User login
Aripiprazole/clozapine combo more effective than monotherapies
Certain antipsychotic polytherapies, including aripiprazole and clozapine, are associated with a lower risk of psychiatric rehospitalization in patients with schizophrenia, according to Jari Tiihonen, MD, PhD, of the Karolinska Institute in Stockholm, and his associates.
The study population included a total of 62,250 patients from the Finnish Hospital Discharge register who were treated for schizophrenia in the inpatient setting from 1972 to 2014. The median patient age was 45.6 years and the median length of follow-up was 14.1 years. Over the study period, 58.8% of this cohort were readmitted for psychiatric inpatient care, 67.2% used antipsychotic polypharmacy during the follow-up, and 57.5% were exposed to antipsychotic polypharmacy for at least 90 days, Dr. Tiihonen and his associates wrote in JAMA Psychiatry.
The combination of aripiprazole and clozapine was associated with the lowest risk of psychiatric rehospitalization, compared with those who received no therapy (hazard ratio, 0.42, 95% confidence interval, 0.39-0.46). Clozapine alone was the most effective antipsychotic monotherapy (HR, 0.49; 95% CI, 0.47-0.51), and when aripiprazole/clozapine was compared with clozapine alone, the polytherapy was significantly more effective (HR, 0.86; 95% CI, 0.79-0.94).
The difference between aripiprazole/clozapine and clozapine alone was even greater in patients who initially were hospitalized for their first episode of schizophrenia (HR, 0.78; 95% CI, 0.63-0.96). Overall, any antipsychotic polypharmacy was associated with a 7%-13% lower risk of hospitalization, compared with any monotherapy; , the authors noted.
“It should be acknowledged that statements about a preferential use of antipsychotic monotherapy for maintenance treatment of schizophrenia lack evidence, and that currently available evidence – although gathered with few nonrandomized cohort studies that have their own limitations – indicates the opposite,” they concluded.
Dr. Tiihonen and several of his associates reported numerous conflicts of interest.
SOURCE: Tiihonen J et al. JAMA Psychiatry. 2019 Feb 20. doi: 10.1001/jamapsychiatry.2018.4320.
Certain antipsychotic polytherapies, including aripiprazole and clozapine, are associated with a lower risk of psychiatric rehospitalization in patients with schizophrenia, according to Jari Tiihonen, MD, PhD, of the Karolinska Institute in Stockholm, and his associates.
The study population included a total of 62,250 patients from the Finnish Hospital Discharge register who were treated for schizophrenia in the inpatient setting from 1972 to 2014. The median patient age was 45.6 years and the median length of follow-up was 14.1 years. Over the study period, 58.8% of this cohort were readmitted for psychiatric inpatient care, 67.2% used antipsychotic polypharmacy during the follow-up, and 57.5% were exposed to antipsychotic polypharmacy for at least 90 days, Dr. Tiihonen and his associates wrote in JAMA Psychiatry.
The combination of aripiprazole and clozapine was associated with the lowest risk of psychiatric rehospitalization, compared with those who received no therapy (hazard ratio, 0.42, 95% confidence interval, 0.39-0.46). Clozapine alone was the most effective antipsychotic monotherapy (HR, 0.49; 95% CI, 0.47-0.51), and when aripiprazole/clozapine was compared with clozapine alone, the polytherapy was significantly more effective (HR, 0.86; 95% CI, 0.79-0.94).
The difference between aripiprazole/clozapine and clozapine alone was even greater in patients who initially were hospitalized for their first episode of schizophrenia (HR, 0.78; 95% CI, 0.63-0.96). Overall, any antipsychotic polypharmacy was associated with a 7%-13% lower risk of hospitalization, compared with any monotherapy; , the authors noted.
“It should be acknowledged that statements about a preferential use of antipsychotic monotherapy for maintenance treatment of schizophrenia lack evidence, and that currently available evidence – although gathered with few nonrandomized cohort studies that have their own limitations – indicates the opposite,” they concluded.
Dr. Tiihonen and several of his associates reported numerous conflicts of interest.
SOURCE: Tiihonen J et al. JAMA Psychiatry. 2019 Feb 20. doi: 10.1001/jamapsychiatry.2018.4320.
Certain antipsychotic polytherapies, including aripiprazole and clozapine, are associated with a lower risk of psychiatric rehospitalization in patients with schizophrenia, according to Jari Tiihonen, MD, PhD, of the Karolinska Institute in Stockholm, and his associates.
The study population included a total of 62,250 patients from the Finnish Hospital Discharge register who were treated for schizophrenia in the inpatient setting from 1972 to 2014. The median patient age was 45.6 years and the median length of follow-up was 14.1 years. Over the study period, 58.8% of this cohort were readmitted for psychiatric inpatient care, 67.2% used antipsychotic polypharmacy during the follow-up, and 57.5% were exposed to antipsychotic polypharmacy for at least 90 days, Dr. Tiihonen and his associates wrote in JAMA Psychiatry.
The combination of aripiprazole and clozapine was associated with the lowest risk of psychiatric rehospitalization, compared with those who received no therapy (hazard ratio, 0.42, 95% confidence interval, 0.39-0.46). Clozapine alone was the most effective antipsychotic monotherapy (HR, 0.49; 95% CI, 0.47-0.51), and when aripiprazole/clozapine was compared with clozapine alone, the polytherapy was significantly more effective (HR, 0.86; 95% CI, 0.79-0.94).
The difference between aripiprazole/clozapine and clozapine alone was even greater in patients who initially were hospitalized for their first episode of schizophrenia (HR, 0.78; 95% CI, 0.63-0.96). Overall, any antipsychotic polypharmacy was associated with a 7%-13% lower risk of hospitalization, compared with any monotherapy; , the authors noted.
“It should be acknowledged that statements about a preferential use of antipsychotic monotherapy for maintenance treatment of schizophrenia lack evidence, and that currently available evidence – although gathered with few nonrandomized cohort studies that have their own limitations – indicates the opposite,” they concluded.
Dr. Tiihonen and several of his associates reported numerous conflicts of interest.
SOURCE: Tiihonen J et al. JAMA Psychiatry. 2019 Feb 20. doi: 10.1001/jamapsychiatry.2018.4320.
FROM JAMA PSYCHIATRY
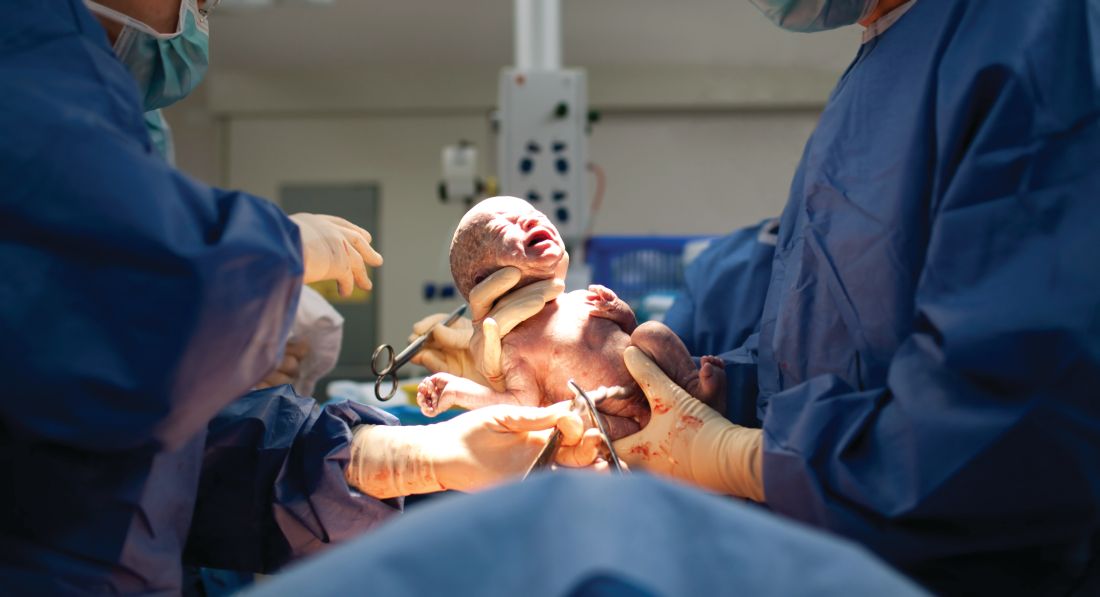
Delayed cord clamping didn’t drop maternal hemoglobin in term cesarean deliveries
LAS VEGAS – according to a recent study.
The change in maternal hemoglobin from preoperative level to postoperative day 1, the study’s primary outcome measure, was not significantly different whether the umbilical cord was clamped within 15 seconds of delivery or clamping was delayed for 1 minute.
For the 56 women who received immediate cord clamping, hemoglobin dropped a mean 1.78 g/dL; for the 57 women who received delayed cord clamping, the drop was 1.85 g/dL (P = .69). Mean estimated blood loss for the delayed clamping group was numerically higher at 884 mL, compared with 830 mL for the immediate clamping group, but this was not a statistically significant difference (P = .13)
However, the practice did result in significantly greater neonatal hemoglobin measured at 24-72 hours post delivery. Hemoglobin data were available for 90 infants, or about 80% of participants. For the 44 infants in the immediate clamping group, mean hemoglobin was 16.4 g/dL; for the delayed clamping group, the figure was 18.1 g/dL (P less than .01).
Although delayed cord clamping has clear benefits to the neonate, whether the practice adversely affects women undergoing cesarean was not clear, said Stephanie Purisch, MD, who discussed the findings of the two-site, randomized, clinical trial during a fellows research session at the meeting sponsored by the Society for Maternal-Fetal Medicine.
“Maternal outcomes have not been a focus of research” in the cord clamping literature, said Dr. Purisch, from Columbia University, New York. A 2013 Cochrane review found that delayed cord clamping did not change postpartum hemoglobin levels or increase blood loss or the need for transfusion. However, she said, the review included only healthy women who expected a vaginal delivery, so cesarean deliveries were undersampled in the data.
Of the 3,911 deliveries included in all prior randomized, controlled trials of delayed cord clamping, just 87, or 2.2%, were cesarean deliveries, she said. In cesarean deliveries, mean blood loss is double that of vaginal deliveries. Delayed clamping could further increase bleeding because the hysterotomy closure is delayed, said Dr. Purisch, so the question of safety in cesarean deliveries is clinically important.
Faced with this knowledge gap, Dr. Purisch and her colleagues constructed a prospective, randomized, controlled trial of delayed cord clamping in cesarean delivery at term, with the hypothesis that maternal blood loss would be increased by the practice.
Patients were eligible if they had singleton gestations with cesarean deliveries scheduled at 37 weeks’ gestation or more. Patients with known placentation problems, significant maternal or known fetal anemia, maternal bleeding disorders, and preeclampsia were excluded. The study also did not include pregnancies with known fetal anomalies or intrauterine growth retardation, or those in which cord blood banking was planned or the mother would refuse blood products.
In an intention-to-treat analysis, Dr. Purisch and her colleagues randomly assigned participants 1:1 to immediate cord clamping, defined as clamping the cord by 15 seconds after delivery, or delayed cord clamping, in which the umbilical cord was clamped 1 minute after delivery.
Oxytocin was routinely administered to each group on delivery, and there was no umbilical cord milking in either group. For the delayed-clamping group, the infant was kept at the level of the placenta and tended by the pediatric team during the minute before clamping. Dr. Purisch explained that cord clamping was performed before 60 seconds in the intervention group if needed for neonatal resuscitation.
Participants were similar in the two study arms, with a median gestational age of 39.1 weeks at delivery. Most women (60%-64%) had one prior cesarean delivery, with about a quarter having two or more prior cesarean deliveries. Preoperative maternal hemoglobin was 11.6-12.0 g/dL. About 41% of participants were Hispanic, and the median prepregnancy body mass index for participants was about 27 kg/m2.
Looking at secondary outcome measures, there was no difference in rates of postpartum hemorrhage or uterotonic administration between the two groups (P = .99 for both). Hemoglobin levels at postoperative day 1 were numerically higher for the delayed cord clamping group, but the difference wasn’t significant (10.2 vs. 9.8 g/dL; P = .18). Just two women, both in the immediate cord clamping group, required blood transfusions.
Additional neonatal secondary outcome measures included birth weight, Apgar scores at 1 and 5 minutes, the need for phototherapy for jaundice, and umbilical cord artery pH. There were no between-group differences except that umbilical cord artery pH was slightly lower in the delayed group (7.2 vs. 7.3; P = .04).
“Delayed cord clamping is not associated with increased maternal blood loss … but it does achieve higher neonatal hemoglobin levels at 24-72 hours of life,” said Dr. Purisch. “These results provide support for the application of current [American College of Obstetricians and Gynecologists] recommendations to women planned for cesarean delivery.”
The study was funded by the Columbia Maternal-Fetal Medicine Fellow Research Fund. Dr. Purisch reported no conflicts of interest.
SOURCE: Purisch, S. et al. Am J Obstet Gynecol. 2019 Jan;220(1):S37-38, Abstract 47.
LAS VEGAS – according to a recent study.
The change in maternal hemoglobin from preoperative level to postoperative day 1, the study’s primary outcome measure, was not significantly different whether the umbilical cord was clamped within 15 seconds of delivery or clamping was delayed for 1 minute.
For the 56 women who received immediate cord clamping, hemoglobin dropped a mean 1.78 g/dL; for the 57 women who received delayed cord clamping, the drop was 1.85 g/dL (P = .69). Mean estimated blood loss for the delayed clamping group was numerically higher at 884 mL, compared with 830 mL for the immediate clamping group, but this was not a statistically significant difference (P = .13)
However, the practice did result in significantly greater neonatal hemoglobin measured at 24-72 hours post delivery. Hemoglobin data were available for 90 infants, or about 80% of participants. For the 44 infants in the immediate clamping group, mean hemoglobin was 16.4 g/dL; for the delayed clamping group, the figure was 18.1 g/dL (P less than .01).
Although delayed cord clamping has clear benefits to the neonate, whether the practice adversely affects women undergoing cesarean was not clear, said Stephanie Purisch, MD, who discussed the findings of the two-site, randomized, clinical trial during a fellows research session at the meeting sponsored by the Society for Maternal-Fetal Medicine.
“Maternal outcomes have not been a focus of research” in the cord clamping literature, said Dr. Purisch, from Columbia University, New York. A 2013 Cochrane review found that delayed cord clamping did not change postpartum hemoglobin levels or increase blood loss or the need for transfusion. However, she said, the review included only healthy women who expected a vaginal delivery, so cesarean deliveries were undersampled in the data.
Of the 3,911 deliveries included in all prior randomized, controlled trials of delayed cord clamping, just 87, or 2.2%, were cesarean deliveries, she said. In cesarean deliveries, mean blood loss is double that of vaginal deliveries. Delayed clamping could further increase bleeding because the hysterotomy closure is delayed, said Dr. Purisch, so the question of safety in cesarean deliveries is clinically important.
Faced with this knowledge gap, Dr. Purisch and her colleagues constructed a prospective, randomized, controlled trial of delayed cord clamping in cesarean delivery at term, with the hypothesis that maternal blood loss would be increased by the practice.
Patients were eligible if they had singleton gestations with cesarean deliveries scheduled at 37 weeks’ gestation or more. Patients with known placentation problems, significant maternal or known fetal anemia, maternal bleeding disorders, and preeclampsia were excluded. The study also did not include pregnancies with known fetal anomalies or intrauterine growth retardation, or those in which cord blood banking was planned or the mother would refuse blood products.
In an intention-to-treat analysis, Dr. Purisch and her colleagues randomly assigned participants 1:1 to immediate cord clamping, defined as clamping the cord by 15 seconds after delivery, or delayed cord clamping, in which the umbilical cord was clamped 1 minute after delivery.
Oxytocin was routinely administered to each group on delivery, and there was no umbilical cord milking in either group. For the delayed-clamping group, the infant was kept at the level of the placenta and tended by the pediatric team during the minute before clamping. Dr. Purisch explained that cord clamping was performed before 60 seconds in the intervention group if needed for neonatal resuscitation.
Participants were similar in the two study arms, with a median gestational age of 39.1 weeks at delivery. Most women (60%-64%) had one prior cesarean delivery, with about a quarter having two or more prior cesarean deliveries. Preoperative maternal hemoglobin was 11.6-12.0 g/dL. About 41% of participants were Hispanic, and the median prepregnancy body mass index for participants was about 27 kg/m2.
Looking at secondary outcome measures, there was no difference in rates of postpartum hemorrhage or uterotonic administration between the two groups (P = .99 for both). Hemoglobin levels at postoperative day 1 were numerically higher for the delayed cord clamping group, but the difference wasn’t significant (10.2 vs. 9.8 g/dL; P = .18). Just two women, both in the immediate cord clamping group, required blood transfusions.
Additional neonatal secondary outcome measures included birth weight, Apgar scores at 1 and 5 minutes, the need for phototherapy for jaundice, and umbilical cord artery pH. There were no between-group differences except that umbilical cord artery pH was slightly lower in the delayed group (7.2 vs. 7.3; P = .04).
“Delayed cord clamping is not associated with increased maternal blood loss … but it does achieve higher neonatal hemoglobin levels at 24-72 hours of life,” said Dr. Purisch. “These results provide support for the application of current [American College of Obstetricians and Gynecologists] recommendations to women planned for cesarean delivery.”
The study was funded by the Columbia Maternal-Fetal Medicine Fellow Research Fund. Dr. Purisch reported no conflicts of interest.
SOURCE: Purisch, S. et al. Am J Obstet Gynecol. 2019 Jan;220(1):S37-38, Abstract 47.
LAS VEGAS – according to a recent study.
The change in maternal hemoglobin from preoperative level to postoperative day 1, the study’s primary outcome measure, was not significantly different whether the umbilical cord was clamped within 15 seconds of delivery or clamping was delayed for 1 minute.
For the 56 women who received immediate cord clamping, hemoglobin dropped a mean 1.78 g/dL; for the 57 women who received delayed cord clamping, the drop was 1.85 g/dL (P = .69). Mean estimated blood loss for the delayed clamping group was numerically higher at 884 mL, compared with 830 mL for the immediate clamping group, but this was not a statistically significant difference (P = .13)
However, the practice did result in significantly greater neonatal hemoglobin measured at 24-72 hours post delivery. Hemoglobin data were available for 90 infants, or about 80% of participants. For the 44 infants in the immediate clamping group, mean hemoglobin was 16.4 g/dL; for the delayed clamping group, the figure was 18.1 g/dL (P less than .01).
Although delayed cord clamping has clear benefits to the neonate, whether the practice adversely affects women undergoing cesarean was not clear, said Stephanie Purisch, MD, who discussed the findings of the two-site, randomized, clinical trial during a fellows research session at the meeting sponsored by the Society for Maternal-Fetal Medicine.
“Maternal outcomes have not been a focus of research” in the cord clamping literature, said Dr. Purisch, from Columbia University, New York. A 2013 Cochrane review found that delayed cord clamping did not change postpartum hemoglobin levels or increase blood loss or the need for transfusion. However, she said, the review included only healthy women who expected a vaginal delivery, so cesarean deliveries were undersampled in the data.
Of the 3,911 deliveries included in all prior randomized, controlled trials of delayed cord clamping, just 87, or 2.2%, were cesarean deliveries, she said. In cesarean deliveries, mean blood loss is double that of vaginal deliveries. Delayed clamping could further increase bleeding because the hysterotomy closure is delayed, said Dr. Purisch, so the question of safety in cesarean deliveries is clinically important.
Faced with this knowledge gap, Dr. Purisch and her colleagues constructed a prospective, randomized, controlled trial of delayed cord clamping in cesarean delivery at term, with the hypothesis that maternal blood loss would be increased by the practice.
Patients were eligible if they had singleton gestations with cesarean deliveries scheduled at 37 weeks’ gestation or more. Patients with known placentation problems, significant maternal or known fetal anemia, maternal bleeding disorders, and preeclampsia were excluded. The study also did not include pregnancies with known fetal anomalies or intrauterine growth retardation, or those in which cord blood banking was planned or the mother would refuse blood products.
In an intention-to-treat analysis, Dr. Purisch and her colleagues randomly assigned participants 1:1 to immediate cord clamping, defined as clamping the cord by 15 seconds after delivery, or delayed cord clamping, in which the umbilical cord was clamped 1 minute after delivery.
Oxytocin was routinely administered to each group on delivery, and there was no umbilical cord milking in either group. For the delayed-clamping group, the infant was kept at the level of the placenta and tended by the pediatric team during the minute before clamping. Dr. Purisch explained that cord clamping was performed before 60 seconds in the intervention group if needed for neonatal resuscitation.
Participants were similar in the two study arms, with a median gestational age of 39.1 weeks at delivery. Most women (60%-64%) had one prior cesarean delivery, with about a quarter having two or more prior cesarean deliveries. Preoperative maternal hemoglobin was 11.6-12.0 g/dL. About 41% of participants were Hispanic, and the median prepregnancy body mass index for participants was about 27 kg/m2.
Looking at secondary outcome measures, there was no difference in rates of postpartum hemorrhage or uterotonic administration between the two groups (P = .99 for both). Hemoglobin levels at postoperative day 1 were numerically higher for the delayed cord clamping group, but the difference wasn’t significant (10.2 vs. 9.8 g/dL; P = .18). Just two women, both in the immediate cord clamping group, required blood transfusions.
Additional neonatal secondary outcome measures included birth weight, Apgar scores at 1 and 5 minutes, the need for phototherapy for jaundice, and umbilical cord artery pH. There were no between-group differences except that umbilical cord artery pH was slightly lower in the delayed group (7.2 vs. 7.3; P = .04).
“Delayed cord clamping is not associated with increased maternal blood loss … but it does achieve higher neonatal hemoglobin levels at 24-72 hours of life,” said Dr. Purisch. “These results provide support for the application of current [American College of Obstetricians and Gynecologists] recommendations to women planned for cesarean delivery.”
The study was funded by the Columbia Maternal-Fetal Medicine Fellow Research Fund. Dr. Purisch reported no conflicts of interest.
SOURCE: Purisch, S. et al. Am J Obstet Gynecol. 2019 Jan;220(1):S37-38, Abstract 47.
REPORTING FROM THE PREGNANCY MEETING
Alcohol abstinence questioned as addiction treatment goal
BONITA SPRINGS, FLA. – Reductions in alcohol use bring about significant improvement in adverse consequences, mental health status, and quality of life, even if the reductions do not reach the level of abstinence, according to recent research presented at the annual meeting of the American Academy of Addiction Psychiatry.
The findings, experts say, demonstrate how a fixation on abstinence or elimination of all heavy drinking – the endpoints the Food and Drug Administration now require in pivotal clinical trials on alcohol use disorder (AUD) treatments – is shortsighted and can unnecessarily discourage people with alcohol use disorder from pursuing treatment.
“We need to think a little differently, or a little out of the box, from the way we’ve been thinking in the past,” said Raymond F. Anton, MD, professor of psychiatry at the Medical University of South Carolina in Charleston and chair of the Alcohol Clinical Trials Initiative (ACTIVE), a group advocating for a new endpoint that recognizes the benefits of lesser reductions in alcohol intake.
In a new analysis using data from the COMBINE study, researchers looked at the associations between reduction in World Health Organization drinking risk levels of alcohol consumption and clinically meaningful outcomes among people in treatment.
There are four levels: very high (more than 7.1 14-g drinks a day for men and more than 4.3 for women); high (4.3-7.1 or 2.9-4.3, respectively); moderate (2.9-4.3 or 1.4-2.9); and low (less than 2.9 or less than 1.4).
Researchers assessed responses to treatment with acamprosate, naltrexone, and psychological intervention in patients an average of 44 years old with 71% of their days being heavy drinking days. They found significant improvement in consequences tied to drinking, according to the Drinker Inventory of Consequences, and in mental health according to the Short Form Health Survey and the WHO Quality of Life assessment – even when the improvement was only by one WHO risk level – or just a few drinks a day – and did not involve abstaining (P less than .001 for all improvement categories).
“Reductions in WHO drinking risk levels are predictive of clinical benefit” or how the patient feels and functions, said Daniel Falk, PhD, health scientist administrator at the National Institute on Alcohol Abuse and Alcoholism.
The ACTIVE group he chairs, Dr. Anton said, is proposing that the FDA add a new endpoint for phase 3 trials: percentage of subjects who attain a 1- or 2-level reduction in WHO drinking risk levels.
Stephanie O’Malley, PhD, professor of psychiatry at Yale University in New Haven, Conn., said a 30-year-old with a moderate drinking problem – occasionally missing a family function, but never letting it interfere with work, say – might be turned off by a treatment plan that preaches abstinence, she said. Varenicline, for example, results in abstinence just 7% of the time, with some risk of suicidality and nausea. That person might not want to stop drinking entirely for the rest of his or her life, but could benefit by reducing the drinking, she said.
But 55% of the time, varenicline produces a reduction of one level of risk, which is associated with clinically meaningful results. That will sound much more appealing to a prospective patient, she said.
“From a clinical perspective, these WHO outcomes have some advantages,” she said. “I think you’re going to, one, encourage more people to accept treatment, and … be more optimistic about the outcomes.”
Dr. Anton reported consulting and/or funding from Alkermes, Allergan, Indivior, Insys Life Epigenetics, and Laboratori Farmaceutico CT. Dr. O’Malley reported consulting and/or funding from Alkermes, Amygdala, Indivior, Mistubishi Tanabe, Opiant, and other sources. Dr. Falk reported no disclosures.
BONITA SPRINGS, FLA. – Reductions in alcohol use bring about significant improvement in adverse consequences, mental health status, and quality of life, even if the reductions do not reach the level of abstinence, according to recent research presented at the annual meeting of the American Academy of Addiction Psychiatry.
The findings, experts say, demonstrate how a fixation on abstinence or elimination of all heavy drinking – the endpoints the Food and Drug Administration now require in pivotal clinical trials on alcohol use disorder (AUD) treatments – is shortsighted and can unnecessarily discourage people with alcohol use disorder from pursuing treatment.
“We need to think a little differently, or a little out of the box, from the way we’ve been thinking in the past,” said Raymond F. Anton, MD, professor of psychiatry at the Medical University of South Carolina in Charleston and chair of the Alcohol Clinical Trials Initiative (ACTIVE), a group advocating for a new endpoint that recognizes the benefits of lesser reductions in alcohol intake.
In a new analysis using data from the COMBINE study, researchers looked at the associations between reduction in World Health Organization drinking risk levels of alcohol consumption and clinically meaningful outcomes among people in treatment.
There are four levels: very high (more than 7.1 14-g drinks a day for men and more than 4.3 for women); high (4.3-7.1 or 2.9-4.3, respectively); moderate (2.9-4.3 or 1.4-2.9); and low (less than 2.9 or less than 1.4).
Researchers assessed responses to treatment with acamprosate, naltrexone, and psychological intervention in patients an average of 44 years old with 71% of their days being heavy drinking days. They found significant improvement in consequences tied to drinking, according to the Drinker Inventory of Consequences, and in mental health according to the Short Form Health Survey and the WHO Quality of Life assessment – even when the improvement was only by one WHO risk level – or just a few drinks a day – and did not involve abstaining (P less than .001 for all improvement categories).
“Reductions in WHO drinking risk levels are predictive of clinical benefit” or how the patient feels and functions, said Daniel Falk, PhD, health scientist administrator at the National Institute on Alcohol Abuse and Alcoholism.
The ACTIVE group he chairs, Dr. Anton said, is proposing that the FDA add a new endpoint for phase 3 trials: percentage of subjects who attain a 1- or 2-level reduction in WHO drinking risk levels.
Stephanie O’Malley, PhD, professor of psychiatry at Yale University in New Haven, Conn., said a 30-year-old with a moderate drinking problem – occasionally missing a family function, but never letting it interfere with work, say – might be turned off by a treatment plan that preaches abstinence, she said. Varenicline, for example, results in abstinence just 7% of the time, with some risk of suicidality and nausea. That person might not want to stop drinking entirely for the rest of his or her life, but could benefit by reducing the drinking, she said.
But 55% of the time, varenicline produces a reduction of one level of risk, which is associated with clinically meaningful results. That will sound much more appealing to a prospective patient, she said.
“From a clinical perspective, these WHO outcomes have some advantages,” she said. “I think you’re going to, one, encourage more people to accept treatment, and … be more optimistic about the outcomes.”
Dr. Anton reported consulting and/or funding from Alkermes, Allergan, Indivior, Insys Life Epigenetics, and Laboratori Farmaceutico CT. Dr. O’Malley reported consulting and/or funding from Alkermes, Amygdala, Indivior, Mistubishi Tanabe, Opiant, and other sources. Dr. Falk reported no disclosures.
BONITA SPRINGS, FLA. – Reductions in alcohol use bring about significant improvement in adverse consequences, mental health status, and quality of life, even if the reductions do not reach the level of abstinence, according to recent research presented at the annual meeting of the American Academy of Addiction Psychiatry.
The findings, experts say, demonstrate how a fixation on abstinence or elimination of all heavy drinking – the endpoints the Food and Drug Administration now require in pivotal clinical trials on alcohol use disorder (AUD) treatments – is shortsighted and can unnecessarily discourage people with alcohol use disorder from pursuing treatment.
“We need to think a little differently, or a little out of the box, from the way we’ve been thinking in the past,” said Raymond F. Anton, MD, professor of psychiatry at the Medical University of South Carolina in Charleston and chair of the Alcohol Clinical Trials Initiative (ACTIVE), a group advocating for a new endpoint that recognizes the benefits of lesser reductions in alcohol intake.
In a new analysis using data from the COMBINE study, researchers looked at the associations between reduction in World Health Organization drinking risk levels of alcohol consumption and clinically meaningful outcomes among people in treatment.
There are four levels: very high (more than 7.1 14-g drinks a day for men and more than 4.3 for women); high (4.3-7.1 or 2.9-4.3, respectively); moderate (2.9-4.3 or 1.4-2.9); and low (less than 2.9 or less than 1.4).
Researchers assessed responses to treatment with acamprosate, naltrexone, and psychological intervention in patients an average of 44 years old with 71% of their days being heavy drinking days. They found significant improvement in consequences tied to drinking, according to the Drinker Inventory of Consequences, and in mental health according to the Short Form Health Survey and the WHO Quality of Life assessment – even when the improvement was only by one WHO risk level – or just a few drinks a day – and did not involve abstaining (P less than .001 for all improvement categories).
“Reductions in WHO drinking risk levels are predictive of clinical benefit” or how the patient feels and functions, said Daniel Falk, PhD, health scientist administrator at the National Institute on Alcohol Abuse and Alcoholism.
The ACTIVE group he chairs, Dr. Anton said, is proposing that the FDA add a new endpoint for phase 3 trials: percentage of subjects who attain a 1- or 2-level reduction in WHO drinking risk levels.
Stephanie O’Malley, PhD, professor of psychiatry at Yale University in New Haven, Conn., said a 30-year-old with a moderate drinking problem – occasionally missing a family function, but never letting it interfere with work, say – might be turned off by a treatment plan that preaches abstinence, she said. Varenicline, for example, results in abstinence just 7% of the time, with some risk of suicidality and nausea. That person might not want to stop drinking entirely for the rest of his or her life, but could benefit by reducing the drinking, she said.
But 55% of the time, varenicline produces a reduction of one level of risk, which is associated with clinically meaningful results. That will sound much more appealing to a prospective patient, she said.
“From a clinical perspective, these WHO outcomes have some advantages,” she said. “I think you’re going to, one, encourage more people to accept treatment, and … be more optimistic about the outcomes.”
Dr. Anton reported consulting and/or funding from Alkermes, Allergan, Indivior, Insys Life Epigenetics, and Laboratori Farmaceutico CT. Dr. O’Malley reported consulting and/or funding from Alkermes, Amygdala, Indivior, Mistubishi Tanabe, Opiant, and other sources. Dr. Falk reported no disclosures.
REPORTING FROM AAAP 2018
Accurately predicting ADHD’s trajectory deemed almost impossible
LAS VEGAS – Despite the strides that clinicians like Anthony L. Rostain, MD, have made in better understanding and treating patients with ADHD, it remains virtually impossible to predict how a child with the disorder will fare in adulthood.
“We cannot predict the trajectory of the disorder,” Dr. Rostain said at an annual psychopharmacology update held by the Nevada Psychiatric Association. “We’re still learning about the variables that affect clinical course. There are many determinants to the trajectory.”
Dr. Rostain, professor of psychiatry and pediatrics at the University of Pennsylvania, Philadelphia, said ADHD commonly presents with numerous other neurodevelopmental disorders and with comorbid psychiatric conditions like bipolar disorder and anxiety.
“In psychiatry, we tend to see the more complicated patients, the ones with multiple comorbidities,” he said. “The most important change in the way we think about people with ADHD has to do with the growing emphasis on how it affects executive functions, in particular the cognitive, affective, and behavioral consequences of executive dysfunction. In this growingly complex world, with what some describe as ‘distracted minds’ emerging from being immersed in all our technology, it’s sometimes hard to tell: Is this person distracted because they’re always looking at their cell phone, or do they have intrinsic difficulty with managing attention?
“That’s going to become a greater challenge as children grow up in this world filled with shiny screens and devices that make [it] easier to connect with others but also harder to set a goal and follow it to its conclusion.”
ADHD changes over time, Dr. Rostain continued, but there is no single theory or biological explanation to explain its heterogeneity. “There is no cookie-cutter approach; you have to individualize when you are treating the individual in your office,” he said.
It is widely accepted that ADHD arises from biological factors, but social factors likely influence the degree of impairment, risk for comorbid disorders, and access to resources, said Dr. Rostain, who is also codirector of the developmental neuropsychiatry program at The Children’s Hospital of Philadelphia and medical director of the Adult ADHD Treatment and Research Program at Penn Medicine.
he said. “If there were one thing we could do to prevent ADHD, it might be to prevent pregnant women from drinking or to reduce poverty and violence, but that’s beyond the scope of this talk.”
He also noted that, because of epigenetics, ADHD risk factors express themselves early in some individuals and later in others. “We’re convinced that developmental disorders unfold in a nonlinear fashion,” he said. “Life [with ADHD] is curvy, not a straight line.”
Numerous studies of ADHD neurobiology have demonstrated frontal subcortical and cerebellar dysfunction – smaller striatal structures in particular. “In MRI studies, we also see difficulties with the differential maturation of important neural circuits, along with the persistence of cortical thickening where it should be thinning,” Dr. Rostain said. He went on to note that the normal brain consists of three main networks: the salience network, “which tells us whether to pay attention or to relax,” the attention and control network, and the default mode network, “which is where our mind goes when we’re daydreaming,” he said. “All of us are constantly switching between attention and daydreaming. That’s normal. In ADHD, the balance and synchrony between the default mode and the attention network is disrupted. Individuals with ADHD either remain too long in the default mode, or their attentional system isn’t powered up enough to keep them paying attention and following through during nonrewarding tasks.”
The presentation of ADHD symptoms tends to differ in children, compared with adults. For example, children with the disorder tend to be squirmy, can’t sit still, are restless, and can’t play or work quietly. On the other hand, adults tend to complain about inefficiencies at work, not being able to finish projects, not being able to sit through meetings. They tend to drive too quickly, and they often talk excessively, and make inappropriate comments. “The symptoms of ADHD emerge from disruptions or inefficiencies in basic functions, whether those are executive functions or motivational processes,” he said. “All of this is thought to be the result of genetic unfolding throughout the lifespan.”
The goal of ADHD medical therapy is to alter catecholamine tone in the prefrontal cortex, an area of the brain “designed to help us guide our thinking toward distal goals and navigate the world around us,” Dr. Rostain said. “It allows us also to inhibit actions that are task-irrelevant or are not serving our purposes. It also enable us to regulate emotions.” In his opinion, the medical treatment of ADHD should focus on helping the prefrontal cortex function optimally. “How much we can do – that remains to be seen – but that’s really where the action is,” he said. “From a functional standpoint, that’s what are we trying to achieve. When we have guided attention and when our responses to the world are appropriate, we can say that we’re ‘in the zone.’ That means we can listen, understand, make sense of the world, and deviate or shift direction if something gets in the way of our goals. Our responses should be flexible. We should be able to say, ‘That doesn’t work? Let me try something else.’ This indicates that the norepinephrine and dopamine circuits of the frontal cortex are optimally operating.”
On the other hand, individuals with ADHD find themselves in what Dr. Rostain described as an “unguided attention state” characterized by distraction and poor impulse control. “We also see it in people who are sleep deprived,” he said. “This could be untreated ADHD. If we treat ADHD properly, we move individuals into the optimal zone. But if we overdo it, if our medications are prescribed at doses that are higher than optimal, what you then see is excessive stimulation of the norepinephrine and dopamine systems. This leads to misguided attention, overfocusing, and mental inflexibility. People in this state report extreme amounts of stress and distress.”
Dr. Rostain recommends that medication plans be embedded in a comprehensive treatment approach that starts with psychoeducation. “When treating ADHD, we’re not going to turn a lion into a lamb, and we’re not going to make someone want to study if they don’t like school,” he said. “One of my patients, a college student, told me that, with the medication I prescribed for him, he was able to sit down and read for the first time for 3 hours straight. I said, ‘Great. Did you read your physics book? He said, No. I read Wired magazine.’ So while he was very focused, he didn’t concentrate on what he needed to focus on.”
Dr. Rostain supports the notion of a triad model of care with psychosocial interventions, medical interventions, and educational/workplace interventions “to improve the performance of demanded tasks, and to achieve a sense of being supported by that environment rather than being criticized,” he said. “If you ask most adults with ADHD what school was like, what will they tell you? They usually say it was bad or terrible, like a prison. If you ask them to describe it, they may have trouble remembering a lot of it, because it was so difficult for them.”
Dr. Rostain reported having received scientific advisory board honoraria from Shire, Ironshore, and Arbor. He also has received consultant honoraria from Major League Baseball, the National Football League, and from SUNY/Upstate.
LAS VEGAS – Despite the strides that clinicians like Anthony L. Rostain, MD, have made in better understanding and treating patients with ADHD, it remains virtually impossible to predict how a child with the disorder will fare in adulthood.
“We cannot predict the trajectory of the disorder,” Dr. Rostain said at an annual psychopharmacology update held by the Nevada Psychiatric Association. “We’re still learning about the variables that affect clinical course. There are many determinants to the trajectory.”
Dr. Rostain, professor of psychiatry and pediatrics at the University of Pennsylvania, Philadelphia, said ADHD commonly presents with numerous other neurodevelopmental disorders and with comorbid psychiatric conditions like bipolar disorder and anxiety.
“In psychiatry, we tend to see the more complicated patients, the ones with multiple comorbidities,” he said. “The most important change in the way we think about people with ADHD has to do with the growing emphasis on how it affects executive functions, in particular the cognitive, affective, and behavioral consequences of executive dysfunction. In this growingly complex world, with what some describe as ‘distracted minds’ emerging from being immersed in all our technology, it’s sometimes hard to tell: Is this person distracted because they’re always looking at their cell phone, or do they have intrinsic difficulty with managing attention?
“That’s going to become a greater challenge as children grow up in this world filled with shiny screens and devices that make [it] easier to connect with others but also harder to set a goal and follow it to its conclusion.”
ADHD changes over time, Dr. Rostain continued, but there is no single theory or biological explanation to explain its heterogeneity. “There is no cookie-cutter approach; you have to individualize when you are treating the individual in your office,” he said.
It is widely accepted that ADHD arises from biological factors, but social factors likely influence the degree of impairment, risk for comorbid disorders, and access to resources, said Dr. Rostain, who is also codirector of the developmental neuropsychiatry program at The Children’s Hospital of Philadelphia and medical director of the Adult ADHD Treatment and Research Program at Penn Medicine.
he said. “If there were one thing we could do to prevent ADHD, it might be to prevent pregnant women from drinking or to reduce poverty and violence, but that’s beyond the scope of this talk.”
He also noted that, because of epigenetics, ADHD risk factors express themselves early in some individuals and later in others. “We’re convinced that developmental disorders unfold in a nonlinear fashion,” he said. “Life [with ADHD] is curvy, not a straight line.”
Numerous studies of ADHD neurobiology have demonstrated frontal subcortical and cerebellar dysfunction – smaller striatal structures in particular. “In MRI studies, we also see difficulties with the differential maturation of important neural circuits, along with the persistence of cortical thickening where it should be thinning,” Dr. Rostain said. He went on to note that the normal brain consists of three main networks: the salience network, “which tells us whether to pay attention or to relax,” the attention and control network, and the default mode network, “which is where our mind goes when we’re daydreaming,” he said. “All of us are constantly switching between attention and daydreaming. That’s normal. In ADHD, the balance and synchrony between the default mode and the attention network is disrupted. Individuals with ADHD either remain too long in the default mode, or their attentional system isn’t powered up enough to keep them paying attention and following through during nonrewarding tasks.”
The presentation of ADHD symptoms tends to differ in children, compared with adults. For example, children with the disorder tend to be squirmy, can’t sit still, are restless, and can’t play or work quietly. On the other hand, adults tend to complain about inefficiencies at work, not being able to finish projects, not being able to sit through meetings. They tend to drive too quickly, and they often talk excessively, and make inappropriate comments. “The symptoms of ADHD emerge from disruptions or inefficiencies in basic functions, whether those are executive functions or motivational processes,” he said. “All of this is thought to be the result of genetic unfolding throughout the lifespan.”
The goal of ADHD medical therapy is to alter catecholamine tone in the prefrontal cortex, an area of the brain “designed to help us guide our thinking toward distal goals and navigate the world around us,” Dr. Rostain said. “It allows us also to inhibit actions that are task-irrelevant or are not serving our purposes. It also enable us to regulate emotions.” In his opinion, the medical treatment of ADHD should focus on helping the prefrontal cortex function optimally. “How much we can do – that remains to be seen – but that’s really where the action is,” he said. “From a functional standpoint, that’s what are we trying to achieve. When we have guided attention and when our responses to the world are appropriate, we can say that we’re ‘in the zone.’ That means we can listen, understand, make sense of the world, and deviate or shift direction if something gets in the way of our goals. Our responses should be flexible. We should be able to say, ‘That doesn’t work? Let me try something else.’ This indicates that the norepinephrine and dopamine circuits of the frontal cortex are optimally operating.”
On the other hand, individuals with ADHD find themselves in what Dr. Rostain described as an “unguided attention state” characterized by distraction and poor impulse control. “We also see it in people who are sleep deprived,” he said. “This could be untreated ADHD. If we treat ADHD properly, we move individuals into the optimal zone. But if we overdo it, if our medications are prescribed at doses that are higher than optimal, what you then see is excessive stimulation of the norepinephrine and dopamine systems. This leads to misguided attention, overfocusing, and mental inflexibility. People in this state report extreme amounts of stress and distress.”
Dr. Rostain recommends that medication plans be embedded in a comprehensive treatment approach that starts with psychoeducation. “When treating ADHD, we’re not going to turn a lion into a lamb, and we’re not going to make someone want to study if they don’t like school,” he said. “One of my patients, a college student, told me that, with the medication I prescribed for him, he was able to sit down and read for the first time for 3 hours straight. I said, ‘Great. Did you read your physics book? He said, No. I read Wired magazine.’ So while he was very focused, he didn’t concentrate on what he needed to focus on.”
Dr. Rostain supports the notion of a triad model of care with psychosocial interventions, medical interventions, and educational/workplace interventions “to improve the performance of demanded tasks, and to achieve a sense of being supported by that environment rather than being criticized,” he said. “If you ask most adults with ADHD what school was like, what will they tell you? They usually say it was bad or terrible, like a prison. If you ask them to describe it, they may have trouble remembering a lot of it, because it was so difficult for them.”
Dr. Rostain reported having received scientific advisory board honoraria from Shire, Ironshore, and Arbor. He also has received consultant honoraria from Major League Baseball, the National Football League, and from SUNY/Upstate.
LAS VEGAS – Despite the strides that clinicians like Anthony L. Rostain, MD, have made in better understanding and treating patients with ADHD, it remains virtually impossible to predict how a child with the disorder will fare in adulthood.
“We cannot predict the trajectory of the disorder,” Dr. Rostain said at an annual psychopharmacology update held by the Nevada Psychiatric Association. “We’re still learning about the variables that affect clinical course. There are many determinants to the trajectory.”
Dr. Rostain, professor of psychiatry and pediatrics at the University of Pennsylvania, Philadelphia, said ADHD commonly presents with numerous other neurodevelopmental disorders and with comorbid psychiatric conditions like bipolar disorder and anxiety.
“In psychiatry, we tend to see the more complicated patients, the ones with multiple comorbidities,” he said. “The most important change in the way we think about people with ADHD has to do with the growing emphasis on how it affects executive functions, in particular the cognitive, affective, and behavioral consequences of executive dysfunction. In this growingly complex world, with what some describe as ‘distracted minds’ emerging from being immersed in all our technology, it’s sometimes hard to tell: Is this person distracted because they’re always looking at their cell phone, or do they have intrinsic difficulty with managing attention?
“That’s going to become a greater challenge as children grow up in this world filled with shiny screens and devices that make [it] easier to connect with others but also harder to set a goal and follow it to its conclusion.”
ADHD changes over time, Dr. Rostain continued, but there is no single theory or biological explanation to explain its heterogeneity. “There is no cookie-cutter approach; you have to individualize when you are treating the individual in your office,” he said.
It is widely accepted that ADHD arises from biological factors, but social factors likely influence the degree of impairment, risk for comorbid disorders, and access to resources, said Dr. Rostain, who is also codirector of the developmental neuropsychiatry program at The Children’s Hospital of Philadelphia and medical director of the Adult ADHD Treatment and Research Program at Penn Medicine.
he said. “If there were one thing we could do to prevent ADHD, it might be to prevent pregnant women from drinking or to reduce poverty and violence, but that’s beyond the scope of this talk.”
He also noted that, because of epigenetics, ADHD risk factors express themselves early in some individuals and later in others. “We’re convinced that developmental disorders unfold in a nonlinear fashion,” he said. “Life [with ADHD] is curvy, not a straight line.”
Numerous studies of ADHD neurobiology have demonstrated frontal subcortical and cerebellar dysfunction – smaller striatal structures in particular. “In MRI studies, we also see difficulties with the differential maturation of important neural circuits, along with the persistence of cortical thickening where it should be thinning,” Dr. Rostain said. He went on to note that the normal brain consists of three main networks: the salience network, “which tells us whether to pay attention or to relax,” the attention and control network, and the default mode network, “which is where our mind goes when we’re daydreaming,” he said. “All of us are constantly switching between attention and daydreaming. That’s normal. In ADHD, the balance and synchrony between the default mode and the attention network is disrupted. Individuals with ADHD either remain too long in the default mode, or their attentional system isn’t powered up enough to keep them paying attention and following through during nonrewarding tasks.”
The presentation of ADHD symptoms tends to differ in children, compared with adults. For example, children with the disorder tend to be squirmy, can’t sit still, are restless, and can’t play or work quietly. On the other hand, adults tend to complain about inefficiencies at work, not being able to finish projects, not being able to sit through meetings. They tend to drive too quickly, and they often talk excessively, and make inappropriate comments. “The symptoms of ADHD emerge from disruptions or inefficiencies in basic functions, whether those are executive functions or motivational processes,” he said. “All of this is thought to be the result of genetic unfolding throughout the lifespan.”
The goal of ADHD medical therapy is to alter catecholamine tone in the prefrontal cortex, an area of the brain “designed to help us guide our thinking toward distal goals and navigate the world around us,” Dr. Rostain said. “It allows us also to inhibit actions that are task-irrelevant or are not serving our purposes. It also enable us to regulate emotions.” In his opinion, the medical treatment of ADHD should focus on helping the prefrontal cortex function optimally. “How much we can do – that remains to be seen – but that’s really where the action is,” he said. “From a functional standpoint, that’s what are we trying to achieve. When we have guided attention and when our responses to the world are appropriate, we can say that we’re ‘in the zone.’ That means we can listen, understand, make sense of the world, and deviate or shift direction if something gets in the way of our goals. Our responses should be flexible. We should be able to say, ‘That doesn’t work? Let me try something else.’ This indicates that the norepinephrine and dopamine circuits of the frontal cortex are optimally operating.”
On the other hand, individuals with ADHD find themselves in what Dr. Rostain described as an “unguided attention state” characterized by distraction and poor impulse control. “We also see it in people who are sleep deprived,” he said. “This could be untreated ADHD. If we treat ADHD properly, we move individuals into the optimal zone. But if we overdo it, if our medications are prescribed at doses that are higher than optimal, what you then see is excessive stimulation of the norepinephrine and dopamine systems. This leads to misguided attention, overfocusing, and mental inflexibility. People in this state report extreme amounts of stress and distress.”
Dr. Rostain recommends that medication plans be embedded in a comprehensive treatment approach that starts with psychoeducation. “When treating ADHD, we’re not going to turn a lion into a lamb, and we’re not going to make someone want to study if they don’t like school,” he said. “One of my patients, a college student, told me that, with the medication I prescribed for him, he was able to sit down and read for the first time for 3 hours straight. I said, ‘Great. Did you read your physics book? He said, No. I read Wired magazine.’ So while he was very focused, he didn’t concentrate on what he needed to focus on.”
Dr. Rostain supports the notion of a triad model of care with psychosocial interventions, medical interventions, and educational/workplace interventions “to improve the performance of demanded tasks, and to achieve a sense of being supported by that environment rather than being criticized,” he said. “If you ask most adults with ADHD what school was like, what will they tell you? They usually say it was bad or terrible, like a prison. If you ask them to describe it, they may have trouble remembering a lot of it, because it was so difficult for them.”
Dr. Rostain reported having received scientific advisory board honoraria from Shire, Ironshore, and Arbor. He also has received consultant honoraria from Major League Baseball, the National Football League, and from SUNY/Upstate.
REPORTING FROM NPA 2019
Experts Weigh in on Medication Overuse Headache
Following the American Headache Society’s Scottsdale Headache Symposium in November 2018, MedPage Today posted an article which shared differing opinions from Drs. Hans-Christoph Diener and Elizabeth Loder on medication overuse headache (MOH). While Dr. Diener noted that “we can identify people with chronic migraine who are at risk to have medication overuse,” and that following successful withdrawal treatment “the majority of patients…revert to episodic migraine,” Dr. Loder pointed out that while MOH may exist and contribute to chronic migraine, “it is over-emphasized and the evidence in support of these concepts is weak.”
For this article, I’ve asked Drs. Marcelo Bigal, Rob Cowan, Jack Schim, and Stewart J. Tepper to share their perspectives on this topic. I also asked both Dr. Diener and Dr. Loder to expand on their comments. We will see Dr. Diener’s response to the article, but we did not hear back from Dr. Loder. Lastly, I will weigh in on the MOH discussion.
Marcelo Bigal, MD, PhD
Chief Medical Officer, Purdue Pharma
The issue of medication overuse headache (MOH) needs to be disentangled into a few separate but related issues. First, do excessive medications make migraine worse? Second, should MOH be considered a distinct form of headache? And how can evidence inform clinical practice?
Robust evidence supports the fact that excessive acute medication use is associated with increased headache frequency among migraineurs. In a large epidemiological study, we demonstrated that exposure (medication) precedes outcome (increased headache frequency).1 The risk was higher for barbiturates, followed by opioids and triptans, and was not increased by nonsteroidal anti-inflammatory drugs (NSAIDs). Dose response and critical exposure levels were identified. Based on this study and several others, we argued that criteria of causality had been demonstrated beyond reasonable doubt.2
However, since the effect is specific to migraine in that the exposure only increases the risk in migraineurs, not in individuals with other types of pain, we do not consider MOH a distinct entity. Instead, we believe that excessive medication is a risk factor for chronic migraine (CM). Therefore, we should be able to subdivide CM into 2 groups, one with and one without excessive medication use.
From a clinical perspective, physicians should monitor acute medication consumption in individuals with migraine and should be liberal in starting preventive therapy. In those with CM and excessive acute medication use we don’t advocate abrupt discontinuation of acute medications, since some preventive medications, especially the newer anti-calcitonin gene-related peptide (CGRP) antibodies, seem to work equally well in individuals with and without excessive use of medication,3 allowing more natural and gradual control of acute medication consumption without the need for detoxification.
Rob Cowan, MD, FAAN, FAHS
Higgins Professor of Neurology and Neurosciences
Chief, Division of Headache Medicine, Dept. of Neurology and Neurosciences
Director, Stanford University School of Medicine
As is often the case when 2 smart people take artificially imposed opposite positions, the truth will lie somewhere in the middle. I doubt either of the debaters would argue either extreme position: MOH does not exist, or MOH when present is solely responsible for chronic daily headache (CDH). The argument that the absence of controlled studies negates the proposition fails the common-sense test: Without a controlled study, we can’t be sure that wearing a helmet when bicycling is better than not. In such a case, observational data is sufficient. Could there be confounders (eg, helmet wearers are more inclined to ride safely)? Of course, but is that important? Similarly, does the fact that some MOH patients continue with CDH after cessation of medication overuse warrant a general de-emphasis? Certainly not for the third-to-half of patients who benefit from limiting medication use.
I suspect both Drs. Diener and Loder would agree that we would benefit from better markers of chronification and that earlier intervention with at-risk patients (eg, patients with increasing headache frequency, severity or duration but still in the episodic phase).
Jack Schim, MD
Co-Director, The Headache Center of Southern California
There has long been recognition that overuse of analgesic medications can be linked to progression of headache disorders. MOH was initially described by Dr. Lee Kudrow in 1982, in a chapter entitled, “Paradoxical effects of frequent analgesic use.”4 The most recent edition of the International Classification of Headache Disorders (ICHD-3) description does not entail features that imply causality. While there is epidemiologic observation of correlation between frequent analgesic use and progression of primary headache disorders, the causal relationship is often obscured by the facts. Overuse of acute medications is quite common in individuals with CM, but not all with CM overuse medications.
In the article being discussed, Drs. Diener and Loder reviewed facts and opinions. They helped clarify that while MOH is widely recognized, much of what is known is descriptive, and not based on solid science. From their presentations, we can conclude that we can recognize MOH based on ICHD-3 criteria, but we cannot tell an individual with chronic headache whether we can best help them by educating them, or by adjusting preventives, or both. The call to action is clear; we need to evaluate best therapeutic approaches in an empiric fashion. Our best new therapies for migraine prevention, CGRP mAbs, work for the majority of patients, with minimal side effects, even in the face of what has been considered MOH. Now, we need to strategize how best to approach these clinically challenged individuals. We need to avoid further stigmatizing our patients. Let’s recognize that our patients do not fail preventives, the prior preventives have failed our patients. Can the introduction of highly effective, well tolerated preventives at an earlier stage help avoid chronification that may drive medication overuse?
Stewart J. Tepper, MD, FAHS
Professor of Neurology, Geisel School of Medicine at Dartmouth
It is clear that overuse of some acute medication is detrimental to patient health. Examples of this include analgesic nephropathy or peptic ulcer disease, and exacerbation of depression with overuse of barbiturate compounds or benzodiazepines. Few doubt the health merits of reduction of acute medication overuse, regardless of whether the acute medications can be proven to transform episodic migraine (EM) to CM.
The good news is that the issues of the existence of true MOH and its proper management are rapidly becoming less important. OnabotulinumtoxinA use decreases triptan use in multiple randomized controlled trials for CM prevention.
Each of the anti-CGRP and anti-CGRP receptor monoclonal antibodies (mAbs) have been effective in preventing CM with medication overuse. All have lowered acute medication use, both triptans and analgesics. It is worth noting, however, that in both the OnabotulinumtoxinA and mAb trials, over-users of opioids and barbiturates were excluded. The mAbs converted patients from acute medication overuse to non-overuse, and from CM with medication overuse to EM without medication. These changes occurred without specific plans for weaning acute medication in place.
Accordingly, patients with CM with acute medication overuse should be treated with optimal prevention, and the evidence is strongest for use of the mAbs to both reduce mean monthly migraine days and all acute medication use, both triptans and analgesics. The new monoclonal antibody effectiveness may make the old arguments moot.
Hans-Christoph Diener, MD, PhD
University of Essen, Germany
I think no one doubts that MOH exists. The worldwide prevalence is between 1% and 2% (Table). The dilemma is that the diagnosis can only be made after the intake of acute medication has been reduced. There are confounders: migraine can improve irrespective of the reduction of acute medication and many physicians will implement migraine prevention at the time of withdrawal. No randomized trial compared the continuation of unchanged intake of medication to treat migraine attacks with reduction or withdrawal.
| Author (year) (reference) | Country | Age Group | Prevalence of MOH |
Castillo et al. (1999)7 | Spain | ≥ 14 | 1,2% |
Wang et al. (2000)8 | Taiwan | ≥ 65 | 1,0% |
Lu et al. (2001)9 | Taiwan | ≥ 15 | 1,1% |
Pascual et al. (2001)10 | Review |
| 1,0-1,9% |
Prencipe et al. (2001)11 | France | ≥ 65 | 1,7% |
Colas et al. (2004)12 | Spain | ≥ 14 | 1,5% |
Zwart et al. (2004)13 | Norway | ≥ 20 | 0,9-1,0% |
Dyb et al. (2006)14 | Norway | 13-18 | 0,2% |
Wang et al. (2006)15 | Taiwan | 12-14 | 0,3% |
Wiendels (2006)16 | Netherlands | 25-55 | 2,6% |
Stovner et al.(2007)17 | Review |
| 0,5-1,0% |
Aaseth et al. (2008, 2009)18,19 | Norway | 30-44 | 1,7% |
Rueda-Sanchez & Diaz-Martinez (2008)20 | Columbia | 18-65 | 4,5% |
Katsarava et al. (2009)21 | Georgia | ≥ 16 | 0,9% |
Da Silva et al. (2009)22 | Brazil | 10-93 | 1,6% |
Straube et al. (2010)23 | Germany | 18-88 | 1,0% |
Jonsson et al. (2011, 2012)24,25 | Sweden | ≥ 15 | 1,8% |
Linde et al. (2011)26 | Norway | ≥ 20 | 1,0% |
Lipton et al. (2011)27 | USA | 12-17 | 1,0% |
Ayzenberg et al. (2012)28 | Russia | 18-65 | 7,2% |
Ertas et al. (2012)29 | Turkey | 18-65 | 2,1% |
Hagen et al. (2012)30 | Norway | ≥ 20 | 0,8% |
Yu et al. (2012)31 | China | 18-65 | 0,9% |
Shahbeigi et al. (2013)32 | Iran | ≥ 10 | 4,9% |
Schramm et al. (2013)33 | Germany | 18-65 | 0,7% |
Park et al. (2014)34 | South Korea | 19-69 | 0,5% |
Kristoffersen & Lundqvist (2014)35 | Multinational summary |
| 1,0-2,0% |
Steiner (2014)36 | Multinational summary |
| 1,0-2,0% |
Westergaard et al. (2015)37 | Denmark |
| 0,5-7,2% |
Bravo (2015)38 | Multinational | Older | 1,0-7,1% |
Mbewe et al. (2015)39 | Zambia | 18-65 | 12,7% (adj. 7,1%) |
Kulkarni et al. (2015)40 | India | 18-65 | 1,2% |
Westergaard et al. (2016)41 | Denmark | ≥ 16 | 1,6% (adj. 1,8%) |
Manandhar et al. (2016)42 | Nepal | 18-65 | 2,2% |
Zebenigus et al. (2016)43 | Ethiopia | 18-65 | 0,8% (adj. 0,7%) |
Al-Hashel et al. (2017)44 | Kuwait | 18-65 | 2,4% |
Rastenyte et al. (2017)45 | Lithuania | 18-65 | 3,5% (adj. 3,2%) |
Henning et al. (2018)46 | Germany | 18-65 | 0,7% |
Global Burden of Disease 201747 | Global |
| 0,8% |
+++
Commentary by Alan M. Rapoport, MD
The above comments by my associates are very informative and help the reader to better understand the arguments about MOH. When Dr. Lee Kudrow taught me and my partner Dr. Fred Sheftell about the entity of analgesic and ergotamine overuse headaches in 1979, we set out to find those patients, observe and treat them. We did not have to wait long as so many patients with frequent and severe headaches came to see us with what we now term “medication overuse headache.” They told us that they had fewer headaches several years before and increased the use of acute care medications as their headaches increased in frequency. They were unaware of the probability that their headaches increased in frequency because their medication did. Some would argue that they increased their intake to feel better as the headache increased on their own.
Of course, we were not sure of the cause and effect, but we saw the result of tapering the acute care medications, whether or not we used preventives, hospitalized those patients or treated them with behavioral medicine approaches, etc. We observed that the combination of these treatments seemed to work better than just detox, but we did not do the proper studies to prove it. We also noticed that about 30% to 40% of patients did not improve as well as others, and daily or near-daily headaches continued, often of a lesser intensity. Almost all felt better in general and had fewer adverse events from the medication. The decrease in those medications was undoubtedly better for their brain function, livers and kidneys.
I do believe that medication overuse makes most patients with frequent EM or CM worse and we should educate patients to avoid it. I agree with Dr. Bigal that preventive medications may help some patients to improve despite the excessive use of acute care medication, but I am not sure that the older preventives work as well and certainly not as quickly as the newer ones. Recently I have seen the anti-CGRP mAbs work wonders with some of my patients who could not decrease their triptan intake. They just stop using the triptans as their headaches decrease on these therapies.
There is another interesting phenomenon that I have seen in practice—mostly with butalbital products, which I no longer prescribe. Forty years ago, patients would say that they only had 4 headaches per month lasting 1 to 2 days and I would prescribe 10 pills for them. They would call in 2 weeks and say they needed more. When queried they would invariably say it worked so well on the bad headaches and made them feel so much better, that they took 1 or 2 on days they thought they were going to get a headache and it prevented them from forming. They were soon taking it frequently and over time they were dependent on the medication, and then it stopped working and was difficult to withdraw.
Dr. Loder’s point that the studies on MOH have not proven that medication overuse causes it may be technically true; but it would be unethical to start patients on too much medication and randomize some to stay on and some to taper off. Dr. Kudrow came the closest by taking existing MOH patients and treating half with withdrawal and half of each with preventives. His breakthrough study in 1982 “proved” the existence of analgesic rebound and directed us to the best treatment at that time.4 This was the first study to examine the effect of stopping the overuse of medication to see the results.
Finally, I am unhappy that ICHD-3 has defined MOH only by number of days of medication use, not at all considering whether or not the patient develops a new type of headache, a worse type or more frequent headache (the way it was in previous versions). We have all seen patients taking 3 triptans per day on their own or with our suggestion, and many actually do better with no headache, for a period of time. This is medication overuse by definition, but not MOH, as they have little headache. But we do not recognize this entity.
The good news is, with education and anti-CGRP therapies, we will probably see less MOH in the future, or at least know better how to treat it.
+++
References
1. Bigal ME, Serrano D, Buse D, et al. Acute migraine medications and evolution from episodic to chronic migraine: a longitudinal population-based study. Headache. 2008;48(8):1157-68. doi: 10.1111/j.1526-4610.2008.01217.x. PubMed PMID: 18808500.
2. Bigal ME, Lipton RB. Overuse of acute migraine medications and migraine chronification. Curr Pain Headache Rep. 2009;13(4):301-7. PubMed PMID: 19586594.
3. Bigal ME, Edvinsson L, Rapoport AM, et al. Safety, tolerability, and efficacy of TEV-48125 for preventive treatment of chronic migraine: a multicentre, randomised, double-blind, placebo-controlled, phase 2b study. Lancet Neurol. 2015;14(11):1091-100. doi: 10.1016/S1474-4422(15)00245-8. PubMed PMID: 26432181.
4. Kudrow L. Paradoxical Effects of Frequent Analgesic Use. Advances in Neurology. 1982;33:335-341.
5. Diener HC, Holle D, Dresler T, Gaul C. Chronic Headache Due to Overuse of Analgesics and Anti-Migraine Agents. Dtsch Arztebl Int. 2018;115(22):365-370.
6. Westergaard ML, Glumer C, Hansen EH, Jensen RH. Prevalence of chronic headache with and without medication overuse: associations with socioeconomic position and physical and mental health status. Pain. 2014;155(10):2005-2013.
7. Castillo J, Munoz P, Guitera V, Pascual J. Epidemiology of chronic daily headache in the general population. Headache. 1999;39:190-196.
8. Wang SJ, Fuh JL, Lu SR, et al. Chronic daily headache in chinese elderly - prevalence, risk factors, and biannual follow-up. Neurology. 2000;54:314-319.
9. Lu SR, Fuh JL, Chen WT, Juang KD, Wang SJ. Chronic daily headache in Taipei, Taiwan: prevalence, follow-up and outcome predictors. Cephalalgia. 2001;21:980-986.
10. Pascual J, Colas R, Castillo J. Epidemiology of chronic daily headache. Curr Pain Headache Rep. 2001;5(6):529-536.
11. Prencipe M, Casini AR, Ferretti C, et al. Prevalence of headache in an elderly population: attack frequency, disability, and use of medication. J Neurol Neurosurg Psychiatry. 2001;70(3):377-381.
12. Colas R, Munoz P, Temprano R, Gomez C, Pascual J. Chronic daily headache with analgesic overuse: epidemiology and impact on quality of life. Neurology. 2004;62:1338-1342.
13. Zwart J, Dyb G, Hagen K, Svebak S, Stovner L, Holmen J. Analgesic overuse among subjects with headache, neck, and low back pain. Neurology. 2004;62:1540-1544.
14. Dyb G, Holmen TL, Zwart JA. Analgesic overuse among adolescents with headache: the Head-HUNT-Youth Study. Neurology. 2006;66(2):198-201.
15. Wang SJ, Fuh JL, Lu SR, Juang KD. Chronic daily headache in adolescents: prevalence, impact, and medication overuse. Neurology. 2006;66(2):193-197.
16. Wiendels NJ, Knuistingh NA, Rosendaal FR, et al. Chronic frequent headache in the general population: prevalence and associated factors. Cephalalgia. 2006;26(12):1434-1442.
17. Stovner L, Hagen K, Jensen R, et al. The global burden of headache: a documentation of headache prevalence and disability worldwide. Cephalalgia. 2007;27(3):193-210.
18. Aaseth K, Grande RB, Kvaerner KJ, Gulbrandsen P, Lundqvist C, Russell MB. Prevalence of secondary chronic headaches in a population-based sample of 30-44-year-old persons. The Akershus study of chronic headache. Cephalalgia. 2008;28(7):705-713.
19. Aaseth K, Grande RB, Lundqvist C, Russell MB. What is chronic headache in the general population? The Akershus study of chronic headache. Acta Neurol Scand Suppl. 2009;(189):30-32.
20. Rueda-Sanchez M, Diaz-Martinez LA. Prevalence and associated factors for episodic and chronic daily headache in the Colombian population. Cephalalgia. 2008;28(3):216-225.
21. Katsarava Z, Dzagnidze A, Kukava M, et al. Primary headache disorders in the Republic of Georgia: prevalence and risk factors. Neurology. 2009;73(21):1796-1803.
22. da Silva A, Jr., Costa EC, Gomes JB, et al. Chronic headache and comorbidities: a two-phase, population-based, cross-sectional study. Headache. 2010;50(8):1306-1312.
23. Straube A, Pfaffenrath V, Ladwig KH, et al. Prevalence of chronic migraine and medication overuse headache in Germany--the German DMKG headache study. Cephalalgia. 2010;30(2):207-213.
24. Jonsson P, Hedenrud T, Linde M. Epidemiology of medication overuse headache in the general Swedish population. Cephalalgia. 2011;31(9):1015-1022.
25. Jonsson P, Linde M, Hensing G, Hedenrud T. Sociodemographic differences in medication use, health-care contacts and sickness absence among individuals with medication-overuse headache. J Headache Pain. 2012;13(4):281-290.
26. Linde M, Stovner LJ, Zwart JA, Hagen K. Time trends in the prevalence of headache disorders. The Nord-Trondelag Health Studies (HUNT 2 and HUNT 3). Cephalalgia. 2011;31(5):585-596.
27. Lipton RB, Manack A, Ricci JA, Chee E, Turkel CC, Winner P. Prevalence and burden of chronic migraine in adolescents: results of the chronic daily headache in adolescents study (C-dAS). Headache. 2011;51(5):693-706.
28. Ayzenberg I, Katsarava Z, Sborowski A, et al. The prevalence of primary headache disorders in Russia: a countrywide survey. Cephalalgia. 2012;32(5):373-381.
29. Ertas M, Baykan B, Orhan EK, et al. One-year prevalence and the impact of migraine and tension-type headache in Turkey: a nationwide home-based study in adults. J Headache Pain. 2012;13(2):147-157.
30. Hagen K, Linde M, Steiner TJ, Stovner LJ, Zwart JA. Risk factors for medication-overuse headache: an 11-year follow-up study. The Nord-Trondelag Health Studies. Pain. 2012;153(1):56-61.
31. Yu S, Liu R, Zhao G, et al. The prevalence and burden of primary headaches in China: a population-based door-to-door survey. Headache. 2012;52(4):582-591.
32. Shahbeigi S, Fereshtehnejad SM, Mohammadi N, et al. Epidemiology of headaches in Tehran urban area: a population-based cross-sectional study in district 8, year 2010. Neurol Sci. 2013;34(7):1157-66.
33. Schramm SH, Obermann M, Katsarava Z, Diener HC, Moebus S, Yoon MS. Epidemiological profiles of patients with chronic migraine and chronic tension-type headache. J Headache Pain. 2013;14:40.
34. Park JW, Moon HS, Kim JM, Lee KS, Chu MK. Chronic daily headache in Korea: prevalence, clinical characteristics, medical consultation and management. J Clin Neurol. 2014;10(3):236-243.
35. Kristoffersen ES, Lundqvist C. Medication-overuse headache: epidemiology, diagnosis and treatment. Ther Adv Drug Saf. 2014;5(2):87-99.
36. Steiner TJ, Stovner LJ, Katsarava Z, et al. The impact of headache in Europe: principal results of the Eurolight project. J Headache Pain. 2014;15:31.
37. Westergaard ML, Hansen EH, Glumer C, Jensen RH. Prescription pain medications and chronic headache in Denmark: implications for preventing medication overuse. Eur J Clin Pharmacol. 2015;71(7):851-860.
38. Bravo TP. Headaches of the elderly. Curr Neurol Neurosci Rep. 2015;15(6):30.
39. Mbewe E, Zairemthiama P, Yeh HH, Paul R, Birbeck GL, Steiner TJ. The epidemiology of primary headache disorders in Zambia: a population-based door-to-door survey. J Headache Pain. 2015;16:515.
40. Kulkarni GB, Rao GN, Gururaj G, Stovner LJ, Steiner TJ. Headache disorders and public ill-health in India: prevalence estimates in Karnataka State. J Headache Pain. 2015;16:67.
41. Westergaard ML, Glumer C, Hansen EH, Jensen RH. Medication overuse, healthy lifestyle behaviour and stress in chronic headache: Results from a population-based representative survey. Cephalalgia. 2016;36(1):15-28.
42. Manandhar K, Risal A, Linde M, Steiner TJ. The burden of headache disorders in Nepal: estimates from a population-based survey. J Headache Pain. 2015;17:3.
43. Zebenigus M, Tekle-Haimanot R, Worku DK, Thomas H, Steiner TJ. The prevalence of primary headache disorders in Ethiopia. J Headache Pain. 2016;17(1):110.
44. Al-Hashel JY, Ahmed SF, Alroughani R. Prevalence of Primary Headache Disorders in Kuwait. Neuroepidemiology. 2017;48(3-4):138-146.
45. Rastenyte D, Mickeviciene D, Stovner LJ, Thomas H, Andree C, Steiner TJ. Prevalence and burden of headache disorders in Lithuania and their public-health and policy implications: a population-based study within the Eurolight Project. J Headache Pain. 2017;18(1):53.
46. Henning V, Katsarava Z, Obermann M, Moebus S, Schramm S. Remission of chronic headache: Rates, potential predictors and the role of medication, follow-up results of the German Headache Consortium (GHC) Study. Cephalalgia. 2018;38(3):551-560.
47. Global Burden of Disease Neurological Disorders Collaborator Group. Global, regional, and national burden of neurological disorders during 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet Neurol. 2017;16(11):877-897.
Following the American Headache Society’s Scottsdale Headache Symposium in November 2018, MedPage Today posted an article which shared differing opinions from Drs. Hans-Christoph Diener and Elizabeth Loder on medication overuse headache (MOH). While Dr. Diener noted that “we can identify people with chronic migraine who are at risk to have medication overuse,” and that following successful withdrawal treatment “the majority of patients…revert to episodic migraine,” Dr. Loder pointed out that while MOH may exist and contribute to chronic migraine, “it is over-emphasized and the evidence in support of these concepts is weak.”
For this article, I’ve asked Drs. Marcelo Bigal, Rob Cowan, Jack Schim, and Stewart J. Tepper to share their perspectives on this topic. I also asked both Dr. Diener and Dr. Loder to expand on their comments. We will see Dr. Diener’s response to the article, but we did not hear back from Dr. Loder. Lastly, I will weigh in on the MOH discussion.
Marcelo Bigal, MD, PhD
Chief Medical Officer, Purdue Pharma
The issue of medication overuse headache (MOH) needs to be disentangled into a few separate but related issues. First, do excessive medications make migraine worse? Second, should MOH be considered a distinct form of headache? And how can evidence inform clinical practice?
Robust evidence supports the fact that excessive acute medication use is associated with increased headache frequency among migraineurs. In a large epidemiological study, we demonstrated that exposure (medication) precedes outcome (increased headache frequency).1 The risk was higher for barbiturates, followed by opioids and triptans, and was not increased by nonsteroidal anti-inflammatory drugs (NSAIDs). Dose response and critical exposure levels were identified. Based on this study and several others, we argued that criteria of causality had been demonstrated beyond reasonable doubt.2
However, since the effect is specific to migraine in that the exposure only increases the risk in migraineurs, not in individuals with other types of pain, we do not consider MOH a distinct entity. Instead, we believe that excessive medication is a risk factor for chronic migraine (CM). Therefore, we should be able to subdivide CM into 2 groups, one with and one without excessive medication use.
From a clinical perspective, physicians should monitor acute medication consumption in individuals with migraine and should be liberal in starting preventive therapy. In those with CM and excessive acute medication use we don’t advocate abrupt discontinuation of acute medications, since some preventive medications, especially the newer anti-calcitonin gene-related peptide (CGRP) antibodies, seem to work equally well in individuals with and without excessive use of medication,3 allowing more natural and gradual control of acute medication consumption without the need for detoxification.
Rob Cowan, MD, FAAN, FAHS
Higgins Professor of Neurology and Neurosciences
Chief, Division of Headache Medicine, Dept. of Neurology and Neurosciences
Director, Stanford University School of Medicine
As is often the case when 2 smart people take artificially imposed opposite positions, the truth will lie somewhere in the middle. I doubt either of the debaters would argue either extreme position: MOH does not exist, or MOH when present is solely responsible for chronic daily headache (CDH). The argument that the absence of controlled studies negates the proposition fails the common-sense test: Without a controlled study, we can’t be sure that wearing a helmet when bicycling is better than not. In such a case, observational data is sufficient. Could there be confounders (eg, helmet wearers are more inclined to ride safely)? Of course, but is that important? Similarly, does the fact that some MOH patients continue with CDH after cessation of medication overuse warrant a general de-emphasis? Certainly not for the third-to-half of patients who benefit from limiting medication use.
I suspect both Drs. Diener and Loder would agree that we would benefit from better markers of chronification and that earlier intervention with at-risk patients (eg, patients with increasing headache frequency, severity or duration but still in the episodic phase).
Jack Schim, MD
Co-Director, The Headache Center of Southern California
There has long been recognition that overuse of analgesic medications can be linked to progression of headache disorders. MOH was initially described by Dr. Lee Kudrow in 1982, in a chapter entitled, “Paradoxical effects of frequent analgesic use.”4 The most recent edition of the International Classification of Headache Disorders (ICHD-3) description does not entail features that imply causality. While there is epidemiologic observation of correlation between frequent analgesic use and progression of primary headache disorders, the causal relationship is often obscured by the facts. Overuse of acute medications is quite common in individuals with CM, but not all with CM overuse medications.
In the article being discussed, Drs. Diener and Loder reviewed facts and opinions. They helped clarify that while MOH is widely recognized, much of what is known is descriptive, and not based on solid science. From their presentations, we can conclude that we can recognize MOH based on ICHD-3 criteria, but we cannot tell an individual with chronic headache whether we can best help them by educating them, or by adjusting preventives, or both. The call to action is clear; we need to evaluate best therapeutic approaches in an empiric fashion. Our best new therapies for migraine prevention, CGRP mAbs, work for the majority of patients, with minimal side effects, even in the face of what has been considered MOH. Now, we need to strategize how best to approach these clinically challenged individuals. We need to avoid further stigmatizing our patients. Let’s recognize that our patients do not fail preventives, the prior preventives have failed our patients. Can the introduction of highly effective, well tolerated preventives at an earlier stage help avoid chronification that may drive medication overuse?
Stewart J. Tepper, MD, FAHS
Professor of Neurology, Geisel School of Medicine at Dartmouth
It is clear that overuse of some acute medication is detrimental to patient health. Examples of this include analgesic nephropathy or peptic ulcer disease, and exacerbation of depression with overuse of barbiturate compounds or benzodiazepines. Few doubt the health merits of reduction of acute medication overuse, regardless of whether the acute medications can be proven to transform episodic migraine (EM) to CM.
The good news is that the issues of the existence of true MOH and its proper management are rapidly becoming less important. OnabotulinumtoxinA use decreases triptan use in multiple randomized controlled trials for CM prevention.
Each of the anti-CGRP and anti-CGRP receptor monoclonal antibodies (mAbs) have been effective in preventing CM with medication overuse. All have lowered acute medication use, both triptans and analgesics. It is worth noting, however, that in both the OnabotulinumtoxinA and mAb trials, over-users of opioids and barbiturates were excluded. The mAbs converted patients from acute medication overuse to non-overuse, and from CM with medication overuse to EM without medication. These changes occurred without specific plans for weaning acute medication in place.
Accordingly, patients with CM with acute medication overuse should be treated with optimal prevention, and the evidence is strongest for use of the mAbs to both reduce mean monthly migraine days and all acute medication use, both triptans and analgesics. The new monoclonal antibody effectiveness may make the old arguments moot.
Hans-Christoph Diener, MD, PhD
University of Essen, Germany
I think no one doubts that MOH exists. The worldwide prevalence is between 1% and 2% (Table). The dilemma is that the diagnosis can only be made after the intake of acute medication has been reduced. There are confounders: migraine can improve irrespective of the reduction of acute medication and many physicians will implement migraine prevention at the time of withdrawal. No randomized trial compared the continuation of unchanged intake of medication to treat migraine attacks with reduction or withdrawal.
| Author (year) (reference) | Country | Age Group | Prevalence of MOH |
Castillo et al. (1999)7 | Spain | ≥ 14 | 1,2% |
Wang et al. (2000)8 | Taiwan | ≥ 65 | 1,0% |
Lu et al. (2001)9 | Taiwan | ≥ 15 | 1,1% |
Pascual et al. (2001)10 | Review |
| 1,0-1,9% |
Prencipe et al. (2001)11 | France | ≥ 65 | 1,7% |
Colas et al. (2004)12 | Spain | ≥ 14 | 1,5% |
Zwart et al. (2004)13 | Norway | ≥ 20 | 0,9-1,0% |
Dyb et al. (2006)14 | Norway | 13-18 | 0,2% |
Wang et al. (2006)15 | Taiwan | 12-14 | 0,3% |
Wiendels (2006)16 | Netherlands | 25-55 | 2,6% |
Stovner et al.(2007)17 | Review |
| 0,5-1,0% |
Aaseth et al. (2008, 2009)18,19 | Norway | 30-44 | 1,7% |
Rueda-Sanchez & Diaz-Martinez (2008)20 | Columbia | 18-65 | 4,5% |
Katsarava et al. (2009)21 | Georgia | ≥ 16 | 0,9% |
Da Silva et al. (2009)22 | Brazil | 10-93 | 1,6% |
Straube et al. (2010)23 | Germany | 18-88 | 1,0% |
Jonsson et al. (2011, 2012)24,25 | Sweden | ≥ 15 | 1,8% |
Linde et al. (2011)26 | Norway | ≥ 20 | 1,0% |
Lipton et al. (2011)27 | USA | 12-17 | 1,0% |
Ayzenberg et al. (2012)28 | Russia | 18-65 | 7,2% |
Ertas et al. (2012)29 | Turkey | 18-65 | 2,1% |
Hagen et al. (2012)30 | Norway | ≥ 20 | 0,8% |
Yu et al. (2012)31 | China | 18-65 | 0,9% |
Shahbeigi et al. (2013)32 | Iran | ≥ 10 | 4,9% |
Schramm et al. (2013)33 | Germany | 18-65 | 0,7% |
Park et al. (2014)34 | South Korea | 19-69 | 0,5% |
Kristoffersen & Lundqvist (2014)35 | Multinational summary |
| 1,0-2,0% |
Steiner (2014)36 | Multinational summary |
| 1,0-2,0% |
Westergaard et al. (2015)37 | Denmark |
| 0,5-7,2% |
Bravo (2015)38 | Multinational | Older | 1,0-7,1% |
Mbewe et al. (2015)39 | Zambia | 18-65 | 12,7% (adj. 7,1%) |
Kulkarni et al. (2015)40 | India | 18-65 | 1,2% |
Westergaard et al. (2016)41 | Denmark | ≥ 16 | 1,6% (adj. 1,8%) |
Manandhar et al. (2016)42 | Nepal | 18-65 | 2,2% |
Zebenigus et al. (2016)43 | Ethiopia | 18-65 | 0,8% (adj. 0,7%) |
Al-Hashel et al. (2017)44 | Kuwait | 18-65 | 2,4% |
Rastenyte et al. (2017)45 | Lithuania | 18-65 | 3,5% (adj. 3,2%) |
Henning et al. (2018)46 | Germany | 18-65 | 0,7% |
Global Burden of Disease 201747 | Global |
| 0,8% |
+++
Commentary by Alan M. Rapoport, MD
The above comments by my associates are very informative and help the reader to better understand the arguments about MOH. When Dr. Lee Kudrow taught me and my partner Dr. Fred Sheftell about the entity of analgesic and ergotamine overuse headaches in 1979, we set out to find those patients, observe and treat them. We did not have to wait long as so many patients with frequent and severe headaches came to see us with what we now term “medication overuse headache.” They told us that they had fewer headaches several years before and increased the use of acute care medications as their headaches increased in frequency. They were unaware of the probability that their headaches increased in frequency because their medication did. Some would argue that they increased their intake to feel better as the headache increased on their own.
Of course, we were not sure of the cause and effect, but we saw the result of tapering the acute care medications, whether or not we used preventives, hospitalized those patients or treated them with behavioral medicine approaches, etc. We observed that the combination of these treatments seemed to work better than just detox, but we did not do the proper studies to prove it. We also noticed that about 30% to 40% of patients did not improve as well as others, and daily or near-daily headaches continued, often of a lesser intensity. Almost all felt better in general and had fewer adverse events from the medication. The decrease in those medications was undoubtedly better for their brain function, livers and kidneys.
I do believe that medication overuse makes most patients with frequent EM or CM worse and we should educate patients to avoid it. I agree with Dr. Bigal that preventive medications may help some patients to improve despite the excessive use of acute care medication, but I am not sure that the older preventives work as well and certainly not as quickly as the newer ones. Recently I have seen the anti-CGRP mAbs work wonders with some of my patients who could not decrease their triptan intake. They just stop using the triptans as their headaches decrease on these therapies.
There is another interesting phenomenon that I have seen in practice—mostly with butalbital products, which I no longer prescribe. Forty years ago, patients would say that they only had 4 headaches per month lasting 1 to 2 days and I would prescribe 10 pills for them. They would call in 2 weeks and say they needed more. When queried they would invariably say it worked so well on the bad headaches and made them feel so much better, that they took 1 or 2 on days they thought they were going to get a headache and it prevented them from forming. They were soon taking it frequently and over time they were dependent on the medication, and then it stopped working and was difficult to withdraw.
Dr. Loder’s point that the studies on MOH have not proven that medication overuse causes it may be technically true; but it would be unethical to start patients on too much medication and randomize some to stay on and some to taper off. Dr. Kudrow came the closest by taking existing MOH patients and treating half with withdrawal and half of each with preventives. His breakthrough study in 1982 “proved” the existence of analgesic rebound and directed us to the best treatment at that time.4 This was the first study to examine the effect of stopping the overuse of medication to see the results.
Finally, I am unhappy that ICHD-3 has defined MOH only by number of days of medication use, not at all considering whether or not the patient develops a new type of headache, a worse type or more frequent headache (the way it was in previous versions). We have all seen patients taking 3 triptans per day on their own or with our suggestion, and many actually do better with no headache, for a period of time. This is medication overuse by definition, but not MOH, as they have little headache. But we do not recognize this entity.
The good news is, with education and anti-CGRP therapies, we will probably see less MOH in the future, or at least know better how to treat it.
+++
References
1. Bigal ME, Serrano D, Buse D, et al. Acute migraine medications and evolution from episodic to chronic migraine: a longitudinal population-based study. Headache. 2008;48(8):1157-68. doi: 10.1111/j.1526-4610.2008.01217.x. PubMed PMID: 18808500.
2. Bigal ME, Lipton RB. Overuse of acute migraine medications and migraine chronification. Curr Pain Headache Rep. 2009;13(4):301-7. PubMed PMID: 19586594.
3. Bigal ME, Edvinsson L, Rapoport AM, et al. Safety, tolerability, and efficacy of TEV-48125 for preventive treatment of chronic migraine: a multicentre, randomised, double-blind, placebo-controlled, phase 2b study. Lancet Neurol. 2015;14(11):1091-100. doi: 10.1016/S1474-4422(15)00245-8. PubMed PMID: 26432181.
4. Kudrow L. Paradoxical Effects of Frequent Analgesic Use. Advances in Neurology. 1982;33:335-341.
5. Diener HC, Holle D, Dresler T, Gaul C. Chronic Headache Due to Overuse of Analgesics and Anti-Migraine Agents. Dtsch Arztebl Int. 2018;115(22):365-370.
6. Westergaard ML, Glumer C, Hansen EH, Jensen RH. Prevalence of chronic headache with and without medication overuse: associations with socioeconomic position and physical and mental health status. Pain. 2014;155(10):2005-2013.
7. Castillo J, Munoz P, Guitera V, Pascual J. Epidemiology of chronic daily headache in the general population. Headache. 1999;39:190-196.
8. Wang SJ, Fuh JL, Lu SR, et al. Chronic daily headache in chinese elderly - prevalence, risk factors, and biannual follow-up. Neurology. 2000;54:314-319.
9. Lu SR, Fuh JL, Chen WT, Juang KD, Wang SJ. Chronic daily headache in Taipei, Taiwan: prevalence, follow-up and outcome predictors. Cephalalgia. 2001;21:980-986.
10. Pascual J, Colas R, Castillo J. Epidemiology of chronic daily headache. Curr Pain Headache Rep. 2001;5(6):529-536.
11. Prencipe M, Casini AR, Ferretti C, et al. Prevalence of headache in an elderly population: attack frequency, disability, and use of medication. J Neurol Neurosurg Psychiatry. 2001;70(3):377-381.
12. Colas R, Munoz P, Temprano R, Gomez C, Pascual J. Chronic daily headache with analgesic overuse: epidemiology and impact on quality of life. Neurology. 2004;62:1338-1342.
13. Zwart J, Dyb G, Hagen K, Svebak S, Stovner L, Holmen J. Analgesic overuse among subjects with headache, neck, and low back pain. Neurology. 2004;62:1540-1544.
14. Dyb G, Holmen TL, Zwart JA. Analgesic overuse among adolescents with headache: the Head-HUNT-Youth Study. Neurology. 2006;66(2):198-201.
15. Wang SJ, Fuh JL, Lu SR, Juang KD. Chronic daily headache in adolescents: prevalence, impact, and medication overuse. Neurology. 2006;66(2):193-197.
16. Wiendels NJ, Knuistingh NA, Rosendaal FR, et al. Chronic frequent headache in the general population: prevalence and associated factors. Cephalalgia. 2006;26(12):1434-1442.
17. Stovner L, Hagen K, Jensen R, et al. The global burden of headache: a documentation of headache prevalence and disability worldwide. Cephalalgia. 2007;27(3):193-210.
18. Aaseth K, Grande RB, Kvaerner KJ, Gulbrandsen P, Lundqvist C, Russell MB. Prevalence of secondary chronic headaches in a population-based sample of 30-44-year-old persons. The Akershus study of chronic headache. Cephalalgia. 2008;28(7):705-713.
19. Aaseth K, Grande RB, Lundqvist C, Russell MB. What is chronic headache in the general population? The Akershus study of chronic headache. Acta Neurol Scand Suppl. 2009;(189):30-32.
20. Rueda-Sanchez M, Diaz-Martinez LA. Prevalence and associated factors for episodic and chronic daily headache in the Colombian population. Cephalalgia. 2008;28(3):216-225.
21. Katsarava Z, Dzagnidze A, Kukava M, et al. Primary headache disorders in the Republic of Georgia: prevalence and risk factors. Neurology. 2009;73(21):1796-1803.
22. da Silva A, Jr., Costa EC, Gomes JB, et al. Chronic headache and comorbidities: a two-phase, population-based, cross-sectional study. Headache. 2010;50(8):1306-1312.
23. Straube A, Pfaffenrath V, Ladwig KH, et al. Prevalence of chronic migraine and medication overuse headache in Germany--the German DMKG headache study. Cephalalgia. 2010;30(2):207-213.
24. Jonsson P, Hedenrud T, Linde M. Epidemiology of medication overuse headache in the general Swedish population. Cephalalgia. 2011;31(9):1015-1022.
25. Jonsson P, Linde M, Hensing G, Hedenrud T. Sociodemographic differences in medication use, health-care contacts and sickness absence among individuals with medication-overuse headache. J Headache Pain. 2012;13(4):281-290.
26. Linde M, Stovner LJ, Zwart JA, Hagen K. Time trends in the prevalence of headache disorders. The Nord-Trondelag Health Studies (HUNT 2 and HUNT 3). Cephalalgia. 2011;31(5):585-596.
27. Lipton RB, Manack A, Ricci JA, Chee E, Turkel CC, Winner P. Prevalence and burden of chronic migraine in adolescents: results of the chronic daily headache in adolescents study (C-dAS). Headache. 2011;51(5):693-706.
28. Ayzenberg I, Katsarava Z, Sborowski A, et al. The prevalence of primary headache disorders in Russia: a countrywide survey. Cephalalgia. 2012;32(5):373-381.
29. Ertas M, Baykan B, Orhan EK, et al. One-year prevalence and the impact of migraine and tension-type headache in Turkey: a nationwide home-based study in adults. J Headache Pain. 2012;13(2):147-157.
30. Hagen K, Linde M, Steiner TJ, Stovner LJ, Zwart JA. Risk factors for medication-overuse headache: an 11-year follow-up study. The Nord-Trondelag Health Studies. Pain. 2012;153(1):56-61.
31. Yu S, Liu R, Zhao G, et al. The prevalence and burden of primary headaches in China: a population-based door-to-door survey. Headache. 2012;52(4):582-591.
32. Shahbeigi S, Fereshtehnejad SM, Mohammadi N, et al. Epidemiology of headaches in Tehran urban area: a population-based cross-sectional study in district 8, year 2010. Neurol Sci. 2013;34(7):1157-66.
33. Schramm SH, Obermann M, Katsarava Z, Diener HC, Moebus S, Yoon MS. Epidemiological profiles of patients with chronic migraine and chronic tension-type headache. J Headache Pain. 2013;14:40.
34. Park JW, Moon HS, Kim JM, Lee KS, Chu MK. Chronic daily headache in Korea: prevalence, clinical characteristics, medical consultation and management. J Clin Neurol. 2014;10(3):236-243.
35. Kristoffersen ES, Lundqvist C. Medication-overuse headache: epidemiology, diagnosis and treatment. Ther Adv Drug Saf. 2014;5(2):87-99.
36. Steiner TJ, Stovner LJ, Katsarava Z, et al. The impact of headache in Europe: principal results of the Eurolight project. J Headache Pain. 2014;15:31.
37. Westergaard ML, Hansen EH, Glumer C, Jensen RH. Prescription pain medications and chronic headache in Denmark: implications for preventing medication overuse. Eur J Clin Pharmacol. 2015;71(7):851-860.
38. Bravo TP. Headaches of the elderly. Curr Neurol Neurosci Rep. 2015;15(6):30.
39. Mbewe E, Zairemthiama P, Yeh HH, Paul R, Birbeck GL, Steiner TJ. The epidemiology of primary headache disorders in Zambia: a population-based door-to-door survey. J Headache Pain. 2015;16:515.
40. Kulkarni GB, Rao GN, Gururaj G, Stovner LJ, Steiner TJ. Headache disorders and public ill-health in India: prevalence estimates in Karnataka State. J Headache Pain. 2015;16:67.
41. Westergaard ML, Glumer C, Hansen EH, Jensen RH. Medication overuse, healthy lifestyle behaviour and stress in chronic headache: Results from a population-based representative survey. Cephalalgia. 2016;36(1):15-28.
42. Manandhar K, Risal A, Linde M, Steiner TJ. The burden of headache disorders in Nepal: estimates from a population-based survey. J Headache Pain. 2015;17:3.
43. Zebenigus M, Tekle-Haimanot R, Worku DK, Thomas H, Steiner TJ. The prevalence of primary headache disorders in Ethiopia. J Headache Pain. 2016;17(1):110.
44. Al-Hashel JY, Ahmed SF, Alroughani R. Prevalence of Primary Headache Disorders in Kuwait. Neuroepidemiology. 2017;48(3-4):138-146.
45. Rastenyte D, Mickeviciene D, Stovner LJ, Thomas H, Andree C, Steiner TJ. Prevalence and burden of headache disorders in Lithuania and their public-health and policy implications: a population-based study within the Eurolight Project. J Headache Pain. 2017;18(1):53.
46. Henning V, Katsarava Z, Obermann M, Moebus S, Schramm S. Remission of chronic headache: Rates, potential predictors and the role of medication, follow-up results of the German Headache Consortium (GHC) Study. Cephalalgia. 2018;38(3):551-560.
47. Global Burden of Disease Neurological Disorders Collaborator Group. Global, regional, and national burden of neurological disorders during 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet Neurol. 2017;16(11):877-897.
Following the American Headache Society’s Scottsdale Headache Symposium in November 2018, MedPage Today posted an article which shared differing opinions from Drs. Hans-Christoph Diener and Elizabeth Loder on medication overuse headache (MOH). While Dr. Diener noted that “we can identify people with chronic migraine who are at risk to have medication overuse,” and that following successful withdrawal treatment “the majority of patients…revert to episodic migraine,” Dr. Loder pointed out that while MOH may exist and contribute to chronic migraine, “it is over-emphasized and the evidence in support of these concepts is weak.”
For this article, I’ve asked Drs. Marcelo Bigal, Rob Cowan, Jack Schim, and Stewart J. Tepper to share their perspectives on this topic. I also asked both Dr. Diener and Dr. Loder to expand on their comments. We will see Dr. Diener’s response to the article, but we did not hear back from Dr. Loder. Lastly, I will weigh in on the MOH discussion.
Marcelo Bigal, MD, PhD
Chief Medical Officer, Purdue Pharma
The issue of medication overuse headache (MOH) needs to be disentangled into a few separate but related issues. First, do excessive medications make migraine worse? Second, should MOH be considered a distinct form of headache? And how can evidence inform clinical practice?
Robust evidence supports the fact that excessive acute medication use is associated with increased headache frequency among migraineurs. In a large epidemiological study, we demonstrated that exposure (medication) precedes outcome (increased headache frequency).1 The risk was higher for barbiturates, followed by opioids and triptans, and was not increased by nonsteroidal anti-inflammatory drugs (NSAIDs). Dose response and critical exposure levels were identified. Based on this study and several others, we argued that criteria of causality had been demonstrated beyond reasonable doubt.2
However, since the effect is specific to migraine in that the exposure only increases the risk in migraineurs, not in individuals with other types of pain, we do not consider MOH a distinct entity. Instead, we believe that excessive medication is a risk factor for chronic migraine (CM). Therefore, we should be able to subdivide CM into 2 groups, one with and one without excessive medication use.
From a clinical perspective, physicians should monitor acute medication consumption in individuals with migraine and should be liberal in starting preventive therapy. In those with CM and excessive acute medication use we don’t advocate abrupt discontinuation of acute medications, since some preventive medications, especially the newer anti-calcitonin gene-related peptide (CGRP) antibodies, seem to work equally well in individuals with and without excessive use of medication,3 allowing more natural and gradual control of acute medication consumption without the need for detoxification.
Rob Cowan, MD, FAAN, FAHS
Higgins Professor of Neurology and Neurosciences
Chief, Division of Headache Medicine, Dept. of Neurology and Neurosciences
Director, Stanford University School of Medicine
As is often the case when 2 smart people take artificially imposed opposite positions, the truth will lie somewhere in the middle. I doubt either of the debaters would argue either extreme position: MOH does not exist, or MOH when present is solely responsible for chronic daily headache (CDH). The argument that the absence of controlled studies negates the proposition fails the common-sense test: Without a controlled study, we can’t be sure that wearing a helmet when bicycling is better than not. In such a case, observational data is sufficient. Could there be confounders (eg, helmet wearers are more inclined to ride safely)? Of course, but is that important? Similarly, does the fact that some MOH patients continue with CDH after cessation of medication overuse warrant a general de-emphasis? Certainly not for the third-to-half of patients who benefit from limiting medication use.
I suspect both Drs. Diener and Loder would agree that we would benefit from better markers of chronification and that earlier intervention with at-risk patients (eg, patients with increasing headache frequency, severity or duration but still in the episodic phase).
Jack Schim, MD
Co-Director, The Headache Center of Southern California
There has long been recognition that overuse of analgesic medications can be linked to progression of headache disorders. MOH was initially described by Dr. Lee Kudrow in 1982, in a chapter entitled, “Paradoxical effects of frequent analgesic use.”4 The most recent edition of the International Classification of Headache Disorders (ICHD-3) description does not entail features that imply causality. While there is epidemiologic observation of correlation between frequent analgesic use and progression of primary headache disorders, the causal relationship is often obscured by the facts. Overuse of acute medications is quite common in individuals with CM, but not all with CM overuse medications.
In the article being discussed, Drs. Diener and Loder reviewed facts and opinions. They helped clarify that while MOH is widely recognized, much of what is known is descriptive, and not based on solid science. From their presentations, we can conclude that we can recognize MOH based on ICHD-3 criteria, but we cannot tell an individual with chronic headache whether we can best help them by educating them, or by adjusting preventives, or both. The call to action is clear; we need to evaluate best therapeutic approaches in an empiric fashion. Our best new therapies for migraine prevention, CGRP mAbs, work for the majority of patients, with minimal side effects, even in the face of what has been considered MOH. Now, we need to strategize how best to approach these clinically challenged individuals. We need to avoid further stigmatizing our patients. Let’s recognize that our patients do not fail preventives, the prior preventives have failed our patients. Can the introduction of highly effective, well tolerated preventives at an earlier stage help avoid chronification that may drive medication overuse?
Stewart J. Tepper, MD, FAHS
Professor of Neurology, Geisel School of Medicine at Dartmouth
It is clear that overuse of some acute medication is detrimental to patient health. Examples of this include analgesic nephropathy or peptic ulcer disease, and exacerbation of depression with overuse of barbiturate compounds or benzodiazepines. Few doubt the health merits of reduction of acute medication overuse, regardless of whether the acute medications can be proven to transform episodic migraine (EM) to CM.
The good news is that the issues of the existence of true MOH and its proper management are rapidly becoming less important. OnabotulinumtoxinA use decreases triptan use in multiple randomized controlled trials for CM prevention.
Each of the anti-CGRP and anti-CGRP receptor monoclonal antibodies (mAbs) have been effective in preventing CM with medication overuse. All have lowered acute medication use, both triptans and analgesics. It is worth noting, however, that in both the OnabotulinumtoxinA and mAb trials, over-users of opioids and barbiturates were excluded. The mAbs converted patients from acute medication overuse to non-overuse, and from CM with medication overuse to EM without medication. These changes occurred without specific plans for weaning acute medication in place.
Accordingly, patients with CM with acute medication overuse should be treated with optimal prevention, and the evidence is strongest for use of the mAbs to both reduce mean monthly migraine days and all acute medication use, both triptans and analgesics. The new monoclonal antibody effectiveness may make the old arguments moot.
Hans-Christoph Diener, MD, PhD
University of Essen, Germany
I think no one doubts that MOH exists. The worldwide prevalence is between 1% and 2% (Table). The dilemma is that the diagnosis can only be made after the intake of acute medication has been reduced. There are confounders: migraine can improve irrespective of the reduction of acute medication and many physicians will implement migraine prevention at the time of withdrawal. No randomized trial compared the continuation of unchanged intake of medication to treat migraine attacks with reduction or withdrawal.
| Author (year) (reference) | Country | Age Group | Prevalence of MOH |
Castillo et al. (1999)7 | Spain | ≥ 14 | 1,2% |
Wang et al. (2000)8 | Taiwan | ≥ 65 | 1,0% |
Lu et al. (2001)9 | Taiwan | ≥ 15 | 1,1% |
Pascual et al. (2001)10 | Review |
| 1,0-1,9% |
Prencipe et al. (2001)11 | France | ≥ 65 | 1,7% |
Colas et al. (2004)12 | Spain | ≥ 14 | 1,5% |
Zwart et al. (2004)13 | Norway | ≥ 20 | 0,9-1,0% |
Dyb et al. (2006)14 | Norway | 13-18 | 0,2% |
Wang et al. (2006)15 | Taiwan | 12-14 | 0,3% |
Wiendels (2006)16 | Netherlands | 25-55 | 2,6% |
Stovner et al.(2007)17 | Review |
| 0,5-1,0% |
Aaseth et al. (2008, 2009)18,19 | Norway | 30-44 | 1,7% |
Rueda-Sanchez & Diaz-Martinez (2008)20 | Columbia | 18-65 | 4,5% |
Katsarava et al. (2009)21 | Georgia | ≥ 16 | 0,9% |
Da Silva et al. (2009)22 | Brazil | 10-93 | 1,6% |
Straube et al. (2010)23 | Germany | 18-88 | 1,0% |
Jonsson et al. (2011, 2012)24,25 | Sweden | ≥ 15 | 1,8% |
Linde et al. (2011)26 | Norway | ≥ 20 | 1,0% |
Lipton et al. (2011)27 | USA | 12-17 | 1,0% |
Ayzenberg et al. (2012)28 | Russia | 18-65 | 7,2% |
Ertas et al. (2012)29 | Turkey | 18-65 | 2,1% |
Hagen et al. (2012)30 | Norway | ≥ 20 | 0,8% |
Yu et al. (2012)31 | China | 18-65 | 0,9% |
Shahbeigi et al. (2013)32 | Iran | ≥ 10 | 4,9% |
Schramm et al. (2013)33 | Germany | 18-65 | 0,7% |
Park et al. (2014)34 | South Korea | 19-69 | 0,5% |
Kristoffersen & Lundqvist (2014)35 | Multinational summary |
| 1,0-2,0% |
Steiner (2014)36 | Multinational summary |
| 1,0-2,0% |
Westergaard et al. (2015)37 | Denmark |
| 0,5-7,2% |
Bravo (2015)38 | Multinational | Older | 1,0-7,1% |
Mbewe et al. (2015)39 | Zambia | 18-65 | 12,7% (adj. 7,1%) |
Kulkarni et al. (2015)40 | India | 18-65 | 1,2% |
Westergaard et al. (2016)41 | Denmark | ≥ 16 | 1,6% (adj. 1,8%) |
Manandhar et al. (2016)42 | Nepal | 18-65 | 2,2% |
Zebenigus et al. (2016)43 | Ethiopia | 18-65 | 0,8% (adj. 0,7%) |
Al-Hashel et al. (2017)44 | Kuwait | 18-65 | 2,4% |
Rastenyte et al. (2017)45 | Lithuania | 18-65 | 3,5% (adj. 3,2%) |
Henning et al. (2018)46 | Germany | 18-65 | 0,7% |
Global Burden of Disease 201747 | Global |
| 0,8% |
+++
Commentary by Alan M. Rapoport, MD
The above comments by my associates are very informative and help the reader to better understand the arguments about MOH. When Dr. Lee Kudrow taught me and my partner Dr. Fred Sheftell about the entity of analgesic and ergotamine overuse headaches in 1979, we set out to find those patients, observe and treat them. We did not have to wait long as so many patients with frequent and severe headaches came to see us with what we now term “medication overuse headache.” They told us that they had fewer headaches several years before and increased the use of acute care medications as their headaches increased in frequency. They were unaware of the probability that their headaches increased in frequency because their medication did. Some would argue that they increased their intake to feel better as the headache increased on their own.
Of course, we were not sure of the cause and effect, but we saw the result of tapering the acute care medications, whether or not we used preventives, hospitalized those patients or treated them with behavioral medicine approaches, etc. We observed that the combination of these treatments seemed to work better than just detox, but we did not do the proper studies to prove it. We also noticed that about 30% to 40% of patients did not improve as well as others, and daily or near-daily headaches continued, often of a lesser intensity. Almost all felt better in general and had fewer adverse events from the medication. The decrease in those medications was undoubtedly better for their brain function, livers and kidneys.
I do believe that medication overuse makes most patients with frequent EM or CM worse and we should educate patients to avoid it. I agree with Dr. Bigal that preventive medications may help some patients to improve despite the excessive use of acute care medication, but I am not sure that the older preventives work as well and certainly not as quickly as the newer ones. Recently I have seen the anti-CGRP mAbs work wonders with some of my patients who could not decrease their triptan intake. They just stop using the triptans as their headaches decrease on these therapies.
There is another interesting phenomenon that I have seen in practice—mostly with butalbital products, which I no longer prescribe. Forty years ago, patients would say that they only had 4 headaches per month lasting 1 to 2 days and I would prescribe 10 pills for them. They would call in 2 weeks and say they needed more. When queried they would invariably say it worked so well on the bad headaches and made them feel so much better, that they took 1 or 2 on days they thought they were going to get a headache and it prevented them from forming. They were soon taking it frequently and over time they were dependent on the medication, and then it stopped working and was difficult to withdraw.
Dr. Loder’s point that the studies on MOH have not proven that medication overuse causes it may be technically true; but it would be unethical to start patients on too much medication and randomize some to stay on and some to taper off. Dr. Kudrow came the closest by taking existing MOH patients and treating half with withdrawal and half of each with preventives. His breakthrough study in 1982 “proved” the existence of analgesic rebound and directed us to the best treatment at that time.4 This was the first study to examine the effect of stopping the overuse of medication to see the results.
Finally, I am unhappy that ICHD-3 has defined MOH only by number of days of medication use, not at all considering whether or not the patient develops a new type of headache, a worse type or more frequent headache (the way it was in previous versions). We have all seen patients taking 3 triptans per day on their own or with our suggestion, and many actually do better with no headache, for a period of time. This is medication overuse by definition, but not MOH, as they have little headache. But we do not recognize this entity.
The good news is, with education and anti-CGRP therapies, we will probably see less MOH in the future, or at least know better how to treat it.
+++
References
1. Bigal ME, Serrano D, Buse D, et al. Acute migraine medications and evolution from episodic to chronic migraine: a longitudinal population-based study. Headache. 2008;48(8):1157-68. doi: 10.1111/j.1526-4610.2008.01217.x. PubMed PMID: 18808500.
2. Bigal ME, Lipton RB. Overuse of acute migraine medications and migraine chronification. Curr Pain Headache Rep. 2009;13(4):301-7. PubMed PMID: 19586594.
3. Bigal ME, Edvinsson L, Rapoport AM, et al. Safety, tolerability, and efficacy of TEV-48125 for preventive treatment of chronic migraine: a multicentre, randomised, double-blind, placebo-controlled, phase 2b study. Lancet Neurol. 2015;14(11):1091-100. doi: 10.1016/S1474-4422(15)00245-8. PubMed PMID: 26432181.
4. Kudrow L. Paradoxical Effects of Frequent Analgesic Use. Advances in Neurology. 1982;33:335-341.
5. Diener HC, Holle D, Dresler T, Gaul C. Chronic Headache Due to Overuse of Analgesics and Anti-Migraine Agents. Dtsch Arztebl Int. 2018;115(22):365-370.
6. Westergaard ML, Glumer C, Hansen EH, Jensen RH. Prevalence of chronic headache with and without medication overuse: associations with socioeconomic position and physical and mental health status. Pain. 2014;155(10):2005-2013.
7. Castillo J, Munoz P, Guitera V, Pascual J. Epidemiology of chronic daily headache in the general population. Headache. 1999;39:190-196.
8. Wang SJ, Fuh JL, Lu SR, et al. Chronic daily headache in chinese elderly - prevalence, risk factors, and biannual follow-up. Neurology. 2000;54:314-319.
9. Lu SR, Fuh JL, Chen WT, Juang KD, Wang SJ. Chronic daily headache in Taipei, Taiwan: prevalence, follow-up and outcome predictors. Cephalalgia. 2001;21:980-986.
10. Pascual J, Colas R, Castillo J. Epidemiology of chronic daily headache. Curr Pain Headache Rep. 2001;5(6):529-536.
11. Prencipe M, Casini AR, Ferretti C, et al. Prevalence of headache in an elderly population: attack frequency, disability, and use of medication. J Neurol Neurosurg Psychiatry. 2001;70(3):377-381.
12. Colas R, Munoz P, Temprano R, Gomez C, Pascual J. Chronic daily headache with analgesic overuse: epidemiology and impact on quality of life. Neurology. 2004;62:1338-1342.
13. Zwart J, Dyb G, Hagen K, Svebak S, Stovner L, Holmen J. Analgesic overuse among subjects with headache, neck, and low back pain. Neurology. 2004;62:1540-1544.
14. Dyb G, Holmen TL, Zwart JA. Analgesic overuse among adolescents with headache: the Head-HUNT-Youth Study. Neurology. 2006;66(2):198-201.
15. Wang SJ, Fuh JL, Lu SR, Juang KD. Chronic daily headache in adolescents: prevalence, impact, and medication overuse. Neurology. 2006;66(2):193-197.
16. Wiendels NJ, Knuistingh NA, Rosendaal FR, et al. Chronic frequent headache in the general population: prevalence and associated factors. Cephalalgia. 2006;26(12):1434-1442.
17. Stovner L, Hagen K, Jensen R, et al. The global burden of headache: a documentation of headache prevalence and disability worldwide. Cephalalgia. 2007;27(3):193-210.
18. Aaseth K, Grande RB, Kvaerner KJ, Gulbrandsen P, Lundqvist C, Russell MB. Prevalence of secondary chronic headaches in a population-based sample of 30-44-year-old persons. The Akershus study of chronic headache. Cephalalgia. 2008;28(7):705-713.
19. Aaseth K, Grande RB, Lundqvist C, Russell MB. What is chronic headache in the general population? The Akershus study of chronic headache. Acta Neurol Scand Suppl. 2009;(189):30-32.
20. Rueda-Sanchez M, Diaz-Martinez LA. Prevalence and associated factors for episodic and chronic daily headache in the Colombian population. Cephalalgia. 2008;28(3):216-225.
21. Katsarava Z, Dzagnidze A, Kukava M, et al. Primary headache disorders in the Republic of Georgia: prevalence and risk factors. Neurology. 2009;73(21):1796-1803.
22. da Silva A, Jr., Costa EC, Gomes JB, et al. Chronic headache and comorbidities: a two-phase, population-based, cross-sectional study. Headache. 2010;50(8):1306-1312.
23. Straube A, Pfaffenrath V, Ladwig KH, et al. Prevalence of chronic migraine and medication overuse headache in Germany--the German DMKG headache study. Cephalalgia. 2010;30(2):207-213.
24. Jonsson P, Hedenrud T, Linde M. Epidemiology of medication overuse headache in the general Swedish population. Cephalalgia. 2011;31(9):1015-1022.
25. Jonsson P, Linde M, Hensing G, Hedenrud T. Sociodemographic differences in medication use, health-care contacts and sickness absence among individuals with medication-overuse headache. J Headache Pain. 2012;13(4):281-290.
26. Linde M, Stovner LJ, Zwart JA, Hagen K. Time trends in the prevalence of headache disorders. The Nord-Trondelag Health Studies (HUNT 2 and HUNT 3). Cephalalgia. 2011;31(5):585-596.
27. Lipton RB, Manack A, Ricci JA, Chee E, Turkel CC, Winner P. Prevalence and burden of chronic migraine in adolescents: results of the chronic daily headache in adolescents study (C-dAS). Headache. 2011;51(5):693-706.
28. Ayzenberg I, Katsarava Z, Sborowski A, et al. The prevalence of primary headache disorders in Russia: a countrywide survey. Cephalalgia. 2012;32(5):373-381.
29. Ertas M, Baykan B, Orhan EK, et al. One-year prevalence and the impact of migraine and tension-type headache in Turkey: a nationwide home-based study in adults. J Headache Pain. 2012;13(2):147-157.
30. Hagen K, Linde M, Steiner TJ, Stovner LJ, Zwart JA. Risk factors for medication-overuse headache: an 11-year follow-up study. The Nord-Trondelag Health Studies. Pain. 2012;153(1):56-61.
31. Yu S, Liu R, Zhao G, et al. The prevalence and burden of primary headaches in China: a population-based door-to-door survey. Headache. 2012;52(4):582-591.
32. Shahbeigi S, Fereshtehnejad SM, Mohammadi N, et al. Epidemiology of headaches in Tehran urban area: a population-based cross-sectional study in district 8, year 2010. Neurol Sci. 2013;34(7):1157-66.
33. Schramm SH, Obermann M, Katsarava Z, Diener HC, Moebus S, Yoon MS. Epidemiological profiles of patients with chronic migraine and chronic tension-type headache. J Headache Pain. 2013;14:40.
34. Park JW, Moon HS, Kim JM, Lee KS, Chu MK. Chronic daily headache in Korea: prevalence, clinical characteristics, medical consultation and management. J Clin Neurol. 2014;10(3):236-243.
35. Kristoffersen ES, Lundqvist C. Medication-overuse headache: epidemiology, diagnosis and treatment. Ther Adv Drug Saf. 2014;5(2):87-99.
36. Steiner TJ, Stovner LJ, Katsarava Z, et al. The impact of headache in Europe: principal results of the Eurolight project. J Headache Pain. 2014;15:31.
37. Westergaard ML, Hansen EH, Glumer C, Jensen RH. Prescription pain medications and chronic headache in Denmark: implications for preventing medication overuse. Eur J Clin Pharmacol. 2015;71(7):851-860.
38. Bravo TP. Headaches of the elderly. Curr Neurol Neurosci Rep. 2015;15(6):30.
39. Mbewe E, Zairemthiama P, Yeh HH, Paul R, Birbeck GL, Steiner TJ. The epidemiology of primary headache disorders in Zambia: a population-based door-to-door survey. J Headache Pain. 2015;16:515.
40. Kulkarni GB, Rao GN, Gururaj G, Stovner LJ, Steiner TJ. Headache disorders and public ill-health in India: prevalence estimates in Karnataka State. J Headache Pain. 2015;16:67.
41. Westergaard ML, Glumer C, Hansen EH, Jensen RH. Medication overuse, healthy lifestyle behaviour and stress in chronic headache: Results from a population-based representative survey. Cephalalgia. 2016;36(1):15-28.
42. Manandhar K, Risal A, Linde M, Steiner TJ. The burden of headache disorders in Nepal: estimates from a population-based survey. J Headache Pain. 2015;17:3.
43. Zebenigus M, Tekle-Haimanot R, Worku DK, Thomas H, Steiner TJ. The prevalence of primary headache disorders in Ethiopia. J Headache Pain. 2016;17(1):110.
44. Al-Hashel JY, Ahmed SF, Alroughani R. Prevalence of Primary Headache Disorders in Kuwait. Neuroepidemiology. 2017;48(3-4):138-146.
45. Rastenyte D, Mickeviciene D, Stovner LJ, Thomas H, Andree C, Steiner TJ. Prevalence and burden of headache disorders in Lithuania and their public-health and policy implications: a population-based study within the Eurolight Project. J Headache Pain. 2017;18(1):53.
46. Henning V, Katsarava Z, Obermann M, Moebus S, Schramm S. Remission of chronic headache: Rates, potential predictors and the role of medication, follow-up results of the German Headache Consortium (GHC) Study. Cephalalgia. 2018;38(3):551-560.
47. Global Burden of Disease Neurological Disorders Collaborator Group. Global, regional, and national burden of neurological disorders during 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet Neurol. 2017;16(11):877-897.
FDA: More safety data needed for 12 sunscreen active ingredients
including some of those frequently used in over-the-counter products.
The ingredients requiring additional investigation are cinoxate, dioxybenzone, ensulizole, homosalate, meradimate, octinoxate, octisalate, octocrylene, padimate O, sulisobenzone, oxybenzone, and avobenzone. The FDA actions were announced during a press briefing Feb. 21 held to discuss the proposed rule to update regulatory requirements for most sunscreen products marketed in the United States.
There are no urgent safety matters associated with these ingredients. The rule is part of FDA’s charge to construct an over-the-counter (OTC) monograph detailing all available data on sunscreen ingredients, as required by the Sunscreen Innovation Act.
OTC monographs establish conditions under which ingredients may be marketed without approved new drug applications because they are generally recognized as safe and effective (GRASE) “and not misbranded,” according to the FDA. The proposed rule classifies active ingredients and other conditions as Category I (proposed to be GRASE and not misbranded), Category II (proposed to be not GRASE or to be misbranded), or Category III (additional data needed).
“We are proposing that these ingredients require additional data before a positive GRASE determination can be made,” FDA press officer Sandy Walsh said in an interview, referring to the 12 ingredients. “This proposed rule does not represent a conclusion by the FDA that the sunscreen active ingredients proposed as having insufficient data are unsafe for use in sunscreens. Rather, we are requesting additional information on these ingredients so that we can evaluate their GRASE status in light of changed conditions, including substantially increased sunscreen usage and evolving information about the potential risks associated with these products since they were originally evaluated.”
Among its provisions, the proposal addresses sunscreen active-ingredient safety, dosage forms, and sun protection factor (SPF) and broad-spectrum requirements. It also proposes updates to how products are labeled to make it easier for consumers to identify key product information
Thus far, the agency says that only two active ingredients – titanium dioxide and zinc oxide – can be marketed without approved new drug applications because they are GRASE.
However, two other ingredients – PABA and trolamine salicylate – are not GRASE for use in sunscreens because of safety issues, Theresa Michele, MD, director of the Division of Nonprescription Drug Products Division of Nonprescription Drug Products in the FDA’s Center for Drug Evaluation and Research. Products that combine sunscreen and insect repellent also not fit the criteria, she said
“There are 12 ingredients for which there are insufficient safety data to make a positive GRASE determination at this time. To address these 12 ingredients, the FDA is asking industry and other interested parties for additional data. The FDA is working closely with industry and has published several guidances to make sure companies understand what data the agency believes is necessary for the FDA to evaluate safety and effectiveness for sunscreen active ingredients, including the 12 ingredients for which the FDA is seeking more data,” she said.
In addition to seeking these additional data, the rule also proposes the following:
- Dosage forms that are GRASE for use as sunscreens should include sprays, oils, lotions, creams, gels, butters, pastes, ointments, and sticks. While powders are proposed to be eligible for inclusion in the monograph, more data are being requested before powders are included. “Wipes, towelettes, body washes, shampoos, and other dosage forms are proposed to be categorized as new drugs because the FDA has not received data showing they are eligible for inclusion in the monograph,” according to the FDA statement outlining the proposed regulation.
- The maximum proposed SPF value on sunscreen labels should be raised from SPF 50 or higher to SPF 60 or higher. “There are not enough data to suggest that consumers get any extra benefit from products with an SPF of more than 60,” Dr. Michele said.
- Sunscreens with an SPF value of 15 or higher should be required to also provide broad-spectrum protection, and for broad-spectrum products, as SPF increases, the magnitude of protection against UVA radiation should also increase. “These proposals are designed to ensure that these products provide consumers with the protections that they expect,” the statement said.
- New sunscreen product labels should be required to make it easier for consumers to identify important information, “including the addition of the active ingredients on the front of the package to bring sunscreen in line with other OTC drugs; a notification on the front label for consumers to read the skin cancer/skin aging alert for sunscreens that have not been shown to help prevent skin cancer; and revised formats for SPF, broad spectrum, and water resistance statements,” the statement said.
- Products that combine sunscreens with insect repellents are not GRASE.
In the meantime, though, consumers should continue to use sunscreens regularly as part of a comprehensive sun protection program, FDA Commissioner Scott Gottlieb, MD, said during the briefing. “Broad spectrum sunscreens with SPF values of at least 15 are critical to the arsenal of tools for preventing skin cancer and protecting the skin from damage caused by the sun’s rays,” he continued. “Given the recognized public health benefits of sunscreen use, Americans should continue to use sunscreens in conjunction with other sun protective measures (such as protective clothing) as this important rule-making effort moves forward.”
To submit comments on this proposed rule, go to https://www.regulations.gov and follow instructions for submitting comments.
including some of those frequently used in over-the-counter products.
The ingredients requiring additional investigation are cinoxate, dioxybenzone, ensulizole, homosalate, meradimate, octinoxate, octisalate, octocrylene, padimate O, sulisobenzone, oxybenzone, and avobenzone. The FDA actions were announced during a press briefing Feb. 21 held to discuss the proposed rule to update regulatory requirements for most sunscreen products marketed in the United States.
There are no urgent safety matters associated with these ingredients. The rule is part of FDA’s charge to construct an over-the-counter (OTC) monograph detailing all available data on sunscreen ingredients, as required by the Sunscreen Innovation Act.
OTC monographs establish conditions under which ingredients may be marketed without approved new drug applications because they are generally recognized as safe and effective (GRASE) “and not misbranded,” according to the FDA. The proposed rule classifies active ingredients and other conditions as Category I (proposed to be GRASE and not misbranded), Category II (proposed to be not GRASE or to be misbranded), or Category III (additional data needed).
“We are proposing that these ingredients require additional data before a positive GRASE determination can be made,” FDA press officer Sandy Walsh said in an interview, referring to the 12 ingredients. “This proposed rule does not represent a conclusion by the FDA that the sunscreen active ingredients proposed as having insufficient data are unsafe for use in sunscreens. Rather, we are requesting additional information on these ingredients so that we can evaluate their GRASE status in light of changed conditions, including substantially increased sunscreen usage and evolving information about the potential risks associated with these products since they were originally evaluated.”
Among its provisions, the proposal addresses sunscreen active-ingredient safety, dosage forms, and sun protection factor (SPF) and broad-spectrum requirements. It also proposes updates to how products are labeled to make it easier for consumers to identify key product information
Thus far, the agency says that only two active ingredients – titanium dioxide and zinc oxide – can be marketed without approved new drug applications because they are GRASE.
However, two other ingredients – PABA and trolamine salicylate – are not GRASE for use in sunscreens because of safety issues, Theresa Michele, MD, director of the Division of Nonprescription Drug Products Division of Nonprescription Drug Products in the FDA’s Center for Drug Evaluation and Research. Products that combine sunscreen and insect repellent also not fit the criteria, she said
“There are 12 ingredients for which there are insufficient safety data to make a positive GRASE determination at this time. To address these 12 ingredients, the FDA is asking industry and other interested parties for additional data. The FDA is working closely with industry and has published several guidances to make sure companies understand what data the agency believes is necessary for the FDA to evaluate safety and effectiveness for sunscreen active ingredients, including the 12 ingredients for which the FDA is seeking more data,” she said.
In addition to seeking these additional data, the rule also proposes the following:
- Dosage forms that are GRASE for use as sunscreens should include sprays, oils, lotions, creams, gels, butters, pastes, ointments, and sticks. While powders are proposed to be eligible for inclusion in the monograph, more data are being requested before powders are included. “Wipes, towelettes, body washes, shampoos, and other dosage forms are proposed to be categorized as new drugs because the FDA has not received data showing they are eligible for inclusion in the monograph,” according to the FDA statement outlining the proposed regulation.
- The maximum proposed SPF value on sunscreen labels should be raised from SPF 50 or higher to SPF 60 or higher. “There are not enough data to suggest that consumers get any extra benefit from products with an SPF of more than 60,” Dr. Michele said.
- Sunscreens with an SPF value of 15 or higher should be required to also provide broad-spectrum protection, and for broad-spectrum products, as SPF increases, the magnitude of protection against UVA radiation should also increase. “These proposals are designed to ensure that these products provide consumers with the protections that they expect,” the statement said.
- New sunscreen product labels should be required to make it easier for consumers to identify important information, “including the addition of the active ingredients on the front of the package to bring sunscreen in line with other OTC drugs; a notification on the front label for consumers to read the skin cancer/skin aging alert for sunscreens that have not been shown to help prevent skin cancer; and revised formats for SPF, broad spectrum, and water resistance statements,” the statement said.
- Products that combine sunscreens with insect repellents are not GRASE.
In the meantime, though, consumers should continue to use sunscreens regularly as part of a comprehensive sun protection program, FDA Commissioner Scott Gottlieb, MD, said during the briefing. “Broad spectrum sunscreens with SPF values of at least 15 are critical to the arsenal of tools for preventing skin cancer and protecting the skin from damage caused by the sun’s rays,” he continued. “Given the recognized public health benefits of sunscreen use, Americans should continue to use sunscreens in conjunction with other sun protective measures (such as protective clothing) as this important rule-making effort moves forward.”
To submit comments on this proposed rule, go to https://www.regulations.gov and follow instructions for submitting comments.
including some of those frequently used in over-the-counter products.
The ingredients requiring additional investigation are cinoxate, dioxybenzone, ensulizole, homosalate, meradimate, octinoxate, octisalate, octocrylene, padimate O, sulisobenzone, oxybenzone, and avobenzone. The FDA actions were announced during a press briefing Feb. 21 held to discuss the proposed rule to update regulatory requirements for most sunscreen products marketed in the United States.
There are no urgent safety matters associated with these ingredients. The rule is part of FDA’s charge to construct an over-the-counter (OTC) monograph detailing all available data on sunscreen ingredients, as required by the Sunscreen Innovation Act.
OTC monographs establish conditions under which ingredients may be marketed without approved new drug applications because they are generally recognized as safe and effective (GRASE) “and not misbranded,” according to the FDA. The proposed rule classifies active ingredients and other conditions as Category I (proposed to be GRASE and not misbranded), Category II (proposed to be not GRASE or to be misbranded), or Category III (additional data needed).
“We are proposing that these ingredients require additional data before a positive GRASE determination can be made,” FDA press officer Sandy Walsh said in an interview, referring to the 12 ingredients. “This proposed rule does not represent a conclusion by the FDA that the sunscreen active ingredients proposed as having insufficient data are unsafe for use in sunscreens. Rather, we are requesting additional information on these ingredients so that we can evaluate their GRASE status in light of changed conditions, including substantially increased sunscreen usage and evolving information about the potential risks associated with these products since they were originally evaluated.”
Among its provisions, the proposal addresses sunscreen active-ingredient safety, dosage forms, and sun protection factor (SPF) and broad-spectrum requirements. It also proposes updates to how products are labeled to make it easier for consumers to identify key product information
Thus far, the agency says that only two active ingredients – titanium dioxide and zinc oxide – can be marketed without approved new drug applications because they are GRASE.
However, two other ingredients – PABA and trolamine salicylate – are not GRASE for use in sunscreens because of safety issues, Theresa Michele, MD, director of the Division of Nonprescription Drug Products Division of Nonprescription Drug Products in the FDA’s Center for Drug Evaluation and Research. Products that combine sunscreen and insect repellent also not fit the criteria, she said
“There are 12 ingredients for which there are insufficient safety data to make a positive GRASE determination at this time. To address these 12 ingredients, the FDA is asking industry and other interested parties for additional data. The FDA is working closely with industry and has published several guidances to make sure companies understand what data the agency believes is necessary for the FDA to evaluate safety and effectiveness for sunscreen active ingredients, including the 12 ingredients for which the FDA is seeking more data,” she said.
In addition to seeking these additional data, the rule also proposes the following:
- Dosage forms that are GRASE for use as sunscreens should include sprays, oils, lotions, creams, gels, butters, pastes, ointments, and sticks. While powders are proposed to be eligible for inclusion in the monograph, more data are being requested before powders are included. “Wipes, towelettes, body washes, shampoos, and other dosage forms are proposed to be categorized as new drugs because the FDA has not received data showing they are eligible for inclusion in the monograph,” according to the FDA statement outlining the proposed regulation.
- The maximum proposed SPF value on sunscreen labels should be raised from SPF 50 or higher to SPF 60 or higher. “There are not enough data to suggest that consumers get any extra benefit from products with an SPF of more than 60,” Dr. Michele said.
- Sunscreens with an SPF value of 15 or higher should be required to also provide broad-spectrum protection, and for broad-spectrum products, as SPF increases, the magnitude of protection against UVA radiation should also increase. “These proposals are designed to ensure that these products provide consumers with the protections that they expect,” the statement said.
- New sunscreen product labels should be required to make it easier for consumers to identify important information, “including the addition of the active ingredients on the front of the package to bring sunscreen in line with other OTC drugs; a notification on the front label for consumers to read the skin cancer/skin aging alert for sunscreens that have not been shown to help prevent skin cancer; and revised formats for SPF, broad spectrum, and water resistance statements,” the statement said.
- Products that combine sunscreens with insect repellents are not GRASE.
In the meantime, though, consumers should continue to use sunscreens regularly as part of a comprehensive sun protection program, FDA Commissioner Scott Gottlieb, MD, said during the briefing. “Broad spectrum sunscreens with SPF values of at least 15 are critical to the arsenal of tools for preventing skin cancer and protecting the skin from damage caused by the sun’s rays,” he continued. “Given the recognized public health benefits of sunscreen use, Americans should continue to use sunscreens in conjunction with other sun protective measures (such as protective clothing) as this important rule-making effort moves forward.”
To submit comments on this proposed rule, go to https://www.regulations.gov and follow instructions for submitting comments.
Who is least adherent to statins, and more
This week in MDedge Cardiocast: Silent strokes are pretty common after noncardiac surgery, troubling news about nonadherence to statins, what cardiologists need to know about ARVC, and how gender inequality in medicine affects the health of ALL women.
This week in MDedge Cardiocast: Silent strokes are pretty common after noncardiac surgery, troubling news about nonadherence to statins, what cardiologists need to know about ARVC, and how gender inequality in medicine affects the health of ALL women.
This week in MDedge Cardiocast: Silent strokes are pretty common after noncardiac surgery, troubling news about nonadherence to statins, what cardiologists need to know about ARVC, and how gender inequality in medicine affects the health of ALL women.
A.I. and U
There is a good chance that your car is equipped with a backup camera. It also may have sensors that alert you when there is another vehicle in one of your blind spots. These wonders of modern technology simply are vision enhancers much like an x-ray or an ultrasound. The sensors merely collect visual data, but the decision of what should be done with this additional information is up to you, just as you decide how to respond to your patient’s lab work and imaging studies.
If you have more disposable income than I do, you may have a vehicle that not only gathers information but also makes decisions based on what it senses by slowing down, applying the brakes, or adjusting the steering. My friends who own these semi-autonomous cars generally have given these control systems positive grades once they have experienced a few events in which the vehicle took over in what it considered a dangerous situation. However, even my friends who are fans of their semi-autonomous cars are uncomfortable about the widespread introduction of fully autonomous vehicles.
The practice of medicine is riding the crest of this same wave of artificial intelligence that promises, or some might say threatens, to remove humans from the driver’s seat (“A.I. Shows Promise Assisting Physicians,” by Cade Metz, The New York Times, Feb. 11, 2019). As reported in the New York Times, a team of physicians has created a system capable of making diagnoses based on a “neural network” that uses complex computer algorithms to learn by analyzing extremely large amounts of data. Once this system had been “taught” to identify certain medical conditions in EMRs, the team tasked the system with analyzing the records of nearly 600,000 patients at a women and children’s hospital in southern China. The investigators claim that the system was able to diagnose asthma with more than 90% accuracy, while physicians can diagnose with an accuracy of 80%-94%, and the system diagnosed gastrointestinal disease with 87% accuracy, well within the physicians’ accuracy range of 82%-90%.
Does this apparent success for A.I. mean that not only will you be vacating your place behind the wheel of your car, but also taking down your shingle and hanging up your stethoscope? Before you rush out and sign up for a federally-funded retraining program, you should remember that this study was done in China, where the privacy laws are somewhat skimpy and the data more voluminous by several scales of magnitude than here. Replicating their results and However, this report should serve as wake-up call to those of you who believe that making diagnoses is at the core of what makes you a physician. If sorting through pages of data to arrive at an explanation for your patients’ complaints is the intellectual challenge that keeps the practice of medicine fresh and exciting, you may want to start looking for other sources of mental stimulation.
A.I. isn’t going to replace the primary care physician. There still will need to be someone available at the initial point of contact who can do a physical exam, take, or at least review, the patient’s history, and then order the lab work and imaging studies that the A.I. system will use to make the diagnosis. In other words, the physician will be primarily responsible for data collection. You may feel that you are almost there already.
Will there be new roles for primary care physicians once A.I. systems are making the diagnoses? It is hard to imagine a fully autonomous health care system in which physicians completely disappear. But, now is the time to think seriously about how we are going to reinvent ourselves to adapt to the inevitable changes and continue as an (or could be "the") essential human element in an increasingly automated system.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at pdnews@mdedge.com.
There is a good chance that your car is equipped with a backup camera. It also may have sensors that alert you when there is another vehicle in one of your blind spots. These wonders of modern technology simply are vision enhancers much like an x-ray or an ultrasound. The sensors merely collect visual data, but the decision of what should be done with this additional information is up to you, just as you decide how to respond to your patient’s lab work and imaging studies.
If you have more disposable income than I do, you may have a vehicle that not only gathers information but also makes decisions based on what it senses by slowing down, applying the brakes, or adjusting the steering. My friends who own these semi-autonomous cars generally have given these control systems positive grades once they have experienced a few events in which the vehicle took over in what it considered a dangerous situation. However, even my friends who are fans of their semi-autonomous cars are uncomfortable about the widespread introduction of fully autonomous vehicles.
The practice of medicine is riding the crest of this same wave of artificial intelligence that promises, or some might say threatens, to remove humans from the driver’s seat (“A.I. Shows Promise Assisting Physicians,” by Cade Metz, The New York Times, Feb. 11, 2019). As reported in the New York Times, a team of physicians has created a system capable of making diagnoses based on a “neural network” that uses complex computer algorithms to learn by analyzing extremely large amounts of data. Once this system had been “taught” to identify certain medical conditions in EMRs, the team tasked the system with analyzing the records of nearly 600,000 patients at a women and children’s hospital in southern China. The investigators claim that the system was able to diagnose asthma with more than 90% accuracy, while physicians can diagnose with an accuracy of 80%-94%, and the system diagnosed gastrointestinal disease with 87% accuracy, well within the physicians’ accuracy range of 82%-90%.
Does this apparent success for A.I. mean that not only will you be vacating your place behind the wheel of your car, but also taking down your shingle and hanging up your stethoscope? Before you rush out and sign up for a federally-funded retraining program, you should remember that this study was done in China, where the privacy laws are somewhat skimpy and the data more voluminous by several scales of magnitude than here. Replicating their results and However, this report should serve as wake-up call to those of you who believe that making diagnoses is at the core of what makes you a physician. If sorting through pages of data to arrive at an explanation for your patients’ complaints is the intellectual challenge that keeps the practice of medicine fresh and exciting, you may want to start looking for other sources of mental stimulation.
A.I. isn’t going to replace the primary care physician. There still will need to be someone available at the initial point of contact who can do a physical exam, take, or at least review, the patient’s history, and then order the lab work and imaging studies that the A.I. system will use to make the diagnosis. In other words, the physician will be primarily responsible for data collection. You may feel that you are almost there already.
Will there be new roles for primary care physicians once A.I. systems are making the diagnoses? It is hard to imagine a fully autonomous health care system in which physicians completely disappear. But, now is the time to think seriously about how we are going to reinvent ourselves to adapt to the inevitable changes and continue as an (or could be "the") essential human element in an increasingly automated system.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at pdnews@mdedge.com.
There is a good chance that your car is equipped with a backup camera. It also may have sensors that alert you when there is another vehicle in one of your blind spots. These wonders of modern technology simply are vision enhancers much like an x-ray or an ultrasound. The sensors merely collect visual data, but the decision of what should be done with this additional information is up to you, just as you decide how to respond to your patient’s lab work and imaging studies.
If you have more disposable income than I do, you may have a vehicle that not only gathers information but also makes decisions based on what it senses by slowing down, applying the brakes, or adjusting the steering. My friends who own these semi-autonomous cars generally have given these control systems positive grades once they have experienced a few events in which the vehicle took over in what it considered a dangerous situation. However, even my friends who are fans of their semi-autonomous cars are uncomfortable about the widespread introduction of fully autonomous vehicles.
The practice of medicine is riding the crest of this same wave of artificial intelligence that promises, or some might say threatens, to remove humans from the driver’s seat (“A.I. Shows Promise Assisting Physicians,” by Cade Metz, The New York Times, Feb. 11, 2019). As reported in the New York Times, a team of physicians has created a system capable of making diagnoses based on a “neural network” that uses complex computer algorithms to learn by analyzing extremely large amounts of data. Once this system had been “taught” to identify certain medical conditions in EMRs, the team tasked the system with analyzing the records of nearly 600,000 patients at a women and children’s hospital in southern China. The investigators claim that the system was able to diagnose asthma with more than 90% accuracy, while physicians can diagnose with an accuracy of 80%-94%, and the system diagnosed gastrointestinal disease with 87% accuracy, well within the physicians’ accuracy range of 82%-90%.
Does this apparent success for A.I. mean that not only will you be vacating your place behind the wheel of your car, but also taking down your shingle and hanging up your stethoscope? Before you rush out and sign up for a federally-funded retraining program, you should remember that this study was done in China, where the privacy laws are somewhat skimpy and the data more voluminous by several scales of magnitude than here. Replicating their results and However, this report should serve as wake-up call to those of you who believe that making diagnoses is at the core of what makes you a physician. If sorting through pages of data to arrive at an explanation for your patients’ complaints is the intellectual challenge that keeps the practice of medicine fresh and exciting, you may want to start looking for other sources of mental stimulation.
A.I. isn’t going to replace the primary care physician. There still will need to be someone available at the initial point of contact who can do a physical exam, take, or at least review, the patient’s history, and then order the lab work and imaging studies that the A.I. system will use to make the diagnosis. In other words, the physician will be primarily responsible for data collection. You may feel that you are almost there already.
Will there be new roles for primary care physicians once A.I. systems are making the diagnoses? It is hard to imagine a fully autonomous health care system in which physicians completely disappear. But, now is the time to think seriously about how we are going to reinvent ourselves to adapt to the inevitable changes and continue as an (or could be "the") essential human element in an increasingly automated system.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at pdnews@mdedge.com.
Pseudoscience redux
My most recent column discussed the problem of pseudoscience that pervades some corners of the Internet. Personally, I respond to pseudoscience primarily by trying to provide accurate and less-biased information. I recognize that not everyone approaches decision making by seeking more information. When dealing a diverse public, a medical professional needs to have other approaches in the armamentarium.1 When dealing with other physicians, I am less flexible. Either the profession of medicine believes in science or it doesn’t.
Since that column was published, there have been major developments. There are measles outbreaks in the states of Washington and New York, and more than 100 deaths from a measles epidemic in the Philippines. The World Health Organization has made vaccine hesitancy one of its ten threats to global health in 2019.
Facebook has indicated that it might demote the priority and frequency with which it recommends articles that promulgate anti-vax information and conspiracy theories.2 Facebook isn’t doing this because it has had an epiphany; it has come under pressure for its role in the spread of misinformation. Current legislation was written before the rise of social media, when Internet Service Providers were primarily conduits to transfer bits and bytes between computers. Those ISPs were not liable for the content of the transmitted Web pages. Facebook, by producing what it called a newsfeed and by making personalized suggestions for other websites to browse, doesn’t fit the passive model of an ISP.
For alleged violations of user’s privacy, Facebook might be subject to billion dollar fines, according to a Washington Post article.3 Still, for a company whose revenue is $4 billion per month and whose stock market value is $400 billion, paying a billion dollar fine for years of alleged misbehaviors that have enabled it to become a giant empire is, “in the scheme of things ... a speeding ticket” in the parlance of the penultimate scene of the movie The Social Network. The real financial risk is people deciding they can’t trust the platform and going elsewhere.
Authorities in the United Kingdom in February 2019 released a highly critical, 108-page report about fake news, which said, “Facebook should not be allowed to behave like ‘digital gangsters’ in the online world.”4 The U.K. report urges new regulations to deal with privacy breaches and with fake news. It endeavors to create a duty for social media companies to combat the spread of misinformation.
Then the Wall Street Journal reported that Pinterest has stopped returning results for searches related to vaccination.5 Pinterest realized that most of the shared images on its platform cautioned against vaccination, which contradicts the recommendations of medical experts. Unable to otherwise combat the flow of misinformation, the company apparently has decided to eliminate returning results, pro or con, for any search terms related to vaccines.
While lamenting the public’s inability to distinguish misinformation on the Internet, I’ve also been observing the factors that lead physicians astray. I expect physicians, as trained scientists and as professionals, to be able to assimilate new information and change their practices accordingly. Those who do research on the translation of technology find that, this doesn’t happen with any regularity.
The February 2019 issue of Hospital Pediatrics has four items on the topic of treating bronchiolitis, including two research articles, a brief report, and a commentary. That is obviously a relevant topic this time of year. The impression after reading those four items is that hospitalists don’t really know how to best treat the most common illness they encounter. And even when they “know” how to do it, many factors distort the science. Those factors are highlighted in the article on barriers to minimizing viral testing.6
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@mdedge.com.
References
1. “Discussing immunization with vaccine-hesitant parents requires caring, individualized approach,” by Jeff Craven, Pediatric News, Nov. 7, 2018; “How do you get anti-vaxxers to vaccinate their kids? Talk to them – for hours,” by Nadine Gartner, Washington Post, Feb. 19, 2019.
2. “Facebook will consider removing or demoting anti-vaccination recommendations amid backlash,” by Taylor Telford, Washington Post, Feb. 15, 2019.
3. “U.S. regulators have met to discuss imposing a record-setting fine against Facebook for privacy violations,” by Tony Romm and Elizabeth Dwoskin, Washington Post, Jan. 18, 2019; “Report: Facebook, FTC discussing ‘multibillion dollar’ fine,” by Associated Press.
4. “Disinformation and ‘fake news’: Final Report,” House of Commons, Feb. 18, 2019, p. 42, item 139.
5. “Pinterest blocks vaccination searches in move to control the conversation,” by Robert McMillan and Daniela Hernandez, The Wall Street Journal, Feb. 20, 2019.
6. “Barriers to minimizing respiratory viral testing in bronchiolitis: Physician perceptions on testing practices,” by MZ Huang et al. Hospital Pediatrics 2019 Feb. doi: 10.1542/hpeds.2018-0108.
My most recent column discussed the problem of pseudoscience that pervades some corners of the Internet. Personally, I respond to pseudoscience primarily by trying to provide accurate and less-biased information. I recognize that not everyone approaches decision making by seeking more information. When dealing a diverse public, a medical professional needs to have other approaches in the armamentarium.1 When dealing with other physicians, I am less flexible. Either the profession of medicine believes in science or it doesn’t.
Since that column was published, there have been major developments. There are measles outbreaks in the states of Washington and New York, and more than 100 deaths from a measles epidemic in the Philippines. The World Health Organization has made vaccine hesitancy one of its ten threats to global health in 2019.
Facebook has indicated that it might demote the priority and frequency with which it recommends articles that promulgate anti-vax information and conspiracy theories.2 Facebook isn’t doing this because it has had an epiphany; it has come under pressure for its role in the spread of misinformation. Current legislation was written before the rise of social media, when Internet Service Providers were primarily conduits to transfer bits and bytes between computers. Those ISPs were not liable for the content of the transmitted Web pages. Facebook, by producing what it called a newsfeed and by making personalized suggestions for other websites to browse, doesn’t fit the passive model of an ISP.
For alleged violations of user’s privacy, Facebook might be subject to billion dollar fines, according to a Washington Post article.3 Still, for a company whose revenue is $4 billion per month and whose stock market value is $400 billion, paying a billion dollar fine for years of alleged misbehaviors that have enabled it to become a giant empire is, “in the scheme of things ... a speeding ticket” in the parlance of the penultimate scene of the movie The Social Network. The real financial risk is people deciding they can’t trust the platform and going elsewhere.
Authorities in the United Kingdom in February 2019 released a highly critical, 108-page report about fake news, which said, “Facebook should not be allowed to behave like ‘digital gangsters’ in the online world.”4 The U.K. report urges new regulations to deal with privacy breaches and with fake news. It endeavors to create a duty for social media companies to combat the spread of misinformation.
Then the Wall Street Journal reported that Pinterest has stopped returning results for searches related to vaccination.5 Pinterest realized that most of the shared images on its platform cautioned against vaccination, which contradicts the recommendations of medical experts. Unable to otherwise combat the flow of misinformation, the company apparently has decided to eliminate returning results, pro or con, for any search terms related to vaccines.
While lamenting the public’s inability to distinguish misinformation on the Internet, I’ve also been observing the factors that lead physicians astray. I expect physicians, as trained scientists and as professionals, to be able to assimilate new information and change their practices accordingly. Those who do research on the translation of technology find that, this doesn’t happen with any regularity.
The February 2019 issue of Hospital Pediatrics has four items on the topic of treating bronchiolitis, including two research articles, a brief report, and a commentary. That is obviously a relevant topic this time of year. The impression after reading those four items is that hospitalists don’t really know how to best treat the most common illness they encounter. And even when they “know” how to do it, many factors distort the science. Those factors are highlighted in the article on barriers to minimizing viral testing.6
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@mdedge.com.
References
1. “Discussing immunization with vaccine-hesitant parents requires caring, individualized approach,” by Jeff Craven, Pediatric News, Nov. 7, 2018; “How do you get anti-vaxxers to vaccinate their kids? Talk to them – for hours,” by Nadine Gartner, Washington Post, Feb. 19, 2019.
2. “Facebook will consider removing or demoting anti-vaccination recommendations amid backlash,” by Taylor Telford, Washington Post, Feb. 15, 2019.
3. “U.S. regulators have met to discuss imposing a record-setting fine against Facebook for privacy violations,” by Tony Romm and Elizabeth Dwoskin, Washington Post, Jan. 18, 2019; “Report: Facebook, FTC discussing ‘multibillion dollar’ fine,” by Associated Press.
4. “Disinformation and ‘fake news’: Final Report,” House of Commons, Feb. 18, 2019, p. 42, item 139.
5. “Pinterest blocks vaccination searches in move to control the conversation,” by Robert McMillan and Daniela Hernandez, The Wall Street Journal, Feb. 20, 2019.
6. “Barriers to minimizing respiratory viral testing in bronchiolitis: Physician perceptions on testing practices,” by MZ Huang et al. Hospital Pediatrics 2019 Feb. doi: 10.1542/hpeds.2018-0108.
My most recent column discussed the problem of pseudoscience that pervades some corners of the Internet. Personally, I respond to pseudoscience primarily by trying to provide accurate and less-biased information. I recognize that not everyone approaches decision making by seeking more information. When dealing a diverse public, a medical professional needs to have other approaches in the armamentarium.1 When dealing with other physicians, I am less flexible. Either the profession of medicine believes in science or it doesn’t.
Since that column was published, there have been major developments. There are measles outbreaks in the states of Washington and New York, and more than 100 deaths from a measles epidemic in the Philippines. The World Health Organization has made vaccine hesitancy one of its ten threats to global health in 2019.
Facebook has indicated that it might demote the priority and frequency with which it recommends articles that promulgate anti-vax information and conspiracy theories.2 Facebook isn’t doing this because it has had an epiphany; it has come under pressure for its role in the spread of misinformation. Current legislation was written before the rise of social media, when Internet Service Providers were primarily conduits to transfer bits and bytes between computers. Those ISPs were not liable for the content of the transmitted Web pages. Facebook, by producing what it called a newsfeed and by making personalized suggestions for other websites to browse, doesn’t fit the passive model of an ISP.
For alleged violations of user’s privacy, Facebook might be subject to billion dollar fines, according to a Washington Post article.3 Still, for a company whose revenue is $4 billion per month and whose stock market value is $400 billion, paying a billion dollar fine for years of alleged misbehaviors that have enabled it to become a giant empire is, “in the scheme of things ... a speeding ticket” in the parlance of the penultimate scene of the movie The Social Network. The real financial risk is people deciding they can’t trust the platform and going elsewhere.
Authorities in the United Kingdom in February 2019 released a highly critical, 108-page report about fake news, which said, “Facebook should not be allowed to behave like ‘digital gangsters’ in the online world.”4 The U.K. report urges new regulations to deal with privacy breaches and with fake news. It endeavors to create a duty for social media companies to combat the spread of misinformation.
Then the Wall Street Journal reported that Pinterest has stopped returning results for searches related to vaccination.5 Pinterest realized that most of the shared images on its platform cautioned against vaccination, which contradicts the recommendations of medical experts. Unable to otherwise combat the flow of misinformation, the company apparently has decided to eliminate returning results, pro or con, for any search terms related to vaccines.
While lamenting the public’s inability to distinguish misinformation on the Internet, I’ve also been observing the factors that lead physicians astray. I expect physicians, as trained scientists and as professionals, to be able to assimilate new information and change their practices accordingly. Those who do research on the translation of technology find that, this doesn’t happen with any regularity.
The February 2019 issue of Hospital Pediatrics has four items on the topic of treating bronchiolitis, including two research articles, a brief report, and a commentary. That is obviously a relevant topic this time of year. The impression after reading those four items is that hospitalists don’t really know how to best treat the most common illness they encounter. And even when they “know” how to do it, many factors distort the science. Those factors are highlighted in the article on barriers to minimizing viral testing.6
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at pdnews@mdedge.com.
References
1. “Discussing immunization with vaccine-hesitant parents requires caring, individualized approach,” by Jeff Craven, Pediatric News, Nov. 7, 2018; “How do you get anti-vaxxers to vaccinate their kids? Talk to them – for hours,” by Nadine Gartner, Washington Post, Feb. 19, 2019.
2. “Facebook will consider removing or demoting anti-vaccination recommendations amid backlash,” by Taylor Telford, Washington Post, Feb. 15, 2019.
3. “U.S. regulators have met to discuss imposing a record-setting fine against Facebook for privacy violations,” by Tony Romm and Elizabeth Dwoskin, Washington Post, Jan. 18, 2019; “Report: Facebook, FTC discussing ‘multibillion dollar’ fine,” by Associated Press.
4. “Disinformation and ‘fake news’: Final Report,” House of Commons, Feb. 18, 2019, p. 42, item 139.
5. “Pinterest blocks vaccination searches in move to control the conversation,” by Robert McMillan and Daniela Hernandez, The Wall Street Journal, Feb. 20, 2019.
6. “Barriers to minimizing respiratory viral testing in bronchiolitis: Physician perceptions on testing practices,” by MZ Huang et al. Hospital Pediatrics 2019 Feb. doi: 10.1542/hpeds.2018-0108.
Experts: Consider enteral therapy in CD, with caveats
LAS VEGAS – Temporarily switching to an enteral diet – without solid food – has the potential to reverse Crohn’s disease (CD), especially in children, a panel of experts told gastroenterologists here.
They acknowledged the controversial treatment requires strict adherence and can be impossible for some patients to tolerate. But it can be successful too, said gastroenterologist Lindsey G. Albenberg, DO, of Children’s Hospital of Philadelphia, where enteral nutrition therapy (ENT) is commonly used in patients with CD.
“Parents are obviously thrilled that there’s no exposure to immunosuppressive medications,” she said in a discussion about ENT at the Crohn’s & Colitis Congress - a partnership of the Crohn’s & Colitis Foundation and the American Gastroenterological Association. “Typically, we provide 80%-90% of calorie needs through a polymeric formula by mouth. If we see clinical response at 4-6 weeks or even earlier, then we will pursue a course of about 8-12 weeks.”
Research into the best role for ENT therapy in CD is limited. A 2018 Cochrane Library review found there’s “very low quality evidence” suggesting that ENT is better than steroids to induce remission in children. It also found there’s “very low quality evidence” that steroids are better than ENT in adults with CD (Cochrane Database Syst Rev. 2018 Apr 1. doi: 10.1002/14651858.CD000542.pub3).
According to clinician-scientist James D. Lewis, MD, MSCE, of the University of Pennsylvania, Philadelphia, ENT “has gotten a bad name in some ways because of a meta-analysis showing it was inferior to corticosteroids to induce remission.” In fact, he said, studies “didn’t look at mucosal healing and pooled together adults and children.”
In children, he said, the treatment seems to clearly be effective. The picture is less promising in adults. “Presumably that’s because those of you who are parents probably have more control over your young children than your own behavior,” he said, referring to management of food intake.
In adults, “there’s no reason to think it wouldn’t work,” he said. “But trying to convince adults to give up food is really challenging.”
Children who try ENT are often required to use a nasogastric feeding tube, an approach that adults tend to avoid. In kids, “it’s a question of knowing your patient,” said gastroenterologist David Suskind, MD, of Seattle Children’s Hospital. “If the patient says, ‘There’s no way you’ll put a nasal gastric tube in, and no way I will drink it [the ENT supplement],’ this may not be the best therapy. If they’re interested, we push forward. We get much better efficacy because the patients will do what we’re asking.”
Several panelists recommended that patients use polymeric formulations instead of elemental formulations because they’re more palatable. It can be a struggle, however, to stick with the treatment.
Kelly Issokson, MS, RD, CNSC, a dietitian with Cedars-Sinai Medical Center in Los Angeles, tried an ENT therapy for 30 days in order to understand what patients experience and said it was “very challenging.”
“When you sit down to a meal, you anticipate it, you start to salivate. With shakes, it was a lot more clinical,” she said. “The other thing I struggled with was texture and having it be so sweet. I’d freeze [the shakes] into ice cube trays and popsicles. That helped break the monotony. It changes the flavor and cuts the sweetness.”
Ms. Issokson urges her patients to stick with ENT for the entire period of therapy. “Studies show when patients introduce real foods the efficacy of inducing remission goes down. We recommend 100% calories and proteins coming from the formula,” she said. That means “no coffee, no broth, no tea, no nothing but the formula. Most of our patients are able to do that exclusively.”
Toward the end of therapy, around week 8 or 11, some patients tell her they crave food like soup. “I say OK, have a tiny bit,” she said, “but remember, this is only temporary. We’re almost at the end. Try to be 100% exclusive.”
Dr. Albenberg and Dr. Suskind report no disclosures. Ms. Issokson reports consulting fees (speaking and teaching) from AGA, Crohn’s & Colitis Foundation, Academy of Nutrition and Dietetics, and United Ostomy Association. Dr. Lewis reports many relationships – including consulting fees, ownership interest, and grant/research support – with Eli Lilly, Bristol‐Myers Squibb, Gilead, and others.
Correction, 2/22/19: An earlier version of this article misidentified the person in the first photo above.
LAS VEGAS – Temporarily switching to an enteral diet – without solid food – has the potential to reverse Crohn’s disease (CD), especially in children, a panel of experts told gastroenterologists here.
They acknowledged the controversial treatment requires strict adherence and can be impossible for some patients to tolerate. But it can be successful too, said gastroenterologist Lindsey G. Albenberg, DO, of Children’s Hospital of Philadelphia, where enteral nutrition therapy (ENT) is commonly used in patients with CD.
“Parents are obviously thrilled that there’s no exposure to immunosuppressive medications,” she said in a discussion about ENT at the Crohn’s & Colitis Congress - a partnership of the Crohn’s & Colitis Foundation and the American Gastroenterological Association. “Typically, we provide 80%-90% of calorie needs through a polymeric formula by mouth. If we see clinical response at 4-6 weeks or even earlier, then we will pursue a course of about 8-12 weeks.”
Research into the best role for ENT therapy in CD is limited. A 2018 Cochrane Library review found there’s “very low quality evidence” suggesting that ENT is better than steroids to induce remission in children. It also found there’s “very low quality evidence” that steroids are better than ENT in adults with CD (Cochrane Database Syst Rev. 2018 Apr 1. doi: 10.1002/14651858.CD000542.pub3).
According to clinician-scientist James D. Lewis, MD, MSCE, of the University of Pennsylvania, Philadelphia, ENT “has gotten a bad name in some ways because of a meta-analysis showing it was inferior to corticosteroids to induce remission.” In fact, he said, studies “didn’t look at mucosal healing and pooled together adults and children.”
In children, he said, the treatment seems to clearly be effective. The picture is less promising in adults. “Presumably that’s because those of you who are parents probably have more control over your young children than your own behavior,” he said, referring to management of food intake.
In adults, “there’s no reason to think it wouldn’t work,” he said. “But trying to convince adults to give up food is really challenging.”
Children who try ENT are often required to use a nasogastric feeding tube, an approach that adults tend to avoid. In kids, “it’s a question of knowing your patient,” said gastroenterologist David Suskind, MD, of Seattle Children’s Hospital. “If the patient says, ‘There’s no way you’ll put a nasal gastric tube in, and no way I will drink it [the ENT supplement],’ this may not be the best therapy. If they’re interested, we push forward. We get much better efficacy because the patients will do what we’re asking.”
Several panelists recommended that patients use polymeric formulations instead of elemental formulations because they’re more palatable. It can be a struggle, however, to stick with the treatment.
Kelly Issokson, MS, RD, CNSC, a dietitian with Cedars-Sinai Medical Center in Los Angeles, tried an ENT therapy for 30 days in order to understand what patients experience and said it was “very challenging.”
“When you sit down to a meal, you anticipate it, you start to salivate. With shakes, it was a lot more clinical,” she said. “The other thing I struggled with was texture and having it be so sweet. I’d freeze [the shakes] into ice cube trays and popsicles. That helped break the monotony. It changes the flavor and cuts the sweetness.”
Ms. Issokson urges her patients to stick with ENT for the entire period of therapy. “Studies show when patients introduce real foods the efficacy of inducing remission goes down. We recommend 100% calories and proteins coming from the formula,” she said. That means “no coffee, no broth, no tea, no nothing but the formula. Most of our patients are able to do that exclusively.”
Toward the end of therapy, around week 8 or 11, some patients tell her they crave food like soup. “I say OK, have a tiny bit,” she said, “but remember, this is only temporary. We’re almost at the end. Try to be 100% exclusive.”
Dr. Albenberg and Dr. Suskind report no disclosures. Ms. Issokson reports consulting fees (speaking and teaching) from AGA, Crohn’s & Colitis Foundation, Academy of Nutrition and Dietetics, and United Ostomy Association. Dr. Lewis reports many relationships – including consulting fees, ownership interest, and grant/research support – with Eli Lilly, Bristol‐Myers Squibb, Gilead, and others.
Correction, 2/22/19: An earlier version of this article misidentified the person in the first photo above.
LAS VEGAS – Temporarily switching to an enteral diet – without solid food – has the potential to reverse Crohn’s disease (CD), especially in children, a panel of experts told gastroenterologists here.
They acknowledged the controversial treatment requires strict adherence and can be impossible for some patients to tolerate. But it can be successful too, said gastroenterologist Lindsey G. Albenberg, DO, of Children’s Hospital of Philadelphia, where enteral nutrition therapy (ENT) is commonly used in patients with CD.
“Parents are obviously thrilled that there’s no exposure to immunosuppressive medications,” she said in a discussion about ENT at the Crohn’s & Colitis Congress - a partnership of the Crohn’s & Colitis Foundation and the American Gastroenterological Association. “Typically, we provide 80%-90% of calorie needs through a polymeric formula by mouth. If we see clinical response at 4-6 weeks or even earlier, then we will pursue a course of about 8-12 weeks.”
Research into the best role for ENT therapy in CD is limited. A 2018 Cochrane Library review found there’s “very low quality evidence” suggesting that ENT is better than steroids to induce remission in children. It also found there’s “very low quality evidence” that steroids are better than ENT in adults with CD (Cochrane Database Syst Rev. 2018 Apr 1. doi: 10.1002/14651858.CD000542.pub3).
According to clinician-scientist James D. Lewis, MD, MSCE, of the University of Pennsylvania, Philadelphia, ENT “has gotten a bad name in some ways because of a meta-analysis showing it was inferior to corticosteroids to induce remission.” In fact, he said, studies “didn’t look at mucosal healing and pooled together adults and children.”
In children, he said, the treatment seems to clearly be effective. The picture is less promising in adults. “Presumably that’s because those of you who are parents probably have more control over your young children than your own behavior,” he said, referring to management of food intake.
In adults, “there’s no reason to think it wouldn’t work,” he said. “But trying to convince adults to give up food is really challenging.”
Children who try ENT are often required to use a nasogastric feeding tube, an approach that adults tend to avoid. In kids, “it’s a question of knowing your patient,” said gastroenterologist David Suskind, MD, of Seattle Children’s Hospital. “If the patient says, ‘There’s no way you’ll put a nasal gastric tube in, and no way I will drink it [the ENT supplement],’ this may not be the best therapy. If they’re interested, we push forward. We get much better efficacy because the patients will do what we’re asking.”
Several panelists recommended that patients use polymeric formulations instead of elemental formulations because they’re more palatable. It can be a struggle, however, to stick with the treatment.
Kelly Issokson, MS, RD, CNSC, a dietitian with Cedars-Sinai Medical Center in Los Angeles, tried an ENT therapy for 30 days in order to understand what patients experience and said it was “very challenging.”
“When you sit down to a meal, you anticipate it, you start to salivate. With shakes, it was a lot more clinical,” she said. “The other thing I struggled with was texture and having it be so sweet. I’d freeze [the shakes] into ice cube trays and popsicles. That helped break the monotony. It changes the flavor and cuts the sweetness.”
Ms. Issokson urges her patients to stick with ENT for the entire period of therapy. “Studies show when patients introduce real foods the efficacy of inducing remission goes down. We recommend 100% calories and proteins coming from the formula,” she said. That means “no coffee, no broth, no tea, no nothing but the formula. Most of our patients are able to do that exclusively.”
Toward the end of therapy, around week 8 or 11, some patients tell her they crave food like soup. “I say OK, have a tiny bit,” she said, “but remember, this is only temporary. We’re almost at the end. Try to be 100% exclusive.”
Dr. Albenberg and Dr. Suskind report no disclosures. Ms. Issokson reports consulting fees (speaking and teaching) from AGA, Crohn’s & Colitis Foundation, Academy of Nutrition and Dietetics, and United Ostomy Association. Dr. Lewis reports many relationships – including consulting fees, ownership interest, and grant/research support – with Eli Lilly, Bristol‐Myers Squibb, Gilead, and others.
Correction, 2/22/19: An earlier version of this article misidentified the person in the first photo above.
EXPERT ANALYSIS FROM THE CROHN’S & COLITIS CONGRESS