User login
Extent of breast surgery is tied to quality of life among young breast cancer survivors
SAN ANTONIO – Younger breast cancer patients who undergo unilateral or bilateral mastectomy report lower breast satisfaction and poorer psychosocial and sexual well-being than counterparts who undergo breast-conserving surgery, finds a cross-sectional cohort study presented by lead investigator Laura S. Dominici, MD, FACS, at the San Antonio Breast Cancer Symposium.
The 560 women studied had a mean age of 37 years and had completed the BREAST-Q questionnaire a median of 5.8 years after their breast cancer diagnosis. Results showed that the mean score for satisfaction with breasts was 65.5 with breast-conserving surgery, 59.3 with unilateral mastectomy, and 60.4 with bilateral mastectomy (P = .008). The mastectomy groups also had poorer scores for psychosocial well-being (P less than .001) and sexual well-being (P less than .001), but not physical well-being. Most of the differences remained significant in meta-analysis. In a video interview, Dr. Dominici, of Dana-Farber Cancer Institute, Boston, discussed worry and anxiety about recurrence and second cancers as drivers of choosing mastectomy, generalizability of the study’s findings, and strategies for incorporating this new information into counseling and shared decision making.
Dr. Dominici disclosed that she had no conflicts of interest. The study was funded by the Agency for Healthcare Research and Quality, Susan G. Komen, the Breast Cancer Research Foundation, and The Pink Agenda.
SAN ANTONIO – Younger breast cancer patients who undergo unilateral or bilateral mastectomy report lower breast satisfaction and poorer psychosocial and sexual well-being than counterparts who undergo breast-conserving surgery, finds a cross-sectional cohort study presented by lead investigator Laura S. Dominici, MD, FACS, at the San Antonio Breast Cancer Symposium.
The 560 women studied had a mean age of 37 years and had completed the BREAST-Q questionnaire a median of 5.8 years after their breast cancer diagnosis. Results showed that the mean score for satisfaction with breasts was 65.5 with breast-conserving surgery, 59.3 with unilateral mastectomy, and 60.4 with bilateral mastectomy (P = .008). The mastectomy groups also had poorer scores for psychosocial well-being (P less than .001) and sexual well-being (P less than .001), but not physical well-being. Most of the differences remained significant in meta-analysis. In a video interview, Dr. Dominici, of Dana-Farber Cancer Institute, Boston, discussed worry and anxiety about recurrence and second cancers as drivers of choosing mastectomy, generalizability of the study’s findings, and strategies for incorporating this new information into counseling and shared decision making.
Dr. Dominici disclosed that she had no conflicts of interest. The study was funded by the Agency for Healthcare Research and Quality, Susan G. Komen, the Breast Cancer Research Foundation, and The Pink Agenda.
SAN ANTONIO – Younger breast cancer patients who undergo unilateral or bilateral mastectomy report lower breast satisfaction and poorer psychosocial and sexual well-being than counterparts who undergo breast-conserving surgery, finds a cross-sectional cohort study presented by lead investigator Laura S. Dominici, MD, FACS, at the San Antonio Breast Cancer Symposium.
The 560 women studied had a mean age of 37 years and had completed the BREAST-Q questionnaire a median of 5.8 years after their breast cancer diagnosis. Results showed that the mean score for satisfaction with breasts was 65.5 with breast-conserving surgery, 59.3 with unilateral mastectomy, and 60.4 with bilateral mastectomy (P = .008). The mastectomy groups also had poorer scores for psychosocial well-being (P less than .001) and sexual well-being (P less than .001), but not physical well-being. Most of the differences remained significant in meta-analysis. In a video interview, Dr. Dominici, of Dana-Farber Cancer Institute, Boston, discussed worry and anxiety about recurrence and second cancers as drivers of choosing mastectomy, generalizability of the study’s findings, and strategies for incorporating this new information into counseling and shared decision making.
Dr. Dominici disclosed that she had no conflicts of interest. The study was funded by the Agency for Healthcare Research and Quality, Susan G. Komen, the Breast Cancer Research Foundation, and The Pink Agenda.
REPORTING FROM SABCS 2018
pCR may obviate need for adjuvant chemotherapy
SAN ANTONIO – Women with localized breast cancer who achieve a pathological complete response (pCR) after neoadjuvant chemotherapy may be able to safely skip adjuvant chemotherapy, suggest new data from a patient-level meta-analysis reported in a session and press conference at the San Antonio Breast Cancer Symposium.
“The focus of many breast cancer trials for several years has been on adding additional systemic therapies to reduce recurrence risk. However, adding therapies can result in additional toxicity and overtreatment for many patients,” noted lead investigator Laura M. Spring, MD, of Massachusetts General Hospital Cancer Center and Harvard Medical School, both in Boston. “The neoadjuvant chemotherapy model offers several additional clinical and research advantages over adjuvant chemotherapy, including the rapid evaluation of treatment response utilizing surrogate biomarkers, such as pathological complete response.”
The meta-analysis of 52 studies, which included a total of 27,895 women who were given neoadjuvant chemotherapy, confirmed a large positive prognostic effect of pCR on outcomes in the entire sample, with a 69% relative reduction in event-free survival (EFS) events and a 78% relative reduction in risk of death, a pattern that was consistent across clinical subtypes of breast cancer. More importantly, among those achieving a pCR, EFS did not differ significantly whether they went on to receive more chemotherapy after surgery or not.
“Achieving pCR following neoadjuvant chemotherapy is associated with significantly improved EFS and overall survival, particularly for triple-negative and HER2-positive breast cancer. The results are highly significant despite inclusion of a variety of neoadjuvant regimens, suggesting the path taken to attain a pCR may not be critical,” Dr. Spring proposed. “The similar outcomes with or without adjuvant chemotherapy in patients who attained pCR after neoadjuvant chemotherapy likely reflects tumor biology and suggests adjuvant chemotherapy could potentially be omitted in certain circumstances. Further research is needed to evaluate the clinical utility of escalation and de-escalation strategies in the adjuvant setting based on neoadjuvant response.”
“Basically, it appears that the impact of chemotherapy is going to be early, or if you use it early, you really don’t lose the impact [that it has] if you wait until after surgery,” commented SABCS codirector and press conference moderator Carlos Arteaga, MD, director of the Harold C. Simmons Comprehensive Cancer Center and associate dean of Oncology Programs at UT Southwestern Medical Center, Dallas, Texas. “So if it was me, I would have it done before the operation, frankly, because at a minimum, it’s not worse than delaying it until after surgery – at a minimum. And you get the benefit of potential breast conservation, a lesser surgery.”
Study details
For the meta-analysis, Dr. Spring and her coinvestigators searched for published studies of localized breast cancer that had 25 patients or more, featured neoadjuvant chemotherapy, and reported pCR using definitions allowed by the FDA (ypT0 ypN0 or ypT0/is ypN0), as well as recurrence and/or survival based on pathologic outcome. They excluded studies reporting only local recurrence and those using neoadjuvant endocrine therapy or neoadjuvant radiation.
Results showed that the pCR rate averaged 21.1% for the entire study population, according to Dr. Spring. But there was wide variation by tumor subtype, as expected, with a rate of less than 10% for hormone receptor–positive/HER2-negative breast cancer, to rates in the mid-30% range for triple-negative breast cancer and HER2-positive breast cancer.
Women who had pCR after neoadjuvant chemotherapy had a significantly lower risk of EFS events than peers who had residual disease (hazard ratio, 0.31; 95% probability interval, 0.24-0.39). The corresponding 5-year EFS rates were 88% and 67%.
Similarly, women who had pCR had a significantly lower risk of death (HR, 0.22; 95% probability interval, 0.15-0.30). The corresponding 5-year overall survival rates were 94% and 75%.
The EFS benefit of pCR versus residual disease was consistently seen across subgroups with triple-negative breast cancer (90% vs. 57%), HER2-positive breast cancer (86% vs. 63%), and hormone receptor–positive/HER2-negative breast cancer (97% vs. 88%). Findings were essentially the same for overall survival, according to Dr. Spring.
Among patients attaining pCR, the 5-year EFS rate was 86% for those who went on to receive adjuvant chemotherapy (HR, 0.36; 95% probability interval, 0.19-0.67) and 88% for those who did not (HR, 0.36; 95% probability interval, 0.27-0.54). The difference in hazard ratios between groups was not significant (P = .60).
Finally, the investigators conducted modeling to assess how the change in pCR rate corresponded with the change in EFS benefit. “This approach could be helpful in the design of neoadjuvant studies,” Dr. Spring explained.
“Assuming pCR is a valid surrogate endpoint, this is, it mediates all treatment effects, and that the average pCR is 50%, the magnitude of pCR change is predictive of treatment effects on EFS within a certain amount of uncertainty, based on the model,” she reported. For example, a change in pCR of 0.3 had a corresponding HR of 0.72, with a 95% probability interval of 0.68-0.77.
Dr. Spring disclosed that she has a consulting or advisory role with Novartis and that she receives institutional research funding from Tesaro. The study was supported by grants from the National Cancer Institute and Susan G. Komen.
SOURCE: Spring LM et al. SABCS 2018, Abstract GS2-03.
SAN ANTONIO – Women with localized breast cancer who achieve a pathological complete response (pCR) after neoadjuvant chemotherapy may be able to safely skip adjuvant chemotherapy, suggest new data from a patient-level meta-analysis reported in a session and press conference at the San Antonio Breast Cancer Symposium.
“The focus of many breast cancer trials for several years has been on adding additional systemic therapies to reduce recurrence risk. However, adding therapies can result in additional toxicity and overtreatment for many patients,” noted lead investigator Laura M. Spring, MD, of Massachusetts General Hospital Cancer Center and Harvard Medical School, both in Boston. “The neoadjuvant chemotherapy model offers several additional clinical and research advantages over adjuvant chemotherapy, including the rapid evaluation of treatment response utilizing surrogate biomarkers, such as pathological complete response.”
The meta-analysis of 52 studies, which included a total of 27,895 women who were given neoadjuvant chemotherapy, confirmed a large positive prognostic effect of pCR on outcomes in the entire sample, with a 69% relative reduction in event-free survival (EFS) events and a 78% relative reduction in risk of death, a pattern that was consistent across clinical subtypes of breast cancer. More importantly, among those achieving a pCR, EFS did not differ significantly whether they went on to receive more chemotherapy after surgery or not.
“Achieving pCR following neoadjuvant chemotherapy is associated with significantly improved EFS and overall survival, particularly for triple-negative and HER2-positive breast cancer. The results are highly significant despite inclusion of a variety of neoadjuvant regimens, suggesting the path taken to attain a pCR may not be critical,” Dr. Spring proposed. “The similar outcomes with or without adjuvant chemotherapy in patients who attained pCR after neoadjuvant chemotherapy likely reflects tumor biology and suggests adjuvant chemotherapy could potentially be omitted in certain circumstances. Further research is needed to evaluate the clinical utility of escalation and de-escalation strategies in the adjuvant setting based on neoadjuvant response.”
“Basically, it appears that the impact of chemotherapy is going to be early, or if you use it early, you really don’t lose the impact [that it has] if you wait until after surgery,” commented SABCS codirector and press conference moderator Carlos Arteaga, MD, director of the Harold C. Simmons Comprehensive Cancer Center and associate dean of Oncology Programs at UT Southwestern Medical Center, Dallas, Texas. “So if it was me, I would have it done before the operation, frankly, because at a minimum, it’s not worse than delaying it until after surgery – at a minimum. And you get the benefit of potential breast conservation, a lesser surgery.”
Study details
For the meta-analysis, Dr. Spring and her coinvestigators searched for published studies of localized breast cancer that had 25 patients or more, featured neoadjuvant chemotherapy, and reported pCR using definitions allowed by the FDA (ypT0 ypN0 or ypT0/is ypN0), as well as recurrence and/or survival based on pathologic outcome. They excluded studies reporting only local recurrence and those using neoadjuvant endocrine therapy or neoadjuvant radiation.
Results showed that the pCR rate averaged 21.1% for the entire study population, according to Dr. Spring. But there was wide variation by tumor subtype, as expected, with a rate of less than 10% for hormone receptor–positive/HER2-negative breast cancer, to rates in the mid-30% range for triple-negative breast cancer and HER2-positive breast cancer.
Women who had pCR after neoadjuvant chemotherapy had a significantly lower risk of EFS events than peers who had residual disease (hazard ratio, 0.31; 95% probability interval, 0.24-0.39). The corresponding 5-year EFS rates were 88% and 67%.
Similarly, women who had pCR had a significantly lower risk of death (HR, 0.22; 95% probability interval, 0.15-0.30). The corresponding 5-year overall survival rates were 94% and 75%.
The EFS benefit of pCR versus residual disease was consistently seen across subgroups with triple-negative breast cancer (90% vs. 57%), HER2-positive breast cancer (86% vs. 63%), and hormone receptor–positive/HER2-negative breast cancer (97% vs. 88%). Findings were essentially the same for overall survival, according to Dr. Spring.
Among patients attaining pCR, the 5-year EFS rate was 86% for those who went on to receive adjuvant chemotherapy (HR, 0.36; 95% probability interval, 0.19-0.67) and 88% for those who did not (HR, 0.36; 95% probability interval, 0.27-0.54). The difference in hazard ratios between groups was not significant (P = .60).
Finally, the investigators conducted modeling to assess how the change in pCR rate corresponded with the change in EFS benefit. “This approach could be helpful in the design of neoadjuvant studies,” Dr. Spring explained.
“Assuming pCR is a valid surrogate endpoint, this is, it mediates all treatment effects, and that the average pCR is 50%, the magnitude of pCR change is predictive of treatment effects on EFS within a certain amount of uncertainty, based on the model,” she reported. For example, a change in pCR of 0.3 had a corresponding HR of 0.72, with a 95% probability interval of 0.68-0.77.
Dr. Spring disclosed that she has a consulting or advisory role with Novartis and that she receives institutional research funding from Tesaro. The study was supported by grants from the National Cancer Institute and Susan G. Komen.
SOURCE: Spring LM et al. SABCS 2018, Abstract GS2-03.
SAN ANTONIO – Women with localized breast cancer who achieve a pathological complete response (pCR) after neoadjuvant chemotherapy may be able to safely skip adjuvant chemotherapy, suggest new data from a patient-level meta-analysis reported in a session and press conference at the San Antonio Breast Cancer Symposium.
“The focus of many breast cancer trials for several years has been on adding additional systemic therapies to reduce recurrence risk. However, adding therapies can result in additional toxicity and overtreatment for many patients,” noted lead investigator Laura M. Spring, MD, of Massachusetts General Hospital Cancer Center and Harvard Medical School, both in Boston. “The neoadjuvant chemotherapy model offers several additional clinical and research advantages over adjuvant chemotherapy, including the rapid evaluation of treatment response utilizing surrogate biomarkers, such as pathological complete response.”
The meta-analysis of 52 studies, which included a total of 27,895 women who were given neoadjuvant chemotherapy, confirmed a large positive prognostic effect of pCR on outcomes in the entire sample, with a 69% relative reduction in event-free survival (EFS) events and a 78% relative reduction in risk of death, a pattern that was consistent across clinical subtypes of breast cancer. More importantly, among those achieving a pCR, EFS did not differ significantly whether they went on to receive more chemotherapy after surgery or not.
“Achieving pCR following neoadjuvant chemotherapy is associated with significantly improved EFS and overall survival, particularly for triple-negative and HER2-positive breast cancer. The results are highly significant despite inclusion of a variety of neoadjuvant regimens, suggesting the path taken to attain a pCR may not be critical,” Dr. Spring proposed. “The similar outcomes with or without adjuvant chemotherapy in patients who attained pCR after neoadjuvant chemotherapy likely reflects tumor biology and suggests adjuvant chemotherapy could potentially be omitted in certain circumstances. Further research is needed to evaluate the clinical utility of escalation and de-escalation strategies in the adjuvant setting based on neoadjuvant response.”
“Basically, it appears that the impact of chemotherapy is going to be early, or if you use it early, you really don’t lose the impact [that it has] if you wait until after surgery,” commented SABCS codirector and press conference moderator Carlos Arteaga, MD, director of the Harold C. Simmons Comprehensive Cancer Center and associate dean of Oncology Programs at UT Southwestern Medical Center, Dallas, Texas. “So if it was me, I would have it done before the operation, frankly, because at a minimum, it’s not worse than delaying it until after surgery – at a minimum. And you get the benefit of potential breast conservation, a lesser surgery.”
Study details
For the meta-analysis, Dr. Spring and her coinvestigators searched for published studies of localized breast cancer that had 25 patients or more, featured neoadjuvant chemotherapy, and reported pCR using definitions allowed by the FDA (ypT0 ypN0 or ypT0/is ypN0), as well as recurrence and/or survival based on pathologic outcome. They excluded studies reporting only local recurrence and those using neoadjuvant endocrine therapy or neoadjuvant radiation.
Results showed that the pCR rate averaged 21.1% for the entire study population, according to Dr. Spring. But there was wide variation by tumor subtype, as expected, with a rate of less than 10% for hormone receptor–positive/HER2-negative breast cancer, to rates in the mid-30% range for triple-negative breast cancer and HER2-positive breast cancer.
Women who had pCR after neoadjuvant chemotherapy had a significantly lower risk of EFS events than peers who had residual disease (hazard ratio, 0.31; 95% probability interval, 0.24-0.39). The corresponding 5-year EFS rates were 88% and 67%.
Similarly, women who had pCR had a significantly lower risk of death (HR, 0.22; 95% probability interval, 0.15-0.30). The corresponding 5-year overall survival rates were 94% and 75%.
The EFS benefit of pCR versus residual disease was consistently seen across subgroups with triple-negative breast cancer (90% vs. 57%), HER2-positive breast cancer (86% vs. 63%), and hormone receptor–positive/HER2-negative breast cancer (97% vs. 88%). Findings were essentially the same for overall survival, according to Dr. Spring.
Among patients attaining pCR, the 5-year EFS rate was 86% for those who went on to receive adjuvant chemotherapy (HR, 0.36; 95% probability interval, 0.19-0.67) and 88% for those who did not (HR, 0.36; 95% probability interval, 0.27-0.54). The difference in hazard ratios between groups was not significant (P = .60).
Finally, the investigators conducted modeling to assess how the change in pCR rate corresponded with the change in EFS benefit. “This approach could be helpful in the design of neoadjuvant studies,” Dr. Spring explained.
“Assuming pCR is a valid surrogate endpoint, this is, it mediates all treatment effects, and that the average pCR is 50%, the magnitude of pCR change is predictive of treatment effects on EFS within a certain amount of uncertainty, based on the model,” she reported. For example, a change in pCR of 0.3 had a corresponding HR of 0.72, with a 95% probability interval of 0.68-0.77.
Dr. Spring disclosed that she has a consulting or advisory role with Novartis and that she receives institutional research funding from Tesaro. The study was supported by grants from the National Cancer Institute and Susan G. Komen.
SOURCE: Spring LM et al. SABCS 2018, Abstract GS2-03.
REPORTING FROM SABCS 2018
Key clinical point: Adjuvant chemotherapy does not further improve outcome after a pathological complete response to neoadjuvant chemotherapy.
Major finding: Patients achieving pCR had a similar reduction in risk of EFS events whether they went on to receive adjuvant chemotherapy (hazard ratio, 0.36) or not (hazard ratio, 0.36; P = .60 for difference between groups).
Study details: Individual-level meta-analysis of 27,895 patients who received neoadjuvant chemotherapy for localized breast cancer.
Disclosures: Dr. Spring disclosed that she has a consulting or advisory role with Novartis and that she receives institutional research funding from Tesaro. The study was supported by grants from the National Cancer Institute and Susan G. Komen.
Source: Spring LM et al. SABCS 2018, Abstract GS2-03.
Dietary sodium still in play as a potential MS risk factor
BERLIN – Among a host of potential risk factors for multiple sclerosis (MS), one emerging risk factor – dietary sodium – has accumulating evidence, bolstered by new imaging techniques and emerging research about the mediating effect of the gut microbiome.
“The word is still out on salt – there’s still some work to do; we are not where we stand with smoking or obesity” and the association with MS, said Ralf Linker, MD, speaking at the annual congress of the European Committee for Treatment and Research in Multiple Sclerosis.
For all potential emerging risk factors for MS, there’s an attractive hypothesis and, often, epidemiologic data, Dr. Linker said. “There are probably good [epidemiologic] data in multiple sclerosis for vitamin D, smoking, obesity, and probably also alcohol,” he said. “The therapeutic consequence, however, is much less clear, the best example of that being, of course, vitamin D.”
“The attractive risk factor is not enough to be a hypothesis, although some people seem to believe that nowadays,” said Dr. Linker, chair of the department of neurology at Friedrich-Alexander University, Erlangen, Germany. “Probably it’s better to start with some basic science and some experimental data to get an idea of the mechanism.”
“Today, we need clear associations with clear markers, well-defined cohorts, and proper epidemiological data telling us whether this is a real risk factor. ... If you look at the clinicians – and there are many among us in the room here – your ultimate goal, of course, is to use this as an intervention.”
For salt intake, there’s a clear overlap between high salt consumption in Westernized diets and increasing incidence of MS. The association also holds for many other autoimmune diseases, Dr. Linker added.
“The next step is experimental evidence,” Dr. Linker said. In a rodent model of experimental autoimmune encephalomyelitis (EAE), rats with high salt intake had a worse clinical course, compared with control rats fed a usual diet (Nature. 2013 Apr 25;496[7446]:518-22).
“There were a lot of follow-up studies on that,” with identification of multiple immune cells that are up- or down-regulated via distinct pathways in a high-salt environment, Dr. Linker said.
More recently, Dr. Linker was a coinvestigator in work showing that healthy humans placed on a high-salt diet had significant increases in T-helper 17 (Th17) cells after just 2 weeks of an additional 6 g of table salt daily over a baseline 2-4 g/day (Nature. 2017 Nov 30;551[7682]:585-9).
“You can also translate it to a more realistic setting,” where individuals who ate fast food four or more times weekly had significantly higher Th17 cell counts than did those who ate less fast food, he noted in reference to unpublished data.
Looking specifically at MS, a single-center study found that increased sodium intake correlated with increased MS clinical disease activity, with the highest sodium intake (more than 4.8 g/day) associated with higher incidence of MS exacerbations. Those in the highest tier of sodium intake also had a higher lesion load, with 3.65 more T2 lesions seen on MRI scans for each gram of salt consumed above average amounts of 2-4.8 g/day (J Neurol Neurosurg Psychiatry. 2015 Jan;86[1]:26-31).
On the other hand, Dr. Linker said, “There have been recent very well-conducted studies in very well-defined cohorts casting doubt on this translation to multiple sclerosis.” In particular, an examination of data from over 70,000 participants in the Nurse’s Health Study showed no association between MS risk and dietary salt assessed by a nutritional questionnaire (Neurology. 2017 Sep 26;89[13]:1322-9). “There was no hint that the diagnosis was linked in any way with salt exposure,” Dr. Linker said.
In the BENEFIT study, both a spot urine sample and a food questionnaire were used, and patients were grouped into quintiles of sodium intake. For demyelinating events and MS diagnosis, the curves for all quintiles were “completely overlapping,” with no sign of increased risk of MS with higher sodium intake (Ann Neurol. 2017;82:20-9).
An important caveat to the null findings in these analyses is the known poor agreement between self-report of salt intake and actual sodium load, Dr. Linker noted. Renal sodium excretion can vary widely despite fixed salt intake, so spot urine and even 24-hour urine collection don’t guarantee accuracy, he said, citing studies from space travel emulations that show wide day-to-day excursions in sodium excretion with a fixed diet.
A promising tool for accurate assessment of sodium load may be sodium-23 skin spectroscopy using MRI, because skin tissue binds sodium in a stable, nonosmotic fashion. Dr. Linker and his colleagues have recently found that skin sodium levels, measured at the calf, are higher in individuals with relapsing-remitting MS. “Indeed, the sodium level in the skin of the MS patients was significantly higher than in the controls” who did not have MS, he said of the study that matched 20 patients with MS with 20 healthy controls. The MRI studies were assessed by radiologists blinded to the disease status of participants.
The increase is seen in only free sodium and seen in skin, but not muscle tissue, Dr. Linker said.
Using MRI spectroscopy with a powerful 7-Tesla magnet, Dr. Linker and his colleagues returned to the rodent EAE model, also finding increased sodium in the skin. Mass spectrometry findings were similar in other rodent autoimmune models, he said. The differences were not seen for sodium in other organs, or for potassium levels in the skin.
“The most difficult point,” Dr. Linker said, is “can we use this therapeutically somehow? Of course, you can put your patients on a salt-free or very low-salt diet, but it’s not very tasty, of course, and adherence would be probably very, very low.”
The microbiome may play a modulating role that adds to the sodium-MS story and provides a potential therapeutic option. In mice, a high-salt diet was associated with marked and rapid depletion of Lactobacillus species in the mouse gut microbiome. In healthy humans as well, the drop in lactobacilli was quick and profound when 6 g/day of salt was added to the diet, Dr. Linker said (P = .0053 versus the control diet of 2-4 g sodium/day).
Working backward with the same healthy cohort, repletion of Lactobacillus by probiotic supplementation normalized systolic blood pressure, which had become elevated with increased dietary sodium. Further, Lactobacillus repletion downregulated Th17 cells to levels seen before the high-sodium diet, even when dietary sodium stayed high.
“This was even transferred to multiple sclerosis,” in work recently published by another group, Dr. Linker said. For patients with MS who consumed a Lactobacillus-containing probiotic, investigators could “clearly show, besides effects on the microbiome itself, that there were effects on antigen-presenting cells in MS patients.” Intermediate monocytes decreased, as did dendritic cells, in the small study that involved both healthy controls and MS patients who received a probiotic and then underwent a washout period. Stool and blood samples were collected in both groups to compare values with and without probiotic administration.
A question from the audience looked back at historic data: 100 or more years ago, salt was used extensively for food preservation in many parts of the world, so dietary sodium intake is thought to have been higher. The incidence of MS, though, was lower then. Dr. Linker pointed out that food preservation practices varied widely, and that a host of other variables make assessment of past or present associations difficult. “It’s hard to argue that salt is the one and only risk factor; I would strongly doubt that.”
Still, he said, this early work invites more study, with a target of establishing whether probiotic supplementation could be used as “add-on therapy to established immune drugs.”
Dr. Linker has received honoraria and research support from Bayer, Biogen, Genzyme, Merck Serono, Novartis, and TEVA.
SOURCE: Linker R. ECTRIMS 2018, Scientific Session 7.
BERLIN – Among a host of potential risk factors for multiple sclerosis (MS), one emerging risk factor – dietary sodium – has accumulating evidence, bolstered by new imaging techniques and emerging research about the mediating effect of the gut microbiome.
“The word is still out on salt – there’s still some work to do; we are not where we stand with smoking or obesity” and the association with MS, said Ralf Linker, MD, speaking at the annual congress of the European Committee for Treatment and Research in Multiple Sclerosis.
For all potential emerging risk factors for MS, there’s an attractive hypothesis and, often, epidemiologic data, Dr. Linker said. “There are probably good [epidemiologic] data in multiple sclerosis for vitamin D, smoking, obesity, and probably also alcohol,” he said. “The therapeutic consequence, however, is much less clear, the best example of that being, of course, vitamin D.”
“The attractive risk factor is not enough to be a hypothesis, although some people seem to believe that nowadays,” said Dr. Linker, chair of the department of neurology at Friedrich-Alexander University, Erlangen, Germany. “Probably it’s better to start with some basic science and some experimental data to get an idea of the mechanism.”
“Today, we need clear associations with clear markers, well-defined cohorts, and proper epidemiological data telling us whether this is a real risk factor. ... If you look at the clinicians – and there are many among us in the room here – your ultimate goal, of course, is to use this as an intervention.”
For salt intake, there’s a clear overlap between high salt consumption in Westernized diets and increasing incidence of MS. The association also holds for many other autoimmune diseases, Dr. Linker added.
“The next step is experimental evidence,” Dr. Linker said. In a rodent model of experimental autoimmune encephalomyelitis (EAE), rats with high salt intake had a worse clinical course, compared with control rats fed a usual diet (Nature. 2013 Apr 25;496[7446]:518-22).
“There were a lot of follow-up studies on that,” with identification of multiple immune cells that are up- or down-regulated via distinct pathways in a high-salt environment, Dr. Linker said.
More recently, Dr. Linker was a coinvestigator in work showing that healthy humans placed on a high-salt diet had significant increases in T-helper 17 (Th17) cells after just 2 weeks of an additional 6 g of table salt daily over a baseline 2-4 g/day (Nature. 2017 Nov 30;551[7682]:585-9).
“You can also translate it to a more realistic setting,” where individuals who ate fast food four or more times weekly had significantly higher Th17 cell counts than did those who ate less fast food, he noted in reference to unpublished data.
Looking specifically at MS, a single-center study found that increased sodium intake correlated with increased MS clinical disease activity, with the highest sodium intake (more than 4.8 g/day) associated with higher incidence of MS exacerbations. Those in the highest tier of sodium intake also had a higher lesion load, with 3.65 more T2 lesions seen on MRI scans for each gram of salt consumed above average amounts of 2-4.8 g/day (J Neurol Neurosurg Psychiatry. 2015 Jan;86[1]:26-31).
On the other hand, Dr. Linker said, “There have been recent very well-conducted studies in very well-defined cohorts casting doubt on this translation to multiple sclerosis.” In particular, an examination of data from over 70,000 participants in the Nurse’s Health Study showed no association between MS risk and dietary salt assessed by a nutritional questionnaire (Neurology. 2017 Sep 26;89[13]:1322-9). “There was no hint that the diagnosis was linked in any way with salt exposure,” Dr. Linker said.
In the BENEFIT study, both a spot urine sample and a food questionnaire were used, and patients were grouped into quintiles of sodium intake. For demyelinating events and MS diagnosis, the curves for all quintiles were “completely overlapping,” with no sign of increased risk of MS with higher sodium intake (Ann Neurol. 2017;82:20-9).
An important caveat to the null findings in these analyses is the known poor agreement between self-report of salt intake and actual sodium load, Dr. Linker noted. Renal sodium excretion can vary widely despite fixed salt intake, so spot urine and even 24-hour urine collection don’t guarantee accuracy, he said, citing studies from space travel emulations that show wide day-to-day excursions in sodium excretion with a fixed diet.
A promising tool for accurate assessment of sodium load may be sodium-23 skin spectroscopy using MRI, because skin tissue binds sodium in a stable, nonosmotic fashion. Dr. Linker and his colleagues have recently found that skin sodium levels, measured at the calf, are higher in individuals with relapsing-remitting MS. “Indeed, the sodium level in the skin of the MS patients was significantly higher than in the controls” who did not have MS, he said of the study that matched 20 patients with MS with 20 healthy controls. The MRI studies were assessed by radiologists blinded to the disease status of participants.
The increase is seen in only free sodium and seen in skin, but not muscle tissue, Dr. Linker said.
Using MRI spectroscopy with a powerful 7-Tesla magnet, Dr. Linker and his colleagues returned to the rodent EAE model, also finding increased sodium in the skin. Mass spectrometry findings were similar in other rodent autoimmune models, he said. The differences were not seen for sodium in other organs, or for potassium levels in the skin.
“The most difficult point,” Dr. Linker said, is “can we use this therapeutically somehow? Of course, you can put your patients on a salt-free or very low-salt diet, but it’s not very tasty, of course, and adherence would be probably very, very low.”
The microbiome may play a modulating role that adds to the sodium-MS story and provides a potential therapeutic option. In mice, a high-salt diet was associated with marked and rapid depletion of Lactobacillus species in the mouse gut microbiome. In healthy humans as well, the drop in lactobacilli was quick and profound when 6 g/day of salt was added to the diet, Dr. Linker said (P = .0053 versus the control diet of 2-4 g sodium/day).
Working backward with the same healthy cohort, repletion of Lactobacillus by probiotic supplementation normalized systolic blood pressure, which had become elevated with increased dietary sodium. Further, Lactobacillus repletion downregulated Th17 cells to levels seen before the high-sodium diet, even when dietary sodium stayed high.
“This was even transferred to multiple sclerosis,” in work recently published by another group, Dr. Linker said. For patients with MS who consumed a Lactobacillus-containing probiotic, investigators could “clearly show, besides effects on the microbiome itself, that there were effects on antigen-presenting cells in MS patients.” Intermediate monocytes decreased, as did dendritic cells, in the small study that involved both healthy controls and MS patients who received a probiotic and then underwent a washout period. Stool and blood samples were collected in both groups to compare values with and without probiotic administration.
A question from the audience looked back at historic data: 100 or more years ago, salt was used extensively for food preservation in many parts of the world, so dietary sodium intake is thought to have been higher. The incidence of MS, though, was lower then. Dr. Linker pointed out that food preservation practices varied widely, and that a host of other variables make assessment of past or present associations difficult. “It’s hard to argue that salt is the one and only risk factor; I would strongly doubt that.”
Still, he said, this early work invites more study, with a target of establishing whether probiotic supplementation could be used as “add-on therapy to established immune drugs.”
Dr. Linker has received honoraria and research support from Bayer, Biogen, Genzyme, Merck Serono, Novartis, and TEVA.
SOURCE: Linker R. ECTRIMS 2018, Scientific Session 7.
BERLIN – Among a host of potential risk factors for multiple sclerosis (MS), one emerging risk factor – dietary sodium – has accumulating evidence, bolstered by new imaging techniques and emerging research about the mediating effect of the gut microbiome.
“The word is still out on salt – there’s still some work to do; we are not where we stand with smoking or obesity” and the association with MS, said Ralf Linker, MD, speaking at the annual congress of the European Committee for Treatment and Research in Multiple Sclerosis.
For all potential emerging risk factors for MS, there’s an attractive hypothesis and, often, epidemiologic data, Dr. Linker said. “There are probably good [epidemiologic] data in multiple sclerosis for vitamin D, smoking, obesity, and probably also alcohol,” he said. “The therapeutic consequence, however, is much less clear, the best example of that being, of course, vitamin D.”
“The attractive risk factor is not enough to be a hypothesis, although some people seem to believe that nowadays,” said Dr. Linker, chair of the department of neurology at Friedrich-Alexander University, Erlangen, Germany. “Probably it’s better to start with some basic science and some experimental data to get an idea of the mechanism.”
“Today, we need clear associations with clear markers, well-defined cohorts, and proper epidemiological data telling us whether this is a real risk factor. ... If you look at the clinicians – and there are many among us in the room here – your ultimate goal, of course, is to use this as an intervention.”
For salt intake, there’s a clear overlap between high salt consumption in Westernized diets and increasing incidence of MS. The association also holds for many other autoimmune diseases, Dr. Linker added.
“The next step is experimental evidence,” Dr. Linker said. In a rodent model of experimental autoimmune encephalomyelitis (EAE), rats with high salt intake had a worse clinical course, compared with control rats fed a usual diet (Nature. 2013 Apr 25;496[7446]:518-22).
“There were a lot of follow-up studies on that,” with identification of multiple immune cells that are up- or down-regulated via distinct pathways in a high-salt environment, Dr. Linker said.
More recently, Dr. Linker was a coinvestigator in work showing that healthy humans placed on a high-salt diet had significant increases in T-helper 17 (Th17) cells after just 2 weeks of an additional 6 g of table salt daily over a baseline 2-4 g/day (Nature. 2017 Nov 30;551[7682]:585-9).
“You can also translate it to a more realistic setting,” where individuals who ate fast food four or more times weekly had significantly higher Th17 cell counts than did those who ate less fast food, he noted in reference to unpublished data.
Looking specifically at MS, a single-center study found that increased sodium intake correlated with increased MS clinical disease activity, with the highest sodium intake (more than 4.8 g/day) associated with higher incidence of MS exacerbations. Those in the highest tier of sodium intake also had a higher lesion load, with 3.65 more T2 lesions seen on MRI scans for each gram of salt consumed above average amounts of 2-4.8 g/day (J Neurol Neurosurg Psychiatry. 2015 Jan;86[1]:26-31).
On the other hand, Dr. Linker said, “There have been recent very well-conducted studies in very well-defined cohorts casting doubt on this translation to multiple sclerosis.” In particular, an examination of data from over 70,000 participants in the Nurse’s Health Study showed no association between MS risk and dietary salt assessed by a nutritional questionnaire (Neurology. 2017 Sep 26;89[13]:1322-9). “There was no hint that the diagnosis was linked in any way with salt exposure,” Dr. Linker said.
In the BENEFIT study, both a spot urine sample and a food questionnaire were used, and patients were grouped into quintiles of sodium intake. For demyelinating events and MS diagnosis, the curves for all quintiles were “completely overlapping,” with no sign of increased risk of MS with higher sodium intake (Ann Neurol. 2017;82:20-9).
An important caveat to the null findings in these analyses is the known poor agreement between self-report of salt intake and actual sodium load, Dr. Linker noted. Renal sodium excretion can vary widely despite fixed salt intake, so spot urine and even 24-hour urine collection don’t guarantee accuracy, he said, citing studies from space travel emulations that show wide day-to-day excursions in sodium excretion with a fixed diet.
A promising tool for accurate assessment of sodium load may be sodium-23 skin spectroscopy using MRI, because skin tissue binds sodium in a stable, nonosmotic fashion. Dr. Linker and his colleagues have recently found that skin sodium levels, measured at the calf, are higher in individuals with relapsing-remitting MS. “Indeed, the sodium level in the skin of the MS patients was significantly higher than in the controls” who did not have MS, he said of the study that matched 20 patients with MS with 20 healthy controls. The MRI studies were assessed by radiologists blinded to the disease status of participants.
The increase is seen in only free sodium and seen in skin, but not muscle tissue, Dr. Linker said.
Using MRI spectroscopy with a powerful 7-Tesla magnet, Dr. Linker and his colleagues returned to the rodent EAE model, also finding increased sodium in the skin. Mass spectrometry findings were similar in other rodent autoimmune models, he said. The differences were not seen for sodium in other organs, or for potassium levels in the skin.
“The most difficult point,” Dr. Linker said, is “can we use this therapeutically somehow? Of course, you can put your patients on a salt-free or very low-salt diet, but it’s not very tasty, of course, and adherence would be probably very, very low.”
The microbiome may play a modulating role that adds to the sodium-MS story and provides a potential therapeutic option. In mice, a high-salt diet was associated with marked and rapid depletion of Lactobacillus species in the mouse gut microbiome. In healthy humans as well, the drop in lactobacilli was quick and profound when 6 g/day of salt was added to the diet, Dr. Linker said (P = .0053 versus the control diet of 2-4 g sodium/day).
Working backward with the same healthy cohort, repletion of Lactobacillus by probiotic supplementation normalized systolic blood pressure, which had become elevated with increased dietary sodium. Further, Lactobacillus repletion downregulated Th17 cells to levels seen before the high-sodium diet, even when dietary sodium stayed high.
“This was even transferred to multiple sclerosis,” in work recently published by another group, Dr. Linker said. For patients with MS who consumed a Lactobacillus-containing probiotic, investigators could “clearly show, besides effects on the microbiome itself, that there were effects on antigen-presenting cells in MS patients.” Intermediate monocytes decreased, as did dendritic cells, in the small study that involved both healthy controls and MS patients who received a probiotic and then underwent a washout period. Stool and blood samples were collected in both groups to compare values with and without probiotic administration.
A question from the audience looked back at historic data: 100 or more years ago, salt was used extensively for food preservation in many parts of the world, so dietary sodium intake is thought to have been higher. The incidence of MS, though, was lower then. Dr. Linker pointed out that food preservation practices varied widely, and that a host of other variables make assessment of past or present associations difficult. “It’s hard to argue that salt is the one and only risk factor; I would strongly doubt that.”
Still, he said, this early work invites more study, with a target of establishing whether probiotic supplementation could be used as “add-on therapy to established immune drugs.”
Dr. Linker has received honoraria and research support from Bayer, Biogen, Genzyme, Merck Serono, Novartis, and TEVA.
SOURCE: Linker R. ECTRIMS 2018, Scientific Session 7.
EXPERT ANALYSIS FROM ECTRIMS 2018
Instructional video for fourth-degree obstetric laceration repair using modified beef tongue model

Visit the Society of Gynecologic Surgeons online: sgsonline.org
Additional videos from SGS are available here, including these recent offerings:
- The art of manipulation: Simplifying hysterectomy by preparing the learner
- Vaginal and bilateral thigh removal of a transobturator sling
- Morcellation at the time of vaginal hysterectomy
Share your thoughts! Send your Letter to the Editor to rbarbieri@mdedge.com. Please include your name and the city and state in which you practice.

Visit the Society of Gynecologic Surgeons online: sgsonline.org
Additional videos from SGS are available here, including these recent offerings:
- The art of manipulation: Simplifying hysterectomy by preparing the learner
- Vaginal and bilateral thigh removal of a transobturator sling
- Morcellation at the time of vaginal hysterectomy
Share your thoughts! Send your Letter to the Editor to rbarbieri@mdedge.com. Please include your name and the city and state in which you practice.

Visit the Society of Gynecologic Surgeons online: sgsonline.org
Additional videos from SGS are available here, including these recent offerings:
- The art of manipulation: Simplifying hysterectomy by preparing the learner
- Vaginal and bilateral thigh removal of a transobturator sling
- Morcellation at the time of vaginal hysterectomy
Share your thoughts! Send your Letter to the Editor to rbarbieri@mdedge.com. Please include your name and the city and state in which you practice.
This video is brought to you by
Study investigates statin-diabetes link
LOS ANGELES – On any given day, type “statins” in the subject line of your favorite search engine and many results are likely to focus on risks: some based on science, others not so much.
“There is all kind of misinformation that are preventing people from taking statins,” Joshua W. Knowles, MD, said at the World Congress on Insulin Resistance, Diabetes & Cardiovascular Disease. “The most important side effects of statins are the increased lifespan and decreased risk of heart attacks, but that’s not what our patients are telling us. One of the things that is true is that .”
In 2016, Dr. Knowles, a cardiologist at the Stanford (Calif.) Center for Inherited Cardiovascular Disease, coauthored a retrospective analysis of data from subjects without diabetes in the Treating to New Targets (TNT) and the Stroke Prevention by Aggressive Reduction in Cholesterol Levels (SPARCL) randomized controlled trials (Am J Cardiol 2016;118[9]:1275-81). The authors found that statins particularly increase the risk of type 2 diabetes in those with prediabetes and insulin resistance. “That’s a risk group that we are all treating,” he said. “But that still doesn’t answer the question as to why this happens. Is this because statins increase insulin resistance, because they decrease beta cell function, or because they increase insulin clearance rate?”
In an effort to find out, Dr. Knowles and his colleagues have launched a clinical trial entitled “Relationship Between Insulin Resistance and Statin Induced Type 2 Diabetes, and Integrative Personal Omics Profiling” (NCT 02437084). Candidates do not have diabetes, yet qualify for statin therapy because they have a greater than 7.5% risk of cardiovascular disease over 10 years. To date, the researchers have enrolled 74 patients: 42 to the insulin-sensitive group (defined as having an LDL above 130 mg/dL and a triglyceride level below 150 mg/dL) and 11 to the insulin-resistant group (defined as having an LDL of 130 mg/dL or greater and a triglyceride level of 150 mg/dL or greater). Dr. Knowles said that about two-thirds of patients have been recruited and that full results are expected in late 2019.
At baseline, subjects underwent the insulin suppression test, the graded glucose infusion test, metabolic characterization, and integrated personal omics profiling (iPOP), a monitoring method. After 3 months of atorvastatin therapy 40 mg/day, the researchers repeated these measures and compared the results between groups. “Basically we were looking for changes in insulin resistance, secretion, and clearance between those groups over time,” said Dr. Knowles, who is the study’s principal investigator.
Of the 74 subjects, 13 decided that they did not want to participate and 6 are still undergoing baseline tests. In all, 55 started statin therapy, and 2 have dropped out. This left 42 in the low-triglyceride group and 11 in the high-triglyceride group.
The average age of the 52 individuals who have completed the study so far is 61 years, 30 are male, 35 are non-Hispanic white, their mean body mass index was 27.9 kg/m2, and their mean blood pressure was 127/79 mm Hg. By the end of statin therapy, body mass index did not change, but total cholesterol fell from a median of 234 mg/dL to a median of 150 mg/dL, triglycerides fell from a median of 109 mg/dL to a median of 78 mg/dL, LDL cholesterol fell from a median of 153 mg/dL to a median of 71 mg/dL, and mean high-sensitivity C-reactive protein dropped from a median of 1.2 mg/L to a median of 0.8 mg/L. All differences were statistically significant.
Fasting glucose levels have been completed on only 35 patients. “Two-hour glucose is going up, but it’s not yet significant, and on the oral glucose tolerance test, the curves are separating slightly but are not yet significant,” Dr. Knowles said.
On average, insulin resistance among the 35 patients worsened slightly, from 156 mg/dL before statin therapy to 170 mg/dL after initiation. “This is nominally significant (P = 0.03), and we’ll have to see if this holds up over time,” he said. The researchers also observed that statin use was associated with slight decreases in insulin secretion and clearance. Dr. Knowles emphasized that these are preliminary results and need to be further validated.
The study is funded by the Doris Duke Charitable Foundation. Dr. Knowles reported having no disclosures.
LOS ANGELES – On any given day, type “statins” in the subject line of your favorite search engine and many results are likely to focus on risks: some based on science, others not so much.
“There is all kind of misinformation that are preventing people from taking statins,” Joshua W. Knowles, MD, said at the World Congress on Insulin Resistance, Diabetes & Cardiovascular Disease. “The most important side effects of statins are the increased lifespan and decreased risk of heart attacks, but that’s not what our patients are telling us. One of the things that is true is that .”
In 2016, Dr. Knowles, a cardiologist at the Stanford (Calif.) Center for Inherited Cardiovascular Disease, coauthored a retrospective analysis of data from subjects without diabetes in the Treating to New Targets (TNT) and the Stroke Prevention by Aggressive Reduction in Cholesterol Levels (SPARCL) randomized controlled trials (Am J Cardiol 2016;118[9]:1275-81). The authors found that statins particularly increase the risk of type 2 diabetes in those with prediabetes and insulin resistance. “That’s a risk group that we are all treating,” he said. “But that still doesn’t answer the question as to why this happens. Is this because statins increase insulin resistance, because they decrease beta cell function, or because they increase insulin clearance rate?”
In an effort to find out, Dr. Knowles and his colleagues have launched a clinical trial entitled “Relationship Between Insulin Resistance and Statin Induced Type 2 Diabetes, and Integrative Personal Omics Profiling” (NCT 02437084). Candidates do not have diabetes, yet qualify for statin therapy because they have a greater than 7.5% risk of cardiovascular disease over 10 years. To date, the researchers have enrolled 74 patients: 42 to the insulin-sensitive group (defined as having an LDL above 130 mg/dL and a triglyceride level below 150 mg/dL) and 11 to the insulin-resistant group (defined as having an LDL of 130 mg/dL or greater and a triglyceride level of 150 mg/dL or greater). Dr. Knowles said that about two-thirds of patients have been recruited and that full results are expected in late 2019.
At baseline, subjects underwent the insulin suppression test, the graded glucose infusion test, metabolic characterization, and integrated personal omics profiling (iPOP), a monitoring method. After 3 months of atorvastatin therapy 40 mg/day, the researchers repeated these measures and compared the results between groups. “Basically we were looking for changes in insulin resistance, secretion, and clearance between those groups over time,” said Dr. Knowles, who is the study’s principal investigator.
Of the 74 subjects, 13 decided that they did not want to participate and 6 are still undergoing baseline tests. In all, 55 started statin therapy, and 2 have dropped out. This left 42 in the low-triglyceride group and 11 in the high-triglyceride group.
The average age of the 52 individuals who have completed the study so far is 61 years, 30 are male, 35 are non-Hispanic white, their mean body mass index was 27.9 kg/m2, and their mean blood pressure was 127/79 mm Hg. By the end of statin therapy, body mass index did not change, but total cholesterol fell from a median of 234 mg/dL to a median of 150 mg/dL, triglycerides fell from a median of 109 mg/dL to a median of 78 mg/dL, LDL cholesterol fell from a median of 153 mg/dL to a median of 71 mg/dL, and mean high-sensitivity C-reactive protein dropped from a median of 1.2 mg/L to a median of 0.8 mg/L. All differences were statistically significant.
Fasting glucose levels have been completed on only 35 patients. “Two-hour glucose is going up, but it’s not yet significant, and on the oral glucose tolerance test, the curves are separating slightly but are not yet significant,” Dr. Knowles said.
On average, insulin resistance among the 35 patients worsened slightly, from 156 mg/dL before statin therapy to 170 mg/dL after initiation. “This is nominally significant (P = 0.03), and we’ll have to see if this holds up over time,” he said. The researchers also observed that statin use was associated with slight decreases in insulin secretion and clearance. Dr. Knowles emphasized that these are preliminary results and need to be further validated.
The study is funded by the Doris Duke Charitable Foundation. Dr. Knowles reported having no disclosures.
LOS ANGELES – On any given day, type “statins” in the subject line of your favorite search engine and many results are likely to focus on risks: some based on science, others not so much.
“There is all kind of misinformation that are preventing people from taking statins,” Joshua W. Knowles, MD, said at the World Congress on Insulin Resistance, Diabetes & Cardiovascular Disease. “The most important side effects of statins are the increased lifespan and decreased risk of heart attacks, but that’s not what our patients are telling us. One of the things that is true is that .”
In 2016, Dr. Knowles, a cardiologist at the Stanford (Calif.) Center for Inherited Cardiovascular Disease, coauthored a retrospective analysis of data from subjects without diabetes in the Treating to New Targets (TNT) and the Stroke Prevention by Aggressive Reduction in Cholesterol Levels (SPARCL) randomized controlled trials (Am J Cardiol 2016;118[9]:1275-81). The authors found that statins particularly increase the risk of type 2 diabetes in those with prediabetes and insulin resistance. “That’s a risk group that we are all treating,” he said. “But that still doesn’t answer the question as to why this happens. Is this because statins increase insulin resistance, because they decrease beta cell function, or because they increase insulin clearance rate?”
In an effort to find out, Dr. Knowles and his colleagues have launched a clinical trial entitled “Relationship Between Insulin Resistance and Statin Induced Type 2 Diabetes, and Integrative Personal Omics Profiling” (NCT 02437084). Candidates do not have diabetes, yet qualify for statin therapy because they have a greater than 7.5% risk of cardiovascular disease over 10 years. To date, the researchers have enrolled 74 patients: 42 to the insulin-sensitive group (defined as having an LDL above 130 mg/dL and a triglyceride level below 150 mg/dL) and 11 to the insulin-resistant group (defined as having an LDL of 130 mg/dL or greater and a triglyceride level of 150 mg/dL or greater). Dr. Knowles said that about two-thirds of patients have been recruited and that full results are expected in late 2019.
At baseline, subjects underwent the insulin suppression test, the graded glucose infusion test, metabolic characterization, and integrated personal omics profiling (iPOP), a monitoring method. After 3 months of atorvastatin therapy 40 mg/day, the researchers repeated these measures and compared the results between groups. “Basically we were looking for changes in insulin resistance, secretion, and clearance between those groups over time,” said Dr. Knowles, who is the study’s principal investigator.
Of the 74 subjects, 13 decided that they did not want to participate and 6 are still undergoing baseline tests. In all, 55 started statin therapy, and 2 have dropped out. This left 42 in the low-triglyceride group and 11 in the high-triglyceride group.
The average age of the 52 individuals who have completed the study so far is 61 years, 30 are male, 35 are non-Hispanic white, their mean body mass index was 27.9 kg/m2, and their mean blood pressure was 127/79 mm Hg. By the end of statin therapy, body mass index did not change, but total cholesterol fell from a median of 234 mg/dL to a median of 150 mg/dL, triglycerides fell from a median of 109 mg/dL to a median of 78 mg/dL, LDL cholesterol fell from a median of 153 mg/dL to a median of 71 mg/dL, and mean high-sensitivity C-reactive protein dropped from a median of 1.2 mg/L to a median of 0.8 mg/L. All differences were statistically significant.
Fasting glucose levels have been completed on only 35 patients. “Two-hour glucose is going up, but it’s not yet significant, and on the oral glucose tolerance test, the curves are separating slightly but are not yet significant,” Dr. Knowles said.
On average, insulin resistance among the 35 patients worsened slightly, from 156 mg/dL before statin therapy to 170 mg/dL after initiation. “This is nominally significant (P = 0.03), and we’ll have to see if this holds up over time,” he said. The researchers also observed that statin use was associated with slight decreases in insulin secretion and clearance. Dr. Knowles emphasized that these are preliminary results and need to be further validated.
The study is funded by the Doris Duke Charitable Foundation. Dr. Knowles reported having no disclosures.
REPORTING FROM WCIRDC 2018
Should metabolic syndrome be renamed circadian syndrome?
LOS ANGELES – In the opinion of Paul Zimmet, MD, PhD, the
This scenario created the “perfect storm” for rising rates of metabolic syndrome, which is related to low HDL cholesterol levels, central obesity, hypertension, hyperglycemia, and high triglyceride levels, Dr. Zimmet said at the World Congress on Insulin Resistance, Diabetes & Cardiovascular Disease. These cardiometabolic risk factors “all seem to cluster together in relation to the changes in our society,” he said. “It’s on that basis and research findings that I think we should understand that most of them, if not all, have been demonstrated to relate to circadian rhythm disturbance.”
In fact, the associated comorbidities sleep apnea, depression, and fatty liver disease should be included in the metabolic syndrome cluster and should be renamed the “circadian syndrome,” according to Dr. Zimmet, professor of diabetes at Monash University, Melbourne.
The term metabolic syndrome is anathema, he said. “There have been numerous different definitions, which finally led to an effort to come up with a harmonized definition” by the International Diabetes Federation Task Force on Epidemiology and Prevention, with involvement from the American Heart Association (Circulation 2009;120[16]:1640-5).
In the early 1970s, Dr. Zimmet and his colleagues at Guys Hospital in London reported on diurnal variation in glucose tolerance. “If you did a glucose tolerance test in the afternoon it could be diabetic, whereas in the morning it was normal,” he noted. “Other researchers reported similar findings. That created in my own mind interest in this area of circadian rhythm. However, I had neglected this until recently, when I was doing background research while trying to find an answer to the elusive question of a central uniting explanation for the cardiometabolic cluster constituting the metabolic syndrome.” So decades later, Dr. Zimmet extended his research to include epigenetics in the quest. Described as the study of heritable changes in gene function that occur without a change in the sequence of the DNA, epigenetic changes “are closely linked to the circadian rhythm, otherwise known as ‘the body clock,’ ” said Dr. Zimmet, who also is codirector with Naftali Stern, MD, of the Sagol Center for Epigenetics of Metabolism and Aging at Tel Aviv Medical Center. “Many aspects of human behavior and metabolism are closely linked to the circadian clock and affected by its rhythm disturbance. We decided that we wanted to further investigate this area: To what extent is circadian rhythm the central feature to explain the clustering of all of these cardiovascular and metabolic risk factors of the metabolic syndrome.”
In recent years, he has been collaborating with Noga Kronfeld-Schor, PhD, of the department of zoology at Tel Aviv (Israel) University. The research focuses on a gerbil from the Negev: Psammomys obesus (otherwise known as the Israeli fat sand rat), which develops elevated blood sugar, obesity, depression, sleep disturbance, fatty liver, and circadian dysrhythmia when removed from the desert environment to the laboratory. “These are all key features of type 2 diabetes in humans,” he said. “This is probably the best animal model of type 2 diabetes, and we felt that it was worth looking more closely to see if there was a similar relationship in humans as to whether circadian dysrhythmia would be causing all or most of these features in humans including obesity.” An epigenetic study of the gerbil in the laboratory of Prof. Sam El-Osta at Monash has shown that parental diet during early life regulated expression of genes associated with DNA methylation in the key FTO gene associated with obesity (Int J Obesity 2016;40:1079-88). It suggests that diet-induced metabolic changes can be transmitted from parent to offspring by mechanisms under epigenetic control.
Published studies from other research groups support the link between other of the cardiometabolic metabolic syndrome characteristics, epigenetic modifications, and circadian dysrhythmia including cardiovascular regulation and disease (Eur Heart J 2018;39[14]:2326-9), sleep loss and alterations in DNA methylation (Science Advances 2018;4[8]:eaar8590), and circadian dysrhythmia and fatty liver (Cell Metab 2012;15[6]:848-60). “In 2009, the FDA approved bromocriptine mesylate, a drug which has effects on circadian rhythm, for treatment of type 2 diabetes, suggesting its use in diabetes may have some role through the alteration of circadian rhythm,” continued Dr. Zimmet, who also is honorary president of the International Diabetes Federation. “Depression is also clearly linked to circadian rhythm and there is evidence from research and human studies that light therapy may be an effective treatment for type 2 diabetes and depression.”
Dr. Zimmet ended his presentation with a strong call for adding sleep apnea, fatty liver, and depression to the existing features of the metabolic syndrome “to encourage clinicians and researchers look at the picture of cardiometabolic risk much more broadly than as just a group of metabolic abnormalities,” he said. “We propose that these comorbidities be embraced within the definition of the cardiometabolic cluster and be renamed the ‘circadian syndrome.’ This cluster is now the main driver of the global chronic disease epidemic and its health burden. This is a disease of civilization – the result of the way we live.”
Dr. Zimmet reported having no disclosures.
LOS ANGELES – In the opinion of Paul Zimmet, MD, PhD, the
This scenario created the “perfect storm” for rising rates of metabolic syndrome, which is related to low HDL cholesterol levels, central obesity, hypertension, hyperglycemia, and high triglyceride levels, Dr. Zimmet said at the World Congress on Insulin Resistance, Diabetes & Cardiovascular Disease. These cardiometabolic risk factors “all seem to cluster together in relation to the changes in our society,” he said. “It’s on that basis and research findings that I think we should understand that most of them, if not all, have been demonstrated to relate to circadian rhythm disturbance.”
In fact, the associated comorbidities sleep apnea, depression, and fatty liver disease should be included in the metabolic syndrome cluster and should be renamed the “circadian syndrome,” according to Dr. Zimmet, professor of diabetes at Monash University, Melbourne.
The term metabolic syndrome is anathema, he said. “There have been numerous different definitions, which finally led to an effort to come up with a harmonized definition” by the International Diabetes Federation Task Force on Epidemiology and Prevention, with involvement from the American Heart Association (Circulation 2009;120[16]:1640-5).
In the early 1970s, Dr. Zimmet and his colleagues at Guys Hospital in London reported on diurnal variation in glucose tolerance. “If you did a glucose tolerance test in the afternoon it could be diabetic, whereas in the morning it was normal,” he noted. “Other researchers reported similar findings. That created in my own mind interest in this area of circadian rhythm. However, I had neglected this until recently, when I was doing background research while trying to find an answer to the elusive question of a central uniting explanation for the cardiometabolic cluster constituting the metabolic syndrome.” So decades later, Dr. Zimmet extended his research to include epigenetics in the quest. Described as the study of heritable changes in gene function that occur without a change in the sequence of the DNA, epigenetic changes “are closely linked to the circadian rhythm, otherwise known as ‘the body clock,’ ” said Dr. Zimmet, who also is codirector with Naftali Stern, MD, of the Sagol Center for Epigenetics of Metabolism and Aging at Tel Aviv Medical Center. “Many aspects of human behavior and metabolism are closely linked to the circadian clock and affected by its rhythm disturbance. We decided that we wanted to further investigate this area: To what extent is circadian rhythm the central feature to explain the clustering of all of these cardiovascular and metabolic risk factors of the metabolic syndrome.”
In recent years, he has been collaborating with Noga Kronfeld-Schor, PhD, of the department of zoology at Tel Aviv (Israel) University. The research focuses on a gerbil from the Negev: Psammomys obesus (otherwise known as the Israeli fat sand rat), which develops elevated blood sugar, obesity, depression, sleep disturbance, fatty liver, and circadian dysrhythmia when removed from the desert environment to the laboratory. “These are all key features of type 2 diabetes in humans,” he said. “This is probably the best animal model of type 2 diabetes, and we felt that it was worth looking more closely to see if there was a similar relationship in humans as to whether circadian dysrhythmia would be causing all or most of these features in humans including obesity.” An epigenetic study of the gerbil in the laboratory of Prof. Sam El-Osta at Monash has shown that parental diet during early life regulated expression of genes associated with DNA methylation in the key FTO gene associated with obesity (Int J Obesity 2016;40:1079-88). It suggests that diet-induced metabolic changes can be transmitted from parent to offspring by mechanisms under epigenetic control.
Published studies from other research groups support the link between other of the cardiometabolic metabolic syndrome characteristics, epigenetic modifications, and circadian dysrhythmia including cardiovascular regulation and disease (Eur Heart J 2018;39[14]:2326-9), sleep loss and alterations in DNA methylation (Science Advances 2018;4[8]:eaar8590), and circadian dysrhythmia and fatty liver (Cell Metab 2012;15[6]:848-60). “In 2009, the FDA approved bromocriptine mesylate, a drug which has effects on circadian rhythm, for treatment of type 2 diabetes, suggesting its use in diabetes may have some role through the alteration of circadian rhythm,” continued Dr. Zimmet, who also is honorary president of the International Diabetes Federation. “Depression is also clearly linked to circadian rhythm and there is evidence from research and human studies that light therapy may be an effective treatment for type 2 diabetes and depression.”
Dr. Zimmet ended his presentation with a strong call for adding sleep apnea, fatty liver, and depression to the existing features of the metabolic syndrome “to encourage clinicians and researchers look at the picture of cardiometabolic risk much more broadly than as just a group of metabolic abnormalities,” he said. “We propose that these comorbidities be embraced within the definition of the cardiometabolic cluster and be renamed the ‘circadian syndrome.’ This cluster is now the main driver of the global chronic disease epidemic and its health burden. This is a disease of civilization – the result of the way we live.”
Dr. Zimmet reported having no disclosures.
LOS ANGELES – In the opinion of Paul Zimmet, MD, PhD, the
This scenario created the “perfect storm” for rising rates of metabolic syndrome, which is related to low HDL cholesterol levels, central obesity, hypertension, hyperglycemia, and high triglyceride levels, Dr. Zimmet said at the World Congress on Insulin Resistance, Diabetes & Cardiovascular Disease. These cardiometabolic risk factors “all seem to cluster together in relation to the changes in our society,” he said. “It’s on that basis and research findings that I think we should understand that most of them, if not all, have been demonstrated to relate to circadian rhythm disturbance.”
In fact, the associated comorbidities sleep apnea, depression, and fatty liver disease should be included in the metabolic syndrome cluster and should be renamed the “circadian syndrome,” according to Dr. Zimmet, professor of diabetes at Monash University, Melbourne.
The term metabolic syndrome is anathema, he said. “There have been numerous different definitions, which finally led to an effort to come up with a harmonized definition” by the International Diabetes Federation Task Force on Epidemiology and Prevention, with involvement from the American Heart Association (Circulation 2009;120[16]:1640-5).
In the early 1970s, Dr. Zimmet and his colleagues at Guys Hospital in London reported on diurnal variation in glucose tolerance. “If you did a glucose tolerance test in the afternoon it could be diabetic, whereas in the morning it was normal,” he noted. “Other researchers reported similar findings. That created in my own mind interest in this area of circadian rhythm. However, I had neglected this until recently, when I was doing background research while trying to find an answer to the elusive question of a central uniting explanation for the cardiometabolic cluster constituting the metabolic syndrome.” So decades later, Dr. Zimmet extended his research to include epigenetics in the quest. Described as the study of heritable changes in gene function that occur without a change in the sequence of the DNA, epigenetic changes “are closely linked to the circadian rhythm, otherwise known as ‘the body clock,’ ” said Dr. Zimmet, who also is codirector with Naftali Stern, MD, of the Sagol Center for Epigenetics of Metabolism and Aging at Tel Aviv Medical Center. “Many aspects of human behavior and metabolism are closely linked to the circadian clock and affected by its rhythm disturbance. We decided that we wanted to further investigate this area: To what extent is circadian rhythm the central feature to explain the clustering of all of these cardiovascular and metabolic risk factors of the metabolic syndrome.”
In recent years, he has been collaborating with Noga Kronfeld-Schor, PhD, of the department of zoology at Tel Aviv (Israel) University. The research focuses on a gerbil from the Negev: Psammomys obesus (otherwise known as the Israeli fat sand rat), which develops elevated blood sugar, obesity, depression, sleep disturbance, fatty liver, and circadian dysrhythmia when removed from the desert environment to the laboratory. “These are all key features of type 2 diabetes in humans,” he said. “This is probably the best animal model of type 2 diabetes, and we felt that it was worth looking more closely to see if there was a similar relationship in humans as to whether circadian dysrhythmia would be causing all or most of these features in humans including obesity.” An epigenetic study of the gerbil in the laboratory of Prof. Sam El-Osta at Monash has shown that parental diet during early life regulated expression of genes associated with DNA methylation in the key FTO gene associated with obesity (Int J Obesity 2016;40:1079-88). It suggests that diet-induced metabolic changes can be transmitted from parent to offspring by mechanisms under epigenetic control.
Published studies from other research groups support the link between other of the cardiometabolic metabolic syndrome characteristics, epigenetic modifications, and circadian dysrhythmia including cardiovascular regulation and disease (Eur Heart J 2018;39[14]:2326-9), sleep loss and alterations in DNA methylation (Science Advances 2018;4[8]:eaar8590), and circadian dysrhythmia and fatty liver (Cell Metab 2012;15[6]:848-60). “In 2009, the FDA approved bromocriptine mesylate, a drug which has effects on circadian rhythm, for treatment of type 2 diabetes, suggesting its use in diabetes may have some role through the alteration of circadian rhythm,” continued Dr. Zimmet, who also is honorary president of the International Diabetes Federation. “Depression is also clearly linked to circadian rhythm and there is evidence from research and human studies that light therapy may be an effective treatment for type 2 diabetes and depression.”
Dr. Zimmet ended his presentation with a strong call for adding sleep apnea, fatty liver, and depression to the existing features of the metabolic syndrome “to encourage clinicians and researchers look at the picture of cardiometabolic risk much more broadly than as just a group of metabolic abnormalities,” he said. “We propose that these comorbidities be embraced within the definition of the cardiometabolic cluster and be renamed the ‘circadian syndrome.’ This cluster is now the main driver of the global chronic disease epidemic and its health burden. This is a disease of civilization – the result of the way we live.”
Dr. Zimmet reported having no disclosures.
EXPERT ANALYSIS FROM THE WCIRDC 2018
Phone app diagnoses STEMI nearly as well as ECG
CHICAGO – A novel smartphone app performed nearly as well as a standard 12-lead ECG for diagnosis of ST-segment elevation MI (STEMI) in patients presenting with chest pain in ST LEUIS, an international, multicenter study.
“This study demonstrates that a 12-lead-equivalent ECG obtained using a smartphone coupled with a software application and inexpensive two-wire attachment can identify STEMI versus non-STEMI with an excellent correlation to a traditional 12-lead ECG. This technology holds substantial promise to improve outcomes in STEMI by enabling more rapid diagnosis and treatment anywhere in the world for inexpensive cost,” J. Brent Muhlestein, MD, said while presenting the ST LEUIS results at the American Heart Association scientific sessions.
This technology could provide a long-sought breakthrough in overcoming patient denial and motivating hard-headed individuals with a life-threatening MI to get to the hospital more quickly after symptom onset, instead of initially shrugging off the matter as indigestion or another nuisance. If individuals can use their handy cell phone or smartwatch to quickly obtain an ECG that shows they’re having a STEMI, they’re going to seek medical attention much sooner, with resultant greater salvage of heart muscle, noted Dr. Muhlestein of Intermountain Healthcare in Salt Lake City.
ST LEUIS tested whether a smartphone ECG app developed by AliveCor can accurately diagnose STEMI in patients with chest pain. The study, which took place at Intermountain Medical Center and a handful of other sites associated with the Duke University Cooperative Cardiovascular Society, included 204 patients who presented to EDs with chest pain. They simultaneously received both a standard 12-lead ECG and an ECG obtained using the AliveCor smartphone app. The matched ECG pairs were evaluated separately, both quantitatively and qualitatively, by a blinded panel of experienced cardiologists and classified as STEMI, left bundle branch block, non-STEMI, or uninterpretable. The study population included 92 patients with chest pain and activation of a STEMI protocol and 112 who came through the ED chest pain protocol.
Side-by-side ECG comparisons weren’t attempted in 14 pairs deemed not interpretable. In 13 cases this was because of technical problems with the smartphone ECG, and in the 14th because of ventricular pacing in the standard 12-lead ECG.
STEMI was diagnosed in 22.5% of the study population by 12-lead ECG and in 29.4% by smartphone app. The discrepancy was explained by small voltage differences in the ST-segment elevation which met criteria for STEMI by smartphone but not standard 12-lead ECG in 15 cases.
“It appears that the ST elevation was a little bit more obvious in the smartphone ECG,” Dr. Muhlestein observed.
Left bundle branch block was identified in 5.4% of patients by both methods.
The key performance numbers: The smartphone ECG had a sensitivity of 89%, specificity of 84%, positive predictive value of 70%, and negative predictive value of 95% for diagnosis of STEMI or left bundle branch block. The positive predictive value was diminished by the increased likelihood that the smartphone would call STEMI in discordant cases.
Dr. Muhlestein said that, despite the AliveCor device’s very good correlation with the standard 12-lead ECG, the system needs further tweaking.
“We definitely think this is not ready for prime time. Further refinements of the software and hardware may improve on our study results and broaden potential applications through increased ease of use and reliability. I’m sure smart engineers can make a much more simple, really user-friendly device now that we know it’s actually feasible. I envision a time when you turn it on and it speaks loud and tells you what to do and how to do it – like an AED [automated external defibrillator] – then uploads the ECG to the cloud, interprets it, and tells you whether you should go to the emergency department or not,” Dr. Muhlestein said.
This is a device that’s going to be a boon not only in the United States but also in developing countries, where even people living without electricity or running water often have cell phones, the cardiologist noted.
Dr. Muhlestein reported having no financial conflicts of interest regarding the study, which was sponsored by the participating medical institutions.
CHICAGO – A novel smartphone app performed nearly as well as a standard 12-lead ECG for diagnosis of ST-segment elevation MI (STEMI) in patients presenting with chest pain in ST LEUIS, an international, multicenter study.
“This study demonstrates that a 12-lead-equivalent ECG obtained using a smartphone coupled with a software application and inexpensive two-wire attachment can identify STEMI versus non-STEMI with an excellent correlation to a traditional 12-lead ECG. This technology holds substantial promise to improve outcomes in STEMI by enabling more rapid diagnosis and treatment anywhere in the world for inexpensive cost,” J. Brent Muhlestein, MD, said while presenting the ST LEUIS results at the American Heart Association scientific sessions.
This technology could provide a long-sought breakthrough in overcoming patient denial and motivating hard-headed individuals with a life-threatening MI to get to the hospital more quickly after symptom onset, instead of initially shrugging off the matter as indigestion or another nuisance. If individuals can use their handy cell phone or smartwatch to quickly obtain an ECG that shows they’re having a STEMI, they’re going to seek medical attention much sooner, with resultant greater salvage of heart muscle, noted Dr. Muhlestein of Intermountain Healthcare in Salt Lake City.
ST LEUIS tested whether a smartphone ECG app developed by AliveCor can accurately diagnose STEMI in patients with chest pain. The study, which took place at Intermountain Medical Center and a handful of other sites associated with the Duke University Cooperative Cardiovascular Society, included 204 patients who presented to EDs with chest pain. They simultaneously received both a standard 12-lead ECG and an ECG obtained using the AliveCor smartphone app. The matched ECG pairs were evaluated separately, both quantitatively and qualitatively, by a blinded panel of experienced cardiologists and classified as STEMI, left bundle branch block, non-STEMI, or uninterpretable. The study population included 92 patients with chest pain and activation of a STEMI protocol and 112 who came through the ED chest pain protocol.
Side-by-side ECG comparisons weren’t attempted in 14 pairs deemed not interpretable. In 13 cases this was because of technical problems with the smartphone ECG, and in the 14th because of ventricular pacing in the standard 12-lead ECG.
STEMI was diagnosed in 22.5% of the study population by 12-lead ECG and in 29.4% by smartphone app. The discrepancy was explained by small voltage differences in the ST-segment elevation which met criteria for STEMI by smartphone but not standard 12-lead ECG in 15 cases.
“It appears that the ST elevation was a little bit more obvious in the smartphone ECG,” Dr. Muhlestein observed.
Left bundle branch block was identified in 5.4% of patients by both methods.
The key performance numbers: The smartphone ECG had a sensitivity of 89%, specificity of 84%, positive predictive value of 70%, and negative predictive value of 95% for diagnosis of STEMI or left bundle branch block. The positive predictive value was diminished by the increased likelihood that the smartphone would call STEMI in discordant cases.
Dr. Muhlestein said that, despite the AliveCor device’s very good correlation with the standard 12-lead ECG, the system needs further tweaking.
“We definitely think this is not ready for prime time. Further refinements of the software and hardware may improve on our study results and broaden potential applications through increased ease of use and reliability. I’m sure smart engineers can make a much more simple, really user-friendly device now that we know it’s actually feasible. I envision a time when you turn it on and it speaks loud and tells you what to do and how to do it – like an AED [automated external defibrillator] – then uploads the ECG to the cloud, interprets it, and tells you whether you should go to the emergency department or not,” Dr. Muhlestein said.
This is a device that’s going to be a boon not only in the United States but also in developing countries, where even people living without electricity or running water often have cell phones, the cardiologist noted.
Dr. Muhlestein reported having no financial conflicts of interest regarding the study, which was sponsored by the participating medical institutions.
CHICAGO – A novel smartphone app performed nearly as well as a standard 12-lead ECG for diagnosis of ST-segment elevation MI (STEMI) in patients presenting with chest pain in ST LEUIS, an international, multicenter study.
“This study demonstrates that a 12-lead-equivalent ECG obtained using a smartphone coupled with a software application and inexpensive two-wire attachment can identify STEMI versus non-STEMI with an excellent correlation to a traditional 12-lead ECG. This technology holds substantial promise to improve outcomes in STEMI by enabling more rapid diagnosis and treatment anywhere in the world for inexpensive cost,” J. Brent Muhlestein, MD, said while presenting the ST LEUIS results at the American Heart Association scientific sessions.
This technology could provide a long-sought breakthrough in overcoming patient denial and motivating hard-headed individuals with a life-threatening MI to get to the hospital more quickly after symptom onset, instead of initially shrugging off the matter as indigestion or another nuisance. If individuals can use their handy cell phone or smartwatch to quickly obtain an ECG that shows they’re having a STEMI, they’re going to seek medical attention much sooner, with resultant greater salvage of heart muscle, noted Dr. Muhlestein of Intermountain Healthcare in Salt Lake City.
ST LEUIS tested whether a smartphone ECG app developed by AliveCor can accurately diagnose STEMI in patients with chest pain. The study, which took place at Intermountain Medical Center and a handful of other sites associated with the Duke University Cooperative Cardiovascular Society, included 204 patients who presented to EDs with chest pain. They simultaneously received both a standard 12-lead ECG and an ECG obtained using the AliveCor smartphone app. The matched ECG pairs were evaluated separately, both quantitatively and qualitatively, by a blinded panel of experienced cardiologists and classified as STEMI, left bundle branch block, non-STEMI, or uninterpretable. The study population included 92 patients with chest pain and activation of a STEMI protocol and 112 who came through the ED chest pain protocol.
Side-by-side ECG comparisons weren’t attempted in 14 pairs deemed not interpretable. In 13 cases this was because of technical problems with the smartphone ECG, and in the 14th because of ventricular pacing in the standard 12-lead ECG.
STEMI was diagnosed in 22.5% of the study population by 12-lead ECG and in 29.4% by smartphone app. The discrepancy was explained by small voltage differences in the ST-segment elevation which met criteria for STEMI by smartphone but not standard 12-lead ECG in 15 cases.
“It appears that the ST elevation was a little bit more obvious in the smartphone ECG,” Dr. Muhlestein observed.
Left bundle branch block was identified in 5.4% of patients by both methods.
The key performance numbers: The smartphone ECG had a sensitivity of 89%, specificity of 84%, positive predictive value of 70%, and negative predictive value of 95% for diagnosis of STEMI or left bundle branch block. The positive predictive value was diminished by the increased likelihood that the smartphone would call STEMI in discordant cases.
Dr. Muhlestein said that, despite the AliveCor device’s very good correlation with the standard 12-lead ECG, the system needs further tweaking.
“We definitely think this is not ready for prime time. Further refinements of the software and hardware may improve on our study results and broaden potential applications through increased ease of use and reliability. I’m sure smart engineers can make a much more simple, really user-friendly device now that we know it’s actually feasible. I envision a time when you turn it on and it speaks loud and tells you what to do and how to do it – like an AED [automated external defibrillator] – then uploads the ECG to the cloud, interprets it, and tells you whether you should go to the emergency department or not,” Dr. Muhlestein said.
This is a device that’s going to be a boon not only in the United States but also in developing countries, where even people living without electricity or running water often have cell phones, the cardiologist noted.
Dr. Muhlestein reported having no financial conflicts of interest regarding the study, which was sponsored by the participating medical institutions.
REPORTING FROM THE AHA SCIENTIFIC SESSIONS
Key clinical point:
Major finding: The app, designed to diagnose ST-segment elevation MI, had a sensitivity of 89%, specificity of 84%, and negative predictive value of 95% for this purpose.
Study details: This multicenter, international study featured blinded expert side-by-side comparisons of standard 12-lead ECGs and ECGs obtained via a smartphone app in 204 patients who presented with chest pain.
Disclosures: The presenter reported having no financial conflicts of interest regarding the study, which was fully sponsored by the participating medical institutions.
Trends in Utilization of Total Hip Arthroplasty for Femoral Neck Fractures in the United States
ABSTRACT
The ideal mode of fixation for patients with femoral neck fractures is not well defined in the current literature. This study describes the recent trends in surgical management of femoral neck fractures with an analysis on perioperative outcomes.
The National Hospital Discharge Survey was used to identify femoral neck fractures in the United States between 1990 and 2007 (n = 1,155,960) treated with open reduction and internal fixation (ORIF), total hip arthroplasty (THA), or hemiarthroplasty (HA). Trends were examined over the following 3 time periods: 1990 to 1995 (group 1), 1996 to 2001 (group 2), and 2002 to 2007 (group 3). Elixhauser Comorbidity Index and perioperative complications were calculated.
Use of HA increased (74.4% to 84.6%), whereas that of THA (7.3% to 4.9%) and ORIF (18.3% to 10.6%) decreased, from group 1 to group 3 in the age group of >80 years. The use of ORIF increased (63.9% to 81.4%), whereas the use of both HA and THA decreased, from group 1 to group 3 in the age group of <50 years. The rate of adverse events increased across all fixation types but was greatest among THA (32.2% to 48.3%).
The femoral neck patient population is now older and has more medical comorbidities. We observed a trend toward performing HA in older patients and ORIF in younger patients. Despite superior functional outcomes reported in THA, this study found a decreased utilization of THA in all age groups along with an increase in adverse events and nonroutine discharges for patients with femoral neck fractures treated with THA.
Funding: This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Continue to: Femoral neck fractures...
Femoral neck fractures are a common occurrence in the United States. A recent study estimated an incidence of >63 per 100,000 population.1-8 Although the incidence appears to have decreased over recent decades, there is a projected exponential increase in the incidence of hip fractures over the next 30 years in the baby boomer population.8,9 Given that these fractures have a significant impact on patient morbidity, mortality, and quality of life, research efforts have been directed toward optimizing the treatment of affected patients and improving the outcomes.4,9-24
The treatment of choice for femoral neck fractures and the use of total hip arthroplasty (THA)11 have been a topic of debate.4,9,10,15-17,22,25 Total hip arthroplasty has been advocated for younger, more active patients, whereas hemiarthroplasty (HA) has been reserved for patients who are older and less active. Although several studies have demonstrated that arthroplasty outperforms open reduction and internal fixation (ORIF) in the elderly population with displaced femoral neck fractures, ORIF is still commonly performed in the United States for nondisplaced fractures and in patients aged <50 years.26-29
In an attempt to quantify the use of THA in the treatment of femoral neck fractures and demonstrate the national trends, Miller and colleagues5 pooled the American Board of Orthopaedic Surgery (ABOS) database and analyzed the treatment trends of surgeons taking part II of the ABOS examination from 1999 to 2011. The authors found an increased utilization of THA by recently graduated orthopedic surgeons. In contrast, Jain and colleagues30 found different national trends when they analyzed data from the National Inpatient Sample containing data between 1990 and 2001 and further found decreased utilization of THA procedures by orthopedic surgeons of all levels of training nationwide. However, neither of these studies reported about the trends in demographics, comorbidities, risk factors, or outcomes in this patient population following surgery.
The purpose of this study was to help clarify the findings of these authors using the largest dataset to date and also report on the perioperative complications associated with each mode of fixation in patients who undergo operative treatment for femoral neck fractures in the United States. Our hypotheses were that the femoral neck fracture patient population has become older and has more medical comorbidities. We also hypothesized that there has been a trend toward performing fewer THA procedures in the United States and that THA is associated with increased perioperative complications compared to those with HA and ORIF.
MATERIALS AND METHODS
We conducted a retrospective epidemiological study using the National Hospital Discharge Survey (NHDS) on surgical trends in the management of femoral neck fractures. The NHDS is a publicly available survey that is conducted annually to provide data of nonfederal, short-stay hospitals to the public. The sample data are weighted to provide nationwide estimates of annual inpatient care. The NHDS includes up to 7 medical diagnoses and 4 procedural codes per case, which are categorized using the International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) codes, that were collected along with patient demographic information, length of stay (LOS), and discharge disposition. The diagnostic and procedural codes used for this study are presented in the Appendix. The year 2007 was chosen as the endpoint of this study due to the fact that the relative standard error of the NHDS doubled in 2008 as a result of a decrease in its survey size. As this is a publicly available database, our study was exempt from institutional review board approval.
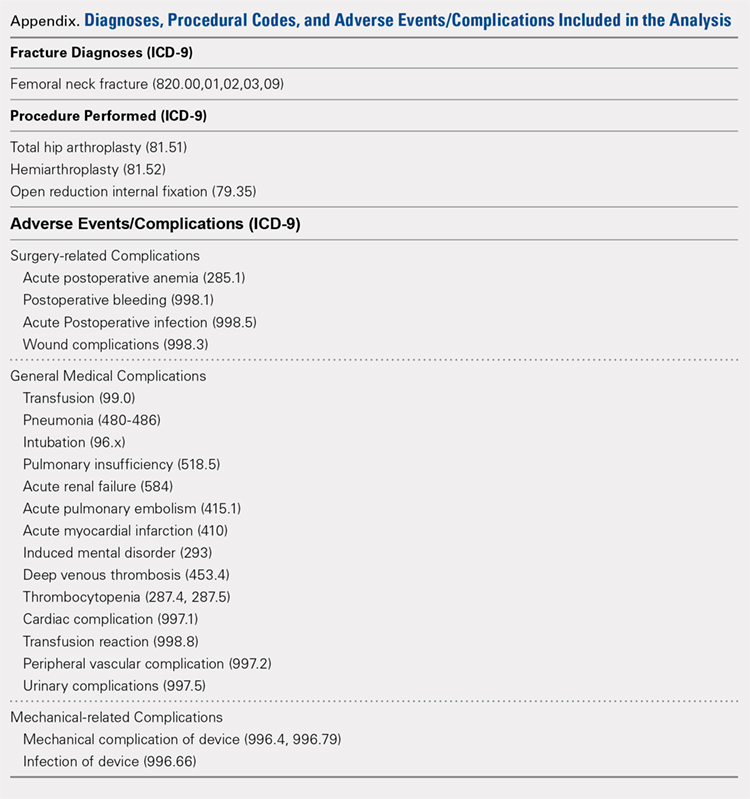

Continue to: All pateints admitted...
All patients admitted with a primary diagnosis of closed transcervical fracture of the femoral neck (ICD-9-CM 820.0x) were selected. This resulted in 1,674,160 fractures. All patients with fractures with a concurrent primary procedural code of ORIF (79.35), HA (81.52), or THA (81.51) were identified, resulting in a total sample size of 1,155,960 surgical fractures. Analysis of the fractures based on additional specificity,ie subcapital versus midcervical versus basicervical, was not carried out because >90% of femoral neck fractures in the database were coded as “unspecified” or “other” (ICD9 CM 820.00 and 820.09, respectively).
Comorbidity burden was quantified using Elixhauser coding algorithms as previously described.31 The Elixhauser comorbidity measure is a model consisting of 31 conditions and has recently been identified as a better predictor of mortality in patients undergoing orthopedic procedures when compared with the Charlson Comorbidity Index.31 Dichotomous variables for each Elixhauser comorbidity were created, and χ2 tests were utilized to assess the association between each comorbidity and mortality. The weighted Elixhauser score for each statistically significant comorbidity was calculated as described by van Walraven and colleagues.32 The Elixhauser comorbidity score was then calculated for each patient by summing the individual weights of all comorbidities. Postoperative adverse events were determined using the complication-screening-package as previously described.33
All adverse events were categorized into 3 categories, including general medical complications, mechanical complications, and surgical complications. All adverse events recorded in the NHDS database are events that occurred during a single hospitalization. Therefore, it does not take into account adverse events that occurred after discharge, and, for example, mortality refers to postoperative mortality that occurs prior to discharge. The study period comprised data captured from 1990 to 2007, and 3 groups were generated from this time period to better characterize patients throughout the large study time frame. Group 1 comprised patients who underwent surgical management of femoral neck fractures from 1990 to 1995, group 2 consisted of patients treated from 1996 to 2001, and group 3 included patients treated from 2002 to 2007.
Categorical data were analyzed using the χ2 test, and continuous data were analyzed by the independent-samples t test and ANOVA. Multivariable binary logistic regression analyses were performed to assess the contributions of individual comorbidities to mortality, adverse events, and nonroutine discharge. Elixhauser comorbidities with a P value of < .10 in the bivariate analysis and presenting in at least 0.2% of the population were included in the logistic regression.31 Odds ratios and confidence intervals were calculated to assess the association between comorbidities and our dichotomous variables. A P value of < .001 defined statistical significance.33 Statistical analysis was conducted using SPSS version 21 (IBM).
RESULTS
Patient Demographics
Our query demonstrated a total of 1,155,960 patients who underwent surgical fixation of femoral neck fractures (Table 1). The most commonly used treatment modality was HA (75%), followed by ORIF (18%) and later by THA (7%). The majority of patients were females in each treatment group. Patients’ age varied according to treatment group, with patients undergoing HA having a mean age of 81.0 ± 9.0 years, patients undergoing ORIF having a mean age of 75.0 ± 17.0 years, and those undergoing THA having a mean age of 79.0 ± 10.0 years (P < .001). The majority of patients were ≥80 years in all treatment groups, but the ORIF group had the greatest proportion of patients <65 years (P < .001). Among patients undergoing HA, 62.4% were ≥80 years, while the ORIF and HA groups consisted of 48.6% and 51.5% of patients in that same age group, respectively.
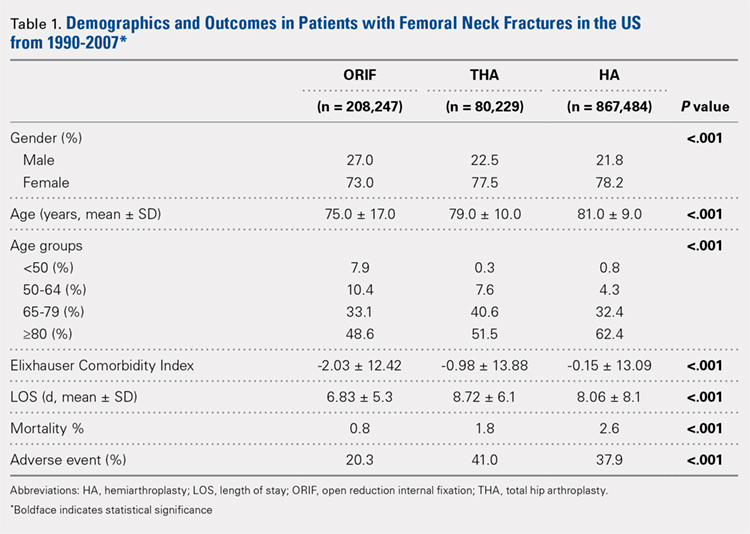
Continue to: TRENDS ANALYSIS
TRENDS ANALYSIS
There was a significant change in the distributions of the procedures performed according to age group over time. Patients >80 years continued to undergo primarily HA, with an increase from 74.4% during 1990 to 1995 up to 84.6% during the 2002 to 2007 period and a concomitant decrease in ORIF from 18.3% to 10.6% during the same time period in this age group. Surgical trends in patients 65 to 79 years demonstrated a significant decrease in management with ORIF from 19.1% in 1990 to 1995 to 16.8% in the 2002 to 2007 cohort (P < .001 for all, Table 2). There was an increase in the use of HA from 71.9% during the 1990 to 1995 period to 75.5% during the final study period (Table 2, Figure 1). The use of THA for all age groups decreased between 1990 and 2007, except for the 50- to 64-year-old group where THA utilization remained constant.
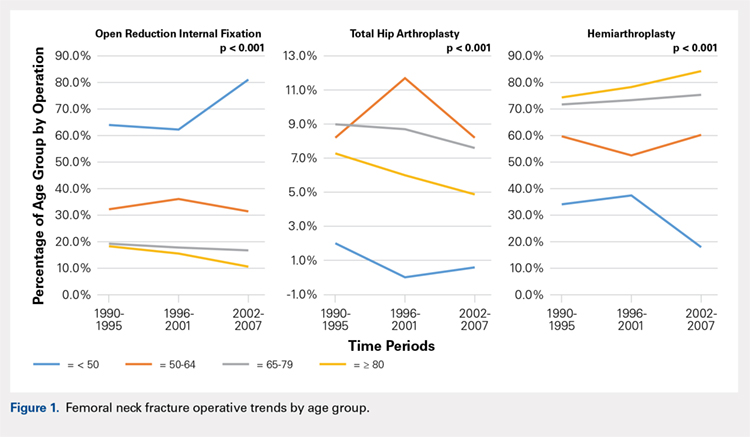
Management patterns in patients 50 to 64 years varied throughout the analysis and demonstrated the following trend: treatment with HA remained the most common technique used but varied slightly from 59.7% during 1990 to 1995 to 60.3% during 2002 to2007 (P < .001, Table 2). The second most common treatment used was ORIF, which decreased from 32.2% to 31.5% (P < .001, Table 2). The use of THA varied significantly from 8.2% among those managed during 1990 to 1995 to 11.7% during 1996 to 2001 but later declined to the initial 8.2% (P < .001, Table 2).
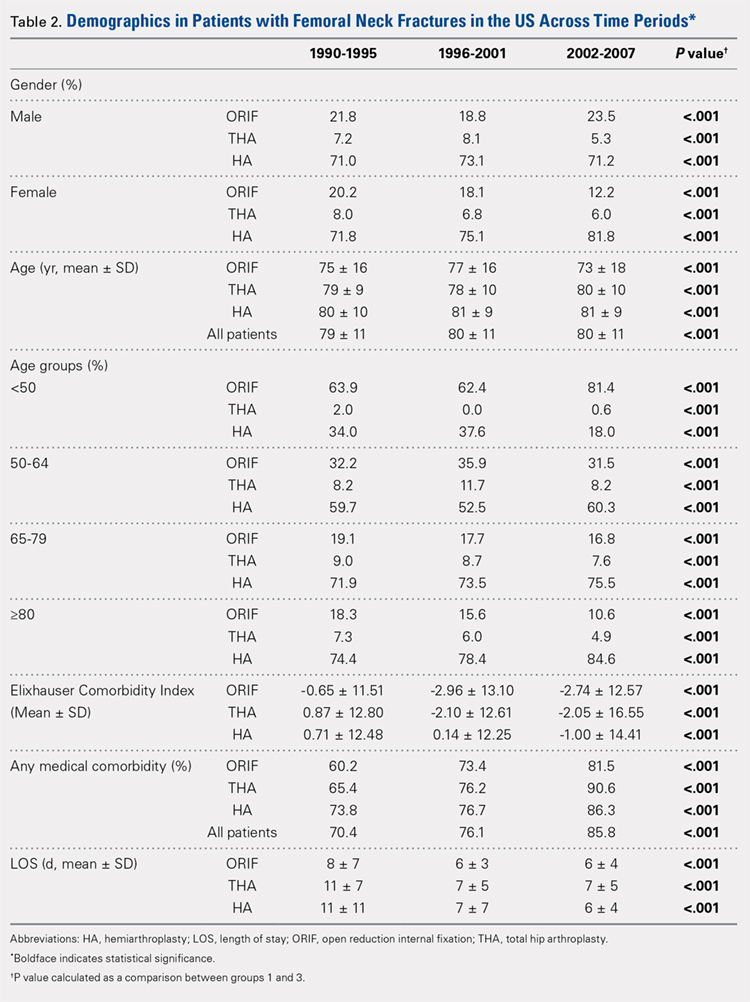
Analysis of patients ≤49 years demonstrated that ORIF was the preferred technique, which experienced a growth from 63.9% during 1990 to 1995 to 81.4% during the 2002 to 2007 period (P < .001, Table 2). A decreased use in THA was observed from 2.0% in the initial period to 0.6% in the final period (P < .001, Table 2). Use of HA decreased from 34.0% in 1990 to 1995 to 18.0% in 2002 to 2007 (P < .001, Table 2).
LENGTH OF STAY
Mean number of in-hospital days decreased throughout the study period for all treatment techniques. During the 1990 to 1995 study period, patients who underwent ORIF had a mean LOS of 8 ± 7 days, which decreased (P < .001, Table 2) to 6 ± 3 days in 1996 to 2001 and remained constant during 2002 to 2007 (mean 6 ± 4 days). This decrease in LOS was also observed in patients who underwent THA (P < .001, Table 2), who initially had a mean LOS of 11 ± 7 days during 1990 to 1995, which later decreased to 7 ± 5 days for the remainder of the study. The LOS for patients who underwent HA also decreased (P < .001, Table 2), which initially was reported to be 11 ± 11 days during 1990 to 1995, decreasing to 7 ±7 days in 1996–2001 and later to 6 ± 4 days in 2002 to 2007.
COMORBIDITIY ANALYSIS
The Elixhauser Comorbidity Index varied significantly among groups over time (P < .001, Table 2). Overall mean Elixhauser Comorbidity Index score per procedure type is provided in Table 1, with HA patients having the highest score (-0.15 ± 13.09, p<.001).
Continue to: Analysis of the preoperative comorbidities...
Analysis of the preoperative comorbidities demonstrated significant differences among each surgical treatment group (P < .001 for all, Table 3). The most common comorbidities in patients who underwent HA were uncomplicated hypertension (33.2%), fluid/electrolyte disorders (17.4%), chronic pulmonary disease (14.9%), and congestive heart failure (13.7%). The most common comorbidities in the ORIF group were uncomplicated hypertension (30.8%), fluid/electrolyte disorders (14.5%), chronic pulmonary disease (14.0%), and uncomplicated diabetes (10.9%). Patients treated with THA had most commonly uncomplicated hypertension (30.1%), fluid/electrolyte disorders (17.2%), uncomplicated diabetes (15.5%), and chronic pulmonary disease (14.4%). The prevalence of comorbidities is displayed in Table 3.
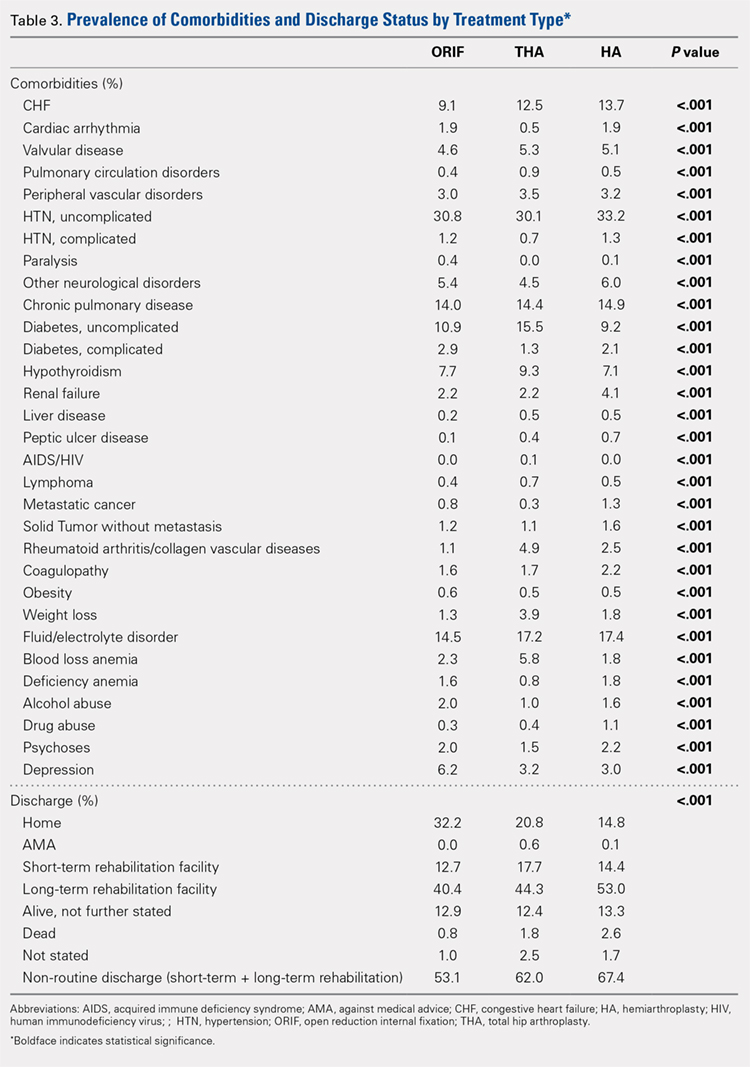
DISCHARGE STATUS
Mortality varied significantly, being lowest in those who underwent ORIF (0.8%), followed those who underwent THA (1.8%), and HA (2.6%) (P < .001, Table 1).
The majority of patients in each group were discharged to long-term rehabilitation facilities, including 53.0% of those treated with HA, 40.4% of those treated with ORIF, and 44.3% of patients treated with THA. The second most common discharge location was home, which included 14.8% of patients who underwent HA, 32.2% of patients treated with ORIF, and 20.8% of those who underwent THA. Table 3 demonstrates the details of the discharge settings.
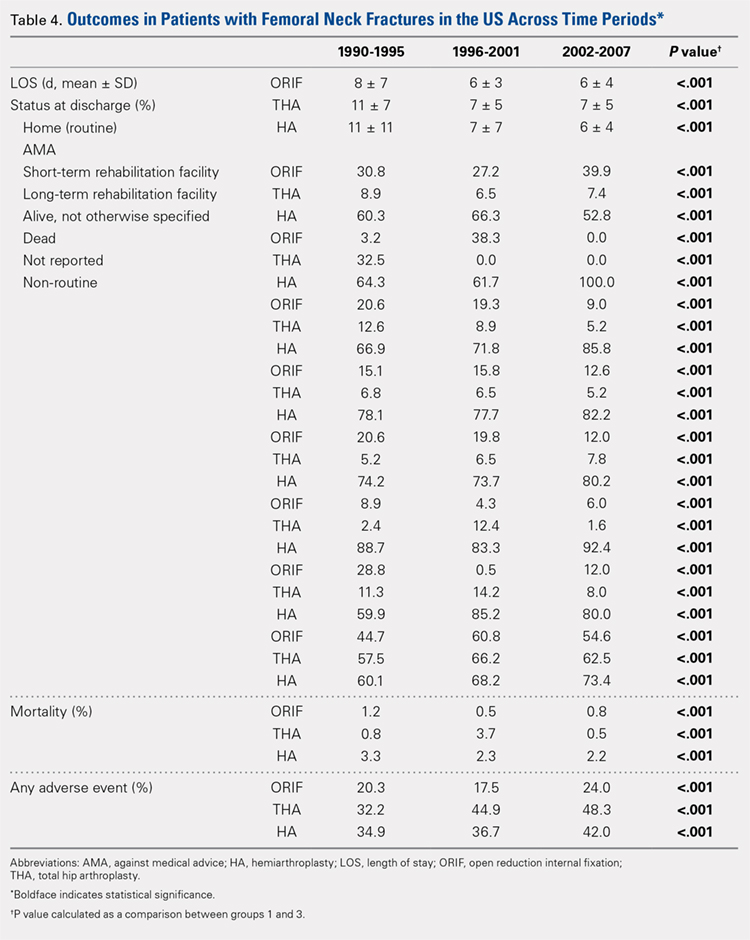
Mortality analysis over time demonstrated a significant decrease in each treatment group (P < .001). Mortality in the ORIF group decreased from 1.2% during 1990 to 1995 to 0.8% in 2002 to 2007. Mortality in the THA group also decreased significantly from 0.8% during 1990 to 1995 to 0.5% during the 2002 to 2007 time period. Patients who underwent HA also exhibited a decrease in mortality rate from 3.3% during 1990 to 1995 to 2.2% during 2002 to 2007 (P < .001, Table 4, Figure 2).
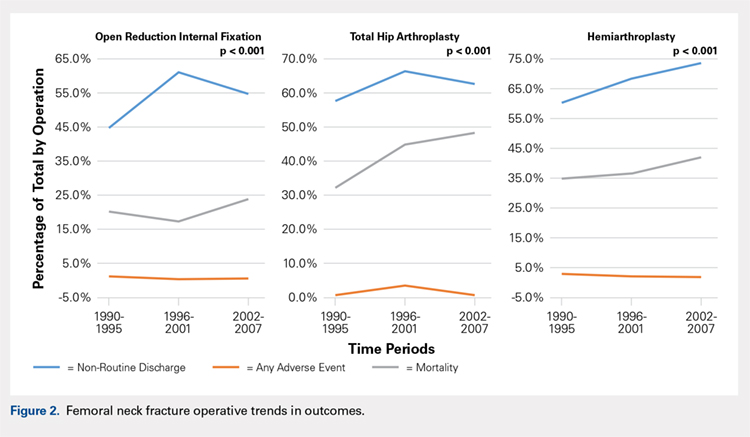
GENERAL ADVERSE EVENTS
There was a significant difference (P < .001) in the percentage of adverse events experienced, the maximum being observed in the THA group (41.0%), followed by the HA group (37.9%) and trailed by the ORIF group (20.3%, (P < .001, Table 1). The prevalence of adverse events is detailed in Table 5.
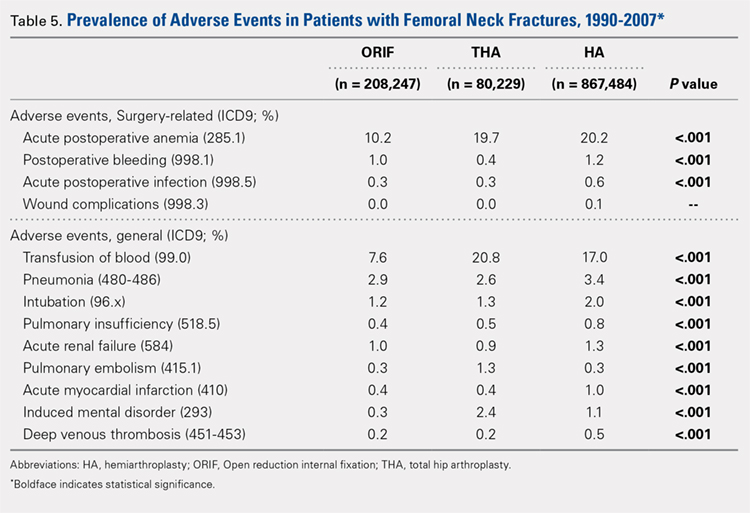
Continue to: Patients who underwent THA...
Patients who underwent THA had the highest rate of any adverse event, LOS, and transfusion rate (Table 1 and Table 5).
The prevalence of postoperative pneumonia was highest in the HA group (3.4%), followed by the ORIF group (2.9%), and the THA group (2.6%) (P < .001, Table 5). There was also a significant difference in rates of intubation, pulmonary insufficiency, acute renal failure, pulmonary embolism, acute myocardial infarction, induced mental disorder, and deep venous thrombosis (P < .001 for all, Table 5).
SURGERY-RELATED ADVERSE EVENTS
Surgery-related outcomes over the entire study period were significantly different according to the type of procedure performed (P < .001, Table 5). Patients who underwent HA had the highest rate of acute postoperative anemia (20.2%), followed by those who underwent THA (19.7%), and ORIF (10.2%). Postoperative bleeding rates also varied significantly, with 1.2% in the HA group, followed by 1.0% in the ORIF group and 0.4% in the THA group (P < .001, Table 5). Acute postoperative infection rates also varied significantly, with the highest rate being observed in the HA group (0.6%) compared to that in the THA and ORIF groups (both 0.3%) (P < .001, Table 5).
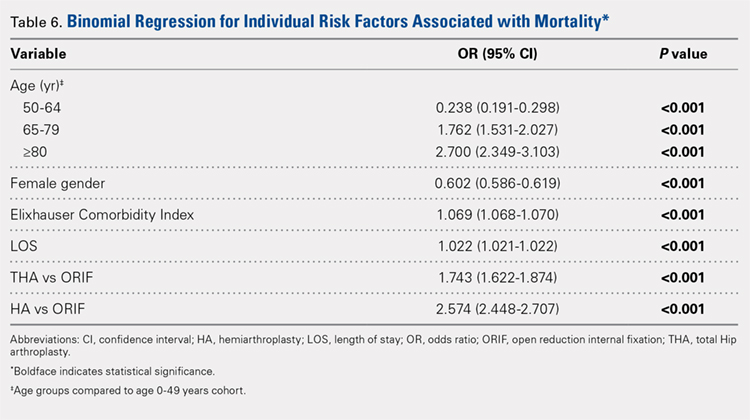

Table 6, Table 7, and Table 8 detail the results of regression analyses in patients with femoral neck fractures for individual risk factors associated with mortality, any adverse event, and nonroutine discharge to a short- or long-term rehabilitation facility, respectively. Increasing age (50–64 years, OR: 0.238; 65–79 years, OR: 1.762; and ≥80 years, OR: 2.700), THA (OR: 1.743), and HA (OR: 2.574) were found to be independent risk factors for mortality in the perioperative period (P < .001 for each, Table 6). Increasing age (50–64 years, OR: 1.888; 65–79 years, OR: 2.983; and ≥80 years, OR: 3.722), THA (OR: 2.489), and HA (OR: 2.098) were also found to be independent risk factors for any adverse event in the perioperative period (P < .001, Table 7). Age (50–64 years, OR: 1.662; 65–79 years, OR: 4.320; and ≥80 years, OR: 7.102) was the best predictor for nonroutine discharge to a short- or long-term rehabilitation facility (P < .001, Table 8).
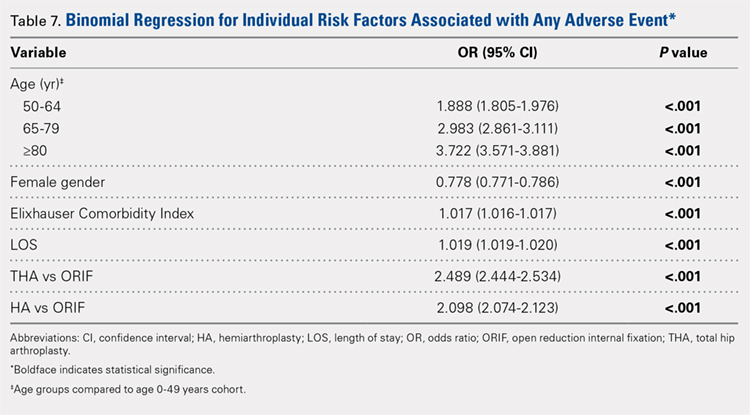
DISCUSSION
Femoral neck fractures in the elderly population present a significant financial burden to the healthcare system.1-3,24,25 Consistent with previous epidemiological studies, our results show that the femoral neck fracture population has become older and has more medical comorbidities over the last 3 decades.27,28. Similarly, we also found that the rate of medical, surgical, and mechanical perioperative complications has increased in the same time period. Interestingly, the mortality rate has remained relatively similar.
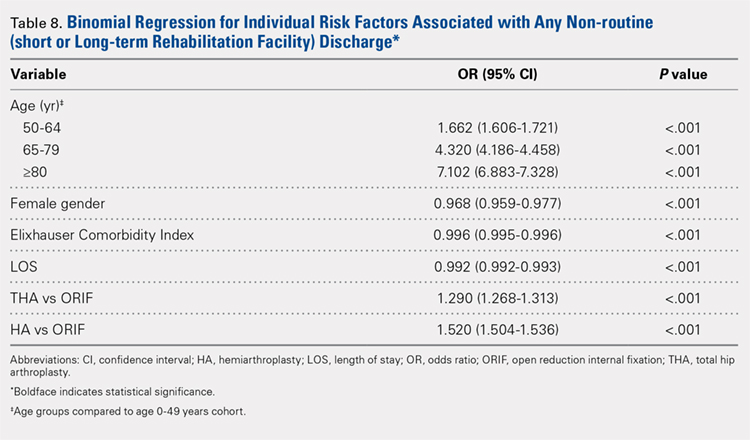
Continue to: Although patients undergoing HA...
Although patients undergoing HA for femoral neck fractures are older and have more medical comorbidities, we found that the rate of adverse events in the perioperative period for patients undergoing THA was higher than that in the HA group. Consistent with prior studies, patients who underwent THA had higher rates of blood transfusion, pulmonary embolism, and induced mental disorders.34 Multivariable regression analysis demonstrated that after controlling for age, medical comorbidity, and type of surgery performed, THA emerged as an independent risk factor for any adverse event in the perioperative period. Increased anesthesia time, reaming of the acetabulum, and increased complexity of surgery probably account for these changes.
Our study results are consistent with those of Jain and colleagues,30 which showed a decrease in utilization of THA for femoral neck fractures between 1990 and 2001. Since THA is generally indicated for younger, more active patients in relatively good health, this would explain why changes in baseline health in this cohort over the last 20 years would lead to fewer THA procedures being performed. Surgeons in the US may be finding there are fewer patients who are candidates for THA. Miller and colleagues5 reported conflicting results and showed an increase in THA utilization in this patient population. However, their study evaluated treatment trends based on data from the ABOS part II of recently graduated orthopedic surgeons and may not be an accurate representation of national practice trends in the US. The trend toward increased subspecialization may explain their findings. As the authors noted, although they found an increase in the use of THA for femoral neck fractures by new adult reconstruction surgeons, the percentage of new surgeons treating femoral neck fractures has declined.5
Our analysis showed very concrete trends in treatment management at the extremes of the age ranges. There were substantial increases in the use of ORIF for patients <50 years (from 63.9% in 1990–1995 to 81.4% in 2002–2007, P < .001) and in the use of HA for patients >80 years (from 74.4% in 1990–1995 to 84.6% in 2002–2007, P < .001). This trend parallels recent studies that purport better outcomes for young patients undergoing ORIF and elderly patients undergoing HA.30 Our analysis did not demonstrate a large shift in surgeon preference for treatment of patients between 50 and 80 years, although there was a statistically significant decrease in ORIF and THA usage and a reflective increase in HA usage in this population as well. The fact that there has not been as substantial a shift in treatment trends for this large age group is potentially due to the wide variations in comorbid conditions and the functionality that abounds in this age group.1
The limitations of the current study are those inherent with a retrospective database analysis. The reliance on accurate coding brings up a potential for error; however, it is unlikely that comorbidities and outcomes are undercoded as hospitals are incentivized to input values that increase the acuity and thus reimbursement for each hospital stay.35 The database also relies on the ICD-9 procedural and diagnostic codes, which are not as specific as the currently adopted ICD-10 codes; hence, we are unable to distinguish between different forms of internal fixation, for example intramedullary nailing versus dynamic hip screw. This also precludes us from including other critical data such as degree of fracture displacement, cemented versus uncemented implantation, surgical approach for arthroplasty, and functional outcomes of individual patients. Moreover, the database used, although the largest inpatient sample available for analysis, represents only approximately 20% of hospitals nationwide. In addition, as patients cannot be tracked over time within the database, we are limited to outcomes in the perioperative period captured in a single hospital stay and cannot identify readmissions. Finally, our analysis is limited to the years 1990 to 2007 because of an increase in the relative standard error of the database in more recent years. Although this results in data that are not the most current, we believe that this study provides valuable insight regarding the trends in surgical treatment and acute postoperative outcomes of these injuries that have hitherto not been reported. To limit the inherent biases and the limitations within this study, prospective, randomized studies with long-term follow-up comparing outcomes across modes of treatment are needed to definitively determine the optimum form of treatment for this fracture type.
CONCLUSION
This is the largest study to date reporting on national trends in the surgical treatment and outcomes of the femoral neck fracture population. Orthopedic surgeons performing THA should be aware that the femoral neck fracture population is changing and at higher risk for perioperative complications. The advent of bisphosphonate therapy has been suggested as a possible reason for the decrease in fragility fractures and why a larger proportion of the femoral neck fracture population is now >80 years.36,37 With an aging population at a higher risk for perioperative complications, clinicians must take special care in choosing the appropriate surgical intervention that will give their patients the best functional outcome while minimizing the risk of surgical complications. Orthopedic surgeons should weigh the added risk associated with THA in this population.
1. Bishop J, Yang A, Githens M, Sox AH. Evaluation of contemporary trends in femoral neck fracture management reveals discrepancies in treatment. Geriatr Orthop Surg Rehabil. 2016;7(3):135. doi:10.1177/2151458516658328.
2. Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A. Incidence and economic burden of osteoporosis-related fractures in the United States, 2005-2025. J Bone Miner Res Off J Am Soc Bone Miner Res. 2007;22(3):465. doi:10.1359/jbmr.061113.
3. Kannus P, Parkkari J, Sievanen H, Heinonen A, Vuori I, Jarvinen M. Epidemiology of hip fractures. Bone. 1996;18(1 Suppl.):57s. doi:10.1016/8756-3282(95)00381-9.
4. Koval KJ, Zuckerman JD. Hip fractures: I. Overview and evaluation and treatment of femoral-neck fractures. J Am Acad Orthop Surg. 1994;2(3):141. doi:10.5435/00124635-199405000-00002.
5. Miller BJ, Callaghan JJ, Cram P, Karam M, Marsh JL, Noiseux NO. Changing trends in the treatment of femoral neck fractures: a review of the American Board of Orthopaedic Surgery database. J Bone Joint Surg. (American) 2014;96(17):e149. doi:10.2106/JBJS.M.01122.
6. Miller BJ, Lu X, Cram P. The trends in treatment of femoral neck fractures in the Medicare population from 1991 to 2008. J Bone Joint Surg. (American) 2013;95(18):e132. doi:10.2106/JBJS.L.01163.
7. Nwachukwu BU, McCormick F, Provencher MT, Roche M, Rubash HE. A comprehensive analysis of Medicare trends in utilization and hospital economics for total knee and hip arthroplasty from 2005 to 2011. J Arthroplast. 2015;30(1):15. doi:10.1016/j.arth.2014.08.025.
8. Su EP, Su SL. Femoral neck fractures: a changing paradigm. Bone Joint J. 2014;96-b(11) Supple A):43. doi:10.1302/0301-620X.96B11.34334.
9. Ahn J, Man LX, Park S, Sodl JF, Esterhai JL. Systematic review of cemented and uncemented hemiarthroplasty outcomes for femoral neck fractures. Clin Orthop Relat Res. 2008;466(10):2513. doi:10.1007/s11999-008-0368-3.
10. Alolabi B, Bajammal S, Shirali J, Karanicolas PJ, Gafni A, Bhandari M. Treatment of displaced femoral neck fractures in the elderly: a cost-benefit analysis. J Orthop Trauma. 2009;23(6):442. doi:10.1097/BOT.0b013e31817614dd.
11. Bentler SE, Liu L, Obrizan M, et al. The aftermath of hip fracture: discharge placement, functional status change, and mortality. Am J Epidemiol. 2009;170(10):1290. doi:10.1093/aje/kwp266.
12. Brox WT, Chan PH, Cafri G, Inacio MC. Similar mortality with general or regional anesthesia in elderly hip fracture patients. Acta Orthop. 2016;87(2):152. doi:10.3109/17453674.2015.1128781.
13. Catal B, Sener M. Treatment and displacement affect the reoperation rate for femoral neck fracture. Clin Orthop Relat Res. 2013;471(12):4096. doi:10.1007/s11999-013-3295-x.
14. Dailiana Z, Papakostidou I, Varitimidis S, Michalitsis S, Veloni A, Malizos K. Surgical treatment of hip fractures: factors influencing mortality. Hippokratia. 2013;17(3):252.
15. Deangelis JP, Ademi A, Staff I, Lewis CG. Cemented versus uncemented hemiarthroplasty for displaced femoral neck fractures: a prospective randomized trial with early follow-up. J Orthop Trauma. 2012;26(3):135. doi:10.1097/BOT.0b013e318238b7a5.
16. Hedbeck CJ, Inngul C, Blomfeldt R, Ponzer S, Tornkvist H, Enocson A. Internal fixation versus cemented hemiarthroplasty for displaced femoral neck fractures in patients with severe cognitive dysfunction: a randomized controlled trial. J Orthop Trauma. 2013;27(12):690. doi:10.1097/BOT.0b013e318291f544.
17. Jia Z, Ding F, Wu Y, et al. Unipolar versus bipolar hemiarthroplasty for displaced femoral neck fractures: a systematic review and meta-analysis of randomized controlled trials. J Orthop Surg Res. 2015;10:8. doi:10.1186/s13018-015-0165-0.
18. Lapidus LJ, Charalampidis A, Rundgren J, Enocson A. Internal fixation of garden I and II femoral neck fractures: posterior tilt did not influence the reoperation rate in 382 consecutive hips followed for a minimum of 5 years. J Orthop Trauma. 2013;27(7):386. doi:10.1097/BOT.0b013e318281da6e.
19. Mariconda M, Costa GG, Cerbasi S, et al. Factors predicting mobility and the change in Activities of Daily Living After hip fracture: A 1-year prospective cohort study. J Orthop Trauma. 2016;30(2):71. doi:10.1097/BOT.0000000000000448.
20. Nyholm AM, Gromov K, Palm H, et al. Time to surgery is associated with thirty-day and ninety-day mortality After proximal femoral fracture: A retrospective observational study on prospectively collected data from the Danish Fracture Database Collaborators. J Bone Joint Surg. (American) 2015;97(16):1333. doi:10.2106/JBJS.O.00029.
21. Samuel AM, Russo GS, Lukasiewicz AM, et al. Surgical treatment of femoral neck fractures after 24 hours in patients between the ages of 18 and 49 is associated with poor inpatient outcomes: an analysis of 1361 patients in the National Trauma Data Bank. J Orthop Trauma. 2016;30(2):89. doi:10.1097/BOT.0000000000000456.
22. Yu L, Wang Y, Chen J. Total hip arthroplasty versus hemiarthroplasty for displaced femoral neck fractures: meta-analysis of randomized trials. Clin Orthop Relat Res. 2012;470(8):2235. doi:10.1007/s11999-012-2293-8.
23. Zi-Sheng A, You-Shui G, Zhi-Zhen J, Ting Y, Chang-Qing Z. Hemiarthroplasty vs primary total hip arthroplasty for displaced fractures of the femoral neck in the elderly: a meta-analysis. J Arthroplast. 2012;27(4):583. doi:10.1016/j.arth.2011.07.009.
24. Zielinski SM, Keijsers NL, Praet SF, et al. Functional outcome after successful internal fixation versus salvage arthroplasty of patients with a femoral neck fracture. J Orthop Trauma. 2014;28(12):e273. doi:10.1097/BOT.0000000000000123.
25. Gu Q, Koenig L, Mather RC, 3rd, Tongue J. Surgery for hip fracture yields societal benefits that exceed the direct medical costs. Clin Orthop Relat Res. 2014;472(11):3536. doi:10.1007/s11999-014-3820-6.
26. Forsh DA, Ferguson TA. Contemporary management of femoral neck fractures: the young and the old. Curr Rev Musculoskelet Med. 2012;5(3):214. doi:10.1007/s12178-012-9127-x.
27. Macaulay W, Pagnotto MR, Iorio R, Mont MA, Saleh KJ. Displaced femoral neck fractures in the elderly: hemiarthroplasty versus total hip arthroplasty. J Am Acad Orthop Surg. 2006;14(5):287. doi:10.5435/00124635-200605000-00004.
28. Miyamoto RG, Kaplan KM, Levine BR, Egol KA, Zuckerman JD. Surgical management of hip fractures: an evidence-based review of the literature. I: Femoral neck fractures. J Am Acad Orthop Surg. 2008;16(10):596. doi:10.5435/00124635-200810000-00005.
29. Probe R, Ward R. Internal fixation of femoral neck fractures. J Am Acad Orthop Surg. 2006;14(9):565. doi:10.5435/00124635-200609000-00006.
30. Jain NB, Losina E, Ward DM, Harris MB, Katz JN. Trends in surgical management of femoral neck fractures in the United States. Clin Orthop Relat Res. 2008;466(12):3116. doi:10.1007/s11999-008-0392-3.
31. Menendez ME, Neuhaus V, van Dijk CN, Ring D. The Elixhauser comorbidity method outperforms the Charlson index in predicting inpatient death after orthopaedic surgery. Clin Orthop Relat Res. 2014;472(9):2878. doi:10.1007/s11999-014-3686-7.
32. Van Walraven C, Austin PC, Jennings A, Quan H, Forster AJ. A modification of the Elixhauser Comorbidity measures into a point system for hospital death using administrative data. Med Care. 2009;47(6):626-633.
33. Best MJ, Buller LT, Falakassa J, Vecchione D. Risk factors for nonroutine discharge in patients undergoing spinal fusion for intervertebral disc disorders. Iowa Orthop J. 2015;35:147.
34. Schairer WW, Lane JM, Halsey DA, Iorio R, Padgett DE, McLawhorn AS. The Frank Stinchfield award: total hip arthroplasty for femoral neck fracture is not a typical DRG 470: A propensity-matched cohort study. Clin Orthop Relat Res. 2017;475(2):353-360. doi:10.1007/s11999-016-4868-2.
35. Nikkel LE, Fox EJ, Black KP, Davis C, Andersen L, Hollenbeak CS. Impact of comorbidities on hospitalization costs following hip fracture. J Bone Joint Surg Am. 2012;94(1):9. doi:10.2106/JBJS.J.01077.
36. Bilezikian JP. Efficacy of bisphosphonates in reducing fracture risk in postmenopausal osteoporosis. Am J Med. 2009;122(2 Suppl.):S14. doi:10.1016/j.amjmed.2008.12.003.
37. Siris ES, Pasquale MK, Wang Y, Watts NB. Estimating bisphosphonate use and fracture reduction among US women aged 45 years and older, 2001-2008. J Bone Miner Res Off J Am Soc Bone Miner Res. 2011;26(1):3. doi:10.1002/jbmr.189.
ABSTRACT
The ideal mode of fixation for patients with femoral neck fractures is not well defined in the current literature. This study describes the recent trends in surgical management of femoral neck fractures with an analysis on perioperative outcomes.
The National Hospital Discharge Survey was used to identify femoral neck fractures in the United States between 1990 and 2007 (n = 1,155,960) treated with open reduction and internal fixation (ORIF), total hip arthroplasty (THA), or hemiarthroplasty (HA). Trends were examined over the following 3 time periods: 1990 to 1995 (group 1), 1996 to 2001 (group 2), and 2002 to 2007 (group 3). Elixhauser Comorbidity Index and perioperative complications were calculated.
Use of HA increased (74.4% to 84.6%), whereas that of THA (7.3% to 4.9%) and ORIF (18.3% to 10.6%) decreased, from group 1 to group 3 in the age group of >80 years. The use of ORIF increased (63.9% to 81.4%), whereas the use of both HA and THA decreased, from group 1 to group 3 in the age group of <50 years. The rate of adverse events increased across all fixation types but was greatest among THA (32.2% to 48.3%).
The femoral neck patient population is now older and has more medical comorbidities. We observed a trend toward performing HA in older patients and ORIF in younger patients. Despite superior functional outcomes reported in THA, this study found a decreased utilization of THA in all age groups along with an increase in adverse events and nonroutine discharges for patients with femoral neck fractures treated with THA.
Funding: This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Continue to: Femoral neck fractures...
Femoral neck fractures are a common occurrence in the United States. A recent study estimated an incidence of >63 per 100,000 population.1-8 Although the incidence appears to have decreased over recent decades, there is a projected exponential increase in the incidence of hip fractures over the next 30 years in the baby boomer population.8,9 Given that these fractures have a significant impact on patient morbidity, mortality, and quality of life, research efforts have been directed toward optimizing the treatment of affected patients and improving the outcomes.4,9-24
The treatment of choice for femoral neck fractures and the use of total hip arthroplasty (THA)11 have been a topic of debate.4,9,10,15-17,22,25 Total hip arthroplasty has been advocated for younger, more active patients, whereas hemiarthroplasty (HA) has been reserved for patients who are older and less active. Although several studies have demonstrated that arthroplasty outperforms open reduction and internal fixation (ORIF) in the elderly population with displaced femoral neck fractures, ORIF is still commonly performed in the United States for nondisplaced fractures and in patients aged <50 years.26-29
In an attempt to quantify the use of THA in the treatment of femoral neck fractures and demonstrate the national trends, Miller and colleagues5 pooled the American Board of Orthopaedic Surgery (ABOS) database and analyzed the treatment trends of surgeons taking part II of the ABOS examination from 1999 to 2011. The authors found an increased utilization of THA by recently graduated orthopedic surgeons. In contrast, Jain and colleagues30 found different national trends when they analyzed data from the National Inpatient Sample containing data between 1990 and 2001 and further found decreased utilization of THA procedures by orthopedic surgeons of all levels of training nationwide. However, neither of these studies reported about the trends in demographics, comorbidities, risk factors, or outcomes in this patient population following surgery.
The purpose of this study was to help clarify the findings of these authors using the largest dataset to date and also report on the perioperative complications associated with each mode of fixation in patients who undergo operative treatment for femoral neck fractures in the United States. Our hypotheses were that the femoral neck fracture patient population has become older and has more medical comorbidities. We also hypothesized that there has been a trend toward performing fewer THA procedures in the United States and that THA is associated with increased perioperative complications compared to those with HA and ORIF.
MATERIALS AND METHODS
We conducted a retrospective epidemiological study using the National Hospital Discharge Survey (NHDS) on surgical trends in the management of femoral neck fractures. The NHDS is a publicly available survey that is conducted annually to provide data of nonfederal, short-stay hospitals to the public. The sample data are weighted to provide nationwide estimates of annual inpatient care. The NHDS includes up to 7 medical diagnoses and 4 procedural codes per case, which are categorized using the International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) codes, that were collected along with patient demographic information, length of stay (LOS), and discharge disposition. The diagnostic and procedural codes used for this study are presented in the Appendix. The year 2007 was chosen as the endpoint of this study due to the fact that the relative standard error of the NHDS doubled in 2008 as a result of a decrease in its survey size. As this is a publicly available database, our study was exempt from institutional review board approval.

Continue to: All pateints admitted...
All patients admitted with a primary diagnosis of closed transcervical fracture of the femoral neck (ICD-9-CM 820.0x) were selected. This resulted in 1,674,160 fractures. All patients with fractures with a concurrent primary procedural code of ORIF (79.35), HA (81.52), or THA (81.51) were identified, resulting in a total sample size of 1,155,960 surgical fractures. Analysis of the fractures based on additional specificity,ie subcapital versus midcervical versus basicervical, was not carried out because >90% of femoral neck fractures in the database were coded as “unspecified” or “other” (ICD9 CM 820.00 and 820.09, respectively).
Comorbidity burden was quantified using Elixhauser coding algorithms as previously described.31 The Elixhauser comorbidity measure is a model consisting of 31 conditions and has recently been identified as a better predictor of mortality in patients undergoing orthopedic procedures when compared with the Charlson Comorbidity Index.31 Dichotomous variables for each Elixhauser comorbidity were created, and χ2 tests were utilized to assess the association between each comorbidity and mortality. The weighted Elixhauser score for each statistically significant comorbidity was calculated as described by van Walraven and colleagues.32 The Elixhauser comorbidity score was then calculated for each patient by summing the individual weights of all comorbidities. Postoperative adverse events were determined using the complication-screening-package as previously described.33
All adverse events were categorized into 3 categories, including general medical complications, mechanical complications, and surgical complications. All adverse events recorded in the NHDS database are events that occurred during a single hospitalization. Therefore, it does not take into account adverse events that occurred after discharge, and, for example, mortality refers to postoperative mortality that occurs prior to discharge. The study period comprised data captured from 1990 to 2007, and 3 groups were generated from this time period to better characterize patients throughout the large study time frame. Group 1 comprised patients who underwent surgical management of femoral neck fractures from 1990 to 1995, group 2 consisted of patients treated from 1996 to 2001, and group 3 included patients treated from 2002 to 2007.
Categorical data were analyzed using the χ2 test, and continuous data were analyzed by the independent-samples t test and ANOVA. Multivariable binary logistic regression analyses were performed to assess the contributions of individual comorbidities to mortality, adverse events, and nonroutine discharge. Elixhauser comorbidities with a P value of < .10 in the bivariate analysis and presenting in at least 0.2% of the population were included in the logistic regression.31 Odds ratios and confidence intervals were calculated to assess the association between comorbidities and our dichotomous variables. A P value of < .001 defined statistical significance.33 Statistical analysis was conducted using SPSS version 21 (IBM).
RESULTS
Patient Demographics
Our query demonstrated a total of 1,155,960 patients who underwent surgical fixation of femoral neck fractures (Table 1). The most commonly used treatment modality was HA (75%), followed by ORIF (18%) and later by THA (7%). The majority of patients were females in each treatment group. Patients’ age varied according to treatment group, with patients undergoing HA having a mean age of 81.0 ± 9.0 years, patients undergoing ORIF having a mean age of 75.0 ± 17.0 years, and those undergoing THA having a mean age of 79.0 ± 10.0 years (P < .001). The majority of patients were ≥80 years in all treatment groups, but the ORIF group had the greatest proportion of patients <65 years (P < .001). Among patients undergoing HA, 62.4% were ≥80 years, while the ORIF and HA groups consisted of 48.6% and 51.5% of patients in that same age group, respectively.

Continue to: TRENDS ANALYSIS
TRENDS ANALYSIS
There was a significant change in the distributions of the procedures performed according to age group over time. Patients >80 years continued to undergo primarily HA, with an increase from 74.4% during 1990 to 1995 up to 84.6% during the 2002 to 2007 period and a concomitant decrease in ORIF from 18.3% to 10.6% during the same time period in this age group. Surgical trends in patients 65 to 79 years demonstrated a significant decrease in management with ORIF from 19.1% in 1990 to 1995 to 16.8% in the 2002 to 2007 cohort (P < .001 for all, Table 2). There was an increase in the use of HA from 71.9% during the 1990 to 1995 period to 75.5% during the final study period (Table 2, Figure 1). The use of THA for all age groups decreased between 1990 and 2007, except for the 50- to 64-year-old group where THA utilization remained constant.

Management patterns in patients 50 to 64 years varied throughout the analysis and demonstrated the following trend: treatment with HA remained the most common technique used but varied slightly from 59.7% during 1990 to 1995 to 60.3% during 2002 to2007 (P < .001, Table 2). The second most common treatment used was ORIF, which decreased from 32.2% to 31.5% (P < .001, Table 2). The use of THA varied significantly from 8.2% among those managed during 1990 to 1995 to 11.7% during 1996 to 2001 but later declined to the initial 8.2% (P < .001, Table 2).

Analysis of patients ≤49 years demonstrated that ORIF was the preferred technique, which experienced a growth from 63.9% during 1990 to 1995 to 81.4% during the 2002 to 2007 period (P < .001, Table 2). A decreased use in THA was observed from 2.0% in the initial period to 0.6% in the final period (P < .001, Table 2). Use of HA decreased from 34.0% in 1990 to 1995 to 18.0% in 2002 to 2007 (P < .001, Table 2).
LENGTH OF STAY
Mean number of in-hospital days decreased throughout the study period for all treatment techniques. During the 1990 to 1995 study period, patients who underwent ORIF had a mean LOS of 8 ± 7 days, which decreased (P < .001, Table 2) to 6 ± 3 days in 1996 to 2001 and remained constant during 2002 to 2007 (mean 6 ± 4 days). This decrease in LOS was also observed in patients who underwent THA (P < .001, Table 2), who initially had a mean LOS of 11 ± 7 days during 1990 to 1995, which later decreased to 7 ± 5 days for the remainder of the study. The LOS for patients who underwent HA also decreased (P < .001, Table 2), which initially was reported to be 11 ± 11 days during 1990 to 1995, decreasing to 7 ±7 days in 1996–2001 and later to 6 ± 4 days in 2002 to 2007.
COMORBIDITIY ANALYSIS
The Elixhauser Comorbidity Index varied significantly among groups over time (P < .001, Table 2). Overall mean Elixhauser Comorbidity Index score per procedure type is provided in Table 1, with HA patients having the highest score (-0.15 ± 13.09, p<.001).
Continue to: Analysis of the preoperative comorbidities...
Analysis of the preoperative comorbidities demonstrated significant differences among each surgical treatment group (P < .001 for all, Table 3). The most common comorbidities in patients who underwent HA were uncomplicated hypertension (33.2%), fluid/electrolyte disorders (17.4%), chronic pulmonary disease (14.9%), and congestive heart failure (13.7%). The most common comorbidities in the ORIF group were uncomplicated hypertension (30.8%), fluid/electrolyte disorders (14.5%), chronic pulmonary disease (14.0%), and uncomplicated diabetes (10.9%). Patients treated with THA had most commonly uncomplicated hypertension (30.1%), fluid/electrolyte disorders (17.2%), uncomplicated diabetes (15.5%), and chronic pulmonary disease (14.4%). The prevalence of comorbidities is displayed in Table 3.

DISCHARGE STATUS
Mortality varied significantly, being lowest in those who underwent ORIF (0.8%), followed those who underwent THA (1.8%), and HA (2.6%) (P < .001, Table 1).
The majority of patients in each group were discharged to long-term rehabilitation facilities, including 53.0% of those treated with HA, 40.4% of those treated with ORIF, and 44.3% of patients treated with THA. The second most common discharge location was home, which included 14.8% of patients who underwent HA, 32.2% of patients treated with ORIF, and 20.8% of those who underwent THA. Table 3 demonstrates the details of the discharge settings.

Mortality analysis over time demonstrated a significant decrease in each treatment group (P < .001). Mortality in the ORIF group decreased from 1.2% during 1990 to 1995 to 0.8% in 2002 to 2007. Mortality in the THA group also decreased significantly from 0.8% during 1990 to 1995 to 0.5% during the 2002 to 2007 time period. Patients who underwent HA also exhibited a decrease in mortality rate from 3.3% during 1990 to 1995 to 2.2% during 2002 to 2007 (P < .001, Table 4, Figure 2).

GENERAL ADVERSE EVENTS
There was a significant difference (P < .001) in the percentage of adverse events experienced, the maximum being observed in the THA group (41.0%), followed by the HA group (37.9%) and trailed by the ORIF group (20.3%, (P < .001, Table 1). The prevalence of adverse events is detailed in Table 5.

Continue to: Patients who underwent THA...
Patients who underwent THA had the highest rate of any adverse event, LOS, and transfusion rate (Table 1 and Table 5).
The prevalence of postoperative pneumonia was highest in the HA group (3.4%), followed by the ORIF group (2.9%), and the THA group (2.6%) (P < .001, Table 5). There was also a significant difference in rates of intubation, pulmonary insufficiency, acute renal failure, pulmonary embolism, acute myocardial infarction, induced mental disorder, and deep venous thrombosis (P < .001 for all, Table 5).
SURGERY-RELATED ADVERSE EVENTS
Surgery-related outcomes over the entire study period were significantly different according to the type of procedure performed (P < .001, Table 5). Patients who underwent HA had the highest rate of acute postoperative anemia (20.2%), followed by those who underwent THA (19.7%), and ORIF (10.2%). Postoperative bleeding rates also varied significantly, with 1.2% in the HA group, followed by 1.0% in the ORIF group and 0.4% in the THA group (P < .001, Table 5). Acute postoperative infection rates also varied significantly, with the highest rate being observed in the HA group (0.6%) compared to that in the THA and ORIF groups (both 0.3%) (P < .001, Table 5).

Table 6, Table 7, and Table 8 detail the results of regression analyses in patients with femoral neck fractures for individual risk factors associated with mortality, any adverse event, and nonroutine discharge to a short- or long-term rehabilitation facility, respectively. Increasing age (50–64 years, OR: 0.238; 65–79 years, OR: 1.762; and ≥80 years, OR: 2.700), THA (OR: 1.743), and HA (OR: 2.574) were found to be independent risk factors for mortality in the perioperative period (P < .001 for each, Table 6). Increasing age (50–64 years, OR: 1.888; 65–79 years, OR: 2.983; and ≥80 years, OR: 3.722), THA (OR: 2.489), and HA (OR: 2.098) were also found to be independent risk factors for any adverse event in the perioperative period (P < .001, Table 7). Age (50–64 years, OR: 1.662; 65–79 years, OR: 4.320; and ≥80 years, OR: 7.102) was the best predictor for nonroutine discharge to a short- or long-term rehabilitation facility (P < .001, Table 8).

DISCUSSION
Femoral neck fractures in the elderly population present a significant financial burden to the healthcare system.1-3,24,25 Consistent with previous epidemiological studies, our results show that the femoral neck fracture population has become older and has more medical comorbidities over the last 3 decades.27,28. Similarly, we also found that the rate of medical, surgical, and mechanical perioperative complications has increased in the same time period. Interestingly, the mortality rate has remained relatively similar.

Continue to: Although patients undergoing HA...
Although patients undergoing HA for femoral neck fractures are older and have more medical comorbidities, we found that the rate of adverse events in the perioperative period for patients undergoing THA was higher than that in the HA group. Consistent with prior studies, patients who underwent THA had higher rates of blood transfusion, pulmonary embolism, and induced mental disorders.34 Multivariable regression analysis demonstrated that after controlling for age, medical comorbidity, and type of surgery performed, THA emerged as an independent risk factor for any adverse event in the perioperative period. Increased anesthesia time, reaming of the acetabulum, and increased complexity of surgery probably account for these changes.
Our study results are consistent with those of Jain and colleagues,30 which showed a decrease in utilization of THA for femoral neck fractures between 1990 and 2001. Since THA is generally indicated for younger, more active patients in relatively good health, this would explain why changes in baseline health in this cohort over the last 20 years would lead to fewer THA procedures being performed. Surgeons in the US may be finding there are fewer patients who are candidates for THA. Miller and colleagues5 reported conflicting results and showed an increase in THA utilization in this patient population. However, their study evaluated treatment trends based on data from the ABOS part II of recently graduated orthopedic surgeons and may not be an accurate representation of national practice trends in the US. The trend toward increased subspecialization may explain their findings. As the authors noted, although they found an increase in the use of THA for femoral neck fractures by new adult reconstruction surgeons, the percentage of new surgeons treating femoral neck fractures has declined.5
Our analysis showed very concrete trends in treatment management at the extremes of the age ranges. There were substantial increases in the use of ORIF for patients <50 years (from 63.9% in 1990–1995 to 81.4% in 2002–2007, P < .001) and in the use of HA for patients >80 years (from 74.4% in 1990–1995 to 84.6% in 2002–2007, P < .001). This trend parallels recent studies that purport better outcomes for young patients undergoing ORIF and elderly patients undergoing HA.30 Our analysis did not demonstrate a large shift in surgeon preference for treatment of patients between 50 and 80 years, although there was a statistically significant decrease in ORIF and THA usage and a reflective increase in HA usage in this population as well. The fact that there has not been as substantial a shift in treatment trends for this large age group is potentially due to the wide variations in comorbid conditions and the functionality that abounds in this age group.1
The limitations of the current study are those inherent with a retrospective database analysis. The reliance on accurate coding brings up a potential for error; however, it is unlikely that comorbidities and outcomes are undercoded as hospitals are incentivized to input values that increase the acuity and thus reimbursement for each hospital stay.35 The database also relies on the ICD-9 procedural and diagnostic codes, which are not as specific as the currently adopted ICD-10 codes; hence, we are unable to distinguish between different forms of internal fixation, for example intramedullary nailing versus dynamic hip screw. This also precludes us from including other critical data such as degree of fracture displacement, cemented versus uncemented implantation, surgical approach for arthroplasty, and functional outcomes of individual patients. Moreover, the database used, although the largest inpatient sample available for analysis, represents only approximately 20% of hospitals nationwide. In addition, as patients cannot be tracked over time within the database, we are limited to outcomes in the perioperative period captured in a single hospital stay and cannot identify readmissions. Finally, our analysis is limited to the years 1990 to 2007 because of an increase in the relative standard error of the database in more recent years. Although this results in data that are not the most current, we believe that this study provides valuable insight regarding the trends in surgical treatment and acute postoperative outcomes of these injuries that have hitherto not been reported. To limit the inherent biases and the limitations within this study, prospective, randomized studies with long-term follow-up comparing outcomes across modes of treatment are needed to definitively determine the optimum form of treatment for this fracture type.
CONCLUSION
This is the largest study to date reporting on national trends in the surgical treatment and outcomes of the femoral neck fracture population. Orthopedic surgeons performing THA should be aware that the femoral neck fracture population is changing and at higher risk for perioperative complications. The advent of bisphosphonate therapy has been suggested as a possible reason for the decrease in fragility fractures and why a larger proportion of the femoral neck fracture population is now >80 years.36,37 With an aging population at a higher risk for perioperative complications, clinicians must take special care in choosing the appropriate surgical intervention that will give their patients the best functional outcome while minimizing the risk of surgical complications. Orthopedic surgeons should weigh the added risk associated with THA in this population.
ABSTRACT
The ideal mode of fixation for patients with femoral neck fractures is not well defined in the current literature. This study describes the recent trends in surgical management of femoral neck fractures with an analysis on perioperative outcomes.
The National Hospital Discharge Survey was used to identify femoral neck fractures in the United States between 1990 and 2007 (n = 1,155,960) treated with open reduction and internal fixation (ORIF), total hip arthroplasty (THA), or hemiarthroplasty (HA). Trends were examined over the following 3 time periods: 1990 to 1995 (group 1), 1996 to 2001 (group 2), and 2002 to 2007 (group 3). Elixhauser Comorbidity Index and perioperative complications were calculated.
Use of HA increased (74.4% to 84.6%), whereas that of THA (7.3% to 4.9%) and ORIF (18.3% to 10.6%) decreased, from group 1 to group 3 in the age group of >80 years. The use of ORIF increased (63.9% to 81.4%), whereas the use of both HA and THA decreased, from group 1 to group 3 in the age group of <50 years. The rate of adverse events increased across all fixation types but was greatest among THA (32.2% to 48.3%).
The femoral neck patient population is now older and has more medical comorbidities. We observed a trend toward performing HA in older patients and ORIF in younger patients. Despite superior functional outcomes reported in THA, this study found a decreased utilization of THA in all age groups along with an increase in adverse events and nonroutine discharges for patients with femoral neck fractures treated with THA.
Funding: This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Continue to: Femoral neck fractures...
Femoral neck fractures are a common occurrence in the United States. A recent study estimated an incidence of >63 per 100,000 population.1-8 Although the incidence appears to have decreased over recent decades, there is a projected exponential increase in the incidence of hip fractures over the next 30 years in the baby boomer population.8,9 Given that these fractures have a significant impact on patient morbidity, mortality, and quality of life, research efforts have been directed toward optimizing the treatment of affected patients and improving the outcomes.4,9-24
The treatment of choice for femoral neck fractures and the use of total hip arthroplasty (THA)11 have been a topic of debate.4,9,10,15-17,22,25 Total hip arthroplasty has been advocated for younger, more active patients, whereas hemiarthroplasty (HA) has been reserved for patients who are older and less active. Although several studies have demonstrated that arthroplasty outperforms open reduction and internal fixation (ORIF) in the elderly population with displaced femoral neck fractures, ORIF is still commonly performed in the United States for nondisplaced fractures and in patients aged <50 years.26-29
In an attempt to quantify the use of THA in the treatment of femoral neck fractures and demonstrate the national trends, Miller and colleagues5 pooled the American Board of Orthopaedic Surgery (ABOS) database and analyzed the treatment trends of surgeons taking part II of the ABOS examination from 1999 to 2011. The authors found an increased utilization of THA by recently graduated orthopedic surgeons. In contrast, Jain and colleagues30 found different national trends when they analyzed data from the National Inpatient Sample containing data between 1990 and 2001 and further found decreased utilization of THA procedures by orthopedic surgeons of all levels of training nationwide. However, neither of these studies reported about the trends in demographics, comorbidities, risk factors, or outcomes in this patient population following surgery.
The purpose of this study was to help clarify the findings of these authors using the largest dataset to date and also report on the perioperative complications associated with each mode of fixation in patients who undergo operative treatment for femoral neck fractures in the United States. Our hypotheses were that the femoral neck fracture patient population has become older and has more medical comorbidities. We also hypothesized that there has been a trend toward performing fewer THA procedures in the United States and that THA is associated with increased perioperative complications compared to those with HA and ORIF.
MATERIALS AND METHODS
We conducted a retrospective epidemiological study using the National Hospital Discharge Survey (NHDS) on surgical trends in the management of femoral neck fractures. The NHDS is a publicly available survey that is conducted annually to provide data of nonfederal, short-stay hospitals to the public. The sample data are weighted to provide nationwide estimates of annual inpatient care. The NHDS includes up to 7 medical diagnoses and 4 procedural codes per case, which are categorized using the International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) codes, that were collected along with patient demographic information, length of stay (LOS), and discharge disposition. The diagnostic and procedural codes used for this study are presented in the Appendix. The year 2007 was chosen as the endpoint of this study due to the fact that the relative standard error of the NHDS doubled in 2008 as a result of a decrease in its survey size. As this is a publicly available database, our study was exempt from institutional review board approval.

Continue to: All pateints admitted...
All patients admitted with a primary diagnosis of closed transcervical fracture of the femoral neck (ICD-9-CM 820.0x) were selected. This resulted in 1,674,160 fractures. All patients with fractures with a concurrent primary procedural code of ORIF (79.35), HA (81.52), or THA (81.51) were identified, resulting in a total sample size of 1,155,960 surgical fractures. Analysis of the fractures based on additional specificity,ie subcapital versus midcervical versus basicervical, was not carried out because >90% of femoral neck fractures in the database were coded as “unspecified” or “other” (ICD9 CM 820.00 and 820.09, respectively).
Comorbidity burden was quantified using Elixhauser coding algorithms as previously described.31 The Elixhauser comorbidity measure is a model consisting of 31 conditions and has recently been identified as a better predictor of mortality in patients undergoing orthopedic procedures when compared with the Charlson Comorbidity Index.31 Dichotomous variables for each Elixhauser comorbidity were created, and χ2 tests were utilized to assess the association between each comorbidity and mortality. The weighted Elixhauser score for each statistically significant comorbidity was calculated as described by van Walraven and colleagues.32 The Elixhauser comorbidity score was then calculated for each patient by summing the individual weights of all comorbidities. Postoperative adverse events were determined using the complication-screening-package as previously described.33
All adverse events were categorized into 3 categories, including general medical complications, mechanical complications, and surgical complications. All adverse events recorded in the NHDS database are events that occurred during a single hospitalization. Therefore, it does not take into account adverse events that occurred after discharge, and, for example, mortality refers to postoperative mortality that occurs prior to discharge. The study period comprised data captured from 1990 to 2007, and 3 groups were generated from this time period to better characterize patients throughout the large study time frame. Group 1 comprised patients who underwent surgical management of femoral neck fractures from 1990 to 1995, group 2 consisted of patients treated from 1996 to 2001, and group 3 included patients treated from 2002 to 2007.
Categorical data were analyzed using the χ2 test, and continuous data were analyzed by the independent-samples t test and ANOVA. Multivariable binary logistic regression analyses were performed to assess the contributions of individual comorbidities to mortality, adverse events, and nonroutine discharge. Elixhauser comorbidities with a P value of < .10 in the bivariate analysis and presenting in at least 0.2% of the population were included in the logistic regression.31 Odds ratios and confidence intervals were calculated to assess the association between comorbidities and our dichotomous variables. A P value of < .001 defined statistical significance.33 Statistical analysis was conducted using SPSS version 21 (IBM).
RESULTS
Patient Demographics
Our query demonstrated a total of 1,155,960 patients who underwent surgical fixation of femoral neck fractures (Table 1). The most commonly used treatment modality was HA (75%), followed by ORIF (18%) and later by THA (7%). The majority of patients were females in each treatment group. Patients’ age varied according to treatment group, with patients undergoing HA having a mean age of 81.0 ± 9.0 years, patients undergoing ORIF having a mean age of 75.0 ± 17.0 years, and those undergoing THA having a mean age of 79.0 ± 10.0 years (P < .001). The majority of patients were ≥80 years in all treatment groups, but the ORIF group had the greatest proportion of patients <65 years (P < .001). Among patients undergoing HA, 62.4% were ≥80 years, while the ORIF and HA groups consisted of 48.6% and 51.5% of patients in that same age group, respectively.

Continue to: TRENDS ANALYSIS
TRENDS ANALYSIS
There was a significant change in the distributions of the procedures performed according to age group over time. Patients >80 years continued to undergo primarily HA, with an increase from 74.4% during 1990 to 1995 up to 84.6% during the 2002 to 2007 period and a concomitant decrease in ORIF from 18.3% to 10.6% during the same time period in this age group. Surgical trends in patients 65 to 79 years demonstrated a significant decrease in management with ORIF from 19.1% in 1990 to 1995 to 16.8% in the 2002 to 2007 cohort (P < .001 for all, Table 2). There was an increase in the use of HA from 71.9% during the 1990 to 1995 period to 75.5% during the final study period (Table 2, Figure 1). The use of THA for all age groups decreased between 1990 and 2007, except for the 50- to 64-year-old group where THA utilization remained constant.

Management patterns in patients 50 to 64 years varied throughout the analysis and demonstrated the following trend: treatment with HA remained the most common technique used but varied slightly from 59.7% during 1990 to 1995 to 60.3% during 2002 to2007 (P < .001, Table 2). The second most common treatment used was ORIF, which decreased from 32.2% to 31.5% (P < .001, Table 2). The use of THA varied significantly from 8.2% among those managed during 1990 to 1995 to 11.7% during 1996 to 2001 but later declined to the initial 8.2% (P < .001, Table 2).

Analysis of patients ≤49 years demonstrated that ORIF was the preferred technique, which experienced a growth from 63.9% during 1990 to 1995 to 81.4% during the 2002 to 2007 period (P < .001, Table 2). A decreased use in THA was observed from 2.0% in the initial period to 0.6% in the final period (P < .001, Table 2). Use of HA decreased from 34.0% in 1990 to 1995 to 18.0% in 2002 to 2007 (P < .001, Table 2).
LENGTH OF STAY
Mean number of in-hospital days decreased throughout the study period for all treatment techniques. During the 1990 to 1995 study period, patients who underwent ORIF had a mean LOS of 8 ± 7 days, which decreased (P < .001, Table 2) to 6 ± 3 days in 1996 to 2001 and remained constant during 2002 to 2007 (mean 6 ± 4 days). This decrease in LOS was also observed in patients who underwent THA (P < .001, Table 2), who initially had a mean LOS of 11 ± 7 days during 1990 to 1995, which later decreased to 7 ± 5 days for the remainder of the study. The LOS for patients who underwent HA also decreased (P < .001, Table 2), which initially was reported to be 11 ± 11 days during 1990 to 1995, decreasing to 7 ±7 days in 1996–2001 and later to 6 ± 4 days in 2002 to 2007.
COMORBIDITIY ANALYSIS
The Elixhauser Comorbidity Index varied significantly among groups over time (P < .001, Table 2). Overall mean Elixhauser Comorbidity Index score per procedure type is provided in Table 1, with HA patients having the highest score (-0.15 ± 13.09, p<.001).
Continue to: Analysis of the preoperative comorbidities...
Analysis of the preoperative comorbidities demonstrated significant differences among each surgical treatment group (P < .001 for all, Table 3). The most common comorbidities in patients who underwent HA were uncomplicated hypertension (33.2%), fluid/electrolyte disorders (17.4%), chronic pulmonary disease (14.9%), and congestive heart failure (13.7%). The most common comorbidities in the ORIF group were uncomplicated hypertension (30.8%), fluid/electrolyte disorders (14.5%), chronic pulmonary disease (14.0%), and uncomplicated diabetes (10.9%). Patients treated with THA had most commonly uncomplicated hypertension (30.1%), fluid/electrolyte disorders (17.2%), uncomplicated diabetes (15.5%), and chronic pulmonary disease (14.4%). The prevalence of comorbidities is displayed in Table 3.

DISCHARGE STATUS
Mortality varied significantly, being lowest in those who underwent ORIF (0.8%), followed those who underwent THA (1.8%), and HA (2.6%) (P < .001, Table 1).
The majority of patients in each group were discharged to long-term rehabilitation facilities, including 53.0% of those treated with HA, 40.4% of those treated with ORIF, and 44.3% of patients treated with THA. The second most common discharge location was home, which included 14.8% of patients who underwent HA, 32.2% of patients treated with ORIF, and 20.8% of those who underwent THA. Table 3 demonstrates the details of the discharge settings.

Mortality analysis over time demonstrated a significant decrease in each treatment group (P < .001). Mortality in the ORIF group decreased from 1.2% during 1990 to 1995 to 0.8% in 2002 to 2007. Mortality in the THA group also decreased significantly from 0.8% during 1990 to 1995 to 0.5% during the 2002 to 2007 time period. Patients who underwent HA also exhibited a decrease in mortality rate from 3.3% during 1990 to 1995 to 2.2% during 2002 to 2007 (P < .001, Table 4, Figure 2).

GENERAL ADVERSE EVENTS
There was a significant difference (P < .001) in the percentage of adverse events experienced, the maximum being observed in the THA group (41.0%), followed by the HA group (37.9%) and trailed by the ORIF group (20.3%, (P < .001, Table 1). The prevalence of adverse events is detailed in Table 5.

Continue to: Patients who underwent THA...
Patients who underwent THA had the highest rate of any adverse event, LOS, and transfusion rate (Table 1 and Table 5).
The prevalence of postoperative pneumonia was highest in the HA group (3.4%), followed by the ORIF group (2.9%), and the THA group (2.6%) (P < .001, Table 5). There was also a significant difference in rates of intubation, pulmonary insufficiency, acute renal failure, pulmonary embolism, acute myocardial infarction, induced mental disorder, and deep venous thrombosis (P < .001 for all, Table 5).
SURGERY-RELATED ADVERSE EVENTS
Surgery-related outcomes over the entire study period were significantly different according to the type of procedure performed (P < .001, Table 5). Patients who underwent HA had the highest rate of acute postoperative anemia (20.2%), followed by those who underwent THA (19.7%), and ORIF (10.2%). Postoperative bleeding rates also varied significantly, with 1.2% in the HA group, followed by 1.0% in the ORIF group and 0.4% in the THA group (P < .001, Table 5). Acute postoperative infection rates also varied significantly, with the highest rate being observed in the HA group (0.6%) compared to that in the THA and ORIF groups (both 0.3%) (P < .001, Table 5).

Table 6, Table 7, and Table 8 detail the results of regression analyses in patients with femoral neck fractures for individual risk factors associated with mortality, any adverse event, and nonroutine discharge to a short- or long-term rehabilitation facility, respectively. Increasing age (50–64 years, OR: 0.238; 65–79 years, OR: 1.762; and ≥80 years, OR: 2.700), THA (OR: 1.743), and HA (OR: 2.574) were found to be independent risk factors for mortality in the perioperative period (P < .001 for each, Table 6). Increasing age (50–64 years, OR: 1.888; 65–79 years, OR: 2.983; and ≥80 years, OR: 3.722), THA (OR: 2.489), and HA (OR: 2.098) were also found to be independent risk factors for any adverse event in the perioperative period (P < .001, Table 7). Age (50–64 years, OR: 1.662; 65–79 years, OR: 4.320; and ≥80 years, OR: 7.102) was the best predictor for nonroutine discharge to a short- or long-term rehabilitation facility (P < .001, Table 8).

DISCUSSION
Femoral neck fractures in the elderly population present a significant financial burden to the healthcare system.1-3,24,25 Consistent with previous epidemiological studies, our results show that the femoral neck fracture population has become older and has more medical comorbidities over the last 3 decades.27,28. Similarly, we also found that the rate of medical, surgical, and mechanical perioperative complications has increased in the same time period. Interestingly, the mortality rate has remained relatively similar.

Continue to: Although patients undergoing HA...
Although patients undergoing HA for femoral neck fractures are older and have more medical comorbidities, we found that the rate of adverse events in the perioperative period for patients undergoing THA was higher than that in the HA group. Consistent with prior studies, patients who underwent THA had higher rates of blood transfusion, pulmonary embolism, and induced mental disorders.34 Multivariable regression analysis demonstrated that after controlling for age, medical comorbidity, and type of surgery performed, THA emerged as an independent risk factor for any adverse event in the perioperative period. Increased anesthesia time, reaming of the acetabulum, and increased complexity of surgery probably account for these changes.
Our study results are consistent with those of Jain and colleagues,30 which showed a decrease in utilization of THA for femoral neck fractures between 1990 and 2001. Since THA is generally indicated for younger, more active patients in relatively good health, this would explain why changes in baseline health in this cohort over the last 20 years would lead to fewer THA procedures being performed. Surgeons in the US may be finding there are fewer patients who are candidates for THA. Miller and colleagues5 reported conflicting results and showed an increase in THA utilization in this patient population. However, their study evaluated treatment trends based on data from the ABOS part II of recently graduated orthopedic surgeons and may not be an accurate representation of national practice trends in the US. The trend toward increased subspecialization may explain their findings. As the authors noted, although they found an increase in the use of THA for femoral neck fractures by new adult reconstruction surgeons, the percentage of new surgeons treating femoral neck fractures has declined.5
Our analysis showed very concrete trends in treatment management at the extremes of the age ranges. There were substantial increases in the use of ORIF for patients <50 years (from 63.9% in 1990–1995 to 81.4% in 2002–2007, P < .001) and in the use of HA for patients >80 years (from 74.4% in 1990–1995 to 84.6% in 2002–2007, P < .001). This trend parallels recent studies that purport better outcomes for young patients undergoing ORIF and elderly patients undergoing HA.30 Our analysis did not demonstrate a large shift in surgeon preference for treatment of patients between 50 and 80 years, although there was a statistically significant decrease in ORIF and THA usage and a reflective increase in HA usage in this population as well. The fact that there has not been as substantial a shift in treatment trends for this large age group is potentially due to the wide variations in comorbid conditions and the functionality that abounds in this age group.1
The limitations of the current study are those inherent with a retrospective database analysis. The reliance on accurate coding brings up a potential for error; however, it is unlikely that comorbidities and outcomes are undercoded as hospitals are incentivized to input values that increase the acuity and thus reimbursement for each hospital stay.35 The database also relies on the ICD-9 procedural and diagnostic codes, which are not as specific as the currently adopted ICD-10 codes; hence, we are unable to distinguish between different forms of internal fixation, for example intramedullary nailing versus dynamic hip screw. This also precludes us from including other critical data such as degree of fracture displacement, cemented versus uncemented implantation, surgical approach for arthroplasty, and functional outcomes of individual patients. Moreover, the database used, although the largest inpatient sample available for analysis, represents only approximately 20% of hospitals nationwide. In addition, as patients cannot be tracked over time within the database, we are limited to outcomes in the perioperative period captured in a single hospital stay and cannot identify readmissions. Finally, our analysis is limited to the years 1990 to 2007 because of an increase in the relative standard error of the database in more recent years. Although this results in data that are not the most current, we believe that this study provides valuable insight regarding the trends in surgical treatment and acute postoperative outcomes of these injuries that have hitherto not been reported. To limit the inherent biases and the limitations within this study, prospective, randomized studies with long-term follow-up comparing outcomes across modes of treatment are needed to definitively determine the optimum form of treatment for this fracture type.
CONCLUSION
This is the largest study to date reporting on national trends in the surgical treatment and outcomes of the femoral neck fracture population. Orthopedic surgeons performing THA should be aware that the femoral neck fracture population is changing and at higher risk for perioperative complications. The advent of bisphosphonate therapy has been suggested as a possible reason for the decrease in fragility fractures and why a larger proportion of the femoral neck fracture population is now >80 years.36,37 With an aging population at a higher risk for perioperative complications, clinicians must take special care in choosing the appropriate surgical intervention that will give their patients the best functional outcome while minimizing the risk of surgical complications. Orthopedic surgeons should weigh the added risk associated with THA in this population.
1. Bishop J, Yang A, Githens M, Sox AH. Evaluation of contemporary trends in femoral neck fracture management reveals discrepancies in treatment. Geriatr Orthop Surg Rehabil. 2016;7(3):135. doi:10.1177/2151458516658328.
2. Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A. Incidence and economic burden of osteoporosis-related fractures in the United States, 2005-2025. J Bone Miner Res Off J Am Soc Bone Miner Res. 2007;22(3):465. doi:10.1359/jbmr.061113.
3. Kannus P, Parkkari J, Sievanen H, Heinonen A, Vuori I, Jarvinen M. Epidemiology of hip fractures. Bone. 1996;18(1 Suppl.):57s. doi:10.1016/8756-3282(95)00381-9.
4. Koval KJ, Zuckerman JD. Hip fractures: I. Overview and evaluation and treatment of femoral-neck fractures. J Am Acad Orthop Surg. 1994;2(3):141. doi:10.5435/00124635-199405000-00002.
5. Miller BJ, Callaghan JJ, Cram P, Karam M, Marsh JL, Noiseux NO. Changing trends in the treatment of femoral neck fractures: a review of the American Board of Orthopaedic Surgery database. J Bone Joint Surg. (American) 2014;96(17):e149. doi:10.2106/JBJS.M.01122.
6. Miller BJ, Lu X, Cram P. The trends in treatment of femoral neck fractures in the Medicare population from 1991 to 2008. J Bone Joint Surg. (American) 2013;95(18):e132. doi:10.2106/JBJS.L.01163.
7. Nwachukwu BU, McCormick F, Provencher MT, Roche M, Rubash HE. A comprehensive analysis of Medicare trends in utilization and hospital economics for total knee and hip arthroplasty from 2005 to 2011. J Arthroplast. 2015;30(1):15. doi:10.1016/j.arth.2014.08.025.
8. Su EP, Su SL. Femoral neck fractures: a changing paradigm. Bone Joint J. 2014;96-b(11) Supple A):43. doi:10.1302/0301-620X.96B11.34334.
9. Ahn J, Man LX, Park S, Sodl JF, Esterhai JL. Systematic review of cemented and uncemented hemiarthroplasty outcomes for femoral neck fractures. Clin Orthop Relat Res. 2008;466(10):2513. doi:10.1007/s11999-008-0368-3.
10. Alolabi B, Bajammal S, Shirali J, Karanicolas PJ, Gafni A, Bhandari M. Treatment of displaced femoral neck fractures in the elderly: a cost-benefit analysis. J Orthop Trauma. 2009;23(6):442. doi:10.1097/BOT.0b013e31817614dd.
11. Bentler SE, Liu L, Obrizan M, et al. The aftermath of hip fracture: discharge placement, functional status change, and mortality. Am J Epidemiol. 2009;170(10):1290. doi:10.1093/aje/kwp266.
12. Brox WT, Chan PH, Cafri G, Inacio MC. Similar mortality with general or regional anesthesia in elderly hip fracture patients. Acta Orthop. 2016;87(2):152. doi:10.3109/17453674.2015.1128781.
13. Catal B, Sener M. Treatment and displacement affect the reoperation rate for femoral neck fracture. Clin Orthop Relat Res. 2013;471(12):4096. doi:10.1007/s11999-013-3295-x.
14. Dailiana Z, Papakostidou I, Varitimidis S, Michalitsis S, Veloni A, Malizos K. Surgical treatment of hip fractures: factors influencing mortality. Hippokratia. 2013;17(3):252.
15. Deangelis JP, Ademi A, Staff I, Lewis CG. Cemented versus uncemented hemiarthroplasty for displaced femoral neck fractures: a prospective randomized trial with early follow-up. J Orthop Trauma. 2012;26(3):135. doi:10.1097/BOT.0b013e318238b7a5.
16. Hedbeck CJ, Inngul C, Blomfeldt R, Ponzer S, Tornkvist H, Enocson A. Internal fixation versus cemented hemiarthroplasty for displaced femoral neck fractures in patients with severe cognitive dysfunction: a randomized controlled trial. J Orthop Trauma. 2013;27(12):690. doi:10.1097/BOT.0b013e318291f544.
17. Jia Z, Ding F, Wu Y, et al. Unipolar versus bipolar hemiarthroplasty for displaced femoral neck fractures: a systematic review and meta-analysis of randomized controlled trials. J Orthop Surg Res. 2015;10:8. doi:10.1186/s13018-015-0165-0.
18. Lapidus LJ, Charalampidis A, Rundgren J, Enocson A. Internal fixation of garden I and II femoral neck fractures: posterior tilt did not influence the reoperation rate in 382 consecutive hips followed for a minimum of 5 years. J Orthop Trauma. 2013;27(7):386. doi:10.1097/BOT.0b013e318281da6e.
19. Mariconda M, Costa GG, Cerbasi S, et al. Factors predicting mobility and the change in Activities of Daily Living After hip fracture: A 1-year prospective cohort study. J Orthop Trauma. 2016;30(2):71. doi:10.1097/BOT.0000000000000448.
20. Nyholm AM, Gromov K, Palm H, et al. Time to surgery is associated with thirty-day and ninety-day mortality After proximal femoral fracture: A retrospective observational study on prospectively collected data from the Danish Fracture Database Collaborators. J Bone Joint Surg. (American) 2015;97(16):1333. doi:10.2106/JBJS.O.00029.
21. Samuel AM, Russo GS, Lukasiewicz AM, et al. Surgical treatment of femoral neck fractures after 24 hours in patients between the ages of 18 and 49 is associated with poor inpatient outcomes: an analysis of 1361 patients in the National Trauma Data Bank. J Orthop Trauma. 2016;30(2):89. doi:10.1097/BOT.0000000000000456.
22. Yu L, Wang Y, Chen J. Total hip arthroplasty versus hemiarthroplasty for displaced femoral neck fractures: meta-analysis of randomized trials. Clin Orthop Relat Res. 2012;470(8):2235. doi:10.1007/s11999-012-2293-8.
23. Zi-Sheng A, You-Shui G, Zhi-Zhen J, Ting Y, Chang-Qing Z. Hemiarthroplasty vs primary total hip arthroplasty for displaced fractures of the femoral neck in the elderly: a meta-analysis. J Arthroplast. 2012;27(4):583. doi:10.1016/j.arth.2011.07.009.
24. Zielinski SM, Keijsers NL, Praet SF, et al. Functional outcome after successful internal fixation versus salvage arthroplasty of patients with a femoral neck fracture. J Orthop Trauma. 2014;28(12):e273. doi:10.1097/BOT.0000000000000123.
25. Gu Q, Koenig L, Mather RC, 3rd, Tongue J. Surgery for hip fracture yields societal benefits that exceed the direct medical costs. Clin Orthop Relat Res. 2014;472(11):3536. doi:10.1007/s11999-014-3820-6.
26. Forsh DA, Ferguson TA. Contemporary management of femoral neck fractures: the young and the old. Curr Rev Musculoskelet Med. 2012;5(3):214. doi:10.1007/s12178-012-9127-x.
27. Macaulay W, Pagnotto MR, Iorio R, Mont MA, Saleh KJ. Displaced femoral neck fractures in the elderly: hemiarthroplasty versus total hip arthroplasty. J Am Acad Orthop Surg. 2006;14(5):287. doi:10.5435/00124635-200605000-00004.
28. Miyamoto RG, Kaplan KM, Levine BR, Egol KA, Zuckerman JD. Surgical management of hip fractures: an evidence-based review of the literature. I: Femoral neck fractures. J Am Acad Orthop Surg. 2008;16(10):596. doi:10.5435/00124635-200810000-00005.
29. Probe R, Ward R. Internal fixation of femoral neck fractures. J Am Acad Orthop Surg. 2006;14(9):565. doi:10.5435/00124635-200609000-00006.
30. Jain NB, Losina E, Ward DM, Harris MB, Katz JN. Trends in surgical management of femoral neck fractures in the United States. Clin Orthop Relat Res. 2008;466(12):3116. doi:10.1007/s11999-008-0392-3.
31. Menendez ME, Neuhaus V, van Dijk CN, Ring D. The Elixhauser comorbidity method outperforms the Charlson index in predicting inpatient death after orthopaedic surgery. Clin Orthop Relat Res. 2014;472(9):2878. doi:10.1007/s11999-014-3686-7.
32. Van Walraven C, Austin PC, Jennings A, Quan H, Forster AJ. A modification of the Elixhauser Comorbidity measures into a point system for hospital death using administrative data. Med Care. 2009;47(6):626-633.
33. Best MJ, Buller LT, Falakassa J, Vecchione D. Risk factors for nonroutine discharge in patients undergoing spinal fusion for intervertebral disc disorders. Iowa Orthop J. 2015;35:147.
34. Schairer WW, Lane JM, Halsey DA, Iorio R, Padgett DE, McLawhorn AS. The Frank Stinchfield award: total hip arthroplasty for femoral neck fracture is not a typical DRG 470: A propensity-matched cohort study. Clin Orthop Relat Res. 2017;475(2):353-360. doi:10.1007/s11999-016-4868-2.
35. Nikkel LE, Fox EJ, Black KP, Davis C, Andersen L, Hollenbeak CS. Impact of comorbidities on hospitalization costs following hip fracture. J Bone Joint Surg Am. 2012;94(1):9. doi:10.2106/JBJS.J.01077.
36. Bilezikian JP. Efficacy of bisphosphonates in reducing fracture risk in postmenopausal osteoporosis. Am J Med. 2009;122(2 Suppl.):S14. doi:10.1016/j.amjmed.2008.12.003.
37. Siris ES, Pasquale MK, Wang Y, Watts NB. Estimating bisphosphonate use and fracture reduction among US women aged 45 years and older, 2001-2008. J Bone Miner Res Off J Am Soc Bone Miner Res. 2011;26(1):3. doi:10.1002/jbmr.189.
1. Bishop J, Yang A, Githens M, Sox AH. Evaluation of contemporary trends in femoral neck fracture management reveals discrepancies in treatment. Geriatr Orthop Surg Rehabil. 2016;7(3):135. doi:10.1177/2151458516658328.
2. Burge R, Dawson-Hughes B, Solomon DH, Wong JB, King A, Tosteson A. Incidence and economic burden of osteoporosis-related fractures in the United States, 2005-2025. J Bone Miner Res Off J Am Soc Bone Miner Res. 2007;22(3):465. doi:10.1359/jbmr.061113.
3. Kannus P, Parkkari J, Sievanen H, Heinonen A, Vuori I, Jarvinen M. Epidemiology of hip fractures. Bone. 1996;18(1 Suppl.):57s. doi:10.1016/8756-3282(95)00381-9.
4. Koval KJ, Zuckerman JD. Hip fractures: I. Overview and evaluation and treatment of femoral-neck fractures. J Am Acad Orthop Surg. 1994;2(3):141. doi:10.5435/00124635-199405000-00002.
5. Miller BJ, Callaghan JJ, Cram P, Karam M, Marsh JL, Noiseux NO. Changing trends in the treatment of femoral neck fractures: a review of the American Board of Orthopaedic Surgery database. J Bone Joint Surg. (American) 2014;96(17):e149. doi:10.2106/JBJS.M.01122.
6. Miller BJ, Lu X, Cram P. The trends in treatment of femoral neck fractures in the Medicare population from 1991 to 2008. J Bone Joint Surg. (American) 2013;95(18):e132. doi:10.2106/JBJS.L.01163.
7. Nwachukwu BU, McCormick F, Provencher MT, Roche M, Rubash HE. A comprehensive analysis of Medicare trends in utilization and hospital economics for total knee and hip arthroplasty from 2005 to 2011. J Arthroplast. 2015;30(1):15. doi:10.1016/j.arth.2014.08.025.
8. Su EP, Su SL. Femoral neck fractures: a changing paradigm. Bone Joint J. 2014;96-b(11) Supple A):43. doi:10.1302/0301-620X.96B11.34334.
9. Ahn J, Man LX, Park S, Sodl JF, Esterhai JL. Systematic review of cemented and uncemented hemiarthroplasty outcomes for femoral neck fractures. Clin Orthop Relat Res. 2008;466(10):2513. doi:10.1007/s11999-008-0368-3.
10. Alolabi B, Bajammal S, Shirali J, Karanicolas PJ, Gafni A, Bhandari M. Treatment of displaced femoral neck fractures in the elderly: a cost-benefit analysis. J Orthop Trauma. 2009;23(6):442. doi:10.1097/BOT.0b013e31817614dd.
11. Bentler SE, Liu L, Obrizan M, et al. The aftermath of hip fracture: discharge placement, functional status change, and mortality. Am J Epidemiol. 2009;170(10):1290. doi:10.1093/aje/kwp266.
12. Brox WT, Chan PH, Cafri G, Inacio MC. Similar mortality with general or regional anesthesia in elderly hip fracture patients. Acta Orthop. 2016;87(2):152. doi:10.3109/17453674.2015.1128781.
13. Catal B, Sener M. Treatment and displacement affect the reoperation rate for femoral neck fracture. Clin Orthop Relat Res. 2013;471(12):4096. doi:10.1007/s11999-013-3295-x.
14. Dailiana Z, Papakostidou I, Varitimidis S, Michalitsis S, Veloni A, Malizos K. Surgical treatment of hip fractures: factors influencing mortality. Hippokratia. 2013;17(3):252.
15. Deangelis JP, Ademi A, Staff I, Lewis CG. Cemented versus uncemented hemiarthroplasty for displaced femoral neck fractures: a prospective randomized trial with early follow-up. J Orthop Trauma. 2012;26(3):135. doi:10.1097/BOT.0b013e318238b7a5.
16. Hedbeck CJ, Inngul C, Blomfeldt R, Ponzer S, Tornkvist H, Enocson A. Internal fixation versus cemented hemiarthroplasty for displaced femoral neck fractures in patients with severe cognitive dysfunction: a randomized controlled trial. J Orthop Trauma. 2013;27(12):690. doi:10.1097/BOT.0b013e318291f544.
17. Jia Z, Ding F, Wu Y, et al. Unipolar versus bipolar hemiarthroplasty for displaced femoral neck fractures: a systematic review and meta-analysis of randomized controlled trials. J Orthop Surg Res. 2015;10:8. doi:10.1186/s13018-015-0165-0.
18. Lapidus LJ, Charalampidis A, Rundgren J, Enocson A. Internal fixation of garden I and II femoral neck fractures: posterior tilt did not influence the reoperation rate in 382 consecutive hips followed for a minimum of 5 years. J Orthop Trauma. 2013;27(7):386. doi:10.1097/BOT.0b013e318281da6e.
19. Mariconda M, Costa GG, Cerbasi S, et al. Factors predicting mobility and the change in Activities of Daily Living After hip fracture: A 1-year prospective cohort study. J Orthop Trauma. 2016;30(2):71. doi:10.1097/BOT.0000000000000448.
20. Nyholm AM, Gromov K, Palm H, et al. Time to surgery is associated with thirty-day and ninety-day mortality After proximal femoral fracture: A retrospective observational study on prospectively collected data from the Danish Fracture Database Collaborators. J Bone Joint Surg. (American) 2015;97(16):1333. doi:10.2106/JBJS.O.00029.
21. Samuel AM, Russo GS, Lukasiewicz AM, et al. Surgical treatment of femoral neck fractures after 24 hours in patients between the ages of 18 and 49 is associated with poor inpatient outcomes: an analysis of 1361 patients in the National Trauma Data Bank. J Orthop Trauma. 2016;30(2):89. doi:10.1097/BOT.0000000000000456.
22. Yu L, Wang Y, Chen J. Total hip arthroplasty versus hemiarthroplasty for displaced femoral neck fractures: meta-analysis of randomized trials. Clin Orthop Relat Res. 2012;470(8):2235. doi:10.1007/s11999-012-2293-8.
23. Zi-Sheng A, You-Shui G, Zhi-Zhen J, Ting Y, Chang-Qing Z. Hemiarthroplasty vs primary total hip arthroplasty for displaced fractures of the femoral neck in the elderly: a meta-analysis. J Arthroplast. 2012;27(4):583. doi:10.1016/j.arth.2011.07.009.
24. Zielinski SM, Keijsers NL, Praet SF, et al. Functional outcome after successful internal fixation versus salvage arthroplasty of patients with a femoral neck fracture. J Orthop Trauma. 2014;28(12):e273. doi:10.1097/BOT.0000000000000123.
25. Gu Q, Koenig L, Mather RC, 3rd, Tongue J. Surgery for hip fracture yields societal benefits that exceed the direct medical costs. Clin Orthop Relat Res. 2014;472(11):3536. doi:10.1007/s11999-014-3820-6.
26. Forsh DA, Ferguson TA. Contemporary management of femoral neck fractures: the young and the old. Curr Rev Musculoskelet Med. 2012;5(3):214. doi:10.1007/s12178-012-9127-x.
27. Macaulay W, Pagnotto MR, Iorio R, Mont MA, Saleh KJ. Displaced femoral neck fractures in the elderly: hemiarthroplasty versus total hip arthroplasty. J Am Acad Orthop Surg. 2006;14(5):287. doi:10.5435/00124635-200605000-00004.
28. Miyamoto RG, Kaplan KM, Levine BR, Egol KA, Zuckerman JD. Surgical management of hip fractures: an evidence-based review of the literature. I: Femoral neck fractures. J Am Acad Orthop Surg. 2008;16(10):596. doi:10.5435/00124635-200810000-00005.
29. Probe R, Ward R. Internal fixation of femoral neck fractures. J Am Acad Orthop Surg. 2006;14(9):565. doi:10.5435/00124635-200609000-00006.
30. Jain NB, Losina E, Ward DM, Harris MB, Katz JN. Trends in surgical management of femoral neck fractures in the United States. Clin Orthop Relat Res. 2008;466(12):3116. doi:10.1007/s11999-008-0392-3.
31. Menendez ME, Neuhaus V, van Dijk CN, Ring D. The Elixhauser comorbidity method outperforms the Charlson index in predicting inpatient death after orthopaedic surgery. Clin Orthop Relat Res. 2014;472(9):2878. doi:10.1007/s11999-014-3686-7.
32. Van Walraven C, Austin PC, Jennings A, Quan H, Forster AJ. A modification of the Elixhauser Comorbidity measures into a point system for hospital death using administrative data. Med Care. 2009;47(6):626-633.
33. Best MJ, Buller LT, Falakassa J, Vecchione D. Risk factors for nonroutine discharge in patients undergoing spinal fusion for intervertebral disc disorders. Iowa Orthop J. 2015;35:147.
34. Schairer WW, Lane JM, Halsey DA, Iorio R, Padgett DE, McLawhorn AS. The Frank Stinchfield award: total hip arthroplasty for femoral neck fracture is not a typical DRG 470: A propensity-matched cohort study. Clin Orthop Relat Res. 2017;475(2):353-360. doi:10.1007/s11999-016-4868-2.
35. Nikkel LE, Fox EJ, Black KP, Davis C, Andersen L, Hollenbeak CS. Impact of comorbidities on hospitalization costs following hip fracture. J Bone Joint Surg Am. 2012;94(1):9. doi:10.2106/JBJS.J.01077.
36. Bilezikian JP. Efficacy of bisphosphonates in reducing fracture risk in postmenopausal osteoporosis. Am J Med. 2009;122(2 Suppl.):S14. doi:10.1016/j.amjmed.2008.12.003.
37. Siris ES, Pasquale MK, Wang Y, Watts NB. Estimating bisphosphonate use and fracture reduction among US women aged 45 years and older, 2001-2008. J Bone Miner Res Off J Am Soc Bone Miner Res. 2011;26(1):3. doi:10.1002/jbmr.189.
TAKE-HOME POINTS
- The femoral neck patient population is older and has more medical comorbidities.
- Hemiarthroplasty (HA) is being performed more commonly in patients > 50 years old for femoral neck fractures.
- Open reduction and internal fixation is being performed more commonly in patients > 80 years old for femoral neck fractures.
- The rate of adverse events following femoral neck fracture is higher in the total hip arthroplasty (THA) group than in the HA group.
- THA is an independent risk factor for adverse events following femoral neck fracture.
Bring Schwartz Rounds to your hospital
A more emotional approach to rounds
If you are not doing Schwartz Rounds, get them started. ASAP.
I recently completed a 4-year tenure as physician moderator for our hospital’s Schwartz Rounds. An amazing team at my hospital helped pull the bimonthly sessions together. These compassionate care rounds are a national initiative to help foster empathy and compassion in the health care setting.
We gather a panel of two to three people involved in our patient presentation who share and move quickly through the clinical details, and head on toward the thornier ethical issues, emotional triggers, and responses. The best sessions are when the audience’s voice is heard for the bulk of the time.
The emotional cadence flows from boiling in frustration, drowning in tears, followed by comfort, and ending in thoughts for the next session. It is a more powerful arc than an episode of the television program “This is Us.” Largely, because this was us. This was real life. Real-time catharsis in the hospital.
In the daily grind, we often skip the step of processing our frustration, sadness, and anger, moving right on to the next patient and walking into the next room with that stoic layer of equanimity. I walk the hallways and find I grab my phone to catch up on emails, walking to the wrong floor because I’m not paying attention. Always something to do, someone to talk to, a family to call, pagers going off, phone calls. When do we sit and reflect?
These Schwartz Rounds are those moments of reflection – a slowdown in the day to think more deeply about the case. We talk about everything and anything. We have discussions with opposing views:
“Everything should have been done!”
“How did you not stop care?!”
“I agree with the doctors.”
“I can see the patient’s view more clearly now.”
Our first Schwartz Rounds tended to be end-of-life stories, particularly regarding the family mantra of “Do everything.” The health care team watches the suffering of a patient, a family, in a seemingly futile situation. Conversations around the end of life, choices, and quality of life are cut short daily by family members who simply recite, “Do everything.”
After several of these sessions, a case swings us in the other direction. The elderly gentleman with treatable cancer, who could easily survive another 20 years, declines treatment. “I’m fine, doc; I’ve lived long enough.” His wife at his bedside, shaking her head, tells us, “I don’t know why he wants to give up. He’s been as stubborn as a mule since the day I met him.” I spend 30 minutes convincing him to stay. The nurse does the same. Now we have a patient with a “Do nothing.” The patient’s decisions conflict with the family and the health care team.
Every day in the hospital provides a new ethical dilemma, a frustrating case, a challenging patient. Fodder for rounds.
Read the full post at hospitalleader.org.
Dr. Messler is a hospitalist at Morton Plant Hospitalist group in Clearwater, Fla. He previously chaired SHM’s Quality and Patient Safety Committee and has been active in several SHM mentoring programs, most recently with Project BOOST and Glycemic Control.
Also on The Hospital Leader
- Incubating Success: How We Used Structured Feedback to Reduce A Dangerous Practice by Rich Bottner, PA-C & Victoria Valencia, MPH
- New SoHM Report Provides Unique Window into Hospital Medicine Practice Trends by Leslie Flores, MHA, SFHM
- IGNITE Change: Improving Care via Interprofessional Clinical Learning Environments by Vineet Arora, MD, MAPP, MHM
A more emotional approach to rounds
A more emotional approach to rounds
If you are not doing Schwartz Rounds, get them started. ASAP.
I recently completed a 4-year tenure as physician moderator for our hospital’s Schwartz Rounds. An amazing team at my hospital helped pull the bimonthly sessions together. These compassionate care rounds are a national initiative to help foster empathy and compassion in the health care setting.
We gather a panel of two to three people involved in our patient presentation who share and move quickly through the clinical details, and head on toward the thornier ethical issues, emotional triggers, and responses. The best sessions are when the audience’s voice is heard for the bulk of the time.
The emotional cadence flows from boiling in frustration, drowning in tears, followed by comfort, and ending in thoughts for the next session. It is a more powerful arc than an episode of the television program “This is Us.” Largely, because this was us. This was real life. Real-time catharsis in the hospital.
In the daily grind, we often skip the step of processing our frustration, sadness, and anger, moving right on to the next patient and walking into the next room with that stoic layer of equanimity. I walk the hallways and find I grab my phone to catch up on emails, walking to the wrong floor because I’m not paying attention. Always something to do, someone to talk to, a family to call, pagers going off, phone calls. When do we sit and reflect?
These Schwartz Rounds are those moments of reflection – a slowdown in the day to think more deeply about the case. We talk about everything and anything. We have discussions with opposing views:
“Everything should have been done!”
“How did you not stop care?!”
“I agree with the doctors.”
“I can see the patient’s view more clearly now.”
Our first Schwartz Rounds tended to be end-of-life stories, particularly regarding the family mantra of “Do everything.” The health care team watches the suffering of a patient, a family, in a seemingly futile situation. Conversations around the end of life, choices, and quality of life are cut short daily by family members who simply recite, “Do everything.”
After several of these sessions, a case swings us in the other direction. The elderly gentleman with treatable cancer, who could easily survive another 20 years, declines treatment. “I’m fine, doc; I’ve lived long enough.” His wife at his bedside, shaking her head, tells us, “I don’t know why he wants to give up. He’s been as stubborn as a mule since the day I met him.” I spend 30 minutes convincing him to stay. The nurse does the same. Now we have a patient with a “Do nothing.” The patient’s decisions conflict with the family and the health care team.
Every day in the hospital provides a new ethical dilemma, a frustrating case, a challenging patient. Fodder for rounds.
Read the full post at hospitalleader.org.
Dr. Messler is a hospitalist at Morton Plant Hospitalist group in Clearwater, Fla. He previously chaired SHM’s Quality and Patient Safety Committee and has been active in several SHM mentoring programs, most recently with Project BOOST and Glycemic Control.
Also on The Hospital Leader
- Incubating Success: How We Used Structured Feedback to Reduce A Dangerous Practice by Rich Bottner, PA-C & Victoria Valencia, MPH
- New SoHM Report Provides Unique Window into Hospital Medicine Practice Trends by Leslie Flores, MHA, SFHM
- IGNITE Change: Improving Care via Interprofessional Clinical Learning Environments by Vineet Arora, MD, MAPP, MHM
If you are not doing Schwartz Rounds, get them started. ASAP.
I recently completed a 4-year tenure as physician moderator for our hospital’s Schwartz Rounds. An amazing team at my hospital helped pull the bimonthly sessions together. These compassionate care rounds are a national initiative to help foster empathy and compassion in the health care setting.
We gather a panel of two to three people involved in our patient presentation who share and move quickly through the clinical details, and head on toward the thornier ethical issues, emotional triggers, and responses. The best sessions are when the audience’s voice is heard for the bulk of the time.
The emotional cadence flows from boiling in frustration, drowning in tears, followed by comfort, and ending in thoughts for the next session. It is a more powerful arc than an episode of the television program “This is Us.” Largely, because this was us. This was real life. Real-time catharsis in the hospital.
In the daily grind, we often skip the step of processing our frustration, sadness, and anger, moving right on to the next patient and walking into the next room with that stoic layer of equanimity. I walk the hallways and find I grab my phone to catch up on emails, walking to the wrong floor because I’m not paying attention. Always something to do, someone to talk to, a family to call, pagers going off, phone calls. When do we sit and reflect?
These Schwartz Rounds are those moments of reflection – a slowdown in the day to think more deeply about the case. We talk about everything and anything. We have discussions with opposing views:
“Everything should have been done!”
“How did you not stop care?!”
“I agree with the doctors.”
“I can see the patient’s view more clearly now.”
Our first Schwartz Rounds tended to be end-of-life stories, particularly regarding the family mantra of “Do everything.” The health care team watches the suffering of a patient, a family, in a seemingly futile situation. Conversations around the end of life, choices, and quality of life are cut short daily by family members who simply recite, “Do everything.”
After several of these sessions, a case swings us in the other direction. The elderly gentleman with treatable cancer, who could easily survive another 20 years, declines treatment. “I’m fine, doc; I’ve lived long enough.” His wife at his bedside, shaking her head, tells us, “I don’t know why he wants to give up. He’s been as stubborn as a mule since the day I met him.” I spend 30 minutes convincing him to stay. The nurse does the same. Now we have a patient with a “Do nothing.” The patient’s decisions conflict with the family and the health care team.
Every day in the hospital provides a new ethical dilemma, a frustrating case, a challenging patient. Fodder for rounds.
Read the full post at hospitalleader.org.
Dr. Messler is a hospitalist at Morton Plant Hospitalist group in Clearwater, Fla. He previously chaired SHM’s Quality and Patient Safety Committee and has been active in several SHM mentoring programs, most recently with Project BOOST and Glycemic Control.
Also on The Hospital Leader
- Incubating Success: How We Used Structured Feedback to Reduce A Dangerous Practice by Rich Bottner, PA-C & Victoria Valencia, MPH
- New SoHM Report Provides Unique Window into Hospital Medicine Practice Trends by Leslie Flores, MHA, SFHM
- IGNITE Change: Improving Care via Interprofessional Clinical Learning Environments by Vineet Arora, MD, MAPP, MHM
Part D proposal includes prior authorization, step therapy
Rules governing the six protected medication classes covered by Medicare Part D could change under a proposal that would allow for utilization management or potential formulary exclusion of a drug for price increases.
Currently, Medicare Part D prescription drug benefit plans must cover “all or substantially all” approved drugs in six classes (antidepressants, antipsychotics, anticonvulsants, antiretrovirals, and antineoplastics). The proposed rule would allow three exceptions aimed at giving plans more negotiating leverage to help lower prices.
Plans would be allowed to implement prior authorization and step therapy for protected-class drugs, “including to determine use for a protected class indication,” according to a fact sheet. They also could exclude a protected-class drug from their formulary “if the drug represents only a new formulation of an existing single-source drug or biological product, regardless of whether the older formulation remains on the market.”
This does not change requirements that at least two drugs per class be covered, Seema Verma, administrator of the Centers for Medicare & Medicaid Services, said at a briefing. “In some classes, there are lots of competitors. For example, for antidepressants, there are lots of new generics available, so we see plans being in a very strengthened negotiating position. But in other classes, where there may not be as many drugs that are available, you might not see the same type of step therapy and prior authorization because there are just not that many options. It is really going to depend on the class of drugs and what’s available and the plans’ ability to negotiate discounts with manufacturers.”
Plans could exclude a protected-class drug if its price had increased greater than inflation, Ms. Verma said, but they could not use this to not cover any drugs in a class if available options are limited to one or two drugs.
“Foremost in our minds was the impact on patients and ensuring affordability and access to prescription drugs,” Ms. Verma said.
Oncologists don’t seem to agree.
“For the first time ever, Medicare patients with cancer and other serious diseases [who] rely on drugs in these protected therapeutic categories, will no longer have guaranteed access to potentially life-saving drugs. Instead, they will be subjected to ‘fail first’ step therapy and formulary restrictions that potentially restrict them from receiving the evidence-based therapies that their trained physicians prescribe as first-line cancer treatment,” Jeff Vacirca, MD, president of the Community Oncology Alliance, said in a statement. “Step therapy requirements are driven by financial interests to save money and not by what is in the best medical interest of patients. Treatment decisions are made by nameless and faceless corporate bureaucrats who are often not board certified in the diseases they are making coverage decisions over.”
AGA is concerned that these proposed changes will limit access for current and future beneficiaries and will add to the growing regulatory burden that physicians already face.
The proposal also would codify a policy implemented for 2019 that allows Medicare Advantage to implement step therapy tools for Part B drugs. And like the 2019 policy, the proposal would apply to new medication starts only, must be reviewed by a plan’s pharmacy and therapeutics committee, and must have an expedited exceptions process.
The proposal also specifically allows pharmacists to advise Part D beneficiaries on lower-cost options – something current regulations prohibit – and would require Part D explanation of benefits forms to include drug pricing information and lower-cost therapeutic alternatives.
The proposal is part of a broader update for Medicare Parts C and D in 2020 issued by CMS. It was published online Nov. 26 and is scheduled for publication in the Federal Register on Nov. 30. Comments can be made at www.regulations.gov through Jan. 25, 2019.
Rules governing the six protected medication classes covered by Medicare Part D could change under a proposal that would allow for utilization management or potential formulary exclusion of a drug for price increases.
Currently, Medicare Part D prescription drug benefit plans must cover “all or substantially all” approved drugs in six classes (antidepressants, antipsychotics, anticonvulsants, antiretrovirals, and antineoplastics). The proposed rule would allow three exceptions aimed at giving plans more negotiating leverage to help lower prices.
Plans would be allowed to implement prior authorization and step therapy for protected-class drugs, “including to determine use for a protected class indication,” according to a fact sheet. They also could exclude a protected-class drug from their formulary “if the drug represents only a new formulation of an existing single-source drug or biological product, regardless of whether the older formulation remains on the market.”
This does not change requirements that at least two drugs per class be covered, Seema Verma, administrator of the Centers for Medicare & Medicaid Services, said at a briefing. “In some classes, there are lots of competitors. For example, for antidepressants, there are lots of new generics available, so we see plans being in a very strengthened negotiating position. But in other classes, where there may not be as many drugs that are available, you might not see the same type of step therapy and prior authorization because there are just not that many options. It is really going to depend on the class of drugs and what’s available and the plans’ ability to negotiate discounts with manufacturers.”
Plans could exclude a protected-class drug if its price had increased greater than inflation, Ms. Verma said, but they could not use this to not cover any drugs in a class if available options are limited to one or two drugs.
“Foremost in our minds was the impact on patients and ensuring affordability and access to prescription drugs,” Ms. Verma said.
Oncologists don’t seem to agree.
“For the first time ever, Medicare patients with cancer and other serious diseases [who] rely on drugs in these protected therapeutic categories, will no longer have guaranteed access to potentially life-saving drugs. Instead, they will be subjected to ‘fail first’ step therapy and formulary restrictions that potentially restrict them from receiving the evidence-based therapies that their trained physicians prescribe as first-line cancer treatment,” Jeff Vacirca, MD, president of the Community Oncology Alliance, said in a statement. “Step therapy requirements are driven by financial interests to save money and not by what is in the best medical interest of patients. Treatment decisions are made by nameless and faceless corporate bureaucrats who are often not board certified in the diseases they are making coverage decisions over.”
AGA is concerned that these proposed changes will limit access for current and future beneficiaries and will add to the growing regulatory burden that physicians already face.
The proposal also would codify a policy implemented for 2019 that allows Medicare Advantage to implement step therapy tools for Part B drugs. And like the 2019 policy, the proposal would apply to new medication starts only, must be reviewed by a plan’s pharmacy and therapeutics committee, and must have an expedited exceptions process.
The proposal also specifically allows pharmacists to advise Part D beneficiaries on lower-cost options – something current regulations prohibit – and would require Part D explanation of benefits forms to include drug pricing information and lower-cost therapeutic alternatives.
The proposal is part of a broader update for Medicare Parts C and D in 2020 issued by CMS. It was published online Nov. 26 and is scheduled for publication in the Federal Register on Nov. 30. Comments can be made at www.regulations.gov through Jan. 25, 2019.
Rules governing the six protected medication classes covered by Medicare Part D could change under a proposal that would allow for utilization management or potential formulary exclusion of a drug for price increases.
Currently, Medicare Part D prescription drug benefit plans must cover “all or substantially all” approved drugs in six classes (antidepressants, antipsychotics, anticonvulsants, antiretrovirals, and antineoplastics). The proposed rule would allow three exceptions aimed at giving plans more negotiating leverage to help lower prices.
Plans would be allowed to implement prior authorization and step therapy for protected-class drugs, “including to determine use for a protected class indication,” according to a fact sheet. They also could exclude a protected-class drug from their formulary “if the drug represents only a new formulation of an existing single-source drug or biological product, regardless of whether the older formulation remains on the market.”
This does not change requirements that at least two drugs per class be covered, Seema Verma, administrator of the Centers for Medicare & Medicaid Services, said at a briefing. “In some classes, there are lots of competitors. For example, for antidepressants, there are lots of new generics available, so we see plans being in a very strengthened negotiating position. But in other classes, where there may not be as many drugs that are available, you might not see the same type of step therapy and prior authorization because there are just not that many options. It is really going to depend on the class of drugs and what’s available and the plans’ ability to negotiate discounts with manufacturers.”
Plans could exclude a protected-class drug if its price had increased greater than inflation, Ms. Verma said, but they could not use this to not cover any drugs in a class if available options are limited to one or two drugs.
“Foremost in our minds was the impact on patients and ensuring affordability and access to prescription drugs,” Ms. Verma said.
Oncologists don’t seem to agree.
“For the first time ever, Medicare patients with cancer and other serious diseases [who] rely on drugs in these protected therapeutic categories, will no longer have guaranteed access to potentially life-saving drugs. Instead, they will be subjected to ‘fail first’ step therapy and formulary restrictions that potentially restrict them from receiving the evidence-based therapies that their trained physicians prescribe as first-line cancer treatment,” Jeff Vacirca, MD, president of the Community Oncology Alliance, said in a statement. “Step therapy requirements are driven by financial interests to save money and not by what is in the best medical interest of patients. Treatment decisions are made by nameless and faceless corporate bureaucrats who are often not board certified in the diseases they are making coverage decisions over.”
AGA is concerned that these proposed changes will limit access for current and future beneficiaries and will add to the growing regulatory burden that physicians already face.
The proposal also would codify a policy implemented for 2019 that allows Medicare Advantage to implement step therapy tools for Part B drugs. And like the 2019 policy, the proposal would apply to new medication starts only, must be reviewed by a plan’s pharmacy and therapeutics committee, and must have an expedited exceptions process.
The proposal also specifically allows pharmacists to advise Part D beneficiaries on lower-cost options – something current regulations prohibit – and would require Part D explanation of benefits forms to include drug pricing information and lower-cost therapeutic alternatives.
The proposal is part of a broader update for Medicare Parts C and D in 2020 issued by CMS. It was published online Nov. 26 and is scheduled for publication in the Federal Register on Nov. 30. Comments can be made at www.regulations.gov through Jan. 25, 2019.














