnicity, age), and region (urban-rural, state).
- Researchers determined crude and age-adjusted mortality rates (AAMRs) per 100,000 population, identified trends in AAMR using annual percent change (APC) and calculated the weighted average of APCs (AAPCs).
- Between 1999 and 2019, there were 636,572 deaths related to CVD+SU, 75.6% of which were among men and 70.6% among non-Hispanic White individuals, with 65% related to alcohol, and where location of death was available, 47.7% occurred in medical facilities.
TAKEAWAY:
- The overall SU+CVD-related AAMR from 1999 to 2019 was 14.3 (95% CI, 14.3-14.3) per 100,000 individuals, with the rate being higher in men (22.5) than in women (6.8) and highest in American Indians or Alaska Natives (37.7) compared with other races/ethnicities.
- Rural areas had higher SU+CVD-related AAMR (15.2; 95% CI, 15.1-15.3) than urban areas, with the District of Columbia having the highest AAMR geographically (25.4), individuals aged 55-69 years having the highest rate agewise (25.1), and alcohol accounting for the highest rate (9.09) among substance types.
- Temporal trends show that the overall SU+CVD-related AAMR increased from 9.9 in 1999 to 21.4 in 2019, a rate that started accelerating in 2012, with an AAPC of 4.0% (95% CI, 3.7-4.3); increases were across all ethnicities and age groups and were particularly pronounced among women (4.8%; 95% CI, 4.5-5.1).
- Cannabis had the highest AAPC of all substances (12.7%), but stimulants had an APC of 21.4 (95% CI, 20.0-22.8) from 2009 to 2019, a period during which stimulants were the fastest-growing substance abuse category.
IN PRACTICE:
These new results identify high-risk groups, which “is crucial for prioritizing preventive measures aiming to reduce substance use and cardiovascular disease-related mortality in these populations,” the researchers wrote.
SOURCE:
Abdul Mannan Khan Minhas, MD, Department of Medicine, University of Mississippi Medical Center, Jackson, Mississippi, and Jakrin Kewcharoen, MD, Division of Cardiology, Loma Linda University Medical Center, Loma Linda, California, were co-first authors of the study, which was published online in the Journal of the American Heart Association.
A version of this article first appeared on Medscape.com.
TOPLINE:
, with the most pronounced rise among women, American Indians, younger people, rural residents, and users of cannabis and psychostimulants, results of new research suggest.
METHODOLOGY:
- From the Centers for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research (CDC WONDER) database and using International Classification of Diseases (ICD) codes, researchers collected data on deaths within the United States where both SU and CVD (SU+CVD) were a contributing or an underlying cause and gathered information on location of death (medical facility, home, hospice, nursing home/long-term care facility), demographics (sex, race/ethnicity, age), and region (urban-rural, state).
- Researchers determined crude and age-adjusted mortality rates (AAMRs) per 100,000 population, identified trends in AAMR using annual percent change (APC) and calculated the weighted average of APCs (AAPCs).
- Between 1999 and 2019, there were 636,572 deaths related to CVD+SU, 75.6% of which were among men and 70.6% among non-Hispanic White individuals, with 65% related to alcohol, and where location of death was available, 47.7% occurred in medical facilities.
TAKEAWAY:
- The overall SU+CVD-related AAMR from 1999 to 2019 was 14.3 (95% CI, 14.3-14.3) per 100,000 individuals, with the rate being higher in men (22.5) than in women (6.8) and highest in American Indians or Alaska Natives (37.7) compared with other races/ethnicities.
- Rural areas had higher SU+CVD-related AAMR (15.2; 95% CI, 15.1-15.3) than urban areas, with the District of Columbia having the highest AAMR geographically (25.4), individuals aged 55-69 years having the highest rate agewise (25.1), and alcohol accounting for the highest rate (9.09) among substance types.
- Temporal trends show that the overall SU+CVD-related AAMR increased from 9.9 in 1999 to 21.4 in 2019, a rate that started accelerating in 2012, with an AAPC of 4.0% (95% CI, 3.7-4.3); increases were across all ethnicities and age groups and were particularly pronounced among women (4.8%; 95% CI, 4.5-5.1).
- Cannabis had the highest AAPC of all substances (12.7%), but stimulants had an APC of 21.4 (95% CI, 20.0-22.8) from 2009 to 2019, a period during which stimulants were the fastest-growing substance abuse category.
IN PRACTICE:
These new results identify high-risk groups, which “is crucial for prioritizing preventive measures aiming to reduce substance use and cardiovascular disease-related mortality in these populations,” the researchers wrote.
SOURCE:
Abdul Mannan Khan Minhas, MD, Department of Medicine, University of Mississippi Medical Center, Jackson, Mississippi, and Jakrin Kewcharoen, MD, Division of Cardiology, Loma Linda University Medical Center, Loma Linda, California, were co-first authors of the study, which was published online in the Journal of the American Heart Association.
A version of this article first appeared on Medscape.com.
TOPLINE:
, with the most pronounced rise among women, American Indians, younger people, rural residents, and users of cannabis and psychostimulants, results of new research suggest.
METHODOLOGY:
- From the Centers for Disease Control and Prevention Wide-Ranging Online Data for Epidemiologic Research (CDC WONDER) database and using International Classification of Diseases (ICD) codes, researchers collected data on deaths within the United States where both SU and CVD (SU+CVD) were a contributing or an underlying cause and gathered information on location of death (medical facility, home, hospice, nursing home/long-term care facility), demographics (sex, race/ethnicity, age), and region (urban-rural, state).
- Researchers determined crude and age-adjusted mortality rates (AAMRs) per 100,000 population, identified trends in AAMR using annual percent change (APC) and calculated the weighted average of APCs (AAPCs).
- Between 1999 and 2019, there were 636,572 deaths related to CVD+SU, 75.6% of which were among men and 70.6% among non-Hispanic White individuals, with 65% related to alcohol, and where location of death was available, 47.7% occurred in medical facilities.
TAKEAWAY:
- The overall SU+CVD-related AAMR from 1999 to 2019 was 14.3 (95% CI, 14.3-14.3) per 100,000 individuals, with the rate being higher in men (22.5) than in women (6.8) and highest in American Indians or Alaska Natives (37.7) compared with other races/ethnicities.
- Rural areas had higher SU+CVD-related AAMR (15.2; 95% CI, 15.1-15.3) than urban areas, with the District of Columbia having the highest AAMR geographically (25.4), individuals aged 55-69 years having the highest rate agewise (25.1), and alcohol accounting for the highest rate (9.09) among substance types.
- Temporal trends show that the overall SU+CVD-related AAMR increased from 9.9 in 1999 to 21.4 in 2019, a rate that started accelerating in 2012, with an AAPC of 4.0% (95% CI, 3.7-4.3); increases were across all ethnicities and age groups and were particularly pronounced among women (4.8%; 95% CI, 4.5-5.1).
- Cannabis had the highest AAPC of all substances (12.7%), but stimulants had an APC of 21.4 (95% CI, 20.0-22.8) from 2009 to 2019, a period during which stimulants were the fastest-growing substance abuse category.
IN PRACTICE:
These new results identify high-risk groups, which “is crucial for prioritizing preventive measures aiming to reduce substance use and cardiovascular disease-related mortality in these populations,” the researchers wrote.
SOURCE:
Abdul Mannan Khan Minhas, MD, Department of Medicine, University of Mississippi Medical Center, Jackson, Mississippi, and Jakrin Kewcharoen, MD, Division of Cardiology, Loma Linda University Medical Center, Loma Linda, California, were co-first authors of the study, which was published online in the Journal of the American Heart Association.
A version of this article first appeared on Medscape.com.
Corticosteroid Injections Don’t Move Blood Sugar for Most
TOPLINE:
Intra-articular corticosteroid (IACS) injections pose a minimal risk of accelerating diabetes for most people, despite temporarily elevating blood glucose levels, according to a study published in Clinical Diabetes.
METHODOLOGY:
- Almost half of Americans with diabetes have arthritis, so glycemic control is a concern for many receiving IACS injections.
- IACS injections are known to cause short-term hyperglycemia, but their long-term effects on glycemic control are not well studied.
- For the retrospective cohort study, researchers at Mayo Clinic in Rochester, Minnesota, used electronic health records from 1169 adults who had received an IACS injection in one large joint between 2012 and 2018.
- They analyzed data on A1C levels for study participants from 18 months before and after the injections.
- Researchers assessed if participants had a greater-than-expected (defined as an increase of more than 0.5% above expected) concentration of A1C after the injection, and examined rates of diabetic ketoacidosis and hyperosmolar hyperglycemic syndrome in the 30 days following an injection.
TAKEAWAY:
- Nearly 16% of people experienced a greater-than-expected A1C level after receiving an injection.
- A1C levels rose by an average of 1.2% in the greater-than-expected group, but decreased by an average of 0.2% in the average group.
- One patient had an episode of severe hyperglycemia that was linked to the injection.
- A baseline level of A1C above 8% was the only factor associated with a greater-than-expected increase in the marker after an IACS injection.
IN PRACTICE:
“Although most patients do not experience an increase in A1C after IACS, clinicians should counsel patients with suboptimally controlled diabetes about risks of further hyperglycemia after IACS administration,” the researchers wrote.
SOURCE:
The study was led by Terin T. Sytsma, MD, of Mayo Clinic in Rochester, Minnesota.
LIMITATIONS:
The study was retrospective and could not establish causation. In addition, the population was of residents from one county in Minnesota, and was not racially or ethnically diverse. Details about the injection, such as location and total dose, were not available. The study also did not include a control group.
DISCLOSURES:
The study was funded by Mayo Clinic and the National Center for Advancing Translational Sciences. The authors reported no relevant disclosures.
A version of this article first appeared on Medscape.com.
TOPLINE:
Intra-articular corticosteroid (IACS) injections pose a minimal risk of accelerating diabetes for most people, despite temporarily elevating blood glucose levels, according to a study published in Clinical Diabetes.
METHODOLOGY:
- Almost half of Americans with diabetes have arthritis, so glycemic control is a concern for many receiving IACS injections.
- IACS injections are known to cause short-term hyperglycemia, but their long-term effects on glycemic control are not well studied.
- For the retrospective cohort study, researchers at Mayo Clinic in Rochester, Minnesota, used electronic health records from 1169 adults who had received an IACS injection in one large joint between 2012 and 2018.
- They analyzed data on A1C levels for study participants from 18 months before and after the injections.
- Researchers assessed if participants had a greater-than-expected (defined as an increase of more than 0.5% above expected) concentration of A1C after the injection, and examined rates of diabetic ketoacidosis and hyperosmolar hyperglycemic syndrome in the 30 days following an injection.
TAKEAWAY:
- Nearly 16% of people experienced a greater-than-expected A1C level after receiving an injection.
- A1C levels rose by an average of 1.2% in the greater-than-expected group, but decreased by an average of 0.2% in the average group.
- One patient had an episode of severe hyperglycemia that was linked to the injection.
- A baseline level of A1C above 8% was the only factor associated with a greater-than-expected increase in the marker after an IACS injection.
IN PRACTICE:
“Although most patients do not experience an increase in A1C after IACS, clinicians should counsel patients with suboptimally controlled diabetes about risks of further hyperglycemia after IACS administration,” the researchers wrote.
SOURCE:
The study was led by Terin T. Sytsma, MD, of Mayo Clinic in Rochester, Minnesota.
LIMITATIONS:
The study was retrospective and could not establish causation. In addition, the population was of residents from one county in Minnesota, and was not racially or ethnically diverse. Details about the injection, such as location and total dose, were not available. The study also did not include a control group.
DISCLOSURES:
The study was funded by Mayo Clinic and the National Center for Advancing Translational Sciences. The authors reported no relevant disclosures.
A version of this article first appeared on Medscape.com.
TOPLINE:
Intra-articular corticosteroid (IACS) injections pose a minimal risk of accelerating diabetes for most people, despite temporarily elevating blood glucose levels, according to a study published in Clinical Diabetes.
METHODOLOGY:
- Almost half of Americans with diabetes have arthritis, so glycemic control is a concern for many receiving IACS injections.
- IACS injections are known to cause short-term hyperglycemia, but their long-term effects on glycemic control are not well studied.
- For the retrospective cohort study, researchers at Mayo Clinic in Rochester, Minnesota, used electronic health records from 1169 adults who had received an IACS injection in one large joint between 2012 and 2018.
- They analyzed data on A1C levels for study participants from 18 months before and after the injections.
- Researchers assessed if participants had a greater-than-expected (defined as an increase of more than 0.5% above expected) concentration of A1C after the injection, and examined rates of diabetic ketoacidosis and hyperosmolar hyperglycemic syndrome in the 30 days following an injection.
TAKEAWAY:
- Nearly 16% of people experienced a greater-than-expected A1C level after receiving an injection.
- A1C levels rose by an average of 1.2% in the greater-than-expected group, but decreased by an average of 0.2% in the average group.
- One patient had an episode of severe hyperglycemia that was linked to the injection.
- A baseline level of A1C above 8% was the only factor associated with a greater-than-expected increase in the marker after an IACS injection.
IN PRACTICE:
“Although most patients do not experience an increase in A1C after IACS, clinicians should counsel patients with suboptimally controlled diabetes about risks of further hyperglycemia after IACS administration,” the researchers wrote.
SOURCE:
The study was led by Terin T. Sytsma, MD, of Mayo Clinic in Rochester, Minnesota.
LIMITATIONS:
The study was retrospective and could not establish causation. In addition, the population was of residents from one county in Minnesota, and was not racially or ethnically diverse. Details about the injection, such as location and total dose, were not available. The study also did not include a control group.
DISCLOSURES:
The study was funded by Mayo Clinic and the National Center for Advancing Translational Sciences. The authors reported no relevant disclosures.
A version of this article first appeared on Medscape.com.
High Rate of Rehospitalization After First Ischemic Stroke
TOPLINE:
Among patients hospitalized with a first ischemic stroke, 80% were rehospitalized, primarily because of subsequent primary cardiovascular and cerebrovascular diagnoses.
METHODOLOGY:
- To gather information on post-stroke hospital admission, investigators followed 1412 participants (mean age, 72.4 years; 52.1% women, 35.3% Black individuals) from the Atherosclerosis Risk in Communities (ARIC) study who were living in Maryland, Minnesota, North Carolina, and Mississippi.
- Participants were recruited between 1987 and 1989 when they were 45-64 years old and were followed on an annual and then semiannual basis from the index discharge until discharge after their second hospitalization, death, or end of the study in December 2019.
- Specific diagnoses for each hospitalization were based on hospital records, discharge diagnoses, and annual and semiannual phone interviews.
TAKEAWAY:
- During the study period, 1143 hospitalizations occurred over 41,849 person-months.
- 81% of participants were hospitalized over a maximum of 26.6 years of follow-up. Primary cardiovascular and cerebrovascular diagnoses were reported for half of readmissions.
- Over the follow-up period, compared with cardioembolic stroke, readmission risk was lower for thrombotic/lacunar stroke (adjusted hazard ratio [aHR], 0.82; 95% CI, 0.71-0.95) and hemorrhagic stroke (aHR, 0.74; 95% CI, 0.58-0.93). However, when adjusting for atrial fibrillation and competing risk for death, there were no significant differences between stroke subtypes.
- Compared with cardioembolic stroke, thrombotic/lacunar stroke was associated with lower readmission risk within 1 month (aHR, 0.66; 95% CI, 0.46-0.93) and from 1 month to 1 year (aHR, 0.78; 95% CI, 0.62-0.97), and hemorrhagic stroke was associated with lower risk from 1 month to 1 year (aHR, 0.60; 95% CI, 0.41-0.87).
IN PRACTICE:
“These results suggest that prevention strategies focused on cardiovascular and cerebrovascular health warrant further investigation, especially within the first year after incident stroke and perhaps particularly among individuals with an incident cardioembolic stroke,” the authors wrote.
SOURCE:
Kelly Sloane, MD, of the University of Pennsylvania Perelman School of Medicine in Philadelphia, led the study along with colleagues at the National Institute of Neurological Disorders and Stroke, Johns Hopkins University in Baltimore, and the University of North Carolina, Chapel Hill. The article was published online on January 5 in Neurology.
LIMITATIONS:
The ARIC study classification of stroke subtype grouped embolic strokes of undetermined source as thrombotic strokes, and investigators were unable to distinguish between the groups. In addition, there was no way to measure stroke severity, which could have played a role in readmission risk.
DISCLOSURES:
The study was funded by the National Heart, Lung, and Blood Institute, the National Institute of Neurological Disorders and Stroke, and the National Institutes of Health.
A version of this article appeared on Medscape.com.
TOPLINE:
Among patients hospitalized with a first ischemic stroke, 80% were rehospitalized, primarily because of subsequent primary cardiovascular and cerebrovascular diagnoses.
METHODOLOGY:
- To gather information on post-stroke hospital admission, investigators followed 1412 participants (mean age, 72.4 years; 52.1% women, 35.3% Black individuals) from the Atherosclerosis Risk in Communities (ARIC) study who were living in Maryland, Minnesota, North Carolina, and Mississippi.
- Participants were recruited between 1987 and 1989 when they were 45-64 years old and were followed on an annual and then semiannual basis from the index discharge until discharge after their second hospitalization, death, or end of the study in December 2019.
- Specific diagnoses for each hospitalization were based on hospital records, discharge diagnoses, and annual and semiannual phone interviews.
TAKEAWAY:
- During the study period, 1143 hospitalizations occurred over 41,849 person-months.
- 81% of participants were hospitalized over a maximum of 26.6 years of follow-up. Primary cardiovascular and cerebrovascular diagnoses were reported for half of readmissions.
- Over the follow-up period, compared with cardioembolic stroke, readmission risk was lower for thrombotic/lacunar stroke (adjusted hazard ratio [aHR], 0.82; 95% CI, 0.71-0.95) and hemorrhagic stroke (aHR, 0.74; 95% CI, 0.58-0.93). However, when adjusting for atrial fibrillation and competing risk for death, there were no significant differences between stroke subtypes.
- Compared with cardioembolic stroke, thrombotic/lacunar stroke was associated with lower readmission risk within 1 month (aHR, 0.66; 95% CI, 0.46-0.93) and from 1 month to 1 year (aHR, 0.78; 95% CI, 0.62-0.97), and hemorrhagic stroke was associated with lower risk from 1 month to 1 year (aHR, 0.60; 95% CI, 0.41-0.87).
IN PRACTICE:
“These results suggest that prevention strategies focused on cardiovascular and cerebrovascular health warrant further investigation, especially within the first year after incident stroke and perhaps particularly among individuals with an incident cardioembolic stroke,” the authors wrote.
SOURCE:
Kelly Sloane, MD, of the University of Pennsylvania Perelman School of Medicine in Philadelphia, led the study along with colleagues at the National Institute of Neurological Disorders and Stroke, Johns Hopkins University in Baltimore, and the University of North Carolina, Chapel Hill. The article was published online on January 5 in Neurology.
LIMITATIONS:
The ARIC study classification of stroke subtype grouped embolic strokes of undetermined source as thrombotic strokes, and investigators were unable to distinguish between the groups. In addition, there was no way to measure stroke severity, which could have played a role in readmission risk.
DISCLOSURES:
The study was funded by the National Heart, Lung, and Blood Institute, the National Institute of Neurological Disorders and Stroke, and the National Institutes of Health.
A version of this article appeared on Medscape.com.
TOPLINE:
Among patients hospitalized with a first ischemic stroke, 80% were rehospitalized, primarily because of subsequent primary cardiovascular and cerebrovascular diagnoses.
METHODOLOGY:
- To gather information on post-stroke hospital admission, investigators followed 1412 participants (mean age, 72.4 years; 52.1% women, 35.3% Black individuals) from the Atherosclerosis Risk in Communities (ARIC) study who were living in Maryland, Minnesota, North Carolina, and Mississippi.
- Participants were recruited between 1987 and 1989 when they were 45-64 years old and were followed on an annual and then semiannual basis from the index discharge until discharge after their second hospitalization, death, or end of the study in December 2019.
- Specific diagnoses for each hospitalization were based on hospital records, discharge diagnoses, and annual and semiannual phone interviews.
TAKEAWAY:
- During the study period, 1143 hospitalizations occurred over 41,849 person-months.
- 81% of participants were hospitalized over a maximum of 26.6 years of follow-up. Primary cardiovascular and cerebrovascular diagnoses were reported for half of readmissions.
- Over the follow-up period, compared with cardioembolic stroke, readmission risk was lower for thrombotic/lacunar stroke (adjusted hazard ratio [aHR], 0.82; 95% CI, 0.71-0.95) and hemorrhagic stroke (aHR, 0.74; 95% CI, 0.58-0.93). However, when adjusting for atrial fibrillation and competing risk for death, there were no significant differences between stroke subtypes.
- Compared with cardioembolic stroke, thrombotic/lacunar stroke was associated with lower readmission risk within 1 month (aHR, 0.66; 95% CI, 0.46-0.93) and from 1 month to 1 year (aHR, 0.78; 95% CI, 0.62-0.97), and hemorrhagic stroke was associated with lower risk from 1 month to 1 year (aHR, 0.60; 95% CI, 0.41-0.87).
IN PRACTICE:
“These results suggest that prevention strategies focused on cardiovascular and cerebrovascular health warrant further investigation, especially within the first year after incident stroke and perhaps particularly among individuals with an incident cardioembolic stroke,” the authors wrote.
SOURCE:
Kelly Sloane, MD, of the University of Pennsylvania Perelman School of Medicine in Philadelphia, led the study along with colleagues at the National Institute of Neurological Disorders and Stroke, Johns Hopkins University in Baltimore, and the University of North Carolina, Chapel Hill. The article was published online on January 5 in Neurology.
LIMITATIONS:
The ARIC study classification of stroke subtype grouped embolic strokes of undetermined source as thrombotic strokes, and investigators were unable to distinguish between the groups. In addition, there was no way to measure stroke severity, which could have played a role in readmission risk.
DISCLOSURES:
The study was funded by the National Heart, Lung, and Blood Institute, the National Institute of Neurological Disorders and Stroke, and the National Institutes of Health.
A version of this article appeared on Medscape.com.