User login
Beyond the lips: Guidance for intraoral procedures
NEW YORK –The work of the dermatologist doesn’t need to stop at the lips, according to Nasim Fazel, MD, DDS, a board-certified dermatologist and dentist. she said, speaking at a session focused on oral health and procedures at the American Academy of Dermatology summer meeting.
Whether to perform an incisional or excisional biopsy on the lips or within the oral cavity is a decision driven by the clinical scenario, said Dr. Fazel, professor of clinical dermatology and director of the oral mucosal disease clinic at the University of California, Davis. Variables to consider, she said, include the size of the lesion, as well as whether the lesion is symptomatic or there’s any functional impairment. Other factors to bear in mind are whether the patient has any comorbid inflammatory conditions and whether the lesion could be malignant.
An excisional biopsy is a good procedure for small lesions that are thought to be benign, especially if they are exophytic, she noted. An example would be a traumatic fibroma, she said. This technique is also appropriate if there’s concern for dysplasia or malignancy if an office excisional biopsy is feasible given lesion size and location.
On the labial mucosa, an elliptical incision is often a good choice.
Cutaneous lip procedures
On the cutaneous lip, a punch incision can be feasible. The vermilion border should be marked to maintain orientation. “Avoid transecting the vermilion border to the extent that it’s possible,” said Dr. Fazel. Keep the vascular anatomy in mind as well, she added, since there’s a risk of severing the superior or inferior labial artery with procedures in this area. If this should happen, the branch can be identified and ligated with 4-0 fast gut or chromic gut suture material, she advised.
Another option on the cutaneous lip is shave removal. Here, a chalazion clamp can be used for both exposure and hemostasis. “Always suture parallel to the lip lines, and caution the patient that there may be significant, noticeable blanching when lip anesthesia’s used,” she said.
Gingival and tongue procedures
Moving to territory that may be less familiar for some dermatologists, Dr. Fazel walked through the process of a gingival punch biopsy. “Use local anesthetic, but a small quantity is sufficient,” she said. Using gentle pressure, the operator can work the punch instrument down to periosteal bone. At that point, just scissors can be used for undermining the specimen, with minimal disturbance of the mucosal surface.
Hemostasis after a gingival punch can be accomplished with silver nitrate or aluminum chloride or by electrocautery. A permanent defect in the gingiva can occur even with good technique, she said – a fact that should be included in the informed consent document for the procedure.
For lesions on the tongue, a shave removal can be considered, as can an incisional punch biopsy. An assistant’s hands are invaluable for stabilizing the tongue, said Dr. Fazel, illustrating that small dry gauze squares help achieve a good grip.
Considerations in biopsy technique
Dr. Fazel offered some tips and considerations when a punch biopsy is being done in the context of a chronic oral inflammatory condition, and the plan is to submit for hematoxylin and eosin (H&E) staining and direct immunofluorescence (DIF). Conditions where an intraoral punch biopsy would be considered include bullous or mucous membrane pemphigoid, pemphigus, lichen planus, and systemic lupus erythematosus, she said.
“Select a site with the most significant inflammatory changes” and aim for the most anterior site that exhibits these characteristics to maximize exposure and ensure a good specimen. The labial mucosa is a better choice in general than buccal mucosa, she said. “Maxillary and mandibular sulci are tricky sites,” especially when perilesional and lesional tissue should be included in the biopsies.
Next, Dr. Fazel walked attendees through general principles of preparing for and performing punch biopsies for H&E and DIF. In planning the biopsies, the DIF specimen should ideally be collected before the H&E specimen because the former technique will have higher yield when the specimen is taken from a less bloody field. “The yield of DIF is higher from the gingiva than from nonkeratinized surfaces.”
When infiltrating the biopsy site with local anesthesia, the needle should be centered within the lesion or general area to be biopsied, and care should be taken to maintain the orientation of the lesion to the surrounding tissue. Anesthesia can be infiltrated within the submucosal plane; the resultant ballooning will elevate the tissue to be biopsied and ease the procedure, she said.
Choose a 3-mm punch tool for gingival biopsies; 4 mm is a good size for other nonkeratinized surfaces. Unlike the procedure used for cutaneous biopsies, on delicate oral tissues, “you don’t need to hub your punch tool,” Dr. Fazel said. Similarly, the tool can be driven with firm rotation in one direction, rather than ratcheting back and forth, which may fray and deform the biopsy margins, she added. The specimen can be freed from surrounding mucosa with scissors alone and a gentle snipping motion; everting the tissue will help achieve the desired clean and gentle technique.
Because of the delicacy of the tissue, “it’s important to minimize the use of forceps, as well as any unnecessary manipulation of tissue in the process of specimen collection,” she said.
Salivary gland biopsies and intraoral suturing
Even minor salivary glands can be biopsied in a fairly straightforward way, though there’s a risk of short- and long-term loss of sensation, as well as more scarring than in other routine intraoral biopsies. Though these salivary glands lie just beneath the oral mucosa, care must be taken to avoid laceration of the orbicularis oris muscle during excision, noted Dr. Fazel. With a minor salivary gland biopsy, as with some other intraoral procedures, sutures will be needed. Consideration for the friability of the oral mucosa should drive suture material choice and closure technique.
First, “take bigger bites on each side of the incision, to minimize the risk of the suture tearing through the mucosa,” she said. Avoid forceps while suturing if possible, but be gentle if they are employed, “and be gentle tying knots: retract the mucosa as little as possible and cinch the knots down tightly with your fingers.”
Electrocautery, silver nitrate, and aluminum chloride are all reasonable options for hemostasis, although patients should be alerted that the tissue will have a charred appearance if electrocautery is used. Primary closure may be all that’s needed for hemostasis, said Dr. Fazel.
If nonabsorbable suture materials are used, nylon and prolene should be avoided since they tend to tear through the oral mucosa. Soft or braided silk are good choices, she said, and sutures can come out in 5-7 days.
Absorbable sutures have the advantage of not requiring removal, but they can be more irritating to the surrounding mucosa. Chromic or fast gut are the choices here, said Dr. Fazel. Whether absorbable or nonabsorbable sutures are placed, the size should be 4-0 or 5-0, she said.
Postoperative care, complications, and the limits of the dermatologist
Postoperatively, patients should know that swelling is to be expected, especially with procedures like minor salivary gland biopsies that involve the lip. Icing 15 minutes per hour for the first few hours will help with swelling; wound care is optimized with gentle salt water rinses. A bland diet that avoids acidic, spicy, and excessively hot foods and beverages will minimize wound irritation. Foods with sharp edges like chips, crackers, and nuts can actually catch sutures and cause pain and bleeding, so these too should be avoided.
As with dental work, care should be taken with eating or drinking until anesthesia has worn off, which may take up to 3 hours. Patients should also be cautioned that sutures are likely to come out prematurely just because of the mobility of the structures of the mouth with normal activities such as eating and talking.
Should a wound infection occur, said Dr. Fazel, it’s likely that mixed aerobic and anaerobic bacteria are to blame; accordingly, broad-spectrum beta-lactam antibiotics can be a good first-line course. More severe infections are more likely to have an anaerobic or gram-negative etiology; metronidazole is a reasonable choice for anaerobic coverage, she noted. The life-threatening complication not to miss is cellulitis of the floor of the mouth, or Ludwig angina. The swelling results in superior and posterior displacement of the tongue, obstructing the upper airway, so any patient suspected of having Ludwig angina needs emergent evaluation and treatment.
When should a dermatologist consider referral to an otolaryngologist rather than diving into a biopsy in the dermatology clinic? If the area of concern is on the posterior third of the tongue, access without special tools or higher levels of anesthesia becomes tricky, Dr. Fazel pointed out. The posterior hard palate, the soft palate, and the floor of the mouth are also regions best left to otolaryngologists, she said.
NEW YORK –The work of the dermatologist doesn’t need to stop at the lips, according to Nasim Fazel, MD, DDS, a board-certified dermatologist and dentist. she said, speaking at a session focused on oral health and procedures at the American Academy of Dermatology summer meeting.
Whether to perform an incisional or excisional biopsy on the lips or within the oral cavity is a decision driven by the clinical scenario, said Dr. Fazel, professor of clinical dermatology and director of the oral mucosal disease clinic at the University of California, Davis. Variables to consider, she said, include the size of the lesion, as well as whether the lesion is symptomatic or there’s any functional impairment. Other factors to bear in mind are whether the patient has any comorbid inflammatory conditions and whether the lesion could be malignant.
An excisional biopsy is a good procedure for small lesions that are thought to be benign, especially if they are exophytic, she noted. An example would be a traumatic fibroma, she said. This technique is also appropriate if there’s concern for dysplasia or malignancy if an office excisional biopsy is feasible given lesion size and location.
On the labial mucosa, an elliptical incision is often a good choice.
Cutaneous lip procedures
On the cutaneous lip, a punch incision can be feasible. The vermilion border should be marked to maintain orientation. “Avoid transecting the vermilion border to the extent that it’s possible,” said Dr. Fazel. Keep the vascular anatomy in mind as well, she added, since there’s a risk of severing the superior or inferior labial artery with procedures in this area. If this should happen, the branch can be identified and ligated with 4-0 fast gut or chromic gut suture material, she advised.
Another option on the cutaneous lip is shave removal. Here, a chalazion clamp can be used for both exposure and hemostasis. “Always suture parallel to the lip lines, and caution the patient that there may be significant, noticeable blanching when lip anesthesia’s used,” she said.
Gingival and tongue procedures
Moving to territory that may be less familiar for some dermatologists, Dr. Fazel walked through the process of a gingival punch biopsy. “Use local anesthetic, but a small quantity is sufficient,” she said. Using gentle pressure, the operator can work the punch instrument down to periosteal bone. At that point, just scissors can be used for undermining the specimen, with minimal disturbance of the mucosal surface.
Hemostasis after a gingival punch can be accomplished with silver nitrate or aluminum chloride or by electrocautery. A permanent defect in the gingiva can occur even with good technique, she said – a fact that should be included in the informed consent document for the procedure.
For lesions on the tongue, a shave removal can be considered, as can an incisional punch biopsy. An assistant’s hands are invaluable for stabilizing the tongue, said Dr. Fazel, illustrating that small dry gauze squares help achieve a good grip.
Considerations in biopsy technique
Dr. Fazel offered some tips and considerations when a punch biopsy is being done in the context of a chronic oral inflammatory condition, and the plan is to submit for hematoxylin and eosin (H&E) staining and direct immunofluorescence (DIF). Conditions where an intraoral punch biopsy would be considered include bullous or mucous membrane pemphigoid, pemphigus, lichen planus, and systemic lupus erythematosus, she said.
“Select a site with the most significant inflammatory changes” and aim for the most anterior site that exhibits these characteristics to maximize exposure and ensure a good specimen. The labial mucosa is a better choice in general than buccal mucosa, she said. “Maxillary and mandibular sulci are tricky sites,” especially when perilesional and lesional tissue should be included in the biopsies.
Next, Dr. Fazel walked attendees through general principles of preparing for and performing punch biopsies for H&E and DIF. In planning the biopsies, the DIF specimen should ideally be collected before the H&E specimen because the former technique will have higher yield when the specimen is taken from a less bloody field. “The yield of DIF is higher from the gingiva than from nonkeratinized surfaces.”
When infiltrating the biopsy site with local anesthesia, the needle should be centered within the lesion or general area to be biopsied, and care should be taken to maintain the orientation of the lesion to the surrounding tissue. Anesthesia can be infiltrated within the submucosal plane; the resultant ballooning will elevate the tissue to be biopsied and ease the procedure, she said.
Choose a 3-mm punch tool for gingival biopsies; 4 mm is a good size for other nonkeratinized surfaces. Unlike the procedure used for cutaneous biopsies, on delicate oral tissues, “you don’t need to hub your punch tool,” Dr. Fazel said. Similarly, the tool can be driven with firm rotation in one direction, rather than ratcheting back and forth, which may fray and deform the biopsy margins, she added. The specimen can be freed from surrounding mucosa with scissors alone and a gentle snipping motion; everting the tissue will help achieve the desired clean and gentle technique.
Because of the delicacy of the tissue, “it’s important to minimize the use of forceps, as well as any unnecessary manipulation of tissue in the process of specimen collection,” she said.
Salivary gland biopsies and intraoral suturing
Even minor salivary glands can be biopsied in a fairly straightforward way, though there’s a risk of short- and long-term loss of sensation, as well as more scarring than in other routine intraoral biopsies. Though these salivary glands lie just beneath the oral mucosa, care must be taken to avoid laceration of the orbicularis oris muscle during excision, noted Dr. Fazel. With a minor salivary gland biopsy, as with some other intraoral procedures, sutures will be needed. Consideration for the friability of the oral mucosa should drive suture material choice and closure technique.
First, “take bigger bites on each side of the incision, to minimize the risk of the suture tearing through the mucosa,” she said. Avoid forceps while suturing if possible, but be gentle if they are employed, “and be gentle tying knots: retract the mucosa as little as possible and cinch the knots down tightly with your fingers.”
Electrocautery, silver nitrate, and aluminum chloride are all reasonable options for hemostasis, although patients should be alerted that the tissue will have a charred appearance if electrocautery is used. Primary closure may be all that’s needed for hemostasis, said Dr. Fazel.
If nonabsorbable suture materials are used, nylon and prolene should be avoided since they tend to tear through the oral mucosa. Soft or braided silk are good choices, she said, and sutures can come out in 5-7 days.
Absorbable sutures have the advantage of not requiring removal, but they can be more irritating to the surrounding mucosa. Chromic or fast gut are the choices here, said Dr. Fazel. Whether absorbable or nonabsorbable sutures are placed, the size should be 4-0 or 5-0, she said.
Postoperative care, complications, and the limits of the dermatologist
Postoperatively, patients should know that swelling is to be expected, especially with procedures like minor salivary gland biopsies that involve the lip. Icing 15 minutes per hour for the first few hours will help with swelling; wound care is optimized with gentle salt water rinses. A bland diet that avoids acidic, spicy, and excessively hot foods and beverages will minimize wound irritation. Foods with sharp edges like chips, crackers, and nuts can actually catch sutures and cause pain and bleeding, so these too should be avoided.
As with dental work, care should be taken with eating or drinking until anesthesia has worn off, which may take up to 3 hours. Patients should also be cautioned that sutures are likely to come out prematurely just because of the mobility of the structures of the mouth with normal activities such as eating and talking.
Should a wound infection occur, said Dr. Fazel, it’s likely that mixed aerobic and anaerobic bacteria are to blame; accordingly, broad-spectrum beta-lactam antibiotics can be a good first-line course. More severe infections are more likely to have an anaerobic or gram-negative etiology; metronidazole is a reasonable choice for anaerobic coverage, she noted. The life-threatening complication not to miss is cellulitis of the floor of the mouth, or Ludwig angina. The swelling results in superior and posterior displacement of the tongue, obstructing the upper airway, so any patient suspected of having Ludwig angina needs emergent evaluation and treatment.
When should a dermatologist consider referral to an otolaryngologist rather than diving into a biopsy in the dermatology clinic? If the area of concern is on the posterior third of the tongue, access without special tools or higher levels of anesthesia becomes tricky, Dr. Fazel pointed out. The posterior hard palate, the soft palate, and the floor of the mouth are also regions best left to otolaryngologists, she said.
NEW YORK –The work of the dermatologist doesn’t need to stop at the lips, according to Nasim Fazel, MD, DDS, a board-certified dermatologist and dentist. she said, speaking at a session focused on oral health and procedures at the American Academy of Dermatology summer meeting.
Whether to perform an incisional or excisional biopsy on the lips or within the oral cavity is a decision driven by the clinical scenario, said Dr. Fazel, professor of clinical dermatology and director of the oral mucosal disease clinic at the University of California, Davis. Variables to consider, she said, include the size of the lesion, as well as whether the lesion is symptomatic or there’s any functional impairment. Other factors to bear in mind are whether the patient has any comorbid inflammatory conditions and whether the lesion could be malignant.
An excisional biopsy is a good procedure for small lesions that are thought to be benign, especially if they are exophytic, she noted. An example would be a traumatic fibroma, she said. This technique is also appropriate if there’s concern for dysplasia or malignancy if an office excisional biopsy is feasible given lesion size and location.
On the labial mucosa, an elliptical incision is often a good choice.
Cutaneous lip procedures
On the cutaneous lip, a punch incision can be feasible. The vermilion border should be marked to maintain orientation. “Avoid transecting the vermilion border to the extent that it’s possible,” said Dr. Fazel. Keep the vascular anatomy in mind as well, she added, since there’s a risk of severing the superior or inferior labial artery with procedures in this area. If this should happen, the branch can be identified and ligated with 4-0 fast gut or chromic gut suture material, she advised.
Another option on the cutaneous lip is shave removal. Here, a chalazion clamp can be used for both exposure and hemostasis. “Always suture parallel to the lip lines, and caution the patient that there may be significant, noticeable blanching when lip anesthesia’s used,” she said.
Gingival and tongue procedures
Moving to territory that may be less familiar for some dermatologists, Dr. Fazel walked through the process of a gingival punch biopsy. “Use local anesthetic, but a small quantity is sufficient,” she said. Using gentle pressure, the operator can work the punch instrument down to periosteal bone. At that point, just scissors can be used for undermining the specimen, with minimal disturbance of the mucosal surface.
Hemostasis after a gingival punch can be accomplished with silver nitrate or aluminum chloride or by electrocautery. A permanent defect in the gingiva can occur even with good technique, she said – a fact that should be included in the informed consent document for the procedure.
For lesions on the tongue, a shave removal can be considered, as can an incisional punch biopsy. An assistant’s hands are invaluable for stabilizing the tongue, said Dr. Fazel, illustrating that small dry gauze squares help achieve a good grip.
Considerations in biopsy technique
Dr. Fazel offered some tips and considerations when a punch biopsy is being done in the context of a chronic oral inflammatory condition, and the plan is to submit for hematoxylin and eosin (H&E) staining and direct immunofluorescence (DIF). Conditions where an intraoral punch biopsy would be considered include bullous or mucous membrane pemphigoid, pemphigus, lichen planus, and systemic lupus erythematosus, she said.
“Select a site with the most significant inflammatory changes” and aim for the most anterior site that exhibits these characteristics to maximize exposure and ensure a good specimen. The labial mucosa is a better choice in general than buccal mucosa, she said. “Maxillary and mandibular sulci are tricky sites,” especially when perilesional and lesional tissue should be included in the biopsies.
Next, Dr. Fazel walked attendees through general principles of preparing for and performing punch biopsies for H&E and DIF. In planning the biopsies, the DIF specimen should ideally be collected before the H&E specimen because the former technique will have higher yield when the specimen is taken from a less bloody field. “The yield of DIF is higher from the gingiva than from nonkeratinized surfaces.”
When infiltrating the biopsy site with local anesthesia, the needle should be centered within the lesion or general area to be biopsied, and care should be taken to maintain the orientation of the lesion to the surrounding tissue. Anesthesia can be infiltrated within the submucosal plane; the resultant ballooning will elevate the tissue to be biopsied and ease the procedure, she said.
Choose a 3-mm punch tool for gingival biopsies; 4 mm is a good size for other nonkeratinized surfaces. Unlike the procedure used for cutaneous biopsies, on delicate oral tissues, “you don’t need to hub your punch tool,” Dr. Fazel said. Similarly, the tool can be driven with firm rotation in one direction, rather than ratcheting back and forth, which may fray and deform the biopsy margins, she added. The specimen can be freed from surrounding mucosa with scissors alone and a gentle snipping motion; everting the tissue will help achieve the desired clean and gentle technique.
Because of the delicacy of the tissue, “it’s important to minimize the use of forceps, as well as any unnecessary manipulation of tissue in the process of specimen collection,” she said.
Salivary gland biopsies and intraoral suturing
Even minor salivary glands can be biopsied in a fairly straightforward way, though there’s a risk of short- and long-term loss of sensation, as well as more scarring than in other routine intraoral biopsies. Though these salivary glands lie just beneath the oral mucosa, care must be taken to avoid laceration of the orbicularis oris muscle during excision, noted Dr. Fazel. With a minor salivary gland biopsy, as with some other intraoral procedures, sutures will be needed. Consideration for the friability of the oral mucosa should drive suture material choice and closure technique.
First, “take bigger bites on each side of the incision, to minimize the risk of the suture tearing through the mucosa,” she said. Avoid forceps while suturing if possible, but be gentle if they are employed, “and be gentle tying knots: retract the mucosa as little as possible and cinch the knots down tightly with your fingers.”
Electrocautery, silver nitrate, and aluminum chloride are all reasonable options for hemostasis, although patients should be alerted that the tissue will have a charred appearance if electrocautery is used. Primary closure may be all that’s needed for hemostasis, said Dr. Fazel.
If nonabsorbable suture materials are used, nylon and prolene should be avoided since they tend to tear through the oral mucosa. Soft or braided silk are good choices, she said, and sutures can come out in 5-7 days.
Absorbable sutures have the advantage of not requiring removal, but they can be more irritating to the surrounding mucosa. Chromic or fast gut are the choices here, said Dr. Fazel. Whether absorbable or nonabsorbable sutures are placed, the size should be 4-0 or 5-0, she said.
Postoperative care, complications, and the limits of the dermatologist
Postoperatively, patients should know that swelling is to be expected, especially with procedures like minor salivary gland biopsies that involve the lip. Icing 15 minutes per hour for the first few hours will help with swelling; wound care is optimized with gentle salt water rinses. A bland diet that avoids acidic, spicy, and excessively hot foods and beverages will minimize wound irritation. Foods with sharp edges like chips, crackers, and nuts can actually catch sutures and cause pain and bleeding, so these too should be avoided.
As with dental work, care should be taken with eating or drinking until anesthesia has worn off, which may take up to 3 hours. Patients should also be cautioned that sutures are likely to come out prematurely just because of the mobility of the structures of the mouth with normal activities such as eating and talking.
Should a wound infection occur, said Dr. Fazel, it’s likely that mixed aerobic and anaerobic bacteria are to blame; accordingly, broad-spectrum beta-lactam antibiotics can be a good first-line course. More severe infections are more likely to have an anaerobic or gram-negative etiology; metronidazole is a reasonable choice for anaerobic coverage, she noted. The life-threatening complication not to miss is cellulitis of the floor of the mouth, or Ludwig angina. The swelling results in superior and posterior displacement of the tongue, obstructing the upper airway, so any patient suspected of having Ludwig angina needs emergent evaluation and treatment.
When should a dermatologist consider referral to an otolaryngologist rather than diving into a biopsy in the dermatology clinic? If the area of concern is on the posterior third of the tongue, access without special tools or higher levels of anesthesia becomes tricky, Dr. Fazel pointed out. The posterior hard palate, the soft palate, and the floor of the mouth are also regions best left to otolaryngologists, she said.
EXPERT ANALYSIS SUMMER AAD 2019
How to distinguish Stevens-Johnson syndrome from its mimickers
NEW YORK – said Lucia Seminario-Vidal, MD, PhD, speaking at a hospital dermatology–focused session of the summer meeting of the American Academy of Dermatology.
Even before histopathologic results are available, dermatologists can help take some of the panic out of the room when Stevens-Johnson syndrome or toxic epidermal necrolysis (SJS/TEN) is first on the differential diagnosis for the referring physician, she said. Physical findings, a careful review of systems, and past history – especially the introduction of any new medications – can go a long way toward ruling out SJS/TEN among many patients.
In a recent study coauthored by Dr. Seminario-Vidal, of the University of South Florida, Tampa, 208 inpatients with suspected SJS/TEN, 72% were given another diagnosis after a dermatologist consultation (J Am Acad Dermatol. 2019 Sep;81[3]:749-57). The study’s authors, led by Allison Weinkle, MD, a dermatology resident at the University of South Florida, performed a retrospective chart review of 208 patients suspected of having SJS/TEN and received inpatient dermatology consultations.
One surprising finding from the review is that “known risk factors for SJS/TEN such as drug exposure, malignancy, and HIV/AIDS are not helpful to differentiate it from its mimickers,” Dr. Seminario-Vidal said.
However, close attention to the clinical presentation is helpful in differentiating the mimickers from true SJS/TEN. Fever, painful skin, Nikolsky sign, and mucosal involvement were all more common in patients with SJS/TEN. “This was something that was really helpful to discuss with the primary teams at our institutions,” Dr. Seminario-Vidal said.
The most common mimickers in the cases she and her colleagues reviewed were severe cutaneous adverse drug reactions (SCARs) and erythema multiforme; in general, the mimickers were conditions that have severe mucocutaneous involvement.
Patients with SJS/TEN will have fever and pain, typically, and the primary lesions are atypical targets with a positive Nikolsky sign. Hepatic enzyme elevation is seen in 15% of patients, and lymphopenia may be present. Common drugs provoking SJS/TEN include antibiotics, anticonvulsants, NSAIDs, allopurinol, and – importantly – programmed cell death protein 1 (PD-1) inhibitors. Because PD-1s are being used for an ever-expanding range of oncology indications, the rate of SJS/TEN may be expected to rise, Dr. Seminario-Vidal noted.
Other common mimics can include a florid generalized fixed drug eruption, which can also be painful and have atypical targets and a positive Nikolsky sign. Here, large, dusky patches may be present, with perioral, genital, and hand/foot involvement common, but fever is absent. Lesions are sharply localized, round or oval, and they recur at the same site with reexposure to the provoking agent. “Histopathologic studies are diagnostic in these patients, but many times, if you have a good clinical history, you don’t need histopathology,” Dr. Seminario-Vidal said.
As with SJS/TEN, mucosal involvement can be present with fixed drug eruptions. However, hepatic enzymes and the complete blood count will not show abnormalities related to the fixed drug eruption.
Sulfonamides have been associated with up to 75% of fixed drug eruptions reported in some case series, she said, noting that common over-the-counter medications such as nonprescription analgesics, loratadine, and pseudoephedrine can also provoke fixed drug eruptions.
Bullous conditions that can mimic SJS/TEN include linear Immunoglobulin A bullous dermatosis. “We know that the classic presentation is the beautiful ‘string of pearls’ sign, but most patients won’t have this,” Dr. Seminario-Vidal said. The condition often appears in intertriginous locations, and Koebnerization can be a strong clue to this diagnosis, she added.
This painful condition rarely has an associated fever, and will occasionally involve the mucosa, but it doesn’t cause alterations in laboratory values. About 70% of cases of drug-induced linear IgA bullous dermatosis are caused by vancomycin, a consideration when patients may be on several antibiotics. “When I first started, I used to stop everything,” said Dr. Seminario-Vidal. Now, she first discontinues vancomycin and rechecks the patient the next day. In the absence of progression, vancomycin can be presumed to be the culprit, she said.
In bullous pemphigoid, mucosal involvement has been reported in up to 30% of patients, which can initially confuse the diagnosis. “A clue is the presence of tense bullae that initially are very pruritic, but they can become painful over time,” Dr. Seminario-Vidal said. “With tense bullae, with no specific primary lesion, but the patient is very itchy, think bullous pemphigoid.” Pain is sometimes present, but fever is rare. Eosinophilia occurs about 50% of the time, offering an additional diagnostic clue.
Furosemide is a common culprit in drug-induced bullous pemphigoid, as is its cousin bumetanide. Certain analgesics, amoxicillin, ciprofloxacin, and angiotensin converting enzyme inhibitors have also been implicated, said Dr. Seminario-Vidal, though most cases are not drug induced. “Go over the drug history of the patients. It’s something that I cannot emphasize enough … because if you find the drug that causes this disease, you can avoid lengthy systemic treatment.”
Pemphigus foliaceus has a characteristic crusting scale that forms with the rupture of flaccid bullae. Nikolsky’s sign is positive. Mucosal involvement is rare, but is sometimes seen on the occasions when the condition is drug-induced, and laboratory values are usually normal, she said. “The clues to diagnosis of these patients are involvement in the seborrheic areas, including the face; there’s a lot of crust in pemphigus foliaceus.”
Drug-induced pemphigus foliaceus is associated with drugs that have a thiol group, or with sulfur groups that are converted to thiol (–SH) groups. These include both angiotensin converting enzyme inhibitors and angiotensin receptor blockers, penicillins, cephalosporins, and piroxicam. However, said Dr. Seminario-Vidal, penicillamine alone accounts for 50% of drug-induced pemphigus foliaceus.
Dr. Seminario-Vidal reported financial relationships with Eli Lilly, Soligenix, Helsinn, Eisai, Boehringer Ingelheim, Corrona, Akros, Novartis, AbbVie, BMS, Celgene, Glenmark, and Kyowa Kirin.
SOURCE: Seminario-Vidal L. Summer AAD 2019, Session F-025.
NEW YORK – said Lucia Seminario-Vidal, MD, PhD, speaking at a hospital dermatology–focused session of the summer meeting of the American Academy of Dermatology.
Even before histopathologic results are available, dermatologists can help take some of the panic out of the room when Stevens-Johnson syndrome or toxic epidermal necrolysis (SJS/TEN) is first on the differential diagnosis for the referring physician, she said. Physical findings, a careful review of systems, and past history – especially the introduction of any new medications – can go a long way toward ruling out SJS/TEN among many patients.
In a recent study coauthored by Dr. Seminario-Vidal, of the University of South Florida, Tampa, 208 inpatients with suspected SJS/TEN, 72% were given another diagnosis after a dermatologist consultation (J Am Acad Dermatol. 2019 Sep;81[3]:749-57). The study’s authors, led by Allison Weinkle, MD, a dermatology resident at the University of South Florida, performed a retrospective chart review of 208 patients suspected of having SJS/TEN and received inpatient dermatology consultations.
One surprising finding from the review is that “known risk factors for SJS/TEN such as drug exposure, malignancy, and HIV/AIDS are not helpful to differentiate it from its mimickers,” Dr. Seminario-Vidal said.
However, close attention to the clinical presentation is helpful in differentiating the mimickers from true SJS/TEN. Fever, painful skin, Nikolsky sign, and mucosal involvement were all more common in patients with SJS/TEN. “This was something that was really helpful to discuss with the primary teams at our institutions,” Dr. Seminario-Vidal said.
The most common mimickers in the cases she and her colleagues reviewed were severe cutaneous adverse drug reactions (SCARs) and erythema multiforme; in general, the mimickers were conditions that have severe mucocutaneous involvement.
Patients with SJS/TEN will have fever and pain, typically, and the primary lesions are atypical targets with a positive Nikolsky sign. Hepatic enzyme elevation is seen in 15% of patients, and lymphopenia may be present. Common drugs provoking SJS/TEN include antibiotics, anticonvulsants, NSAIDs, allopurinol, and – importantly – programmed cell death protein 1 (PD-1) inhibitors. Because PD-1s are being used for an ever-expanding range of oncology indications, the rate of SJS/TEN may be expected to rise, Dr. Seminario-Vidal noted.
Other common mimics can include a florid generalized fixed drug eruption, which can also be painful and have atypical targets and a positive Nikolsky sign. Here, large, dusky patches may be present, with perioral, genital, and hand/foot involvement common, but fever is absent. Lesions are sharply localized, round or oval, and they recur at the same site with reexposure to the provoking agent. “Histopathologic studies are diagnostic in these patients, but many times, if you have a good clinical history, you don’t need histopathology,” Dr. Seminario-Vidal said.
As with SJS/TEN, mucosal involvement can be present with fixed drug eruptions. However, hepatic enzymes and the complete blood count will not show abnormalities related to the fixed drug eruption.
Sulfonamides have been associated with up to 75% of fixed drug eruptions reported in some case series, she said, noting that common over-the-counter medications such as nonprescription analgesics, loratadine, and pseudoephedrine can also provoke fixed drug eruptions.
Bullous conditions that can mimic SJS/TEN include linear Immunoglobulin A bullous dermatosis. “We know that the classic presentation is the beautiful ‘string of pearls’ sign, but most patients won’t have this,” Dr. Seminario-Vidal said. The condition often appears in intertriginous locations, and Koebnerization can be a strong clue to this diagnosis, she added.
This painful condition rarely has an associated fever, and will occasionally involve the mucosa, but it doesn’t cause alterations in laboratory values. About 70% of cases of drug-induced linear IgA bullous dermatosis are caused by vancomycin, a consideration when patients may be on several antibiotics. “When I first started, I used to stop everything,” said Dr. Seminario-Vidal. Now, she first discontinues vancomycin and rechecks the patient the next day. In the absence of progression, vancomycin can be presumed to be the culprit, she said.
In bullous pemphigoid, mucosal involvement has been reported in up to 30% of patients, which can initially confuse the diagnosis. “A clue is the presence of tense bullae that initially are very pruritic, but they can become painful over time,” Dr. Seminario-Vidal said. “With tense bullae, with no specific primary lesion, but the patient is very itchy, think bullous pemphigoid.” Pain is sometimes present, but fever is rare. Eosinophilia occurs about 50% of the time, offering an additional diagnostic clue.
Furosemide is a common culprit in drug-induced bullous pemphigoid, as is its cousin bumetanide. Certain analgesics, amoxicillin, ciprofloxacin, and angiotensin converting enzyme inhibitors have also been implicated, said Dr. Seminario-Vidal, though most cases are not drug induced. “Go over the drug history of the patients. It’s something that I cannot emphasize enough … because if you find the drug that causes this disease, you can avoid lengthy systemic treatment.”
Pemphigus foliaceus has a characteristic crusting scale that forms with the rupture of flaccid bullae. Nikolsky’s sign is positive. Mucosal involvement is rare, but is sometimes seen on the occasions when the condition is drug-induced, and laboratory values are usually normal, she said. “The clues to diagnosis of these patients are involvement in the seborrheic areas, including the face; there’s a lot of crust in pemphigus foliaceus.”
Drug-induced pemphigus foliaceus is associated with drugs that have a thiol group, or with sulfur groups that are converted to thiol (–SH) groups. These include both angiotensin converting enzyme inhibitors and angiotensin receptor blockers, penicillins, cephalosporins, and piroxicam. However, said Dr. Seminario-Vidal, penicillamine alone accounts for 50% of drug-induced pemphigus foliaceus.
Dr. Seminario-Vidal reported financial relationships with Eli Lilly, Soligenix, Helsinn, Eisai, Boehringer Ingelheim, Corrona, Akros, Novartis, AbbVie, BMS, Celgene, Glenmark, and Kyowa Kirin.
SOURCE: Seminario-Vidal L. Summer AAD 2019, Session F-025.
NEW YORK – said Lucia Seminario-Vidal, MD, PhD, speaking at a hospital dermatology–focused session of the summer meeting of the American Academy of Dermatology.
Even before histopathologic results are available, dermatologists can help take some of the panic out of the room when Stevens-Johnson syndrome or toxic epidermal necrolysis (SJS/TEN) is first on the differential diagnosis for the referring physician, she said. Physical findings, a careful review of systems, and past history – especially the introduction of any new medications – can go a long way toward ruling out SJS/TEN among many patients.
In a recent study coauthored by Dr. Seminario-Vidal, of the University of South Florida, Tampa, 208 inpatients with suspected SJS/TEN, 72% were given another diagnosis after a dermatologist consultation (J Am Acad Dermatol. 2019 Sep;81[3]:749-57). The study’s authors, led by Allison Weinkle, MD, a dermatology resident at the University of South Florida, performed a retrospective chart review of 208 patients suspected of having SJS/TEN and received inpatient dermatology consultations.
One surprising finding from the review is that “known risk factors for SJS/TEN such as drug exposure, malignancy, and HIV/AIDS are not helpful to differentiate it from its mimickers,” Dr. Seminario-Vidal said.
However, close attention to the clinical presentation is helpful in differentiating the mimickers from true SJS/TEN. Fever, painful skin, Nikolsky sign, and mucosal involvement were all more common in patients with SJS/TEN. “This was something that was really helpful to discuss with the primary teams at our institutions,” Dr. Seminario-Vidal said.
The most common mimickers in the cases she and her colleagues reviewed were severe cutaneous adverse drug reactions (SCARs) and erythema multiforme; in general, the mimickers were conditions that have severe mucocutaneous involvement.
Patients with SJS/TEN will have fever and pain, typically, and the primary lesions are atypical targets with a positive Nikolsky sign. Hepatic enzyme elevation is seen in 15% of patients, and lymphopenia may be present. Common drugs provoking SJS/TEN include antibiotics, anticonvulsants, NSAIDs, allopurinol, and – importantly – programmed cell death protein 1 (PD-1) inhibitors. Because PD-1s are being used for an ever-expanding range of oncology indications, the rate of SJS/TEN may be expected to rise, Dr. Seminario-Vidal noted.
Other common mimics can include a florid generalized fixed drug eruption, which can also be painful and have atypical targets and a positive Nikolsky sign. Here, large, dusky patches may be present, with perioral, genital, and hand/foot involvement common, but fever is absent. Lesions are sharply localized, round or oval, and they recur at the same site with reexposure to the provoking agent. “Histopathologic studies are diagnostic in these patients, but many times, if you have a good clinical history, you don’t need histopathology,” Dr. Seminario-Vidal said.
As with SJS/TEN, mucosal involvement can be present with fixed drug eruptions. However, hepatic enzymes and the complete blood count will not show abnormalities related to the fixed drug eruption.
Sulfonamides have been associated with up to 75% of fixed drug eruptions reported in some case series, she said, noting that common over-the-counter medications such as nonprescription analgesics, loratadine, and pseudoephedrine can also provoke fixed drug eruptions.
Bullous conditions that can mimic SJS/TEN include linear Immunoglobulin A bullous dermatosis. “We know that the classic presentation is the beautiful ‘string of pearls’ sign, but most patients won’t have this,” Dr. Seminario-Vidal said. The condition often appears in intertriginous locations, and Koebnerization can be a strong clue to this diagnosis, she added.
This painful condition rarely has an associated fever, and will occasionally involve the mucosa, but it doesn’t cause alterations in laboratory values. About 70% of cases of drug-induced linear IgA bullous dermatosis are caused by vancomycin, a consideration when patients may be on several antibiotics. “When I first started, I used to stop everything,” said Dr. Seminario-Vidal. Now, she first discontinues vancomycin and rechecks the patient the next day. In the absence of progression, vancomycin can be presumed to be the culprit, she said.
In bullous pemphigoid, mucosal involvement has been reported in up to 30% of patients, which can initially confuse the diagnosis. “A clue is the presence of tense bullae that initially are very pruritic, but they can become painful over time,” Dr. Seminario-Vidal said. “With tense bullae, with no specific primary lesion, but the patient is very itchy, think bullous pemphigoid.” Pain is sometimes present, but fever is rare. Eosinophilia occurs about 50% of the time, offering an additional diagnostic clue.
Furosemide is a common culprit in drug-induced bullous pemphigoid, as is its cousin bumetanide. Certain analgesics, amoxicillin, ciprofloxacin, and angiotensin converting enzyme inhibitors have also been implicated, said Dr. Seminario-Vidal, though most cases are not drug induced. “Go over the drug history of the patients. It’s something that I cannot emphasize enough … because if you find the drug that causes this disease, you can avoid lengthy systemic treatment.”
Pemphigus foliaceus has a characteristic crusting scale that forms with the rupture of flaccid bullae. Nikolsky’s sign is positive. Mucosal involvement is rare, but is sometimes seen on the occasions when the condition is drug-induced, and laboratory values are usually normal, she said. “The clues to diagnosis of these patients are involvement in the seborrheic areas, including the face; there’s a lot of crust in pemphigus foliaceus.”
Drug-induced pemphigus foliaceus is associated with drugs that have a thiol group, or with sulfur groups that are converted to thiol (–SH) groups. These include both angiotensin converting enzyme inhibitors and angiotensin receptor blockers, penicillins, cephalosporins, and piroxicam. However, said Dr. Seminario-Vidal, penicillamine alone accounts for 50% of drug-induced pemphigus foliaceus.
Dr. Seminario-Vidal reported financial relationships with Eli Lilly, Soligenix, Helsinn, Eisai, Boehringer Ingelheim, Corrona, Akros, Novartis, AbbVie, BMS, Celgene, Glenmark, and Kyowa Kirin.
SOURCE: Seminario-Vidal L. Summer AAD 2019, Session F-025.
EXPERT ANALYSIS FROM SUMMER AAD 2019
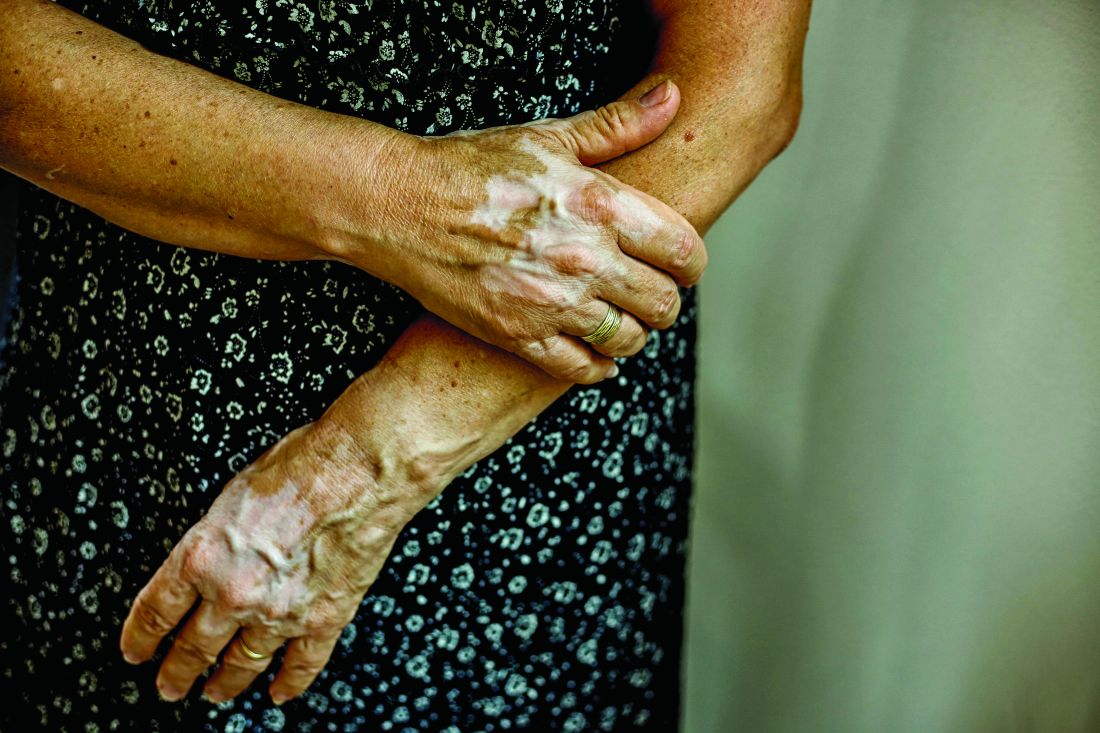
Recent progress in vitiligo treatment might be heading to vitiligo cure
NEW YORK – but also might be leading to a strategy that will prevent the inevitable relapse that occurs after treatment is stopped, according to an update at the American Academy of Dermatology summer meeting.
Recently, trial results with a Janus kinase (JAK) pathway inhibitor have shown promise for treatment of vitiligo, but the ultimate fix for this recurring autoimmune disease might be elimination of resident-memory T cells, according to John Harris, MD, PhD, of the department of dermatology at the University of Massachusetts, Worcester.
In a murine vitiligo model, targeting interleukin-15, a cytokine thought to be essential for maintaining memory T cells, produced rapid and durable repigmentation without apparent adverse effects in a series of studies sufficiently promising that clinical trials are now being actively planned, Dr. Harris said. The ongoing work to eliminate resident-memory T cells to prevent relapse of vitiligo comes at the end of other recent advances that have provided major insights into the pathophysiology of vitiligo.
As outlined by Dr. Harris, vitiligo involves an autoimmune sequence that includes up-regulation of interferon-gamma, activation of the JAK signaling pathway, and mobilization of the cytokine CXCl10, all of which are part of the sequence of events culminating in activation of T cells that attack the melanocyte. The process can be stopped when any of these events are targeted, according to the experimental studies. These findings have already been translated into new drug development.
“There are now three ongoing clinical trials with JAK inhibitors. This is a tremendous advance in a disease for which there have been no clinical trials for decades,” Dr. Harris said. He cited highly positive data with the JAK inhibitor ruxolitinib, which were reported just weeks earlier at the World Congress of Dermatology, to confirm that this principle of intervention is viable.
However, relapse after discontinuation of ruxolitinib, like other treatments for vitiligo, is high. The observation that relapses typically occur in the exact spot where skin lesions occurred previously created the framework of a new potential wave of advances, according to Dr. Harris, director of the Vitiligo Clinic and Research Center at the University of Massachusetts, Worcester.
These advances involve progress in understanding the role of resident-memory T cells in driving autoimmune disease relapse.
In principle, memory-resident T cells are left behind in order to stimulate a rapid immune response in the event of a recurrence of a virus or another pathogen. According to work performed in animal models of vitiligo, they also appear to play a critical role in reactivation of this autoimmune disease, Dr. Harris said.
This role was not surprising, but the potential breakthrough in vitiligo surrounds evidence that the cytokine IL-15 is essential to the creation and maintenance of these memory cells. Evidence suggests vitiligo in animal models does not recur in the absence of IL-15, making it a potential target for treatment.
Initially, there was concern that inhibition of IL-15 would have off-target effects, but this concern has diminished with antibodies designed to inhibit IL-15 signaling in the animal model.
“It turns out that autoreactive cells are much more dependent on the cytokine than other T cells,” he said.
In the animal model, repigmentation has occurred more rapidly with anti-IL-15 therapy than with any other treatment tested to date, but more importantly, these mice then appear to be protected from vitiligo recurrence for extended periods, Dr. Harris noted.
Studies conducted with human tissue have provided strong evidence that the same mechanisms are in play. There are now several approaches to blocking IL-15 signaling, including a monoclonal antibody targeted at the IL-15 receptor, in development. This latter approach is now the focus of a company formed by Dr. Harris.
It is not yet clear if one approach to the inhibition of IL-15 will be superior to another, but Dr. Harris is highly optimistic that this will be a viable approach to control of vitiligo. Noting that good results have been achieved in experimental models by skin injections, thereby avoiding systemic exposure, he is also optimistic that this approach will be well tolerated.
“Based on these data, we are expecting clinical trials soon,” he said.
Dr. Harris reported serving as a consultant and/or investigator for multiple pharmaceutical companies including Aclaris Therapeutics, Celgene, EMD Serono, Genzyme, Incyte, and Janssen Biotech.
NEW YORK – but also might be leading to a strategy that will prevent the inevitable relapse that occurs after treatment is stopped, according to an update at the American Academy of Dermatology summer meeting.
Recently, trial results with a Janus kinase (JAK) pathway inhibitor have shown promise for treatment of vitiligo, but the ultimate fix for this recurring autoimmune disease might be elimination of resident-memory T cells, according to John Harris, MD, PhD, of the department of dermatology at the University of Massachusetts, Worcester.
In a murine vitiligo model, targeting interleukin-15, a cytokine thought to be essential for maintaining memory T cells, produced rapid and durable repigmentation without apparent adverse effects in a series of studies sufficiently promising that clinical trials are now being actively planned, Dr. Harris said. The ongoing work to eliminate resident-memory T cells to prevent relapse of vitiligo comes at the end of other recent advances that have provided major insights into the pathophysiology of vitiligo.
As outlined by Dr. Harris, vitiligo involves an autoimmune sequence that includes up-regulation of interferon-gamma, activation of the JAK signaling pathway, and mobilization of the cytokine CXCl10, all of which are part of the sequence of events culminating in activation of T cells that attack the melanocyte. The process can be stopped when any of these events are targeted, according to the experimental studies. These findings have already been translated into new drug development.
“There are now three ongoing clinical trials with JAK inhibitors. This is a tremendous advance in a disease for which there have been no clinical trials for decades,” Dr. Harris said. He cited highly positive data with the JAK inhibitor ruxolitinib, which were reported just weeks earlier at the World Congress of Dermatology, to confirm that this principle of intervention is viable.
However, relapse after discontinuation of ruxolitinib, like other treatments for vitiligo, is high. The observation that relapses typically occur in the exact spot where skin lesions occurred previously created the framework of a new potential wave of advances, according to Dr. Harris, director of the Vitiligo Clinic and Research Center at the University of Massachusetts, Worcester.
These advances involve progress in understanding the role of resident-memory T cells in driving autoimmune disease relapse.
In principle, memory-resident T cells are left behind in order to stimulate a rapid immune response in the event of a recurrence of a virus or another pathogen. According to work performed in animal models of vitiligo, they also appear to play a critical role in reactivation of this autoimmune disease, Dr. Harris said.
This role was not surprising, but the potential breakthrough in vitiligo surrounds evidence that the cytokine IL-15 is essential to the creation and maintenance of these memory cells. Evidence suggests vitiligo in animal models does not recur in the absence of IL-15, making it a potential target for treatment.
Initially, there was concern that inhibition of IL-15 would have off-target effects, but this concern has diminished with antibodies designed to inhibit IL-15 signaling in the animal model.
“It turns out that autoreactive cells are much more dependent on the cytokine than other T cells,” he said.
In the animal model, repigmentation has occurred more rapidly with anti-IL-15 therapy than with any other treatment tested to date, but more importantly, these mice then appear to be protected from vitiligo recurrence for extended periods, Dr. Harris noted.
Studies conducted with human tissue have provided strong evidence that the same mechanisms are in play. There are now several approaches to blocking IL-15 signaling, including a monoclonal antibody targeted at the IL-15 receptor, in development. This latter approach is now the focus of a company formed by Dr. Harris.
It is not yet clear if one approach to the inhibition of IL-15 will be superior to another, but Dr. Harris is highly optimistic that this will be a viable approach to control of vitiligo. Noting that good results have been achieved in experimental models by skin injections, thereby avoiding systemic exposure, he is also optimistic that this approach will be well tolerated.
“Based on these data, we are expecting clinical trials soon,” he said.
Dr. Harris reported serving as a consultant and/or investigator for multiple pharmaceutical companies including Aclaris Therapeutics, Celgene, EMD Serono, Genzyme, Incyte, and Janssen Biotech.
NEW YORK – but also might be leading to a strategy that will prevent the inevitable relapse that occurs after treatment is stopped, according to an update at the American Academy of Dermatology summer meeting.
Recently, trial results with a Janus kinase (JAK) pathway inhibitor have shown promise for treatment of vitiligo, but the ultimate fix for this recurring autoimmune disease might be elimination of resident-memory T cells, according to John Harris, MD, PhD, of the department of dermatology at the University of Massachusetts, Worcester.
In a murine vitiligo model, targeting interleukin-15, a cytokine thought to be essential for maintaining memory T cells, produced rapid and durable repigmentation without apparent adverse effects in a series of studies sufficiently promising that clinical trials are now being actively planned, Dr. Harris said. The ongoing work to eliminate resident-memory T cells to prevent relapse of vitiligo comes at the end of other recent advances that have provided major insights into the pathophysiology of vitiligo.
As outlined by Dr. Harris, vitiligo involves an autoimmune sequence that includes up-regulation of interferon-gamma, activation of the JAK signaling pathway, and mobilization of the cytokine CXCl10, all of which are part of the sequence of events culminating in activation of T cells that attack the melanocyte. The process can be stopped when any of these events are targeted, according to the experimental studies. These findings have already been translated into new drug development.
“There are now three ongoing clinical trials with JAK inhibitors. This is a tremendous advance in a disease for which there have been no clinical trials for decades,” Dr. Harris said. He cited highly positive data with the JAK inhibitor ruxolitinib, which were reported just weeks earlier at the World Congress of Dermatology, to confirm that this principle of intervention is viable.
However, relapse after discontinuation of ruxolitinib, like other treatments for vitiligo, is high. The observation that relapses typically occur in the exact spot where skin lesions occurred previously created the framework of a new potential wave of advances, according to Dr. Harris, director of the Vitiligo Clinic and Research Center at the University of Massachusetts, Worcester.
These advances involve progress in understanding the role of resident-memory T cells in driving autoimmune disease relapse.
In principle, memory-resident T cells are left behind in order to stimulate a rapid immune response in the event of a recurrence of a virus or another pathogen. According to work performed in animal models of vitiligo, they also appear to play a critical role in reactivation of this autoimmune disease, Dr. Harris said.
This role was not surprising, but the potential breakthrough in vitiligo surrounds evidence that the cytokine IL-15 is essential to the creation and maintenance of these memory cells. Evidence suggests vitiligo in animal models does not recur in the absence of IL-15, making it a potential target for treatment.
Initially, there was concern that inhibition of IL-15 would have off-target effects, but this concern has diminished with antibodies designed to inhibit IL-15 signaling in the animal model.
“It turns out that autoreactive cells are much more dependent on the cytokine than other T cells,” he said.
In the animal model, repigmentation has occurred more rapidly with anti-IL-15 therapy than with any other treatment tested to date, but more importantly, these mice then appear to be protected from vitiligo recurrence for extended periods, Dr. Harris noted.
Studies conducted with human tissue have provided strong evidence that the same mechanisms are in play. There are now several approaches to blocking IL-15 signaling, including a monoclonal antibody targeted at the IL-15 receptor, in development. This latter approach is now the focus of a company formed by Dr. Harris.
It is not yet clear if one approach to the inhibition of IL-15 will be superior to another, but Dr. Harris is highly optimistic that this will be a viable approach to control of vitiligo. Noting that good results have been achieved in experimental models by skin injections, thereby avoiding systemic exposure, he is also optimistic that this approach will be well tolerated.
“Based on these data, we are expecting clinical trials soon,” he said.
Dr. Harris reported serving as a consultant and/or investigator for multiple pharmaceutical companies including Aclaris Therapeutics, Celgene, EMD Serono, Genzyme, Incyte, and Janssen Biotech.
EXPERT ANALYSIS FROM SUMMER AAD 2019
Dermatologists urged to take ownership of preventable AEs
NEW YORK – according to Galen T. Foulke, MD, who discussed avoidable clinical disasters in practice at the American Academy of Dermatology summer meeting.
Of a list of known and predictable risks that “fall under the purview of ‘You Should Have Known Better,’ ” Dr. Foulke focused on glucocorticoid-associated osteoporosis and infections associated with biologics.
Prior to delivering advice about preventing osteoporosis in patients taking glucocorticoids, he polled the audience about what they considered appropriate prophylaxis in this setting. The vast majority opted for vitamin D and calcium supplementation.
“This is a common answer, but it is the wrong answer,” said Dr. Foulke, a dermatologist affiliated with Penn State Milton S. Hershey Medical Center in Hershey, Pennsylvania.
The available data show that patients on vitamin D and calcium supplementation will continue to lose bone density on therapeutic doses of steroids, according to Dr. Foulke. This is true even when the daily doses for these supplements exceed 800 units and 900 mg, respectively. Moreover, calcium supplementation is associated with an increased risk of heart disease in patients without a calcium deficiency, he noted.
The correct answer is a bisphosphonate, said Dr. Foulke. Of the bisphosphonates, he recommended alendronate as one that is particularly well tolerated and readily reimbursed.
He believes that dermatologists prescribing glucocorticoids should not overlook the substantial risk of osteoporosis or their responsibility to discuss strategies for risk mitigation. Moreover, he believes dermatologists should consider prescribing alendronate in the appropriate candidates, not just refer to another specialist.
“In the first year of steroid use, substantial bone loss is a risk even at doses below 5 mg,” Dr. Foulke warned. At higher doses, patients can lose up to 25% of their bone density, he added.
Of preventable risks of biologics, Dr. Foulke focused on infection. In particular, he urged dermatologists who prescribe these drugs to routinely inform patients about the role and safety of vaccines in infection prevention.
“An immunosuppressant suppresses the immune system, increasing the risk of infection. It is our responsibility to protect patients from the known risks of the therapies we offer them,” he said.
Several organizations recommend the pneumococcal vaccine series and the annual influenza vaccine for patients taking biologics. Although Dr. Foulke was unable to find reliable data on vaccination rates among patients prescribed a biologic for a dermatologic indication, he cited rheumatology practice data to suggest that less than half of patients receive this protection.
A major reason for the low rate of vaccination was failure of the biologic prescriber to assume responsibility for this recommended step, according to Dr. Foulke. Although he does not believe that biologic prescribers need to administer the vaccine, and he acknowledged that he does not stock vaccines in his clinic, he does believe they should inform patients when vaccination is safe and appropriate.
Live attenuated vaccines, in his opinion, are not safe. Although he reported that this is an area of controversy, he takes a conservative approach, advising candidates for a live attenuated vaccine to undergo vaccination prior to starting the biologic or during a break from biologic therapy.
When he polled the audience about which vaccines are live attenuated vaccines, several failed to recognize that the MMR vaccine falls into this category. However, he also noted that the majority of vaccines are not live attenuated and should be considered. He specifically singled out the recombinant herpes zoster as a vaccine recommended by the American College of Rheumatology in patients on biologics.
“We do not have to give the shots, but we should be the ones who start the discussion,” said Dr. Foulke, referring to vaccines in patients on a biologic. He called these important steps “to protect patients from preventable disasters.”
Dr. Foulke reported no potential conflicts of interest.
SOURCE: Summer AAD 2019, Session F02.
NEW YORK – according to Galen T. Foulke, MD, who discussed avoidable clinical disasters in practice at the American Academy of Dermatology summer meeting.
Of a list of known and predictable risks that “fall under the purview of ‘You Should Have Known Better,’ ” Dr. Foulke focused on glucocorticoid-associated osteoporosis and infections associated with biologics.
Prior to delivering advice about preventing osteoporosis in patients taking glucocorticoids, he polled the audience about what they considered appropriate prophylaxis in this setting. The vast majority opted for vitamin D and calcium supplementation.
“This is a common answer, but it is the wrong answer,” said Dr. Foulke, a dermatologist affiliated with Penn State Milton S. Hershey Medical Center in Hershey, Pennsylvania.
The available data show that patients on vitamin D and calcium supplementation will continue to lose bone density on therapeutic doses of steroids, according to Dr. Foulke. This is true even when the daily doses for these supplements exceed 800 units and 900 mg, respectively. Moreover, calcium supplementation is associated with an increased risk of heart disease in patients without a calcium deficiency, he noted.
The correct answer is a bisphosphonate, said Dr. Foulke. Of the bisphosphonates, he recommended alendronate as one that is particularly well tolerated and readily reimbursed.
He believes that dermatologists prescribing glucocorticoids should not overlook the substantial risk of osteoporosis or their responsibility to discuss strategies for risk mitigation. Moreover, he believes dermatologists should consider prescribing alendronate in the appropriate candidates, not just refer to another specialist.
“In the first year of steroid use, substantial bone loss is a risk even at doses below 5 mg,” Dr. Foulke warned. At higher doses, patients can lose up to 25% of their bone density, he added.
Of preventable risks of biologics, Dr. Foulke focused on infection. In particular, he urged dermatologists who prescribe these drugs to routinely inform patients about the role and safety of vaccines in infection prevention.
“An immunosuppressant suppresses the immune system, increasing the risk of infection. It is our responsibility to protect patients from the known risks of the therapies we offer them,” he said.
Several organizations recommend the pneumococcal vaccine series and the annual influenza vaccine for patients taking biologics. Although Dr. Foulke was unable to find reliable data on vaccination rates among patients prescribed a biologic for a dermatologic indication, he cited rheumatology practice data to suggest that less than half of patients receive this protection.
A major reason for the low rate of vaccination was failure of the biologic prescriber to assume responsibility for this recommended step, according to Dr. Foulke. Although he does not believe that biologic prescribers need to administer the vaccine, and he acknowledged that he does not stock vaccines in his clinic, he does believe they should inform patients when vaccination is safe and appropriate.
Live attenuated vaccines, in his opinion, are not safe. Although he reported that this is an area of controversy, he takes a conservative approach, advising candidates for a live attenuated vaccine to undergo vaccination prior to starting the biologic or during a break from biologic therapy.
When he polled the audience about which vaccines are live attenuated vaccines, several failed to recognize that the MMR vaccine falls into this category. However, he also noted that the majority of vaccines are not live attenuated and should be considered. He specifically singled out the recombinant herpes zoster as a vaccine recommended by the American College of Rheumatology in patients on biologics.
“We do not have to give the shots, but we should be the ones who start the discussion,” said Dr. Foulke, referring to vaccines in patients on a biologic. He called these important steps “to protect patients from preventable disasters.”
Dr. Foulke reported no potential conflicts of interest.
SOURCE: Summer AAD 2019, Session F02.
NEW YORK – according to Galen T. Foulke, MD, who discussed avoidable clinical disasters in practice at the American Academy of Dermatology summer meeting.
Of a list of known and predictable risks that “fall under the purview of ‘You Should Have Known Better,’ ” Dr. Foulke focused on glucocorticoid-associated osteoporosis and infections associated with biologics.
Prior to delivering advice about preventing osteoporosis in patients taking glucocorticoids, he polled the audience about what they considered appropriate prophylaxis in this setting. The vast majority opted for vitamin D and calcium supplementation.
“This is a common answer, but it is the wrong answer,” said Dr. Foulke, a dermatologist affiliated with Penn State Milton S. Hershey Medical Center in Hershey, Pennsylvania.
The available data show that patients on vitamin D and calcium supplementation will continue to lose bone density on therapeutic doses of steroids, according to Dr. Foulke. This is true even when the daily doses for these supplements exceed 800 units and 900 mg, respectively. Moreover, calcium supplementation is associated with an increased risk of heart disease in patients without a calcium deficiency, he noted.
The correct answer is a bisphosphonate, said Dr. Foulke. Of the bisphosphonates, he recommended alendronate as one that is particularly well tolerated and readily reimbursed.
He believes that dermatologists prescribing glucocorticoids should not overlook the substantial risk of osteoporosis or their responsibility to discuss strategies for risk mitigation. Moreover, he believes dermatologists should consider prescribing alendronate in the appropriate candidates, not just refer to another specialist.
“In the first year of steroid use, substantial bone loss is a risk even at doses below 5 mg,” Dr. Foulke warned. At higher doses, patients can lose up to 25% of their bone density, he added.
Of preventable risks of biologics, Dr. Foulke focused on infection. In particular, he urged dermatologists who prescribe these drugs to routinely inform patients about the role and safety of vaccines in infection prevention.
“An immunosuppressant suppresses the immune system, increasing the risk of infection. It is our responsibility to protect patients from the known risks of the therapies we offer them,” he said.
Several organizations recommend the pneumococcal vaccine series and the annual influenza vaccine for patients taking biologics. Although Dr. Foulke was unable to find reliable data on vaccination rates among patients prescribed a biologic for a dermatologic indication, he cited rheumatology practice data to suggest that less than half of patients receive this protection.
A major reason for the low rate of vaccination was failure of the biologic prescriber to assume responsibility for this recommended step, according to Dr. Foulke. Although he does not believe that biologic prescribers need to administer the vaccine, and he acknowledged that he does not stock vaccines in his clinic, he does believe they should inform patients when vaccination is safe and appropriate.
Live attenuated vaccines, in his opinion, are not safe. Although he reported that this is an area of controversy, he takes a conservative approach, advising candidates for a live attenuated vaccine to undergo vaccination prior to starting the biologic or during a break from biologic therapy.
When he polled the audience about which vaccines are live attenuated vaccines, several failed to recognize that the MMR vaccine falls into this category. However, he also noted that the majority of vaccines are not live attenuated and should be considered. He specifically singled out the recombinant herpes zoster as a vaccine recommended by the American College of Rheumatology in patients on biologics.
“We do not have to give the shots, but we should be the ones who start the discussion,” said Dr. Foulke, referring to vaccines in patients on a biologic. He called these important steps “to protect patients from preventable disasters.”
Dr. Foulke reported no potential conflicts of interest.
SOURCE: Summer AAD 2019, Session F02.
EXPERT ANALYSIS FROM SUMMER AAD 2019
Nicotinamide-containing products gaining interest for aging, dermatologic disorders
NEW YORK – More patients are inquiring about the antiaging claims made for nicotinamide products, according to Christine DeWitt MD, of the department of dermatology, Georgetown University, Washington. She encouraged attendees at the American Academy of Dermatology summer meeting to gain familiarity with the underlying mechanisms and potential uses of nicotinamide for aging skin and prevention of skin cancer as well as for a variety of dermatologic disorders, including atopic dermatitis and bullous pemphigoid.
The ability of nicotinamide to increase oxidized nicotinamide adenine dinucleotide (NAD+) is credited for most of its dermatologic benefits, according to Dr. DeWitt. She explained that NAD+ has a central role in cell metabolism, including serving as a substrate for sirtuins, which help prevent deterioration of telomeres, now thought to be a critical event in aging.
Downstream effects include an improved barrier function to reduce transdermal water loss in patients with atopic dermatitis and anti-inflammatory effects that are relevant to acne and bullous pemphigoid.
The related but unique forms of vitamin B3, nicotinamide riboside and nicotinamide mononucleotide, appear to increase more directly and effectively NAD+ with the potential to provide more potent enzymatic antiaging effects, according to Dr. DeWitt. Not all of the more than 90 active and recruiting trials listed for these compounds on clinicaltrials.gov relate to aging, but many do list this or a related condition, such as frailty or sarcopenia, as the therapeutic target.
The trials are being conducted even as OTC nicotinamide riboside and nicotinamide mononucleotide products are being promoted with terms such as “antiaging DNA repair” and “sirtuins activator.” Dr. DeWitt said that favorable reviews of these products on Internet forums are leading many patients to ask her specifically about their clinical value.
“Patients are starting to look at aging and longevity as an entity to manage and to treat,” Dr. DeWitt explained. Increasingly, patients bring up terms like autophagy and ask about the science behind antiaging products.
The clinical role of nicotinamide-related products, whether to reduce events related to aging or provide other benefits, remains unproven.
Nevertheless, Dr. DeWitt often offers nicotinamide to her patients for such indications as acne and atopic dermatitis. In patients with bullous pemphigoid, nicotinamide is an adjunct to other therapies “in most of my patients.”
When recommending nicotinamide, Dr. DeWitt specifies a brand, not because there is evidence that one brand is better than another but because of a reputation of quality control with branded OTC products.
In general, nicotinamide, which is not generally associated with the flushing that accompanies niacin, is well tolerated. She recommends 500 mg twice daily for most indications.
Dr. DeWitt advised reviewing published studies on nicotinamide in order to respond appropriately to patient inquiries. She noted that many patients come to the clinician’s office already aware of the science behind the potential role of NAD+ to inhibit aging and will be seeking an objective point of view.
Dr. DeWitt reports no conflicts of interest.
NEW YORK – More patients are inquiring about the antiaging claims made for nicotinamide products, according to Christine DeWitt MD, of the department of dermatology, Georgetown University, Washington. She encouraged attendees at the American Academy of Dermatology summer meeting to gain familiarity with the underlying mechanisms and potential uses of nicotinamide for aging skin and prevention of skin cancer as well as for a variety of dermatologic disorders, including atopic dermatitis and bullous pemphigoid.
The ability of nicotinamide to increase oxidized nicotinamide adenine dinucleotide (NAD+) is credited for most of its dermatologic benefits, according to Dr. DeWitt. She explained that NAD+ has a central role in cell metabolism, including serving as a substrate for sirtuins, which help prevent deterioration of telomeres, now thought to be a critical event in aging.
Downstream effects include an improved barrier function to reduce transdermal water loss in patients with atopic dermatitis and anti-inflammatory effects that are relevant to acne and bullous pemphigoid.
The related but unique forms of vitamin B3, nicotinamide riboside and nicotinamide mononucleotide, appear to increase more directly and effectively NAD+ with the potential to provide more potent enzymatic antiaging effects, according to Dr. DeWitt. Not all of the more than 90 active and recruiting trials listed for these compounds on clinicaltrials.gov relate to aging, but many do list this or a related condition, such as frailty or sarcopenia, as the therapeutic target.
The trials are being conducted even as OTC nicotinamide riboside and nicotinamide mononucleotide products are being promoted with terms such as “antiaging DNA repair” and “sirtuins activator.” Dr. DeWitt said that favorable reviews of these products on Internet forums are leading many patients to ask her specifically about their clinical value.
“Patients are starting to look at aging and longevity as an entity to manage and to treat,” Dr. DeWitt explained. Increasingly, patients bring up terms like autophagy and ask about the science behind antiaging products.
The clinical role of nicotinamide-related products, whether to reduce events related to aging or provide other benefits, remains unproven.
Nevertheless, Dr. DeWitt often offers nicotinamide to her patients for such indications as acne and atopic dermatitis. In patients with bullous pemphigoid, nicotinamide is an adjunct to other therapies “in most of my patients.”
When recommending nicotinamide, Dr. DeWitt specifies a brand, not because there is evidence that one brand is better than another but because of a reputation of quality control with branded OTC products.
In general, nicotinamide, which is not generally associated with the flushing that accompanies niacin, is well tolerated. She recommends 500 mg twice daily for most indications.
Dr. DeWitt advised reviewing published studies on nicotinamide in order to respond appropriately to patient inquiries. She noted that many patients come to the clinician’s office already aware of the science behind the potential role of NAD+ to inhibit aging and will be seeking an objective point of view.
Dr. DeWitt reports no conflicts of interest.
NEW YORK – More patients are inquiring about the antiaging claims made for nicotinamide products, according to Christine DeWitt MD, of the department of dermatology, Georgetown University, Washington. She encouraged attendees at the American Academy of Dermatology summer meeting to gain familiarity with the underlying mechanisms and potential uses of nicotinamide for aging skin and prevention of skin cancer as well as for a variety of dermatologic disorders, including atopic dermatitis and bullous pemphigoid.
The ability of nicotinamide to increase oxidized nicotinamide adenine dinucleotide (NAD+) is credited for most of its dermatologic benefits, according to Dr. DeWitt. She explained that NAD+ has a central role in cell metabolism, including serving as a substrate for sirtuins, which help prevent deterioration of telomeres, now thought to be a critical event in aging.
Downstream effects include an improved barrier function to reduce transdermal water loss in patients with atopic dermatitis and anti-inflammatory effects that are relevant to acne and bullous pemphigoid.
The related but unique forms of vitamin B3, nicotinamide riboside and nicotinamide mononucleotide, appear to increase more directly and effectively NAD+ with the potential to provide more potent enzymatic antiaging effects, according to Dr. DeWitt. Not all of the more than 90 active and recruiting trials listed for these compounds on clinicaltrials.gov relate to aging, but many do list this or a related condition, such as frailty or sarcopenia, as the therapeutic target.
The trials are being conducted even as OTC nicotinamide riboside and nicotinamide mononucleotide products are being promoted with terms such as “antiaging DNA repair” and “sirtuins activator.” Dr. DeWitt said that favorable reviews of these products on Internet forums are leading many patients to ask her specifically about their clinical value.
“Patients are starting to look at aging and longevity as an entity to manage and to treat,” Dr. DeWitt explained. Increasingly, patients bring up terms like autophagy and ask about the science behind antiaging products.
The clinical role of nicotinamide-related products, whether to reduce events related to aging or provide other benefits, remains unproven.
Nevertheless, Dr. DeWitt often offers nicotinamide to her patients for such indications as acne and atopic dermatitis. In patients with bullous pemphigoid, nicotinamide is an adjunct to other therapies “in most of my patients.”
When recommending nicotinamide, Dr. DeWitt specifies a brand, not because there is evidence that one brand is better than another but because of a reputation of quality control with branded OTC products.
In general, nicotinamide, which is not generally associated with the flushing that accompanies niacin, is well tolerated. She recommends 500 mg twice daily for most indications.
Dr. DeWitt advised reviewing published studies on nicotinamide in order to respond appropriately to patient inquiries. She noted that many patients come to the clinician’s office already aware of the science behind the potential role of NAD+ to inhibit aging and will be seeking an objective point of view.
Dr. DeWitt reports no conflicts of interest.
EXPERT ANALYSIS FROM SUMMER AAD 2019
Botulinum toxin injections: Err on the side of undercorrecting in first-time users
NEW YORK – In patients receiving first-time botulinum toxin injections for cosmetic enhancements, it is prudent to use a relatively low dose, Gary Goldenberg, MD, advised at the American Academy of Dermatology summer meeting.
Optimal dosing varies by individual, and undertreatment is easier to correct than is excess treatment. “This is a pearl. I always undercorrect, especially if I am injecting a patient for the first time,” said Dr. Goldenberg, an assistant clinical professor of dermatology and pathology at the Icahn School of Medicine at Mount Sinai, New York.
All patients are invited to return 2 weeks after their initial treatments, when the maximum effect is reached. Dr. Goldenberg does not charge for touch-ups administered at that time. “I want the patient to have the best possible experience,” he said.
The demand for botulinum toxin injections is skyrocketing, even among patients in their 20s. Also, men now represent a substantial proportion of those seeking cosmetic botulinum toxin injections.
Botulinum toxin injections are a source of high levels of patient satisfaction, according to Dr. Goldenberg. They are also a good way to get started in performing cosmetic procedures as skills in the injection of botulinum toxin are readily acquired, While some primary care physicians and gynecologists also are offering botulinum toxin injections for cosmetic purposes, dermatologists “are going to do a better job because we know the anatomy the best,” he said.
Dr. Goldenberg said botulinum toxin injections should be offered as a service in promotional efforts for one’s practice, but any mention to patients should be tactful. Patients should be informed that there are solutions for damaged or wrinkled skin, but the topic should be dropped if there is no apparent interest.
“I only suggest. I do not push,” he said. “I never talk about money. If they want to know how much (injections) will cost, they must speak to my office staff.”
With the recent approval of prabotulinumtoxinA (Jeuveau), there are four botulinum toxin injection products available in the United States. These include the original product, onabotulinumtoxinA (Botox), incobotulinumtoxinA (Xeomin), and abobotulinumtoxinA (Dysport). Dr. Goldenberg, who has administered them all, is not so far convinced there are important differences between them in regard to either efficacy or safety.
“There is another product now in clinical trials, so perhaps we will have a fifth product in a year or so,” said Dr. Goldenberg, who noted that the competition has resulted in claims and counterclaims regarding such issues as speed of onset and durability.
For dermatologists new to providing botulinum toxin injections, Dr. Goldenberg suggested restricting initial procedures to the face, particularly glabellar lines for which all of the available products are indicated. The companies that make these products also should offer a broad array of resources for improving skills, he said.
Dr. Goldenberg reports no potential conflicts of interest with companies that make botulinum toxins.
NEW YORK – In patients receiving first-time botulinum toxin injections for cosmetic enhancements, it is prudent to use a relatively low dose, Gary Goldenberg, MD, advised at the American Academy of Dermatology summer meeting.
Optimal dosing varies by individual, and undertreatment is easier to correct than is excess treatment. “This is a pearl. I always undercorrect, especially if I am injecting a patient for the first time,” said Dr. Goldenberg, an assistant clinical professor of dermatology and pathology at the Icahn School of Medicine at Mount Sinai, New York.
All patients are invited to return 2 weeks after their initial treatments, when the maximum effect is reached. Dr. Goldenberg does not charge for touch-ups administered at that time. “I want the patient to have the best possible experience,” he said.
The demand for botulinum toxin injections is skyrocketing, even among patients in their 20s. Also, men now represent a substantial proportion of those seeking cosmetic botulinum toxin injections.
Botulinum toxin injections are a source of high levels of patient satisfaction, according to Dr. Goldenberg. They are also a good way to get started in performing cosmetic procedures as skills in the injection of botulinum toxin are readily acquired, While some primary care physicians and gynecologists also are offering botulinum toxin injections for cosmetic purposes, dermatologists “are going to do a better job because we know the anatomy the best,” he said.
Dr. Goldenberg said botulinum toxin injections should be offered as a service in promotional efforts for one’s practice, but any mention to patients should be tactful. Patients should be informed that there are solutions for damaged or wrinkled skin, but the topic should be dropped if there is no apparent interest.
“I only suggest. I do not push,” he said. “I never talk about money. If they want to know how much (injections) will cost, they must speak to my office staff.”
With the recent approval of prabotulinumtoxinA (Jeuveau), there are four botulinum toxin injection products available in the United States. These include the original product, onabotulinumtoxinA (Botox), incobotulinumtoxinA (Xeomin), and abobotulinumtoxinA (Dysport). Dr. Goldenberg, who has administered them all, is not so far convinced there are important differences between them in regard to either efficacy or safety.
“There is another product now in clinical trials, so perhaps we will have a fifth product in a year or so,” said Dr. Goldenberg, who noted that the competition has resulted in claims and counterclaims regarding such issues as speed of onset and durability.
For dermatologists new to providing botulinum toxin injections, Dr. Goldenberg suggested restricting initial procedures to the face, particularly glabellar lines for which all of the available products are indicated. The companies that make these products also should offer a broad array of resources for improving skills, he said.
Dr. Goldenberg reports no potential conflicts of interest with companies that make botulinum toxins.
NEW YORK – In patients receiving first-time botulinum toxin injections for cosmetic enhancements, it is prudent to use a relatively low dose, Gary Goldenberg, MD, advised at the American Academy of Dermatology summer meeting.
Optimal dosing varies by individual, and undertreatment is easier to correct than is excess treatment. “This is a pearl. I always undercorrect, especially if I am injecting a patient for the first time,” said Dr. Goldenberg, an assistant clinical professor of dermatology and pathology at the Icahn School of Medicine at Mount Sinai, New York.
All patients are invited to return 2 weeks after their initial treatments, when the maximum effect is reached. Dr. Goldenberg does not charge for touch-ups administered at that time. “I want the patient to have the best possible experience,” he said.
The demand for botulinum toxin injections is skyrocketing, even among patients in their 20s. Also, men now represent a substantial proportion of those seeking cosmetic botulinum toxin injections.
Botulinum toxin injections are a source of high levels of patient satisfaction, according to Dr. Goldenberg. They are also a good way to get started in performing cosmetic procedures as skills in the injection of botulinum toxin are readily acquired, While some primary care physicians and gynecologists also are offering botulinum toxin injections for cosmetic purposes, dermatologists “are going to do a better job because we know the anatomy the best,” he said.
Dr. Goldenberg said botulinum toxin injections should be offered as a service in promotional efforts for one’s practice, but any mention to patients should be tactful. Patients should be informed that there are solutions for damaged or wrinkled skin, but the topic should be dropped if there is no apparent interest.
“I only suggest. I do not push,” he said. “I never talk about money. If they want to know how much (injections) will cost, they must speak to my office staff.”
With the recent approval of prabotulinumtoxinA (Jeuveau), there are four botulinum toxin injection products available in the United States. These include the original product, onabotulinumtoxinA (Botox), incobotulinumtoxinA (Xeomin), and abobotulinumtoxinA (Dysport). Dr. Goldenberg, who has administered them all, is not so far convinced there are important differences between them in regard to either efficacy or safety.
“There is another product now in clinical trials, so perhaps we will have a fifth product in a year or so,” said Dr. Goldenberg, who noted that the competition has resulted in claims and counterclaims regarding such issues as speed of onset and durability.
For dermatologists new to providing botulinum toxin injections, Dr. Goldenberg suggested restricting initial procedures to the face, particularly glabellar lines for which all of the available products are indicated. The companies that make these products also should offer a broad array of resources for improving skills, he said.
Dr. Goldenberg reports no potential conflicts of interest with companies that make botulinum toxins.
EXPERT ANALYSIS FROM SUMMER AAD 2019
Beyond sunscreen: Skin cancer preventive agents finding a role
NEW YORK – (KCs) that deserves to be considered for selective use in at-risk patients, according to an update at the American Academy of Dermatology summer meeting.
In providing her perspective on the available options, Rebecca Hartman, MD, MPH, director of melanoma epidemiology at Brigham and Women’s Hospital, Boston, emphasized that the therapies are not interchangeable but deserve to be used selectively according to their relative protection and relative risks.
Of oral agents, she characterized two, nicotinamide and acitretin, as “clinic-ready.” Acitretin is “an oldie but goodie,” but there is an important issue of tolerability. In the published studies, 15%-39% of patients withdrew because of adverse events, according to Dr. Hartman, which suggests the need for a motivated patient.
In addition, acitretin can be esterified into etretinate, a teratogen that can persist as long as 3 years after the drug is discontinued, making this drug contraindicated in women of childbearing potential, she noted.
However, most patients in need of prophylaxis for KCs are older, so teratogenicity is not an issue. In her practice, she offers acitretin to patients who are developing three or more KCs per year, as well as in situations of extensive skin damage in which a course of acitretin might provide some degree of clearing.
“When you are faced with the potential of a large number of biopsies, you could start acitretin to see if lesions can be reduced,” Dr. Hartman said .
Prevention of KCs became somewhat more attractive as a routine practice following publication of a phase 3 trial with nicotinamide. In this study, nicotinamide, an over-the-counter water-soluble form of vitamin B3, was associated with significantly reduced nonmelanoma skin cancers, including KCs and actinic keratoses, relative to placebo (N Engl J Med. 2015 Oct 22;373[17]:1618-26). Importantly, there was no greater risk of adverse events relative to placebo.
When assessed individually, the relative reduction in squamous cell carcinomas (SCCs; P = .05) and basal cell carcinomas (P = .12) fell short of statistical significance, but there was a highly significant 13% reduction in actinic keratoses after 12 months (P less than .001). An increase in SCCs was observed after therapy was stopped, which led Dr. Hartman to conclude that nicotinamide must be used on a “use-it-or-lose-it” basis. However, she does routinely offer this option.
“When do I recommend nicotinamide? Any patient with multiple actinic keratoses who wants to get ahead of the game and wants something that is relative safe,” Dr. Hartman explained. She uses the same dosing employed in the study, which was 500 mg twice daily.
There are other options for chemoprevention of KCs, but they are less attractive.
For example, capecitabine is effective, but tolerability is an even greater issue with this agent than it is for acitretin. According to Dr. Hartman, “we use this therapy very rarely and only in select cases.” As an alternative to the 14 days on and 7 days off schedule used for treatment of cancer, capecitabine is sometimes better tolerated in a 7 day on and 7 day off schedule, she said.
Topical 5-fluorouracil with or without calcipotriol is another chemoprevention option for those who can tolerate a skin reaction that lasts several days, Dr. Hartman said. She cited one study that associated this therapy with a nearly 80% reduction in face and scalp SCC.
Ultimately, she offers 5-fluorouracil with or without calcipotriol to “patients who want an evidence-based chemoprevention,” but she indicated that patients must be motivated to endure the adverse effects.
Many remain unaware of the array of options for chemoprevention of KCs, but Dr. Hartman emphasized that this is an area of active research with new options expected.
“I am really excited about the future direction of chemoprevention in skin cancer,” said Dr. Hartman, citing ongoing work to develop vitamin A, polypodium leucotomas extract, and human papillomavirus vaccine as options.
“If we can stop skin cancer in the first place, avoiding the morbidity and mortality of treatment, we will also hopefully save costs as well,” she commented. So far, essentially all of the strategies for chemoprevention, other than sunscreen, involve KCs, which leaves a large unmet need for better ways to prevent melanoma. However, Dr. Hartman noted that KCs represent the most common type of cancer of any type.
Just days after Dr. Hartman spoke at the meeting, a prospective study of vitamin A that found an inverse association between vitamin A intake and cutaneous SCC risk was, in fact, published in JAMA Dermatology (2019 Jul 31. doi: 10.1001/jamadermatol.2019.1937).
Dr. Hartman reported no financial relationships relevant to her presentation.
NEW YORK – (KCs) that deserves to be considered for selective use in at-risk patients, according to an update at the American Academy of Dermatology summer meeting.
In providing her perspective on the available options, Rebecca Hartman, MD, MPH, director of melanoma epidemiology at Brigham and Women’s Hospital, Boston, emphasized that the therapies are not interchangeable but deserve to be used selectively according to their relative protection and relative risks.
Of oral agents, she characterized two, nicotinamide and acitretin, as “clinic-ready.” Acitretin is “an oldie but goodie,” but there is an important issue of tolerability. In the published studies, 15%-39% of patients withdrew because of adverse events, according to Dr. Hartman, which suggests the need for a motivated patient.
In addition, acitretin can be esterified into etretinate, a teratogen that can persist as long as 3 years after the drug is discontinued, making this drug contraindicated in women of childbearing potential, she noted.
However, most patients in need of prophylaxis for KCs are older, so teratogenicity is not an issue. In her practice, she offers acitretin to patients who are developing three or more KCs per year, as well as in situations of extensive skin damage in which a course of acitretin might provide some degree of clearing.
“When you are faced with the potential of a large number of biopsies, you could start acitretin to see if lesions can be reduced,” Dr. Hartman said .
Prevention of KCs became somewhat more attractive as a routine practice following publication of a phase 3 trial with nicotinamide. In this study, nicotinamide, an over-the-counter water-soluble form of vitamin B3, was associated with significantly reduced nonmelanoma skin cancers, including KCs and actinic keratoses, relative to placebo (N Engl J Med. 2015 Oct 22;373[17]:1618-26). Importantly, there was no greater risk of adverse events relative to placebo.
When assessed individually, the relative reduction in squamous cell carcinomas (SCCs; P = .05) and basal cell carcinomas (P = .12) fell short of statistical significance, but there was a highly significant 13% reduction in actinic keratoses after 12 months (P less than .001). An increase in SCCs was observed after therapy was stopped, which led Dr. Hartman to conclude that nicotinamide must be used on a “use-it-or-lose-it” basis. However, she does routinely offer this option.
“When do I recommend nicotinamide? Any patient with multiple actinic keratoses who wants to get ahead of the game and wants something that is relative safe,” Dr. Hartman explained. She uses the same dosing employed in the study, which was 500 mg twice daily.
There are other options for chemoprevention of KCs, but they are less attractive.
For example, capecitabine is effective, but tolerability is an even greater issue with this agent than it is for acitretin. According to Dr. Hartman, “we use this therapy very rarely and only in select cases.” As an alternative to the 14 days on and 7 days off schedule used for treatment of cancer, capecitabine is sometimes better tolerated in a 7 day on and 7 day off schedule, she said.
Topical 5-fluorouracil with or without calcipotriol is another chemoprevention option for those who can tolerate a skin reaction that lasts several days, Dr. Hartman said. She cited one study that associated this therapy with a nearly 80% reduction in face and scalp SCC.
Ultimately, she offers 5-fluorouracil with or without calcipotriol to “patients who want an evidence-based chemoprevention,” but she indicated that patients must be motivated to endure the adverse effects.
Many remain unaware of the array of options for chemoprevention of KCs, but Dr. Hartman emphasized that this is an area of active research with new options expected.
“I am really excited about the future direction of chemoprevention in skin cancer,” said Dr. Hartman, citing ongoing work to develop vitamin A, polypodium leucotomas extract, and human papillomavirus vaccine as options.
“If we can stop skin cancer in the first place, avoiding the morbidity and mortality of treatment, we will also hopefully save costs as well,” she commented. So far, essentially all of the strategies for chemoprevention, other than sunscreen, involve KCs, which leaves a large unmet need for better ways to prevent melanoma. However, Dr. Hartman noted that KCs represent the most common type of cancer of any type.
Just days after Dr. Hartman spoke at the meeting, a prospective study of vitamin A that found an inverse association between vitamin A intake and cutaneous SCC risk was, in fact, published in JAMA Dermatology (2019 Jul 31. doi: 10.1001/jamadermatol.2019.1937).
Dr. Hartman reported no financial relationships relevant to her presentation.
NEW YORK – (KCs) that deserves to be considered for selective use in at-risk patients, according to an update at the American Academy of Dermatology summer meeting.
In providing her perspective on the available options, Rebecca Hartman, MD, MPH, director of melanoma epidemiology at Brigham and Women’s Hospital, Boston, emphasized that the therapies are not interchangeable but deserve to be used selectively according to their relative protection and relative risks.
Of oral agents, she characterized two, nicotinamide and acitretin, as “clinic-ready.” Acitretin is “an oldie but goodie,” but there is an important issue of tolerability. In the published studies, 15%-39% of patients withdrew because of adverse events, according to Dr. Hartman, which suggests the need for a motivated patient.
In addition, acitretin can be esterified into etretinate, a teratogen that can persist as long as 3 years after the drug is discontinued, making this drug contraindicated in women of childbearing potential, she noted.
However, most patients in need of prophylaxis for KCs are older, so teratogenicity is not an issue. In her practice, she offers acitretin to patients who are developing three or more KCs per year, as well as in situations of extensive skin damage in which a course of acitretin might provide some degree of clearing.
“When you are faced with the potential of a large number of biopsies, you could start acitretin to see if lesions can be reduced,” Dr. Hartman said .
Prevention of KCs became somewhat more attractive as a routine practice following publication of a phase 3 trial with nicotinamide. In this study, nicotinamide, an over-the-counter water-soluble form of vitamin B3, was associated with significantly reduced nonmelanoma skin cancers, including KCs and actinic keratoses, relative to placebo (N Engl J Med. 2015 Oct 22;373[17]:1618-26). Importantly, there was no greater risk of adverse events relative to placebo.
When assessed individually, the relative reduction in squamous cell carcinomas (SCCs; P = .05) and basal cell carcinomas (P = .12) fell short of statistical significance, but there was a highly significant 13% reduction in actinic keratoses after 12 months (P less than .001). An increase in SCCs was observed after therapy was stopped, which led Dr. Hartman to conclude that nicotinamide must be used on a “use-it-or-lose-it” basis. However, she does routinely offer this option.
“When do I recommend nicotinamide? Any patient with multiple actinic keratoses who wants to get ahead of the game and wants something that is relative safe,” Dr. Hartman explained. She uses the same dosing employed in the study, which was 500 mg twice daily.
There are other options for chemoprevention of KCs, but they are less attractive.
For example, capecitabine is effective, but tolerability is an even greater issue with this agent than it is for acitretin. According to Dr. Hartman, “we use this therapy very rarely and only in select cases.” As an alternative to the 14 days on and 7 days off schedule used for treatment of cancer, capecitabine is sometimes better tolerated in a 7 day on and 7 day off schedule, she said.
Topical 5-fluorouracil with or without calcipotriol is another chemoprevention option for those who can tolerate a skin reaction that lasts several days, Dr. Hartman said. She cited one study that associated this therapy with a nearly 80% reduction in face and scalp SCC.
Ultimately, she offers 5-fluorouracil with or without calcipotriol to “patients who want an evidence-based chemoprevention,” but she indicated that patients must be motivated to endure the adverse effects.
Many remain unaware of the array of options for chemoprevention of KCs, but Dr. Hartman emphasized that this is an area of active research with new options expected.
“I am really excited about the future direction of chemoprevention in skin cancer,” said Dr. Hartman, citing ongoing work to develop vitamin A, polypodium leucotomas extract, and human papillomavirus vaccine as options.
“If we can stop skin cancer in the first place, avoiding the morbidity and mortality of treatment, we will also hopefully save costs as well,” she commented. So far, essentially all of the strategies for chemoprevention, other than sunscreen, involve KCs, which leaves a large unmet need for better ways to prevent melanoma. However, Dr. Hartman noted that KCs represent the most common type of cancer of any type.
Just days after Dr. Hartman spoke at the meeting, a prospective study of vitamin A that found an inverse association between vitamin A intake and cutaneous SCC risk was, in fact, published in JAMA Dermatology (2019 Jul 31. doi: 10.1001/jamadermatol.2019.1937).
Dr. Hartman reported no financial relationships relevant to her presentation.
EXPERT ANALYSIS FROM SUMMER AAD 2019
Clues to eczematous cheilitis may lie in the history
NEW YORK – , but patients may be slow to seek help, Bethanee Schlosser, MD, PhD, said at the American Academy of Dermatology summer meeting.
One of the challenges in helping patients with lip problems is that lips are constantly in motion and constantly interacting with the outside world, said Dr. Schlosser, of the department of dermatology, Northwestern University, Chicago. There’s ongoing low-level trauma with phonation, eating, drinking, and general environmental exposure, she said. Eczematous cheilitis will present with scaling and erythema of the vermilion lips, with lower lip involvement often more pronounced than symptoms on the upper lip. Fissuring and erosion are sometimes, but not always, present as well.
In addition to flaking and redness, Dr. Schlosser noted that patients will complain of dry lips, irritation, itching, and sometimes tingling.
Sorting out the etiology of eczematous cheilitis requires a thorough history. “Ask about habits, such as lip licking, picking, or biting,” she said. Recent dental work, braces, or other appliances for alignment or temporomandibular joint problems can introduce both mechanical irritation and potential allergens, and even musical instruments can be culprits, such as when an oboe reed causes an allergic reaction.
Personal hygiene products, cosmetics, gum chewing, and candy consumption can be the irritant culprits, noted Dr. Schlosser. Careful questioning of patients and examination of the products used can provide clues, since dyes and pigments in cosmetics and gum may provoke reactions.
History taking should also include questions about tobacco in all forms, marijuana, and prescription medication, which can cause lip problems. And it’s important to ask about skin disease in general, to determine if symptoms are present in other anatomic locations, and to ask about any family history of skin disease, she said.
Endogenous contributors can include true atopic dermatitis, psoriasis, and nutritional deficiencies. Psoriatic cheilitis can have prominent crusting and exfoliation. In a Brazilian study that evaluated patents with cutaneous psoriasis and age-, race-, and sex-matched controls with no history of skin disease, psoriasis was associated with geographic tongue, with an odds ratio of 5.0 (95% CI 1.5-16.8). Geographic stomatitis can also be seen, said Dr. Schlosser. Tongue fissures were also more common among those with psoriasis cheilitis (OR 2.7, 95% confidence interval, 1.3-5.6) in the same study (Med Oral Patol Oral Cir Bucal. 2009 Aug 1;14[8]:e371-5).
For psoriatic cheilitis, looking beyond the lips can help refine the diagnosis, she noted. There may be intra-oral signs or signs of extra-oral involvement, especially on the scalp, ears, and genitalia. Koebnerization may be difficult to detect on the lips, but may be present elsewhere. A family history of psoriasis may also tip the scales toward this diagnosis.
Exogenous causes of eczematous cheilitis are much more common and can include contact with irritants and allergens, factitial cheilitis, and cheilitis medicamentosa, Dr Schlosser pointed out.
Allergic contact dermatitis can come from local exposure (to cosmetics and other personal care items, for example) or from incidental exposures. Components of saliva can become concentrated when saliva dries outside the oral cavity, so for chronic lip lickers, saliva alone can be sufficiently irritating to provoke a cheilitis, Dr. Schlosser said.
Transfer of an irritant or allergen is also possible from other body sites, as when a nail-chewer develops allergic cheilitis from an ingredient in nail polish. Transfer from products used on other facial areas and the hair is also possible, as is “connubial transfer,” when an allergen is transferred from an intimate partner.
Cutaneous patch tests can be helpful in pinpointing the offending agent, or agents, according to Dr. Schlosser. She cited a study of 91 patients (77% of whom were female) who underwent patch testing for eczematous cheilitis. The researchers determined that 45% of patients had allergic contact cheilitis (Int J Dermatol. 2016 Jul;55[7]:e386-91).
The patch testing revealed that fragrances, balsam of Peru (Myroxylon pereirae resin), preservatives, and even metals such as nickel and gold were common allergens. The findings echo those in another database review that showed fragrances, M. pereirae, and nickel as the top three allergens on patch testing for lip cheilitis.
Dr. Schlosser said that the most common offending sources are lipsticks, makeup, other cosmetic products, and moisturizer, which are responsible for 10% or more of reactions.
Whatever the etiology, the treatment of eczematous cheilitis can be divided conceptually into two phases. During the induction phase, use of a low- to mid-potency topical corticosteroid ointment quiets inflammation. Examples include alclometasone 0.05%, desonide 0.05%, fluticasone 0.005%, or triamcinolone 0.1%. “Ointment formulations are preferred,” said Dr. Schlosser, since they won’t dissolve so easily with lip licking and will adhere well to the surface of the vermilion lip.
Next, a topical calcineurin inhibitor such as tacrolimus 0.1% can be used for maintenance. Other topical medications, especially topical anesthetics, should be used with caution, she said.
For psoriatic cheilitis, induction with 5% salicylic acid ointment can be followed by the topical calcineurin inhibitor phase, said Dr. Schlosser.
Dr. Schlosser disclosed financial relationships with Beiersdorf, Decision Support in Medicine, and UpToDate.
koakes@mdedge.com
NEW YORK – , but patients may be slow to seek help, Bethanee Schlosser, MD, PhD, said at the American Academy of Dermatology summer meeting.
One of the challenges in helping patients with lip problems is that lips are constantly in motion and constantly interacting with the outside world, said Dr. Schlosser, of the department of dermatology, Northwestern University, Chicago. There’s ongoing low-level trauma with phonation, eating, drinking, and general environmental exposure, she said. Eczematous cheilitis will present with scaling and erythema of the vermilion lips, with lower lip involvement often more pronounced than symptoms on the upper lip. Fissuring and erosion are sometimes, but not always, present as well.
In addition to flaking and redness, Dr. Schlosser noted that patients will complain of dry lips, irritation, itching, and sometimes tingling.
Sorting out the etiology of eczematous cheilitis requires a thorough history. “Ask about habits, such as lip licking, picking, or biting,” she said. Recent dental work, braces, or other appliances for alignment or temporomandibular joint problems can introduce both mechanical irritation and potential allergens, and even musical instruments can be culprits, such as when an oboe reed causes an allergic reaction.
Personal hygiene products, cosmetics, gum chewing, and candy consumption can be the irritant culprits, noted Dr. Schlosser. Careful questioning of patients and examination of the products used can provide clues, since dyes and pigments in cosmetics and gum may provoke reactions.
History taking should also include questions about tobacco in all forms, marijuana, and prescription medication, which can cause lip problems. And it’s important to ask about skin disease in general, to determine if symptoms are present in other anatomic locations, and to ask about any family history of skin disease, she said.
Endogenous contributors can include true atopic dermatitis, psoriasis, and nutritional deficiencies. Psoriatic cheilitis can have prominent crusting and exfoliation. In a Brazilian study that evaluated patents with cutaneous psoriasis and age-, race-, and sex-matched controls with no history of skin disease, psoriasis was associated with geographic tongue, with an odds ratio of 5.0 (95% CI 1.5-16.8). Geographic stomatitis can also be seen, said Dr. Schlosser. Tongue fissures were also more common among those with psoriasis cheilitis (OR 2.7, 95% confidence interval, 1.3-5.6) in the same study (Med Oral Patol Oral Cir Bucal. 2009 Aug 1;14[8]:e371-5).
For psoriatic cheilitis, looking beyond the lips can help refine the diagnosis, she noted. There may be intra-oral signs or signs of extra-oral involvement, especially on the scalp, ears, and genitalia. Koebnerization may be difficult to detect on the lips, but may be present elsewhere. A family history of psoriasis may also tip the scales toward this diagnosis.
Exogenous causes of eczematous cheilitis are much more common and can include contact with irritants and allergens, factitial cheilitis, and cheilitis medicamentosa, Dr Schlosser pointed out.
Allergic contact dermatitis can come from local exposure (to cosmetics and other personal care items, for example) or from incidental exposures. Components of saliva can become concentrated when saliva dries outside the oral cavity, so for chronic lip lickers, saliva alone can be sufficiently irritating to provoke a cheilitis, Dr. Schlosser said.
Transfer of an irritant or allergen is also possible from other body sites, as when a nail-chewer develops allergic cheilitis from an ingredient in nail polish. Transfer from products used on other facial areas and the hair is also possible, as is “connubial transfer,” when an allergen is transferred from an intimate partner.
Cutaneous patch tests can be helpful in pinpointing the offending agent, or agents, according to Dr. Schlosser. She cited a study of 91 patients (77% of whom were female) who underwent patch testing for eczematous cheilitis. The researchers determined that 45% of patients had allergic contact cheilitis (Int J Dermatol. 2016 Jul;55[7]:e386-91).
The patch testing revealed that fragrances, balsam of Peru (Myroxylon pereirae resin), preservatives, and even metals such as nickel and gold were common allergens. The findings echo those in another database review that showed fragrances, M. pereirae, and nickel as the top three allergens on patch testing for lip cheilitis.
Dr. Schlosser said that the most common offending sources are lipsticks, makeup, other cosmetic products, and moisturizer, which are responsible for 10% or more of reactions.
Whatever the etiology, the treatment of eczematous cheilitis can be divided conceptually into two phases. During the induction phase, use of a low- to mid-potency topical corticosteroid ointment quiets inflammation. Examples include alclometasone 0.05%, desonide 0.05%, fluticasone 0.005%, or triamcinolone 0.1%. “Ointment formulations are preferred,” said Dr. Schlosser, since they won’t dissolve so easily with lip licking and will adhere well to the surface of the vermilion lip.
Next, a topical calcineurin inhibitor such as tacrolimus 0.1% can be used for maintenance. Other topical medications, especially topical anesthetics, should be used with caution, she said.
For psoriatic cheilitis, induction with 5% salicylic acid ointment can be followed by the topical calcineurin inhibitor phase, said Dr. Schlosser.
Dr. Schlosser disclosed financial relationships with Beiersdorf, Decision Support in Medicine, and UpToDate.
koakes@mdedge.com
NEW YORK – , but patients may be slow to seek help, Bethanee Schlosser, MD, PhD, said at the American Academy of Dermatology summer meeting.
One of the challenges in helping patients with lip problems is that lips are constantly in motion and constantly interacting with the outside world, said Dr. Schlosser, of the department of dermatology, Northwestern University, Chicago. There’s ongoing low-level trauma with phonation, eating, drinking, and general environmental exposure, she said. Eczematous cheilitis will present with scaling and erythema of the vermilion lips, with lower lip involvement often more pronounced than symptoms on the upper lip. Fissuring and erosion are sometimes, but not always, present as well.
In addition to flaking and redness, Dr. Schlosser noted that patients will complain of dry lips, irritation, itching, and sometimes tingling.
Sorting out the etiology of eczematous cheilitis requires a thorough history. “Ask about habits, such as lip licking, picking, or biting,” she said. Recent dental work, braces, or other appliances for alignment or temporomandibular joint problems can introduce both mechanical irritation and potential allergens, and even musical instruments can be culprits, such as when an oboe reed causes an allergic reaction.
Personal hygiene products, cosmetics, gum chewing, and candy consumption can be the irritant culprits, noted Dr. Schlosser. Careful questioning of patients and examination of the products used can provide clues, since dyes and pigments in cosmetics and gum may provoke reactions.
History taking should also include questions about tobacco in all forms, marijuana, and prescription medication, which can cause lip problems. And it’s important to ask about skin disease in general, to determine if symptoms are present in other anatomic locations, and to ask about any family history of skin disease, she said.
Endogenous contributors can include true atopic dermatitis, psoriasis, and nutritional deficiencies. Psoriatic cheilitis can have prominent crusting and exfoliation. In a Brazilian study that evaluated patents with cutaneous psoriasis and age-, race-, and sex-matched controls with no history of skin disease, psoriasis was associated with geographic tongue, with an odds ratio of 5.0 (95% CI 1.5-16.8). Geographic stomatitis can also be seen, said Dr. Schlosser. Tongue fissures were also more common among those with psoriasis cheilitis (OR 2.7, 95% confidence interval, 1.3-5.6) in the same study (Med Oral Patol Oral Cir Bucal. 2009 Aug 1;14[8]:e371-5).
For psoriatic cheilitis, looking beyond the lips can help refine the diagnosis, she noted. There may be intra-oral signs or signs of extra-oral involvement, especially on the scalp, ears, and genitalia. Koebnerization may be difficult to detect on the lips, but may be present elsewhere. A family history of psoriasis may also tip the scales toward this diagnosis.
Exogenous causes of eczematous cheilitis are much more common and can include contact with irritants and allergens, factitial cheilitis, and cheilitis medicamentosa, Dr Schlosser pointed out.
Allergic contact dermatitis can come from local exposure (to cosmetics and other personal care items, for example) or from incidental exposures. Components of saliva can become concentrated when saliva dries outside the oral cavity, so for chronic lip lickers, saliva alone can be sufficiently irritating to provoke a cheilitis, Dr. Schlosser said.
Transfer of an irritant or allergen is also possible from other body sites, as when a nail-chewer develops allergic cheilitis from an ingredient in nail polish. Transfer from products used on other facial areas and the hair is also possible, as is “connubial transfer,” when an allergen is transferred from an intimate partner.
Cutaneous patch tests can be helpful in pinpointing the offending agent, or agents, according to Dr. Schlosser. She cited a study of 91 patients (77% of whom were female) who underwent patch testing for eczematous cheilitis. The researchers determined that 45% of patients had allergic contact cheilitis (Int J Dermatol. 2016 Jul;55[7]:e386-91).
The patch testing revealed that fragrances, balsam of Peru (Myroxylon pereirae resin), preservatives, and even metals such as nickel and gold were common allergens. The findings echo those in another database review that showed fragrances, M. pereirae, and nickel as the top three allergens on patch testing for lip cheilitis.
Dr. Schlosser said that the most common offending sources are lipsticks, makeup, other cosmetic products, and moisturizer, which are responsible for 10% or more of reactions.
Whatever the etiology, the treatment of eczematous cheilitis can be divided conceptually into two phases. During the induction phase, use of a low- to mid-potency topical corticosteroid ointment quiets inflammation. Examples include alclometasone 0.05%, desonide 0.05%, fluticasone 0.005%, or triamcinolone 0.1%. “Ointment formulations are preferred,” said Dr. Schlosser, since they won’t dissolve so easily with lip licking and will adhere well to the surface of the vermilion lip.
Next, a topical calcineurin inhibitor such as tacrolimus 0.1% can be used for maintenance. Other topical medications, especially topical anesthetics, should be used with caution, she said.
For psoriatic cheilitis, induction with 5% salicylic acid ointment can be followed by the topical calcineurin inhibitor phase, said Dr. Schlosser.
Dr. Schlosser disclosed financial relationships with Beiersdorf, Decision Support in Medicine, and UpToDate.
koakes@mdedge.com
EXPERT ANALYSIS FROM SUMMER AAD 2019
What’s the best way to sort out red nail discoloration?
NEW YORK – Nail discoloration, in all its variety, has a wide differential. And while that differential narrows when a patient presents with concerns about nails with red discoloration, there’s still a long list of diagnoses to consider.
During a nail-focused session at the American Academy of Dermatology summer meeting, Shari Lipner, MD, PhD, took attendees through a presentation-based approach that gets to the root etiology of erythronychia and guides diagnosis and treatment options.
“However, regardless of the etiology, erythronychia shares a common pathogenesis,” said Dr. Lipner, a dermatologist at New York–Presbyterian Hospital and Weil Cornell Medicine. The process begins in the distal nail matrix, resulting in a thin long strip of ventral nail becoming discolored, with the nail bed filling in the concavity. The engorged nail bed also makes the affected nail unit prone to splinter hemorrhages, and the thinned, transparent nail makes the erythema more visible, she explained.
Polydactylous longitudinal erythronychia
For erythronychia affecting several nails, onychotillomania is among the possible causes. This condition “often goes hand in hand with onychophagia,” and trichotillomania, skin-picking, or other self-mutilating disorders may also be present, she said. In both the adult and pediatric population, onychotillomania can accompany psychiatric disorders, including depression and obsessive-compulsive disorder, and may be associated with suicidal ideation, she added.
When onychotillomania is the cause, erythronychia may be accompanied by paronychia, and patients will often have a shortened nail bed and an atrophic nail plate. Dorsal pterygium may also be present.
Dermoscopy can provide some clues that onychotillomania is the culprit, said Dr. Lipner, citing a study that looked at dermoscopic images of 36 cases, which found scales in 94%, absence of the nail plate in 83%, and characteristic wavy lines in 69% (J Am Acad Dermatol. 2018 Oct;79[4]:702-5). Other frequent dermoscopy findings included hemorrhages (64%), crusts (61%), nail bed pigmentation (47%), and speckled dots (39%).
Lichen planus can also affect the nails, with erythronychia among its manifestations, she noted. Though lichen planus is thought of as a disease of middle or older age, usually affecting those aged 50-70 years, “15% of those affected are less than 20 years old,” she said.
The erythronychia of lichen planus is often accompanied by longitudinal riding, splitting, and atrophy of the nail plate, she said. Pterygium can also be present, representing a scar in the nail matrix. Dermatopathology will reveal a patchy, bandlike lichenoid infiltrate, with variable sawtooth hypergranulosis and hyperplasia.
“There’s not much evidence about how to treat lichen planus of the nails,” noted Dr. Lipner. Options can include intralesional corticosteroid injections at the nail matrix, topical corticosteroids, oral methotrexate, and retinoids.
Darier disease, an inherited condition caused by mutations in ATP2A2, has both skin and nail manifestations. Characteristic skin signs include hyperkeratotic papules, cobblestone papules, and palmar pits, she said. When nails are affected – as they are in up to 95% of Darier disease patients – they can have a characteristic “candy cane” appearance, with bands of longitudinal erythronychia alternating with normal-colored nail. The nails can also have V-shaped notching, she added.
Patients with systemic lupus erythematosus can also have longitudinal erythronychia; here, dermoscopy will show the characteristic prominent capillary loops in the proximal nail folds, she said.
Foreign substances such as nail polish and dyes, when they’re the source of erythronychia in one or several nails, can usually be wiped off with alcohol or acetone; also, “the proximal margin of discoloration will follow the same pattern as the nail fold,” said Dr. Lipner.
Localized longitudinal erythronychia
When the red discoloration is limited to a single nail, the differential shifts, said Dr. Lipner. With a hematoma, there’s often a history of trauma, and dermoscopy will show characteristic globules and streaks.
The first clue that erythronychia caused by onychopapilloma can be seen at the lunula: There will often be a comet- or pencil-shaped point to the discoloration in that region. But, she said, “the key is to do dermoscopy at the free edge of the nail plate. In 100 percent of cases, there will be a subungual hyperkeratotic papule” that will solidify the diagnosis.
Histopathology of onychopapillomas – a relatively recently recognized entity – will show nail bed and distal matrix acanthosis, with the distal nail bed showing matrix metaplasia, Dr. Lipner said.
Glomus tumors arise from cells of the glomus body, a specialized vascular apparatus that is involved in temperature regulation. “These structures are abundant in the digits and the subungual region,” said Dr. Lipner, which means that glomus tumors – a benign lesion – may develop subungually. Glomus tumors can be idiopathic, but she added, “think neurofibromatosis type 1 if you see multiple glomus tumors.”
Glomus tumors will present with longitudinal erythronychia, with a distal split of the nail sometimes accompanying the discoloration. A round bluish to gray nodule can also be seen. A thorough history and exam can help solidify the diagnosis, said Dr. Lipner; there’s a characteristic triad of point tenderness with the application of pressure to the nail, pain, and cold hypersensitivity.
Classically, the point tenderness is assessed by Love’s test, which elicits severe pain when the subungual tumor is pressed with a small object like the end of paper clip or a ballpoint pen. Application of a tourniquet to the arm after elevation, termed Hildreth’s test, should alleviate subungual glomus tumor pain, and release of the tourniquet causes an abrupt and marked recurrence of pain. Immersing the patient’s affected hand in cold water also increases glomus tumor pain.
“Imaging can be quite helpful” to confirm a glomus tumor diagnosis, said Dr. Lipner. “X-ray is cheap, and you can see erosions in 50% of patients.” However, she added, doppler ultrasound and magnetic resonance imaging are more sensitive, detecting tumors as small as 2 mm.
“Biopsy with histopathology is the gold standard in making the diagnosis” of glomus tumor, though, she noted. Pathologic examination will show monomorphic cells with small caliber vascular channels.
Malignancy is actually uncommon with erythronychia, though it’s always in the differential diagnosis, she said.
In one case series examining subungual squamous cell carcinomas, common findings included onycholysis and localized hyperkeratosis, along with longitudinal erythronychia. “This may be subtle; splinter hemorrhages can also be present,” noted Dr. Lipner, adding, “If there are any symptoms, or an evolving band, a biopsy is indicated.”
“Even with erythronychia, the presentation can be quite variable,” she said. Nail unit melanoma can count erythronychia among the presenting signs. Clues that should raise suspicion for melanoma can include a wide band and prominent onycholysis, especially distal onycholysis and splintering. Again, she said, “biopsy with histopathology is the gold standard in making the diagnosis”; any symptoms or evidence of an evolving band should trigger a biopsy.
Dr. Lipner had no conflicts of interest relevant to her presentation.
SOURCE: Lipner S. Summer AAD 2019, Presentation F035.
NEW YORK – Nail discoloration, in all its variety, has a wide differential. And while that differential narrows when a patient presents with concerns about nails with red discoloration, there’s still a long list of diagnoses to consider.
During a nail-focused session at the American Academy of Dermatology summer meeting, Shari Lipner, MD, PhD, took attendees through a presentation-based approach that gets to the root etiology of erythronychia and guides diagnosis and treatment options.
“However, regardless of the etiology, erythronychia shares a common pathogenesis,” said Dr. Lipner, a dermatologist at New York–Presbyterian Hospital and Weil Cornell Medicine. The process begins in the distal nail matrix, resulting in a thin long strip of ventral nail becoming discolored, with the nail bed filling in the concavity. The engorged nail bed also makes the affected nail unit prone to splinter hemorrhages, and the thinned, transparent nail makes the erythema more visible, she explained.
Polydactylous longitudinal erythronychia
For erythronychia affecting several nails, onychotillomania is among the possible causes. This condition “often goes hand in hand with onychophagia,” and trichotillomania, skin-picking, or other self-mutilating disorders may also be present, she said. In both the adult and pediatric population, onychotillomania can accompany psychiatric disorders, including depression and obsessive-compulsive disorder, and may be associated with suicidal ideation, she added.
When onychotillomania is the cause, erythronychia may be accompanied by paronychia, and patients will often have a shortened nail bed and an atrophic nail plate. Dorsal pterygium may also be present.
Dermoscopy can provide some clues that onychotillomania is the culprit, said Dr. Lipner, citing a study that looked at dermoscopic images of 36 cases, which found scales in 94%, absence of the nail plate in 83%, and characteristic wavy lines in 69% (J Am Acad Dermatol. 2018 Oct;79[4]:702-5). Other frequent dermoscopy findings included hemorrhages (64%), crusts (61%), nail bed pigmentation (47%), and speckled dots (39%).
Lichen planus can also affect the nails, with erythronychia among its manifestations, she noted. Though lichen planus is thought of as a disease of middle or older age, usually affecting those aged 50-70 years, “15% of those affected are less than 20 years old,” she said.
The erythronychia of lichen planus is often accompanied by longitudinal riding, splitting, and atrophy of the nail plate, she said. Pterygium can also be present, representing a scar in the nail matrix. Dermatopathology will reveal a patchy, bandlike lichenoid infiltrate, with variable sawtooth hypergranulosis and hyperplasia.
“There’s not much evidence about how to treat lichen planus of the nails,” noted Dr. Lipner. Options can include intralesional corticosteroid injections at the nail matrix, topical corticosteroids, oral methotrexate, and retinoids.
Darier disease, an inherited condition caused by mutations in ATP2A2, has both skin and nail manifestations. Characteristic skin signs include hyperkeratotic papules, cobblestone papules, and palmar pits, she said. When nails are affected – as they are in up to 95% of Darier disease patients – they can have a characteristic “candy cane” appearance, with bands of longitudinal erythronychia alternating with normal-colored nail. The nails can also have V-shaped notching, she added.
Patients with systemic lupus erythematosus can also have longitudinal erythronychia; here, dermoscopy will show the characteristic prominent capillary loops in the proximal nail folds, she said.
Foreign substances such as nail polish and dyes, when they’re the source of erythronychia in one or several nails, can usually be wiped off with alcohol or acetone; also, “the proximal margin of discoloration will follow the same pattern as the nail fold,” said Dr. Lipner.
Localized longitudinal erythronychia
When the red discoloration is limited to a single nail, the differential shifts, said Dr. Lipner. With a hematoma, there’s often a history of trauma, and dermoscopy will show characteristic globules and streaks.
The first clue that erythronychia caused by onychopapilloma can be seen at the lunula: There will often be a comet- or pencil-shaped point to the discoloration in that region. But, she said, “the key is to do dermoscopy at the free edge of the nail plate. In 100 percent of cases, there will be a subungual hyperkeratotic papule” that will solidify the diagnosis.
Histopathology of onychopapillomas – a relatively recently recognized entity – will show nail bed and distal matrix acanthosis, with the distal nail bed showing matrix metaplasia, Dr. Lipner said.
Glomus tumors arise from cells of the glomus body, a specialized vascular apparatus that is involved in temperature regulation. “These structures are abundant in the digits and the subungual region,” said Dr. Lipner, which means that glomus tumors – a benign lesion – may develop subungually. Glomus tumors can be idiopathic, but she added, “think neurofibromatosis type 1 if you see multiple glomus tumors.”
Glomus tumors will present with longitudinal erythronychia, with a distal split of the nail sometimes accompanying the discoloration. A round bluish to gray nodule can also be seen. A thorough history and exam can help solidify the diagnosis, said Dr. Lipner; there’s a characteristic triad of point tenderness with the application of pressure to the nail, pain, and cold hypersensitivity.
Classically, the point tenderness is assessed by Love’s test, which elicits severe pain when the subungual tumor is pressed with a small object like the end of paper clip or a ballpoint pen. Application of a tourniquet to the arm after elevation, termed Hildreth’s test, should alleviate subungual glomus tumor pain, and release of the tourniquet causes an abrupt and marked recurrence of pain. Immersing the patient’s affected hand in cold water also increases glomus tumor pain.
“Imaging can be quite helpful” to confirm a glomus tumor diagnosis, said Dr. Lipner. “X-ray is cheap, and you can see erosions in 50% of patients.” However, she added, doppler ultrasound and magnetic resonance imaging are more sensitive, detecting tumors as small as 2 mm.
“Biopsy with histopathology is the gold standard in making the diagnosis” of glomus tumor, though, she noted. Pathologic examination will show monomorphic cells with small caliber vascular channels.
Malignancy is actually uncommon with erythronychia, though it’s always in the differential diagnosis, she said.
In one case series examining subungual squamous cell carcinomas, common findings included onycholysis and localized hyperkeratosis, along with longitudinal erythronychia. “This may be subtle; splinter hemorrhages can also be present,” noted Dr. Lipner, adding, “If there are any symptoms, or an evolving band, a biopsy is indicated.”
“Even with erythronychia, the presentation can be quite variable,” she said. Nail unit melanoma can count erythronychia among the presenting signs. Clues that should raise suspicion for melanoma can include a wide band and prominent onycholysis, especially distal onycholysis and splintering. Again, she said, “biopsy with histopathology is the gold standard in making the diagnosis”; any symptoms or evidence of an evolving band should trigger a biopsy.
Dr. Lipner had no conflicts of interest relevant to her presentation.
SOURCE: Lipner S. Summer AAD 2019, Presentation F035.
NEW YORK – Nail discoloration, in all its variety, has a wide differential. And while that differential narrows when a patient presents with concerns about nails with red discoloration, there’s still a long list of diagnoses to consider.
During a nail-focused session at the American Academy of Dermatology summer meeting, Shari Lipner, MD, PhD, took attendees through a presentation-based approach that gets to the root etiology of erythronychia and guides diagnosis and treatment options.
“However, regardless of the etiology, erythronychia shares a common pathogenesis,” said Dr. Lipner, a dermatologist at New York–Presbyterian Hospital and Weil Cornell Medicine. The process begins in the distal nail matrix, resulting in a thin long strip of ventral nail becoming discolored, with the nail bed filling in the concavity. The engorged nail bed also makes the affected nail unit prone to splinter hemorrhages, and the thinned, transparent nail makes the erythema more visible, she explained.
Polydactylous longitudinal erythronychia
For erythronychia affecting several nails, onychotillomania is among the possible causes. This condition “often goes hand in hand with onychophagia,” and trichotillomania, skin-picking, or other self-mutilating disorders may also be present, she said. In both the adult and pediatric population, onychotillomania can accompany psychiatric disorders, including depression and obsessive-compulsive disorder, and may be associated with suicidal ideation, she added.
When onychotillomania is the cause, erythronychia may be accompanied by paronychia, and patients will often have a shortened nail bed and an atrophic nail plate. Dorsal pterygium may also be present.
Dermoscopy can provide some clues that onychotillomania is the culprit, said Dr. Lipner, citing a study that looked at dermoscopic images of 36 cases, which found scales in 94%, absence of the nail plate in 83%, and characteristic wavy lines in 69% (J Am Acad Dermatol. 2018 Oct;79[4]:702-5). Other frequent dermoscopy findings included hemorrhages (64%), crusts (61%), nail bed pigmentation (47%), and speckled dots (39%).
Lichen planus can also affect the nails, with erythronychia among its manifestations, she noted. Though lichen planus is thought of as a disease of middle or older age, usually affecting those aged 50-70 years, “15% of those affected are less than 20 years old,” she said.
The erythronychia of lichen planus is often accompanied by longitudinal riding, splitting, and atrophy of the nail plate, she said. Pterygium can also be present, representing a scar in the nail matrix. Dermatopathology will reveal a patchy, bandlike lichenoid infiltrate, with variable sawtooth hypergranulosis and hyperplasia.
“There’s not much evidence about how to treat lichen planus of the nails,” noted Dr. Lipner. Options can include intralesional corticosteroid injections at the nail matrix, topical corticosteroids, oral methotrexate, and retinoids.
Darier disease, an inherited condition caused by mutations in ATP2A2, has both skin and nail manifestations. Characteristic skin signs include hyperkeratotic papules, cobblestone papules, and palmar pits, she said. When nails are affected – as they are in up to 95% of Darier disease patients – they can have a characteristic “candy cane” appearance, with bands of longitudinal erythronychia alternating with normal-colored nail. The nails can also have V-shaped notching, she added.
Patients with systemic lupus erythematosus can also have longitudinal erythronychia; here, dermoscopy will show the characteristic prominent capillary loops in the proximal nail folds, she said.
Foreign substances such as nail polish and dyes, when they’re the source of erythronychia in one or several nails, can usually be wiped off with alcohol or acetone; also, “the proximal margin of discoloration will follow the same pattern as the nail fold,” said Dr. Lipner.
Localized longitudinal erythronychia
When the red discoloration is limited to a single nail, the differential shifts, said Dr. Lipner. With a hematoma, there’s often a history of trauma, and dermoscopy will show characteristic globules and streaks.
The first clue that erythronychia caused by onychopapilloma can be seen at the lunula: There will often be a comet- or pencil-shaped point to the discoloration in that region. But, she said, “the key is to do dermoscopy at the free edge of the nail plate. In 100 percent of cases, there will be a subungual hyperkeratotic papule” that will solidify the diagnosis.
Histopathology of onychopapillomas – a relatively recently recognized entity – will show nail bed and distal matrix acanthosis, with the distal nail bed showing matrix metaplasia, Dr. Lipner said.
Glomus tumors arise from cells of the glomus body, a specialized vascular apparatus that is involved in temperature regulation. “These structures are abundant in the digits and the subungual region,” said Dr. Lipner, which means that glomus tumors – a benign lesion – may develop subungually. Glomus tumors can be idiopathic, but she added, “think neurofibromatosis type 1 if you see multiple glomus tumors.”
Glomus tumors will present with longitudinal erythronychia, with a distal split of the nail sometimes accompanying the discoloration. A round bluish to gray nodule can also be seen. A thorough history and exam can help solidify the diagnosis, said Dr. Lipner; there’s a characteristic triad of point tenderness with the application of pressure to the nail, pain, and cold hypersensitivity.
Classically, the point tenderness is assessed by Love’s test, which elicits severe pain when the subungual tumor is pressed with a small object like the end of paper clip or a ballpoint pen. Application of a tourniquet to the arm after elevation, termed Hildreth’s test, should alleviate subungual glomus tumor pain, and release of the tourniquet causes an abrupt and marked recurrence of pain. Immersing the patient’s affected hand in cold water also increases glomus tumor pain.
“Imaging can be quite helpful” to confirm a glomus tumor diagnosis, said Dr. Lipner. “X-ray is cheap, and you can see erosions in 50% of patients.” However, she added, doppler ultrasound and magnetic resonance imaging are more sensitive, detecting tumors as small as 2 mm.
“Biopsy with histopathology is the gold standard in making the diagnosis” of glomus tumor, though, she noted. Pathologic examination will show monomorphic cells with small caliber vascular channels.
Malignancy is actually uncommon with erythronychia, though it’s always in the differential diagnosis, she said.
In one case series examining subungual squamous cell carcinomas, common findings included onycholysis and localized hyperkeratosis, along with longitudinal erythronychia. “This may be subtle; splinter hemorrhages can also be present,” noted Dr. Lipner, adding, “If there are any symptoms, or an evolving band, a biopsy is indicated.”
“Even with erythronychia, the presentation can be quite variable,” she said. Nail unit melanoma can count erythronychia among the presenting signs. Clues that should raise suspicion for melanoma can include a wide band and prominent onycholysis, especially distal onycholysis and splintering. Again, she said, “biopsy with histopathology is the gold standard in making the diagnosis”; any symptoms or evidence of an evolving band should trigger a biopsy.
Dr. Lipner had no conflicts of interest relevant to her presentation.
SOURCE: Lipner S. Summer AAD 2019, Presentation F035.
EXPERT ANALYSIS FROM SUMMER AAD 2019
Trained interpreters essential for treating non–English-speaking patients
NEW YORK – Clinicians should resist the temptation to use untrained interpreters, such as a child, another relative, or their own limited language skills, when treating patients who cannot communicate in English, according to an expert reviewing this issue at the American Academy of Dermatology summer meeting.
In clinical encounters with patients who have limited English proficiency, “ reported Amy Y.Y. Chen, MD, who is affiliated with Central Connecticut Dermatology in Canton.
In many situations, interpreter services are required by law. This includes a provision of the 1963 Civil Rights Act that specifies these services should be made available to any individual with limited English proficiency receiving federal financial assistance (with the exception of Medicare Part B).
In reviewing this and other laws, Dr. Chen explained that many prohibitions are explicit. For example, it is against the law for clinicians to communicate with the patient through children, whether or not they are related to the patient. A patient’s adult companions are also prohibited from interpreting unless the patient has provided express permission.
Despite the rules, some clinicians might be tempted to forgo a translator when none is readily available, opting for an improvised solution. Dr. Chen said that this is ill advised even when it is not illegal.
“There are a lot of potential problems with using nonprofessional interpreters, starting with the issue of confidentiality,” Dr. Chen warned.
As defined by the Department of Health & Human Services, a qualified interpreter establishes competency by developing familiarity with specialized terminology; by communicating accurately, effectively, and impartially; and by recognizing the ethical issues, including confidentiality, essential to their role.
By itself, language fluency might not be sufficient. Many physicians have conversational fluency in one or more languages other than English, but Dr. Chen pointed out that complex and nuanced clinical descriptions might be difficult to follow for a nonnative speaker. Moreover, many individuals who have no problem posing questions in a foreign language don’t do nearly as well in following the answers.
As interpreters, family members can be particularly problematic. In addition to the issues of confidentiality and medical terminology, a family member might have his or her own agenda that influences how questions and answers are conveyed.
Moreover, family members and others untrained in translating might edit answers based on their own sense of relevance. Many clinicians working through an interpreter will recognize the experience of receiving a yes or no answer after a lengthy discussion between a nontrained interpreter and patient. In such situations, the clinician can reasonably worry that important information was lost.
Typically, major hospitals already offer a systematic approach to providing interpreters when needed, but physicians working in private practice or other smaller practice settings might not. According to Dr. Chen, who recently collaborated on review of this issue (J Am Acad Dermatol. 2019 Mar;80:829-31), they should.
Interpreter services are available by telephone or Internet. Fees typically fall in the range of $2-$5 per minute. In offices with bilingual staff members, formal medical interpreter training might make sense. The Certification Commission for Healthcare Interpreters and the National Board of Certification for Medical Interpreters can help in this process.
When using a medical interpreter, Dr. Chen had some tips.
“Maintain eye contact and talk to the patient,” said Dr. Chen, suggesting that the interpreter, if present in the room, be seated next to or behind the patient. Whether the interpreter is in the room or participating remotely, Dr. Chen advised against speaking through the interpreter with such phases as “tell her that.” Rather, she advised speaking directly to the patient with the interpreter providing the translation.
More practically, Dr. Chen recommended speaking slowly and posing only one question at a time. She also recommended strategies to elicit reassurance that the patient has understood what was communicated. Not least, she recommended a “show me” approach in which a patient can repeat or demonstrate what he or she has learned.
Citing evidence that poor and incomplete translation contributes to medical errors and patient dissatisfaction, Dr. Chen reiterated that engaging unbiased trained translators is advisable for good clinical care even if it were not mandated by law.
NEW YORK – Clinicians should resist the temptation to use untrained interpreters, such as a child, another relative, or their own limited language skills, when treating patients who cannot communicate in English, according to an expert reviewing this issue at the American Academy of Dermatology summer meeting.
In clinical encounters with patients who have limited English proficiency, “ reported Amy Y.Y. Chen, MD, who is affiliated with Central Connecticut Dermatology in Canton.
In many situations, interpreter services are required by law. This includes a provision of the 1963 Civil Rights Act that specifies these services should be made available to any individual with limited English proficiency receiving federal financial assistance (with the exception of Medicare Part B).
In reviewing this and other laws, Dr. Chen explained that many prohibitions are explicit. For example, it is against the law for clinicians to communicate with the patient through children, whether or not they are related to the patient. A patient’s adult companions are also prohibited from interpreting unless the patient has provided express permission.
Despite the rules, some clinicians might be tempted to forgo a translator when none is readily available, opting for an improvised solution. Dr. Chen said that this is ill advised even when it is not illegal.
“There are a lot of potential problems with using nonprofessional interpreters, starting with the issue of confidentiality,” Dr. Chen warned.
As defined by the Department of Health & Human Services, a qualified interpreter establishes competency by developing familiarity with specialized terminology; by communicating accurately, effectively, and impartially; and by recognizing the ethical issues, including confidentiality, essential to their role.
By itself, language fluency might not be sufficient. Many physicians have conversational fluency in one or more languages other than English, but Dr. Chen pointed out that complex and nuanced clinical descriptions might be difficult to follow for a nonnative speaker. Moreover, many individuals who have no problem posing questions in a foreign language don’t do nearly as well in following the answers.
As interpreters, family members can be particularly problematic. In addition to the issues of confidentiality and medical terminology, a family member might have his or her own agenda that influences how questions and answers are conveyed.
Moreover, family members and others untrained in translating might edit answers based on their own sense of relevance. Many clinicians working through an interpreter will recognize the experience of receiving a yes or no answer after a lengthy discussion between a nontrained interpreter and patient. In such situations, the clinician can reasonably worry that important information was lost.
Typically, major hospitals already offer a systematic approach to providing interpreters when needed, but physicians working in private practice or other smaller practice settings might not. According to Dr. Chen, who recently collaborated on review of this issue (J Am Acad Dermatol. 2019 Mar;80:829-31), they should.
Interpreter services are available by telephone or Internet. Fees typically fall in the range of $2-$5 per minute. In offices with bilingual staff members, formal medical interpreter training might make sense. The Certification Commission for Healthcare Interpreters and the National Board of Certification for Medical Interpreters can help in this process.
When using a medical interpreter, Dr. Chen had some tips.
“Maintain eye contact and talk to the patient,” said Dr. Chen, suggesting that the interpreter, if present in the room, be seated next to or behind the patient. Whether the interpreter is in the room or participating remotely, Dr. Chen advised against speaking through the interpreter with such phases as “tell her that.” Rather, she advised speaking directly to the patient with the interpreter providing the translation.
More practically, Dr. Chen recommended speaking slowly and posing only one question at a time. She also recommended strategies to elicit reassurance that the patient has understood what was communicated. Not least, she recommended a “show me” approach in which a patient can repeat or demonstrate what he or she has learned.
Citing evidence that poor and incomplete translation contributes to medical errors and patient dissatisfaction, Dr. Chen reiterated that engaging unbiased trained translators is advisable for good clinical care even if it were not mandated by law.
NEW YORK – Clinicians should resist the temptation to use untrained interpreters, such as a child, another relative, or their own limited language skills, when treating patients who cannot communicate in English, according to an expert reviewing this issue at the American Academy of Dermatology summer meeting.
In clinical encounters with patients who have limited English proficiency, “ reported Amy Y.Y. Chen, MD, who is affiliated with Central Connecticut Dermatology in Canton.
In many situations, interpreter services are required by law. This includes a provision of the 1963 Civil Rights Act that specifies these services should be made available to any individual with limited English proficiency receiving federal financial assistance (with the exception of Medicare Part B).
In reviewing this and other laws, Dr. Chen explained that many prohibitions are explicit. For example, it is against the law for clinicians to communicate with the patient through children, whether or not they are related to the patient. A patient’s adult companions are also prohibited from interpreting unless the patient has provided express permission.
Despite the rules, some clinicians might be tempted to forgo a translator when none is readily available, opting for an improvised solution. Dr. Chen said that this is ill advised even when it is not illegal.
“There are a lot of potential problems with using nonprofessional interpreters, starting with the issue of confidentiality,” Dr. Chen warned.
As defined by the Department of Health & Human Services, a qualified interpreter establishes competency by developing familiarity with specialized terminology; by communicating accurately, effectively, and impartially; and by recognizing the ethical issues, including confidentiality, essential to their role.
By itself, language fluency might not be sufficient. Many physicians have conversational fluency in one or more languages other than English, but Dr. Chen pointed out that complex and nuanced clinical descriptions might be difficult to follow for a nonnative speaker. Moreover, many individuals who have no problem posing questions in a foreign language don’t do nearly as well in following the answers.
As interpreters, family members can be particularly problematic. In addition to the issues of confidentiality and medical terminology, a family member might have his or her own agenda that influences how questions and answers are conveyed.
Moreover, family members and others untrained in translating might edit answers based on their own sense of relevance. Many clinicians working through an interpreter will recognize the experience of receiving a yes or no answer after a lengthy discussion between a nontrained interpreter and patient. In such situations, the clinician can reasonably worry that important information was lost.
Typically, major hospitals already offer a systematic approach to providing interpreters when needed, but physicians working in private practice or other smaller practice settings might not. According to Dr. Chen, who recently collaborated on review of this issue (J Am Acad Dermatol. 2019 Mar;80:829-31), they should.
Interpreter services are available by telephone or Internet. Fees typically fall in the range of $2-$5 per minute. In offices with bilingual staff members, formal medical interpreter training might make sense. The Certification Commission for Healthcare Interpreters and the National Board of Certification for Medical Interpreters can help in this process.
When using a medical interpreter, Dr. Chen had some tips.
“Maintain eye contact and talk to the patient,” said Dr. Chen, suggesting that the interpreter, if present in the room, be seated next to or behind the patient. Whether the interpreter is in the room or participating remotely, Dr. Chen advised against speaking through the interpreter with such phases as “tell her that.” Rather, she advised speaking directly to the patient with the interpreter providing the translation.
More practically, Dr. Chen recommended speaking slowly and posing only one question at a time. She also recommended strategies to elicit reassurance that the patient has understood what was communicated. Not least, she recommended a “show me” approach in which a patient can repeat or demonstrate what he or she has learned.
Citing evidence that poor and incomplete translation contributes to medical errors and patient dissatisfaction, Dr. Chen reiterated that engaging unbiased trained translators is advisable for good clinical care even if it were not mandated by law.
EXPERT ANALYSIS FROM SUMMER AAD 2019